Healthcare Policy
Financial and Work Satisfaction: Impacts of Participation in Primary Care Reform on Physicians in Ontario
Abstract
Governments in Ontario have promised family physicians (FPs) that participation in primary care reform would be financially as well as professionally rewarding. We compared work satisfaction, incomes and work patterns of FPs practising in different models to determine whether the predicted benefits to physicians really materialized. Study participants included 332 FPs in Ontario practising in five models of care. The study combined self-reported survey data with administrative data from ICES and income data from the Canada Revenue Agency. FPs working in non–fee-for-service (FFS) models had higher levels of work satisfaction than those in FFS models. Incomes were similar across groups prior to the advent of primary care reform. Incomes of family health network FPs rose by about 30%, while family health group FPs saw increases of about 10% and those in FFS experienced minimal changes or decreases. Self-reported change in income was not reliable, with only 47% of physicians correctly identifying whether their income remained stable, increased or decreased. The availability of a variety of FFS- and non–FFS-based payment options, each designed to accommodate physicians with different types or styles of practice, may be a useful tool for governments as they grapple with issues of physician recruitment and retention.
A key element in Canadian primary care reform is a focus on finding the most appropriate funding mechanism for providers (Romanow 2002; Shortt 2004). Fee-for-service models (FFS), still the dominant approach in Canada, pay a fixed rate per service provided. Capitated models provide a fixed rate per patient rostered, while salary models pay providers a negotiated amount for a fixed period of service. Mixed/blended models combine elements of more than one of the above models, and some schemes provide bonus payments for particular activities or for meeting quality targets. The adoption of non-FFS models is considered a key element of primary care reform, and physician interest in these options has been rising, although there is little interest in purely capitated models (Hutchison 2004; Hutchison et al. 2001; Hunter et al. 2004; Macinko et al. 2003; Martin 2003; Shortt 2004; Starfield and Shi 2002). Ontario has introduced a number of alternatives to FFS (Table 1), with predictions of higher incomes and greater work satisfaction used as incentives for physicians to convert. We conducted a cross-sectional study to determine whether the predicted benefits to physicians actually materialized, by comparing work satisfaction, work patterns and income for physicians remaining in FFS with those who had recently switched to one of two new models, family health networks (FHN) and family health groups (FHG), or who practised in one of two established alternatives to FFS, health services organizations (HSO) and community health centres (CHC).
| TABLE 1. Primary care payment models of interest and elements of primary care reform | ||||||
| Model | Patient enrolment (rostering) | Enhanced access (mandatory after-hours access and on-call) | Support for multidisciplinary team approaches | Support for enhanced information technology | Non-FFS payment | Payment method |
| FFS | No | No | No | No | No | FFS |
| FHG | Yes | Yes | No | No | No | FFS + bonuses |
| FHN | Yes | Yes | Yes | Yes | Yes | Blended |
| HSO | Yes | Yes | Yes | Yes | Yes | Capitation |
| CHC | Yes | Yes | Yes | Yes | Yes | Salary |
| Note: Above reflects the status of each model in 2004/05. Since then, other patient enrolment models (PEMs) have been developed in Ontario, and IT support has been extended to more models. Pay-for-performance quality bonuses have also been extended to all PEMs. | ||||||
Methods
All primary care physicians in Ontario were eligible for selection. All FHN, HSO and CHC physicians and a random selection of FFS and FHG physicians were identified for recruitment. We used a modified Dillman technique that included reminders and repeat mailings to recruit participants (Dillman 1999; Field et al. 2002). Participants were asked to consent to a review of five years of their income tax records by a third party (an accounting firm); to consent to a review of the administrative data on all billings submitted to the Ontario Health Insurance Plan (OHIP) to determine workload; and to complete a self-reported survey on work satisfaction (Bovier and Perneger 2003) and primary care reform that was included with the recruitment package. Participants sent their surveys, along with consents for the income and administrative data portions of the study, directly to KPMG, a national accounting firm, which assigned a study ID number for each physician.
All physicians were also asked to complete a Canada Revenue Agency form T1013, giving KPMG authorization to access their data for tax years 2000 to 2004. All personal tax information remained in the custody of KPMG at all times and was never released to the study team in an identifiable format. Income information (gross professional/business income, net professional/business income, employment income, investment income) for each of the tax years was added to survey information by KPMG. A key file was created with the study ID number and identifying information for the participating physicians; following completion of data quality checks, the identifying information was deleted from the data set prior to transfer to the research team.
A copy of the key file created by KMPG was sent to the Institute for Clinical Evaluative Sciences (ICES), where it was used to identify the study physicians in the OHIP claims database and the Ontario Physician Workforce Database (OPWD). Once the required data had been acquired, all identifying information except the study ID number was removed from this data set and the key file was destroyed. Summary information on physician characteristics was obtained from the OPWD for our study physicians and for all family physicians in Ontario (by model), while practice characteristics and workload measures were obtained from the OHIP claims database.
The study was reviewed and approved by the Research Ethics Boards at Queen's University, the University of Ottawa and Sunnybrook and Women's College Hospital.
Results
Three hundred and thirty-two family physicians (FPs) agreed to participate, with the overall participation rate for all groups being 20.2%. This rate varied significantly by model of practice, from a high of 38% for FHN physicians to a low of only 7.5% for FFS, with the other groups ranging from 16% to 23%. Some physicians had anomalous income results, with increases or decreases in income of greater than 50% of baseline. Review of responses to other questions found that almost all were absent from practice for all or part of our pre-/post-change index years, leaving a sample size of 220 for the income change analysis.
Non-FFS physicians (FHN, HSO, CHC) were more satisfied overall with their payment model, and in almost all of the measured dimensions of work satisfaction, than physicians in FFS models (FHG and FFS). Inter-group differences were statistically significant (ANOVA) for all items except quality of patient care (Table 2). Regression models were used to adjust for possible confounding variables. Items included in the model were gender, age, location of practice, patient volume (number of visits), years since graduation and payment model (FFS-based = FHG+FFS vs. blended/capitated/salary-based = FHN/HSO/CHC). Regression analysis was repeated using only FFS/FHG and FHN respondents. In the regression models, payment model was the only statistically significant predictor of overall satisfaction (p<0.001), satisfaction with model (p<0.001) and the personal rewards (p=0.02) and income (p<0.001) domain scales. Patient volume (number of visits) was the only significant predictor for the burden domain score (p=0.002), and there were no significant predictors for the patient care domain. When asked whether they would choose their current primary practice model again, FHN physicians were significantly more likely (85.3%) than either FHG (54.8%) or FFS (41.0%) physicians to indicate that they would definitely or probably choose their current model.
| TABLE 2. Relationships of work satisfaction to practice model | ||||||||
| n | % | General satisfaction | Practice model | Personal rewards | Burden | Patient care | Income | |
| Type of practicea | p<0.001 | p<0.001 | p=0.001 | p=0.002 | p=0.056 | p<0.001 | ||
| FHN | 112 | 34 | 5.31 (1.05)dc | 5.56 (1.02)dc | 5.56 (0.74)d | 3.76 (1.21) | 4.94 (0.92) | 5.32 (1.19)dc |
| FHG | 127 | 38 | 4.67 (1.25)bef | 4.61 (1.24)bef | 5.57 (0.78) | 3.39 (1.22)e | 4.70 (1.03) | 4.13 (1.14)bef |
| FFS | 38 | 11 | 4.55 (1.33)bef | 4.71 (1.51)bef | 4.96 (0.91)bf | 3.88 (1.42) | 4.52 (1.12) | 4.00 (1.24)bef |
| CHC | 32 | 10 | 5.41 (1.04)dc | 5.69 (1.09)dc | 5.49 (0.86) | 4.34 (1.13)c | 5.06 (0.85) | 5.09 (1.19)dc |
| HSO | 23 | 7 | 5.57 (0.99)dc | 5.91 (0.73)dc | 5.64 (0.70)d | 3.61 (1.13) | 4.88 (0.88) | 5.30 (1.11)dc |
| a ANOVA, differences between groups | ||||||||
| b Post hoc Bonferroni, significantly different (p<0.05) from FHN | ||||||||
| c Post hoc Bonferroni, significantly different (p<0.05) from FHG | ||||||||
| d Post hoc Bonferroni, significantly different (p<0.05) from FFS | ||||||||
| e Post hoc Bonferroni, significantly different (p<0.05) from CHC | ||||||||
| f Post hoc Bonferroni, significantly different (p<0.05) from HSO | ||||||||
Physicians had also been assured that participating in primary care reform initiatives would be financially rewarding. Survey participants were asked if they felt their real net incomes over the previous five years had increased, decreased or remained the same. There were significant differences in perceptions among groups, with 79.1% of FHN physicians reporting an increase, compared to 34.8% of FHG physicians and 26.7% of those in FFS (p<0.001) (Table 3). We felt it was also important to evaluate this claim quantitatively using an accurate source of data, in this case obtained from the Canada Revenue Agency by KMPG and passed on to the research team in an anonymous fashion with the consent of the participating physicians.
| TABLE 3. Real versus perceived changes in income | |||||
| Actual changes vs. perceived changes and discrepancy | |||||
| Payment model | |||||
| FFS | FHN | CHC | FHG | HSO | |
| n | 30 | 86 | 25 | 109 | 22 |
| Actual Changes in Real Net Income (2000–2004) (Proportions) | |||||
| Decreased* | 23.33 | 15.12 | 12.00 | 16.51 | 9.09 |
| Remained the same (±10%)** | 36.67 | 17.44 | 48.00 | 33.94 | 40.91 |
| Increased* | 40.00 | 67.44 | 40.00 | 49.54 | 50.00 |
| Pearson chi2(8) = 16.1523 Pr = 0.040 |
|||||
| Perceived Changes in Real Net Income (2000–2004) (Proportions) | |||||
| Decreased* | 53.33 | 4.65 | 40.00 | 35.78 | 27.27 |
| Remained the same** | 20.00 | 16.28 | 28.00 | 29.36 | 36.36 |
| Increased* | 26.67 | 79.07 | 32.00 | 34.86 | 36.36 |
| Pearson chi2(8) = 58.8233 Pr = 0.000 |
|||||
| Discrepancy between Perceived and Actual Changes (Proportions) | |||||
| Under-perceived | 50.00 | 10.47 | 44.00 | 43.12 | 31.82 |
| Right-perceived | 33.33 | 63.95 | 40.00 | 36.70 | 63.64 |
| Over-perceived | 16.67 | 25.58 | 16.00 | 20.18 | 4.55 |
| Pearson chi2(8) = 35.0645 Pr = 0.000 |
|||||
| * By over 10% | |||||
| ** ±10% | |||||
Annual income was defined as the sum of net professional, net business and employment income (investment income was not included), and was adjusted for the cost of living by converting all figures into real 2004 dollars using the Ontario Consumer Price Index. All groups were similar prior to the change, with the mean real net income for all study physicians at $163,300. There were no significant differences among groups in income levels, the growth rates in income, the attributes of the patient population or activity levels prior to change in payment model. Post-change, significant differences were noted among groups, with FHN and HSO physicians having mean/median incomes between $196,000 and $211,000 while FHG, FFS and CHC physicians were sitting between $170,000 and $177,000. FHN physicians experienced gains in mean and median income of greater than 30%, FHG physicians experienced gains of about 10% and FFS physicians either had minimal increases or decreases in income over the same period (Table 4). We also estimated the "treatment effect" or "difference in difference" on FP income of switching to new payment models. These measures represent the gain that they realize relative to what they would have earned had they remained within the FFS model. Using this method of analysis, the average growth rate of income was 31% for FHN doctors and 12% for FHG doctors relative to their FFS counterparts. Estimates of change for income growth are very similar (28% for FHN doctors, 13% for FHG doctors) in the multivariate analysis (adjusted for age, gender and year of graduation).
| TABLE 4. Pre- and post-change real net income (2004 dollars) by model | ||||||
| Current payment model | Actual number of months after change | Total annual real net income pre-/post-change | ||||
| Pre-change income (Year 2000) | Post-change income (Year 2004) | Actual change in income (Post – Pre) | % change in income (Post – Pre)/Pre | |||
| FHN | Mean | 10.13 | 161,596.9 | 206,763.1 | 45,166.2 | 31.3 |
| SD | 2.67 | 62,316.8 | 87,657.7 | 53,369.6 | 32.1 | |
| Median | 11.50 | 153,350.2 | 196,573.5 | 43,069.2 | 33.7 | |
| 25 Percentile | 9.00 | 118,090.4 | 14,454.2 | 14,447.5 | 9.6 | |
| 75 Percentile | 12.00 | 208,599.4 | 252,669 | 75,461.8 | 50.1 | |
| FHG | Mean | 10.08 | 162,583.4 | 176,808.8 | 14,225.4 | 11.8 |
| SD | 2.94 | 71,344.6 | 86,164.8 | 43,952.8 | 27.9 | |
| Median | 12.00 | 157,381.6 | 160,113 | 12,517 | 9.6 | |
| 25 Percentile | 9.00 | 115,464.6 | 127,979 | –6,117.5 | –4 | |
| 75 Percentile | 12.00 | 198,181.3 | 215,096.5 | 33,078.5 | 22.3 | |
| FFS | Mean | 12.00 | 165,718.5 | 170,138.9 | 4,420.4 | 3.2 |
| SD | 0.00 | 66,791.7 | 81,070 | 49,921.2 | 30.6 | |
| Median | 12.00 | 150,776.1 | 178,673 | –2,048 | –1.6 | |
| 25 Percentile | 12.00 | 122,409.4 | 115,186 | –10,623.2 | –9.3 | |
| 75 Percentile | 12.00 | 217,471.7 | 227,474 | 30,801.3 | 20.8 | |
| CHC | Mean | N/A | 148,036.6 | 171,894.5 | 23,858 | 19.2 |
| SD | 45,722.8 | 44,915.5 | 25,991.1 | 23.5 | ||
| Median | 138,045.6 | 155,137 | 15,648.6 | 9.2 | ||
| 25 Percentile | 121,915.6 | 145,355 | 5,790.6 | 4.1 | ||
| 75 Percentile | 153,283.7 | 195,718 | 32,711.4 | 26.8 | ||
| HSO | Mean | N/A | 183,037.1 | 210,440.8 | 27,403.7 | 24.2 |
| SD | 66,862 | 52,945.6 | 41,334.6 | 36.4 | ||
| Median | 178,408.1 | 204,792.5 | 20,713.8 | 10.1 | ||
| 25 Percentile | 114,963.6 | 186,052 | 2,225.9 | 0.9 | ||
| 75 Percentile | 229,466.4 | 251,932 | 38,015.5 | 45.4 | ||
| Total | Mean | 10.35 | 163,307.4 | 187,998.4 | 2,4691 | 18.5 |
| SD | 2.70 | 66,014.6 | 82,665 | 48,750.8 | 31.5 | |
| Median | 12.00 | 156,006.9 | 176,906 | 18,295.6 | 11.6 | |
| 25 Percentile | 9.00 | 116,629.8 | 130,984 | –2,624.9 | –2.8 | |
| 75 Percentile | 12.00 | 204,682.4 | 232,065.5 | 52,652.2 | 36.9 | |
| Note: Number of doctors in each model: 25 in FFS, 70 in FHN, 92 in FHG, 15 in CHC and 18 in HSO. | ||||||
| Total number of doctors in all models: 220. | ||||||
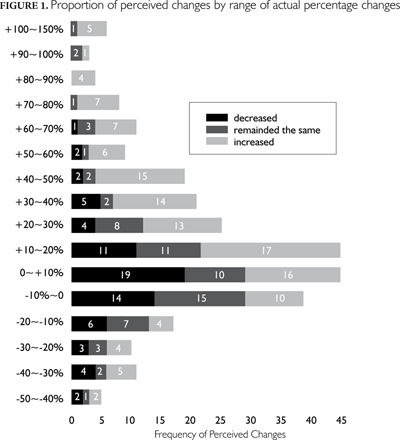
Because we had both quantitative and self-reported data on income change, we were also able to evaluate the accuracy of the perceptions reported by study participants. Table 3 summarizes the results of this evaluation by payment model. Fewer than half of the study participants correctly identified their direction of income change. The degree of discrepancy varied significantly by model, with FHN and HSO physicians having the most accurate perceptions (p<0.001). Participants in all models except for FHN were more likely to under-perceive their actual change in income, while FHN physicians were more likely to over-perceive this. Figure 1 presents a summary of responses by the degree of actual income change.
OHIP data were used to compare the patient populations for each group pre- and post-change for a range of factors including gender, age and prevalence of common chronic diseases, such as diabetes and heart disease. Inter-group comparisons indicated the groups were quite similar. In addition, a number of workload measures, including total visits, ER visits, nursing home visits, hospital visits, home/office visits and involvement in obstetrics were assessed before, during and after transition. Some inter-group differences were noted both pre- and post-change, with FHN physicians being more active in the provision of ER services, hospital visits, nursing home visits and obstetrics than physicians in the FFS or FHG groups. This finding may be explained at least in part by the fact that FHN physicians are more likely to be located in rural regions. There was minimal change in the number of days worked. FHN physicians saw a decrease in total visits and visits per day, while there was no change for FHG physicians and a slight increase for FFS physicians (Figure 2). We did not identify any clear changes in work patterns or practice composition that might account for major changes in income or differences in work satisfaction observed during the study period.
Discussion
Physicians' satisfaction with their work is important, as this factor has been linked both to improved retention and possibly to improved performance (Grol et al. 1985; Lichetenstein 1984). It has also been identified as an important indicator of success for primary care reform efforts in Canada (CIHI 2006; Watson et al. 2004). International research has suggested that payment model may be related to physicians' work satisfaction, but results do not consistently support any one model (Grembowski et al. 2003; Murray et al. 2001; Nadler et al. 1999; Simoens et al. 2002). In Canada, physicians' work satisfaction has been reported as either poor or at best middling, with family medicine ranking among the least satisfied specialties (Baerlocher 2006; Spurgeon 2003; Sullivan and Buske 1998). Studies in Ontario showed that work satisfaction among FPs declined between 1993 and 1999, that few FPs felt that primary care reform had a favourable effect on their practices and that few supported capitation or patient rostering (Cohen et al. 2001; Hunter et al. 2004). In contrast, the differences in work satisfaction discerned in this study favoured funding models that included both these elements.
Study informants who participated in new funding models both perceived and achieved increases in real net income. While Figure 1 shows that the greater the change in income, the more likely it is that the perception is correct, it also shows that misperceptions occur even with large changes in real net income. When changes are examined between a loss or gain of 30% (which represents the vast majority of income change expectations one would encounter), the reported changes in income are not significantly different from a random allocation of the participants to the response categories. These findings emphasize the need for data sources on professional income that do not rely on self-reported perceptions. They also point to the need for communication of accurate data on income and future income expectations to physicians and physicians in training, as these can affect career-choice decisions for trainees as well as work satisfaction for practising physicians (Nicholson and Souleles 2001, 2002).
Limitations and strengths
Our results need to be interpreted cautiously, given some important limitations. First and foremost is the participation rate, which was low overall and which varied significantly by group. We are therefore most confident of the results reported for within-group changes in the FHN physicians (38% participation rate) and less certain about comparisons across groups, most particularly for comparisons with FFS physicians (only 7.5% participation rate). When considering how to interpret this limitation, readers should bear in mind that response rates for physician surveys for any purpose are generally only moderate (54% in a review of published surveys) (Asch et al. 1997), and that response rates are lower when surveys are anonymous (Asch et al. 1997, 2000; Dillman 1999; Field et al. 2002). As we were requesting sensitive and confidential personal information, such as billing data and income tax data, in addition to a self-reported survey, we were not surprised by a poor response rate. We had considered other methods of acquiring the data, but were not able to identify any other means of accurately quantifying income change over time that did not rely on self-reporting, a method that we felt would not have been reliable. This concern was confirmed by the results of this study.
To the best of our knowledge, this is the first study of physicians from any country that has ever requested and obtained access to income data from such a reliable source. We are somewhat reassured by the fact that our observed income changes in each group are fairly close to estimates of expected income change generated by practice profiling and modelling of anticipated billings under different payment schemes that were communicated to physicians at the time (R. Wilson, former CEO, Ontario Family Health Networks, personal communication 2006). To account for the risk of a significant non-respondent bias, particularly for the FFS group, we sought evidence to identify the ways in which the study physicians differed from the general Ontario physician population. We were able to use administrative data to conduct a fairly comprehensive comparison of study participants to the overall Ontario physician population within each model of care (Table 5). Study participants of all group types were more likely to be Canadian-trained and practising in rural areas. In addition, we used analytic techniques, such as regression models including possible confounding variables, that are aimed at minimizing the impact of these biases on our conclusions. We acknowledge that the generalizabilty of these findings will nonetheless remain questionable, but feel they are still valuable additions to our understanding of the impact of participation in primary care reform in Ontario, particularly in terms of understanding the experience of early adopters of new payment models. We can fairly securely say that FHN physicians experienced significant financial gains and were highly satisfied with their decision to change models. There is much less certainty about how this finding compares to the experiences of physicians in other payment models.
| TABLE 5. Comparison of study physicians to Ontario GP/FP population | ||||||||||
| Total Ontario GP/FP physician population | Study physicians | |||||||||
| CHC | FFS | FHG | FHN | HSO | CHC | FFS | FHG | FHN | HSO | |
| n | 186 | 5,349 | 3,706 | 590 | 165 | 31 | 39 | 123 | 105 | 21 |
| Age (mean) | 42.56 | 50.06 | 46.82 | 45.02 | 50.25 | 41.61 | 43 | 45.54 | 46.12 | 51.86 |
| Sex (% male) | 41.94% | 66.14% | 64.81% | 64.92% | 72.73% | 51.61% | 61.54% | 60.98% | 64.76% | 85.71% |
| Years since graduation (mean) | 16.37 | 23.72 | 21.11 | 19.18 | 24.51 | 14.9 | 16.79 | 20.02 | 20.34 | 26.9 |
| Foreign trained (%) | 9.68% | 24.72% | 18.20% | 10.45% | 9.09% | 6.45% | 13.16% | 9.76%* | 6.67% | 23.81%* |
| Rural (%) | 9.14% | 10.54% | 8.09% | 32.71% | 2.42% | 19.35% | 15.38% | 22.76%* | 33.33% | 4.76% |
| Total Visits | N/A | 4,418 | 6,725 | 5,329 | N/A | N/A | 5,229 | 5,862 | 5,454 | N/A |
| Emergency Visits | N/A | 243 | 170 | 331 | N/A | N/A | 642 | 703* | 666* | N/A |
| Office Visits | N/A | 3,772 | 5,907 | 4,279 | N/A | N/A | 4,350 | 4,884 | 4,251 | N/A |
| Total Payments | N/A | $145,131.43 | $216,007.30 | $161,879.64 | N/A | N/A | $173,331.21 | $198,692.40 | $150,831.12 | N/A |
| Classification data for HSO and CHCs based on 2003/04 status and for FHGs and FHNs based on Dec. 1, 2005. all demographic and workload data based on 2003/04. | ||||||||||
| *p<0.05 for difference between study physicians and total Ontario GP/FP population (within the same model) (ER visits based on proportion ER visits/total visits | ||||||||||
| Physicians were placed in groups based on the following hierarchy: 1 HSO, 2 CHC, 3 FHN, 4 FHG, 5 FFS |
||||||||||
| Physicians in HSO or CHC do not have reliable or useful OHIP claims data for these measures. | ||||||||||
Selection bias is another issue that needs to be addressed. Physicians self-selected into the various payment models based on their own priorities and preferences and perceived benefits or risks of the models. Because the study took place during an early, introductory phase of the implementation of the FHN and FHG models, our sample is limited to the early adopters. It is quite possible that these physicians represent those who were either most likely to benefit from change or most dissatisfied with FFS. If this interpretation is correct, the positive findings of the study in terms of income and work satisfaction might be attenuated for those physicians making the change later on.
Conclusions
There is sufficient overlap at the individual level in both the work satisfaction and income results to support the notion that some physicians will enjoy both financial success and a high level of work satisfaction in each of the different models. However, the results of this study show that for some physicians, there is a benefit in moving to a non-FFS model. Given the significant challenges that Ontario faces in the recruitment and retention of FPs, the availability of a menu of payment models that may be attractive to physicians with different practice styles may help both to attract new physicians and also to retain those currently in practice (Shortt et al. 2005).
We limited our focus to the impact of primary care reforms on physicians, as uptake of reformed models will require the enthusiastic participation of this key professional group if it is to succeed. Evaluation of the impact of the various practice models on a wide range of process and outcome measures, including access and quality of care, is required as primary care reform continues to evolve.
Satisfaction au travail et satisfaction financière : impact de la réforme des soins de santé primaires sur les médecins, en Ontario
Résumé
En Ontario, les gouvernements ont promis aux médecins de famille que leur participation à la réforme des soins de santé primaires comporterait des avantages à la fois financiers et professionnels. Nous avons comparé la satisfaction au travail, le revenu et les régimes de travail de médecins de famille œuvrant dans divers modèles de pratique, afin de déterminer si les avantages prévus se sont effectivement matérialisés. Cette étude comptait sur la participation de 332 médecins de famille en Ontario œuvrant selon cinq modèles de prestation de soins. Nous avons tenu compte de données de sondage déclarées volontairement par les médecins ainsi que de données administratives provenant de l'Institut de recherche en services de santé (IRSS) et de l'Agence du revenu du Canada. Les médecins de famille qui travaillent selon des modèles autres que la rémunération à l'acte (RAA) ont indiqué de meilleurs taux de satisfaction au travail que ceux qui fonctionnent selon la RAA. Avant l'instauration de la réforme des soins de santé primaires, les revenus entre les groupes étaient similaires. Le revenu des médecins qui travaillent dans les réseaux de santé familiale a augmenté de 30 pour cent et celui des médecins qui travaillent dans les groupes de santé familiale a augmenté de 10 pour cent, tandis que les médecins qui travaillent selon la RAA ont vu peu de changement ou une diminution de leur revenu. Les fluctuations de revenu déclarées volontairement ne sont pas fiables, car seulement 47 pour cent des médecins ont indiqué avec précision si leur revenu s'était maintenu, avait augmenté ou avait diminué. La présence d'une variété de modèles de rémunération (RAA ou non), qui sont conçus pour offrir aux médecins différents types et divers styles de pratique, peut s'avérer un outil pratique pour les gouvernements, car elle permet d'aborder la question du recrutement et du maintien en poste des médecins.
About the Author(s)
Michael E. Green, MD, MPH, CCFP, Associate Professor, Departments of Family Medicine & Community Health and Epidemiology, Centre for Health Services and Policy Research, Centre for Studies in Primary Care, Queen's University, Kingston, ON
William Hogg, MD, BSC (HONS), MSC, MCISC, CCFP, FCFP, Professor, Department of Family Medicine, Director, CT Lamont Primary Health Care Research Centre, Elizabeth Bruyère Research Institute, Principal Scientist, Institute for Population Health, University of Ottawa, Ottawa, ON
David Gray, PHD, Professor, Department of Economics, University of Ottawa, Ottawa, ON
Doug Manuel, MD, MSC, FRCPC, Senior Scientist, Ottawa Hospital Research Institute, PHAC/CIHR Chair in Applied Public Health Sciences, Associate Professor, Departments of Family Medicine and Epidemiology, Community Medicine, University of Ottawa, Adjunct Scientist, Institute for Clinical Evaluative Sciences, Ottawa ON
Michelle Koller, BA, MA, Former Research Associate, Centre for Health Services and Policy Research, Department of Community Health and Epidemiology, Queen's University, Kingston, ON
Sarah Maaten, MSC, Research Associate, Institute for Clinical Evaluative Sciences, Toronto, ON
Yan Zhang, Economist, Small Area and Administrative Data Division, Statistics Canada, Ottawa, ON
Samuel E.D. Shortt, MD, PHD, FCFP, Former Professor, Department of Community Health and Epidemiology, Former Director, Centre for Health Services and Policy Research, Queen's University, Director, Knowledge Transfer and Practice Policy, Canadian Medical Association, Ottawa, ON
Correspondence may be directed to: Dr. Michael E. Green, Assistant Professor, Depts. of Family Medicine and Community Health and Epidemiology, Centre for Health Services and Policy Research, Queen's University, Abramsky Hall, 3rd floor, 21 Arch St., Kingston, ON K7L 3N6; tel.: 613-533-6358; e-mail: mg13@post.queensu.ca.
Acknowledgment
This project was supported by a Primary Health Care Transition Fund Grant from the Ontario Ministry of Health and Long-Term Care. We would also like to thank Dr. W. Rosser, Dr. G. Viner, Dr. S. McGuire, Dr. G. Wells and Jackie Schultz for their assistance and input.References
Asch, S., S.E. Connor, E.G. Hamilton and S.A. Fox. 2000. "Problems in Recruiting Community-Based Physicians for Health Services Research." Journal of General Internal Medicine 15: 591–99.
Asch, D.A., M.K. Jedrziewski and N.A. Christakis. 1997. "Response Rates to Mail Surveys Published in Medical Journals." Journal of Clinical Epidemiology 50(10): 1129–36.
Baerlocher, M.O. 2006. "Happy Doctors? Satisfaction with Professional Life." Canadian Medical Association Journal 174(8): 1079.
Bovier, P. and T. Perneger. 2003. "Predictors of Work Satisfaction among Physicians." European Journal of Public Health 13(4): 299–305.
Canadian Institute for Health Information (CIHI). 2006. Pan-Canadian Primary Health Care Indicators: Report 1, Volumes 1 and 2. Ottawa: Author.
Cohen, M., B. Ferrier, C.A. Woodward and J. Brown. 2001. "Health Care System Reform: Ontario Family Physicians' Reactions." Canadian Family Physician 47: 1777–84.
Dillman, D.A. 1999. Mail and Internet Surveys: The Tailored Design Method. New York: John Wiley and Sons.
Field, T.S., C.A. Cadoret, M.L. Brown, M. Ford, S.M. Greene et al. 2002. "Surveying Physicians: Do Components of the ‘Total Design Approach’ to Optimizing Survey Response Rates Apply to Physicians?" Medical Care 40(7): 596–606.
Grembowski, D., C.M. Ulrich, D. Paschane, P. Diehr, W. Katon et al. 2003. "Managed Care and Primary Physician Satisfaction." Journal of the American Board of Family Practitioners 16: 383–93.
Grol, R., H. Mokkink, A. Smits, J. Van Eijk, P. Mesker and J. Mesker-Niesten. 1985. "Work Satisfaction of General Practitioners and the Quality of Patient Care." Family Practice 2: 128–35.
Hunter, D.J.W., S.E.D. Shortt, P.M. Walker and M. Godwin. 2004. "Family Physician Views about Primary Care Reform in Ontario: A Postal Questionnaire." BMC Family Practice 5(2). Retrieved May 17, 2009. <http://www.biomedcentral.com/1471-2296/5/2>.
Hutchison, B. 2004. "Primary Health Care Renewal in Canada: Are We Nearly There?" In R. Wilson, S.E.D. Shortt and J. Dorland, eds., Implementing Primary Care Reform: Barriers and Facilitators (pp. 111–28). Kingston, ON: McGill-Queen's University Press.
Hutchison, B., J. Abelson and J. Lavis. 2001. "Primary Care in Canada: So Much Innovation, So Little Change." Health Affairs 20(3): 116–31.
Lichtenstein, R. 1984. "Measuring the Job Satisfaction of Physicians in Organized Settings." Medical Care 22(1): 56–68.
Macinko, J., B. Starfield and L. Shi. 2003. "The Contribution of Primary Care Systems to Health Outcomes within the Organization for Economic Development (OECD) Countries, 1970–1998." Health Services Research 38(3): 831–65.
Martin, S. 2003. "Fee-for-Service v. Salary: The Debate Is Heating Up." Canadian Medical Association Journal 169(7): 701.
Murray, A., J.E. Montgomery, H. Chang, W.H. Rogers, T. Inui and D.G. Safran. 2001. "Doctor Discontent: A Comparison of Physician Satisfaction in Different Delivery System Settings, 1986 and 1997." Journal of General Internal Medicine 16: 451–59.
Nadler, E.S., S. Sims, P.H. Tyrance, D.G. Fairchild, T.A. Brennan et al. 1999. "Does a Year Make a Difference? Changes in Physician Satisfaction and Perception in an Increasingly Capitated Environment." American Journal of Medicine 107: 38–44.
Nicholson, S. and N. Souleles. 2001. Physician Income Expectations and Specialty Choice. NBER Working Paper #8536. Cambridge, MA: National Bureau of Economic Research.
Nicholson, S. and N. Souleles. 2002. Physician Income Prediction Errors: Sources and Implications for Behaviour. NBER Working Paper #8907. Cambridge, MA: National Bureau of Economic Research.
Romanow, R.J. 2002. "Primary Health Care and Prevention." In Building on Values: The Future of Health Care in Canada (pp. 115–35). Saskatoon: Commission on the Future of Health Care in Canada.
Shortt, S.E.D. 2004. "Primary Care Reform: Is There a Clinical Rationale?" In R. Wilson, S.E.D. Shortt and J. Dorland, eds., Implementing Primary Care Reform: Barriers and Facilitators (pp. 11–24). Kingston, ON: McGill-Queen's University Press.
Shortt, S.E.D., M.E. Green and C. Keresztes. 2005. "Family Physicians for Ontario: An Approach to Production and Retention Policy." Canadian Public Policy 21(2): 207–21.
Simoens, S., A. Scott and B. Sibbald. 2002. "Job Satisfaction, Work-Related Stress and Intentions to Quit of Scottish GPs." Scottish Medical Journal. Retrieved May 17, 2009. <http://www.smj.org.uk/0802/job_satisfaction.htm>.
Spurgeon, D. 2003. "Medicine, the Unhappy Profession?" Canadian Medical Association Journal 168(6): 751–52.
Starfield, B. and L. Shi. 2002. "Policy Relevant Determinants of Health: An International Perspective." Health Policy 60(3): 201–18.
Sullivan, P. and L. Buske. 1998. "Results from CMA's Huge 1998 Physician Survey Point to a Dispirited Profession." Canadian Medical Association Journal 159(5): 525–28.
Watson, D.E., A.M. Broemeling, R. Reid and C. Black. 2004. "A Results-Based Logic Model for Primary Health Care: Laying an Evidence-Based Foundation to Guide Performance Measurement, Monitoring and Evaluation." Vancouver: Centre for Health Services and Policy Research, University of British Columbia. Retrieved May 17, 2009. <http://www.chspr.ubc.ca/files/publications/2004/chspr04-19.pdf>.
Footnotes
The views reflected here are those of the authors and not of the Ministry of Health and Long-Term Care.Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed