World Health & Population
Mental Health Symptoms among Rural-to-Urban Migrants in China: A Comparison with Their Urban and Rural Counterparts
Abstract
Objective: To examine the mental health symptoms among rural-to-urban migrants in China, in comparison with representative samples of their counterparts in the rural areas from where they emigrated and urban communities to which they immigrated.
Methods: A cross-sectional survey conducted in 2004-2005 in China. Both rural-to-urban migrants (n = 1006) and urban residents (n=1000) were recruited in Beijing; the rural resident sample (n=1020) was recruited from the eight provinces of origin for 75% of the migrant sample. Mental health symptoms were measured using the Symptom Checklist-90 (SCL-90).
Results: Both rural-to-urban migrants and rural residents scored higher than urban residents in all the SCL-90 global indices and subscales. The rural-to-urban migrants scored higher than rural residents on the SCL-90 Positive Symptom Distress Index and two subscales (depression and psychoticism). The difference remained significant after controlling for a number of key individual characteristics (age, gender, marital status, education, income and perceived general health) in the multivariate model.
Conclusions: The data in the current study demonstrate that rural-to-urban migrants suffer from lower mental health status than both urban residents in the immigrating communities and their rural counterparts in the emigrating communities. The data suggest a possible deteriorative effect of migratory experience on mental health status among rural-to-urban migrants in China and suggest an urgent need for etiological studies and for mental health promotion and prevention efforts among this growing population.
Introduction
The relationship between migration and health has been extensively explored in the global literature, but the data have been inconclusive. Some researchers have suggested that migration, particularly rural-to-urban migration, might result in improved physical and mental health because of increases in both income and healthcare access (De Jong et al. 2002). Previous studies also suggested that migrants might be healthier than non-migrants because of a selection process by which more healthy individuals tend to migrate (e.g., "healthy migrant syndrome") (Fuentes-Afflick et al. 1999; Muening and Fahs 2002; Razum et al. 2000; Signh and Siahpush 2001; Swerdlow 1991). In contrast, a substantial amount of global literature suggests that migration is associated with increased risk for poor mental and physical health (McKay et al. 2003). This increased risk may be related to contextual and psychosocial factors associated with migration experience or migratory lifestyle such as adjustment to the new socio-cultural environment, changes in traditions and lifestyles, economic transitions or barriers to access to local community services, including healthcare delivery. Previous research has also documented that the stigmatization encountered by migrants in their new destination causes anxiety that may contribute to mental and physical illnesses (Darmon and Khlat 2001; Li et al. 2006b; Pudaric et al. 2000).
In addition, the existing literature on the relationship between migration and health has largely been limited to migrants within North American and European countries and those seeking permanent resettlements, such as trans-culture or trans-country immigrants and war refugees (Darmon and Khlat 2001; Diaz et al. 2001; Pernice and Brook 1996; Pudaric et al. 2000). During the past decades, there have been massive internal migrations in many developing countries, including China. These internal migrations provide an excellent opportunity to study the relationship between migration and mental health. However, data are limited regarding the relationship between migration and health status among temporary, rural-to-urban migrants in many developing countries, including China, which is home to one fifth of the world's population.
Migration from rural to urban areas in China was restricted through the official household registration (hukou) system for almost a quarter century until economic reform took place in the late 1970s (Li et al. 2006a). Under the hukou system, each individual is officially registered as either a rural or an urban resident. Rural residents could not freely move to or settle in urban areas in order to become urban residents. With the introduction in 1979 of the Rural Household Contract Responsibility System, a form of rural economic reform, China experienced rapid growth in agricultural productivity (e.g., agricultural GDP increased from 2.7% in 1970-1978 to 7.1% in 1979-1984) and a subsequent surplus of rural labour (e.g., agriculture labourers as a percentage of the working population decreased from 81% in 1970 to 49% in 2000) (Anderson et al. 2003). Concurrently, rapid economic growth in urban China widened the income gap between the urban and rural areas to a historically high level in the 1990s (Anderson et al. 2003). Both the surplus of rural labour and the increasing urban-rural income disparity have provided strong motivation and incentives for rural residents to migrate to urban areas in search of employment opportunities and better lives. Consequently, millions of Chinese farmers have left their villages for cities, giving impetus to rural-to-urban migration, which has now become one of the largest internal migrations in China's recent history (Zhang 2001).
According to Chinese governmental statistics, there are approximately 114 million rural-to-urban migrants in China, accounting for 23.2% of total rural labour and 9% of the total population in China (China National Bureau of Statistics 2004). Rural-to-urban migrants are defined as individuals who moved from rural to urban areas for jobs (Li et al. 2006b). These migrants work or live in urban areas without official urban household registration. Because of legal restrictions on household registration, approximately 80% of the migrants do not permanently relocate (i.e., obtain official urban hukou) (Zhang 2001).
Limited data are available at present on the mental health status of rural-to-urban migrants in China. Shen and colleagues examined the mental health symptoms among 371 (166 men and 205 women) migrant workers in Shenzhen, China (Shen et al. 1998). They found that young migrant workers (mean age 22.90± 2.67 years) had poorer mental health status than their urban counterparts. Using data from qualitative interviews, Li and colleagues found that rural-to-urban migrants in cities demonstrated hostile behaviour and poor social adjustment (Li et al. 2006b). A cross-sectional survey among more than 4000 rural-to-urban migrants in China also revealed that increases in mobility were associated with elevated levels of substance use and increased depressive symptoms (Li et al. 2006b). While these few studies suggest that rural-to-urban migrants experience increased mental health symptoms in their urban destinations, the lack of appropriate comparison groups from non-migrant residents in either the emigrating or immigrating communities makes it difficult to draw decisive conclusions on the complex relationship between rural-to-urban migration and mental health symptoms.
Several recent studies among migrant workers in China with comparison groups from non-migrant urban and rural residents yielded a different result. By comparing 4453 migrant workers, 1957 urban workers and 1909 rural residents in western Zhejiang province in China, Hesketh and colleagues found that individuals in their migrant sample were not especially vulnerable to poorer mental health and other health risks (e.g., HIV and syphilis) than their urban and rural counterparts (Hesketh et al. 2008; Li et al. 2007). While these findings were inconsistent with previous studies that suggested a higher risk for mental health problems among migrants, the authors did warn that poor living condition and inadequate healthcare access might make migrants vulnerable to poor long-term health (Hesketh et al. 2006).
Given the rapid increase of the rural migrant population in China and the inconclusive findings in the literature on the relationship between rural migration and mental health, more research is needed to assess the impact of rural-to-urban migration on mental health symptoms in China and other developing countries. Therefore, the current study was designed to examine the mental health symptoms among rural-to-urban migrants, in comparison with representative samples of their counterparts in the rural emigrating and urban immigrating communities.
Methods
Sampling Procedures
Rural-to-urban migrant sample. The rural-to-urban migrant sample was recruited in Beijing, China. Beijing, the capital city of China, covers 16,808 square kilometres with a permanent population of 13 million. The Beijing municipal government has jurisdiction over four central urban districts, four near-suburban districts, eight outer-suburban districts and two counties. There were more than three million rural-to-urban migrants (69% men and 31% women) in Beijing in 2003 (Beijing Bureau of Statistics 2004). It was estimated that the majority (80%) were between 18 and 40 years of age (Beijing Bureau of Statistics 2004). Given the absence of other relevant sampling frames for the migrant population (e.g., household census data on migrants), we employed the occupational cluster-based "quota-sampling" scheme to ensure the representative nature of the migrant sample (Li et al. 2004; 2006a).
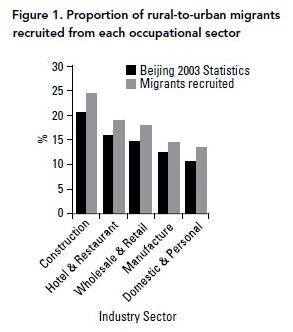
Based on 2003 government statistics of migrant employment, five occupational clusters employed 81.9% of the rural-to-urban migrants in Beijing (i.e., 22.8% in construction, 17.7% in hotel and restaurant, 16.2% in wholesale and retail, 13.6% in manufacturing and 11.6% in domestic service and other service sectors) (Beijing Bureau of Statistics 2004). These five occupational clusters were selected as the sampling frame for rural-to-urban migrants in the current study. The number of participants recruited in each cluster was approximately proportionate to the overall estimated distribution of migrants in the cluster (Figure 1). In addition to occupational clusters, the sampling was also stratified by gender to match the overall gender distribution of the migrant population in Beijing (i.e., 69% men and 31% women).
Migrants were eligible for participation in the study if they (1) came from rural areas; (2) worked in Beijing without obtaining a permanent Beijing residency; (3) had been in Beijing for at least 1 month; and (4) were between 18 and 40 years of age. The local research teams used workplaces (store, shop, club, office, factory and construction site) as the sampling units. Streets were used as the sampling units for migrants who did not have fixed workplaces (such as repairmen, street vendors). Because of the lack of relevant sampling frames for the migrant population, we employed several outreach strategies to identify the sampling units for the migrant sample. These strategies included direct contact (53% of the sampling units) and referral by local community or business leaders (47% of the sampling units).
Once a sampling unit was identified and selected according to the pre-established sampling scheme, employers (or managers) at the sampling unit were contacted for permission to conduct the survey on their premises. Upon receiving permission, the interviewers randomly approached available rural-to-urban migrants at the sampling unit and verified their eligibility for participation. This process was repeated until target numbers of sampling units or numbers of participants in each sampling stratum were reached. To prevent over-sampling of migrants from any single sampling unit, the number of migrants recruited from any unit was limited to 50 individuals. The final sample of 1006 rural-to-urban migrant workers was recruited from 34 sampling units. These sampling units, stratified by occupational cluster, were spread across 10 large geographic locations (e.g., metropolitan areas, business districts, major streets and suburban townships) in two central urban districts, two near-suburban districts and two outer-suburban districts/counties in Beijing.
Urban resident sample. The urban resident sample was recruited from the same geographic areas as the migrant sample. Urban residents were eligible to participate if they (1) were between 18 and 40 years of age and (2) lived in Beijing with permanent Beijing residence status. We recruited eligible urban residents from the same sampling units as rural-to-urban migrants if the sampling units employed both migrants and urban residents. For migrants recruited from some migrant-dominated occupational sectors (e.g., men in construction and women in domestic service and entertainment establishments), we recruited "matching" urban residents from other occupations that required similar levels of skills or education, at the same geographic locations. Similar proportions of urban residents and migrants were recruited from each of the 10 geographic locations in Beijing (Figure 2).
[Figure 2]
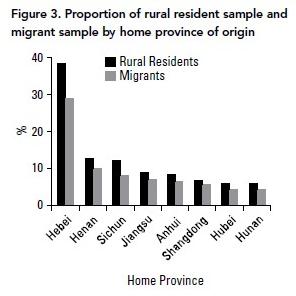
Rural resident sample. Rural residents were recruited using multiple-stage cluster sampling. Once individuals had been recruited for the migrant sample, their provinces of origin were tallied. While the migrant sample in the current study originated from 25 provinces across mainland China, 75% of the sample came from eight provinces (Hebei, Henan, Sichuan, Jiangsu, Anhui, Shangdong, Hubei and Hunan). These eight provinces were selected as the first sampling stratum for the rural residents. The proportion of rural residents recruited from each province was set to be approximately equal to that of the migrant sample that originated from the same province (Figure 3). The county within each province served as the second sampling stratum. A total of 34 counties were selected from these eight provinces (range from one to 11 counties per province, with an average of 4.25 counties per province). The rural village within each county served as the third sampling stratum. A total of 63 villages were selected from the 34 counties (range from one to four villages, with an average of 1.85 villages per county). Outreach strategies employed to identify counties/villages included referrals from local government or direct personal contacts with village leaders. Once permission was granted by the village leaders to conduct the survey in their areas, the research team randomly approached available residents in villages and verified their eligibility for participation. Rural residents were eligible to participate if they (1) lived in a rural area and had permanent rural residency; (2) had stayed in their home town for at least 1 month; and (3) were between 18 and 40 years of age. To prevent over-sampling of rural residents from any village, the number of rural residents recruited from any village was capped at 30.
Survey procedures
Once an eligible individual was identified in a sampling unit, trained interviewers (psychology graduate students and faculty members at a local university in Beijing) provided the individual with a detailed description of the study design and the consenting procedure and invited her or him to participate in the survey. Eligible individuals who declined to participate were enumerated and their gender was noted. Eligible individuals who agreed to participate and provided informed consents were asked to complete a self-administered questionnaire developed through the joint efforts of investigators in both China and the United States. Similar questionnaires, with some sample-specific modifications (e.g., migration-related measures for the migrant sample), were developed for each of the three study samples (i.e., urban residents, rural-to-urban migrants and rural residents). Questionnaires were pilot-tested for comprehension among migrants in Beijing and typically took about 45 minutes to complete. Participants completed the survey individually or in a small group (three to five people) at workplaces, homes or other locations preferred by the participants. Trained interviewers provided assistance to a small number of rural-to-urban migrants and rural residents with limited literacy by reading survey items to them. Respondents were provided with a small monetary compensation for their participation. The study protocol was approved by the Institutional Review Boards at Wayne State University in the United States and Beijing Normal University in China.
Measures
Individual characteristics. All participants were asked to provide their age, ethnicity (Han versus non-Han), level of formal schooling and marital status. For the purpose of data analysis in the current study, the response to schooling question was grouped into three categories: no more than middle school (i.e., 9 years of compulsory education in China), high school (10-12 years of schooling) and post-secondary education (more than 12 years of schooling). Marital status was grouped into "never married" or "married." The latter category included 1.7% of the participants who were currently either divorced or widowed. Participants were asked to self-rate their overall health status on a 5-point scale: very good, good, fair, poor and very poor. For the purpose of data analysis in the current study, the response was grouped into three categories: good, fair and poor. All participants were asked about their average monthly income (in Chinese currency, yuan). The rural sample and some migrants who did not receive salary or payment on a monthly basis were instructed to divide their total annual income by 12 as an approximation of their monthly income.
Mental health symptoms. Participants' mental health symptoms during the most recent 7 days were measured with the Symptom Checklist-90 (SCL-90) (Derogatis et al. 1973). The SCL-90 is a multidimensional self-report inventory designed to screen for a broad range of psychological problems and symptoms of psychopathology. The SCL-90 has nine primary symptom dimensions (somatization, obsessive-compulsive, interpersonal sensitivity, depression, anxiety, hostility, phobic anxiety, paranoid ideation and psychoticism) and three global indices, including the global severity index (the measure of overall psychological distress), positive symptom distress index (the measure of intensity of symptoms) and positive symptom total (the number of self-reported symptoms). The scale, originally developed for assessing the symptomatic behaviour of psychiatric outpatients, has been used with a variety of populations, from the non-patient "normal" population to medical patients or individuals with psychiatric disorders, and has been translated into numerous languages including Chinese (Derogatis et al. 1973; Wang 1993). Within the Chinese population, the SCL-90 has been used to assess mental health symptoms or trauma symptoms among community samples, nurses, women undergoing an early abortion, adolescents, patients with functional dyspepsia, unemployed workers and migrant workers (Hu et al. 1997; Jiang et al. 2000; Luo et al. 1996; Shen et al. 1998; Wang et al. 2000; Wu et al. 2001; Xia and Qian 2001). Based on results of our pilot testing (e.g., infrequency of "extreme" response), the response option of SCL-90 was modified from the original 5 points (0 to 4) to 4 points (0 to 3). The internal consistency estimates (Cronbach alpha) of the 10 subscales ranged from .74 to .88 for the entire sample, .75 to .88 for the urban sample, .70 to .87 for the migrant sample and .75 to .89 for the rural sample (Table 1).
| Table 1. Estimates of internal consistency (Cronbach alpha) of SCL-90 scales among three Chinese samples | |||||
| Sample | |||||
| Overall | Urban | Migrant | Rural | ||
| Somatization | 12 | .88 | .88 | .86 | .89 |
| Obsessive-Compulsive | 10 | .82 | .84 | .81 | .81 |
| Interpersonal sensitivity | 9 | .81 | .83 | .79 | .79 |
| Depression | 13 | .88 | .88 | .87 | .88 |
| Anxiety | 10 | .85 | .86 | .83 | .85 |
| Hostility | 6 | .79 | .80 | .78 | .80 |
| Phobic anxiety | 7 | .79 | .82 | .78 | .78 |
| Paranoid ideation | 6 | .75 | .79 | .70 | .75 |
| Psychsticism | 10 | .83 | .86 | .79 | .83 |
| Additional items | 7 | .74 | .75 | .71 | .75 |
| Full scale | 90 | .98 | .98 | .97 | .98 |
As shown in Table 2, the internal consistency estimates were consistent between gender (ranging from .76 to .88 for female and .72 to .88 for male) and across different levels of educational attainment (ranging from .72 to .88 for ≤ middle school, .74 to .88 for high school and .77 to .89 for post-secondary education).
| Table 2. Estimates of internal consistency (Cronbach alpha) of SCL-90 scales by gender and education attainment | |||||
| Gender | Education attainment | ||||
| Female | Male | = Middle school | High school | Post-secondary | |
| Somatization | .88 | .88 | .87 | .88 | .89 |
| Obsessive-compulsive | .83 | .82 | .81 | .82 | .84 |
| Interpersonal sensitivity | .82 | .80 | .78 | .81 | .84 |
| Depression | .88 | .88 | .88 | .88 | .88 |
| Anxiety | .86 | .84 | .84 | .85 | .86 |
| Hostility | .80 | .79 | .79 | .81 | .79 |
| Phobic anxiety | .79 | .80 | .78 | .79 | .83 |
| Paranoid ideation | .77 | .74 | .74 | .75 | .78 |
| Psychoticism | .83 | .83 | .81 | .83 | .85 |
| Additional items | .76 | .72 | .72 | .74 | .77 |
| Full scale | .98 | .98 | .97 | .98 | .98 |
Analysis
First, Chi-square (for categorical variables) or ANOVA (for continuous variables) was employed to examine the difference of individual characteristics among the three groups. Second, one-way ANOVA was performed to compare the group differences in the three SCL-90 global indices and 10 SCL-90 subscales. Post-hoc comparison was conducted using the least significance difference (LSD) criterion. Third, ANOVA or Pearson product moment correlation coefficients were employed to assess the association of mental health symptoms with key individual characteristics. Finally, the general linear model (GLM) was employed to simultaneously assess the group difference in all 10 SCL-90 subscales, controlling for key individual characteristics of the samples. Individual characteristics in the GLM model included gender, marital status, age, level of education, monthly income and perceived general health status. All statistical analyses were performed using SPSS for Windows Version 11.5.
Results
Individual Characteristics of Study Samples
Approximately, 1025 eligible participants were approached in each of the three target groups. Total participation rates were 97.6%, 98.4% and 99.3% for urban residents, rural-to-urban migrants and rural residents, respectively. Approximately equal numbers of men and women in each group refused to participate (i.e., 11 women and 14 men in the urban sample, six women and eight men in the migrant sample, and three women and four men in the rural sample). The final database contained 1000 urban residents, 1006 rural-to-urban migrants and 1020 rural residents.
As shown in Table 3, these three groups differed in a number of individual characteristics. The mean age was 25.39 years for the migrant sample, younger than either the urban (27.52 years) or rural samples (28.79 years). There were more women in the urban sample (48%) than either the migrant (33%) or rural samples (39%). The proportion of Han ethnicity was lower in the urban sample (90%) than either the migrant (96%) or rural samples (95%). The urban sample had more participants who had completed post-secondary education (51%) than the migrant (6%) or rural samples (6%). The proportion of participants who were never married was similar between the urban sample (59%) and the migrant sample (61%), but lower in the rural sample (30%). About 70% of the migrant and rural samples perceived that they had very good or good health, compared with 49% of the urban sample. The average monthly income was 1664 yuan (~ US 208 dollars at the time of survey), 980 yuan (~ US 122 dollars) and 604 yuan (~ US 75 dollars) for the urban, migrant and rural samples, respectively.
| Table 3. Individual characteristics of study sample | ||||
| Sample | ||||
| Overall | Urban | Migrant | Rural | |
| N (%) | 3026 (100%) | 1000 (33%) | 1006 (34%) | 1020 (33%) |
| Mean age in years (SD) | 27.24 (6.44) | 27.52 (6.28) | 25.39 (6.21) | 28.79 (6.38)* |
| Mean monthly income (SD)a | 1079 (972) | 1664 (1255) | 980 (703) | 604 (450)* |
| Gender b | ||||
| Woman | 1204 (40%) | 479 (48%) | 332 (33%) | 393 (39%) |
| Man | 1808 (60%) | 515 (52%) | 670 (67%) | 623 (61%) |
| Han ethnicity | 2832 (94%) | 896 (90%) | 968 (96%) | 968 (95%)* |
| Education b | ||||
| ≤ Middle school | 1528 (51%) | 74 (7%) | 721 (72%) | 733 (72%) |
| High school | 858 (29%) | 412 (41%) | 223 (22%) | 223 (22%) |
| Post-secondary education | 627 (21%) | 512 (51%) | 57 (6%) | 58 (6%) |
| Martial status b | ||||
| Single | 1502 (50%) | 587 (59%) | 612 (61%) | 303 (30%) |
| Ever married | 1506 (50%) | 409 (41%) | 386 (39%) | 711 (70%) |
| Perceived health b | ||||
| Good | 2007 (67%) | 589 (59%) | 716 (72%) | 702 (69%) |
| Fair | 869 (29%) | 352 (35%) | 243 (24%) | 274 (27%) |
| Poor | 135 (5%) | 57 (6%) | 41 (4%) | 37 (4%) |
| Measured in Chinese currency, yuan (8 yuan ≅ 1 US dollar at the time of survey). bDifference among groups was significant (p< .0001) * p<.0001. | ||||
Mental Health Symptoms
As shown in Table 4, there were significant differences in the three SCL-90 global indices, with both migrants and rural residents scoring higher on these indices than urban residents. Migrants and rural residents differed only in the positive symptom distress index (PSDI), with migrants scoring higher than rural residents for intensity of the symptoms. The three groups differed significantly in all 10 SCL-90 subscales (i.e., nine primary subscales and the scale with additional items). The post-hoc pair-wise comparison revealed that both migrants and rural residents scored higher than urban residents on each of the subscales. Migrants scored higher than rural residents on the depression scale and the psychoticism scale.
| Table 4. Group difference of mental health symptoms as measured by SCL-90 | |||||
| Sample | Post-Hoc Comparison (Significant Pairs) | ||||
| Overall | Urban (1) | Migrant (2) | Rural (3) | ||
| SCL-90 Global Indices | |||||
| GSI | .55 (.41) | .49 (.41) | .59 (.41) | .57 (.41)** | (1,2) (1,3) |
| PST | 36.82 (22.56) | 34.21 (24.16) | 37.92 (21.14) | 38.30 (22.09)** | (1,2) (1,3) |
| PSDI | 1.27 (.29) | 1.22 (.25) | 1.33 (.34) | 1.26 (.27)** | (1,2) (1,3) (2,3) |
| SCL-90 Subscales | |||||
| Somatization | .46 (.45) | .42 (.43) | .48 (.45) | .48 (.47)* | (1,2) (1,3) |
| Obsessive-compulsive | .72 (.49) | .63 (.48) | .78 (.51) | .75 (.48)** | (1,2) (1,3) |
| Interpersonal sensitivity | .65 (.48) | .55 (.46) | .69 (.50) | .69 (.46)** | (1,2) (1,3) |
| Depression | .57 (.48) | .51 (.46) | .63 (.50) | .57 (.48)** | (1,2) (1,3) (2,3) |
| Anxiety | .49 (.45) | .45 (.44) | .52 (.45) | .51 (.46)** | (1,2) (1,3) |
| Hostility | .61 (.53) | .56 (.52) | .62 (.54) | .64 (.54)* | (1,2) (1,3) |
| Phobic anxiety | .39 (.47) | .34 (.45) | .43 (.48) | .40 (.47)** | (1,2) (1,3) |
| Paranoid ideation | .59 (.50) | .54 (.50) | .63 (.49) | .61 (.50)** | (1,2) (1,3) |
| Psychoticism | .47 (.44) | .42 (.44) | .53 (.45) | .48 (.43)** | (1,2) (1,3) (2,3) |
| Additional items | .58 (.47) | .53 (.46) | .62 (.49) | .58 (.46)** | (1,2) (1,3) |
| GSI = Global Severity Index, the average score of the 90 items of SCL-90; PST = Positive Symptoms Total, the number of items scored above zero; PSDI = Positive Symptom Distress Index, the average score of the items scored above zero. * p<.01. ** p<.0001. |
|||||
Both SCL-90 global indices and subscales were associated with a number of individual characteristics (Table 5). Compared with women, men reported fewer positive symptoms but higher levels of intensity of these symptoms. Women reported more symptoms for depression, anxiety and phobic anxiety than men, while men reported more symptoms for paranoid ideation and psychoticism. Participants who had never married reported more symptoms and higher intensity of the symptoms than married participants. Specifically, singles reported more symptoms in all nine SCL-90 primary subscales except for somatization and obsessive-compulsive scales. Age was negatively associated with all nine SCL-90 primary subscales except for somatization, which was positively associated with age. Likewise, education, income and perceived health were all negatively associated with both global indices and all subscales of SCL-90.
Multivariate Analysis
The General Linear Model analysis of 10 SCL-90 subscales, controlling for key individual characteristics (age, gender, marital statue, education, income and perceived status of general health) revealed significant omnibus difference among the three groups for mental health status (Table 6). Gender, marital status, age, education, income and perceived health were also associated with mental health status in the multivariate test. Residency status (i.e., urban residents, migrants and rural residents) also showed a main effect on four of the SCL-90 subscales (obsessive-compulsive, interpersonal sensitivity, depression and psychoticism) after controlling for the key individual characteristics. As shown in Table 6, gender was significantly associated with depression, anxiety, phobic anxiety, paranoid ideation and psychoticism in the GLM model. Marital status was significantly associated with all SCL-90 subscales except somatization and hostility.
[Table 5]
There was a significant group-by-gender interaction term in the multivariate test. However, the interaction term was not significant for any of the SCL-90 subscales. Other two-way or three-way interaction terms among group, gender and marital status were not significant for multivariate tests or for individual scales. The strongest covariates for mental health status were the level of education and perceived status of general health, as they were significantly associated with all SCL-90 subscales. Age was associated with hostility, phobic anxiety and paranoid ideation. Monthly income was associated with four SCL-90 subscales (obsessive-compulsive, interpersonal sensitivity, depression and the scale of additional items).
[Table 6]
Discussion
Rural-to-urban migrants in the present study had inferior mental health status compared with urban residents in the communities to which they had immigrated. The difference remained significant even after controlling for age, gender, marital status, education, income and perceived general health. The data in the current study also suggest that migrants did not enjoy a more positive mental health status than their rural counterparts. Migrants reported more symptoms of depression and psychoticism than their rural counterparts in the emigrating communities. The data did not provide support for a "healthy migrant syndrome," but instead suggested a possible deteriorative effect of the migratory experience or migratory lifestyle on mental health status among rural-to-urban migrants in China.
One of the strengths in this study is the inclusion of three comparison groups: rural-to-urban migrants, urban residents in the communities to which the migrants had immigrated, and rural residents in the communities from which the migrants had emigrated. Our objective of sampling was to recruit a representative sample of the migrant population in Beijing and also to select the urban and rural samples to match the migrant sample. One of the major challenges in this study was the recruitment of urban and rural samples that were not only comparable to the migrant sample, but were also representative of the target populations. Several steps were taken to ensure both the comparability and the representative nature of the samples. We matched the samples by geographic location either at the urban destination or at the home province of origin, as well as by age range and other factors. Within those matched sampling frames, we tried to recruit participants who were representative of the study population.
Because of the existing differences between these study populations in terms of their demographic characteristics (e.g., age and gender composition), as well as income and level of education, our representative samples inherited these differences. For example, differences in age, education and marital status among the three groups in our study were consistent with the China 2000 Census Data (the most current national database with demographic characteristics), which indicated that migrants were younger than either urban permanent residents or rural permanent residents, that the migratory population was less educated than urban residents and that there were more singles among migrants (Beijing Bureau of Statistics 2003; China National Bureau of Statistics 2001). The fact that there were substantially fewer women in the migrant sample is consistent with the demographics of migrants (China National Bureau of Statistics 2001). We are less certain of the explanation for the low proportion of women in the rural population and conjecture that it results at least in part from the cultural tradition in rural China that men (rather than women) in the household communicate with outsiders (Dai 1991).
Nevertheless, the fact that both the migrant and urban resident samples were recruited from a single major metropolitan area using convenience sampling limits our ability to generalize our findings to migrants and their urban counterparts from other areas of China. The second limitation was the potential sample selection bias due to the non-random identification of the sampling units and participants (in both urban and rural areas). The third limitation is the potential overestimation of income for rural residents. While the difference in income among the three samples was consistent with the urban-rural income disparity in China (China National Bureau of Statistics 2006), the measures of monthly income among rural residents might not be comparable to that of the other two samples (urban residents and migrants). Rural residents were instructed to estimate their average monthly income by dividing their estimated annual income by 12. Because it is difficult to allocate farming incomes to individual family members, it is most likely that their calculation was based on their annual household income, while the other two groups (migrants and urban residents) might report their individual-level income.
The fourth potential limitation was the modification of the response option of SCL-90 items (i.e., reducing the range of response options from 0-4 to 0-3). Although the intention of a change of this nature was to reduce the response burden by simplifying the response options, such an alteration could cause an underestimation of the intensity of the symptoms and make it difficult to compare the findings with other studies using different response options. The fifth limitation was that the data analysis in the current study did not take into account the multistage and cluster sampling methods of the design; this could potentially inflate some of the differences in outcome measures based on residential status. Finally, because of the lack of normed data or criterion score on SCL-90 measures for the Chinese population, we were unable to assess the clinical significance of the differences in SCL-90 scores among various study samples.
Despite these methodological limitations, the current study is one of the first efforts to compare the mental health symptoms among migrants and their urban and rural counterparts. The findings in this study underscore the importance of mental health promotion and prevention efforts among rural-to-urban migrants. While a detailed examination of possible causes or determinants of elevated mental health symptoms among rural-to-urban migrants is beyond the scope of the current study, previous studies have documented a wide spectrum of possible reasons that could result in increased mental health symptoms among this population. These possibilities include separation from their families and community at origin, social isolation and social stigmatization in the urban destination, unstable living arrangements, substandard employment conditions and inadequate health-seeking behaviours (Hong et al. 2006; Li et al. 2006b, 2006a; Yang 2004). Future mental health promotion or intervention efforts should take these factors into consideration in order to improve the psychological well-being of rural-to-urban migrants in China and other developing countries. The findings in the current study also suggest a need for etiological studies and mental health promotion and prevention efforts among Chinese rural residents who suffer from more mental health problems than urban residents, an issue that has largely been overlooked in the literature.
About the Author(s)
Xiaoming Li, Pediatric Prevention Research Center, Wayne State University School of Medicine, United States
Bonita Stanton, Pediatric Prevention Research Center, Wayne State University School of Medicine, United States
Xiaoyi Fang, Beijing Normal University Institute of Developmental Psychology, China
Qing Xiong, Beijing Normal University Institute of Developmental Psychology and Jiangxi University of Finance and Economics School of Humanities Sciences, China
Shuli Yu, Pediatric Prevention Research Center, Wayne State University School of Medicine, United States
Danhua Lin, Beijing Normal University Institute of Developmental Psychology, China
Yan Hong, Texas A & M Health Science Center Department of Social and Behavioral Health, United States
Liying Zhang, Pediatric Prevention Research Center, Wayne State University School of Medicine, United States
Xinguang Chen, Pediatric Prevention Research Center, Wayne State University School of Medicine, United States
Bo Wang, Pediatric Prevention Research Center, Wayne State University School of Medicine, United States
Xiaoming Li, PhD, Prevention Research Center, Carmen and Ann Adams Department of Pediatrics, Wayne State University School of Medicine, Hutzel Building 5th Floor W534, 4707 Saint Antoine St., Detroit, MI 48201 Tel: 313-745-8663, Fax: 313-745-4993, Email: xiaoli@med.wayne.edu
Acknowledgment
This research was supported by NIH Research Grant #R21TW006375 funded by the Fogarty International Center and the National Institute of Mental Health. The authors wish to thank dedicated students and faculty members from Beijing Normal University for their assistance in field data collection. The authors also want to thank Dr. Ambika Mathur and Ms. Joanne Zwemer for assistance in manuscript preparation.References
Anderson, K., J. Huang and E. Ianchovichina. 2003. Long-Run Impacts of China's WTO Accession on Farm-Nonfarm Income Inequality and Rural Poverty. World Bank Policy Research Working Paper #3052. Washington DC: World Bank.
Beijing Bureau of Statistics. 2003. Brief Statistics on Migrant Population in Beijing. Beijing: Beijing Bureau of Statistics.
Beijing Bureau of Statistics. 2004. Brief Statistics on Migrant Population in Beijing. Beijing: Beijing Bureau of Statistics.
China National Bureau of Statistics. 2001. Characteristics of Chinese Rural Migrants 2000. Beijing: China National Bureau of Statistics.
China National Bureau of Statistics. 2004. China's Rural-to-Urban Migrants Exceed 114 Million. Beijing: China National Bureau of Statistics.
China National Bureau of Statistics. 2006. China 2005 Social Economics and Social Development Statistics. Beijing: China National Bureau of Statistics.
Dai, K. 1991. "The Life Experience and Status of Chinese Rural Women from Observation of Three Age Groups." International Sociology 6(1): 5-23.
Darmon, N. and M. Khlat. 2001. "An Overview of the Health Status of Migrants in France, in Relation to Their Dietary Practices." Public Health Nutrition 4(2): 163-72.
De Jong, G.F., A. Chamratrithirong and Q.G. Tran. 2002. "For Better, for Worse: Life Satisfaction Consequences of Migration." International Migration Review 36(3): 838-64.
Derogatis, L.R., R.S. Lipman and L. Covi. 1973. "SCL-90: An Outpatient Psychiatric Rating Scale - Preliminary Report." Psychopharmacology Bulletin 9(1): 13-28.
Diaz, R.M., G. Ayla, E. Bein, J. Henne and B.V. Marin. 2001. "The Impact of Homophobia, Poverty, and Racism on the Mental Health of Gay and Bisexual Latino Men: Findings From 3 US Cities." American Journal of Public Health 91(6): 927-32.
Fuentes-Afflick, E., N. Hessol and E. Pérez-Stable. 1999. "Testing the Epidemiologic Paradox of Low Birth Weight in Latinos." Archives of Pediatric & Adolescent Medicine 153(2): 147-53.
Hesketh, T., L. Li, X. Ye, H. Wang, M. Jiang and A. Tomkins. 2006. "HIV and Syphilis in Migrant Workers in Eastern China." Sexually Transmitted Infections 82(1): 11-4.
Hesketh, T., X.J. Ye, L. Li and H.M. Wang. 2008. "Health Status and Access to Health Care of Migrant Workers in China." Public Health Reports 123(2): 189-97.
Hong, Y., X. Li, B. Stanton, D. Lin, X. Fang, R. Mao and J. Wang. 2006. "Too Costly to Be Ill: Access to Health Care and Health Seeking Behaviors among Rural-to-urban Migrants in China." World Health and Population 8(2): 22-34.
Hu, M.Y., C.J. Zhou and S.Y. Xiao. 1997. "Psychological Health Level and Related Psychosocial Factors of Nurses in Changsha." Journal of Chinese Medicine 32(4): 192-5.
Jiang, B., J. Lin and Y. Zhang. 2000. "Clinical Observation on the Mental Symptoms of Functional Dyspepsia and its Treatment." Chinese Medicine and Western Medicine Integration 20(6): 424-6.
Li, L., H.M. Wang, X.J. Ye, M.M. Jiang, Q.Y. Lou and T. Hesketh. 2007. "The Mental Health Status of Chinese Rural-Urban Migrant Workers: Comparison with Permanent Urban and Rural Dwellers." Soc Psychiatry and Psychiatric Epidemiology 42(9): 16-22.
Li, X., B. Stanton, X. Chen, X. Fang, D. Lin, R. Mao and J. Wang. 2006. "Health Indicators and Geographic Mobility among Young Rural-to-Urban Migrants in China." World Health and Population 8(2): 5-21.
Li, X., B. Stanton, X. Fang and D. Lin. 2006. "Social Stigma and Mental Health among Rural-to-Urban Migrants in China: A Conceptual Framework and Future Research Needs." World Health and Population 8(3): 14-31.
Li, X., B. Stanton, X. Fang, D. Lin, R. Mao, J. Wang, L. Cottrell and C. Harris. 2004. "HIV/STD Risk Behaviors and Perceptions among Rural-to-Urban Migrants in China." AIDS Education and Prevention 16(6): 538-56.
Luo, L., S. Wu, X. Chen, M. Li and T. Pullum. 1996. "A Follow-up Study of First Trimester Induced Abortions at Hospitals and Family Planning Clinics in Sichuan Province, China." Contraception 53(5): 267-73.
McKay, L., S. Macintyre and A. Ellaway. 2003. Migration and Health: A Review of the International Literature. Glasgow, UK: Occasional Paper No 12, University of Glasgow, Medical Research Council (MRC) Social and Public Health Sciences Unit.
Muening, P. and M. Fahs. 2002. "Health Status and Hospital Utilization among Immigrants to New York City." Preventive Medicine 35(3): 225-32.
Pernice, R. and J. Brook. 1996. "The Mental Health Pattern of Migrants: Is There a Euphoric Period Followed By a Mental Health Crisis?" International Journal of Social Psychiatry 42(1): 18-27.
Pudaric, S., J. Sundquist and S.E. Johansson. 2000. "Major Risk Factors for Cardiovascular Disease in Elderly Migrants in Sweden." Ethnicity & Health 5(2): 137-50.
Razum, O., H. Zeeb and S. Rohrmann. 2000. "The 'Healthy Migrant Effect' - Not Merely a Fallacy of Inaccurate Denominator Figures." International Journal of Epidemiology 29(1): 191-2.
Shen, Q., Y. Lu and C. Hu. 1998. "A Preliminary Study of the Mental Health of Young Migrant Workers in Shenzhen." Psychiatry and Clinical Neurosciences 52(Suppl): S370-3.
Signh, G.K. and M. Siahpush. 2001. "All-Cause and Cause-Specific Mortality of Immigrants and Native Born in the United States." American Journal of Public Health 91(3): 392-9.
Swerdlow, A.J. 1991. "Mortality and Cancer Incidence in Vietnamese Refugees in England and Wales: A Follow-Up Study." International Journal of Epidemiology 20(1): 13-9.
Wang, X. 1993. Rating Scales for Mental Health. (Chinese Journal of Mental Health Supplement) Beijing: Chinese Association of Mental Health.
Wang, X., L. Gao, N. Shinfuku, H. Zhang, C. Zhao and Y. Shen. 2000. " Longitudinal Study of Earthquake-Related PTSD in a Randomly Selected Community Sample in North China." American Journal of Psychiatry 57(8): 1260--6.
Wu, H., L. Jiang and H. Guan. 2001. "Mental Health of Unemployed Chinese Worker." Chinese Mental Health Journal 15(1): 16-8.
Xia, G. and M. Qian. 2001. "The Relationship of Parenting Style to Self-reported Mental Health among Two Subcultures of Chinese." Journal of Adolescence 24(2): 251-60.
Yang, X. 2004. "Temporary Migration and the Spread of STDs/HIV in China: Is There a Link?" International Migration Review 38(1): 212-35.
Zhang, L. 2001. "Migration and Privatization of Space and Power in Late Socialist China." American Ethnologist 28(1): 179-205.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed

