World Health & Population
Reducing Maternal Mortality in Senegal: Using GIS to Identify Priority Regions for the Expansion of Human Resources for Health
Abstract
In 2005, Senegal had an estimated maternal mortality ratio of 980 deaths per 100,000 live births, well above the global average of 400. The concentration of health workers has been shown to be associated with improved health outcomes, including maternal mortality. To explore this relationship, this paper uses geographic information systems (GIS) to examine the regional distribution of human resources for health and related maternal health indicators in Senegal. Results show that a regional imbalance in the distribution of health personnel and health indicators exists in Senegal. This disparity may contribute to the disproportionate burden of disease experienced in the eastern part of the country. Based on a spatial analysis, a priority index is used to identify regions to target for the recruitment and training of midwives. GIS is an appropriate and practical tool for governments and other agencies to use in identifying regional disparities and for priority setting.
Introduction
Reducing maternal mortality is recognized globally as a major health priority and is listed as a United Nations Millennium Development Goal (Sachs and McArthur 2005). Emphasis has been placed on addressing maternal mortality in developing countries, where 99% of pregnancy and childbirth complications occur annually (WHO et al. 2010). However, even in developing countries, maternal deaths are not distributed evenly, with the worst maternal health indicators occurring in sub-Saharan Africa.
Contributing to these poor health indicators is the scarcity as well as maldistribution of human resources for health, most notably in regions with the greatest global burden of disease, such as sub-Saharan Africa. According to the World Health Report 2006, despite bearing nearly 25% of the global disease burden, sub-Saharan Africa has only 3% of the global health workforce. This can be compared to the Americas (namely the United States and Canada), which bears 10% of the global disease burden but has nearly 40% of the global health workforce (WHO 2006).
Examining current resources across countries and regions may be an effective first step in addressing the general dearth and disparity of human resources for health. This paper uses national health data from Senegal, a country of 12 million inhabitants located in West Africa, to spatially examine the regional distribution of human resources for health as well as health indicators related to maternal mortality. Geographic information systems (GIS) software was used to present the data and to identify priority regions in Senegal that require targeted programs to mitigate regional disparities in maternal health. Findings from this research will contribute to the GIS health-related literature in showing that GIS can be used to examine spatial disparity and to prioritize areas of need.
Maternal Health in Senegal
Each year approximately 250,000 women die of pregnancy-related causes in sub-Saharan Africa (WHO 2006), representing nearly 50% of global maternal deaths. In Senegal, the World Health Organization (WHO) estimated a maternal mortality ratio of 450 deaths per 100,000 live births in 2008. To place this number in context, the United States had a maternal mortality ratio of 24 deaths per 100,000 live births in 2008 (WHO et al. 2010).
Maternal deaths are clustered around labour, delivery and the immediate postpartum period (Ronsmans and Graham 2006). Moreover, maternal deaths are highly associated with three delays that affect the utilization of life-saving obstetric services: (1) a delay in the decision-making process to seek care in the event of an emergency, (2) a delay in reaching obstetric services, and (3) a delay in receiving the emergency care upon reaching obstetric services (Killewo et al. 2006; Ronsmans and Graham 2006). Expanding the coverage of health workers who are present at birth, particularly that of midwifery care, can have an impact on each of these delays, thus minimizing the risk of severe complications that could lead to death (Killewo et al. 2006; Hongoro and McPake 2004).
There is strong evidence that the number of health workers in a region is associated with improved health outcomes, including maternal mortality (Hongoro and McPake 2004). Moreover, increasing the coverage of professional midwifery care at birth has a great impact on reducing the number of maternal deaths, both in developed and developing countries (Hongoro and McPake 2004; Van Lerberghe and De Brouwere 2001). Major initiatives that expanded professional training and care in Sri Lanka, Malaysia and Thailand have markedly lowered the maternal mortality ratio to under 50 deaths per 100,000 live births (Van Lerberghe and De Brouwere 2001). It is important to note that the expansion-of-care campaigns in these countries were multi-pronged approaches that targeted an increase in access to hospital care as well as a reduction in infectious diseases. That is, no single strategy is likely to achieve similar success in reducing maternal deaths. This evidence does, however, show the importance of professional care at birth in reducing maternal deaths.
Geographic Information System (GIS) and Health
The association between geography and health outcomes has been well researched and articulated (Cummins et al. 2007; Curtis and Jones 1998; Kearns 1993; Macintyre 2002). The theory behind the associations between geography and health stems from shared patterning and diffusion of physical and biological risk factors as well as shared social and economic conditions (Curtis and Jones 1998). That is not to say that processes and variation occurring at the individual level do not influence health outcomes; rather, it is acknowledging that people and geography have a reciprocal relationship (Cummins et al. 2007). Within regions and communities there may be variation in health status and outcomes that are not attributable to place; however, examining the relationship between health variation and geography provides important contextual information.
More specifically in the developing world context, geography plays a significant role in healthcare access (McLafferty 2003). Environmental barriers, such as access to trained health providers or proximity to a healthcare facility, greatly influence maternal health outcomes in the developing world, especially among women (Ojanuga and Gilbert 1992). Recent studies have used GIS tools to examine the relationship between place and health (Bullen et al. 1996; Foody 2006; McLafferty 2003; Plescia et al. 2001) and have generally concluded that place and location are important and significant determinants when examining health outcomes.
A recent review of the GIS health-related literature identified four main categories of GIS application in public health: disease surveillance, risk analysis, health access and planning, and community health profiling (Nykiforuk and Flaman 2011). The most common and traditional use of GIS in public health is in disease surveillance. Used in this way, data on disease incidence and prevalence are tracked spatially and subsequently mapped (Nykiforuk and Flaman 2011; Gao et al. 2008). This paper applies GIS as a tool for community health profiling. Community health profiling spatially examines health behaviours and health access, allowing for the analysis of relationships between health and setting. Moreover, identifying geographic disparities may lead to targeted strategies to meet the health needs of communities (Nykiforuk and Flaman 2011).
Community health profiling using GIS can be an invaluable asset for policy makers, public health officials and community development projects to show resources and need based on geographic areas (Maclachlan et al. 2007). Examining maternal health indicators and the current distribution of human resources for health in Senegal through a community health profile lens may provide important information for policy development and targeted intervention. Specifically, results from this investigation can help inform both governmental and non-governmental agencies on the allocation of resources to best mitigate regional disparities (Maclachlan et al. 2007). In an effort to prioritize midwife service expansion, GIS is used to describe and examine the relationship between the spatial distribution of human resources for health and regional variations in maternal health outcomes in Senegal.
Methods
Despite a rather standard definition, measuring maternal mortality can be challenging and the accuracy of data can vary greatly from region to region (Ronsmans and Graham 2006). Due to the complexity of measurements, indicators of maternal mortality are often available only in the aggregate; that is, only countrywide maternal mortality ratios are reported. To investigate variations in maternal health within countries, examining multiple regional health indicators can provide more specific information (Ronsmans and Graham 2006). Regional health measures that may be used as maternal health proxies include the percent of childbirths occurring unassisted by health professionals, the number of antenatal care visits during a pregnancy and the location of childbirth (Ronsmans and Graham 2006).
Data from the National Agency for Demography and Statistics (2008) were used to examine the regional distribution of human resources for health in Senegal. All maternal health indicators, as well as city locations, were gathered from the 2005 Demographic and Health Survey (Ndiaye and Ayad 2005). Maps for Africa and Senegal were obtained from the Environmental Systems Research Institute (ESRI). Locations for health services, including hospitals, health centres and health posts, were obtained from the WHO.
Two indices are used to analyze maternal health and healthcare access across Senegal: (1) index for shortage of midwives, and (2) priority areas index for midwife service expansion. The first index is calculated by taking the current number of midwives by region in Senegal and dividing it by the WHO-recommended number of midwives per population (1 midwife per 300 women of reproductive age), creating a "percent met" indicator (WHO 2010). Percent shortage is then calculated by subtracting the percent met from 1 and multiplying by 100.
The second index highlights priority regions for midwife service expansion based on a hot spot analysis of four indicators: (1) percent shortage of midwives, calculated at the regional level as described above, (2) percent of childbirths per region occurring unassisted by health professionals, (3) percent of women per region who receive no antenatal care during their pregnancy, and (4) percent of childbirths per region that take place at a health facility. A hot spot analysis can display aggregate data based on parameter settings, in this case priority levels by region. To conduct the hot spot analysis, each indicator is first made into an ordinal variable using the Jenks natural breaks classification method (Jenks 1977). Next, the variable is assigned a numerical value based on the regional indicator prevalence; higher values are given to prevalence rates associated with poorer health outcomes. The four indicators are then summed and mapped by region, creating a hot spot analysis that identifies regions with the poorest cumulative maternal health indicators. Based on this analysis, regions are then prioritized for midwife service expansion.
Results
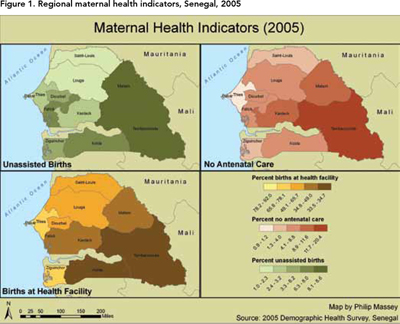
To better identify spatial patterns of health disparity, maternal health indicators are mapped at the regional level in Senegal. Figure 1 shows the regional prevalence rates of the three health indicators: percent of childbirths occurring unassisted by health professionals, percent of women that receive no antenatal care during their pregnancy, and percent of childbirths that take place at a health facility. Dakar has the lowest percent of unassisted childbirths at 1%, whereas Tambacounda and Matam both have greater than 8% of childbirths occurring without assistance by a trained professional. Furthermore, Dakar exhibits the lowest percent of women who attended no antenatal care visits during their pregnancy, at less than 1%. The two eastern regions of Tambacounda and Matam both exhibit the greatest percent of women who attended no antenatal care visits, at 20.4% and 11.6% respectively. The percent of births at health facilities is also uneven, with Dakar exhibiting the greatest percent and Tambacounda and Kolda the lowest. In general, the eastern regions of Matam, Tambacounda and Kolda present the poorest health indicators.
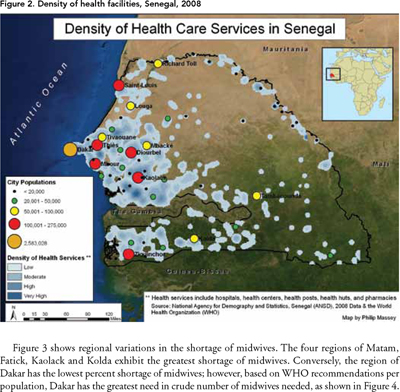
Environmental barriers, such as proximity to health facilities, may contribute to the regional disparity in maternal health indicators. Figure 2 displays the density of health facilities in Senegal; health facilities include hospitals, health centres, health posts, health huts and pharmacies. Note also that the densely populated western regions of Senegal also exhibit the highest density of health facilities. The eastern part of the country, which includes the regions of Matam and Tambacounda, has the lowest density of health facilities. Not surprisingly, these same regions have the lowest percent of births at a health facility, displayed in Figure 1.
Figure 3 shows regional variations in the shortage of midwives. The four regions of Matam, Fatick, Kaolack and Kolda exhibit the greatest shortage of midwives. Conversely, the region of Dakar has the lowest percent shortage of midwives; however, based on WHO recommendations per population, Dakar has the greatest need in crude number of midwives needed, as shown in Figure 4.
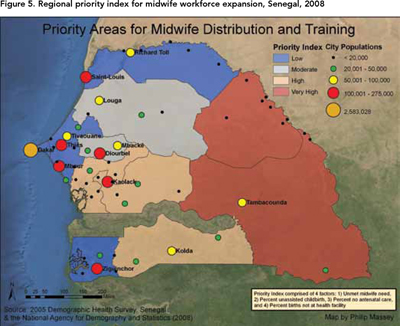
To prioritize regional maternal health needs, an index was created using the three maternal health indicators as well as the percent shortage for midwives. Figure 5 shows the regional priority index for midwife expansion. Based on the midwife priority index, the regions of Matam and Tambacounda have the highest need and should be targeted for midwife recruitment and training.
Discussion
Expanding Health Worker Coverage: A Determinants Framework
Based on the imbalance of health professionals in Senegal, strategies that extend workforce coverage to reduce maternal health disparities and ultimately lower the maternal mortality ratio should be pursued. Expanding coverage will require focusing on recruitment, training, deployment and retention (Dussault and Franceschini 2006; Koblinsky et al. 2006). To be most effective, strategies should target areas of need and incorporate determinants for health practice in underserved areas (Wilson et al. 2009). Recruitment and training of health personnel should be tailored and targeted to maximize its potential for success, applying the findings of this investigation.
Recent studies have identified a set of factors associated with the distribution of the health workforce in the developing world (Dussault and Franceschini 2006; Lehmann et al. 2008; Wilson et al. 2009). These factors are individual factors, the organizational environment, the healthcare and educational system, the institutional environment and the socio-cultural environment (Dussault and Franceschini 2006; Wilson et al. 2009).
Individual factors, including birthplace and career aspirations, are strong predictors for practice in underserved and rural areas (Dussault and Franceschini 2006; Wilson et al. 2009); therefore, recruitment of health professionals from underserved settings may serve to mitigate the maldistribution of the workforce. Once health professionals have been recruited, factors in the organizational environment, including management style, salary scales and career ladders, can serve as strategies to retain health workers (Dussault and Franceschini 2006; Fitzgerald and Carlson 2002; Golith 2000).
The healthcare and educational system focuses on the location of training facilities. Health workforce coverage can be expanded to underserved areas by developing more medical training facilities or satellite campuses in or around those settings (Wilson et al. 2009). The national government can also play an important role in shaping the institutional environment; decentralization of training and service delivery can improve local resources and increase regional authority in decisions related to health worker recruitment and retention (Koblinsky et al. 2006).
Lastly, socio-cultural factors are important determinants in the distribution of health professionals. Negative socio-cultural factors, including extreme conservative practices and fundamentalism, can limit the dispersal of health personnel, particularly that of midwives and other female health workers (Wilson et al. 2009). On the other hand, access to social, cultural, educational and professional opportunities can greatly increase the likelihood of a professional staying in a particular location (Dussault and Franceschini 2006).
These five categories provide a robust set of factors associated with the distribution of the health workforce in developing countries. However, despite its comprehensiveness, the list is not exhaustive but rather provides a framework from which to identify salient factors to be incorporated into program and policy development.
Recommendations for Moving Forward
To mitigate the inequitable burden of disease and maldistribution of human resources for health in Senegal as well as in other environments with similar needs and resources, this paper presents a set of five factors developed through prior research that are associated with health worker recruitment, training, deployment and retention (Dussault and Franceschini 2006; Lehmann et al. 2008; Wilson et al. 2009). Based on these factors as well as the data presented, "contextually competent" initiatives should focus on developing regional capacity to manage daily maternal health needs as well as emergencies.
A recent program implemented in Senegal entitled "Plan Cobra" is an example of an initiative targeting organizational and institutional change that gives health workers more control over tailoring their worker contracts (Zurn et al. 2010). This program allows health workers to negotiate for a specific post for a specific length of time. Along with increased negotiating power, the workers are entitled to special benefits provided by the government (Zurn et al. 2010). The program's success (witnessed through the re-opening of 122 health posts) indicates that flexible contracting systems can have a role in reducing disparities in health worker distribution. Additional strategies that decentralize semi-professional medical training may also serve as a positive influence in reducing regional disparities.
Another organizational strategy that may expand health workforce coverage is the advent of career ladders (Fitzgerald and Carlson 2002; Golith 2000). This strategy could target trained birth attendants and midwives, promoting career advancement that includes increasing salaries, benefits and training based on service location. This strategy will not only improve the distribution of health personnel, but may also serve to improve the quality of services. This is evidenced through a study in Senegal that found that more training completed by a health worker is associated with a higher quality of service delivery (Bitran 1995).
Finally, strategies aimed at developing the Senegalese health workforce may leverage the increasing role of new technologies. A recent World Bank report on global indicators asserted that among African nations, Senegal was second only to Morocco in the amount of money spent on information and communication technologies proportionate to its GDP (World Bank 2010). The increasing access and utilization of digital and mobile technologies throughout Senegal can be used for training, capacity building and professional development of human resources for health through distance learning programs. As Internet centres continue to expand throughout Senegal, there is a need to expand distance learning and training programs for semi-professional health workers to mitigate the imbalance of health professionals. Furthermore, increased access to technologies may help address socio-cultural factors, particularly if technologies can be used to connect isolated health workers to allow better information sharing and support (Thioune 2003).
Conclusion
The application of GIS in examining geographic health disparities and in identifying priority regions for targeted intervention provides a novel approach for community health profiling. These data provide another layer of information that is critical in identifying disparities and is often more easily understood by policy makers as well as for community members. With this information, both governmental and non-governmental agencies can implement strategies in areas with the greatest need for maternal health personnel.
However, although these data show spatial disparities in the number and concentration of midwives in Senegal, they do not provide information on the quality of services or accessibility of services by particular sub-groups. This limitation is acknowledged; the data only provide a crude picture of the distribution and infrastructure of healthcare professionals in Senegal.
More broadly, understanding the relationship between geography and health is important in developing and delivering contextually competent policy interventions. The significance of geography should not supersede the impact of individual factors on health outcomes. Rather, work should be conducted in concert to provide a holistic understanding of individual and population health.
Individual characteristics are no longer thought to be the sole contributor to health outcomes; rather, individuals operate within a broad social system with structural constraints and resources that affect personal development and functioning. In other words, only examining individual characteristics as the sole determinant of health is incomplete and inadequate, as it does not address larger structural conditions in which individuals function. As evidenced through this investigation on the distribution of health personnel and maternal health indicators, there is a significant structural component to need in Senegal. Specifically, poorer health outcomes are concentrated outside the capital region of Dakar. Targeted and tailored policies are necessary to address health worker imbalances as well as the disproportionate health burden experienced throughout Senegal. As research in this field continues to develop methods for prioritizing need, GIS should be considered an appropriate and useful tool for examining health within a geographic context.
About the Author(s)
Correspondence may be directed to: Philip Massey, Department of Community Health Sciences, P.O. Box 951772, Los Angeles, CA 90095-1772; e-mail: pmassey@ucla.edu.
Acknowledgment
I gratefully acknowledge the guidance of Dr. Leobardo Estrada in the Department of Urban Planning at UCLA, whose expertise in Geographic Information Systems provided invaluable support. I also thank Dr. Deborah Glik and Dr. Michael Prelip for their leadership and support in working in West Africa.
References
Bitran, R. 1995. "Efficiency and Quality in the Public and Private Sectors in Senegal." Health Policy and Planning 10(3): 271–83.
Bullen, N., G. Moon and K. Jones. 1996. "Defining Localities for Health Planning: A GIS Approach." Social Science & Medicine 42(6): 801–16.
Cummins, S., S. Curtis, A.V. Diez-Roux and S. Macintyre. 2007. "Understanding and Representing 'Place' in Health Research: A Relational Approach." Social Science & Medicine 65(9): 1825–38.
Curtis, S. and I.R. Jones. 1998. "Is There a Place for Geography in the Analysis of Health Inequality?" Sociology of Health & Illness 20(5): 645–72.
Dussault, G. and M.C. Franceschini. 2006. "Not Enough There, Too Many Here: Understanding Geographical Imbalances in the Distribution of the Health Workforce." Human Resources for Health 4(12): 1–16.
Fitzgerald, J. and V. Carlson. 2002. "Ladders to a Better Life." The American Prospect. Retrieved month day, year. <http://prospect.org/cs/articles?article=ladders_to_a_better_lifeon>.
Foody, G.M. 2006. "GIS: Health Applications." Progress in Physical Geography 30(5): 691–5.
Gao, S., D. Mioc, F. Anton, X. Yi and D.J. Coleman. 2008. "Online GIS Services for Mapping and Sharing Disease Information." International Journal of Health Geographics 7: 8.
Golith, R. 2000. "Learning from the Field: Economic Growth and Workforce Development in the 1990s." Economic Development Quarterly 14(4): 340–59.
Hongoro, C. and B. McPake. 2004. "How to Bridge the Gap in Human Resources for Health." The Lancet 364(9443): 1451–6.
Jenks, G.F. 1977. "Optimal Data Classification for Choropleth Maps." Occasional Paper No. 2, Kansas: Department of Geography, University of Kansas.
Kearns, R.A. 1993. "Place and Health: Towards a Reformed Medical Geography." Professional Geographer 45(2): 139–47.
Killewo J., I. Anwar, I. Bashir, M. Yunus and J. Chakraborty. 2006. "Perceived Delay in Healthcare-Seeking for Episodes of Serious Illness and Its Implications for Safe Motherhood Interventions in Rural Bangladesh." Journal of Health Population and Nutrition 24(4): 403–12.
Koblinksy, M., Z. Matthews, J. Hussein, D. Mavalankar, M.K. Mridha, I. Anwar et al. 2006. "Going to Scale with Professional Skilled Care." The Lancet 368(9544): 1377–86.
Lehmann, U., M. Dieleman and T. Martineau. 2008. "Staffing Remote Rural Areas in Middle- and Low-Income Countries: A Literature Review of Attraction and Retention." BMC Health Services Research 8(19): 1–10.
Macintyre, S. 2002. "Place Effects on Health: How Can We Conceptualise, Operationalise and Measure Them?" Social Science & Medicine 55(1): 125–39.
Maclachlan, J.C., M. Jerrett, T. Abernathy, M. Sears and M.J. Bunch. 2007. "Mapping Health on the Internet: A New Tool for Environmental Justice and Public Health Research." Health & Place 13(1): 72–86.
McLafferty, S.L. 2003. "GIS and Health Care." Annual Review of Public Health 24(1): 25–42.
National Agency for Statistics and Demography (NASD) in Senegal. 2008. The Social and Economic Situation in Senegal. Retrieved November 15, 2010. <http://www.ansd.sn/publications/annuelles/SES_2008.pdf>.
Ndiaye, S. and M. Ayad. 2005. Senegal Demographic and Health Survey 2005. Dakar, Senegal and Calverton, Maryland, USA: Center for Research and Human Development [Senegal] and ORC Macro.
Nykiforuk, C.I.J. and L.M. Flaman. 2011. "Geographic Information Systems (GIS) for Health Promotion and Public Health: A Review." Health Promotion Practice 12(1): 63–73.
Ojanuga, D.N. and C. Gilbert. 1992. "Women's Access to Health Care in Developing Countries." Social Science & Medicine 35(4): 613–7.
Plescia, M., S. Koontz and S. Laurent. 2001. "Community Assessment in a Vertically Integrated Health Care System." American Journal of Public Health 91(5): 811–4.
Ronsmans, C. and W.J. Graham. 2006. "Maternal Mortality: Who, When, Where, and Why." The Lancet 368(9544): 1189–1200.
Sachs, J.D. and J.W. McArthur. 2005. "The Millennium Project: A Plan for Meeting the Millennium Development." The Lancet 365(9456): 347–53.
Thioune, R.M. 2003. Information and Communication Technologies for Development in Africa: Opportunities and Challenges for Community Development, Vol. 1. Ottawa: International Development Research Centre.
Van Lerberghe, W. and V. De Brouwere. 2001. "Of Blind Alleys and Things That Have Worked: History's Lessons on Reducing Maternal Mortality." Studies in Health Service Organization Policy 17: 7–33.
Wilson, N.W., I.D. Couper, E. De Vries, S. Reid, T. Fish and B.J. Marais. 2009. "A Critical Review of Interventions to Redress the Inequitable Distribution of Healthcare Professionals to Rural and Remote Areas." Rural and Remote Health 9(2): 1060.
World Health Organization (WHO). 2006. The World Health Report 2006; Working together for Health. Geneva: World Health Organization.
World Health Organization (WHO). 2010. Increasing Access to Health Workers in Remote and Rural Areas through Improved Retention: Global Policy Recommendations. Geneva: World Health Organization; 2010.
World Health Organization, United Nations Children's Fund, United Nations Population Fund, The World Bank. 2010. Trends in Maternal Mortality: 1990–2008. Estimates Developed by WHO, UNICEF, UNFPA and the World Bank. Geneva: World Health Organization.
World Bank. 2010. Africa Development Indicators. Washington, DC: Oxford University Press for the World Bank.
Zurn, P., L. Codjia, F.L. Sall and J.M. Braichet. 2010. "How to Recruit and Retain Health Workers in Underserved Areas: The Senegalese Experience." Bulletin of the World Health Organization 88(5): 386–9.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed