Healthcare Quarterly
Cardiac Care Quality Indicators: A New Hospital-Level Quality Improvement Initiative for Cardiac Care in Canada
Abstract
Health system stakeholders at different levels are focused more than ever on improvements to quality of care. With heart disease continuing to be a top health issue for Canadians, quality improvement initiatives aimed at improving cardiac care are increasingly important. The Cardiac Care Quality Indicators are one such initiative, with the goal of supporting cardiac care centres in their quality improvement efforts by providing comparable facility-level information on a number of cardiac quality outcome indicators. Working together, the Canadian Institute for Health Information and the Cardiac Care Network of Ontario completed the pilot project for this initiative in Ontario and British Columbia in 2010. Based on the success of the pilot, a national expansion of the initiative is currently under way. This article details some of the processes that led to the success of the project and presents some high-level, de-identified results.
Although outcomes for patients living with heart disease are improving, heart disease continues to be a major health concern for Canadians. It has both high human and economic costs. A conservative estimate is that about 1.6 million Canadians are living with the disease, and in the latest figures available from 2000 it was estimated that costs in healthcare and lost productivity amounted to over $22 billion per annum (Public Health Agency of Canada 2009).
Considerable progress has been made in developing effective treatments and therapies, and well-defined indicators or performance measures can provide further direction to hospitals to support quality improvement efforts that can lead to better care for patients (Brown et al. 2005; Canadian Health Services Research Foundation 2008; Morris and Zelmer 2005). However, well-defined indicators are dependent on high-quality data.
The Canadian Institute for Health Information (CIHI) has been working with Canadian cardiovascular experts to enhance data quality to ensure that comparable and relevant information is available. For example, differentiating types of heart attacks is important for decisions related to treatment, which influences patient outcomes. Through CIHI's efforts to improve Canadian Coding Standards, it is now possible to distinguish ST-segment elevation myocardial infarction (STEMI) and non-ST-segment elevation myocardial infarction (NSTEMI) in clinical administrative data. STEMI cases require immediate intervention including revascularization or drug therapy to minimize damage to the myocardium and optimize patient outcomes. In 2008–2009, approximately one third of heart attacks in Canada were classified as STEMI, with 68% of these cases receiving a revascularization procedure within 30 days, whereas 39% of NSTEMI patients received this procedure. STEMI patients were also more likely than NSTEMI patients to be treated with percutaneous coronary intervention (PCI) versus coronary artery bypass graft (CABG) (CIHI 2010). Further study using this information will be helpful to monitor differences in treatment delivery and outcomes for these two groups.
Over the past 10 years, cardiac indicators have been routinely reported on to monitor (1) risk differences of heart disease and (2) cardiac intervention use in Canada (CIHI 2011). It was clear that also being able to monitor the outcomes associated with different cardiac interventions and variations in practice would add to the existing cardiac indicators and provide information to support improvements in the quality of care delivered to cardiac patients. Recognizing the need for more specific indicators focused on the quality of cardiac care in Canada, the Cardiac Care Network of Ontario (CCN) initiated a pilot project in 2008 with CIHI to identify and develop nationally comparable facility-level cardiac quality indicators. The goal was to develop indicators to support cardiac care centres in their quality improvement efforts by providing comparable facility-level information and to create a forum for knowledge sharing and care process discussions. The partnership between CCN and CIHI ensured that the indicators developed were relevant to stakeholders and meaningful to their quality improvement efforts. Indicators were developed for cardiac care facilities in Ontario and British Columbia. Results of the pilot project were shared with facilities in 2010, and the success of the pilot has led to a national expansion of the initiative.
Cardiac Care Quality Indicators
The Cardiac Care Quality Indicators were developed in close consultation with a national clinical expert panel of representatives from cardiology, cardiac surgery, hospital administration and the Canadian Cardiovascular Society. Fourteen indicators were developed examining quality outcomes including acute renal failure (ARF), stroke and mortality for patients undergoing the following cardiac interventions: diagnostic cardiac catheterization, PCI, isolated CABG, isolated valve surgery, and combined CABG and valve surgery (Table 1). The suite of indicators was selected as a starting point for reporting as the intervention groups represent a growing number of cardiac interventions and variations in practice. Additionally, literature and clinical input supported the outcomes as related to quality of care; data were available and consistently captured to identify quality outcomes; and, previously, only limited Canadian hospital-level information was available on these clinical outcomes and interventions.
| Table 1. Cardiac Care Quality Indicators | |
| Outcomes | Indicators |
| ARF | PCI cases with ARF within 14 days |
| CABG (isolated) cases with ARF within 14 days | |
| CABG + valve surgery cases with ARF within 14 days | |
| Valve surgery (isolated) cases with ARF within 14 days | |
| Stroke | Cardiac catheterization cases with stroke within same episode of care |
| PCI cases with stroke within 14 days | |
| CABG (isolated) cases with stroke within 14 days | |
| CABG + valve surgery cases with stroke within 14 days | |
| Valve surgery (isolated) cases with stroke within 14 days | |
| Mortality | 30 day in-hospital mortality for PCI cases |
| 30 day in-hospital mortality for CABG (isolated) cases | |
| 30 day in-hospital mortality for CABG + valve surgery cases | |
| 30 day in-hospital mortality for valve surgery (isolated) cases | |
| CABG and PCI | PCI cases with CABG within 2 days |
| ARF = acute renal failure; CABG = coronary artery bypass graft; PCI = percutaneous coronary intervention. | |
Using data from CIHI's Discharge Abstract Database and National Ambulatory Care Reporting System on acute in-patient and day-surgery separations, indicator rates were calculated at provincial and facility levels. Patients were followed up across episodes of care to link transfers and readmissions to enable the capture of outcomes occurring at different facilities for a more complete picture of patient care. This was important because stroke and ARF outcomes were identified at facilities other than the ones performing the cardiac intervention and, in fact, over 25% of PCI cases with ARF or stroke in 2009–2010 were identified in facilities that did not perform the PCI intervention. Crude rates were adjusted by age, sex and select clinical risk factors (e.g., pre-admission co-morbid diagnoses) using regression models to increase the comparability of results among hospitals.
Pilot Project Results and Interpretation
In 2009–2010, the volume of cardiac intervention episodes of care for British Columbia and Ontario were as follows:
- Diagnostic cardiac catheterization – 43,400
- PCI – 26,622
- CABG – 8,751
- CABG plus valve surgery – 2,004
- Valve surgery – 2,864
Over 65% of cases were male, and approximately half were 65 years or older. The gender split identified further supports the findings of other studies showing differences in the use of cardiac catheterization and revascularization among men and women with cardiovascular disease (Fang and Alderman 2006; Nguyen et al 2008). Statistically significant variations in indicator results were observed at different levels. Among the outcomes examined, ARF was the most common, followed by mortality and stroke. This trend was mostly consistent across the different intervention groups. The risk of an adverse outcome was also found to increase as the invasiveness of the intervention increased. The combined CABG and valve surgery group had the highest rates of stroke, mortality and ARF compared with the other intervention groups (Figure 1).
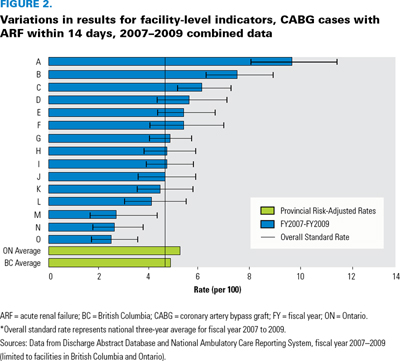
Figure 2 displays the variation in rates by hospital for isolated CABG cases with ARF within 14 days. The overall average was 4.7%, with rates ranging from 2.6 to 9.2%. The variations observed signal to hospitals that further investigation into pre-intervention assessment practices (e.g., renal function testing to identify high-risk individuals) and post-intervention care protocols (e.g., nephrology consultation and infection monitoring) may be needed to understand and identify areas for quality improvement.
Summary
Improving quality of care continues to be a priority in Canadian healthcare. The Cardiac Care Quality Indicators can serve as an important tool for healthcare decision-makers and clinicians in targeting efforts to improve patient outcomes and support a sustainable healthcare system. The success of this pilot project is attributed to several factors including working collaboratively with partners; convening an expert clinical panel early in project development; having a pilot phase to support the development and refinement of indicators; providing outreach and client support to hospitals; and engaging hospitals in the validation/review of results. Some of the challenges were targeting the information to the right stakeholders within facilities; representing complexities in the patient experience through complex indicator criteria; and data availability related to the capture of relevant risk factors.
Based on the success of the pilot, CIHI is expanding the initiative to include cardiac care centres across Canada, offering additional opportunities for comparison and knowledge sharing. Additionally, in the future, the facility-level indicator results will be available in the Canadian Hospital Reporting Project eTool (www.cihi.ca/hospitalreporting), an interactive web-based tool that provides users with additional contextual information for peer identification and drill-down capabilities to assist with quality improvement efforts.
About the Author(s)
Vanita Gorzkiewicz, MSc, is a project lead in the Hospital Reports Department at the Canadian Institute for Health Information (CIHI). She has extensive experience using health data to inform health system decision-makers and improve healthcare.
Jeanie Lacroix, MPA, is the manager of Hospital Reports at CIHI. She has over 10 years' experience leading and managing health research initiatives in the areas of health services research and performance measurement. Her recent work has focused on developing new national health indicators, producing comparative hospital performance reports and knowledge transfer to apply health indicators for quality improvement in the field.
Kori Kingsbury, MSN, MPA is the chief executive officer for the Cardiac Care Network of Ontario, in Toronto, with responsibility to serve as a healthcare system resource for cardiovascular services in the province of Ontario.
Acknowledgment
The authors gratefully acknowledge the contributions from Linda Choy, Jennifer D'Sliva, Sara Grimwood, Bernadee Koh-Bilodeau, Taryn Johnston, Edgar Manukyan, Indra Pulcins, Kristin Ramdeen, Sping Wang and the Cardiac Care Quality Indicators National Clinical Expert Panel in the development, preparation and analysis of the Cardiac Care Quality Indicators information.
References
Brown, A.D., H. Bhimani and H. MacLeod. 2005. "Making Performance Reports Work." Healthcare Papers 6: 8–22.
Canadian Health Services Research Foundation. 2008. "Performance Reporting to Help Organizations Promote Quality Improvement." Healthcare Policy 4: 70–74.
Canadian Institute for Health Information. 2010. Health Care in Canada 2010. Ottawa, ON: Author.
Canadian Institute for Health Information. 2011. Health Indicators 2011. Ottawa, ON: Author.
Fang, J. and M.H. Alderman. 2006. "Gender Differences of Revascularization in Patients with Acute Myocardial Infarction." American Journal of Cardiology 97: 1722–26.
Morris, K. and J. Zelmer. 2005. Public Reporting of Performance Measures in Health Care. Ottawa, ON: Canadian Policy Research Networks Inc. Accessed September 8, 2011. http://www.lachsr.org/documents/events/antigua06/Performance_Measures_Canada_2005-Morris.pdf>.
Nguyen, J.T., A.K. Berger, S. Duval and R.V. Luepker. 2008. "Gender Disparity in Cardiac Procedures and Medication Use for Acute Myocardial Infarction." American Heart Journal 155: 862–68.
Public Health Agency of Canada. 2009. 2009 Tracking Heart Disease and Stroke in Canada. Ottawa, ON: Author. Accessed September 7, 2011 <http://www.phac-aspc.gc.ca/publicat/2009/cvd-avc/pdf/cvd-avs-2009-eng.pdf>.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed