Healthcare Policy
A Comparison of Drug Coverage in Alberta Before and After the Introduction of the National Common Drug Review Process
Abstract
Objective: The integration of the Common Drug Review (CDR) was a substantial change for Canada's public drug plans. Detailed comparisons of time-to-listing and proportion of medications covered by the province of Alberta's drug plans within the context of the CDR process have not been rigorously conducted.
Methods: New drugs approved by Health Canada were identified five years prior to the CDR's first recommendation (May 2004) and five years after. The time-to-listing and proportion of new drugs covered on the Alberta Health and Wellness Drug Benefit List (AHWDBL) was compared between these periods. The level of agreement between CDR recommendations and coverage in Alberta was calculated using a kappa score.
Results: Two hundred and twenty new drugs were identified and met the study eligibility criteria (118 pre-CDR, 102 post-CDR). The median time-to-listing was 312 vs. 524 days in the pre-CDR and post-CDR periods, respectively, with the difference largely driven by time from notice of compliance (NOC) to the CDR recommendation. The level of agreement between 73 drugs with CDR recommendations and coverage in Alberta was fair (kappa 0.55).
Conclusion: Following the implementation of the CDR, the proportion of drugs covered has decreased and overall median time-to-listing of new drugs has increased in the province of Alberta. For drugs listed on the AHWDBL, the proportion of time attributable to the CDR process (NOC to CDR recommendation) was 63% of the overall time-to-listing.
Pharmaceutical coverage in Canada is an important topic to many Canadians and has increasingly received significant media coverage as healthcare budgets are expanding while allocations are being squeezed. The pharmaceutical reimbursement system in Canada comprises a mixture of public and private drug plans. Currently, 19 publicly funded drug plans exist across the country, all of which vary in their scope and coverage (Gregoire et al. 2001). Some plans are universal, meaning they cover the entire population they serve; other plans are specific to a cohort, such as seniors. Federal public plans cover specific groups, including First Nations and Inuit individuals, federal inmates, members of the Canadian Armed Forces, immigrants and refugees, members of the Royal Canadian Mounted Police and veterans. Each province has its own public drug plan, and the variation in drug coverage in these plans has been studied extensively (Anis et al. 2001; Gregoire et al. 2001; MacDonald and Potvin 2004; Morgan et al. 2009). Each drug plan is responsible for deciding which drugs will be covered for their respective beneficiaries.
The Common Drug Review (CDR), which is administered by the Canadian Agency for Drugs and Technologies in Health (CADTH 2009b), was introduced in Canada to establish a centralized drug review process that would reduce duplication of drug reviews within government-sponsored drug plans (CADTH 2009a,d; McMahon et al. 2006; Tierney and Manns 2008). The CDR process is intended to be transparent and rigorous, and to provide evidence-based recommendations to participating publicly funded drug plans in Canada. Provinces were free to participate, or not, in the CDR process. The province of Quebec opted not to participate, while all other provinces opted in. The CDR uses a reproducible framework whereby a review team consisting of internal and external experts across various disciplines (e.g., epidemiology, pharmacy, medicine, health economics and information science) conducts a systematic review to critically appraise the clinical and economic importance of each drug reviewed. Following this extensive review, a report is provided to the Canadian Drug Expert Advisory Committee (CEDAC), which is responsible for assessing the drug's clinical and cost effectiveness compared to existing treatment options and providing a recommendation for formulary listing to the provinces.
Although the CDR was established in 2002, it made its first recommendation on May 27, 2004. CDR recommendations may include listing the drug without any restriction, not listing the drug, listing the drug in a similar manner to other drugs in the same class, or listing the drug with criteria or conditions. Although a clear formulary recommendation is made for each drug reviewed, each of the participating drug plans is still required to make a final decision for its respective formulary. Participating drug plans are reported to agree with CEDAC recommendations approximately 90% of the time (CADTH 2009d).
As previously noted, significant differences in drug coverage exist across plans (Anis et al. 2001; Gregoire et al. 2001; MacDonald and Potvin 2004; Morgan et al. 2009), and although these differences may result in vastly different costs to patients (Demers et al. 2008), the majority of top-selling drugs are covered under all provincial plans (Morgan et al. 2009). Prior to the implementation of the CDR, each provincial and territorial jurisdiction was entirely responsible for its own drug reviews based on its own criteria. Each jurisdiction would perform its own evaluation of a drug submitted by the manufacturer for its respective government-sponsored drug plan. Thus, it is important to describe and analyze the differences among these time periods.
To our knowledge, a comparison of the time to drug reimbursement before and after the introduction of the CDR has not been rigorously conducted. Tierney and Manns (2008) concluded that the time from Health Canada's approval of a new drug to its listing on drug plan formularies has not changed with the implementation of the CDR process, based on a study by Kallah (2006). Skinner and Rovere (2009) have described federal and provincial delays in accessing new drugs approved by Health Canada, and Wyatt and colleagues (2008) have compared drug reimbursement decisions of drugs reviewed by the CDR within a national and international context.
We aimed to compare the time-to-listing and the proportion of new drug entities, both new chemical entities and new combination products, covered by Alberta's government-sponsored drug plans that received a notice of compliance (NOC) by Health Canada's Therapeutic Product Directorate five years prior to and five years following the CDR's first recommendation. We believe that describing Alberta's experience provides a useful case study for other researchers and policy makers interested in Canada's CDR process, especially those involved in Alberta's process. Furthermore, this topic is relevant given that several provinces, including Alberta, are currently undergoing various pharmaceutical policy reforms, one of which is the drug review process.
Methods
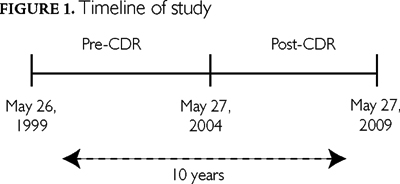
New drug entities that received an NOC between May 26, 1999, and May 27, 2009, were identified using Health Canada's Drug Products Database (DPD) available on its website (Health Canada 2009). Figure 1 illustrates the study timeline. Data extracts of the active and inactive DPD were imported, merged and analyzed using Stata/IC 10.1 (StataCorp LP, College Station, TX, USA). Exclusions included generic drugs, over-the-counter drugs, drugs scheduled for ethical use (i.e., do not require a prescription but are usually prescribed by a medical practitioner, e.g., nitroglycerine), homeopathic products, veterinary use products, neoplastic agents, vitamins, blood products and drugs withdrawn from the Canadian market. The date of the first NOC issued was used, or date of marketing notification if an NOC date was missing; thus, an NOC due to change in manufacturer, approved indications, route of administration or manufacturing processes was excluded. New drug entities were identified using the second portion (five digits) of the unique 10-digit active ingredient group number, which identifies the unique products with unique groups of active ingredients. These groups may have various strengths and will therefore be captured only once. These new drug entities were categorized into two mutually exclusive categories: five years prior to (May 26, 1999, to May 26, 2004) and five years after (May 27, 2004, to May 27, 2009) the CDR's first recommendation.
Alberta has several government-sponsored drug plans, including coverage for seniors, social services, child health benefits and others. For this analysis, only drugs listed on the Alberta Health and Wellness Drug Benefit List (AHWDBL) were included. Drug benefit lists were collected from April 1999 to April 2010 and combined into a single PDF document. The date of coverage for the new drug entities receiving an NOC in the pre-specified pre-CDR and post-CDR time periods was determined using the advanced search function in Adobe Acrobat 8 Professional Version 8.1.2 (Adobe Systems Inc., San Jose, California). We considered drug-listing decisions up until April 2010 to allow a reasonable lag time between the last CDR recommendation and formulary coverage. Drugs were further categorized into three mutually exclusive groups: drugs that were listed as a full benefit, drugs that were listed with a set of pre-specified criteria (restricted or special authorization products) and drugs that were not listed.
CDR recommendations completed as of May 27, 2009, were identified using the CDR drug database available on the CADTH website (2009c). If a drug had more than one recommendation (i.e., initial submission and repeat submission) for the same indication, only the latest recommendation was used in the analysis. For drug products that contained the identical active ingredient but were reviewed by CDR more than once because of a new indication or different manufacturer, only the first submission was included (e.g., tramadol).
Analysis
New drugs approved in the pre-CDR and post-CDR were classified according to their World Health Organization Anatomical Therapeutic and Chemical Classification (WHO 2009) and their AHWDBL status. Drugs with a completed CDR recommendation before May 27, 2009, were tabulated in order of calendar date of CEDAC recommendation. The proportions of new drugs according to coverage status (full benefit, restricted/special authorization and not listed) were stratified by study period and compared using chi-squared tests.
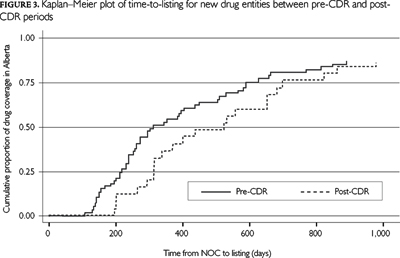
The median time from the date of Health Canada's NOC to listing on the AHWDBL was calculated for all drugs in the pre-CDR period and the post-CDR period. Median time-to-listing was the most appropriate measure of the central tendency, as opposed to the mean, owing to the skewed distribution of this variable. To further explore the notion of time-to-listing, we divided the time frames into two periods: time from NOC to CDR recommendation (i.e., federal time) and time from CDR recommendation to listing on the AHWDBL (i.e., provincial time). A Kaplan–Meier plot was used to describe the time-to-listing data, and a log-rank test was used to compare the time-to-event curves between the two study periods. Only drugs that were ultimately listed on the AHWDBL were included in the survival analysis. Kappa scores were used to measure the proportion of non-random agreement between CDR recommendations and AHWDBL status. In addition, a subgroup analysis of the change in time-to-listing between study periods was evaluated separately for drugs with full benefit status and those drugs with a restricted/special authorization status.
All analyses used two-sided hypothesis tests with an alpha level of 0.05, considered statistically significant. Analyses were performed using Stata/IC 10.1.
Results
There were 220 new drug entities identified that received an NOC between May 26, 1999, and May 27, 2009, and met the study eligibility criteria. The drug names according to therapeutic class and study period are listed in Table 1. One hundred and eighteen (54%) drugs were identified pre-CDR's first recommendation and 102 (46%) were identified post-CDR. Alberta listed 52% (61/118) of new drug entities in the period five years pre-CDR compared to 25% (25/102) in the five years post-CDR. Table 2 shows the number of drugs that were listed, listed with a restriction and not listed in Alberta according to the study period.
| Table 1. New drug entities according to ATC code, stratified by study period (bolded medications are listed on Alberta's government-sponsored drug plans) | ||||
| Pre-CDR (n=118) | Post-CDR (n=102) | |||
| Therapeutic class (ATC) | Drug | Date of NOC | Drug | Date of NOC |
| Alimentary tract and metabolism | orlistat | 03-Jun-99 | laronidase | 31-May-04 |
| rosiglitazone | 21-Mar-00 | rosiglitazone/glimepiride | 21-Oct-04 | |
| pioglitazone | 17-Aug-00 | insulin aspart/insulin aspart protamine | 25-Feb-05 | |
| sibutramine | 28-Dec-00 | insulin detemir | 29-Sep-05 | |
| rabeprazole | 07-May-01 | insulin glulisine | 12-Apr-06 | |
| insulin aspart | 18-Jul-01 | alglucosidase | 14-Aug-06 | |
| esomeprazole | 17-Aug-01 | idursulfase | 13-Jun-07 | |
| glimepiride | 25-Jan-02 | aprepitant | 24-Aug-07 | |
| nateglinide | 13-Feb-02 | sitagliptin | 14-Dec-07 | |
| insulin glargine | 03-Apr-02 | methylnaltrexone | 28-Mar-08 | |
| rosiglitazone/metformin | 13-Feb-03 | |||
| agalsidase beta | 23-Jan-04 | |||
| agalsidase alfa | 06-Feb-04 | |||
| miglustat | 31-Mar-04 | |||
| Blood and blood-forming organs | eptifibatide | 11-Jun-99 | dabigatran | 10-Jun-08 |
| tirofiban | 19-Aug-99 | rivaroxaban | 15-Sep-08 | |
| lepirudin | 01-Oct-99 | romiplostim | 19-Feb-09 | |
| argatroban | 04-Jun-01 | |||
| tenecteplase | 17-Oct-01 | |||
| fondaparinux | 13-Jun-02 | |||
| hydroxyethylstarch | 08-Jul-02 | |||
| darbepoetin alfa | 02-Aug-02 | |||
| treprostinil | 04-Oct-02 | |||
| bivalirudin | 09-Oct-02 | |||
| drotrecogin alfa | 31-Jan-03 | |||
| Cardiovascular system | eprosartan | 07-Jul-99 | eprosartan/hydrochlorothiazide | 08-Jun-04 |
| telmisartan | 26-Aug-99 | niacin/lovastatin | 31-Aug-05 | |
| bisoprolol | 08-Nov-99 | amlodipine/atorvastatin | 17-Nov-05 | |
| erbesartan/hydrochlorothiazide | 29-Feb-00 | pravastatin/acetylsalicylic acid | 07-Dec-05 | |
| valsartan/hydrochlorothiazide | 15-Mar-00 | ramipril/hydrochlorothiazide | 13-Jul-06 | |
| ibutilide | 14-Jul-00 | sitaxsentan | 30-May-07 | |
| candesartan/hydrochlorothiazide | 18-Jun-01 | nesiritide | 08-Nov-07 | |
| telmisartan/hydrochlorothiazide | 15-Aug-01 | aliskiren | 14-Nov-07 | |
| bosentan | 30-Nov-01 | ambrisentan | 20-Mar-08 | |
| perindopril/hydrochlorothiazide | 18-Oct-02 | nifedipine/acetylsalicylic acid | 11-Jul-08 | |
| rosuvastatin | 18-Feb-03 | olmesartan | 28-Oct-08 | |
| ezetimibe | 12-May-03 | olmesartan/hydrochlorothiazide | 21-Nov-08 | |
| eplerenone | 26-Feb-09 | |||
| Dermatologicals | clindamycin/benzoyl peroxide | 11-Dec-00 | ||
| mequinol/tretinoin | 17-Jan-01 | |||
| eflornithine | 10-May-01 | |||
| calcipotriol/betamethasone | 11-Jul-01 | |||
| pimecrolimus | 19-Mar-03 | |||
| ciclopirox | 19-Apr-04 | |||
| Genito-urinary system and sex hormones | norethisterone/estrogen | 13-Mar-00 | oxybutynin | 22-Jun-04 |
| follitropin beta | 13-Jun-00 | desogestrel/ethinyl estradiol | 19-Aug-04 | |
| cabergoline | 30-Jun-00 | drospirenone/ethinyl estradiol | 10-Dec-04 | |
| medroxyprogesterone/estrogen | 16-Oct-00 | choriogonadotropin alfa | 16-Dec-04 | |
| alfuzosin | 21-Feb-02 | lutropin alfa | 24-Jun-05 | |
| norelgestromin/ethinyl estradiol | 20-Aug-02 | drospirenone/ethinyl estradiol | 08-Jul-05 | |
| human menopausal gonadotrophin | 02-Jul-03 | darifenacin | 14-Nov-05 | |
| dutasteride | 22-Jul-03 | trospium | 10-Jan-06 | |
| tadalafil | 17-Sep-03 | solifenacin | 20-Feb-06 | |
| butoconazole | 23-Dec-03 | |||
| vardenafil | 17-Mar-04 | |||
| levonorgestrel/ethinyl estradiol | 08-Apr-04 | |||
| etonogestrel/ethinyl estradiol | 11-May-04 | |||
| Systemic hormonal preparations excluding sex hormones | glucagon | 11-Jan-01 | teriparatide | 03-Jun-04 |
| doxercalciferol | 30-Apr-01 | cinacalcet | 09-Aug-04 | |
| ganirelix | 01-May-02 | paricalcitol | 31-Mar-05 | |
| cetrorelix | 13-Aug-03 | pegvisomant | 17-Oct-05 | |
| lanreotide | 17-Jul-06 | |||
| desmopressin | 08-Sep-06 | |||
| General anti-infectives for systemic use | abacavir | 04-Jun-99 | voriconazole | 20-Aug-04 |
| fosfomycin | 09-Jun-99 | fosamprenavir | 10-Dec-04 | |
| zanamivir | 02-Nov-99 | abacavir/lamivudine | 25-Jul-05 | |
| quinopristin/dalfopristin | 10-Dec-99 | emtricitabine | 21-Nov-05 | |
| oseltamivir | 23-Dec-99 | tipranavir | 21-Nov-05 | |
| moxifloxacin | 19-Oct-00 | emtricitabine/tenofovir | 06-Jan-06 | |
| lopinavir | 09-Mar-01 | entecavir | 16-Jun-06 | |
| linezolid | 02-Apr-01 | darunavir | 28-Jul-06 | |
| caspofungin | 19-Jul-01 | tigecycline | 14-Sep-06 | |
| zidovudine/lamivudine/abacavir | 17-Oct-01 | telbivudine | 28-Nov-06 | |
| valganciclovir | 03-May-02 | posaconazole | 26-Mar-07 | |
| palivizumab | 15-May-02 | micafungin | 22-May-07 | |
| tenofovir | 18-Mar-03 | maraviroc | 21-Sep-07 | |
| ertapenem | 12-May-03 | daptomycin | 24-Sep-07 | |
| telithromycin | 28-May-03 | efavirenz/emtricitabine/tenofovir | 15-Oct-07 | |
| enfuvirtide | 14-Jul-03 | anidulafungin | 14-Nov-07 | |
| adefovir | 27-Aug-03 | raltegravir | 27-Nov-07 | |
| atazanavir | 05-Dec-03 | etravirine | 27-Mar-08 | |
| ceftobiprole | 26-Jun-08 | |||
| Immunomodulating agents | daclizumab | 04-Jan-00 | adalimumab | 24-Sep-04 |
| leflunomide | 16-Mar-00 | alefacept | 06-Oct-04 | |
| basiliximab | 01-Sep-00 | mycophenolate | 04-Feb-05 | |
| peginterferon alfa-2b | 20-Oct-00 | efalizumab | 24-Oct-05 | |
| etanercept | 01-Dec-00 | abatacept | 29-Jun-06 | |
| sirolimus | 05-Jan-01 | natalizumab | 28-Sep-06 | |
| infliximab | 06-Jun-01 | temsirolimus | 21-Dec-07 | |
| aminolevulinic acid | 20-Jun-01 | lenalidomide | 17-Jan-08 | |
| imatinib | 19-Sep-01 | ustekinumab | 12-Dec-08 | |
| anakinra | 24-May-02 | |||
| peginterferon alfa-2b/ribavirin | 31-May-02 | |||
| peginterferon alfa-2a | 13-Aug-03 | |||
| pegfilgrastim | 12-Mar-04 | |||
| peginterferon alfa-2a/ribavirin | 10-May-04 | |||
| Musculo-skeletal system | zoledronic acid | 21-Aug-00 | alendronate/cholecalciferol | 03-Feb-06 |
| meloxicam | 31-Aug-00 | risedronate/calcium | 17-May-06 | |
| Nervous system | rizatriptan | 16-Jul-99 | eletriptan | 05-Aug-04 |
| oxcarbazepine | 13-Apr-00 | frovatriptan | 03-Sep-04 | |
| rivastigmine | 13-Apr-00 | memantine | 08-Dec-04 | |
| riluzole | 30-Aug-00 | atomoxetine | 24-Dec-04 | |
| entacapone | 08-May-01 | escitalopram | 24-Dec-04 | |
| mirtazapine | 18-May-01 | delta-9-tetrahydrocannabinol/cannabidiol | 15-Apr-05 | |
| methadone | 30-Jul-01 | pregabalin | 03-Jun-05 | |
| galantamine | 31-Jul-01 | tramadol/acetaminophen | 20-Jul-05 | |
| levetiracetam | 06-Mar-03 | sodium oxybate | 05-Aug-05 | |
| almotriptan | 29-Sep-03 | rasagiline | 17-Aug-06 | |
| mixed amphetamine salts | 23-Jan-04 | tramadol | 28-Sep-06 | |
| varenicline | 24-Jan-07 | |||
| acamprosate | 16-Mar-07 | |||
| buprenorphine/naloxone | 18-May-07 | |||
| ziprasidone | 27-Aug-07 | |||
| paliperidone | 26-Sep-07 | |||
| duloxetine | 01-Nov-07 | |||
| carbidopa/levodopa/entacapone | 18-Feb-08 | |||
| idebenone | 23-Jul-08 | |||
| desvenlafaxine | 04-Feb-09 | |||
| Respiratory system | salmeterol/fluticasone | 03-Sep-99 | omalizumab | 18-Nov-04 |
| formoterol/budesonide | 08-Feb-02 | nitric oxide | 23-Sep-05 | |
| tiotropium bromide | 20-Nov-02 | ciclesonide | 11-Sep-06 | |
| fluticasone | 14-Aug-07 | |||
| Sensory organs | verteporfin | 31-May-00 | pegaptanib | 02-May-05 |
| travoprost | 09-Nov-01 | travoprost/timolol | 17-Mar-06 | |
| bimatoprost | 24-May-02 | ranibizumab | 26-Jun-07 | |
| latanoprost/timolol | 15-Oct-02 | nepafenac | 17-Apr-08 | |
| brimonidine/timolol | 09-Dec-03 | |||
| ciprofloxacin/dexamethasone | 10-May-04 | |||
| Various | sevelamer | 24-Feb-00 | palifermin | 09-Dec-05 |
| fomepizole | 30-Nov-00 | lanthanum | 17-Oct-06 | |
| thyrotrophin | 31-May-02 | deferasirox | 18-Oct-06 | |
| rasburicase | 29-Oct-03 | |||
| Table 2. Summary of new drug entity coverage in Alberta, stratified by 5 years pre-CDR and 5 years post-CDR | ||
| Variable | Pre-CDR n (%) | Post-CDR n (%) |
| Number of drugs listed or not listed | ||
| Listed | 61 (51%) | 25 (25%) |
| Full benefit | 24 (20%) | 14 (14%) |
| Restricted | 37 (31%) | 11 (11%) |
| Not listed | 57 (48%) | 77 (75%) |
| Time from NOC to listing (n=86) | ||
| Median (days) | 312 | 524 |
| Range (days) | 106–2,821 | 198–1,450 |
| Average (days) | 551 | 581 |
| Full benefit (n=38) | ||
| Median (days) | 296 | 544 |
| Range (days) | 133–2,821 | 202–1,450 |
| Average (days) | 527 | 607 |
| Restricted (n=48) | ||
| Median (days) | 353 | 440 |
| Range (days) | 106–2,297 | 198–1,007 |
| Average (days) | 567 | 548 |
| Time from NOC to listing for drugs listed with a CDR recommendation (n=24) | ||
| Median (days) | n/a | 482 |
| Range (days) | n/a | 198–1,450 |
| Average (days) | n/a | 569 |
| Time from NOC decision to CDR recommendation for listed drugs (n=24) | ||
| Median (days) | n/a | 239 |
| Range (days) | n/a | 93–1,249 |
| Average (days) | n/a | 356 |
| Time from NOC decision to CDR recommendation for non-listed drugs (n=49) | ||
| Median (days) | n/a | 278 |
| Range (days) | n/a | 135–1,272 |
| Average (days) | n/a | 356 |
| Time from CDR decision to listing (n=24) | ||
| Median (days) | n/a | 167 |
| Range (days) | n/a | 15–677 |
| Average (days) | n/a | 213 |
The CDR provided 133 drug coverage recommendations as of May 27, 2009; 73 of these reviews met our eligibility criteria (Table 3). We excluded 39 of the 133 drugs for the following reasons: duplicate generics (n=26); neoplastic agents (n=7); market withdrawal (n=1); manufacturer change or formulation change (n=5). A further 21 drugs were excluded because they were issued an NOC prior to CDR's first recommendation (May 27, 2004); thus, the manufacturers may have submitted an application to be listed directly to Alberta Health and Wellness. Of the 73 drugs that received an NOC in the post-CDR period and were used in the analysis, CEDAC recommend 41 of these to be listed on the participating public drug plans: four recommended to "list," nine recommended to "list in a similar manner to other drugs in class" and 28 recommended to "list with criteria/condition." Table 4 shows the frequency of drugs in each coverage classification for the province of Alberta by CDR recommendation.
| Table 3. CDR recommendations of study drugs in order of calendar date of recommendation until May 27, 2009 (n=73) | ||||
| Drugs reviewed | Date of NOC | Date of recommendation | CDR recommendation | |
| Generic name | Brand name | |||
| eprosartan/hydrochlorothiazide | Teveten Plus | 08-Jun-04 | 15-Dec-04 | List in a similar manner to other drugs in class |
| teriparatide | Forteo | 03-Jun-04 | 22-Dec-04 | Do not list |
| adalimumab | Humira | 24-Sep-04 | 11-Feb-05 | List with criteria/condition |
| cinacalcet | Sensipar | 09-Aug-04 | 23-Mar-05 | Do not list |
| eletriptan | Relpax | 05-Aug-04 | 23-Mar-05 | Do not list |
| voriconazole | Vfend | 20-Aug-04 | 14-Apr-05 | List with criteria/condition |
| fosamprenavir | Telzir | 10-Dec-04 | 16-Jun-05 | List in a similar manner to other drugs in class |
| drospirenone/ethinyl estradiol | Yasmin | 10-Dec-04 | 16-Jun-05 | List |
| mycophenolate | Myfortic | 04-Feb-05 | 08-Jul-05 | List in a similar manner to other drugs in class |
| laronidase | Aldurazyme | 31-May-04 | 14-Jul-05 | Do not list |
| atomoxetine | Strattera | 24-Dec-04 | 28-Sep-05 | Do not list |
| memantine | Ebixa | 08-Dec-04 | 23-Nov-05 | Do not list |
| abacavir/lamivudine | Kivexa | 25-Jul-05 | 07-Dec-05 | List in a similar manner to other drugs in class |
| pregabalin | Lyrica | 03-Jun-05 | 25-Jan-06 | Do not list |
| omalizumab | Xolair | 18-Nov-04 | 07-Mar-06 | Do not list |
| niacin/lovastatin | Advicor | 31-Aug-05 | 26-Apr-06 | List |
| insulin aspart/insulin aspart protamine | Novomix | 25-Feb-05 | 26-Apr-06 | Do not list |
| tipranavir | Aptivus | 21-Nov-05 | 17-May-06 | List with criteria/condition |
| amlodipine/atorvastatin | Caduet | 17-Nov-05 | 17-May-06 | List with criteria/condition |
| pegaptanib | Macugen | 02-May-05 | 25-May-06 | Do not list |
| insulin detemir | Levemir | 29-Sep-05 | 02-Aug-06 | Do not list |
| pegvisomant | Somavert | 17-Oct-05 | 02-Aug-06 | Do not list |
| travoprost/timolol | Duotrav | 17-Mar-06 | 24-Aug-06 | List with criteria/condition |
| efalizumab | Raptiva | 24-Oct-05 | 24-Aug-06 | List with criteria/condition |
| trospium | Trosec | 10-Jan-06 | 24-Aug-06 | List with criteria/condition |
| alefacept | Amevive | 06-Oct-04 | 27-Sep-06 | Do not list |
| alendronate/cholecalciferol | Fosavance | 03-Feb-06 | 27-Sep-06 | Do not list |
| ciclesonide | Alvesco | 11-Sep-06 | 20-Dec-06 | List |
| escitalopram | Cipralex | 24-Dec-04 | 24-Jan-07 | Do not list |
| solifenacin | Vesicare | 20-Feb-06 | 24-Jan-07 | Do not list |
| darunavir | Prezista | 28-Jul-06 | 14-Feb-07 | List with criteria/condition |
| rasagiline | Azilect | 17-Aug-06 | 28-Mar-07 | Do not list |
| deferasirox | Exjade | 18-Oct-06 | 19-Apr-07 | List with criteria/condition |
| tramadol/acetaminophen | Tramacet | 20-Jul-05 | 17-May-07 | Do not list |
| ramipril/hydrochlorothiazide | Altace | 13-Jul-06 | 14-Jun-07 | List |
| alglucosidase | Myozyme | 14-Aug-06 | 14-Jun-07 | List with criteria/condition |
| abatacept | Orencia | 29-Jun-06 | 27-Jun-07 | List with criteria/condition |
| lanreotide | Somatuline | 17-Jul-06 | 19-Jul-07 | List in a similar manner to other drugs in class |
| varenicline | Champix | 24-Jan-07 | 16-Aug-07 | List with criteria/condition |
| tramadol | Zytram | 28-Sep-06 | 26-Sep-07 | Do not list |
| delta-9-tetrahydrocannabinol/cannabidiol | Sativex | 15-Apr-05 | 26-Sep-07 | Do not list |
| telbivudine | Sebivo | 28-Nov-06 | 26-Sep-07 | Do not list |
| entecavir | Baraclude | 16-Jun-06 | 28-Nov-07 | List with criteria/condition |
| idursulfase | Elaprase | 13-Jun-07 | 19-Dec-07 | Do not list |
| posaconazole | Posanol | 26-Mar-07 | 30-Jan-08 | Do not list |
| lanthanum | Fosrenol | 17-Oct-06 | 30-Jan-08 | Do not list |
| aprepitant | Emend | 24-Aug-07 | 20-Feb-08 | List with criteria/condition |
| ranibizumab | Lucentis | 26-Jun-07 | 27-Mar-08 | List with criteria/condition |
| acamprosate | Campral | 16-Mar-07 | 27-Mar-08 | List with criteria/condition |
| efavirenz/emtricitabine/tenofovir | Atripla | 15-Oct-07 | 17-Apr-08 | List with criteria/condition |
| raltegravir | Isentress | 27-Nov-07 | 14-May-08 | List with criteria/condition |
| paliperidone | Invega | 26-Sep-07 | 28-May-08 | Do not list |
| sitagliptin | Januvia | 14-Dec-07 | 18-Jun-08 | Do not list |
| aliskiren | Rasilez | 14-Nov-07 | 25-Jun-08 | Do not list |
| etravirine | Intelence | 27-Mar-08 | 14-Aug-08 | List with criteria/condition |
| duloxetine | Cymbalta | 01-Nov-07 | 14-Aug-08 | List with criteria/condition |
| ziprasidone | Zeldox | 27-Aug-07 | 14-Aug-08 | List with criteria/condition |
| buprenorphine/naloxone | Suboxone | 18-May-07 | 24-Sep-08 | List with criteria/condition |
| daptomycin | Cubicin | 24-Sep-07 | 24-Sep-08 | Do not list |
| carbidopa/levodopa/entacapone | Stalevo | 18-Feb-08 | 16-Oct-08 | List in a similar manner to other drugs in class |
| maraviroc | Celsentri | 21-Sep-07 | 12-Nov-08 | List with criteria/condition |
| ambrisentan | Volibris | 20-Mar-08 | 17-Dec-08 | List with criteria/condition |
| emtricitabine/tenofovir | Truvada | 06-Jan-06 | 17-Dec-08 | List with criteria/condition |
| rivaroxaban | Xarelto | 15-Sep-08 | 17-Dec-08 | List with criteria/condition |
| methylnaltrexone | Relistor | 28-Mar-08 | 28-Jan-09 | Do not list |
| dabigatran | Pradax | 10-Jun-08 | 28-Jan-09 | Do not list |
| sodium oxybate | Xyrem | 05-Aug-05 | 28-Jan-09 | Do not list |
| sitaxsentan | Thelin | 30-May-07 | 28-Jan-09 | Do not list |
| insulin glulisine | Apidra | 12-Apr-06 | 19-Feb-09 | List in a similar manner to other drugs in class |
| natalizumab | Tysabri | 28-Sep-06 | 25-Feb-09 | List with criteria/condition |
| darifenacin | Enablex | 14-Nov-05 | 16-Apr-09 | List with criteria/condition |
| olmesartan/hydrochlorothiazide | Olmetec Plus | 21-Nov-08 | 27-May-09 | List in a similar manner to other drugs in class |
| olmesartan | Olmetec | 28-Oct-08 | 27-May-09 | List in a similar manner to other drugs in class |
| Table 4. Alberta Health and Wellness coverage, stratified by CDR recommendation | ||||
| Alberta drug benefit status | ||||
| CDR recommendation | Full benefit | Restricted/Special authorization | Not listed | Total |
| List | 3 (75%) | 0 | 1 (25%) | 4 |
| List in a similar manner | 5 (56%) | 1 (11%) | 3 (33%) | 9 |
| List with criteria/condition | 5 (18%) | 10 (36%) | 13 (46%) | 28 |
| Do not list | 0 | 0 | 32 (100%) | 32 |
| Total | 13 | 11 | 49 | 73 |
| * Chi-squared test, p value < 0.001 | ||||
There were 41 drugs recommended to be listed in some manner by the CDR, of which 24 (59%) were approved for listing on the AHWDBL. All drugs that received a "do not list" recommendation from the CDR were not listed on the AHWDBL (32/32). The kappa score was 0.55 when CDR recommendations were classified as "to list" (regardless of criteria) or "not to list," and drugs on the AHWDBL were classified as "listed" (with or without criteria) or "not listed." This level of agreement between CDR recommendations and AHWDBL would be considered fair to good (Fleiss 1981).
The median time-to-listing from NOC issue was 312 days (n=61; interquartile range [IQR] = 219 to 588 days) in the pre-CDR period (average 551 days; min. 106 days; max. 2,821 days) and 524 days (n=25; IQR=315 to 700 days) in the post-CDR period (average 581 days; min. 198 days; max. 1,450 days) (Table 2 and Figure 2). Figure 2 illustrates the increase in time-to-listing for drugs issued an NOC post-CDR implementation. There are noticeably fewer outliers in the post-CDR period. The Kaplan–Meier plot provides a comparison between the pre-CDR and post-CDR periods, and a log-rank test failed to demonstrate a statistically significant difference between the two periods (p value = 0.53) (Figure 3). Among drugs that received full benefit status, the median time-to-listing was 248 days longer following the implementation of the CDR process (period 1: n=24; median=296; IQR=206 to 580 and period 2: n=14; median = 544; IQR=314 to 700). The median time-to-listing for drugs that were listed as restricted or available via special authorization was 87 days longer (period 1: n=37; median=353; IQR=236 to 588 and period 2: n=11; median=440; IQR=315 to 825).
Table 2 provides the median, mean and ranges for time-to-listing for drugs with a CDR recommendation broken into two time frames: time from NOC to CDR recommendation, and time from CDR recommendation to listing on the AHWDBL. The median time from NOC to CDR recommendation was 275 days (mean: 356 days) for all 73 drugs with a CDR recommendation. To explore the potential time delay responsible for the increase in time-to-listing post-CDR, we compared the median time-to-listing for the 24 drugs listed with a CDR recommendation. The median time from NOC to CDR recommendation was 72 days longer than the median time from CDR recommendation to listing. On average, for drugs listed on the AHWDBL, the proportion of time attributable to the CDR process (NOC to CDR recommendation) was 63% (356 days of 569) of the overall time-to-listing.
Discussion
Main findings
The implementation of the CDR, intended to streamline the process of drug reimbursement by public drug plans, was associated with an increased median time-to-listing in the province of Alberta. In the five years following the CDR's first recommendation, the median time from Health Canada's issuing an NOC to drug approval in Alberta was 212 days longer compared to the five-year period prior to the CDR's first recommendation. Notably, however, the majority of the time between NOC and listing was spent between the NOC's being issued and the CDR recommendation. This finding suggests that the CDR may provide a more efficient system for province-level decision-making, as opposed to the overall timeline of listing of drugs. In fact, the median and average time-to-listing prior to CDR (from NOC to listing) was 312 and 551 days, respectively, whereas post-CDR the median and mean time-to-listing from CDR recommendation to listing was 167 and 213 days, respectively.
The implications of this finding on the health of the population and individuals are context-specific and dependent on the risks and benefits of each drug and, subsequently, the use (whether appropriate or inappropriate) of each drug. This difference represents more than a six-month time frame, which may represent a substantial amount of time from the drug manufacturer's perspective; however, efficiencies for the payer, in this case Alberta Health and Wellness, may have been gained.
Alberta's drug review process
Currently, there are five separate government ministries that administer government-sponsored drug plans in Alberta: Health and Wellness, Children and Youth Services, Employment and Immigration, Seniors and Community Supports, and Solicitor General and Public Security. Each of these ministries administers its own drug programs for which different rules and eligibility apply; however, the AHWDBL serves as a common core list for each of the programs. Many of the programs cover drugs that are not listed on the AHWDBL, for example, hospitalized patients, cancer patients and transplant patients.
The drug review process in Alberta is outlined within the publicly available Alberta Health and Wellness Drug Benefit List (Government of Alberta 2010b). The AHWDBL was implemented in 1991, lists over 3,600 drugs and is currently updated on a quarterly basis. The Alberta Health and Wellness Expert Committee on Drug Evaluation and Therapeutics (ECDET), comprising physicians and pharmacists, recommends listing decisions for drugs to Alberta Health and Wellness through the Executive Director of the Pharmaceutical Funding and Guidance Branch. The Minister of Health and Wellness is responsible for the final listing decision. The ECDET considers both clinical and economic evidence for its recommendations. The AHWDBL lists general criteria that the ECDET and the minister are to consider prior to making a recommendation or listing decision; however, the criteria are not rigid and permit flexibility depending on the situation. Hospital-based drugs, childhood vaccinations, cancer agents, tuberculosis agents and drugs used to treat erectile dysfunction are not considered for coverage under the AHWDBL. The AHWDBL lists a drug as a regular benefit, special authorization benefit, optional special authorization, step therapy, restricted benefit or limited restricted benefit. Special authorization guidelines are available for each drug product that assist in determining coverage eligibility. These requests can be made by prescribers and are reviewed by clinical pharmacists, analysts or both. Restricted benefits refer to drugs that have restricted coverage criteria that are automatically adjudicated (i.e., a person is not required to be screened).
In the July 1, 2004 AHWDBL, the CDR process was integrated into Alberta's drug review procedure. Introduction of the CDR affected several components of Alberta's drug review process. Firstly, for both new chemical entities and new combination products, drug manufacturers no longer initiated the drug review process at the provincial level. Instead, they were required to submit drugs that fell under the CDR mandate directly to the CDR. Second, the ECDET is provided with recommendations regarding listing status from CEDAC. If the recommendation is not to list, the drug is not reviewed by the ECDET; the ECDET is simply informed of the decision. Our study supports this notion, as 32 drugs with a "do not list" recommendation from CDR were not listed on the AHWDBL. If the CDR recommends a product to be listed, listed in a similar manner to other drugs in class, or listed with criteria/condition, the ECDET is usually (a small number of products with a "yes" recommendation with no criteria/conditions have not been additionally reviewed by the ECDET) provided with a summary and complete clinical and pharmaco-economic review report from the CDR. In addition, the ECDET considers a review of provincial economic considerations (pricing, utilization and budget impact) for drugs for which CDR makes recommendations.
Notwithstanding changes due to the CDR process, normal changes in the policy environment (elected and unelected AHW personnel) and changes to the ECDET's committee membership, the drug review process in Alberta remained similar before and after the CDR was introduced. Major reforms to the drug review process are currently being implemented through the Alberta Pharmaceutical Strategy, although these changes did not occur during this study period (Government of Alberta 2010a).
Comparison to previous reports on time-to-listing
We are aware of three previous reports that have commented on provincial drug reimbursement decisions, time-to-listing post-CDR implementation or both (Kallah 2006; Skinner and Rovere 2009; Wyatt et al. 2008).
An IMS Health report, Provincial Reimbursement Advisor (Kallah 2006) calculated the average time-to-listing of all drugs that had completed a CDR review as of October 20, 2006. Alberta had listed 10 of 22 drugs reviewed, with an average time-to-listing of 413 days. Because the IMS report used single-source products only and included alternative formulations of similar products, the number of listings is not directly comparable to our analysis. The report also showed an average historical time-to-listing of 406 days for Alberta, which was defined as the average time-to-listing for drugs approved between September 1, 2000, and August 31, 2003 (i.e., a two-year period prior to the CDR). Based on this report, Tierney and Manns (2008) found that the time-to-listing of drugs had not changed from before the CDR compared to after its implementation (471 vs. 479 days). This finding is misleading because there was substantial variability among average times-to-listing across provinces (Kallah 2006). Among participating drug plans in the CDR process, the minimum time-to-listing was 372 days (Nova Scotia) and the maximum was 753 days (PEI) post-CDR (Kallah 2006). There was also a wide range in the time-to-listing changes among different drug plans, with Ontario's time-to-listing decreasing by 85 days but non-insured health benefits (NIHB) time-to-listing increasing by 173 days (Kallah 2006). Although the data presented in the IMS Provincial Reimbursement Advisor (Kallah 2006) describe time-to-listing for public drug plans participating in the CDR and compare the time-to-listing before and after CDR's implementation, there were no formal statistical comparisons. Our study demonstrates a six-month difference and one-month difference in median and mean time-to-listing for one participating drug plan – Alberta's.
A report published by Wyatt Health (Wyatt et al. 2008) compared provincial drug reimbursement decisions and those of other countries for drugs issued a CEDAC recommendation as of December 31, 2007. Of 78 different drugs with a recommendation, 36 drugs were included in Wyatt's comparisons because they were common among all countries. These authors reported that provincial drug plans made positive decisions 49% of the time and contrasted this with CEDAC's recommending reimbursement for 61% of the 36 drugs and 14 EU countries' averaging a 91% reimbursement. We found that Alberta listed 24 (58%) drugs for which CEDAC recommended reimbursement.
The third annual report by the Fraser Institute (Skinner and Rovere 2009) examining wait times for access to medications at both the federal and provincial levels provides information regarding the proportion of drugs reimbursed in Alberta from 2004–2007 that received an NDS-class NOC from Health Canada. The report found that out of 174 NOCs issued for NDS-class drugs, 20 (11.5%) were approved in Alberta. Within this time period (2004–2007), we identified 24 drugs approved of 96 (25% approval rate) deemed eligible for our study. Our approval rate is expected to be somewhat higher, as we did not limit our comparison to NDS-class drugs. Skinner and Rovere (2009) also report time-to-listing for new drugs approved by Health Canada separately for 2004 through 2007. There appears to be a wide variation between the years for Alberta, ranging from approximately 250 days in 2007 to over 600 days in 2005. Our average time-to-listing for drugs receiving an NOC between 2004 and 2007 followed a similar pattern, with 2005 having the longest time-to-listing.
Clinical and policy implications
In order to define what constitutes a meaningful difference in terms of time-to-listing, one must consider the clinical perspective as well as the population health perspective. A meaningful difference from a clinical perspective depends on individuals having access to new drug products that may be of benefit or harm to their health. For certain individuals who have tried the currently available therapies and cannot afford more expensive innovative therapies, any amount of time may be important, especially for symptomatic treatment. Conversely, a rapid increase in the use of a drug (potentially as a consequence from a listing decision) may be associated with harm, as was the case in Ontario, which had a more liberal drug policy compared to British Columbia when COX-2 inhibitors were introduced to the market. Consequently, Ontario experienced a larger increase in the hospitalization rate for upper gastrointestinal haemorrhage compared to British Columbia (Mamdani et al. 2006).
From a population health perspective, one must consider the nature of the drug and prevalence of its indicated use within the population. For example, a drug that is expected to be used by <1% of the population will not have as large an impact on health outcomes compared to a drug of equal effectiveness for conditions with a higher prevalence (i.e., >10%). Further, the degree to which newly marketed drugs are truly considered to be "innovative" should also be considered. New products that are "me-toos" or fixed-dose combinations or previously listed products may have less of an impact than new products that truly represent therapeutic breakthroughs.
For each drug that the CDR recommends, there is often a specific indication associated with the recommendation. This practice has policy implications for the province of Alberta, because when a drug is given full-benefit status no specific indication is attached. The drug may be listed under special authority to address an indication's specific requirements, although this depends on the nature of the drug, particularly if it is indicated for both acute and chronic requirements; a special authority policy may have a negative impact on the population's health (Jackevicius et al. 2008).
Under current pharmaceutical policy reforms, Alberta is Canada's first province with a government-sponsored drug plan for rare diseases, which came into effect on April 1, 2009. Diseases for which treatment coverage will be considered include Gaucher's disease, Fabry's disease, MPS I (Hurler's/Hurler Scheie syndrome), Hunter's syndrome and Pompe's disease. The CDR has made recommendations for listing regarding drugs used to treat some of these diseases, such as alglusidase (Pompe), agalsidase beta (Fabry) and idursulfase (Hunter). For this class of medications, it is especially difficult to make listing decisions using the same framework and standards regarding clinical and economic evidence as drugs used for more prevalent conditions.
Limitations
Several limitations of our study must be addressed. First, our measurement of time-to-listing started when a drug was issued an NOC, which may not accurately reflect time-to-listing because a time lag occurs between time of NOC and submission for reimbursement. Second, it was not possible to discern which drugs Alberta Health and Wellness reviewed and subsequently declined. Thus, drugs that were not listed include both those that were reviewed as well as those not reviewed. Third, drugs may not be reviewed because a manufacturer may decide not to submit its product for coverage, especially for medications that belong to a class of drugs that is pre-specified not to be covered (e.g., hospital-based drugs or drugs used for erectile dysfunction). Fourth, the difference between median time-to-listing in the pre-CDR and post-CDR periods may be exaggerated owing to delays for drugs with an NOC issued around the time of CDR implementation, most likely because of institutional procedural adjustments and adaptations. When drugs issued an NOC in 2005 are excluded, our results are consistent (pre-CDR median 312 days vs. post-CDR median 440 days). Lastly, unknown changes in the drug review process, government personnel changeover and secular changes, such as the types of drugs receiving marketing approval, may have influenced the results of our study.
Conclusions
The CDR has been completing drug reviews and recommendations for Canada's publicly funded drug plans for over five years now. Although Alberta's government-funded drug plan is a participating drug plan, it does not always follow the CDR's recommendations. The overall agreement in the first five years of CDR recommendation was fair to good (kappa= 0.55); the time to drug coverage slowed significantly (median time is 212 days longer), although it is more consistent. Moreover, the CDR may act as a catalyst and speed up the decisions for reimbursement at the provincial level. Whether similar results would be observed in other provinces and territories, or only in select parts of the country, remains to be demonstrated in the peer-reviewed literature.
Appendices
Legend
CDR recommendations:
Y=List
S=List in a similar manner to other drugs in class
R=List with criteria/condition
N=Not list
Alberta Coverage Status:
Y=Listed as a full benefit
R=Listed with restriction/special authorization
N=Not listed
| Appendix 1. Drugs that were not listed in Alberta and were recommended to be listed by the CDR (n=17) | |||
| Generic name | Brand name | AB coverage status | CDR recommendation |
| abacavir/lamivudine | Kivexa | N | S |
| acamprosate | Campral | N | R |
| alglucosidase alfa | Myozyme | N | R |
| ambrisentan | Volibris | N | R |
| atorvastatin/amlodipine | Caduet | N | R |
| darunavir | Prezista | N | R |
| emtricitabine/tenofovir/efavirenz | Atripla | N | R |
| emtricitabine/tenofovir | Truvada | N | R |
| etravirine | Intelence | N | R |
| fosamprenavir | Telzir | N | S |
| maraviroc | Celsentri | N | R |
| mycophenolic acid | Myfortic | N | S |
| niacin/lovastatin | Advicor | N | Y |
| raltegravir | Isentress | N | R |
| ranibizumab | Lucentis | N | R |
| tipranavir | Aptivus | N | R |
| varenicline* | Champix | N | R |
|
* Under review as of April 2010 |
|||
| Appendix 2. Drugs that were listed in Alberta and recommended to be listed by the CDR (n=24) | |||
| Generic name | Brand name | AB coverage status | CDR recommendation |
| abatacept | Orencia | R | R |
| adalimumab | Humira | R | R |
| aprepitant | Emend | R | R |
| buprenorphine/naloxone | Suboxone | Y | R |
| carbidopa/levodopa/entacapone | Stalevo | Y | S |
| ciclesonide | Alvesco | Y | Y |
| darifenacin | Enablex | R | R |
| deferasirox | Exjade | R | R |
| drospirenone/esthinyl estradiol | Yasmin | Y | Y |
| duloxetine | Cymbalta | R | R |
| efalizumab | Raptiva | R | R |
| entecavir | Baraclude | R | R |
| eprosartan/hydrochlorothiazide | Teveten Plus | Y | S |
| insulin glulisine | Apidra | Y | S |
| lanreotide | Somatuline | R | S |
| natalizumab | Tysabri | R | R |
| olmesartan | Olmetec | Y | S |
| olmesartan/hydrochlorothiazide | Olmetec Plus | Y | S |
| ramipril/hydrochlorothiazide | Altace-HCT | Y | Y |
| rivaroxaban | Xarelto | R | R |
| travoprost/timolol | Duo Trav | Y | R |
| trospium | Trosec | R | R |
| voriconazole | Vfend | R | R |
| ziprasidone | Zeldox | Y | R |
| Appendix 3. Drugs that were not listed in Alberta and were not recommended to be listed by the CDR (n=2) | |||
| Generic name | Brand name | AB coverage status | CDR recommendation |
| alefacept | Amevive | N | N |
| alendronate/cholecalciferol | Fosavance | N | N |
| aliskiren | Rasilez | N | N |
| atomoxetine | Strattera | N | N |
| cinacalcet | Sensipar | N | N |
| dabigatran | Pradax | N | N |
| daptomycin | Cubicin | N | N |
| delta-9-tetrahydrocannabinol/cannabidiol | Sativex | N | N |
| eletriptan | Relpax | N | N |
| escitalopram | Cipralex | N | N |
| idursulfase | Elaprase | N | N |
| insulin aspart/protamine | Novomix | N | N |
| insulin detemir | Levemir | N | N |
| lanthanum carbonate | Fosrenol | N | N |
| laronidase | Aldurazyme | N | N |
| memantine | Ebixa | N | N |
| methylnaltrexone | Relistor | N | N |
| omalizumab | Xolair | N | N |
| paliperidone | Invega | N | N |
| pegaptanib | Macugen | N | N |
| pegvisomant | Somavert | N | N |
| posaconazole | Posanol | N | N |
| pregabalin | Lyrica | N | N |
| rasagiline | Azilect | N | N |
| sitagliptin | Januvia | N | N |
| sitaxsentan | Thelin | N | N |
| sodium oxybate | Xyrem | N | N |
| solifenacin | Vesicare | N | N |
| telbivudine | Sebivo | N | N |
| teriparatide | Forteo | N | N |
| tramadol | Zytram | N | N |
| tramadol/acetaminophen | Tramacet | N | N |
Comparaison de la couverture pour les médicaments en Alberta avant et après la mise en place du Programme commun d'évaluation des médicaments
Résumé
Objectif: La mise en place du Programme commun d'évaluation des médicaments (PCEM) a constitué un changement important dans les régimes publics d'assurance-médicaments au Canada. Il n'y a pas encore eu de comparaisons rigoureuses, dans le contexte du PCEM, entre les délais d'inscription à la liste et la proportion de médicaments couverts par le régime d'assurance-médicaments de l'Alberta.
Méthodologie: Cette comparaison tient compte des nouveaux médicaments approuvés par Santé Canada cinq ans avant et cinq ans après la mise en place du PCEM (mai 2004). Les délais d'inscription et la proportion de nouveaux médicaments couverts par le régime d'assurance-médicaments de l'Alberta (Alberta Health and Wellness Drug Benefit List, AHWDBL) ont été comparés pour ces périodes. Le degré de concordance entre les recommandations du PCEM et la couverture en Alberta a été calculé au moyen du coefficient kappa.
Résultats: Deux cent vingt nouveaux médicaments qui réunissaient les critères de l'étude ont été répertoriés (118 avant la mise en place du PCEM et 102 après). Les délais médians d'inscription à la liste étaient de 312 jours pour les médicaments pré-PCEM et de 524 jours pour les médicaments post-PCEM, la différence étant grandement attribuable au temps entre l'avis de conformité et la recommandation du PCEM. Pour 73 médicaments, le taux de concordance entre les recommandations du PCEM et la couverture en Alberta était modéré (kappa 0.55).
Conclusion: Suite à la mise en place du PCEM, la proportion de médicaments couverts a diminué et le temps médian global d'inscription des nouveaux médicaments à la liste a augmenté dans la province de l'Alberta. Pour les médicaments inscrits sur la liste de l'AHWDBL, la proportion de temps attribuable au processus du PCEM (soit de l'avis de conformité à la recommandation du PCEM) équivaut à 63% du temps global pour l'inscription à la liste.
About the Author(s)
John-Michael Gamble, BSc(Pharm), MSc, Research Assistant, School of Public Health, University of Alberta, Edmonton, AB
Dean T. Eurich, PhD, Assistant Professor, School of Public Health, University of Alberta, Edmonton, AB
Jeffrey A. Johnson, PhD, Professor, School of Public Health, University of Alberta, Edmonton, AB
Correspondence may be directed to: Dr. Dean T. Eurich, Assistant Professor, School of Public Health, 2-040 Li Ka Shing Centre for Health Research Innovation, University of Alberta, Edmonton, AB, Canada, T6G 2E1; tel.: 780-492-6333; e-mail: deurich@ualberta.ca.
Acknowledgment
Mr. Gamble receives salary support through a full-time Health Research Studentship from the Alberta Heritage Foundation for Medical Research Endowment fund and a Canada Graduate Scholarship from the Canadian Institutes of Health Research (CIHR); Dr. Eurich is a population health investigator with Alberta Innovates – Health Solutions and a New Investigator with the CIHR. Dr. Johnson is a senior health scholar with Alberta Innovates – Health Solutions and Canada Research Chair in Diabetes Health Outcomes.
The authors would like to thank Mr. Steve Long, Ms. Mary Jo Macleay and Dr. Carlyn Volume-Smith for their assistance in gathering background information for this manuscript.
Dr. Johnson is a member of the Expert Committee for Drug Evaluation and Therapeutics for Alberta Health and Wellness. The opinions expressed in this manuscript are his and not those of AHW or the ECDET.
References
Anis, A.H., D. Guh and X. Wang. 2001. "A Dog's Breakfast: Prescription Drug Coverage Varies Widely across Canada." Medical Care 39(4): 315–26.
Canadian Agency for Drugs and Technologies in Health (CADTH). 2009a. "CADTH Submission to the House of Commons Standing Committee on Health." Retrieved October 12, 2010. <http://www.cadth.ca/media/media/CADTH_Submission_to_Standing_Committee_on_Health_070409.pdf>.
Canadian Agency for Drugs and Technologies in Health (CADTH). 2009b. "About CADTH." Retrieved October 12, 2010. <http://www.cadth.ca/index.php/en/cadth>.
Canadian Agency for Drugs and Technologies in Health (CADTH). 2009c. "Search CDR Drug Database." Retrieved October 12, 2010. <http://www.cadth.ca/index.php/en/cdr/search?&status=complete&order_field=drug_name>.
Canadian Agency for Drugs and Technologies in Health (CADTH). 2009d. "CDR Overview." Retrieved October 12, 2010. <http://www.cadth.ca/index.php/en/cdr/cdr-overview>.
Demers, V., M. Melo, C. Jackevicius, J. Cox, D. Kalavrouziotis, S. Rinfret, K.H. Humphries, H. Johansen, J.V. Tu and L. Pilote. 2008. "Comparison of Provincial Prescription Drug Plans and the Impact on Patients' Annual Drug Expenditures." Canadian Medical Association Journal 178(4): 405–9.
Fleiss, J.L. 1981. Statistical Methods for Rates and Proportions (2nd ed.). New York: John Wiley & Sons.
Government of Alberta. 2010a. "Alberta Pharmaceutical Strategy." Retrieved October 12, 2010. <http://www.health.alberta.ca/initiatives/pharmaceutical-strategy.html>.
Government of Alberta. 2010b. "Printable Drug Benefit List and Related Publications." Retrieved October 12, 2010. <http://www.ab.bluecross.ca/dbl/publications.html>.
Gregoire, J.P., P. MacNeil, K. Skilton, J. Moisan, D. Menon, P. Jacobs, E. McKenzie and B. Ferguson. 2001. "Inter-provincial Variation in Government Drug Formularies." Canadian Journal of Public Health 92(4): 307–12.
Health Canada. 2009. "What Is the DPD Data Extract? Health Canada Drug Product Database (DPD)." Retrieved October 12, 2010. <http://www.hc-sc.gc.ca/dhp-mps/prodpharma/databasdon/dpd_bdpp_data_extract-eng.php>.
Jackevicius, C.A., J.V. Tu, V. Demers, M. Melo, J. Cox, S. Rinfret, D. Kalavrouziotis, H. Johansen, H. Behlouli, A. Newman and L. Pilote. 2008. "Cardiovascular Outcomes After a Change in Prescription Policy for Clopidogrel." New England Journal of Medicine 359(17): 1802–10.
Kallah, J. 2006. "Formulary Acceptance: Monitoring and Evaluation." Provincial Reimbursement Advisor 9(4): 57–77.
MacDonald, K. and K. Potvin. 2004. "Interprovincial Variation in Access to Publicly Funded Pharmaceuticals: A Review Based on the WHO Anatomical Therapeutic Chemical Classification System." Canadian Pharmacists Journal 137(7): 29–34.
Mamdani, M., L. Warren, A. Kopp, J.M. Paterson, A. Laupacis, K. Bassett and G.M. Anderson. 2006. "Changes in Rates of Upper Gastrointestinal Hemorrhage After the Introduction of Cyclooxygenase-2 Inhibitors in British Columbia and Ontario." Canadian Medical Association Journal 175(12): 1535–38.
McMahon, M., S. Morgan and C. Mitton. 2006. "The Common Drug Review: A NICE Start for Canada?" Health Policy 77(3): 339–51.
Morgan, S., G. Hanley and C. Raymond. 2009. "Breadth, Depth and Agreement among Provincial Formularies in Canada." Healthcare Policy 4(4): e162–e184.
Skinner, B. and M. Rovere. 2009. Access Delayed, Access Denied: Waiting for New Medicines in Canada: 2009 Report. Calgary: Fraser Institute.
Tierney, M. and B. Manns. 2008. "Optimizing the Use of Prescription Drugs in Canada through the Common Drug Review." Canadian Medical Association Journal 178(4): 432–35.
World Health Organization (WHO). 2009. "The Anatomical Therapeutic Chemical Classification System with Defined Daily Doses (ATC/DDD)." Retrieved October 12, 2010. <http://www.who.int/classifications/atcddd/en/>.
Wyatt, G., V. Fladu, K. McDonald-Taylor, R. MacPhee, A. Coley and J. Milne. 2008. The 2007 Wyatt Health International Comparison. Access to Innovative Pharmaceuticals: How Do Countries Compare? Oakville, ON: Wyatt Health Management.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed