Healthcare Quarterly
A Health System for Patients with Complex Conditions: Reflections from Bridgepoint’s Transformation
Introduction
How can a traditional chronic care and rehabilitation hospital transform itself to provide high-quality care to people with complex health conditions – those with multiple health problems together with psycho-social issues – who need a thoughtful, evidence-informed but personalized approach to healthcare? How can health policy support this type of innovation? Bridgepoint has been on a journey for almost 20 years to transform care for the growing population at large and within our healthcare system, with increasingly complex health conditions. Until very recently, those of us who are convinced that both chronic disease and complexity are the next frontier of modern healthcare were lonely voices. Recent recognition of the existence of these patients, through analysis of healthcare utilization and accounts of inadequate care, is a critical development. Recognition is the first step to challenging the current construct of our healthcare system to make the necessary changes to deliver better care for patients and create better value for governments and taxpayers. Having places like Bridgepoint share their journey will also open up key insights into new roles for healthcare services and pathways that governments can use to support them in this journey.
Bridgepoint
Bridgepoint is a hospital, a family health practice and a research collaboratory in Toronto. It recently amalgamated with Mount Sinai Hospital and affiliated with Circle of Care (a home care agency) to form the Sinai Health System.
Bridgepoint has been on the front line of dealing with patients with complex health conditions, who are the most visible symbol of both the progress in our health and care delivery systems as well as of a critical need for transformative change. Thanks to the success of modern medicine, people are living longer, and experiencing increasingly complex health conditions.
I often describe the existence of these patients and our response to them as the great paradox of modern medicine – all the hype, noise and public and political outcry about the sustainability of our healthcare system are actually because we've been so spectacularly successful.
Healthcare Advances
The first part of the last century saw the greatest improvement in population health in human history, at least in the developed world. And that improvement was overwhelmingly driven by advances in public health. Clean water and better hygiene, combined with immunizations, helped us conquer infectious disease. Healthcare played a part, too, through interventions like antibiotics and better access to medical care. These great advances in public health resulted in new challenges. As the incidence of diseases like cholera plummeted, cancer rates grew. People began living long enough to develop more cancer, heart disease, diabetes and other conditions.
A second era of innovation took the spotlight, focusing mainly on basic science and life-saving acute care, delivered primarily through hospitals. From the 1950s through to the turn of this century, science and medicine turned their attention to understanding human biology and how to diagnose and treat when things go wrong. Our acute hospital–centric system was designed – well designed, in fact – to treat these new disease states and provide focused interventions. And it worked. The death rate from cardiovascular disease dropped by more than half. Joint replacements, unknown fifty years ago, enable 60,000 Canadians a year to regain mobility. Disease by disease, intervention by intervention, at every age cohort, the list of successes goes on. But what does that mean for the health of the population and for our healthcare system? Well, it's now full of survivors.
The Complexity Challenge
The reality in Ontario today is that 13 million people – roughly 70% – have one chronic condition, 80% have two or more and we've now heard from the Institute for Clinical Evaluative Sciences (ICES), Canadian Institute for Health Information (CIHI) and the government about the 5% of patients who use 70% of all healthcare resources. The result is that we are now managing something that was unknown 50 years ago – complex patients living for years with multiple chronic conditions. These are the patients of Bridgepoint. But because they utilize healthcare resources in huge quantities, they are also the patients of our entire healthcare system. Bridgepoint identified and started to focus on this issue almost 20 years ago.
In 1997, the Ontario Government's Health Services Restructuring Commission decided that hospitals like Bridgepoint (then Riverdale Hospital) that, more through good luck than good planning, had come to specialize in providing care for patients with chronic and increasing complex illnesses, were no longer necessary. This policy direction certainly caught our attention and started us on what has turned out to be an evolving transformation in our understanding of patients with complex health issues and how to serve them.
We started by looking for evidence to support our intuition that what we were seeing in our hospital – a huge change in the complexity of the people we were serving – might be a prevalent phenomenon, with implications for not just our future, but also for that of our entire healthcare system. We decided to dig deeper into this issue. The early evidence we uncovered convinced us, and ultimately the Government of Ontario, that chronic disease and complexity were on the rise and that hospitals like Bridgepoint should not be closed; it was not closed.
Bridgepoint – Understanding the Complex Patient Population and Its Needs
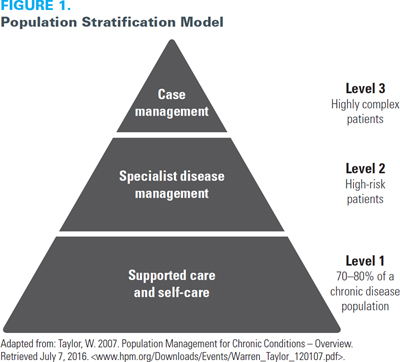
With that crisis resolved, we set ourselves on a course to use Bridgepoint and the patients we serve as a living laboratory to gain insight into what we really need to do as a healthcare system and society to address this emerging need. We looked at leading systems and health maintenance organizations (HMOs) around the world and found resonance in Kaiser Permanante's Population Stratification Model (Figure 1) – this was a moment of insight for us.
We started to look at our own population and health system through this lens.
Of course, what we uncovered is now a recognized global phenomenon: in Ontario, 170,000 patients use $9 billion of healthcare funding per year and are not getting good outcomes.
These are the people at the top of the Kaiser pyramid, characterized by multiple, complex health issues, yet we knew very little about them apart from utilization data. We also could not find many insights into how to manage these patients, except for the Chronic Disease Management (CDM) concepts of intensive case management and interprofessional care. There was very little evidence-based medicine, and there were no clinical pathways for treating these patients. Virtually all clinical trials and most clinical pathways are conducted on or created for patients without complications. Therefore, the vast majority of our most complex patients are actually excluded from "evidence-based" healthcare.
In 2005, we declared that there is a new disease out there. It's not just chronic disease – it's illness combinations such as "neurodiabesity," "osteocanceritis," and the list goes on! We also declared that the growing incidence and prevalence of complex health conditions is a game changer for health systems and policy.
The Strategy
Against that backdrop, Bridgepoint developed a bold, 10-year strategy and vision to transform itself to respond to Ontario's and Canada's biggest healthcare challenge. We made it our mission to revolutionize care delivery, create new science, develop new curricula, and forge new relationships with innovators in the field to "change the world for complex patients."
To deliver on our vision and mission, we did the following:
- Established the Bridgepoint Collaboratory for Research and Innovation, the first in the world devoted entirely to developing the evidence and new models required to address the needs of these patients.
- Established the Bridgepoint family health team as an incubator and exemplar of primary care models and practices that could effectively manage and prevent chronic disease and complexity in the population.
- Developed new models and competencies to address the growing needs of these patients.
- Became affiliated with the University of Toronto to drive evidence-based practice and lay the ground for new curriculum.
- Built a new hospital and campus of care, the first of its kind, designed specifically to meet the needs of complex patients.
The Bridgepoint Collaboratory started its work with a piece of groundbreaking research – "The Bridgepoint Study" – which confirmed many of the things we had already suspected. The study showed that the complex patient's journey often presents with a single chronic disease that is just the "tip of the iceberg." What appears at first belies the multiple layers of potential complexity that, left unaddressed, will erupt into a complex patient.
Complex patients are characterized by clinical complexity: multimorbidity, polypharmacy, high treatment burden and fragmented care (in our predominately acute, reactive, highly specialized and fragmented healthcare delivery system).
These patients are also characterized by social complexity: social vulnerability, depression, addiction, social isolation and coping and adaptation challenges.
The study revealed high variability in the complex patient population and significant gaps between our current system and their needs:
- Existing data systems do not capture complexity.
- The current acute, episodic system is a poor fit for complex patients.
- Care plans do not address coping, adaptation or transitions effectively.
- Significant missed opportunities exist for prevention all the way through these patients' trajectory.
These results led us to conclude that we need fundamental change at all levels of our healthcare system: (a) at the level of the patient in the evidence used to treat them; (b) at the level of the system in how we organize care delivery; and (c) at the policy, planning and research levels and in the data we use for decision-making, outcome and performance measurement.
Bridgepoint's Transformation
With that evidence in hand, we started our transformation journey, beginning at the level of the patient. Our team designed a new approach to care, which included:
- A comprehensive 360-degree assessment by an interprofessional team, which has been implemented on our complex medical care units
- Treatment and management strategies for physical as well as psychosocial issues
- A shift in focus to optimal function and compression of morbidity and risk
- A high quality, safe experience in and out of hospital
- Support for coping and adaptation
- Advocacy, training and support for formal and informal caregivers
- Creating and offering a community-connecting, health-promoting environment
We redefined which outcomes it would be appropriate to focus on for these patients: optimized health and well-being; improved quality of life; optimized functionality; improved coping, adaptation and self-efficacy; reduced risk and healthcare utilization and enhanced social capital.
At the level of the system, the Bridgepoint team developed a new model of care delivery. The model is based on the idea that addressing the needs of these patients begins with a fundamental paradigm shift. That paradigm shift would evolve and replace our acute, episodic, reactive care model – where acute care hospitals are the entry point to everything – with a proactive, comprehensive, integrated, continuous "health hub," with primary care and patients at the centre (Figure 2).
We began implementing the Bridgepoint Model by partnering with primary care and community providers in our catchment area, developing a short-stay evaluation unit with direct access from primary care; implementing complexity clinics; and starting a new "Bridges to Home" program, to follow high-risk patients in "shared care" with their primary care doctors.
While Bridgepoint made good progress on its own in rethinking and reorganizing care for these patients, we ultimately knew that in order to make meaningful inroads, the whole system would need to change.
The Case for Integration Within a Bigger System
There is abundant evidence that without a comprehensive, integrated health and care system, we create unnecessary burden of illness in the population; utilize more healthcare resources and subject patients to duplication that is unnecessary at best and harmful at worst. Nowhere is this more evident than in the care of complex patients. There is a huge role and a missed opportunity for hospitals to engage in primary and secondary prevention. When complex patients do need care, they need a single care plan, single care team, aligned goals and incentives, across the life course and across the continuum.
Hospitals and the people in them need to see themselves as part of the community, not separate from it. They also need to be full partners, not just with patients and their families while they are in our care, but with primary care, public health and the community in preventing and managing the increasing burden of illness in the population.
Funding for the care also needs to be better integrated so that there is incentive in the system to truly provide care in the right place at the right time. Our current siloed, industrial funding model, which promotes reactive, episodic, volume-based care, is totally misaligned with the needs of patients with complex health conditions.
That's why Bridgepoint reimagined itself as part of a hub and spoke model, in partnership with the community and primary care. That is also why we joined with Mount Sinai Hospital (an academic, acute/tertiary care hospital) and Circle of Care (a multi-service home support agency) to create an exemplar of an integrated healthcare system – bringing together all the elements required to address the needs of complex patients.
Sinai Health System
The vision of Sinai Health System is to create Canada's leading integrated health system, pushing the boundaries to realize the best health and care, from healthy beginnings to healthy aging for people with complex health needs. We will achieve this vision through delivering exceptional care in hospital, community and home, focusing on the health conditions with the greatest impact on the overall health of the population.
We are also committed to discovering and translating scientific breakthroughs, developing practical health solutions, educating future clinical and scientific leaders, and leading efforts to eliminate health inequities. This is our mission!
As a vertically integrated system, we are now implementing seamless care across more of the continuum, such as admitting patients directly to Bridgepoint from the emergency department without requiring an acute admission. We are also bringing an increasingly capable group of specialists and sub-specialists into interprofessional care teams to develop integrated care plans for a wide range of complex patients. Ultimately, patients will be enrolled and followed on a proactive basis by Sinai Health System, in partnership with primary care.
Beyond Sinai Health System, at the macro level, our broader system needs major change to enable us and others to provide truly comprehensive and integrated care, in the areas of money, integration, data and intervention research, assessment and performance tools, and training.
1. Money
Funding and incentives need to support and reward earlier treatment and prevention and treatment in the right setting of care. We know that is true for all patients, but with no other population is it more urgent than for patients with complex health issues, who are the highest users of health services. Risk-adjusted, bundled payments for the care of specific populations, especially complex patients, are the way of the future.
2. Integration
We are convinced that the kind of vertical integration Sinai Health System has helped to pioneer will need to continue, with more elements of the care continuum for complex patients within integrated provider organizations that are accountable for a complex patient's whole experience and capable of managing the most important parts of it.
3. Data and intervention research
Our health system needs data, research and new evidence to help us understand and address the numerous clinical and health system questions that arise when dealing with people who have multiple health conditions and need complex care. We simply do not have solid evidence on what works – or even what constitutes safe care – for a patient with six conditions and 12 medications.
Sinai Health System is dramatically expanding the research on complexity pioneered by Bridgepoint's Collaboratory for Research, within the Lunenfeld-Tanenbaum Research Institute, and connecting the network of clinicians and scientists in our organization and around the world who are focused on clinical and health services research in the field of complexity. A number of research teams and collaborations have been developed over the last five years.
4. Assessment and performance tools
From a patient quality and safety perspective, our current acute-focused approach and many of the tools that have been enormously successful with single illnesses and disabilities will be insufficient to address complexity. There is no checklist for a patient with diabetes, Parkinson's disease and a broken hip, who is on 14 medications and appears to be reacting badly. At a minimum, research needs to inform principles, guidelines and standards on providing quality care, as do the health performance organizations like the Institute for Healthcare Improvement (IHI), Canadian Patient Safety Institute, and others.
5. Training
We need to develop and teach new curriculum, based on evidence specific to these patients. We will always need oncologists, but we will also need "complexity specialists" – hospital and community-based professionals with deep training in how to manage multiple conditions in the same patient. We will also need health policy experts and administrators who are trained in complexity and health systems reform.
The evolving success Sinai Health System has begun to experience in advancing care for complex patients is rooted in deeply held values of patient-centredness, the dignity of individual patients and caregivers, and a belief that we really can make these people's lives better. Each of the organizations that came together to form Sinai Health System was originally founded to address some health inequity. It is that tradition that now inspires us to focus on complex patients.
Conclusion
I began by saying that it is encouraging that the healthcare world is beginning to take notice and focus on the central challenge and opportunity of complexity in our health system. As I reflect on what Bridgepoint – now Sinai Health System – has accomplished, I am even more encouraged because we see the path ahead and are already producing results.
Sinai Health System is just one organization. While we have the advantage of being highly focused on people with complex conditions, truly changing the world for these patients will require a national and global effort. I look forward to the help of the growing community of clinicians, researchers and policy makers who share my conviction that addressing the needs of people living with complex health conditions truly is the next frontier of healthcare. As others begin to focus on this issue – and I would encourage them to do so – they have willing partners and collaborators in Sinai Health System. There is much to learn and much to do better.
About the Author(s)
Marian Walsh, long-time president and CEO of Bridgepoint Active Healthcare, is now associate CEO and chief transformation officer of Sinai Health System, which includes: Bridgepoint; Mount Sinai Hospital; and Circle of Care, a home and community support agency. Marian has had a 30-plus year career as a CEO in healthcare and has been an effective advocate for transforming the healthcare system to meet the evolving needs of patients.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed