Healthcare Policy
The Delivery of Patient Care in Ontario’s Family Health Teams during the First Wave of the COVID-19 Pandemic
Abstract
Objective: The objective of this paper was to identify continuations and changes in care delivery methods in primary care teams during the COVID-19 pandemic.
Design: The study used a cross-sectional, web-based survey comprising close-ended and open-ended questions.
Setting: The setting comprised family health teams (FHTs) across Ontario, Canada.
Participants: The participants included executive directors of FHTs or designates of their choosing.
Survey: Descriptive statistics were derived from responses to close-ended questions, and responses to open-ended questions were coded using thematic analysis.
Results: With 93 participants, the response rate was 48%. Participants reported the continuation of in-person care, the implementation of virtual care across FHTs and collaboration within these teams and their communities.
Introduction
Primary care is a first line of defence in a pandemic (Alex et al. 2020; Rawaf et al. 2020). Having long-standing relationships with patients means primary care is optimally positioned to help manage patients at home and identify patients who require hospitalization (Alex et al. 2020; Rawaf et al. 2020). The onset of the COVID-19 pandemic required primary care to quickly transform to adhere to physical distancing requirements while still maintaining connection with patients (Alex et al. 2020; Krelle et al. 2020; Lewnard and Lo 2020).
Healthcare Delivery during the COVID-19 Pandemic
Before the COVID-19 pandemic, few primary care practices routinely used virtual care for direct patient assessments (Krelle et al. 2020). Virtual care refers to "any interaction between patients and/or members of their circle of care, occurring remotely, using any forms of communication or information technologies, with the aim of facilitating or maximizing the quality and effectiveness of patient care" (Jamieson et al. 2015: 4). Many primary care practices have undergone rapid expansion of synchronous virtual care (e.g., telephone and video appointments) with minimal preparation time while maintaining as much continuity as possible for patients (Donnelly et al. 2021; Krelle et al. 2020; Rawaf et al. 2020). The pandemic has accelerated virtual primary care in Canada and worldwide, with limited evidence to guide this full-scale pivot (Krelle et al. 2020; Government of Ontario 2019a). Other challenges include prioritizing which patients require in-person assessments, accessing personal protective equipment (PPE) due to a worldwide shortage and collaborating with other providers who may be facing gaps in care delivery due to limited resources (Alex et al. 2020; Lewnard and Lo 2020; Rawaf et al. 2020).
Team-Based Primary Care in Ontario, Canada
Team-based primary care brings family physicians together to work in tandem with a range of interprofessional healthcare providers (IHPs) – such as nurses, nurse practitioners, social workers, dietitians and pharmacists among others – in the same practice setting (Donnelly et al. 2021). Primary care teams are associated with improved clinical outcomes, positive patient experiences and decreased healthcare utilization (Gocan et al. 2014; Khan et al. 2021; Manns et al. 2012; Morgan et al. 2020; Mulvale et al. 2009; Strumpf et al. 2017).
Different primary care models respond to different types of community needs, patient populations and provider preferences (Glazier et al. 2012; Hutchison and Glazier 2013). In Canada, Ontario has advanced interprofessional primary care particularly with the investment and expansion of several team-based primary care models including family health teams (FHTs), community health centres (CHCs), nurse practitioner–led clinics (NPLCs) and Indigenous interprofessional primary care teams (IIPCTs) (Brown and Ryan 2018; Government of Ontario 2018; Haydt 2018; Heale et al. 2018; Hutchison and Glazier 2013). FHTs are an example of a newer team-based model of primary care that emerged in 2005 from a period of healthcare system reform (Hutchison et al. 2011). There are 184 FHTs providing services to approximately 25% of Ontario's population, with the FHTs being the largest team-based primary care model in Canada (Glazier et al. 2012; Somé et al. 2020). The implementation of FHTs was intended to expand access to comprehensive healthcare services, particularly for the prevention, treatment and management of chronic conditions (Hutchison et al. 2011). FHTs vary in terms of organizational size, composition of types and numbers of providers (Ashcroft et al. 2021b; Rudoler et al. 2019). There is also variation in the types and numbers of services offered by family physicians and other interprofessional providers across FHTs (Hutchison and Glazier 2013). Provincially, the trend is for FHTs to enroll patients who are healthier and have higher socio-economic status than CHCs (Glazier et al. 2015). This is not necessarily the case, however, for communities that have a broad distribution of FHTs across all neighbourhoods or for FHTs located in neighborhoods with significant socio-economic disparities (Ly et al. 2021).
Originally established in the 1970s, CHCs prioritize care for vulnerable populations and are most likely to serve disadvantaged populations (Collins et al. 2014; Hastings 1972; Haydt 2018). CHCs are driven by a social-determinants-of-health framework and are designed to meet a broad range of patient and local community needs unique to the disadvantaged populations they serve (Collins et al. 2014; Glazier et al. 2012). Additionally, CHCs are a community-involved and community-governed model of primary care and include a broad range of services including community outreach activities (Haydt 2018). NPLCs were created in 2007, and 24 NPLCs are currently operating across Ontario (Haydt 2018). In NPLCs, nurse practitioners are the clinical leaders of an interprofessional team that is inclusive of providers from a broad range of disciplinary backgrounds, including physicians. Physicians in NPLCs mainly act as consultants and provide guidance for issues that fall outside of the nurse practitioners' scope of practice (Haydt 2018). Most recently, IIPCTs were established in 2018 (Government of Ontario 2018). Interprofessional teams comprise a diverse range of healthcare providers, including traditional Indigenous healers (Government of Ontario 2018). IIPCTs are primary care teams located in Indigenous communities, are Indigenous governed and are community driven (Government of Ontario 2018).
Team-based primary care provides access to a wide range of comprehensive physical, behavioural and mental health services (Beaulieu et al. 2013; CFPC 2019; Tadic et al. 2020); thus, primary care teams are well-positioned to address the wide-range of patient needs that have emerged during the COVID-19 pandemic (Donnelly et al. 2021; Holmes et al. 2020). Early reports are beginning to emerge about the role of primary care during the COVID-19 pandemic (Bhatti et al. 2020; Donnelly et al. 2021; Kearon and Risdon 2020). There is little understanding, however, of the continuations and changes in care delivery methods in team-based primary care in Ontario as shaped by the first wave of the COVID-19 pandemic.
Rationale and Objective
We conducted a survey to better understand how team-based primary care practices in Ontario, Canada, delivered care during the first wave of the COVID-19 pandemic. Our study will shed some light on the experiences of primary care in order to better prepare physicians and other primary care providers, leaders and policy makers for the ongoing demands of the COVID-19 and future pandemics. The overarching objective of our study was to determine how Ontario-based primary care teams delivered patient care throughout the first wave of the COVID-19 pandemic. We report the results of that study here, drawing important policy lessons for other jurisdictions on the planning and sustainability issues involved in primary care's pivot to virtual care delivery. To our knowledge, this is the first study to survey leadership in team-based primary care for this purpose.
Method
Study design
We developed and implemented a cross-sectional, web-based survey to answer the following questions: How did team-based primary care practices deliver patient care during the first wave of the COVID-19 pandemic? What is the future of virtual care appointments in team-based primary care? We obtained ethics approval from the University of Toronto Research Ethics Board (REB Protocol #39432).
A previous survey of primary care teams during COVID-19, which focused on the interprofessional healthcare providers' perspectives (Donnelly et al. 2021), inspired the development of this web-based survey. In partnership with The Association of Family Health Teams of Ontario (AFHTO) – a provincial organization that supports and advocates on behalf of primary care teams in Ontario – we developed our survey using Qualtrics software. The final web-based survey included close- and open-ended questions that aligned with the study objectives. Survey questions were related to delivery of care during the pandemic, the use of virtual care during the pandemic and recommendations for virtual care post-pandemic.
Sample
We used a convenience sampling technique to engage a population of executive directors – or designates of their choosing – of team-based primary care organizations. Potential participants were those who were able to complete a web-based survey in English and were employed at the time of survey within one of the 191 primary care teams that are members of AFHTO. Although the composition of providers varies within each of AFHTO's member organizations, teams typically comprise family physicians, nurse practitioners, nurses, social workers, pharmacists, dietitians and/or other IHPs (Hutchison et al. 2011). AFHTO's member organizations include 184 FHTs, 5 NPLCs, 1 CHC and 1 interprofessional care team.
Recruitment
Executive directors of all AFHTO member organizations were sent an invitation to participate in the web-based survey through recruitment e-mails. The web-based survey was open from July 17, 2020, to September 15, 2020. No recruitment incentive was used.
Data analysis
Descriptive statistics were conducted on the 21 close-ended questions using the Qualtrics software. We conducted a thematic analysis on the subset of the responses to the open-ended questions (Braun and Clarke 2006). After importing the qualitative data from the open-ended questions from Qualtrics to Microsoft Excel, two researchers (RA and MD) analyzed the data. First, the two researchers became familiar with the data by reviewing the open text responses. One researcher acting as the primary coder completed the analysis, and the secondary coder reviewed the coding structure in detail. The two researchers regularly met throughout the duration of the initial coding process to review, discuss and refine codes as needed. The two researchers reviewed the codes for potential themes, following which the entire research team had an opportunity to review the themes and provide input at a virtual team meeting. During this process, we also identified quotes exemplifying key themes. The coding process and the thematic development were inductive.
Results
The response rate was 48%, with participants representing 92 primary care organizations. A total of 93 individual participants completed the survey; however, two participants were from the same FHT. Therefore, only 92 distinct primary care organizations participated in our study. Almost all of the participants identified as being in a leadership position, with 87% (n = 81) of participants being either executive directors, 5% (n = 5) being managers or administrative leads, 4% (n = 4) being in a clinic director role, 1% (n = 1) identifying as a program coordinator, 1% (n = 1) being a nurse practitioner and 1% (n = 1) remaining unknown because the participant did not identify their role. The 93 participants represented the following 92 primary care organizations: 88 FHTs, 3 NPLCs and 1 CHC that spanned all five geographical regions (Government of Ontario 2019b).
Continuing in-person care
Nearly all participants (99%) indicated that some in-person care continued to be offered throughout the first wave (March through August, 2020) of the COVID-19 pandemic. Well-baby (91%) and prenatal visits (88%) were the most frequently provided assessments in-person (see Figure 1).
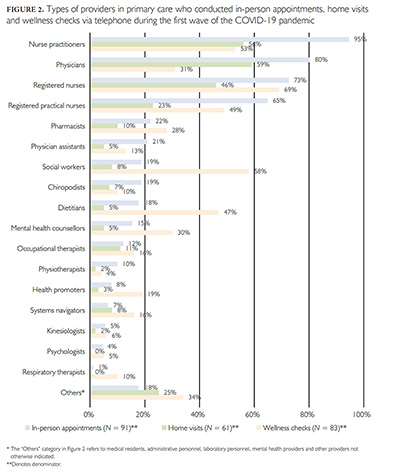
A wide range of providers continued to offer in-person appointments and home visits (see Figure 2). Despite continuing in-person patient care, some participants (49%) reported difficulties securing access to an adequate supply of PPE for their team. For those respondents indicating difficulties securing PPE, solutions identified by participants included relying on donations (78%), implementing strict protocols including locking up PPE (28%) supplies, self-procuring at big-box stores (28%) and reusing PPE (10%). Organizational changes that accommodated in-person care included the following: modified physical environment, reduced overlaps of in-person patients to promote social distancing, and newly implemented preventative protocols to reduce the risk of transmission of COVID-19 infection according to local public health recommendations (see Table 1).
| TABLE 1. Themes and illustrative quotes representative of qualitative data collected from open-text boxes | |
| Themes | Illustrative quotes |
| 1. Organizational changes that accommodated in-person care | |
| Regular screening | "Clinic includes an initial phone/video consult[ation] before any in-person visit is completed." |
| Minimizing patient overlap | "We stagger [appointments] and have 10 minutes between each booked in-person appointment to allow time for disinfecting procedures." "If there is a specific appointment time [in the clinic], do not come early … Only [the] patient and, if necessary, a caregiver [should come]. Appointments are spaced one half-hour apart and the room is sanitized after every patient [leaves]." |
| Desk barriers at reception | "Reception[ists] wear medical-grade masks and sit behind a plexiglass barrier." |
| Escorting patients | "Patients ring [the] door bell to enter the building and the clinician meets them." |
| On-site screening | "Patients are screened at the door and brought into an exam room right away." |
| Disinfection protocols | "[We have] established [a] sign system to confirm [that the] room has been disinfected. [The p]rovider disinfects [the] room after [the] patient leaves." "Longer time [has been allocated] between appointments for cleaning." |
| Use of PPE | "… every patient wears a mask in the clinic …" "… [Regarding] PPE worn by providers in clinic, [there have been] changes over the [past] 4 months, with [providers] currently wearing face masks and shields …" |
| Waiting room modifications | "Wait room has been changed and limited seating is available. Because the space is shared, if too many patients arrive, patients are required to wait in their vehicle or outside." |
| Reducing the number of people in the clinic | "… only the patient attends the appointment unless a support person is required. Only one parent attends [the] well-baby visits or children's appointment." |
| Staff reallocation for distancing | "[We are] relocating staff to other workstations to maintain distancing." |
| Signs | "[There are] passive screening signs on the door. Sign require[s] face covering for entry…" |
| 2. Providers' experiences of rapid shift to virtual care during the first wave of COVID-19 | |
Challenges
|
"[It was] gradual. [It] took time initially to set up parameters that providers/patients were comfortable with, but now [they] are using [them] well." "Initially [it] was a bit rocky with some providers needing more technical support and guidance with regard to how to provide care through a virtual platform. Now it is pretty smooth …" "Initially [it was] difficult because of the change of practice yet two-thirds of the physicians enjoy it …" "…Change came rapidly and it also brought in lots of uncertainty at a heightened time of being scary [of] providing care to anyone …" |
Facilitators
|
"We had already completed all the security assessments and requirements for OTN so providers could switch over in 2 days …" "[We] appreciated being able to continue offering care and staying safe during the pandemic; overall, [we] found new ways to deliver care programs and services …" "It is all about the board and management communicating and coordinating change management with the clinical staff. It was important to have transparent, open and candid discussions – sharing ideas about balancing staff safety, patient health, operational effectiveness and government directives …" "At first there was resistance from the physicians due to financial reasons. Once that was confirmed the physicians embraced this new form of care." |
| 3. Anticipated future of virtual care following the COVID-19 pandemic | |
| Virtual care that will continue for some patients and some types of appointments | "Virtual care will be beneficial to people who struggle to get into the office." "Patients are loving virtual care. They are able to stop their own work for 15 mins, consult with their provider and then get right back to work. This is opposed what might be [over] 1.5 hrs to get to the clinic, wait for their appointment and commute home." "I foresee virtual care being an integral part of our process for patient care." "I think that some appointments that can be managed virtually should continue." "Our mental health patients also are really enjoying virtual visits. I can see this continuing in the future." "Due to connectivity shortages in our geography and elderly population that don't feel comfortable with technology, a good portion of our contacts will remain [on] phone." |
| Virtual care that will change practice | "With an expected long-term transition to virtual care for over 70% of our patient appointments, there will be a reduced demand for physical space and consequential large rental costs." "I do not see virtual care impacting in-person visits in the long-run. However, I do see [a] major opportunity for collaborative visits for virtual care." |
| Virtual care that will be dependent on provider preferences | "I see the use of virtual care being primarily dictated by the MD preferences. FHT staff are interested in virtual care, but some MDs are and some are not." |
| Advancements in virtual care that will require a continuation of physician billing codes | "If the billing codes remain then I'm sure the virtual means of providing primary care will continue." "Critical to the continuation of virtual care is the retaining of billing codes for this type of care." |
| MD = medical doctor; OTN = Ontario Telemedicine Network; PPE = personal protective equipment. | |
New patient-care activities
During the first wave of the COVID-19 pandemic, some participants (29%) indicated that their clinic site was carrying out COVID-19 testing, while the majority (71%) were not offering direct testing. The vast majority of participants (90%) indicated that a range of healthcare professionals within the team conducted wellness checks by proactively telephoning patients, which was a new activity initiated by FHTs during the first wave of the pandemic (Figure 2). Wellness checks meant that FHTs initiated telephone calls with their patients who were elderly, were postpartum and/or had a history of complex health and/or mental health issues to ensure that they had adequate medication, groceries and/or social supports.
Implementation of virtual care
There was a dramatic change in the modalities used to provide direct patient care immediately following the provincial declaration of emergency on March 17, 2020 (Government of Ontario 2020). Before the COVID-19 pandemic, in-person appointments were the most frequent mechanism for patient care, whereas during the first wave, telephone appointments became the most frequently used modality to provide patient care, followed by video and in-person appointments (Figure 3).
Participants described the challenges and facilitators that they encountered during the rapid shift to virtual care during the first wave of the pandemic. Challenges included infrastructure and technology, a rapid transition process and a lack of education and training. Facilitators included providers' preferences, previous experience and exposure to technology, flexibility and openness, a change management process and billing codes for virtual care (Table 1).
For video appointments with patients, Ontario Telemedicine Network (OTN) was the most frequently used platform (72%) followed by Zoom (56%), Telus Practice Solutions (40%) and Doxy (22%), as well as a range of other platforms (28%) (https://doxy.me/en/; https://otn.ca/; https://www.telus.com/en/health/health-professionals/clinics/emr-add-ons/virtual-visit; https://zoom.us/). Most participants (52%) indicated that their practice site offered virtual group sessions to patients for various topics: mental health, diet and nutrition, parenting and infant care, mindfulness, lifestyle and exercise, COVID-19, smoking cessation and caregiver support. Some respondents (10%) indicated that although their primary care clinic did not offer virtual groups during the first wave of the pandemic, they were planning to incorporate them in the near future. The most common video platform used for group programming was Zoom (81%). Participants reported that a combination of in-person, telephone and video appointments would continue following the pandemic (Figure 4).
We identified four themes in the qualitative data related to the future of virtual care: i) virtual care will continue for some patients and for some types of appointments; ii) virtual care will change practice; iii) virtual care is dependent on provider preferences; and iv) the advancements in virtual care requires continuation of physician billing codes (Table 1).
Collaboration and partnerships
During the first wave of the COVID-19 pandemic, most participants (67%) indicated that their primary care team continued team meetings. Telephone (70%) was the most frequently used modality to facilitate team-based conferencing. The next most frequent methods were the video platforms Zoom (54%) and OTN (32%), followed by video platforms embedded in the practices' electronic medical record (EMR; 9%). Asynchronous methods used by primary care teams for case conferencing including secure e-mail (16%) and messaging (10%).
Collaboration and partnerships extended beyond the immediate clinic's practice. Many (55%) indicated that their interprofessional team provided care to patients of physicians in their community who were not directly a member of their clinic's practice. In addition, most participants (65%) reported that someone from their primary care team was directly involved in a regional COVID-19 planning and leadership implementation table. Lastly, some providers in primary care held multiple roles in their community. For example, many participants (49%) reported that at least one member of their team was working in a high-priority area outside of the direct primary care clinic, including COVID-19 assessment centres (73%), long-term care facilities (33%), acute care hospitals (20%), as well as other congregate type settings (i.e., group homes, retirement facilities; 31%).
Discussion
Reports on the rapid transitions occurring in primary care during the first wave of the pandemic have focused on the implementation of virtual care (Alex et al. 2020; Rawaf et al. 2020). Little is known about how primary care teams shifted toward virtual care or how in-person patient care continued during that period (Bhatti et al. 2020). Our study demonstrates that primary care physicians and other members of the team continued providing some in-person preventative, medical and mental healthcare services to their patients. Some in-person patient care continued at all of our participants' primary care organizations except one. To do so, primary care teams redesigned workplaces and implemented new safety measures to comply with physical distancing and for prevention and control of the spread of COVID-19. A problem faced by our participants, similar to challenges faced worldwide, was the availability of PPE (Culpepper 2021; Rawaf et al. 2020). According to Rawaf et al. (2020), "some family physicians have withdrawn their services because of the lack of adequate PPE" (p. 131). In the US, the lack of PPE led to the closure of some primary care offices (Culpepper 2021). As the pandemic continues, ensuring adequate availability of PPE is essential for the safety of patients and providers in primary care.
The COVID-19 pandemic has stimulated innovation within primary care with the implementation of new technologies for the delivery of patient care (Dearing and Cox 2018; Schiavo 2015). Participants in our study described an astoundingly rapid implementation of virtual care following the Ontario declaration of emergency for COVID-19. In the US, there are reports of practice closures because of the many technological and administrative challenges associated with this dramatic shift (Gausvik and Jabbarpour 2021). Although some key foundations for virtual care are now in place, further capacity building is needed for ongoing durability and scale (Dearing and Cox 2018; Schiavo 2015) – for example, determining the optimal roles for future inclusion of synchronous (i.e., telephone and video appointments) and asynchronous (i.e., direct messaging) virtual care in direct patient care activities and team collaborations to complement in-patient care.
Key facilitators identified in our study that helped FHTs transition to virtual care included providers' previous exposure to using technology, providers' flexibility and openness to using virtual technology and organizational change management. Key barriers identified in our study that created challenges to implementing virtual care included the lack of infrastructure and technology in primary care organizations, as well as the lack of provider education and training in using virtual modalities to deliver patient care. The sustainability of virtual care requires educators to integrate virtual competencies and training into healthcare education programs. Team-based practices require appropriate technology, adequate training and structural supports from policy and decision makers.
Our study demonstrated the level of coordination undertaken by primary care teams with the new implementation of wellness checks. Wellness checks meant that primary care teams were able to generate lists of patients they considered vulnerable using their EMR system and proactively make contact with each of these patients. This level of coordination is possible because of the continuous relationships that primary care has with patients. Wellness checks served as real-time assessments, were a significant source of support for patients during the first wave of the pandemic and are only one example of primary care teams' contribution to population health early in the pandemic (Donnelly et al. 2021). However, it is not clear if primary care teams' rapid ability to coordinate, identify and reach distinct patient populations has been fully harnessed by public health during the pandemic (Crawley 2021; Marchildon 2021). One of the challenges for primary care teams is to find new ways to collaborate with one another in the context of physical distancing during the pandemic (Donnelly et al. 2021). Team collaboration in primary care often relies on frequent and informal in-person encounters in an appropriate physical space (Goldman et al. 2010; Levesque et al. 2017; Morgan et al. 2020). Our study demonstrates that primary care teams were using a range of alternate modalities to stay engaged with one another early in the pandemic. A risk of virtual collaboration is that the frequency of team interactions may decrease while the formality of interactions may increase (Morgan et al. 2020). It is crucial to ensure that primary care teams maintain their ability to interact with one another despite the challenges presented in virtual care, especially given the significant investments made in the recent past to establish primary care teams in Ontario and elsewhere (Hutchison et al. 2011). Collaboration in teams is critical for supporting integrated care (Wagner et al. 2018). As virtual care continues, however, it may bring changes to the organizational structures in ways that can offer new opportunities for greater integration of social and community services in team-based settings. Virtual care modalities may present opportunities for creative collaboration across organizations and sectors, for even more comprehensive patient-centred care (Shaw et al. 2017).
Policy implications
The future of virtual care requires strong system leadership (Shaw et al. 2017). While there has been intense focus on acute care in the early phases of the pandemic, policy makers need to give greater attention to primary care teams because they are uniquely positioned to deliver preventative care, manage chronic diseases and respond to the overwhelming mental healthcare demands that have emerged during the COVID-19 pandemic (Ashcroft et al. 2021a; DeVoe and Bazemore 2021). Before the pandemic, wide differences existed across primary care organizations and models in Ontario (Rudoler et al. 2019). Early in the pandemic, there was a lack of coordinated change management strategies across primary care organizations that quickly adapted workplaces and delivery of care. Our study demonstrated some of the variations that existed early in the pandemic with different types of virtual platforms used to deliver patient care.
The health system context in which primary care operates is impacted by planned and unexpected change (Rudoler et al. 2019). The pandemic is an example of a catalyst resulting in unexpected change as with the implementation of virtual care. There are some early reports that virtual care has improved access to some types of care provided by primary care physicians and interprofessional teams during the COVID-19 pandemic (Donnelly et al. 2021; Gomez et al. 2021). In some cases, virtual care facilitated more timely access and allowed for innovative partnerships and collaboration by opening up even beyond the roster. Virtual care provides an opportunity for policy makers to consider innovative collaborations across the health and social sectors to best meet patients' care needs.
Patients need to be the focal point of decisions on the future developments of virtual care (Shaw et al. 2017). There are concerns that virtual care may be further disadvantaging vulnerable and complex patients and perpetuating digital inequity (Bhatti et al. 2020; Nouri et al. 2020). When asked about the anticipated future of virtual care, participants in our study expressed concerns that virtual care will continue for some patients, yet connectivity difficulties in certain geographical regions will create access barriers for other patients. Limited access to stable high-speed internet may disadvantage patients residing in rural and remote communities (Baylak et al. 2020; Lints-Martindale et al. 2018). Despite some improvements over the past decade (Jong et al. 2019), commitment by policy makers to ensure equitable access to consistent high-speed internet access in rural and remote geographical regions is needed to sustain virtual care (Baylak et al. 2020; Lints-Martindale et al. 2018). Moreover, protocols and guidelines developed in the primary care team context can help shape the future of virtual care so that the delivery of care aligns with patients' care needs. In addition, establishing competencies and best practices for virtual care can help guide educators in preparing future primary care providers for this new context. For example, providers and leaders in primary care need guidance on privacy and confidentiality concerns unique to virtual care (Bassan 2020; Hall and McGraw 2014).
The sustainability of virtual care is dependent on adequate incentive systems. Participants in our study emphasized the need for physician billing codes as one key facilitator for sustainable virtual care. In Canada, provincial and territorial governments quickly adapted physician fee schedules to support virtual care services during the COVID-19 pandemic (CIHI 2021). Currently, physician billing codes that support virtual care in Ontario have been extended to September 2022 (Government of Ontario 2020). Leveraging incentives to drive long-term use of virtual care in a meaningful way (Shaw et al. 2017) requires policy and decision makers to determine the goals for virtual care for these team settings. For example, as corporate virtual "walk-in" clinics are growing momentum (Hardcastle and Ogbogu 2020), policy and decision makers can use incentives to take a stance supporting comprehensive patient-centred primary care. In addition, Shaw et al. (2017) recommended using outcome-based payment models to drive patient-centred virtual care in teams. The development of incentive systems for virtual care also needs to account for the interprofessional primary care team context. For example, incentives can shape collaborative care activities when provider remuneration is entwined with team funding models and team activities (Wranik et al. 2017). Incentive schemes inappropriately designed for their context – in this case, a collaborative team context – can create disincentives to the provision of certain types of care, increase costs and affect quality of care (McDonald et al. 2009; Scott et al. 2011; Wranik et al. 2017). In addition, policy makers are encouraged to design incentive schemes that maximize virtual care's potential to harness innovative cross-sector partnerships and promote interprofessional collaboration.
By engaging primary care providers and patients, policy and decision makers can learn valuable information from their experiences since the onset of the pandemic that can inform future decisions for the durability and scaling up of virtual care. Planning for the future of virtual care in a coordinated way is essential and needs to consider the type of virtual care modalities that work best for patients and providers, as well as the type of care best suited for virtual care. Primary care brings the needed systemic understanding to health policy planning activities given the multiple cross-sector roles held by providers. The challenge, however, is that many primary care providers may not have the capacity to engage with policy makers because of lack of resources for such time-intensive consultation work (Rudoler et al. 2019), particularly during such an intensive time as the pandemic.
Limitations
We conducted this study with primary care teams in Ontario, which are not reflective of all primary care models in other jurisdictions. Our survey was conducted in the first wave of the COVID-19 pandemic, and it is anticipated that the experiences and innovations in primary care will continue to evolve. The surveys were completed by one organizational representative and may not reflect the experiences of all of the providers on the team. Ongoing research is needed to examine the total impact of the pandemic on team-based primary care.
Conclusion
Primary care has continued to play an important role during the pandemic. Providers are responding rapidly to the evolving impact of the pandemic to ensure patients are able to access services in various ways. There is no doubt that the delivery of primary care will be changed, and data from these early studies offer critical insights to shape the optimal use of a variety of both virtual and in-person care services throughout this pandemic and beyond.
La prestation des soins aux patients dans les équipes Santé familiale de l'Ontario pendant la première vague de la pandémie de COVID-19
Résumé
Objectif: L'objectif de cet article était d'identifier la continuation et les changements dans les méthodes de prestation de soins au sein des équipes de soins primaires pendant la pandémie de COVID-19.
Conception: L'étude a consisté en une enquête transversale en ligne comprenant des questions fermées et ouvertes.
Milieu: Le milieu concerné comprenait des équipes Santé familiale (ESF) en Ontario, au Canada.
Participants: Les participants comprenaient des directeurs administratifs d'ESF ou les personnes désignées de leur choix.
Enquête: Les statistiques descriptives ont été dérivées à partir des réponses aux questions fermées, et les réponses aux questions ouvertes ont été codées à l'aide d'une analyse thématique.
Résultats: Avec 93 participants, le taux de réponse était de 48%. Les participants ont fait état de la continuation des soins en personne, de la mise en œuvre des soins virtuels dans les ESF et de la collaboration au sein des équipes et de leurs communautés.
About the Author(s)
Rachelle Ashcroft, PhD, Assistant Professor, Factor-Inwentash Faculty of Social Work, University of Toronto, Toronto, ON
Catherine Donnelly, PhD, Associate Professor, Faculty of Health Sciences, Queen's University, Kingston, ON
Sandeep Gill, MSc, Quality and Knowledge Translation Manager, Association of Family Health Teams of Ontario, Toronto, ON
Maya Dancey, BSc, MSc, Research Intern, Telfer School of Management, University of Ottawa, Ottawa, ON
Simon Lam, MSW, Research Associate, Factor-Inwentash Faculty of Social Work, University of Toronto, Toronto, ON
Allan K. Grill, MD, Associate Professor, Department of Family & Community Medicine, University of Toronto, Toronto, ON, Lead Physician, Markham Family Health Team, Chief, Department of Family Medicine, Markham Stouffville Hospital, Markham, ON
Kavita Mehta, MBA, Chief Executive Officer, Association of Family Health Teams of Ontario, Toronto, ON
Correspondence may be directed to: Rachelle Ashcroft, Factor-Inwentash Faculty of Social Work, University of Toronto, 246 Bloor Street West, Toronto, ON M5S 1V4. She can be reached by phone at 416 978 6314 or by e-mail at rachelle.ashcroft@utoronto.ca
References
Alex, K.H., J.E. DeVoe, A. Cheng, T. Ehrlich and S. Jones. 2020. Redesigning Primary Care to Address the COVID-19 Pandemic in the Midst of the Pandemic. Annals of Family Medicine 18(4): 349–54. doi:10.1370/afm.2557.
Ashcroft, R., C. Donnelly, M. Dancey, S. Gill, S. Lam, T. Kourgiantakis et al. 2021a. Primary Care Teams' Experiences of Delivering Mental Health Care during the Covid-19 Pandemic: A Qualitative Study. BMC Family Practice 22: 143. doi:10.1186/s12875-021-01496-8.
Ashcroft, R., M. Menear, J. Silveira, S. Dahrouge, M. Emode, J. Booton, and K. McKenzie. 2021b. Inequities in the Delivery of Mental Health Care: A Grounded Theory Study of the Policy Context of Primary Care. International Journal for Equity in Health 20: 144. doi:10.1186/s12939-021-01492-5.
Bassan, S. 2020. Data Privacy Considerations for Telehealth Consumers amid COVID-19. Journal of Law and the Biosciences 7(1): 1–12. doi:10.1093/jlb/lsaa075.
Baylak, A., N. Dublin, C. Eastwood, S. Gill, J. Lee, R. Mattu et al. 2020. Telehealth in Rural Canada: Emergent Technologies to Address Historical Issues. Canadian Journal of Nursing Informatics 15(2).
Beaulieu, M.D., J. Haggerty, P. Tousignant, J. Barnsley, W. Hogg, R. Geneau et al. 2013. Characteristics of Primary Care Practices Associated with High Quality of Care. CMAJ 185(12): E590–96. doi:10.1503/ cmaj.121802.
Bhatti, S., E. Commisso and J. Rayner. 2020. A Rapid Primary Healthcare Response to COVID-19: An Approach to Care Ensuring that No One Is Left Behind. Healthcare Quarterly 23(3): 29–33. doi:10.12927/hcq.2020.26336.
Braun, V. and V. Clarke. 2006. Using Thematic Analysis in Psychology. Qualitative Research in Psychology 3(2): 77–101. doi:10.1191/1478088706qp063oa.
Brown, J.B. and B.L. Ryan. 2018. Processes that Influence the Evolution of Family Health Teams. Canadian Family Physician 64(6): e283–89.
Canadian Institute for Health Information (CIHI). 2021. Physician Billing Codes in Response to COVID-19. Retrieved February 24, 2021. <https://www.cihi.ca/en/physician-billing-codes-in-response-to-covid-19>.
The College of Family Physicians of Canada (CFPC). 2019. Summary of a New Vision for Canada: Family Practice – the Patient's Medical Home 2019. Retrieved October 15, 2021. <https://patientsmedicalhome.ca/files/uploads/PMH2019Summary_ENG.pdf>.
Collins, P.A., S.J. Resendes and J.R. Dunn. 2014. The Untold Story: Examining Ontario's Community Health Centres' Initiatives to Address Upstream Determinants of Health. Healthcare Policy 10(1): 14–29. doi:10.12927/hcpol.2014.23977.
Crawley, M. 2021. Ontario Hopes Family Doctors Can Reach Those Unvaccinated against COVID-19. CBC News. Retrieved October 25, 2021. <https://www.cbc.ca/news/canada/toronto/ontario-covid-vaccine-family-doctors-1.6093059>.
Culpepper, G. 2021. Protecting Family Medicine by Changing the Reimbursement Model Post-COVID-19. Journal of the American Board of Family Medicine 34: S10–12. doi:10.3122/jabfm.2021.S1.200628.
Dearing, J. and J. Cox. 2018. Diffusion of Innovations Theory, Principles, and Practice. Health Affairs 37(2):183–90. doi:10.1377/hlthaff.2017.1104.
DeVoe, J. and A. Bazemore. 2021. Primary Care in the COVID-19 Pandemic: Essential, and Inspiring. Journal of the American Board of Family Medicine 34: S1–S6. doi:10.3122/jabfm.2021.S1.200631.
Donnelly, C., R. Ashcroft, N. Bobbette, S. Gill, C. Mills, A. Mofina et al. 2021. Interprofessional Primary Care during COVID-19: The Provider Perspective. BMC Family Practice 22(1): 31. doi:10.1186/s12875-020-01366-9.
Gausvik, C. and Y. Jabbarpour. 2021. COVID-19 Timeline: Centres for Medical and Medicaid Services (CMS) Changes and Primary Care Support Were Not Enough to Prevent Practice Losses. Journal of the American Board of Family Medicine 34: S7–S9. doi:10.3122/jabfm.2021.S1.200305.
Glazier, R.H., B. Hutchison and A. Kopp. 2015, November. Comparison of Family Health Teams to Other Ontario Primary Care Models, 2004/05 to 2011/12. ICES. Retrieved October 16, 2021. <https://www.ices.on.ca/Publications/Atlases-and-Reports/2015/Comparison-of-Family-Health-Teams>.
Glazier, R.H., B.M. Zagorski and J. Rayner. 2012, March. Comparison of Primary Care Models in Ontario by Demographics, Case Mix and Emergency Department Use, 2008/09 to 2009/10. ICES. Retrieved October 16, 2021. <https://www.ices.on.ca/Publications/Atlases-and-Reports/2012/Comparison-of-Primary-Care-Models>.
Gocan, S., M.A. Laplante and K. Woodend. 2014. Interprofessional Collaboration in Ontario's Family Health Teams: A Review of the Literature. Journal of Research in Interprofessional Practice and Education 3(3): 1–19. doi:10.22230/jripe.2014v3n3a131.
Goldman, J., J. Meuser, J. Rogers, L. Lawrie and S. Reeves. 2010. Interprofessional Collaboration in Family Health Teams: An Ontario-Based Study. Canadian Family Physician 56(10): e368–74.
Gomez, T., Y.B. Anaya, K.J. Shih and D.M. Tarn. 2021. A Qualitative Study of Primary Care Physicians' Experiences with Telemedicine during COVID-19. Journal of the American Board of Family Medicine 34: S61–S70. doi:10.3122/jabfm.2021.S1.200517.
Government of Ontario. 2018, February 14. Ontario Investments in Indigenous Health and Wellness [News release]. Retrieved October 16, 2021. <https://news.ontario.ca/en/backgrounder/48195/ontario-investments-in-indigenous-health-and-wellness>.
Government of Ontario. 2019a, November 13. Ontario Expanding Digital and Virtual Health Care: Giving Patients More Options Part of Province's Plan to End Hallway Health Care [News release]. Retrieved October 16, 2021. <https://news.ontario.ca/mohltc/en/2019/11/ontario-expanding-digital-and-virtual-health-care.html>.
Government of Ontario. 2019b, November 13. Ontario Taking Next Steps to Integrate Health Care System: Changes Will Protect Uninterrupted Access to Patient Care [News release]. Retrieved October 16, 2021. <https://news.ontario.ca/en/release/54585/ontario-taking-next-steps-to-integrate-health-care-system>.
Government of Ontario. 2020, March 17. Ontario Enacts Declaration of Emergency to Protect the Public [News release]. Retrieved October 16, 2021. <https://news.ontario.ca/en/release/56356/ontario-enacts-declaration-of-emergency-to-protect-the-public>.
Hall, J.L. and D. McGraw. 2014. For Telehealth to Succeed, Privacy and Security Risks Must be Identified and Addressed. Health Affairs 33(2): 216–21. doi:10.1377/hlthaff.2013.0997.
Hardcastle, L. and U. Ogbogu. 2020. Virtual Care: Enhancing Access or Harming Care? Healthcare Management Forum 33(6): 288–92. doi:10.1177/0840470420938818.
Hastings, J.E.F. 1972. The Community Health Centre in Canada. Information Canada.
Haydt, S.M. 2018. Politics and Professions: Interdisciplinary Team Models and Their Implications for Health Equity in Ontario. International Journal of Health Services 48(2): 302–327. doi:10.1177/0020731417717384.
Heale, R., S. James, E. Wenghofer and M.-L. Garceau. 2018. Nurse Practitioner's Perceptions of the Impact of the Nurse Practitioner-Led Clinic Model on the Quality of Care of Complex Patients. Primary Health Care Research & Development 19(6): 553–60. doi:10.1017/S1463423617000913.
Holmes, E.A., R.C. O'Connor, V.H. Perry, I. Tracey, S. Wessely, L. Arseneault et al. 2020. Multidisciplinary Research Priorities for the COVID-19 Pandemic: A Call for Action for Mental Health Science. Lancet Psychiatry 7(6): 547–60. doi:10.1016/S2215-0366(20)30168-1.
Hutchison, B., J.-F. Levesque, E. Strumpf and N. Coyle. 2011. Primary Health Care in Canada: Systems in Motion. Milbank Quarterly 89(2): 256–88. doi:10.1111/j.1468-0009.2011.00628.
Hutchison, B. and R. Glazier. 2013. Ontario's Primary Care Reforms Have Transformed the Local Care Landscape, but a Plan Is Needed for Ongoing Improvement. Health Affairs 32(4): 695–703. doi:10.1377/hlthaff.2012.1087.
Jamieson, T., R. Wallace, K. Armstrong, P. Agarwal, B. Griffin, I. Wong et al. 2015, June 11. Virtual Care: A Framework for a Patient-Centric System. Women's College Hospital Institute for Health Systems Solutions and Virtual Care. Retrieved October 16, 2021. <https://www.womenscollegehospital.ca/assets/pdf/wihv/WIHV_VirtualHealthSymposium.pdf>.
Jong, M., I. Mendez and R. Jong. 2019. Enhancing Access to Care in Northern Rural Communities via Telehealth. International Journal of Circumpolar Health 78(2): 1554174. doi: 10.1080/22423982.2018.1554174.
Kearon, J. and C. Risdon. 2020. The Role of Primary Care in a Pandemic: Reflections during the COVID-19 Pandemic in Canada. Journal of Primary Care & Community Health 11: 2150132720962871. doi:10.1177/2150132720962871.
Khan, A.I., J. Barnsley, J.K. Harris and W.P. Wodchis. 2021. Examining the Extent and Factors Associated with Interprofessional Teamwork in Primary Care Settings. Journal of Interprofessional Care. doi:10.1080/13561820.2021.1874896.
Krelle, H., J.A. Dodson and L. Horwitz. 2020. Virtual Primary Care—Is Its Expansion Due to COVID-19 All Upside? JAMA Health Forum 1(7): e200900. doi:10.1001/jamahealthforum.2020.0900.
Levesque, J.F., M.F. Harris, C. Scott, B. Crabtree, W. Miller, L.M. Halma et al. 2017. Dimensions and Intensity of Inter-Professional Teamwork in Primary Care: Evidence from Five International Jurisdictions. Family Practice 35(3): 285–94. doi:10.1093/fampra/cmx103.
Lewnard, J.A. and N.C. Lo. 2020. Scientific and Ethical Basis for Social-Distancing Interventions against COVID-19. Lancet Infectious Diseases 20(6): 631–33. doi:10.1016/S1473-3099(20)30190-0.
Lints-Martindale, A.C., A.A. Carlson, S.L. Goodwin and S.N. Thompson. 2018. Putting Recommendations into Practice: Improving Psychological Services in Rural and Northern Canada. Canadian Psychology 59(4): 323–31. doi:10.1037/cap0000158.
Ly, O., D. Price, R. Saskin and M. Howard. 2021. Low-Acuity Emergency Department Use among Patients in Different Primary Care Models in Hamilton and Ontario. Healthcare Management Forum 34(4): 234–39. doi:10.1177/08404704211012027.
Manns, B.J., M. Tonelli, J. Zhang, D.J.T. Campbell, P. Sargious, B. Ayyalasomayajula et al. 2012. Enrolment in Primary Care Networks: Impact on Outcomes and Processes of Care for Patients with Diabetes. CMAJ 184(2): E144–52. doi:10.1503/cmaj.110755.
Marchildon, G.P. 2021. The Rollout of the COVID-19 Vaccination: What Can Canada Learn from Israel? Israel Journal of Health Policy Research 10: 12. doi:10.1186/s13584-021-00449-x.
McDonald, R., J. White, and T.R. Marmor. 2009. Paying for Performance in Primary Medical Care Learning about and Learning from "Success" and "Failure" in England and California. Journal of Health Politics, Policy and Law 34(5): 747–76.
Morgan, S., S. Pullon, E. McKinlay, S. Garrett, J. Kennedy and B. Watson. 2020. Collaborative Care in Primary Care: The Influence of Practice Interior Architecture on Informal Face-to-Face Communication – An Observational Study. Health Environments Research & Design Journal 14(1): 190–209. doi:10.1177/1937586720939665.
Mulvale, G.M., U. Danner and D. Pasic. 2009. Advancing Community-Based Collaborative Mental Health Care through Interdisciplinary Family Health Teams in Ontario. Canadian Journal of Community Mental Health 27(2): 55–73. doi:10.7870/cjcmh-2008-0018.
Nouri, S., E.C. Khoong, C.R. Lyles and L. Karliner. 2020. Addressing Equity in Telemedicine for Chronic Disease Management during the COVID-19 Pandemic. NEJM Catalyst. doi:10.1056/CAT.20.0123.
Rawaf, S., L.N. Allen, F.L. Stigler, D. Kringos, H.Q. Yamamoto, C. van Weel et al. 2020. Lessons on the COVID-19 Pandemic, for and by Primary Care Professionals Worldwide. European Journal of General Practice 26(1): 129–33. doi:10.1080/13814788.2020.1820479.
Rudoler, D., A. Peckham, A. Grudniewicz and G. Marchildon. 2019. Coordinating Primary Care Services: A Case of Policy Layering. Health Policy 123(2): 215–21. doi:10.1016/j.healthpol.2018.12.002.
Schiavo, R. 2015. Social Innovation as a Key Imperative in Global Health. Journal of Communication in Healthcare 8(2): 87–90. doi:10.1179/1753806815Z.000000000117.
Scott, A., P. Sivey, D. Ait Ouakrim, L. Willenberg, L. Naccarella, J. Furler and D. Young. 2011. The Effect of Financial Incentives on the Quality of Health Care Provided by Primary Care Physician. Cochrane Database of Systematic Reviews 9: CD008451. doi:10.1002/14651858.CD008451.pub2.
Shaw, J., T. Jamieson, P. Agarwal, B. Griffin, I. Wong and R.S Bhatia. 2017. Virtual Care Policy Recommendations for Patient-Centred Primary Care: Findings of a Consensus Policy Dialogue Using a Nominal Group Technique. Journal of Telemedicine and Telecare 24(9): 608–15. doi:10.1177/1357633X17730444.
Somé, N.H., R.A. Devlin, N. Mehta, G.S. Zaric and S. Sarma. 2020. Team-Based Primary Care Practice and Physician's Services: Evidence from Family Health Teams in Ontario, Canada. Social Science & Medicine 264: 113310. doi:10.1016/j.socscimed.2020.113310.
Strumpf, E., M. Ammi, M. Diop, J. Fiset-Laniel and P. Tousignant. 2017. The Impact of Team-Based Primary Care on Health Care Services Utilization and Costs: Quebec's Family Medicine Groups. Journal of Health Economics 55: 76–94. doi:10.1016/j.jhealeco.2017.06.009.
Tadic, V., R. Ashcroft, J.B. Brown and S. Dahrouge. 2020. The Role of Social Workers in Interprofessional Primary Health Care Teams. Healthcare Policy 16(1): 27–42.
Wagner, E.H., L. LeRoy, J. Schaefer, M. Bailit, K. Coleman, C. Zhan and D. Meyers. 2018. How Do Innovative Primary Care Practices Achieve the Quadruple Aim? Journal of Ambulatory Care Management. 41(4): 288–97. doi:10.1097/jac.0000000000000249.
Wranik, W.D., S.M. Haydt, A. Katz, A.R. Levy, M. Korchagina, J.M. Edwards and I. Bower. 2017. Funding and Remuneration of Interdisciplinary Primary Care Teams in Canada: A Conceptual Framework and Application. BMC Health Services Research 17: 351. doi.org/10.1186/s12913-017-2290-4.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed