Healthcare Quarterly
The Burden of Unhealthy Living in Ontario: The Impact of Smoking, Alcohol, Diet, Physical Inactivity and Stress on Life Expectancy
Douglas G. Manuel for the Healthy Living in Ontario Report Committee
The Issue
The 2009 report What Does It Take to Make a Healthy Province? (Manuel et al.) raised concern that Ontario was lagging behind Canada's healthiest provinces. Since the mid-1990s, British Columbia has been the healthiest province, with the highest life expectancy and, compared with Ontario, the smallest proportion of residents who smoke, have poor fruit and vegetable consumption or are physically inactive. Despite improvements in the rates of some unhealthy behaviour in the past decade, Ontario and all other provinces continue to lag behind British Columbia in healthy living.
The four "SAFE" health behaviours – the World Health Organization acronym for smoking, alcohol, food and exercise – are widely regarded as important factors for healthy living. But how much does healthy living contribute to the overall health of Canadians? Does healthy living in British Columbia explain why the life expectancy of its residents is the highest among all provinces? If residents of Ontario or other provinces improve their healthy living, will this achievement result in meaningful health gains?
The Study
Investigators from the Institute for Clinical Evaluative Sciences and Public Health Ontario recently co-published a report that examined five behavioural health risks, related mortality and health-related quality of life in Ontario (Manuel et al. 2012). The study base was all community-dwelling Ontarians aged 20 years and older. The report examined two questions: What is the health of Ontarians who have various kinds of healthy versus unhealthy living? And how much would Ontarians' health improve if they collectively reduced their behavioural risks?
The study had two main components. First, the Ontario sample of the 2001–2005 cycles of the Canadian Community Health Survey, individually linked to death records from 2001 to 2010, was used to create a model. This model was used to predict the risk of death based on exposure to five unhealthy behaviours – smoking, unhealthy alcohol consumption, poor diet, physical inactivity and high stress – and to assess the contribution of each behavioural risk and combinations of risks toward the risk of death.
Second, the risk model was applied to Statistics Canada's 2007 Canadian Community Health Survey. Using a period life table approach, the probability of death was used to estimate life expectancy and health-adjusted life expectancy for respondents, based on their behavioural risk exposure as well as selected socio-economic and personal factors (including age, sex, ethnicity, education and neighbourhood characteristics that reflect material and social infrastructure). A second calculation assessed the contribution of the behavioural risks to the risk of death by estimating the probability of death for each respondent if there had been no exposure to the behavioural risk. For example, the risk of death for current smokers was assessed and then re-assessed assuming they had never smoked. The difference between the two calculations estimated the contribution of smoking to the risk of death.
The impact on health-related quality of life was calculated by comparing the Health Utilities Index scores (Feeney et al. 1995) of people with a behavioural risk to the scores from the remaining Ontario population. The burden associated with a health risk was the difference in health-related quality of life between these two groups.
Key Findings
The risk of death from the five behavioural risk factors was calculated using responses from 78,597 Ontarians who were surveyed between 2001 and 2005 and followed up to 2010. In total, there were 568,997 person-years of follow-up and 6,399 deaths.
Life Expectancy and Health-Adjusted Life Expectancy for Ontarians with Different Levels of Risk Exposure
Figure 1 shows the life expectancy in 2007 for Ontarians with the unhealthiest risk exposure compared with those with healthy behaviour. People with exposure to all five health risks had a life expectancy that was more than 20 years lower than that of people with no health risks (68.5 versus 88.6 years for men, 71.5 versus 92.5 years for women).
Population Health Impact of Behavioural Risks
The population health impact of each behavioural risk is a combination of the number of people exposed to and the increase in mortality associated with that risk. These two components resulted in some unexpected findings. For example, the risk of death from heavy smoking (2.8 for men, 2.9 for women) was higher than the risk associated with physical inactivity (1.4 for men, 1.5 for women). However, in 2007 more Ontarians were inactive (49.3% of men and 56.6% of women) than were heavy smokers (8.4% of men and 3.8% of women). As a result, physical inactivity had an equally high impact on Ontarians' health overall. The combined impact of all behavioural risks accounted for 59.9% of deaths in 2007.
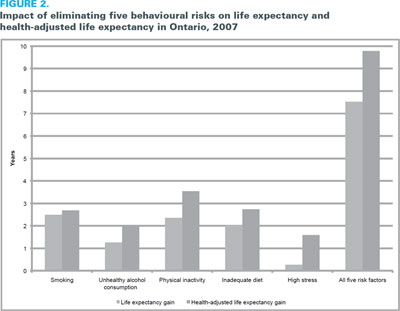
The population health impact of eliminating behavioural risks is shown in Figure 2. Smoking, physical inactivity and inadequate diet had the greatest impact on life expectancy (2.5, 2.4 and 2.0 years, respectively). Combined, the five risk factors represent a loss of 7.5 years of life expectancy and 9.8 years of health-adjusted life expectancy.
Not surprisingly, life expectancy differed by socio-economic position in the Ontario cohort. There was a 4.5-year gap between the least-deprived and most-deprived neighbourhoods. However, if behavioural risks were the same across neighbourhoods, the gap would be reduced by almost 50% (two years less). Of the five risks examined, smoking was the biggest contributor to the equity gap in both life expectancy and health-adjusted life expectancy.
Policy Scenarios
The predictive model allows for policy evaluation, and two policy scenarios were examined. In the first scenario, the health impact of Ontarians individually improving their highest risk behaviour was examined. Nearly all Ontarians reported at least one of the five unhealthy behaviours; only 1.4% had none. If each person optimized his or her single most important unhealthy behaviour (e.g., if all physically inactive people became active), life expectancy in Ontario would increase by 3.7 years.
In the second scenario, the potential impact of Ontario achieving British Columbia's targets for improved health behaviour (nine of 10 residents will not smoke, seven of 10 will eat at least five fruits and vegetables each day and seven of 10 will be physically active) was examined. Ontarians would gain 3.0 years of life expectancy by collectively reaching these goals. For Ontario to achieve all three of the targets, 77% of Ontarians would need to change at least one behaviour.
What Do These Finding Mean?
This study suggests that remarkable gains in life expectancy could be achieved in Ontario and other Canadian provinces through healthier living. The potential gains in health-adjusted life expectancy are even larger. Improving health behaviours would add "life to years" as well as "years to life" and could be expected to reduce demands on both the healthcare system and informal family caregiving.
While this study confirms findings from previous studies demonstrating large differences in life expectancy and health-adjusted life expectancy across different socio-economic groups (Wilkins et al. 2002), it also suggests that reducing behavioural health risks in low socio-economic groups could play a large role in reducing health inequities.
Examining individual and population burdens provides different perspectives on the impact of behavioural risks. This study enables the evaluation of policies aimed at improving health behaviour at the population level, including evaluating the impact on current socio-economic disparities. It also gives individuals the means to evaluate the impact of their health behaviour on their own life expectancy using a life expectancy calculator (see https://www.rrasp-phirn.ca/risktools) – potentially leading to behaviour change.
Next Steps
Future research should focus on the impact of health behaviours on the development of chronic diseases. Additionally, the hypothesis that demands on the healthcare system and informal caregiving are reduced with improved health behaviour warrants examination.
About the Author(s)
Douglas G. Manuel, MD, FRCPC, MSc, is a senior scientist at the Ottawa Hospital Research Institute and an adjunct scientist with the Institute for Clinical Evaluative Sciences. He has a Canadian Institutes of Health Research/Public Health Agency of Canada chair in applied public health sciences. He is an associate professor at the University of Ottawa and the University of Toronto. Dr. Manuel is a co-lead with the Population Health Improvement Research Network and an associate scientist at the C.T. Lamont Primary Health Care Research Centre, Élisabeth Bruyèr e Research Institute. He is also a senior medical advisor at Statistics Canada. He can be contacted by e-mail at dmanuel@ohri.ca.
References
Feeny, D., W. Furlong, M. Boyle and G.W. Torrance. 1995. "Multiattribute Health Status Classification Systems. Health Utilities Index." Pharmacoeconomics 7(6): 490–502.
Manuel, D.G., M.I. Creatore, L.C. Rosella and D.A. Henry. 2009. What Does It Take to Make a Healthy Province? A Benchmark Study of Jurisdictions in Canada and Around the World with the Highest Levels of Health and the Best Health Behaviours. Toronto, ON: Institute for Clinical Evaluative Sciences.
Manuel, D.G., R. Perez, C. Bennett, L. Rosella, M. Taljaard, M. Roberts et al. 2012. Seven More Years: The Impact of Smoking, Alcohol, Diet, Physical Activity and Stress on Health and Life Expectancy in Ontario. Toronto, ON: Institute for Clinical Evaluative Sciences, Public Health Ontario.
Wilkins, R., J.M. Berthelot and E. Ng. 2002. "Trends in Mortality by Neighbourhood Income in Urban Canada from 1971 to 1996." Health Reports 13(Suppl.): 45–72.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed