Healthcare Quarterly
All-Cause Readmission to Acute Care for Cancer Patients
Hong Ji, Hani Abushomar, Xi-Kuan Chen, Cheng Qian and Darren Gerson
Abstract
A recent Canadian Institute for Health Information report on all-cause readmission identified that cancer patients had higher-than-average readmission rates. This study provides further insight on the experience of cancer patients, exploring the risk factors associated with readmission at patient, hospital and community levels. An analysis showed that patient characteristics, including the reason for initial hospitalization, sex, co-morbidity levels, admission through the emergency department and the number of previous acute care admissions, were associated with readmission for cancer patients. In addition, we found that the readmission rate for these patients varied by hospital size and whether the patients lived in rural or urban locations.
Unplanned readmissions have been identified as costly (Anderson and Steinberg 1984; Jencks et al. 2009) and potentially avoidable (Frankl et al. 1991; Greenblatt et al. 2010). A recent Canadian Institute for Health Information (CIHI) report, All-Cause Readmission to Acute Care and Return to the Emergency Department, indicated that about 8.5% of acute care patients were readmitted to acute care hospitals within 30 days of their index discharge. Cancer condition was among the top five case mix groups with the highest readmission volumes (CIHI 2012). Cancer patients have a high rate of hospitalization and readmission (Greenblatt et al. 2010; Public Health Agency of Canada 2008). Various risk factors have been identified as potential predictors of readmissions for different cancer patients (Gonzalez et al. 2005; Reddy et al. 2009; Weaver et al. 2006).
This article examines the pan-Canadian readmission rate in cancer patients and explores the risk factors associated with readmission at patient, hospital and community levels. Identifying and understanding risk factors is an important first step toward informing strategies to reduce readmission rates.
Data Sources and Methods
In this study, the outcome was defined as unplanned all-cause readmission to acute care within 30 days of the index discharge. The study data were derived from CIHI's Discharge Abstract Database (DAD) 2010–2011 and the 2009–2010 MED-ÉCHO data from Quebec. To ensure that all patients could be followed for up to 30 days following discharge, the index hospitalizations were restricted to acute care discharges in the first 11 months of the fiscal year, while the readmission discharges included all discharges in the study period.
The unit of analysis was an episode of care. An episode of care refers to all adjoining in-patient hospitalizations and same-day surgery visits. Cancer patients were identified if there was any cancer diagnosis during the episode. Patients were categorized into surgical, medical, obstetric and pediatric groups, and hospitals were categorized into teaching, large, medium and small community hospitals. Readmissions with chemotherapy as the most responsible diagnosis were excluded because most readmissions for chemotherapy are planned. The cost of readmission was estimated based on CIHI's 2011 case mix groups methodology which aggregates acute care inpatients with similar clinical and resource utilization characteristics and 2009–2011 cost per weighted case. Details about these methodologies can be found in CIHI's readmission report (CIHI 2012).
Logistic regression models were used to evaluate the association of readmission with selected risk factors. Logistic regression modelling was also used to calculate the risk-adjusted readmission rate across jurisdictions, with control for patient group, age, sex, number of acute care hospitalization in the previous six months prior to index, admission via the emergency department (ED) in index, Charlson Index score and case mix group.
Findings
In 2010–2011, a total of 211,670 patients were hospitalized with a diagnosis of cancer during the 11-month study period. The majority of cancer patients were initially hospitalized for medical (48.0%) or surgical (48.3%) care. Nearly 4% (3.6%) were pediatric patients, and a small number were obstetric patients (0.07%).
Among cancer patients, 30,902 patients were readmitted to acute in-patient care within 30 days of their index discharges – an unplanned all-cause readmission rate of 14.6%. The readmission rate after medical visits was 19.6%, which was more than double the rate after surgical visits (9.3%). Cancer readmission represents 17% of all readmissions to acute care, whereas cancer hospitalization only represents 10% of all hospitalizations. Readmission rates for cancer patients remained stable in Canada (excluding Quebec) between 2008–2009 and 2010–2011.
The variation of risk-adjusted readmission rate among jurisdictions was modest. Among provinces, the risk-adjusted readmission rate in cancer patients was the highest in Saskatchewan (18%) and the lowest in Newfoundland and Labrador (14%) (Figure 1).
Patient Effects
Patient characteristics of patient group, sex, Charlson Index score, admission through the ED and the number of acute care admissions prior to index were identified to be associated with the risk of readmission in cancer patients. Male patients had a higher readmission rate than female patients (odds ratio [OR] 1.15, 95% confidence interval [CI] 1.12–1.17). Surgical patients were less likely than medical patients to be readmitted (OR 0.65, 95% CI 0.63–0.67), while no differences were found between obstetric, pediatric and medical patients. Patients with higher Charlson Index scores (OR for 2 versus 0: 1.25, 95% CI 1.21–1.29), with more acute care visits six months prior to the index (OR for 2+ versus 0: 1.69, 95% CI 1.63–1.75) and admitted through ED in the index (OR 1.51, 95% CI 1.46–1.55) were at higher risk of readmission.
Among medical patients, the top-five case mix groups with the highest readmission volumes accounted for 19% of all cancer readmissions. These conditions included cancers of the respiratory system, radiotherapy/chemotherapy and cancers of the digestive system, agranulocytosis and lymphoma. For medical cancer patients, the most common reason for readmission was the same condition treated in the index. For surgical cancer patients, the top-five conditions were colostomy/enterostomy, large intestine/rectum resection, lymphoma interventions, radical excision of prostate and open thoracic lung resection. The most common reasons for readmission were surgical complications or gastrointestinal obstruction.
Hospital Effects
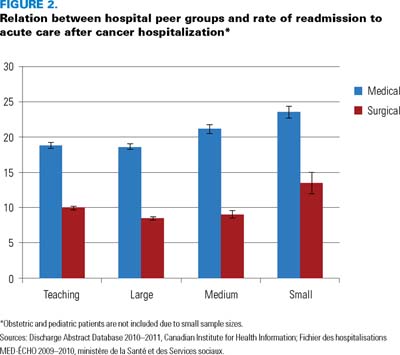
Readmission rates for medical patients were greater than for surgical patients in all four hospital peer groups. Cancer patients discharged from small community hospitals were more likely to be readmitted than patients from other hospital peer groups (Figure 2).
Community Effects
In this study, patient residence – rural/urban residency and neighbourhood income quintiles – was used as a proxy for community care service levels. Compared with those from the most affluent neighbourhood, cancer patients from the least affluent neighbourhood had a higher readmission rate (OR 1.11, 95% CI 1.06–1.15). Readmission rates were higher among patients living in rural areas than among those in urban areas (OR 1.14, 95% CI 1.11–1.18). The impact of patient residency has been reported in previous studies (Greenblatt et al. 2010; Lai et al. 2007).
Discussion
Our study demonstrated that cancer patients were more likely to be readmitted to acute in-patient care compared with the rest of the in-patient population. The most common reason for readmission for medical cancer patients was the same condition as the one treated during the index. In contrast, surgical cancer patients were most often readmitted for complications or gastrointestinal obstruction. Prior studies suggested that readmissions due to complications and gastrointestinal obstruction after cancer surgery were inversely associated with hospital procedure volume. Prior studies showed that hospitals that did more procedures had fewer readmissions. This could be partly due to the multidisciplinary approach in these hospitals (Gouma et al. 2000; Greenblatt et al. 2010).
The results highlighted in this report with regard to the effects of hospital size and patient residency on cancer readmission suggest that the transition between in-patient and post–acute care may be improved by additional pre-discharge and post-discharge interventions. Reducing readmission rates, however, is not a simple task; rather, it is a multi-faceted issue and, therefore, requires multiple actions from all levels of the healthcare system. This study has identified multiple factors at the patient, hospital and community levels that were associated with the risk of readmission for cancer patients. An improved understanding of these factors may contribute to increased collaboration among leaders of the different system components to improve readmission outcomes.
About the Author(s)
Hong Ji, MSc, is a senior analyst in health services research at the Canadian Institute for Health Information (CIHI). Ji is responsible for performing analyses and provides methodological support to projects, as well as participating in writing reports.
Hani Abushomar, MSc, is a senior analyst in health reports at CIHI. Abushomar is responsible for performing analyses and provides methodological support to projects, as well as participating in writing reports.
Xi-Kuan Chen, PhD, is a project lead in health services research at CIHI, in Toronto, Ontario. He leads the analysis and development of methodology for CIHI reports.
Cheng Qian, BSc, PMP, is a project lead in health services research at CIHI, in Toronto. She leads and coordinates the design and development of analytical plans for CIHI reports.
Darren Gerson, MBA, is the manager of health services research at CIHI, in Toronto. He oversees the development and production of health services research initiatives.
References
Anderson, G.F. and E.P. Steinberg. 1984. "Hospital Readmissions in the Medicare Population." New England Journal of Medicine 311: 1349–53.
Canadian Institute for Health Information. 2012. All Cause Readmission to Acute Care and Return to the Emergent Department. Ottawa, ON: Author.
Frankl, S.E., J.L. Breeling and L. Goldman. 1991. "Preventability of Emergent Hospital Readmission." American Journal of Medicine 90(6): 667–74.
Gonzalez, J.R., E. Fernandez, V. Moreno, J. Ribes, M.Peris, M.Navarro et al. 2005. "Sex Differences in Hospital Readmission among Colorectal Cancer Patients." Journal of Epidemiology and Community Health 59: 506–11.
Gouma, D.J., R.C.I. van Geenen, T.M. van Gulik, R.J. de Haan, L.T. de Wit, O.R.C. Busch et al. 2000. "Rates of Complications and Death after Pancreaticoduodenectomy: Risk Factors and the Impact of Hospital Volume." Annals of Surgery 232(6): 786–95.
Greenblatt, D.Y., S.M. Weber, E.S. O'Connor, N.K. LoConte, J. Liou and M.A. Smith. 2010. "Readmission after Colectomy for Cancer Predicts One-Year Mortality." Annals of Surgery 251(4): 659–69.
Jencks, S.F., M.V. Williams and E.A. Coleman. 2009. "Rehospitalizations among Patients in the Medicare Fee-for-Service Program." New England Journal of Medicine 360: 1418–28.
Lai, J.K., M.A. Martin, R. Meyricke, T. O'Neill and S. Roberts. 2007. "Factors Associated with Short-Term Hospital Readmission Rates for Breast Cancer Patients in Western Australia: An Observational Study." Journal of the American College of Surgeon 204(2): 193–200.
Public Health Agency of Canada. 2008. Leading Causes of Death and Hospitalization in Canada. Ottawa, ON: Author. Retrieved April 4, 2012. <http://www.phac-aspc.gc.ca/publicat/lcd-pcd97/index-eng.php>.
Reddy, D.M., C.M. Townsend Jr., Y.F. Kuo, J.L. Freeman, J.S. Goodwin and T.S. Riall. 2009. "Readmission after Pancreatectomy for Pancreatic Cancer in Medicare Patients." Journal of Gastrointestinal Surgery 13(11): 1963–74.
Weaver, C., L. Schiech, J. Held-Warmkessel, P. Kedziera, E. Haney, G. DiLullo et al. 2006. "Risk for Unplanned Hospital Readmission of Patients with Cancer: Results of a Retrospective Medical Record Review." Oncology Nursing Forum 33(3): E44–52.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed