World Health & Population
Abstract
Improving household use of healthcare facilities is a vital public health strategy to reduce burden of disease in India. Our study set out to understand the importance of the interplay of household characteristics and state-level public health covariates in accessing inpatient healthcare services. The study is based on morbidity and healthcare data from the 60th round of the Indian National Sample Survey Organisation, 2004. We used multilevel logistic regression to disentangle dependence among the observations. We observed that the education level of household heads and the household's economic well-being had a significant positive influence on accessing inpatient healthcare services. Distance from the household to the health facility showed a significant inverse association with use of health facilities for inpatient treatment. Further, we found a significant variation across the states. Variability in accessing inpatient services at the household and state levels are 1.7% and 21% respectively.
Introduction
Household use of healthcare facilities can go a long way in reducing the burden of disease in developing countries. In India, accessibility of healthcare remains a major challenge. At the macro level social, administrative, geographical and cultural factors all converge to influence health-seeking behaviour and access to health services. At the household level, cost is a major deterrent for poor people. This includes also so-called hidden costs such as transportation, loss of working time, and the cost of pathological or clinical tests or drugs that are not provided by health facilities.
Cultural perceptions and health practices of peers also determine health seeking behaviour. The poor in particular are more likely to first ignore ailments, and then turn to traditional practitioners before seeking formal healthcare. Within the household, social and economic conditions are key factors in determining use of healthcare services. Health behaviour is a dynamic process that depends on knowledge, resources, information and availability of health services locally. Lack of knowledge, cultural reasons and gender discrimination in particular prevent individuals from using basic healthcare services. In addition to gender, disparities in access are accentuated by old age and poor economic status of the household.
A number of studies have noted large inequities in healthcare accessibility for low-income and minority populations without health insurance coverage, lack of access to a regular source of care, gaps in preventive care, postponement of healthcare, and higher rates of morbidity, hospitalization, and mortality that could have been avoided with appropriate access to care (Brown 2000).
Access to healthcare services is the outcome of interactions of two broad sets of characteristics - one at the household or individual level and the other involving the healthcare delivery system. Many researchers have argued that access can best be evaluated through outcomes of the individual's passage through the system, looking at indicators such as utilization rates or satisfaction scores. These measures, they argue, permit "external validation" of the importance of the system and individual characteristics. Most often, accessibility is considered synonymous with the availability of financial and health system resources in an area (Aday and Anderson 1974).
Studies on access tend to focus on comparing utilization with health system infrastructure (supply factors) rather than a patient's health-seeking behaviour (demand factors). There are a number of theoretical models for describing access (Aday and Anderson 1974; Andersen et al. 1983; Penchansky and Thomas 1981; Donabedian 1973), many of which viewed access as a matching between predisposing factors on one side and enabling and health system factors on the other (Aday and Anderson 1974). Predisposing factors include an individual's perception of an illness, as well as population-specific cultural, social and epidemiological factors. Enabling factors include the means available to individuals for using health services. Health system factors include resources, infrastructures, institutions, procedures and regulations through which health services are delivered. Despite numerous studies measuring access, the literature about the approach for quantifying the contribution of various household characteristics and health system factors is scarce. Such an understanding could prove extremely useful in identifying specific constraints in health service delivery and could guide policy direction to provide effective stewardship.
Although empirical studies have often found that use of healthcare services depends as much on their availability and accessibility as on users' socio-economic characteristics, studies of the determinants of use of health services have focused on individual-level factors, with little attention given to the health infrastructure (Stephenson and Tsui 2002). This is partly due to the lack of adequate data. However, there is a growing interest in the ways in which healthcare services influence care-seeking behaviour. In the case of maternal care, for instance, Thaddeus and Maine (1994) pointed out the importance of community differences in accessing health facilities, the availability of healthcare providers and the adequacy of transport systems in timely care-seeking for obstetric complications. A handful of studies have indicated that distance to healthcare services is inversely associated with use (Gregory et al. 2000; Jones and Bentham 1997; Sexton and Sexton 2000). Important deterrents to accessing health services include geographic isolation, poor transport links, shortage of healthcare providers and an overall lower socio-economic status (Jong et al. 2004). Some studies have also pointed out that intense use of health services is evident if a health facility is located in the community or neighbourhood. In India, it was found that increasing the number of doctors in the community significantly increased use of health services related to delivery of care (Stephenson and Tsui 2002).
Research findings consistently support the finding that low income and high cost of services are the main constraints on service utilization and that socio-economic factors such as income, household wealth, education and working status are stronger predictors of service use than measures of the availability and accessibility of health services (Celik and Hotchkiss 2000; Valdivia 2002; Falkingham 2003; Kandel et al. 2004). In general, studies have found that people in the poorest neighbourhoods are least likely to access services adequate to meet basic healthcare needs (Pearl et al. 2001; Collins and Schulte 2003; Magadi et al. 2003). Other studies indicate that healthcare facilities are grossly inadequate and their uneven distribution depicts serious inequalities in accessibility across households and regions (Ajala et al. 2005). These studies concluded that there is an urgent need for government intervention in provision of healthcare facilities that are focused on equitable distribution and accessibility to enhance sustainable rural development.
Our study is designed to fill the gap in the literature on household access of inpatient healthcare in India, considering the factors of the number of doctors in the population, distance to facilities and public health expenditure.
Data and Methods
The unit-level data on morbidity and healthcare for this study is from the 60th round (January-June 2004) survey of the National Sample Survey Organisation (2006). The survey covers a nationally representative sample of 73,868 individuals from 58,967 households. The sample design adopted is a two-stage stratified design, with census villages and urban blocks as the first-stage units for rural and urban areas respectively, and households as the second stage-units in both the cases. The survey also collected information on hospitalized status for each person in the household during the 365 days prior to the survey date. At the household level, survey data includes residence (urban or rural), educational level of the household head, and the household's monthly expenditure. The unit of analysis for our study is households selected to represent the states. The other data sources at the state level are distance to government hospital (International Institute for Population Sciences [IIPS] 2000), percentage living in urban areas (Ministry of Health and Family Welfare [MoHFW] 2001), health expenditure as a percentage of net state domestic product at factor cost (MoHFW 2005; Central Statistical Organisation 2007) and doctor-population ratio (MoHFW 2003).
Our study attempts to understand the relationship of household characteristics and health infrastructure/resources at the state level and household use of inpatient healthcare services. The unit of analysis is the household, and the outcome variable for our analysis is the proportion of hospitalized persons in each household. It is calculated as the ratio of number of persons in a household hospitalized in the last 365 days to the number of individuals in the same household. In India, healthcare is primary the responsibility of the states and is expected to vary substantially from state to state. Inpatient healthcare accessibility to households within states would, by and large, depend on knowledge and affordability, which may also differ across states. We used multilevel logistic regression to estimate the effects of state-level public health variables and household characteristics on the outcome variable of accessibility of inpatient healthcare. Multilevel logistic regression is appropriates to capture hierarchical data structure (Subramanian et al. 2000, 2001), and the approach facilitates understanding the effects of several state- and household-level covariates on household use of health facilities for inpatients care.
The logit of proportion of hospitalized individuals in the household is modelled as
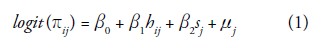
where i and j are the level 1 (household) and level 2 (state) units, respectively; πij is the probability of the outcome for the ith household in the jth state; βs are the fixed coefficients; μj~N(0, σj2) indicates the random effects for the jth state; and h and s refer to household and state characteristics, respectively. Estimates are based on a second-order penalized quasi-likelihood (PQL) procedure under the standard assumption that the outcome yij has a binomial distribution, where the nij observations are all equal to 1. Hence, yij~Binomial(1, πij), which has a binomial variance of πij(1-πij). The binomial variation assumption was tested by fitting extra-binomial variations, and found that most parameters are close to 1.0, suggesting that the Bernoulli distribution is an adequate assumption for the data (Goldstein 1995).
The analytical strategy consists of fitting five different models. The first is an empty model without any covariates. The second includes only household-level covariates in order to understand the effects of household characteristics on household accessibility to inpatient healthcare services. The state-level variables are included in third model, and the fourth model considers, in addition to household characteristics, state-level characteristics that facilitate understanding the mediating effects of state-level factors. In the last model we have included interaction terms of residence with household head's education and monthly per capita consumption expenditure (MPCE) to capture the confounding effects of education and consumption expenditure. All models were fitted with a state-level random intercept term, which represents the extent to which the outcome varies between states after controlling for the independent variables and factors that were omitted from the model or that could not be readily quantified in a large-scale survey, such as state variations in attitudes about service utilization. Regression results are presented in terms of odds ratios. Descriptive and bivariate analyses were derived using STATA Version 9.0 (StataCorp 2003), and all models were fitted in MLwIN 2.02 (MLwiN 2003). The proportion of variation explained by variables at level 1 and level 2 is measured by the formulas given by Snijders and Bösker (1999) as

where σ^2u, σ^2eand n are the estimated errors of level 2, level 1 and average number of households in each state.
Results
Characteristics of the Sample
Descriptive statistics of the outcome variable, household characteristics and state healthcare infrastructures and resources for each state are shown in Table 1. In most of the states, households were predominantly in rural areas, except in Maharashtra and Tamil Nadu. Looking at the outcome variable, the highest mean proportion of inpatient hospitalization of household members was in Kerala, at 0.114; the lowest was in Bihar, at 0.064. The overall mean proportion of household members hospitalized for inpatient treatment was 0.083. Punjab had the highest economic status, with a monthly per capita expenditure of Rs. 942 (approximately US$25); Orissa had the lowest, at Rs. 457. Healthcare need at the household level is integrated into the analysis as the percentage of household members who had reported an ailment in the 1-year period preceding the survey. As most ailments are age-related, the calculation for "mean percentage ailing" took into account the average age of household members. To understand awareness of healthcare services, the study included the household head's education, categorized into three levels. Most household heads were educated at most to the middle level,that is eight years of complete schooling under the Indian system of education. As many as half of household heads in Andhra Pradesh were not literate, while Haryana had the highest number of households headed by a person educated to at least the secondary level, at 32.6%.
The most important variable affecting accessibility of healthcare facilities was the distance from the hospital, and our study attempts to capture this influence. Mean distance to a government hospital was found to be greatest in the state of Rajasthan, at 23 km, and least in Tamil Nadu, at 7 km.
Another variable with direct bearing on accessibility is the doctor-population ratio, measured as the number of doctors per 1000 population. The overall average was 65/1000; Jammu and Kashmir had the most doctors, at 253/1000, whereas Haryana had the least, at 9/1000. The lowest level of spending on healthcare (health expenditure as a percentage of net state domestic product) was in Karnataka, at 6%; Bihar had the highest, at 23%, against the overall average of 12%.
[Table 1]
Multilevel Analysis
In this study, five competing versions of multilevel logistic regression are discussed in order to understand the interplay of household- and state-level factors in explaining accessibility of healthcare facilities. The significance of the state-level variance at a 5% level of significance in all the models indicates a considerable unexplained variation in accessibility of inpatient healthcare services at the state level that cannot be captured by the observed covariates. Relative importance of household-level and state-level variables in accounting for variation in the accessibility outcome is obtained by considering Model-I, which is a null model with no explanatory variables as a base model for comparison. For assessing the fitness of alternative models, a summary statistic is also included in the form of deviance measuring the extent to which the fitted model deviates from the saturated model. The approach for assessing model fit is to find the difference in the deviances for the alternative models, noting that the difference in deviance follows an exact Chi-square distribution, with degrees of freedom equal to the difference in the number of parameters in the competing models. First of all, it is found from the multilevel modelling that there exists a significant variation in accessibility of inpatient services between state units, at p < .05. The dispersion of residuals in Figure 1 depict this variability in accessibility across the state units. States with low health expenditures measured as percentage share of domestic product are concentrated in state units having lower levels of hospitalization.
[Figure 1]
From Model-II, which includes only household characteristics, it is found that the odds of urban households using inpatient care services are lowered by 0.13 compared with rural households (Table 2). This may reflect exposure of rural households to adverse work conditions, making them prone to accidents and injuries that required hospitalization. Patel (2009) found that incidence of disability due to burns, accidents and injury is higher in rural areas. The key to developing equitable health systems and reducing social exclusion for the poor is in removing barriers on access to healthcare services (Feachem 2000). Even among the poor, high utilization of services was found in the case of Kerala , the state known for high literacy level, well informed citizen and good governance (Krishnan 2000; Mahal et al. 2001).
[Table 2]
This study also showed that higher economic status is likely to increase healthcare accessibility. The odds of receiving inpatient healthcare services by households in the medium quintile income group in terms of MPCE were higher by 0.22 compared to households in the lowest quintile income group, and they were higher by 0.55 for households in the highest quintile income group after controlling other household characteristics. Both effects were significant at p < .05. This clearly indicates that households with greater economic well-being had a higher probability of accessing services for inpatients care.
Educational attainment is the key to awareness of healthcare needs and use of healthcare facilities. Our study supports this notion and revealed that the odds of accessing inpatient facilities were higher by 0.07 and 0.15 for households headed by someone educated at most to the middle level and secondary and above, compared with households headed by a non-literate person, respectively, after controlling the effects of other covariates. These results are significant at p < .05. The proxy for household healthcare need - the percentage of household members with reported ailments in the 1-year period leading up to the survey - was a significant association at 1% of significance with household access of inpatient healthcare facilities. In regard to the importance of age on use of inpatient care, we found that the higher the mean age of household members, the lower the likelihood of a household having accessed inpatient healthcare. This inverse association, after controlling other household and state confounders, was statistically significant at p < .01. The result is a reflection of aging on morbidity and ailments.
From Model-III, which includes only the state-level variables, we found that distance to government hospital was inversely association with the odds of using inpatient care facilities; it was statistically significant at p < .01. This finding is aligned with results of other studies, which found that having health facilities in the neighbourhood resulted in higher odds of making four or more antenatal care visits (Anastasia and Calixte 2006). Level of urbanization at the state level is considered as a proxy for availability of healthcare infrastructure and health facilities. Level of urbanization is measured as the percentage of the population that lives in urban areas. The better the healthcare infrastructure, the greater household use of healthcare facilities. If we assume a one-to-one correspondence between percentage urban population and healthcare infrastructure, we can conclude that the odds of household use of healthcare facilities for inpatient treatment becomes higher by 0.01, corresponding to 1% improvement in health infrastructure. This association is significant at p < .05. There is no doubt that each state's investment in public health also plays a major role in accessing health facilities. Though the association between health expenditure as percentage of state domestic product and household access of inpatient care, controlling for other confounders, was found to be positive, it was not statistically significant. Further, the influence of the doctor-population ratio on inpatient healthcare facilities, though positive in the sense that the higher the ratio the greater the accessibility, was again found to be statistically insignificant.
Model-IV integrates both household-level and state-level characteristics in describing use of inpatient care facilities. Most of the preceding findings remain intact. With the integration of state-level covariates, there is a reduction of 38% in the variance initially observed between state units, compared to the result of Model-II, which includes only household-level covariates. The magnitudes of healthcare access differential explained by household- and state-level covariates included in Model-IV are 1.7% and 21% respectively. This indicates the importance of state-level covariates in explaining variability of outcome, as in other studies (Ladusingh and Singh 2006).
Now to explore the relationship between residence and accessibility of services, where it is important to know whether place variability is determined by the household head's level of education or by the economic well-being of the household. To arrive at a comprehensive interpretation, two sets of interacting terms are included in Model-V - residence and education, and residence and MPCE quintile. In this model it should be noted that the influences of residence and education on use of inpatient services lose their statistical significance, though the nature of their relationships still holds up. The introduction of interactions between residence and household head's education, residence and MPCE quintile, facilitates a comparative assessment of the likelihood of using the services by each level of education within each level of economic status. The interaction results show that household access to inpatient healthcare facilities across place of residence do not significantly vary by the education level of the household head, that is, there is no significant contribution of interaction between residence and education. However, the contribution of interaction between residence and household economic well-being on household use of services is significant at p < .01. This proportion of variation in access by household- and state-level factors remains unchanged, as in Model-IV. Nonetheless, significant state-level variances in the last two models suggest unexplained variations remaining in the data at the state level. The test of difference in deviance statistics indicates that results drawn from Model-V are preferable over that of Model-IV.
Conclusion
The analysis presented here has highlighted the importance of household characteristics and state-level health infrastructure in explaining healthcare accessibility for inpatient care in India. It indicates that the education level of the head of the household plays a major role in explaining accessibility at the household level. Our study confirms the results of other studies, that household economic well-being measured in terms of monthly per capita expenditure has a significant direct influence on use of healthcare services. From the findings of our study, it seems that rural households are more prone to ailments that required inpatient treatment, as in a study in Vietnam probably related to accidents and injuries indicated in Patel (2009). The finding that inpatient healthcare services decrease with mean age of household is also aligned with findings from other studies. Most of the results of our study related to education level of the household head, household economic well-being and rural location conform to the findings of Sepehri et al. (2008) and Lin et al. (2004). For state-level factors, distance to government hospitals had a significant inverse association with accessibility of services. This aligns with other studies by Gregory et al. (2000), Jones and Bentham (1997) and Sexton and Sexton (2000). The availability of health infrastructure, measured in terms of level of urbanization, was found to have a significant association with household use of inpatient healthcare facilities. The number of doctors in the population had a positive effect on the use of inpatient services, though it is not pronounced enough to be significant. One of the most valuable findings is that household factors dominated over state-level healthcare infrastructure and expenditure. This study also indicates that a sizeable proportion of the variability in access is explained by state-level factors.
About the Author(s)
Chungkham Holendro Singh, Lecturer, Department of Statistics, North-Eastern Hill University, Umshing Mawkynroh, Meghalaya, Shillong, India
Laishram Ladusingh, Professor, Department of Mathematical Demography & Statistics, International Institute for Population Sciences, Mumbai, India
Chungkham Holendro Singh, Department of Statistics, North-Eastern Hill University, Umshing Mawkynroh, Meghalaya, Shillong-793022, India, Tel. +91-0364-2722901, email. holendrosingh@gmail.com; holendro@iips.net
References
Aday, L.A. and R.A. Anderson. 1974. "A Framework for the Study of Access to Medical Care." Health Services Research 9: 208-20.
Ajala, O.A. S.L. Lekan and S.A. Adeyinka. 2005. "Accessibility to Health Care Facilities: A Panacea for Sustainable Rural Development in Osun State Southwestern, Nigeria." Journal of Human Ecology 18(2): 121-8.
Anastasia, J.G. and M.G. Calixte. 2006. "Effects of the Physical Accessibility of Maternal Health Services on Their Use in Rural Haiti." Population Studies 60 (3): 271-88.
Andersen, R.M., A. McCutcheon, L.A. Aday, G.Y. Chiu and R. Bell. 1983. "Exploring Dimensions of Access to Medical Care." Health Services Research 18(1): 49-74.
Brown, E.R., V.D. Ojeda, W.R. Roberta and R. Levan. 2000. Racial and Ethnic Disparities in Access to Health Insurance and Health Care. University of California, LA: Policy Research Report.
Celik, Y. and D.R. Hotchkiss. 2000. "The Socio-Economic Determinants of Maternal Health Care Utilization in Turkey." Social Science and Medicine 50(12): 1797-1806
Central Statistical Organisation. 2007. Net State Domestic Product, New Series, 2007. Government of India: Ministry of Statistics & Programme Implementation.
Collins J.W. and N.F. Schulte. 2003 "Infant Health: Race, Risk and Residence." In I. Kawachi and L.F. Berkman, eds., Neighborhoods and Health pp. 223-232. New York: Oxford University Press.
Donabedian, A. 1973. Aspects of Medical Care Administration. Cambridge: Harvard University Press.
Falkingham, J. 2003. "Inequality and Changes in Women's Use of Maternal Health-Care Services in Tajikistan." Studies in Family Planning 34(1): 32-43.
Feachem, R.G. 2000. "Poverty and Inequity: A Proper Focus for the New Century." Bulletin of the World Health Organisation 78: 1-2.
Goldstein, H. 1995. Multilevel Statistical Models. London: Edward Arnold.
Government of India. 2003. Health Information of India. Central Bureau of Health Intelligence, MoHFW, Government of India.
Gregory, P.M., E.S. Malka, J.B. Kostis, A.C. Wilson, J.K. Arora and G.G. Rhoads. 2000. "Impact of Geographic Proximity to Cardiac Revascularization Services on Service Utilization." Medical Care 38(1): 45-57.
International Institute for Population Sciences (IIPS) and ORC Macro. 2000. National Family Health Survey, 1998-99. Mumbai: IIPS.
Jones, A.P. and G. Bentham. 1997. "Health Service Accessibility and Deaths from Asthma in 401 Local Authority Districts in England and Wales 1988-92." Thorax 52: 218-22.
Jong, K.E., D.P. Smith, X.Q. Yu, L. O'Connell, D. Goldstein and B.K. Armstrong. 2004. "Remoteness of Residence and Survival from Cancer in New South Wales." Medical Journal of Australia 180: 618-22.
Kandel, D.B., G.E. Kiros, C. Schaffran and M.C. Hu. 2004. "Racial/Ethnic Differences in Cigarette Smoking Initiation and Progression to Daily Smoking: A Multilevel Analysis." American Journal of Public Health 94(1): 128-35.
Krishnan, T.N. 2000. "Access to Health and the Burden of Treatment in India: An Inter-State Comparison." In M. Rao, ed., Disinvesting in Health pp. 208-232. New Delhi: Sage.
Ladusingh, L. and C.H. Singh. 2006. "Place, Community Education, Gender and Child Mortality in North-East India." Population, Space and Place 12: 65-76.
Lin, J.D., J.L. Wu and P.N. Lee. 2004. "Utilization of Inpatient Care and Its Determinants among Persons with Intellectual Disabilities in Day Care Centres in Taiwan." Journal of Intellectual Disability Research 48(7): 655-62.
Magadi, M.A, E.M., Zulu and M. Brockerhoff. 2003. "The Inequality of Maternal Health Care in Sub-Saharan Africa in the 1990's." Population Studies 57 (3): 347-66.
Mahal, A., A.S. Yazbecl and D.H. Peters. 2001. The Poor and Health Service Use in India. HNP Discussion Paper. Washington, DC: The World Bank.
Ministry of Health and Family Welfare (MoHFW). 2005. National Health Accounts, 2001-2002. New Delhi: National Health Accounts Cell, MoHFW, Government of India.
MlwiN Software Version 2.02. 2003. Multilevel Models Project. London: Institute of Education, University of London .
National Sample Survey Organisation. 2006. Morbidity, Health Care and Conditions of Aged, 60th Round, January-June, 2004, Schedule 25.0. New Delhi: National Sample Survey Organisation, Department of Statistics, Government of India.
Patel, S.K. 2009. A Study of Disability and Health Expectancy in India. Unpublished PhD, International Institute for Population Sciences, Mumbai, India.
Pearl, M., P. Braveman and B. Abrahams. 2001. "The Relationship of Neighborhood of Socioeconomic Characteristics to Birth Weight among 5 Ethnic Groups in California." American Journal of Public Health 91 (11): 1808-14.
Penchansky, R. and J.W. Thomas. 1981. "The Concept of Access: Definition and Relationship to Consumer Satisfaction." Medical Care 19: 127-40.
Sepehri, A., S. Moshiri, W. Simpson and S. Sarma. 2008. "Taking Account of Context: How Important Are Household Characteristics in Explaining Adult Health-Seeking Behavior? The Case of Vietnam." Health Policy and Planning 23: 397-407.
Sexton, P. and T.L.H. Sexton. 2000. "Excess Coronary Mortality among Australian Men and Women Living outside the Capital City Statistical Divisions." Medical Journal of Australia 172: 370-4.
Snijders, T.A.B. and R.J. Bösker. 1999. Multilevel Analysis: An Introduction to Basic and Advanced Multilevel Modeling. London: Sage.
StataCorp. 2003. Stata Statistical Software: Release 9.0. College Station, TX: Stata Corp.
Stephenson, R. and A.O. Tsui. 2002. "Contextual Influences on Reproductive Health Services Use Uttar Pradesh, India." Studies in Family Planning 33(4): 309-20.
Subramanian, S.V., C., Duncan and K., Jones. 2000. "'Illiterate People' or 'Illiterate Places': the Indian Evidence." Indian Social Science Review 2: 237-74.
Subramanian, S.V., C. Duncan, K. and Jones. 2001. "Multilevel Perspective on Modeling Census Data." Environment and Planning A; 33: 399-417.
Thaddeus, S. and D. Maine. 1994. "Too Far to Walk: Maternal Mortality in Context." Social Science and Medicine 38(8): 1091-110.
Valdivia, M. 2002. "Public Health Infrastructure and Equity in the Utilisation of Outpatient Health Care Services in Peru." Health Policy and Planning 17 (Suppl.): 12-19.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed

