Healthcare Quarterly
Patient/Provider Internet Connectivity: Leading the Revolution of Healthcare Delivery
Abstract
Current Market Trends
Healthcare in the United States is transforming in fundamental
ways. Recent trends in the healthcare industry include:
- Rapid consolidation of care provision
- Increased managed care penetration
- Increased focus on quality improvement and performance
measurement
- A growing sense of "consumerism" among the beneficiaries of the care system
Provision of healthcare is in the process of becoming a more efficient operation as healthcare providers and payers explore new ways to become more efficient and sophisticated, and reduce costs while focusing on quality improvement and outcomes. Faced with the pressures of managed care, organizations have developed performance measurement and quality improvement tools such as disease management and care management programs that are now common in managed care and hospital settings. At the same time, patients, increasingly frustrated with the healthcare system, have started to approach their healthcare decisions with the same sense of "consumerism" with which they approach other purchases. This new era of patient involvement has increased the level of responsibility consumers take in their own care and has raised the expectations for quality improvements in healthcare delivery.
Fortunately, the trends currently transforming the healthcare delivery system have been paralleled and enabled by recent developments in Information Technology (IT). Historically the healthcare industry has been slow to adopt and invest in this type of technology. However, the Internet's low cost, ease of use and flexibility can provide the platform to support dramatic changes in the healthcare industry. Powerful IT systems are the tools needed to empower healthcare providers to do their jobs more effectively and efficiently. The development of such systems has allowed healthcare providers, managed-care organizations, employers and other players in the healthcare industry to consolidate and organize information, to use this information in clinical settings and to have speedy access to this information. IT systems have evolved from basic administrative and financial management tools to systems which have become an integral component of the care-delivery model. Use of these information systems has empowered the healthcare industry to quickly and accurately convey clinical information amongst its constituents with a "need to know"- the patient, the provider and the payer.
The Internet: A Tool in Care Management Programs
Faced with cost-savings pressures, providers and payers have explored new interventions that will keep patients away from costly healthcare services while maintaining the quality of care. Among these new interventions is a trend towards care management programs.The goals of care management programs are to contain costs while increasing the quality of care, providing early proactive intervention with educational programs, and preventing costly exacerbation of disease. For instance, active patient monitoring and self-management of chronic conditions has been shown to dramatically affect chronic disease outcomes (Diabetes Control and Complications Trial Research Group 1993; NIH 1991, 1993). Many studies have provided a basis for the establishment and maturation of care management programs at the patient level and disease management programs at the population level.
However to implement such programs successfully, certain
challenges need to be addressed. These include enhanced
communication between patients, physicians and providers and timely
acquisition of data to monitor a patient's health status. This is
no easy task and requires effective information management. Several
technologies have emerged based on new approaches to
patient/provider communication such as:
- Web-database systems
- Interactive voice response (IVR) systems
- Nurse call centers utilizing computerized systems
- Modem enabled technologies for transfer of electronic medical data from patients to healthcare providers.
Today, the Internet's ability to provide low-cost access and information exchange amongst all of the healthcare constituents (providers, payers, pharmacies and consumers) and support enhanced communication is significantly increasing the impact of such care management programs.
Healthcare electronic data interchange (EDI) started to gain
momentum in the mid- to late-1980's with the automation of pharmacy
claims, and later, physician claims. IT can provide even greater
benefit, however, when it supports flexible information exchange,
not just simple, standardizable transaction processing. In disease
management, for instance, there has been an emergence of the
following types of IT, each of which supports important information
exchange:
- Telephone technology
- Computer networks
- "Smart" devices
Today, the Internet creates the ideal platform for disease
management applications by facilitating communication between
patients, providers and payers. Some of the Internet's
characteristics are:
- Easy access to information
- Two-way communication
- Flexibility and timeliness
- Cross platform connectivity
- Low cost
The Internet as a Care Management Communication Platform
One important use of the Internet will be to create an ideal communication platform for disease management applications that improve outcomes and care management. This will be achieved by interactivity amongst patients, providers and payers, enabling and enhancing:- Rapid and accurate candidate identification
- Personalized outreach capabilities
- Interoperability with delivery environments
- Dynamic response capability
- Systematic data collection and analysis
Of note, some emerging healthcare companies already are
developing and implementing Internet-enabled solutions for managed
care organizations, providers and patients. These companies share a
common goal: The use of improved information management strategies
to solve real problems in the healthcare delivery environment. Such
companies include:
- Active Health: Performs real-time multi-stream clinical data set analysis and identifies intervention opportunities. This helps providers detect important clinical situations where there may be a more effective or safer therapeutic approach available.
- NaviMedix: Provides Internet-enabled administrative and clinical workflow support at the physician's office. This allows the ambulatory office to be the hub of a communications matrix that includes the patient, the provider, the payer, pharmacies and other suppliers.
- Health Hero: Provides an Internet-based solution designed to improve the quality of care while reducing its cost. The company offers a flexible, easy-to-deploy value-added communication platform that can serve as the foundation for new disease management program or supplement and extend such programs. This allows for monitoring, education and effective intervention, leading to better medical management and outcomes assessment.
The above approaches are intriguing, inasmuch as potential
benefits extend to patients, providers, and insurers. At the most
basic level, these strategies significantly reduce the
administrative costs associated with both care and resource
management. But there are clear clinical benefits as
well:
- Patients who interact more frequently with their providers report satisfaction in managing their everyday regimen, increased convenience and self-empowerment.
- For physicians, increased data collection and communication with their patients enables them to spend more time teaching and motivating patients - thereby preventing acute disease episodes - and less time managing them.
- For insurers, financial benefits to health plans are obvious if diseases are better managed via the use of technology. Additional benefits include operational efficiency and decreased cost for collection of information.
- Other benefits include the ability to measure and survey member satisfaction and to screen for high-risk patients and help implement, enhance and focus the delivery of disease management interventions.
Care management programs typically involve the use of a wide array of information management and decision support tools to identify and assess a patient's health status and to deploy, measure and track specific strategic interventions. They also rely on technologies that leverage extensive hardware and software infrastructures, i.e., web-database systems and modem-enabled technologies for transfer of electronic medical data from patients to healthcare providers. But most importantly, these programs rely on effective and frequent communication between patients and providers, for which Internet-based infrastructure is an ideal platform.
Patient/Provider Connectivity: Extending Care Management to the Patient's Home
Chronic medical conditions are costly for society and for the individual. Of the 100 million Americans with chronic medical conditions, 12 million are unable to fully conduct normal daily activities. The cost to society reached an annual expenditure of about $1.2 trillion in 1998. The active involvement of the patient in the treatment of these conditions promotes effective outcomes and prevents exacerbation of the chronic condition. Behavioral modification is a critical goal of the patient's self-involvement in its own care. These changes might vary from smoking cessation to participation in home monitoring and self-management of cardiovascular disease. Key elements for successfully assisting patients with self-management and compliance include:- Educating the patient about why and how to change behaviors or
participate in their treatment
- Monitoring the actual degree of compliance with recommended
behavioral changes
- Monitoring treatment and disease progression
- Providing motivational feedback to the patient, with rewards for compliance and notification for noncompliance
Intensive communication between the patient and the healthcare provider is one of the most important processes for affecting self-management and compliance. However, as we've discussed, communication is also the most challenging factor in a healthcare system - it is labor-intensive and expensive. It requires synchronization between the caregiver and patient. The following model describes the use of a new Internet-based disease management communication platform.
CHF Disease Management Program Using Internet-Based Communication Platform: A Case Study
A CHF disease management program was conducted by the Santa Clara County Individual Practice Association (SCCIPA), the eighth largest IPA in California including over 800 physicians responsible for 125,000 HMO members. The pilot study focused on 52 patients with CHF handled by one nurse care manager.The pilot study examined the effectiveness of a disease management program utilizing an Internet-based communication platform connecting the healthcare provider directly to the patient at home. The platform leverages the Internet and advancements in microelectronics to create an improved communication infrastructure allowing a cost-effective, highly efficient, two-way communication link between caregivers and patients. This platform increases patient/provider connectivity and empowers the nurse/care manager to collect, analyze, and report on the day-to-day condition of patients in the home. It allows for quick identification of changes in patients' health conditions and fosters management by exception, thereby focusing on those patients in need of immediate intervention.
Program Objectives
On the caregiver side, the objective was to determine the effectiveness of a disease management program using an Internet-based communication platform and how the technology enables the care provider to:- Track weight, blood pressure, edema and shortness of
breath
- Track diet and medication compliance
- Facilitate timely follow-up care:
- Appointments/screenings
- Medications and lab results
- Appointments/screenings
- Advise and educate each patient every day
- Use on-call advice triage nights and weekends
- Encourage wellness classes
From the patient side, this program was developed as very
personal and engaging to promote their involvement in their own
care and by evaluating such parameters as:
- Self-monitoring of vital signs
- Medication and program compliance
- Better involvement and participation in one's own
care
- Education and information
How the Health Hero Internet-Based Communication Platform Works
Each patient receives a personal information appliance that he or she simply plugs into a phone line. The design of the appliance is the result of extensive evaluation with diverse age groups including young, elderly and disabled patients. The device is extremely easy-to-use and is designed for achieving high patient compliance, especially to a senior population.The appliance gathers quantitative and qualitative patient information through simple question-and-answer sessions that are transmitted to the device over normal telephone lines from a data center. The patients view questions and information on a brightly lit, high-contrast liquid crystal display, and respond via four large buttons. Once the device is plugged into both electrical and phone outlets, it begins by walking the patient through a brief, repeatable training exercise designed to give the patient an opportunity to practice answering the range of questions they will encounter in their sessions. When it is properly connected, the device will prompt the patient that everything is okay and instruct the patient to check back for the first session per instructions given by the care manager. That evening, the appliance will re-connect to the network, the day's session will be downloaded, and the device will be ready for patient interaction.
To load and transmit patient information, the appliance calls the data center via a toll-free telephone number. The data center, which houses the website and database servers, is developed in conjunction with and managed by EDS. The data center is a distributed data management system designed to handle 2,000,000 patient connections daily. The central patient database is online, storing all patient updates and metric data, and is accessible only by authorized medical personnel. The data center uses both the Netscape Enterprise web server and the BEA Weblogic application server to serve HTTPS pages. All data is encrypted to the 128-bit RSA standards. In accordance with industry standards, the hardware, software and database are designed with appropriate redundancy and high security. The service provider and the data center's operations staff handle high-level account administration. Clients are responsible for their own system administration (primarily creating and updating patient and client account information).
The data center is programmed to transmit patient information collected during the previous day and receive new information and questions for the coming day. The question types include multiple choice, extended multiple choice, range, numeric, prompt, escalate, read meter and reminders. This information and all patient medical data are transmitted between the service data center and the user's PC using two different protocols. User ID's, passwords, and patient reports are transmitted as Web pages using HTTPS protocol. Web-based applications used by the care manager to interact with the patients communicate with the data center using Enterprise Java Beans (EJB) via the Secure Socket Layer (SSL) protocol. The care manager accesses these applications through a password-protected website using Explorer or Netscape Navigator web browser software. The web-based applications allow him or her to track patient status via an Internet connection and collect information, analyze patient's health status, and report on the day-to-day condition of patients in the home. Formal training is available to instruct in the use of these web-based tools and the website. Additionally, online documentation, training, Frequently Asked Questions (FAQ) and technical tips are accessible 24 hours through the website.
Specific applications currently available include:
- Care Administrator™: This application enables care
managers to enroll a patient, initiating an automatic fulfillment
of a patient's appliance and performing other routine
administrative functions
- Care Director™: This application enables an authorized
care manager or physician to access patient data and send queries
to patients. This provides a view of the patient population,
stratified by risk, sorting patient data daily. This allows the
care manager to identify those patients who are currently at risk
or who require attention.
- Care Composer™: This application enables the care manager to write or adapt queries to their own specific requirements or to specific disease states and store them in the data center.
More specifically, these applications enable the care manager
to:
- Easily query patient populations creating their own
personalized questionnaire or template using Care
Composer™
- Analyze patient responses and alerts and customize sessions for
individuals using Care Director™
- Review patient trends and receive notifications of escalation
or failure of patient response. All online patient results can be
retrieved individually or in aggregate form across groups of
patients for viewing and further analysis in tables and
graphs.
- Present population and patient reports to physicians. Reports can be stored as files or printed after creation. The care manager communicates specific clinical parameters/events to primary care practitioners and cardiologists by phone, fax and/or email. Additionally, patient response data, including dialogues, questions and answers, and metric data, can be exported from the system. IT programs can be developed, by or for customers or licensees, to export patient results for integration into an off-line database. Patient confidentiality is protected through rigorous authorization and validation, and data encryption.
How the CHF Program Works
Traditionally, patient care is based on episodic encounters between patients and their care providers. Working from the website, the SCCIPA care manager interacts with patients by assigning daily, pre-defined queries customized to the patient's needs. The dialogue used by SCCIPA includes questions related to heart failure and queries about the patient's functional health status. The software sorts patients' responses according to risk levels defined by the caregiver. Color coded risk alerts allow the provider to, at-a-glance, quickly determine if a patient needs immediate intervention. One advantage of this system is that if CHF patients enter information correctly and there are no abnormal readings, the nurse does not need to call the patients. This leaves more time for the nurse to spend with patients who really need the one-on-one assistance.Technology-driven disease management programs, leveraging the
power of the Internet, provide key value components such
as:
- Cost-effectiveness approach
- Reliable assessment tools
- Centralized data management and retrieval
- Patient follow-up
- Management by exception


Study Preliminary Results
The participants were asked about:- Their attitudes and opinions regarding the maintenance of their
health and living with CHF
- Their self-management behavior
- Their knowledge of self-management
- Their satisfaction with the personal information appliance
The preliminary evaluation was based on data for compliance and patient satisfaction collected in August 1999 through telephone interviews, site visits and data analysis. In summary, this study suggests that increased communication between patients and providers can improve patient's perceived quality of life and compliance to a sometimes very demanding health program.
Compliance: The data collected shows that patients who plug their device in the phone line and start using the appliance use it almost everyday, missing about one day in nine on average. In addition, the study collected information on patient's compliance to specific CHF diet (Figure 1) and showed a real improvement in patients' overall compliance to their diet. Compliance is defined in the study by the number of days that a non-hospitalized patient or a group of patients answered the survey (Figure 2). Compliance is very important to measure, as it in fact may compromise outcomes if a patient doesn't respond. The absence of response makes it difficult for a care manager to identify problems early on and prevent hospitalizations. Furthermore, low compliance may increase care management costs due to increased number of interventions necessary to manage the patient.
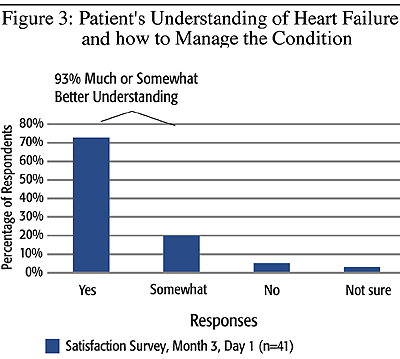
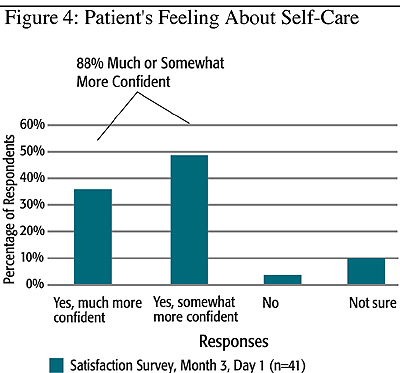
Patient Satisfaction: The result of the evaluation showed that 93% of patients have a much or somewhat better understanding of heart failure and how to manage the condition (Figure 3). Additionally,88% of patients feel much or somewhat more confident in taking care of their condition as a results of the program (Figure 4).
Although data has not yet been collected for medical outcomes
and cost-savings for this specific case study, other studies have
demonstrated that remote patient monitoring facilitates earlier
interventions and eliminates emergency visits and hospitalizations
and decreases cost of care. For instance, a Pediatric Asthma
Self-Management Program (Reissiger et al. 1998), combining
education, nursing assessment and series of surveys
reported:
- 61% reduction in hospitalization
- 46% reduction in physicians visits
- Estimated annual savings of more than $11,500 per patient
Another congestive heart failure home monitoring program using
patient education, daily self-monitoring, and physician
notification for abnormal weight gain, vital signs, and symptoms
reported:
- 85.5% daily compliance rate per patient
- 66% reduction in ER visits
- 73% reduction in Intensive Care Unit admissions
Conclusion
Disease management programs leveraging an Internet-based population management platform empower healthcare providers to collect, analyze and report information on the day-to-day conditions of patients in their home. This technology also enables healthcare providers to quickly focus on patients in need of intervention and assure compliance with health regimens, which ultimately results in better outcomes at lower costs to the healthcare system. Additionally, patients have a better understanding of their condition and how to manage it.In such scenarios, care management programs allow for the collection and analysis of medical data, such as pre-visit screenings, laboratory results, prior to the patient's visit, thereby enabling the care provider to spend more time interacting with and educating the patient. Further, the physician can have a printed report of the patient's health status and history so that the time with the patient can be spent teaching and intervening rather than data collecting.
Utilizing technology-driven disease management and care management systems facilitates a care manager's ability to provide proactive healthcare at a low cost and responds to healthcare's major challenges. Web-enabled technologies, as presented in the case study, enhance effective communication between all healthcare constituents, promoting an interactive exchange of information. Increased patient/provider connectivity enables care managers to monitor patients more efficiently, thereby increasing productivity and reducing crises for patients. These benefits can be translated to dollar savings for the healthcare industry and better outcomes for patients.
About the Author(s)
Jeremy Nobel, MD, MPH, is a course director in the Harvard School of Public Health. He also designs healthcare management and delivery systems. His particular interest is in the development of computer based information technology applications that coordinate critical aspects of healthcare delivery.
Veronique Boissonnas is a healthcare communications consultant at Noonan/Russo Communications. She specializes in managed care and e-health communications.
Acknowledgment
Copyright © 2000 by the Healthcare Information and Management Systems Society.References
The Diabetes Control and Complications Trial Research Group. 1993. "The effect of Intensive Treatment of Diabetes on the Development and Progression of Long-Term Complications in Insulin-Dependent Diabetes Mellitus." N England J Med 329: 977-86.
National Institutes of Health. 1991. National Heart, Lung and Blood Institute. Executive Summary: Guidelines for the Diagnosis and Management of Asthma. Publication 91-3042A.
National Institutes of Health. 1993. National High Blood Pressure Education Program. Working group report on primary prevention of hypertension. Publication 93-2669.
Reissiger, A., D. Schlumper, W. Wyckoff. Olsten Health Services. 1998. "A Pediatric Asthma Self-Management Program That Gets Results." Drug Benefits Trends 10(1): 24-26
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed

