Healthcare Policy
Abstract
Purpose: To examine service use by adults with serious mental illness (SMI) rostered in new primary care models: enhanced fee-for-service (FFS), blended-capitation (CAP) and team-based capitation (TBC) models with and without mental health workers (MHW) in Ontario.
Methods: This cross-sectional study used administrative health service databases to compare use of mental health and general health services among persons with SMI enrolled in new models (n = 125,233).
Results: Relative to persons rostered in enhanced FFS, those in CAP and TBC had fewer mental health primary care visits (adjusted rate ratios and 95% confidence limits: CAP: 0.77 [0.74, 0.81]; TBC with MHW: 0.72 [0.68, 0.76]; TBC with no MHW: 0.81 [0.72, 0.93]). Compared to patients in enhanced FFS, those in TBC models also had more mental health hospital admissions (TBC with MHW: 1.12 [1.05, 1.20]; TBC with no MHW: 1.22 [1.05, 1.41]). Patterns of use of general services were similar.
Conclusion: Further attention to financial incentives in capitation that influence care of persons with SMI is necessary to determine if they are aligned with aims of primary care reform.
Persons with serious mental illness (SMI), such as psychosis, often experience symptoms that are disabling, are persistent and require continual monitoring and treatment (Gold et al. 2008; Institute of Psychiatry 2007: August). These patients are also more likely than others to have comorbid disorders, such as cardiovascular disease and diabetes (Gold et al. 2008; Narrow et al. 2000; Oud et al. 2010; Samele et al. 2007; Thornicroft 2011). However, despite higher levels of need, there is evidence that persons with psychotic disorders are roughly half as likely as others to have a primary care physician (PCP), and up to seven times more likely to report difficulties in accessing care (Bradford et al. 2008; Lawrence and Kisely 2010). Even so, PCPs remain their most commonly contacted healthcare providers, and are often the only providers contacted for mental healthcare (Lin et al. 1996; Regier et al. 1993; Vasiliadis et al. 2007). In the US and Canada, PCPs prescribe between 60% and 80% of psychotropic medications (Lavoie and Fleet 2002; Shearer et al. 2012).
Models of stepped care dictate that primary care services should be accessed before other types of mental healthcare, as primary care is cheaper and less intensive than more specialized care (National Institute for Health and Clinical Excellence 2012). Over the past decade, the Government of Ontario, Canada, has embarked on a major restructuring of primary care to increase access, improve quality and manage costs (Deber 2008; Glazier and Redelmeier 2010). This restructuring resulted in three major types of primary care models: enhanced fee-for-service (FFS), capitation-based (CAP) and team-based capitation (TBC), which all include enrolling patients, 24/7 access to care and enhanced information technology (Glazier et al. 2009; Glazier and Redelmeier 2010; Rosser et al. 2010).
The new models offer insured physician-provided services, as is required in Ontario where medically necessary services, delivered by physicians or in hospitals, are required to be covered for "insured persons" (residents) (Durbin et al. 2013). However, TBC models also offer insured non-physician-provided outpatient services, such as those delivered by nurse practitioners, dieticians, or mental health workers (MHWs). MHWs include persons with Bachelor of Arts, Bachelor of Social Work or Master of Social Work degrees who provide mental health counselling. The integration of non-physician providers into TBC models creates new opportunities for service coordination, especially because the same team of providers treats physical and mental health problems (Durbin et al. 2013). Coordinated care is particularly important for people with SMI who often have complex illness profiles, with high rates of substance use disorders as well as physical illness and receive inadequate physical healthcare (Durbin et al. 2013).
These three primary care models also differ in physician reimbursement and economic incentives for providers (Deber et al. 2008; Goldberg 1999; Schlesinger and Mechanic 1993). As FFS models reimburse physicians per service delivered (claims for each provided service are paid in full), there is incentive to provide more services and/or to preferentially provide more lucrative services (Deber et al. 2008; Kralj and Kantarevic 2013). Under capitation, the PCP receives a fixed payment per enrolled patient for delivery of required care. In theory, this encourages early intervention and collaboration with other providers (Durbin et al. 2013). However, unless compensation is adjusted for patient morbidity, high-needs patients represent a larger financial risk to PCPs. In Ontario, the only adjustments are for age and sex (Glazier et al. 2012). This could contribute to the exclusion of high-needs patients from new primary care models, as they use more physician time (Gosden et al. 2001; Hellinger, 1996; Petersen et al. 2006; Rothbard et al. 2004). In these capitation models, physicians also receive a portion of the FFS amount for each service provided. During the study period, 10% and later 15% of FFS claims were paid to these PCPs.
US studies that compared care delivered to persons with SMI in different primary care models have shown that capitation is associated with increased or decreased use of outpatient care (Busch et al. 2004; Chou et al. 2005; Leff et al. 2005; Morrissey et al. 2002) and fewer mental health hospital admissions (Bloom et al. 2002; Leff et al. 2005; Rothbard et al. 2004; Warner and Huxley 1998). Many of those studies, however, are dated, and many were based on unrepresentative samples.
Primary care reform in Ontario provides a unique opportunity to explore broad system change and utilization of health services by groups of interest in a single-payer healthcare system with universal health insurance. In this study, we examine the association between the type of primary care model and health service utilization among patients with SMI.
Due to the differences in remuneration across models, we tested two hypotheses. The first is that there would be more outpatient service use in enhanced FFS models in TBC models, compared to CAP models. The second was that there would be less in-patient service use in enhanced FFS and TBC models, compared to CAP models.
Methods
Study design
This cross-sectional study used administrative claims data to examine rostered patients with psychotic or bipolar disorders in different primary care models in Ontario. Data were accessed through a comprehensive research agreement with the Ontario Ministry of Health and Long-Term Care (MOHLTC). This study was conducted using datasets that were linked using unique, encoded identifiers and analyzed at the Institute for Clinical Evaluative Sciences (ICES). The study was approved by the Research Ethics Board of Sunnybrook Health Sciences Centre in Toronto, Ontario.
Study population
The pool from which the sample was drawn included patients with at least one diagnostic billing code for psychotic or bipolar disorders over the two-year period that preceded March 31, 2009 (see Appendix A for codes), who were enrolled to a PCP in a model type under study (enhanced FFS, CAP and TBC model). Additional inclusion criteria were being between 18 and 105 years on March 31, 2009, and having at least one outpatient healthcare contact between April 1, 2009 and March 31, 2011. To be included, PCPs had to be in a model type under study on March 31, 2011. We excluded physicians in other remuneration models (less than 5%).
Measures and data sources
Primary care models
Primary care model types were enhanced FFS, CAP and TBC models. The latter was divided into three groups: with MHW, without MHW and with MHW unknown. However, given the small size of the TBC models with MHW unknown group (0.7% of patients in the study sample), we did not report results for them.
Patient characteristics
We obtained patient age, sex and postal code from Ontario's Registered Persons Database. We also used this database to identify recent registrants as a proxy for recent immigrants. Recent registrants are non-newborn individuals who received new healthcare coverage in Ontario within the past 10 years. Recent registration has been shown to be a good proxy for recent immigration to Ontario (Ray et al. 2007). We used Statistics Canada's Postal Code Conversion File to link patients' postal codes to census data. Census subdivisions of patient residence in 2006 were used to assign a rurality score to patients according to the Ontario Medical Association's 2008 Rurality Index of Ontario (Kralj 2009). We assigned household income quintile by linking postal codes with 2006 census dissemination areas after taking into account average household size and community of residence.
We used the Johns Hopkins Adjusted Clinical Groups Case-Mix System to adjust for the presence of co-morbidities. This system uses administrative diagnostic codes to describe and predict a patient's use of healthcare resources (The Johns Hopkins ACG Case-Mix System 2008). The system allows the calculation of aggregated diagnosis groups (ADGs) ranging from 0 (no diagnosis) to 10 or more (at least 10 distinct diagnosis groups). We also calculated resource utilization bands (RUBs), which were used to categorize patients based on their expected use of healthcare resources. They range from 0 (lowest expected healthcare costs) to 5 (highest expected healthcare costs). We used the validated Ontario Diabetes Database to identify study patients who had incident or prevalent diabetes mellitus (Hux et al. 2002). Hypertension (Tu et al. 2007) and congestive heart failure (Schultz et al. 2013) were also identified using validated diagnostic code algorithms. Patient enrolment and the presence of MHWs in the models were determined using Client Agency Program Enrolment tables and data provided directly to the research team from the MOHLTC. PCP characteristics were assigned using data from the MOHLTC's Corporate Physician Database.
Outcomes
Outcomes assessed over a two-year observation period (April 1, 2009 to March 31, 2011) were mental health and general visits to PCPs, visits to psychiatrists, mental health emergency department (ED) visits, general ED visits, mental health hospital admissions, general hospital admissions and average lengths of stay for each hospitalization. Office visits to physicians were categorized by type of provider visited ("00" for general practitioner/family physician; "19" for psychiatrist) according to the Ontario Health Insurance Plan (OHIP) specialty code. Mental health visits were identified using ICD-9 diagnostic codes (see Appendix B). This method for identifying mental health visits to PCPs had a sensitivity of 81% and a specificity of 97%. This method appears to be highly specific for identifying visits for psychotic or bipolar diagnoses (99.4%), although less sensitive (55.3%) (Steele 2003). ED visits were determined using the National Ambulatory Care Reporting System. Mental health and general admissions and lengths of stay were determined from the Canadian Institute for Health Information's Discharge Abstract Database and the Ontario Mental Health Reporting System. Mental health ED visits and hospital admissions were defined as visits/admissions for which the main reason for presentation or admission was related to any mental health disorder (see Appendix B).
Data analysis
We investigated the characteristics of patients and physicians as of March 31, 2011 (the end of the study period), by model type. We also examined unadjusted mental health service use and general health service use across model types from April 1, 2009 to March 31, 2011. Next we examined these relationships in negative binomial regression models. Each model was adjusted for patient factors and physician factors. Patient factors were age group, sex, rurality, recent registrants, ADGs, RUBs, diabetes, hypertension, congestive heart failure and income quintile. Physician factors adjusted for in this analysis were gender, years since graduation, Canadian or foreign medical graduate and practice size (number of enrolled patients). First, we ran negative binomial models that did not account for clustering of patients within physician practices and physicians within practice groups. Subsequently, we re-ran the same models with generalized estimating equations to account for the clustering (Hardin and Hilbe 2003). Estimates changed very little, so we reported estimates for clustered models (see Appendix C for estimates for full models).
Results
Patient and physician descriptive characteristics
A total of 7,344,398 patients were in the primary care models under study in Ontario from April 1, 2007 to March 31, 2009. Among them, 125,233 enrolled patients (1.7%) had billings for psychotic or bipolar disorders. Percentages of patients with these billings were similar across primary care models (enhanced FFS: 1.7%; CAP: 1.6%; TBC: 1.8%). As of March 31, 2011, patients with psychotic-bipolar disorder in enhanced FFS models had higher ADG and RUB scores, and were more likely to be immigrants, have diabetes and hypertension and to live in urban areas with lower-income quintiles (see Table 1 at www.longwoods.com/content/23926).
Characteristics of the 6,652 physicians in Ontario in enhanced FFS, CAP or TBC models from April 1, 2007 to March 31, 2009, are presented in Table 1. The characteristics are presented at March 31, 2011. In comparison to PCPs in other models, those in enhanced FFS had lower numbers of enrolled patients per physician, were less likely to have received their medical education in Canada and were more likely to have been in practice for more years.
Bivariate analysis
Compared to patients in enhanced FFS models, those in CAP and TBC had fewer office visits to PCPs, for both mental health and general reasons, and to psychiatrists. The number of mental health ED visits was highest among patients in enhanced FFS models and lower in both CAP models. However, the number of general ED visits was lowest in enhanced FFS models and highest in both TBC models. For both mental health and general admission, the number of hospital admissions was greatest in TBC models with no MHWs – they were lower in enhanced FFS models and lowest in CAP models. Lengths of stay were longest in both kinds of TBC models, followed by enhanced FFS models and CAP models (see Table 2 at www.longwoods.com/content/23926).
Adjusted results
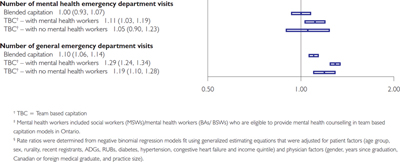
Compared to patients in enhanced FFS models, patients in CAP and TBC with and without MHW had fewer mental health and fewer general office visits to PCPs (Figure 1). Similarly, patients in both TBC models had fewer psychiatrist visits, but CAP patients had more visits to psychiatrists. Compared to patients in enhanced FFS, only individuals in TBC models with MHW had more emergency mental health visits (Figure 2). The numbers of general ED visits were higher in all capitation models, compared to enhanced FFS models.
Patients in both TBC models had more mental health and general hospital admissions than patients in enhanced FFS models (Figure 3). However, patients in CAP models only had significantly more general admissions than enhanced FFS patients; there were no significant differences in mental health admissions between CAP and enhanced FFS models. Average lengths of stay were longer for patients in TBC models with and without MHW compared to enhanced FFS models (Figure 3). There were no significant differences between patients in CAP and enhanced FFS.
For patients, male sex was associated with increases in all outcomes except for PCP visits (female sex was associated with more visits) and psychiatry visits (no relationship). Lower income was associated with an increase in all hospital outcomes. Urban residence was related to greater office visits and longer hospital admissions. Immigrant status was associated with increased PCP visits for general reasons but decreased mental health office visits to PCPs and psychiatrists. Immigrant status was also associated with decreased hospital outcomes. Similarly, increased comorbidities were associated with increased outcomes, while congestive heart failure, hypertension and diabetes were associated with increased general hospital admissions. Regarding physicians, males were associated with increases in all outcomes except for psychiatry visits and mental health ED visits; female physicians were associated with more psychiatry visits. Graduates from a Canadian medical school were associated with increased primary care office visits, while larger physician practices were associated with more general ED visits (see Appendix C).
Discussion
Relative to patients enrolled in enhanced FFS models, patients enrolled in CAP and TBC had fewer primary care visits for mental health and general reasons, more general ED visits and more general hospital admissions. Patients in TBC models also had fewer psychiatry visits, more mental health hospital admissions and longer lengths of stay for both types of admissions than patients in enhanced FFS. The findings of significant differences in hospital admission rates for patients in TBC compared to enhanced FFS models are particularly notable, as mental health hospitalization rates are low overall.
This study adds to the existing literature by describing differences in service use across models in Ontario. However, the reasons for differences are not known. For example, data were not available on visits to non-physician providers in TBC models (e.g., dieticians). Accordingly, it is possible that patients with SMI could have been seeing other providers in the team-based model in addition to or instead of their PCP, and these visits would not have been captured in the data. For example, patients may have had fewer visits to physicians and more to non-physician providers who assisted with non-medical aspects of their care. This is more likely because of the broad range of diagnoses included in this study. If more visits to non-physicians and fewer to physicians were observed, this may indicate that providers in TBC models are shifting responsibilities in caring for persons with SMI. This may help providers in TBC models use improved methods of assessment of need for hospitalization, suggesting that the observed increased hospital use was appropriate.
Present findings align with findings from other research on the general Ontario populations that suggested that PCPs in CAP models provide roughly 6-7% fewer services and visits than PCPs in enhanced FFS (Kralj and Kantarevic 2013). In addition, ED use trends observed in this study are consistent with a recent report (Glazier et al. 2012) that found that average number of ED visits per person was higher than expected in CAP and TBC and lower than expected in enhanced FFS.
However, our results did not replicate US findings that reported that compared to FFS, capitation models were associated with fewer mental health hospital admissions, fewer psychiatric ED visits (Bloom et al. 2002; Leff et al. 2005; Rothbard et al. 2004; Warner and Huxley 1998) and mixed patterns of outpatient mental health service use (Busch et al. 2004; Chou et al. 2005; Leff et al. 2005; Morrissey et al. 2002). Like our study, Morrissey et al. (2002) reported that among patients with SMI, being in a full-risk health maintenance organization with a capitation fee, compared to an FFS model, was associated with less use of outpatient psychiatric services and other counselling services. Similarly, a study on Medicaid enrollees with schizophrenia (Busch et al. 2004) reported that persons in a carve-out were one-fourth to one-fifth as likely to receive individual therapy, or group therapy. However, Leff et al. (2005) reported that patients with SMI in managed care had more hours of primary care visits than FFS patients. A Cochrane systematic review (Scott et al. 2011) noted that despite the popularity of different payment systems in primary care, there is little rigorous evidence assessing potential improvements of the quality of this care, and of the cost-effectiveness of these approaches. This difference might be related to systemic policy differences between the Ontario context and many American jurisdictions. Specifically, an access bonus is available to capitation PCPs in Ontario. This bonus decreases when an enrolled patient uses specific out-of-practice services (e.g., visits a walk-in clinic). However, ED visits, specialist visits and hospital admissions are exempt from this financial penalty, meaning there is no deduction from the access bonus even if an enrolled patient visits an ED for non-emergency care (MOHLTC 2011). This suggests that Ontario PCPs may have an inadvertent incentive to have their patients use the ED in preference to other primary care services.
Limitations
This study had several limitations. The accuracy of using individual OHIP codes for identifying a true mental health diagnosis remains unknown. However, administrative measures of mental health service use have been validated in a primary care setting and appear to accurately identify health services provided for mental illness (Bulloch et al. 2011; Spettell et al. 2003; Steele et al. 2004). While the sensitivity (55.3%) for identifying visits related to psychotic disorders is relatively low, this validation was done prior to the institution of incentives for assigning diagnostic codes for psychotic disorders (Steele 2003). Accordingly, the actual sensitivity during the study period was likely higher.
We could not account for variables not included in administrative databases (e.g., severity of mental disorder or visits to non-physicians in TBC models). For the same reason, we could not include individuals with no healthcare use during the study period or examine use of services that are not insured in Ontario (e.g., visits to traditional healers, services delivered by community mental health organizations). In addition, patient characteristics (e.g., income quintile) were measured at one point but may have changed over time, which could have introduced some measurement error. Length of physician visits also could not be measured.
Using shadow billing1 data (only 10% and later 15% of claims were paid in the capitation models) to define mental health groups may have resulted in an underestimation of the number of patients with mental disorders in capitation practices. Alternatively, it is possible that issues are more commonly billed as separate visits in FFS models.
This could have exaggerated the difference between enhanced FFS and CAP models. Whether shadow billing is associated with decreased billings has not been examined in Ontario, but it does not appear likely, as 10%–15% of physician income is based on these billings.
There may have been a selection bias, as in Ontario, PCPs choose the primary care practice in which they work and influence their patient case-mix. A recent Ontario study (Steele et al. 2013) reported that persons with mental illness are under-represented in rosters of capitation models. In spite of this, in the present study, patient characteristics seemed similar across models. However, payment models differed in some measurable characteristics such as percentage of Canadian educated physicians, roster size and physician years in practice. There may also be additional differences in unmeasured characteristics (e.g., physician attitudes) that we did not account for.
There were also limitations associated with this study's cross-sectional design that examined relationships between model membership and service use at one point in time. Accordingly, service use may have occurred when a patient or PCP was in a different model than the one to which they were assigned in the study (i.e., the model in which they were a member) on March 31, 2011. This design also prevented conclusions related to temporal precedence (or causality), such as whether patterns were pre-existing or if they developed after physicians joined new models (Glazier et al. 2009). Independent of when these patterns first developed, they still warrant consideration by policy makers.
Due to the study design and analysis, reasons for observed patterns also could not be ascertained. However, even with this limitation, this study helps to fill the knowledge gap surrounding mental health service use by patients with SMI in different types of primary care models in a setting with universal health insurance. There is a particular need for this research, given that these models were already introduced in Ontario. They are also receiving consideration from policy makers in many jurisdictions including other Canadian provinces (Quebec, Alberta) with ongoing primary care reform. After models have stabilized following changes that occurred over the past decade, future studies on service use for SMI persons should use longitudinal and qualitative methods to examine trends across time and reasons for these trends.
These results are likely not explained by residual confounding by case-mix, as patients in enhanced FFS tend to be sicker (i.e., have higher morbidity levels) than patients in CAP and TBC models (Glazier et al. 2012). However, residual con founding by urban–rural status may contribute to the present results because CAP and TBC models are more common in rural areas. Similarly, largely due to small sample sizes, the findings related to TBC models with and without MHWs were inconclusive.
Strengths and implications
This study found that enrolled patients with SMI in capitation-based models had fewer primary care visits and more ED visits and hospitalizations than patients in enhanced FFS models. As hospitalizations are associated with high costs and disruptions for patients and families, this marks a concern for the Ontario Government and other jurisdictions in the midst of mental health and primary care policy reform (Kirby and Keon 2006; Legislative Assembly of Ontario 2009; SEEI Coordinating Centre 2009). Although we do not report cost data, our study improves on previous research by providing a comprehensive portrait of in-patient and outpatient service use by patients with psychotic or bipolar diagnoses enrolled in enhanced FFS or capitation-based primary care practices (CAP and TBC) in a single-payer system. Moreover, while this study was done in a setting with universal health insurance, factors related to physician remuneration (e.g., risk adjustment) are relevant across jurisdictions. One such jurisdiction is the US, where recent legislative changes (e.g., Patient Protection and Affordable Care Act) put risk adjustment and reinsurance, especially for high-needs patients such as persons with SMI, at the forefront of policy discussions (Barry et al. 2012; NAMI State Advocacy 2011).
In Ontario, careful attention to financial incentives under capitation may be needed to align mental healthcare provision with health system goals. It has been noted that paying larger amounts for caring for patients with specific illnesses is necessary to increase their attractiveness to doctors (Blomqvist and Busby 2012). This applies to patients with SMI who have higher needs than most patients. One possible response is to incorporate adjustments for case-mix into remuneration for PCPs in capitation models. Alternatively, the introduction of additional care incentives could increase the appeal of caring for this population (Steele et al. 2013). For example, process of care incentives could improve quality of primary healthcare delivered to SMI populations in primary care. Quality-of-care incentives in Ontario are already available to PCPs for management of other chronic diseases (e.g., diabetes) (Kiran et al. 2012). As well, existent practice guidelines could provide a basis for incentivizing quality care for people with SMIs in capitation models.
Réforme des soins primaires et utilisation des services chez les usagers souffrant d'un grave problème de santé mentale en Ontario
Résumé
Objet: Cette étude portait sur l'utilisation des services par des adultes aux prises avec un grave problème de santé mentale (GPSM) dans le contexte des nouveaux modèles de prestation de soins primaires: paiement à l'acte amélioré (PA), capitation pondérée (CAP) et capitation fondée sur le nombre d'effectifs (CNE) avec ou sans travailleurs en santé mentale (TSM) en Ontario.
Méthode: Cette étude transversale a fait appel aux bases de données administratives des services de santé afin de comparer l'utilisation des services de santé mentale et des services généraux chez les personnes aux prises avec un GPSM dans le contexte des nouveaux modèles (n=125233).
Résultats: Comparé aux personnes dans le modèle du PA amélioré, ceux des modèles de CAP et de CNE ont fait moins de consultations de premiers soins pour des questions de santé mentale (ratios des taux ajustés et limites de confiance à 95%: CAP: 0,77 [0,74, 0,81]; CNE avec TSM: 0,72 [0,68, 0,76]; CNE sans TSM: 0,81 [0,72, 0,93]). Comparativement aux patients dans le modèle du PA amélioré, ceux des modèles de CNE ont connu plus d'admissions à l'hôpital pour des raisons de santé mentale (CNE avec TSM: 1,12 [1,05, 1,20]; CNE sans TSM: 1,22 [1,05, 1,41]). Les schémas d'utilisation pour les services généraux étaient similaires.
Conclusion: Dans le modèle par capitation, il faudra porter plus d'attention aux incitatifs financiers qui influencent les soins apportés aux personnes souffrant d'un GPSM afin de déterminer s'ils sont conformes aux objectifs visés par la réforme des soins primaires.
About the Author(s)
Leah S. Steele, PhD, Methadone Works, Toronto, ON
Anna Durbin, MPH, Institute of Health Policy Management & Evaluation, University of Toronto, Toronto, ON
Elizabeth Lin, PhD, Provincial System Support Program, Centre for Addiction and Mental Health,, Toronto, ON
J. Charles Victor, MSc, Institute for Clinical Evaluative Sciences, Institute of Health Policy Management & Evaluation, University of Toronto, Toronto, ON
Julie Klein-Geltink, MHSc, Senior Manager, Surveillance, Cancer Care Ontario, Toronto, ON
Richard H. Glazier, MD, MPH, Institute for Clinical Evaluative Sciences, University of Toronto, Toronto, ON
Brandon Zagorski, MS, Institute of Health Policy Management & Evaluation,
Alexander Kopp, BA, Institute for Clinical Evaluative Sciences, Toronto, ON.
Correspondence may be directed to: Leah S. Steele, Methadone Works, 277 Victoria St., Toronto, ON M5B 1W2; tel.: 416-668-4010; e-mail: lssteele@gmail.com.
Acknowledgment
Drs. Steele and Glazier are supported as Clinician Scientists in the Department of Family and Community Medicine at the University of Toronto and at St. Michael's Hospital.
This study was supported by the Institute for Clinical Evaluative Sciences (ICES), which is funded by an annual grant from the Ontario Ministry of Health and Long-Term Care (MOHLTC). The opinions, results and conclusions reported in this paper are those of the authors and are independent from the funding sources. No endorsement by ICES or the Ontario MOHLTC is intended or should be inferred.
References
Barry, C.L., J.P. Weiner, K. Lemke and S.H. Busch. 2012. "Risk Adjustment in Health Insurance Exchanges for Individuals with Mental Illness." The American Journal of Psychiatry 169(7): 704–09.
Blomqvist, Å. and C. Busby. 2012. How to Pay Family Doctors: Why "Pay Per Patient" is Better than Fee-for-Service Primary. CD Howe Institute: Toronto.
Bloom, J.R. T.W. Hu, N. Wallace, B. Cuffel, J.W. Hausman, M.L Sheu et al. 2002. "Mental Health Costs and Access under Alternative Capitation Systems in Colorado." Health Services Research 37(2): 315–40.
Bradford, D.W., M.M. Kim, L.E. Braxton, C.E. Marx, M. Butterfield and E.B. Elbogen. 2008. "Access to Medical Care among Persons with Psychotic and Major Affective Disorders." Psychiatric Services 59(8): 847–52.
Bulloch, A.G., S. Currie, L. Guyn, J.V. Williams, D.H. Lavorato and S.B. Patten. 2011. "Estimates of the Treated Prevalence of Bipolar Disorders by Mental Health Services in the General Population: Comparison of Results from Administrative and Health Survey Data." Chronic Diseases and Injuries in Canada 31(3): 129–34.
Busch, A.B., R.G. Frank and A.F. Lehman. 2004. "The Effect of a Managed Behavioral Health Carve-Out on Quality of Care for Medicaid Patients Diagnosed as Having Schizophrenia." Archives of General Psychiatry 61(5): 442–48.
Chou, A.F., N. Wallace, J.R. Bloom and T.W. Hu. 2005. "Variation in Outpatient Mental Health Service Utilization under Capitation." The Journal of Mental Health Policy and Economics 8(1): 3–14.
Deber, R.B., M.J. Hollander and P. Jacobs. 2008. "Models of Funding and Reimbursement in Health Care: A Conceptual Framework." Canadian Public Administration 51(3): 381.
Deber, R.B. 2008. "Access without Appropriateness: Chicken Little in Charge?" Healthcare Policy 4(1): 23–29.
Durbin, A., J. Durbin, J. Hensel and R. Deber. 2013. "Barriers and Enablers to Integrating Mental Health and Addictions into Primary Care: A Policy Analysis." Journal of Behavioral Health Services & Research 1–13. doi: 10.1007/s11414-013-9359-6.
Glazier, R.H., B.M. Zagorski and J. Rayner. 2012. Comparison of Primary Care Models in Ontario by Demographics, Case Mix and Emergency Department Use, 2008/09 to 2009/10. Toronto: Institute for Clinical Evaluative Sciences.
Glazier, R.H., J. Klein-Geltink, A. Kopp and L.M. Sibley. 2009. "Capitation and Enhanced Fee-for-Service Models for Primary Care Reform: A Population-Based Evaluation." Canadian Medical Association Journal 180(11): E72–81.
Glazier, R.H. and D.A. Redelmeier. 2010. "Building the Patient-Centered Medical Home in Ontario." The Journal of the American Medical Association 303(21): 2186–87.
Gold, K.J., A.M. Kilbourne and M. Valenstein. 2008. "Primary Care of Patients with Serious Mental Illness: Your Chance to Make a Difference." The Journal of Family Practice 57(8): 515–25.
Goldberg, R.J. 1999. "Financial Incentives Influencing the Integration of Mental Health Care and Primary Care." Psychiatric Services 50(8): 1071–75.
Gosden, T., F. Forland, I.S. Kristiansen, M. Sutton, B. Leese, A. Giuffrida et al. 2001. "Impact of Payment Method on Behaviour of Primary Care Physicians: A Systematic Review." Journal of Health Services Research and Policy 6(1): 44–55.
Hardin, J.W. and J.M. Hilbe. 2003. Generalized Estimating Equations. Chapman and Boca Raton, FL: Hall/CRC
Hellinger, F.J. 1996. "The Impact of Financial Incentives on Physician Behavior in Managed Care Plans: A Review of the Evidence." Medical Care Research and Review: MCRR 53(3): 294–314.
Hux, J.E., F. Ivis, V. Flintoft and A. Bica. 2002. "Diabetes in Ontario: Determination of Prevalence and Incidence Using a Validated Administrative Data Algorithm." Diabetes Care 25(3): 512–16.
Institute of Psychiatry. 2007. Mental Health Care. Schizophrenia. What's the Difference Between Schizophrenia and Psychosis. Retrieved July 22, 2014. <http://www.mentalhealthcare.org.uk/content/?id=188>.
The Johns Hopkins Adjusted Clinical Groups (ACG) Case-Mix System. 2008. Retrieved September 21, 2009. <http://www.acg.jhsph.edu/>.
Kiran, T., C. Victor, A. Kopp, B. Shah and R.H. Glazier. 2012. "The Relationship between Financial Incentives and Quality of Diabetes Care in Ontario." Diabetes Care 35(5): 1038–46.
Kirby, M. and M.J. Keon. 2006. Out of the Shadows at Last: Transforming Mental Health, Mental Illness, and Addictions in Canada. Ottawa, ON: The Standing Senate Committee on Social Affairs, Science, and Technology. Retrieved July 22, 2014. <http://www.parl.gc.ca/39/1/parlbus/commbus/senate/com-e/soci-e/rep-e/pdf/rep02may06part1-e.pdf>.
Kralj, B. 2009. Measuring Rurality - RIO2008_BASIC: Methodology and Results. Retrieved July 22, 2014. <https://www.oma.org/Resources/Documents/2008RIO-FullTechnicalPaper.pdf>.
Kralj, B. and J. Kantarevic. 2013. "Quality and Quantity in Primary Care Mixed-payment Models: Evidence from Family Health Organizations in Ontario." Canadian Journal of Economics 46(1): 208–38.
Lavoie, K.L. and R.P. Fleet. 2002. "Should Psychologists be Granted Prescription Privileges? A Review of the Prescription Privilege Debate for Psychiatrists." Canadian Journal of Psychiatry 47(5): 443–49.
Lawrence, D. and S. Kisely. 2010. "Inequalities in Healthcare Provision for People with Severe Mental Illness." Journal of Psychopharmacology 24(4 Suppl): 61–68.
Leff, H.S., D.A. Wieman, B.H. McFarland, J.P. Morrissey, A. Rothbard, D.L. Shern et al. 2005. "Assessment of Medicaid Managed Behavioral Health Care for Persons with Serious Mental Illness." Psychiatric Services 56(10): 1245–53.
Legislative Assembly of Ontario. 2009. Committee Transcripts: Select Committee on Mental Health and Addictions - September 16, 2009 - Mental Health And Addictions Strategy. Unpublished manuscript.
Lin, E., P. Goering, D.R. Offord, D. Campbell and M.H. Boyle. 1996. "The Use of Mental Health Services in Ontario: Epidemiologic Findings." Canadian Journal of Psychiatry 41(9): 572–77.
Ministry of Health and Long Term Care (MOHLTC). 2011. Chapter 3. Section 3.06. Funding Alternatives for Family Physicians in 2011 Annual Report of the Office of the Auditor General of Ontario. 2013. Retrieved July 22, 2014. <http://www.auditor.on.ca/en/reports_en/en11/306en11.pdf>.
Morrissey, J.P., T.S. Stroup, A.R. Ellis and E. Merwin. 2002. "Service use and Health Status of Persons with Severe Mental Illness in Full-Risk and No-Risk Medicaid Programs." Psychiatric Services 53(3): 293–98.
NAMI State Advocacy. 2011. The Affordable Care Act. 2013. Retrieved July 22, 2014. <http://www.nami.org/Content/NavigationMenu/State_Advocacy/About_the_Issue/Affordable_Care_Act_Fact_Sheet_2011.pdf>.
Narrow, W.E., D.A. Regier, G. Norquist, D.S. Rae, C. Kennedy and B. Arons. 2000. "Mental Health Service use by Americans with Severe Mental Illnesses." Social Psychiatry and Psychiatric Epidemiology 35(4): 147–55.
National Institute for Health and Clinical Excellence. 2012. Stepped Care Models [Internet]. Retrieved June 10, 2014. <http://www.nice.org.uk/usingguidance/commissioningguides/cognitivebehaviouraltherapyservice/steppedcaremodels.jsp>.
Oud, M.J., J. Schuling, K.H. Groenier, P.F. Verhaak, C.J. Slooff, J.H. Dekker et al. 2010. "Care Provided by General Practitioners to Patients with Psychotic Disorders: A Cohort Study." BMC Family Practice 11(1): 92.
Petersen, L.A., L.D. Woodard, T. Urech, C. Daw and S. Sookanan. 2006. "Does Pay-for-Performance Improve the Quality of Health Care?" Annals of Internal Medicine 145(4): 265–72.
Ray, J.G., M.J. Vermeulen, M.J. Schull, G. Singh, R. Shah and D.A. Redelmeier. 2007. "Results of the Recent Immigrant Pregnancy and Perinatal Long-Term Evaluation Study (RIPPLES)." Canadian Medical Association Journal 176(10): 1419–26.
Regier, D.A., W.E. Narrow, D.S. Rae, R.W. Manderscheid, B.Z. Locke and F.K. Goodwin. 1993. "The de Facto US Mental and Addictive Disorders Service System. Epidemiologic Catchment Area Prospective 1-year Prevalence Rates of Disorders and Services." Archives of General Psychiatry 50(2): 85–94.
Rosser, W.W., J.M. Colwill, J. Kasperski and L. Wilson. 2010. "Patient-Centered Medical Homes in Ontario." New England Journal of Medicine 362(3): e7.
Rothbard, A.B., E. Kuno, T.R. Hadley and J. Dogin. 2004. "Psychiatric Service Utilization and Cost for Persons with Schizophrenia in a Medicaid Managed Care Program." The Journal of Behavioral Health Services and Research 31(1): 1–12.
Samele, C., M. Patel, J. Boydell, M. Leese, S. Wessely and R. Murray. 2007. "Physical Illness and Lifestyle Risk Factors in People with their First Presentation of Psychosis." Social Psychiatry and Psychiatric Epidemiology 42(2): 117–24.
Schlesinger, M. and D. Mechanic. 1993. "Challenges for Managed Competition from Chronic Illness." Health Affairs (Project Hope) 12(Suppl): 123–37.
Schultz, S., D.M. Rothwell, Z. Chen and K. Tu. 2013. "Identifying Cases of Congestive Heart Failure from Administrative Data: A Validation Study Using Primary Care Patient Records." Chronic Diseases in Canada 33(3): 160–66.
Scott, A., P. Sivey, D. Ait Ouakrim, L. Willenberg, L. Naccarella, J. Furler et al. 2011. "The Effect of Financial Incentives on the Quality of Health Care Provided by Primary Care Physicians." Cochrane Database of Systematic Reviews 9(9). doi: 10.1002/14651858.CD008451.
SEEI Coordinating Centre. 2009. Moving in the Right Direction: SEEI Final Report. Health Systems Research and Consulting Unit. Toronto. Centre for Addiction and Mental Health.
Shearer, D.S., S.C. Harmon, B.M. Seavey and A.Y. Tiu. 2012. "The Primary Care Prescribing Psychologist Model: Medical Provider Ratings of the Safety, Impact and Utility of Prescribing Psychology in a Primary Care Setting." Journal of Clinical Psychology in Medical Settings 19(4): 420–29.
Spettell, C.M., T.C. Wall, J. Allison, J. Calhoun, R. Kobylinski, R. Fargason et al. 2003. "Identifying Physician-recognized Depression from Administrative Data: Consequences for Quality Measurement." Health Services Research 38(4): 1081–102.
Steele, L.S. 2003. Measuring Ambulatory Mental Health Services Using Administrative Data. In: Ambulatory Mental Health Service Use in an Inner City Setting: Measurement, Patterns and Trends [Doctoral Dissertation]. Toronto, ON: University of Toronto.
Steele, L.S., A. Durbin, L.M. Sibley and R.H. Glazier. 2013. "Inclusion of Persons with Mental Illness in Patient-Centred Medical Homes: Cross-sectional Findings from Ontario, Canada." Open Medicine 7(1): e9–20.
Steele, L.S., R.H. Glazier, E. Lin and M. Evans. 2004. "Using Administrative Data to Measure Ambulatory Mental Health Service Provision in Primary Care." Medical Care 42(10): 960–65.
Thornicroft, G. 2011. "Physical Health Disparities and Mental Illness: The Scandal of Premature Mortality." The British Journal of Psychiatry: The Journal of Mental Science 199(6): 441–42.
Tu, K., N.R. Campbell, Z.I. Chen, K.J. Cauch-Dudek and F.A. McAlister. 2007. "Accuracy of Administrative Databases in Identifying Patients with Hypertension." Open Medicine: A Peer-Reviewed, Independent, Open-Access Journal 1(1): e18–26.
Vasiliadis H.M., A. Lesage, C. Adair, P.S. Wang and R.C. Kessler. 2007. "Do Canada and the United States Differ in Prevalence of Depression and Utilization of Services?" Psychiatric Services 58(1): 63–71.
Warner, R. and P. Huxley. 1998. "Outcome for People with Schizophrenia Before and After Medicaid Capitation at a Community Agency in Colorado." Psychiatric Services 49(6): 802–07.
Footnotes
1. Shadow billing involves submitting information about the services a physician provides. Information, however, is submitted for administrative/tracking purposes, not for reimbursement.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed