ElectronicHealthcare
A. Introduction
For more than a decade, Québec has acknowledged that its vision of healthcare delivery requires the enabling assistance of e-Health standards and solutions. The ongoing debate among the province's healthcare stakeholders has focused on what Québec expects to achieve from its efforts and investments in e-Health and how to proceed efficiently and effectively to secure those outcomes for its entire population in a reasonable period of time.
The most recent phase of Québec's healthcare debate was inaugurated in 2001, when the Clair Commission issued "The Emerging Solution": a comprehensive review of the present and future of the province's healthcare delivery system. Prominent among its recommendations were those concerning the reorganization of primary healthcare delivery services by establishing family practice groups, and creating an insurance fund to expand home health and institutional services for the province's growing elderly population. The Commission's final recommendation focused on promoting expanded use of information technology in healthcare to support clinical decisions and healthcare management, measure performance and evaluate outcomes. Specifically, the Commission recommended the creation of a Québec Techmed Foundation to foster investment in medical technology (Chodos 2001).
Since 2001, and especially over the last three years, the debate about enabling more efficient and effective healthcare delivery at all levels – provincial, regional and local – has increasingly focused on finding the appropriate tactics and techniques for effective implementation of a provincial e-Health strategy.
- In 2008, the Castonguay Group – headed by Claude Castonguay, former minister of health – issued its Report of the Task Force on the Funding of Health Care, which recommended prioritizing implementation of an electronic medical record (EMR) that would connect patient records in healthcare facilities (Task Force on Health Funding 2008).
- In the 2009 "Appraisal Report on the Performance of Québec's Health and Social Services System," the provincial Health and Welfare Commissioner moved in the same direction as the Castonguay Group by recommending that the government "support the implementation of electronic medical records and Québec's shareable Electronic Health Record" (Health and Welfare Commissioner 2009).
- On March 22, 2011, Québec's Minister of Health, Dr. Yves Bolduc, announced that development of most components of Québec's Dossier de santé du Québec (DSQ), or provincial electronic health record (EHR), is close to completion. Many of these components are already operational, and others will be deployed gradually in 2011 and 2012 (Bolduc 2011a). In a press conference following the announcement, the Minister of Health indicated that the province's DSQ/EHR is slated to be fully operational across Québec by 2016 (Les dossiers médicaux 2011).
- Most recently, in the Rapport du Vérificateur général du Québec à l'Assemblée nationale pour l'année 2010–2011, issued in May 2011, the province's Auditor General reaffirmed the importance of the government's e-Health initiatives aimed at improving Québec's healthcare access and delivery. But he also stressed that the risks involved in prolonging the status quo of partial implementation of the province's DSQ/EHR need to be addressed immediately (Vérificateur général du Québec 2010, 2011; Journal des débats 2011a, 2011b).
|
Five Criteria or National Principles of the Canada Health Act
|
In addition to policy and administrative decisions effecting Québec's e-Health strategy, several important provincial legislative enactments have shaped the development of provincial healthcare policy focused on developing e-Health standards and solutions. It should be noted that all legislative decisions of the province's National Assembly are taken in compliance with the five "criteria" or "national principles" of the Canada Health Act, adopted in 1984 (Madore 2005). In that context, provincial legislation enacted since 2005 has pointedly defined and mandated conditions for implementation of e-Health to enable efficient and effective healthcare delivery. The most relevant pieces of legislation – which were approved in 2005 (Law 83), 2010 (Law 100) and 2011 (Law 133) – are as follows:
- Projet de loi no. 83 (2005, chapitre 32) is the first legislation to introduce the subject of les systèmes d'échange d'informations en santé, or health information exchanges (HIE), as well as rules governing the security and confidentiality of electronic health records for patients who were participants in e-Health pilot projects. (Note: Law 83 is currently under revision to finalize the concepts of health information exchange, clinical data repositories, governance and responsibility.) (National Assembly 2005).
- Projet de loi no. 100 (2010, chapitre 20) mandated restoration of fiscal balance for the 2013–2014 budgets and reduction of the provincial debt. All government facilities and services, including those of health and social services, must cut 10% of their administrative costs for the next three years. The mandates of law 100 impact IT and IS budgets, including those for e-Health (National Assembly 2010).
- Projet de loi no 133 (2011, chapitre 19) aims at ensuring access to and quality of public services that are provided by all government ministries including health and education. The law installed mechanisms to improve ministerial governance, allow for fiscal optimization and rationalization by pooling projects and information technology (IT) and information service (IS) infrastructures, and require transparency on financial issues for all major IT projects (National Assembly 2011).
An important cumulative effect of these laws has been to concentrate the government's efforts – as it initiates the final phases of populating and integrating the province's DSQ/EHR with multiple interfaced patient information resources – on moving forward in a fiscally and administratively rigorous manner that avoids extending the cost overruns and implementation delays of the past decade. As with her sister provinces' and territories', Québec's e-Health journey has incurred expensive and time-consuming experimentation along the unexplored path of transitioning healthcare delivery from an often error-prone and untimely paperless environment to the efficiencies and efficacies of electronic enablement. In the current era of restricted government budgets wrestling with debt burden and reduced revenues, e-Health is no longer immune to operating and capital spending reductions. Thus, it is not surprising that investment by Québec health facilities in IT and IS technology is approximately 1.58% of their global budget, with the percentage for capital spending varying from one region to another. By contrast, European healthcare facilities invest an average of 3.65% to 6.5% of their global budgets in IT (Monrozier 2011). The coming challenge for Québec, as it turns the corner toward the home stretch of the DSQ/EHR project slated for completion in 2016, is how to optimize performance outcomes in an environment of complex IT and IS integration on restrained budgets.
For these reasons, the ten-year debate over the need for timely and comprehensive implementation of a provincial EHR coalesced in March 2011 when the government announced the creation of the Bureau de programme de l'informatisation du réseau, or e-Health Program Office, under the direction of the Assistant Deputy Minister of Health and Social Services. With its mandate to manage, supervise and coordinate all e-Health resources and activities, the Bureau will provide unified governance for the computerization of Québec's health network. Three committees report directly to the Bureau:
- Le Conseil de gouvernance is responsible for providing counsel to the Bureau regarding all decisions adopted to realize its mandate of facilitating the final implementation of the DSQ/EHR.
- Le Comité consultatif des besoins cliniques is responsible for securing the participation of the end users of the DSQ/EHR and guiding the connectivity between clinical needs and possible technology.
- La Table d'interopérabilité, operating under the leadership of the president of the Régie de l'assurance maladie du Québec (RAMQ), is charged with defining the rules, norms and specifications required for integrating the components of the diverse information systems, which generate, support and exchange clinical information from different electronic records (Bolduc 2011a; Bureau de programme 2011).
The Bureau's oversight is needed to synchronize all aspects involved in completing implementation and integration of the province's e-Health network, including interfacing with and integration of the provincial DSQ/EHR, acute DCI/ EMR and the Dossier médical électronique (DMÉ), or physician office EMR. As Madame Lise Verreault, Assistant Deputy Minister of Health and Social Services, indicated in her recent presentation detailing the responsibilities and structure of the Bureau – "Un Réseau, Une Vision, Une Gouverne," delivered on October 13 in Québec City at AQESSS' "La santé électronique 2011" – "We are at a time where the great technological shifts are intervening directly in our ways of working, principally at the level of the means required for the delivery of care and services to the population" (Verreault 2011; my translation).
B. The Role of AQESSS and HIMSS Analytics in Québec's e-Health Journey
For some five years, l'Association québecoise d'établissements de santé et de services sociaux (AQESSS), representing 85% of Québec's healthcare organizations, has contributed to the province's e-Health debate summarized above by tracking and analyzing the province's host of ongoing healthcare projects. Based on assessing the track record of these projects to date, l'AQESSS has developed an abstract of the conditions that would be required to successfully achieve the optimal objectives of the province's e-Health strategy within the announced time frame of completing the provincial EHR by 2016.
- A common and shared understanding of e-Health IS, IT and information management (IM) required to obtain anticipated benefits
- A clear vision of the roles and responsibilities of the stakeholders in diverse projects (local, regional, national levels)
- A concerted governance to establish priorities, optimize actual assets, and develop interoperability integration and coherence
- Resolution of the financial issues surrounding these projects in a context of budget restrictions
- A positive leadership relation between health professionals, health administrations and IT teams
AQESSS is a 131-institutional member non-profit association of Québec's CSSSs, teaching centres, affiliated hospital centres, university institutes and affiliated university centres, as well as stand-alone hospitals and long-term care facilities. AQESSS's mission is to act as leader for these institutions and their collective public voice for the sake of ensuring the quality of services and sustainability of the health and social services network. AQESSS's website is <https://www.aqesss.qc.ca/fr/accueil.aspx?sortcode=1>.
HIMSS Analytics is a non-profit healthcare research organization that collects and analyzes healthcare data relating to IT processes and environments, products, IS department composition, costs and management metrics, healthcare trends and purchasing decisions. HIMSS Analytics' clients include healthcare providers and IT companies, consulting firms, government agencies, pharmaceutical companies, and university research and healthcare degree programs. HIMSS Analytics' website is <https://www.himssanalytics.org/>.
In spring 2011, AQESSS – in collaboration with Québec's Ministère de la santé et des service sociaux (MSSS) – formed a partnership with Chicago-based Health Information Management Systems Society (HIMSS) Analytics to develop an information technology and communications (ICT) inventory of healthcare-related software and hardware for all Québec in-patient and ambulatory facilities. The joint AQESSS/MSSS initiative with HIMSS Analytics is in keeping with AQESSS's mission to serve as a credible and influential participant in important provincial debates over health and social service issues involving governmental organizations, its own member partners and the population that its members serve (Aqesss 2011b). HIMSS Analytics' collaboration with AQESSS is an important dimension of its global healthcare data collection and measurement initiatives – including efforts in the United States, Canada, Europe, the Middle East and Asia PAC. HIMSS Analytics' global data initiatives produce vital acute and ambulatory electronic medical record adoption model (EMRAM) scores and more than 76 benchmarking reports, which provide strategic intelligence for participating providers (HIMSS Analytics 2011a).
The AQESSS/MSSS–HIMSS Analytics inventory process is being conducted in three phases, to be concluded some time in 2012. The first phase involves assessing the status of all clinical and back-office software installations at Québec's 121 in-patient healthcare facilities. As of October 2011, 52 facilities had submitted completed studies, with more to be obtained in winter 2012. The first results of the inventory study were presented and discussed at AQESSS' "La santé électronique 2011," which was held on October 13 and 14 at the Centre des congrès de Québec in Québec City (Powers 2011). The second and third phases involve completing the inventory of acute care facilities and undertaking a similar inventory of the province's non-acute and ambulatory facilities.
Presentation and evaluation of the first EMRAM scores for Québec is addressed below in the section entitled "Measuring Québec's EMR Capabilities with the HIMSS Analytics Acute EMRAM," which follows sections on an "Overview of Québec Healthcare Delivery in Five Parts," "Provincial e-Health: Québec's Electronic Health Record" and "Québec's Hospital and Physician Office Electronic Medical Records."
C. Overview of Québec Healthcare Delivery in Five Parts
1. Québec Demographics
Québec had an estimated 7.95 million residents, or approximately 23.1% of Canada's estimated 33.3 million residents, as of April 1, 2011 (Statistics Canada 2011). Some regions and their suburbs have a high population density, namely Montréal, Laval, l'Outaouais, Québec City (provincial capital) and Sherbrooke. On the whole, however, Québec's population is spread over a vast territory of 1,667,441 km (Institut de la statistique du Québec 2009).
Important characteristics of the province's current population are the following. Longevity is an average of 78 years for men and 83 years for women. The fertility rate is only 1.62 children per female. It is projected that by 2031 25% of Québec's population will be 65 years of age and older. Even more important is the fact that the ongoing increase in the number of elderly is matched by a significant reduction in the number of working-age people. (Immigration et Communautés culturelles Québec 2006). The low birth-rate is only partially off-set by ongoing immigration, which adds to demographic growth.
As with most industrial countries, the province of Québec and its health sector face social, economic and technological changes requiring transition to a knowledge- and information-based society. Already, 50% of people over the age of 50 have a cellular telephone and a computer at home (Institut d'études prospectives technologiques 2004). Québec's health consumers of the future will have new knowledge and technological expectations. Increasingly, they are seeking more qualitative health information on the Internet and via cellular phones. The growing need for home care services among the elderly will accelerate the demand for accessing customized healthcare information via mobile devices.
The province's demographic changes increase the pressure for expanded technology-enabled healthcare services (Monrozier 2011). Yet Québec suffers from a shortage of human resources both in the health and technology sectors to meet the growing demand. The rapid increase of an aging population triggers conflicting demands for improvement of access to and investment in expanded healthcare services at a time when the state of public finances requires reduced spending in all sectors and an urgent need for health cost controls.
2. Québec's Program-Oriented Health System
Québec's health and social services system is divided into service programs and support programs, such that the organization of services is guided by the needs of the population or population groups grappling with a particular problem (The Québec Health and Social Services System 2011b). This arrangement provides a framework for planning, allocating resources and accountability reporting. There are currently nine service programs, as follows:
- Two service programs respond to the needs of the entire provincial population:
- Public health – that is, the promotion, prevention and protection of health and well-being as well as surveillance of health status
- General services – clinical and assistance activities, which cover primary care services in the area of health or specific social problems
- Seven service programs are devoted to specific issues:
- Loss of autonomy linked to aging
- Physical impairment for disabilities linked to hearing, vision, language and speech, or motor skills
- Mental impairment and pervasive developmental disorders (PDDs)
- Young persons with a range of problems
- Dependencies, such as alcoholism, drug addiction, pathological gambling, and so forth
- Mental health
- Physical health, which covers emergency services, specialized and highly specialized services, continuous services requiring systematic follow-up (e.g., chronic diseases, cancer) and palliative care
- There are currently two support programs involving administrative and technical activities that provide support for the nine service programs:
- Administration and support
- Buildings and equipment management
3. Québec's Health System of Local Networks
In order to ensure that the citizen is at the centre of the province's health and social system, the provision of services is organized around local networks that bring together all service stakeholders, including family physicians, in order to collectively share responsibility for the healthcare of a local territory's population. Québec's geographically defined healthcare delivery model, which supports adaptation of local healthcare services delivery, is known as the Réseau local de services (RLS), or continuum of care (Santé et Services sociaux Québec 2011b).
At the heart of the local network of services is the Centre de santé et services sociaux (CSSS), or health and social services centre, which integrates the quality and continuity of patient care between facilities, caregivers and patients in a given locality. The CSSS is the foundation for an integrated provision of services ensuring accessibility, case management, follow-up and coordination of services for a specific local population. The CSSS model focuses on the provision of a wide range of primary care services, including public health services, in close proximity to the living environment of a local resident; and on the establishment of mechanisms of referral and follow-up to ensure access to secondary and tertiary care (specialized and highly specialized services). In this way, the range of providers of health and social services for a local population are able to respond to the needs of the residents and to facilitate their progression, especially that of vulnerable individuals, through the healthcare delivery system (see Figure 1).
4. The Human Resources of the Québec Health System
Québec's healthcare delivery system depends on diverse human resources to implement the organizational changes and e-Health technologies that are required to support future expectations for the province's health and social services programs.
The province's social and healthcare network employs more than 10% of the active workforce in Québec. This represents more than 127,000 persons, including a mix of professionals in addition to nurses and physicians (see Table 1).
| Table 1. Quebec healthcare professionals | |
| Category | Total |
| Physicians | 15,109 |
| Pharmacists | 7,446 |
| Nurses | 70,057 |
| Nutritionists | 2,900 |
| Social services professionals | 25,747 |
| Ergotherapists, Inhalotherapists, Physiotherapists, Orthophonists, Audiologists | 6,277 |
| Total | 127,536 |
Most physicians work as independent entrepreneurs who are not employed by the provincial government, but reimbursed on a fee-for-service basis. They provide their services to local CSSSs, hospitals, primary healthcare facilities and services, or are affiliated with hospital outpatient departments.
Nurses are primarily employed in acute care institutions (hospitals); however, they also provide community healthcare, including home care and public health services. Important ancillary health professionals include pharmacists, nutritionists, criminologists, psychologists, social workers, functional therapists, inhalotherapists, physiotherapists, orthophonists, audiologists, and so forth.
5. Structure of Québec's Healthcare Delivery Organization
The province's healthcare system, similar to that of most other provinces and territories though somewhat differently organized, consists of provincial, regional, academic medical practice and, most importantly, local levels with varying responsibilities for healthcare planning, funding and delivery (Santé et Services sociaux Québec 2011e; Aqesss 2011a).
At the provincial level, the Ministère de la santé et des services sociaux is responsible for establishing the direction and assessment of healthcare and social services policies. Specifically, the MSSS plans, funds and allocates financial resources and oversees outcomes assessment of healthcare delivery throughout the province.
At the regional level, the Agence de la santé et des services sociaux (ASSS) develops policy directions and priorities, ensures the allocation of budgets to institutions and subsidies to community organizations, and exercises regional public health functions. The domain of each of the 18 regional ASSSs covers a specified geographic area (see Table 2). Among its specific responsibilities, the ASSS must "facilitate the deployment and management of local service networks … [and] also insure that the [local] population participates in the management of services.…" (Santé et Services sociaux Québec 2011e).
| Table 2. Québec Agence de la santé et des services sociaux (AQESSS) | ||||
| Headquarters | Population | Acute care facilities | Number of beds | Website |
| (01) ASSS du Bas-Saint-Laurent, Rimouski | 200,600 | 8 | 656 | https://www.agencesssbsl.gouv.qc.ca |
| (02) ASSS du Saguenay – Lac-Saint-Jean, Chicoutimi | 272,600 | 6 | 847 | https://www.regional02.ca |
| (03) ASSS de la Capitale-Nationale, Quebec City | 650,000 | 9 | 2,460 | https://www.agencesss04.qc.ca |
| (04) ASSS de la Maurice et du Centre-du-Québec, Trois-Rivières | 209,000 | 7 | 1,114 | https://www.agencesss04.qc.ca |
| (05) ASSS de l'Estrie, Sherbrooke | 303,000 | 8 | 1,158 | https://www.santeestrie.qc.ca/agence |
| (06) ASSS de Montréal, Montréal | 1,620,00 | 26 | 7,364 | https://www.santemontreal.qc.ca |
| (07) ASSS de l'Outaouais, Gatineau | 324,000, | 5 | 662 | https://www.santepublique-outaouais.qc.ca |
| (08) ASSS de l'Abitibi-Témiscamingue, Rouyn-Noranda | 146,000 | 6 | 472 | https://www.sante-abitibi-temiscamingue.gouv.qc.ca |
| (09) ASSS de la Côte-Nord, Baie-Comeau | 95,000 | 8 | 284 | https://www.agencesante09.gouv.qc.ca |
| (10) ASSS du Nord-du-Québec, Chibougamau | 40,000 | 1 | 38 | https://www.crsssbaiejames.gouv.qc.ca |
| (11) ASSS de la Gaspésie-Îles-de-la-Madeleine, Gaspé | 97,000 | 5 | 262 | https://www.agencesssgim.ca |
| (12) ASSS de Chaudière-Appalaches, Sainte-Marie | 397,000 | 5 | 1,361 | https://www.agencesss12.gouv.qc.ca |
| (13) ASSS de Laval, Laval | 369,000 | 2 | 584 | https://www.sssslaval.gouv.qc.ca |
| (14) ASSS de Lanaudière, Joliette | 429,000 | 2 | 627 | https://www.agencelanaudiere.qc.ca |
| (15) ASSS des Laurentides, St-Jérome | 90,000 | 5 | 973 | https://www.rrsss17phototheque.gouv.qc.ca/fra/intro.html |
| (16) ASSS de la Montérégie, Longueuil | 229,330 | 12 | 2,595 | https://www.rrsss16.gouv.qc.ca |
| (17) RRSSS (Régie régionale de la santé et des services sociaux) du Nunavik, Kuujjuaq | 11,000 | 2 | 54 | https://www.rrsss17.gouv.qc.ca/en/nunavik |
| (18) CCSSS (Conseil Cri de la santé et des services sociaux) de la Baie-James, Chisabibi | 13,000 | 1 | 36 | https://www.creehealth.org/ |
At the local level, healthcare delivery is organized around 95 CSSSs. As outlined above, the local CSSS is the heart of Québec's strategy for delivering healthcare that impacts and improves the personal lives of all residents. The CSSS provides and coordinates prevention and health assessment services, as well as general and specialized hospital services, to the public in a local district. Typically, a CSSS is organized around a hospital and integrates one or a few community care centres and long-term care sites into an integrated local healthcare delivery entity including, among others, public health, family physicians or groups of physicians, community pharmacies, and clinics and hospitals for secondary and tertiary care referrals. Specifically, most CSSSs include the following institutions (The Québec Health and Social Services System 2011a):
- Centre d'hébergement de soins de longue durée (CHSLD), or residential and long-term care centre, provides services both to people with decreasing autonomy and the elderly
- Centre hospitalier (CH), or hospital centre, provides short-term first-line, second-line and third-line general, specialized and psychiatric healthcare services. Across the province's 95 CSSSs, there are 121 in-patient acute care CHs
- Centre de réadaptation (CR), or rehabilitation centre, offers healthcare and social services to people with physical, intellectual, or developmental disabilities and to people with addiction problems
- Centre de protection de l'enfance et de la jeunesse (CPEJ), or child and youth protection centre, provides a wide variety of services to young people who have developmental or behavioural problems and their families
- Centre local de services communautaires (CLSC), or community health clinic, offers a wide variety of services including psychological and health services; there are 147 CLSCs across the province's 95 CSSSs
In addition, four Réseaux universitaires intégrés de santé (RUIS), or integrated university health networks, ensure delivery of specialized and highly specialized care to all regions of Québec (Atlas de la Santé et des Services sociaux du Québec 2011; RUIS McGill 2011). The primary mandate of the four RUISs, each of which is affiliated with one of the province's four universities that include a faculty of medicine (see below for descriptions of CHUS, CHUQ, CUSM and CHUM), is to make recommendations to the MSSS and the province's health and social services agencies on:
- The provision of service, the establishment of corridors of service and the prevention of breaks in service in institutions in all regions of Québec
- Medical training and distribution of students, coordination of research activities and knowledge transfer
- The organization of specialized medical services to enhance their effectiveness and avoid duplication
- The development of a university medical staffing plan in relation to the regional medical staffing plan
D. Provincial e-Health – Québec's Electronic Health Record
The Ministère de la Santé et des Services sociaux manages the province's most structured, complex and comprehensive e-Health initiative, namely, the Dossier de santé du Québec, or the province's Electronic Health Record (sometimes referred to as le Système d'échange d'information en santé, or health information exchange [HIE]) (Santé et Services sociaux Québec 2011c). The goal of the DSQ/EHR is the creation of a seamless integrated, interoperable and sharable DSQ/EHR of patient data on all Québec residents. Foundational sources of patient data feeding the DSQ/EHR are laboratories, pharmacies and diagnostic imaging repositories (Bolduc 2011a, 2011b). Equally important to implementing a robust patient DSQ/EHR in a reasonable time period will be the exchange and integration, via access to a provincial viewer, of existing patient demographic and clinical information residing on a hospital's Dossier clinique informatisé, or acute hospital electronic medical record, on a physician office's Dossier médical électronique, or physician office EMR, and in other patient information sources. Also important will be the contribution of Québec's Centre de services partagés du Québec with its Réseau intégré de télécommunications multimédia (RITM).
|
In the Québec environment, "Dossier clinique informatisé" (DCI), or acute hospital EMR in American terms, refers normally to the acute care environment, but could also include the "ambulatory or community" services delivered by a CSSS or a hospital. In the physician office space, Québec's electronic solution is referred to as the "Dossier médical électronique" (DMÉ), or physician office EMR in American terms. Finally, Québec's "Dossier de santé du Québec" (DSQ), or electronic health record (EHR), involves the exchange of patient information between healthcare stakeholders, including connectivity to registries (namely Patients, Providers, Facilities, Consent) and provincial domain clinical data repositories (CDR) (namely laboratory, diagnostic imaging, medication or pharmacy). In most other Canadian jurisdictions – including western and northern provinces and territories, Ontario and some Atlantic province providers – EMR refers normally to the ambulatory environment of physician offices, health centres or outpatient clinics; while electronic patient record (EPR) refers – as for most provincial RHAs, DHAs, Health Regions or LHINs – to the in-patient hospital environment. EHR, as described above for Québec, is universally recognized across Canada. |
The DSQ/EHR's patient health record will contain the following personal health information components, which are generally considered by healthcare professionals to be most useful for clinical treatment, especially for emergency procedures: patient identity; providers; laboratory test results; diagnostic imaging results; pharmacy medication and dosage schedule list; electronic medication prescriptions from physician offices; allergies and intolerances. The major clinical and back-office components of the DSQ/EHR, which will provide this information in a single patient record, include the following (Vérificateur général du Québec 2010):
- Health Information Access Layer (HIAL): providing communications management and access control to health records
- Patient Consent Registry and Management Services
- Master Patient Index and Client Registry
- Provider Registry
- SecurSanté: a system of certification, authentication and identification of provider access
- Three clinical domains, with patient information being saved in supra-regional or provincial repositories:
- Le Domaine laboratoire: warehousing results from public biomedical laboratories
- Le Domaine médicament: Système québecois d'Information sur les médicaments (SQIM), providing a pharmacological profile including prescription records from the province's community pharmacies – L'Association québecoise des pharmaciens propriétaires (AQPP)
- Le Domaine imagerie médicale: PACS implementation or replacement for the entire province, plus three repositories of diagnostic images, reports and orders located in each of the three cities in a geographical RUIS; these three repositories, by providing a unified view for clinicians through a standardized index, XDSi, would assemble data from public and private organizations
- Panorama: the pan-Canada public health system for surveillance and health protection in the area of infectious diseases
- Télésanté: systems supporting inter-facility telehealth, téléformation, téléconsultation and télétriage–beside the other existing telehealth initiatives
- Integrated Services for the Elderly Network
- Visualiseur du DSQ/EHR Viewer: providing interoperable access to and viewing of the interfaced provincial electronic patient health information resources
A regional pilot version of the DSQ/EHR was announced for the ASSS de la Capitale-Nationale in January 2010 (following on an earlier experimental phase in 2008–2009). Facilities involved in the pilot for ASSS de la Capitale-Nationale include primary care clinic sites such as groupes de médecine familiale (GMF) (5), community pharmacies (31), public facilities for laboratory testing, three acute care facilities of the le Centre hospitalier universitaire de Québec (CHUQ), two centres hospitalier affilié universitaire de Québec (CHA) (5), and all public facilities offering diagnostic imaging in ASSS de la Capitale-Nationale.
In mid-2011, the MSSS announced that expanded implementation of the province's DSQ/EHR is also under way in the ASSS de l'Estrie and ASSS de Lanaudière (Santé et Services sociaux Québec 2011d). In October 2011, Assistant Deputy Minister Verreault also announced that a fourth region, in the Montreal area, would commence integration of its DCI/Acute EMR and other e-Health networks to the provincial DSQ/EHR in 2012.
E. Québec's Hospital and Physician Office Electronic Medical Records
As mentioned above, much of the patient information essential to developing a comprehensive and integrated DSQ/EHR – such as patient medical histories, provider notes and orders – resides on hospital DCI/EMRs and physician office DMÉ/EMRs, which will need to be interfaced to the provincial DSQ/EHR via HIAL technology. Hospital DCI/EMR projects are under way in most of the provinces' ASSSs. Prominent among these hospital DCI/EMR projects are those involving the four academic/teaching consortiums located in Sherbrooke, Québec City and Montréal (two).
-
Le Centre hospitalier universitaire de Sherbrooke (CHUS), with 557 combined acute care beds (including general medical, surgery, intensive and intermediate, pediatrics, mothers and babies and neonatology) at two in-patient facilities (l'Hôpital Fleurimont and l'Hôtel-Dieu), is the fourth largest, by population base, of Québec's four hospital/academic medical centres. CHUS serves a population of approximately 303,000 residents in the Estrie region, or Eastern Townships. Additionally, as a teaching hospital complex, CHUS co-partners with the Faculty of Medicine and Health Sciences (medical school) at l'Université de Sherbrooke to provide tertiary services for more than 1 million, or 13.49%, of Québec residents.
CHUS's DCI/EMR, Ariane, operates on Quadramed's Computerized-Patient Record (QCPR) (CHUS 2011). QCPR has been installed for clinical data repository (CDR), clinical decision support system (CDSS), electronic order entry (OE), computerized physician order entry (CPOE) and physician documentation. All physicians are required to use CPOE; and currently 75% of all medication orders are captured using CPOE. With regard to nursing care, CHUS has implemented nursing documentation. It has acquired but not yet implemented Quadramed's electronic medication administration record (eMAR) solution. As of spring 2011, CHUS has also implemented Ariane's QCPR DCI/EMR solution for all ancillary clinical applications, including laboratory and radiology information systems, as well as the pharmacy management system. Bar-coding, which improves the accuracy of the patient record and patient safety, is currently live and operational only for laboratory. Ten PACS modules employing the Toshiba PACS solution are live and operational at both CHUS hospitals (HIMSS Analytics 2011c).
-
Le Centre hospitalier universitaire de Québec (CHUQ), with 883 combined beds at three in-patient acute care facilities (l'Hôtel-Dieu de Québec, l'Hôpital Saint-François d'Assise and le Centre hospitalier de Université Laval), as well as affiliated teaching hospitals, is the third largest, by population base, of Québec's four hospital/academic medical centres. CHUQ serves a population of approximately 650,000 residents in the ASSS de la Capitale-Nationale. Additionally, as a teaching hospital complex, CHUQ co-partners with the Faculty of Medicine at l'Université Laval to provide tertiary services for more than 1.7 million, or 22.8%, of the province's residents.
CHUQ's DCI/EMR, Cristal-Net, is an open source, internet-based solution for interfacing and integrating existing clinical application suites at multiple hospitals to deliver a single patient electronic health record. The Cristal-Net solution was developed in conjunction with the CHU of Grenoble, France, ten years ago (CHUQ 2011). CHUQ's Cristal-Net DCI/EMR solution provides CDR and CDSS capabilities, along with OE. Cristal-Net is also the portal for nursing documentation, which is reportedly used by 100% of the hospitals' nurses. As of spring 2011, CHUQ's three hospitals have implemented SAP/Technidata's TD-Synergy's laboratory information system, Québec-based Artéfact Informatique's Syphac solution for a pharmacy management system and Lawson's Healthvision/Medrad product for the radiology information system. Bar-coding has been implemented for all three ancillary clinical applications. AGFA is the vendor for 10 PACS modules, which are live and operational at the three CHUQ hospitals (HIMSS Analytics 2011b).
-
Le Centre universitaire de santé McGill (CUSM): with 899 combined acute care beds at three major in-patient acute care facilities (l'Hôpital Royal Victoria, l'Hôpital général de Montréal and l'Hôpital de Montréal pour enfants), as well as affiliated teaching hospitals, is the second largest, by population base, of Québec's four hospital/academic medical centres. CUSM serves a population of approximately l.62 million residents in the metropolitan region of Montréal (along with CHUM, discussed below). Additionally, as a teaching hospital, CUSM co-partners with the McGill Faculty of Medicine at McGill University to provide tertiary care for more than 1.743 million, or 23%, of Québec's residents.
CUSM's clinical information system (CIS), or DCI/EMR, operates on Telus Health Solutions' OACIS hospital EHR. Thus far, CUSM reports having brought OACIS live and operational for its CDR, CDSS, OE and nursing documentation, with 20% of nurses using the clinical solution. OACIS' CPOE solution is in preparation. The three CUSM in-patient hospitals report using Cerner's laboratory information system, GE's Centricity solution for a pharmacy management system and Intelerad's Intelepacs radiology information system. Bar-coding is implemented for all ancillary systems at the three facilities. CUSM has nine PACS modules live and operational. Digital mammography, which is currently on film, will be transitioned to PACS in the near future. The PACS suite is integrated with CUSM's DCI/EMR (HIMSS Analytics 2011d).
-
Le Centre hospitalier de l'Université de Montréal (CHUM), with 1,161 combined acute care beds at three inpatient facilities (l'Hôtel-Dieu, l'Hôpital Notre-Dame and l'Hôpital Saint-Luc), and affiliated teaching hospitals, is the largest, by population base, of Québec's four hospital/academic medical centres. CHUM, along with CUSM, also in Montréal, serves a population of more than 1.62 million residents in the Montréal region. Additionally, as a teaching hospital, CHUM co-partners with the Faculty of Medicine at l'Université de Montréal to provide tertiary care for more than 1.743 million, or 23%, of Québec's residents.
CHUM's DCI/EMR initiative, Système d'information clinique (SIC), operates on Telus Health Solutions' OACIS hospital EHR. Thus far, CHUM has brought OACIS live and operational for its CDR, CDSS, physician documentation and some nursing documentation. CHUM's three in-patient hospitals currently operate the Meditech solution for the laboratory information system (which is planned for replacement in the near future) and pharmacy management system. The radiology information system is provided by Artéfact Informatique – IBM's Radimage. Bar-coding is implemented for all ancillary systems at the three CHUM facilities. AGFA's Impax product is implemented for nine PACS modules, but not nuclear medicine. The radiology information system is integrated with CHUM's DCI (HIMSS Analytics 2011e).
Québec has also initiated a project to expand adoption by the province's groupes de médecine familiale (GMF) of physician office DMÉ/EMR solutions (Santé et Services sociaux Québec 2011a). In particular, physicians will be able to access medication information directly via a module of the DMÉ/EMR. For 2011–2012, approved DMÉ/EMR vendors will be announced in stages. In February 2011, the MSSS announced four DMÉ/EMR vendors whose solutions meet all required functionality criteria. These vendors are Kinlogix Medicin, Omni-Med's Clinique médicale virtuelle, Purkinje-Dossier and Logiciels INFO-DATA's MED-Office (Info GMF Express 2011).
Additionally, Le Centre de services partagés du Québec, the province's shared services organization, has initiated the Réseau intégré de télécommunications multimédia (RITM), which will facilitate data exchange among Québec's healthcare stakeholders participating in the DSQ/EHR. RITM will integrate two existing telecommunications networks focused, in the first instance, on social and health telecommunications and, in the second instance, on multimedia telecommunications. The integrated network will be accessed by 350 health and social service organizations, as well as by 160 ministries. For instance, RITM's network allows physicians, no matter what their location, to share and exchange medical images with other authorized health professionals. RITM's main characteristics are end-to-end security management, guaranteed integrity and permanence of information, personal information protection mechanisms, and interoperability (Centre de services partagés 2011).
F. Measuring Québec's Hospital DCI/EMR Capabilities with the HIMSS Analytics Acute EMRAM
In light of recent investments and efforts by the MSSS and the province's healthcare stakeholders in diverse yet interconnected e-Health integration projects – namely, DSQ/EHR, acute care DCIs/EMRs, DMÉs/Physician EMRs and other e-Health implementations – it is timely for the province to undertake an inventory of its e-Health IT/IS/IM capabilities. Measurement of the types and stages of electronic clinical connectivity at Québec's acute hospitals – followed by measurement of its ambulatory and physician office facilities and eventually of all health and social service facilities and services in each of the 18 regions – would establish a reliable and rigorous information base about the operational status of hospital DCI/EMR clinical solutions throughout the province. Armed with an acute healthcare IT inventory and measurement, the province's stakeholders can more effectively plan and schedule how and when it will be possible to implement effective interoperability among the full array of the province's healthcare facilities. The twofold goal of the three-phase acute and ambulatory data collection effort, spread out over the next 18 months – which is currently under way by AQESSS and HIMSS Analytics with the agreement of the MSSS and province's health organizations – is to provide a comprehensive healthcare IT inventory and e-Health implementation measurement for all acute and ambulatory healthcare facilities in Québec.
Why is the HIMSS Analytics Canadian ICT Study a valuable inventory tool – worth Québec's investment of time and effort – for all Canadian healthcare delivery organizations to use in measuring their clinical e-Health progress? Since 2007, Canadian providers have increasingly participated in the HIMSS Analytics Canada ICT Study in order to access the HIMSS Analytics Electronic Medical Record Adoption Model score and collateral benchmarking reports. The methodology and algorithms of the hospital EMRAM Score are currently used to automatically score more than 600 Canadian acute care facilities, which have participated in the 2011 Canada ICT Study, and more than 5,000 US hospitals. In particular, the annual survey targets detailed information about an acute care hospital's DCI/EMR environment. Those providers completing the entire acute study can access 76 combined regional and hospital benchmarking reports, which HIMSS Analytics makes available to regional healthcare organizations and their acute facilities. Of the 76 benchmarking reports, 47 are regional reports and 29 are hospital reports that compare a region or facility's capabilities to those of other regional organizations or acute facilities based on factors such as IS department operating budget, nurse full-time equivalents (FTEs), IS department FTEs and EMRAM scores.
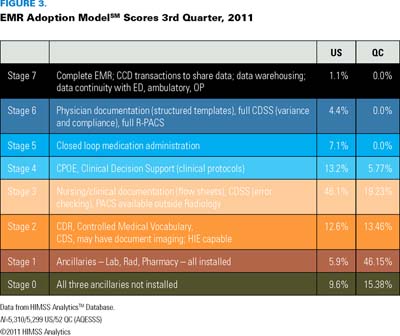
What is the HIMSS Analytics EMRAM score, which is currently provided for acute facilities – and will also be available for ambulatory facilities in late 2012 – and why is it useful for healthcare providers and stakeholders? The acute care EMRAM Score measures levels of electronic or paperless acute care DCI/EMR capabilities. The scale of measurement ranges from limited ancillary department systems to a fully electronic environment on a continuum of eight stages from zero to seven (see Figure 2).
Stage 7 of the HIMSS Analytics EMRAM requires that clinical information be readily shared via electronic transactions, or exchange of electronic records, between other healthcare organizations, government entities and patients in the US, Canada or globally. For US acute care facilities, most of which operate as stand-alone facilities, it is normally only at Stage 7 that clinical information – such as laboratory, drug and diagnostic imaging results – can be readily shared with other organizations via electronic transactions, or exchange of electronic records, through participation in what, in the US, is termed a health information exchange. The American HIE often operates on HIAL technology similar to that being proposed by various stakeholders in Québec, as well as by other provinces or territories and Canada Health Infoway, as a more effective and efficient way of securing interoperability at the regional and provincial levels.
By contrast, as early as Stage 2 in Québec, and likewise in most other Canadian provinces and territories, there has been significant development of regional and province-wide inter-facility patient information sharing initiatives, or what is known in Québec as un système d'échange d'information en santé. In Québec, important data exchanges between healthcare organizations include the province's three diagnostic imaging repositories, which are fed images by local or regional PACS solutions; the Services québécois d'information sur les médicaments, or SQIM, which will be fed medication data by the community pharmacies; and the provincial Système d'information intégré sur les activités transfusionnelles et d'hémovigilance, or SIIATH, the laboratory blood bank repository. The data exchanged inter-organizationally on extended local, regional or provincial levels will be accessible by the Visualiseur du DSQ, or provincial EHR Viewer.
Since 2008, HIMSS Analytics has published EMRAM scores for Canadian hospitals, based on the most recent data collection for the acute care environment across the ten provinces, Yukon, Northwest Territories and Nunavut. The annual status of Canada's progress at implementing a comprehensive e-Health strategy for acute care facilities in ten provinces and three northern territorial jurisdictions is documented quarterly in the HIMSS Analytics Canada EMR Adoption ModelSM scores.
The first reliable scores for Québec facilities became available early in fall 2011, based on the previously mentioned acute care data collection collaboration between AQESSS/MSSS and HIMSS Analytics that has been under way since spring 2011. It should be noted that even these scores reflect only acute care data collected thus far for slightly less than 50% of the province's 121 acute care facilities. See Figures 3 and 4 for the EMR Adoption Model ScoresSM 3rd Quarter, 2011, for Québec's participating 52 hospitals as measured in relation to the US and for the rest of Canada.
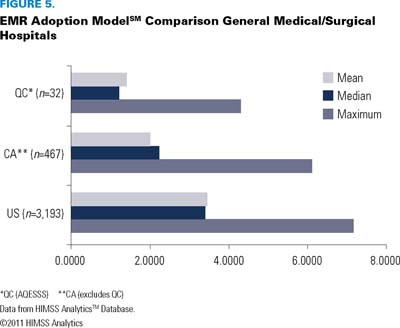
As Figure 5 indicates, preliminary EMRAM scores for Québec's academic/teaching hospitals are comparable to those for similar acute academic facilities in the other Canadian provinces. For 18 of Québec's 26 hospitals, designated as academic/teaching facilities, which completed HIMSS Analytics' acute ICT Canada Study, the median EMRAM score was 3.0, by comparison with a median EMRAM score of 2.1 for academic medical facilities in the other provinces and territories.
G. Conclusion
Now that Québec has begun implementing a comprehensive and interoperable provincial e-Health vision, the province's CSSSs, CHUs, ASSSs and the MSSS are well positioned to take advantage of the anticipated resource outcomes of the newly formed AQESSS/MSSS-HIMSS Analytics collaboration. The anticipated benefits include the following:
- To develop a rigorous and reliable inventory of Québec's healthcare IT capabilities at the acute, ambulatory/primary care and other levels
- To deliver EMRAM scores for participating acute care and ambulatory facilities, and benchmarking reports, for hospitals, CSSSs and ASSSs
- To enhance the knowledge base of the province's providers and healthcare stakeholders for assessing how to proceed in developing their acute DCI/EMR capabilities, especially in its interoperable dimensions
- To advance to the higher stages of the EMRAM – involving error-checking, closed loop medication, advanced analytics, and so forth – enabling integration of a wider set of patient information and more advanced clinical software applications in the clinical decision-making process that enhances the probabilities of establishing meaningful correlations between levels of IT capacity and measurements of clinical and safety outcomes
Access to HIMSS Analytics' inventory of Québec IT information and measurements will provide provincial, regional and local stakeholders with an accurate and rich method of assessing the preparedness of Québec's acute care service providers to participate in the province's DSQ/EHR initiatives. In particular, such IT information and measurements will contribute to furthering the exchange of health information across organizations needed to support the province's clinical priorities, namely, chronic disease management, elderly services management, cancer prevention and treatment, mental health, and so forth. Improving patient clinical outcomes in these areas depends on realizing the information exchange potential of the province's DSQ/EHR, since effective medical treatment of these conditions relies heavily on sharing and exchanging patient-related information among diverse clinicians affiliated with different provider organizations.
To be sure, the inventory and measurement efforts currently under way in Québec's acute care environment are not adequate to address the province's clinical IT information needs. E-Health measurement in Québec's acute care environment must be supplemented by the adoption of other e-Health adoption and maturity models that assess the IT capabilities and utility of the entire continuum of healthcare delivery, from the local RLS/CSSS to the regional/ASSS and RUIS levels. To that end, HIMSS Analytics' Ambulatory Study and EMRAM Score, to debut in 2012, are designed to inventory and measure levels of DCI/EMR solutions in the non-acute environment of outpatient facilities and DMÉ/EMR solutions in health centres, speciality clinics and physician offices. The Ambulatory EMRAM measures facilities and services on a continuum of six stages from 0 to 5, ranging from an entirely paper environment to a fully electronic adoption level. As well, eventually, procedures need to be developed for applying existing acute and ambulatory EMRAM tools to other dimensions of the healthcare continuum, in Québec and elsewhere, such as Community Services, Youth Services, Mental Health Services, and so forth.
Until the province's blueprint for province-wide clinical interoperability is grounded on sound and comprehensive knowledge of real clinical needs and reliable IT information – keeping in mind the resource shortages faced by Québec's healthcare stakeholders – it remains difficult for e-Healthcare stakeholders to measure meaningful use or return on investment (ROI) of the province's e-Health strategy for supporting and enhancing the quality and safety of care delivery for all residents.
However, once the province's stakeholders are armed with a reliable inventory and measurement of the kind and degree of hospital DCI/EMR and physician office DMÉ/EMR capacity that is currently operational at, or planned for, the province's acute facilities and extensive ambulatory and physician office environment, then Québec will be better prepared to assess the best ways – keeping in mind the pervasive resource shortages mentioned above – of planning for and investing in the full continuum of healthcare through the enabling functionality of the province's DSQ/EHR, hospital DCI/EMR and physician DMÉ/EMR. If the province is to deliver on its promise of implementing an inter-organizational patient data exchange platform and a comprehensive patient EHR for all Québec residents by the newly announced projected completion date of 2016, then it is essential for the province to persevere in its adoption of the inventory and measurement tools outlined above for the sake of confirming and enhancing the viability of Québec's all-important interoperable DSQ/EHR strategy.
About the Author(s)
Patrick Powers, PhD, is a Senior Research Manager at HIMSS Analytics with oversight responsibility for the Canada ICT database and research, and a visiting professor in humanities, philosophy and government at several American colleges and universities, most recently at Thomas More College of Liberal Arts in Merrimack, NH.
References
Aqesss – Association québecoise d'établissements de santé et de services sociaux. 2011a. "Le Réseau de la Santé – Québécois." Unpublished Study.
Aqesss – Association québécoise d'établissements de santé et de services sociaux. 2011b. "Organisation – Au service de ses membres." Retrieved August 30, 2011. <http://www.aqesss.qc.ca/409/Organisation.aqesss>.
Atlas de la Santé et des Services sociaux du Québec. "Réseaux universitaires intégrés de santé." 2011. Retrieved December 27, 2011. <http://www.msss.gouv.qc.ca/statistiques/atlas/atlas/index.php?id_carte=86>.
Bolduc, Y. 2011a, March 22. "Le point sur l'informatisation du réseau de la santé – Le Ministre Yves Bolduc mise sur l'informatisation pour optimizer l'offre de soins." Retrieved September 4, 2011. <http://209.171.32.187/gouvqc/communiques/GPQF/Mars2011/22/c5285.html>.
Bolduc, Y. 2011b, March 22. "Informatisation du réseau de la santé et des services sociaux du Québec." <www.msss.gouv.qc.ca/documentation/salle-de-presse/medias/CPPT_v6d.pps>.
Bureau de programme pour l'informatisation du RSSS. 2011. Retrieved December 28, 2011. <http://msssa4.msss.gouv.qc.ca/extranet/ri.nsf/04bdef86723b0cf8852566de004c8583/cba99b6aad51e11d85257927005c7be3?OpenDocument>.
Centre de services partagés. 2011. "Infrastructures de télécommunications." Retrieved December 23, 2011. <http://www.cspq.gouv.qc.ca/reseau/ressources-informationnelles/communications-informatiques.asp>.
Chodos, H. 2001, February 26. Québec's Health Review – The Clair Commission. Retrieved December 21, 2011. <http://publications.gc.ca/collections/Collection-R/LoPBdP/BP/prb0037-e.htm>.
CHUQ – Le Centre hospitalier universitaire de Québec. 2011. "Nouvelles." Retrieved August 30, 2011. <http://www.chuq.qc.ca/fr/actualites/nouvelles/module_iplan.htm>.
CHUS – Le Centre hospitalier universitaire de Sherbrooke. 2011. "Dossier clinique informatisé Ariane." Retrieved August 30, 2011. <http://www.chus.qc.ca/fr/pointes-dexcellence/dossier-clinique-informatise-ariane/>.
Health and Welfare Commissioner. 2009. 2009 Appraisal Report on the Performance of Québec's Health and Social System. Retrieved December 18, 2011. <http://www.csbe.gouv.qc.ca/fileadmin/www/RapportAppreciation/csbe_RethinkingHowThingsSummary.pdf>.
HIMSS Analytics. 2011a. "About HIMSS Analytics." Retrieved August 30, 2011. <http://www.himssanalytics.org/general/about.asp>.
HIMSS Analytics. 2011b, August. HIMSS Analytics Canada Technologies and Applications Study for ASSS de la Capitale-Nationale – Hôtel-Dieu, Hôpital Saint-François d'Assise and Centre Hospitalier de Université Laval. Unpublished Study.
HIMSS Analytics. 2011c, August. HIMSS Analytics Canada Technologies and Applications Study for ASSS de l'Estrie – Hôpital de Fleurimont and Hôtel-Dieu. Unpublished Study.
HIMSS Analytics. 2011d, August. HIMSS Analytics Canada Technologies and Applications Study for ASSS de Montréal – Hôpital Royal Victoria, Hôpital général de Montréal and Hôpital de Montréal pour enfants. Unpublished Study.
HIMSS Analytics. 2011e, August. HIMSS Analytics Canada Technologies and Applications Study for ASSS de Montréal – Hôtel-Dieu, Hôpital Notre-Dame and Hôpital Saint-Luc. Unpublished Study.
Immigration et Communautés culturelles Québec. 2006. Caractéristiques de la population et démographie. Retrieved December 22, 2011. <http://www.immigration-quebec.gouv.qc.ca/fr/avantages/societe/population-demographie/index.html>.
Info GMF Express. 2011, April. "Bulletin d'information des groups de médecine de famille (GMF). Announce de solutions DME homologues pour 2011–2012." Unpublished bulletin.
Institut d'études prospectives technologiques. 2004. "Executive Summary – eHealth in the Context of a European Ageing Society – A Prospective Study." Retrieved December 22, 2011. <http://fiste.jrc.ec.europa.eu/pages/detail.cfm?prs=1207>.
Institut de la statistique du Québec. 2009, mars. Le Québec chiffres en main, édition 2009. Retrieved December 22, 2011. <http://www.stat.gouv.qc.ca/publications/referenc/pdf2009/QCM2009_fr.pdf>.
Journal des débats de la Commission de l'administration publique, 39 législature, 2 session (début 23 février 2011), Vol. 42 N° 3, 1, pp. 40f. 2011a, septembre 22. "Audition de la Commission de l'administration publique, Entendre le sous-ministre de la Santé et des Services sociaux concernant la Vigie relative au projet Dossier de santé du Québec." Retrieved December 26, 2011. <http://www.vgq.gouv.qc.ca/fr/fr_publications/fr_Audition-CAP/fr_Audition-CAP-2010-2011-T1-Chap5_2010-2011-T2-Chap3.pdf>.
Journal des débats de la Commission de l'administration publique, 39 législature, 2 session (début 23 février 2011), Vol. 42 N° 3, p. 40. 2011b, septembre 22. "Rapport de la Commission de l'Administration publique, Entendre le sous-ministre de la Santé et des Services sociaux concernant la Vigie relative au projet Dossier de santé du Québec." Retrieved December 26, 2011. <http://www.vgq.gouv.qc.ca/fr/fr_publications/fr_Audition-CAP/fr_Audition-CAP-2010-2011-T1-Chap5_2010-2011-T2-Chap3.pdf>.
"Les dossiers médicaux informatisés fonctionneront dans cinq ans, promet Bolduc." 2011, March 22. Retrieved November 15, 2011. <http://www.ledevoir.com/societe/sante/319349/les-dossiers-medicaux-informatises-fonctionneront-dans-cinq-ans-promet-bolduc>.
Madore, O. 2005, May 16."Parliament of Canada, The Canada Health Act: Overview and Options." Retrieved September 9, 2011. <http://www.parl.gc.ca/Content/LOP/ResearchPublications/944-e.htm>.
Monrozier, X. J. IRIS Europe – Initiatives Régionales – Innovations et Stratégies. "Analyses – TIC et santé. " Retrieved 22, 2011. <http://www.iris-europe.eu/spip.php?article3481>.
National Assembly, First Session, Thirty-Ninth Legislature. Projet de loi no. 100 (2010, chapitre 20). 2010, June 12. An Act to Implement Certain Provisions of the Budget Speech of 30 March 2010, Reduce the Debt and Return to a Balanced Budget in 2013–2014. Retrieved December 26, 2011. <http://www2.publicationsduquebec.gouv.qc.ca/dynamicSearch/telecharge.php?type=5&file=2010C20A.PDF>.
National Assembly, First Session, Thirty-Seventh Legislature. Projet de loi no. 83 (2005, chapitre 32). 2005, November 30. An Act to Amend the Act Respecting Health Services and Social Services and Other Legislative Provisions. Retrieved December 26, 2011. <http://www2.publicationsduquebec.gouv.qc.ca/dynamicSearch/telecharge.php?type=5&file=2005C32A.PDF>.
National Assembly, Second Session, Thirty-Ninth Legislature. 2011, June 13. Projet de loi no 133 (2011, chapitre 19). An Act Respecting the Governance and Management of the Information Resources of Public Bodies and Government Enterprises. Retrieved December 26, 2011. <http://www2.publicationsduquebec.gouv.qc.ca/dynamicSearch/telecharge.php?type=5&file=2011C19A.PDF>.
Powers, Patrick. 2011, Octobre 13. Aqesss – Association québécoise d'établissements de santé et de services sociaux, Salle des nouvelles – Archives 2011. "Une première évaluation scientifique." Retrieved November 26, 2011. <http://www.aqesss.qc.ca/1852/Archives_2011.aqesss>.
RUIS McGill. 2011 "What Is RUIS?" Retrieved December 1, 2011. <http://www.medicine.mcgill.ca/ruis/home_whatisRUIS.htm>.
Santé et Services sociaux Québec. 2011a. "À propos des GMF." Retrieved September 4, 2011. <http://www.msss.gouv.qc.ca/sujets/organisation/gmf/index.php?a-propos-fr>.
Santé et Services sociaux Québec. 2011b. "Centres de santé et de services sociaux – RLS." Retrieved 27 December 2011. <http://www.msss.gouv.qc.ca/reseau/rls/>.
Santé et Services sociaux Québec. 2011c. "Le Dossier de santé du Québec." Retrieved August 30, 2011. <http://www.dossierdesante.gouv.qc.ca/fonctionnement-du-dossier-de-sante.phtml>.
Santé et Services sociaux Québec. 2011d. "Les régions participant au projet du DSQ." Retrieved August 30, 2011. <http://www.dossierdesante.gouv.qc.ca/fr_citoyens_experimentation.phtml>.
Santé et Services sociaux Québec. 2011e. The Québec Health and Social Services System in Brief. Retrieved August 30, 2011. <http://msssa4.msss.gouv.qc.ca/en/document/publication.nsf/ff52dbec0b2ed788852566de004c8584/bb002a2ad3cb32ee8525753c00650ca1?OpenDocument>.
Statistics Canada. 2011, June 22. "Canada's Population Estimates." Retrieved August 30, 2011. <http://www.statcan.gc.ca/daily-quotidien/110622/dq110622a-eng.htm>.
Task Force on Health Funding. 2008, February. Report of the Task Force on the Funding of Health Care. Getting Our Money's Worth. Retrieved December 19, 2011. <http://www.financementsante.gouv.qc.ca/financementsante/en/rapport/pdf/RapportENG_FinancementSante.pdf>.
The Québec Health and Social Services System. 2011a. "Establishments Formed into Networks." Retrieved November 10, 2011. <http://www.msss.gouv.qc.ca/sujets/organisation/ssss_enbref/index.php?reseau_en>.
The Québec Health and Social Services System. 2011b. "Other Characteristics." Retrieved 26 December 2011. <http://www.msss.gouv.qc.ca/sujets/organisation/ssss_enbref/index.php?autres_caracteristiques_en>.
Vérificateur général du Québec. 2010, mai 12. Rapport du vérificateur général du Québec à l'Assemblée nationale pour l'année 2010-2011, Tome 1 Chapitre 5.111. Retrieved November 10, 2011. <http://www.vgq.gouv.qc.ca/fr/fr_publications/fr_rapport-annuel/fr_2010-2011-T1/fr_Rapport2010-2011-T1-Chap05.pdf>.
Vérificateur général du Québec. 2011, May 4. Rapport du Vérificateur général du Québec à l'Assemblée nationale pour l'année 2010-2011,Tome II, chapitre 3/Report of the Auditor General of Québec to the National Assembly for 2010–2011 – Volume II, Highlights. Retrieved August 30, 2011. <http://www.vgq.gouv.qc.ca/en/en_publications/en_rapport-annuel/en_fichiers/en_Highlights2010-2011-T2.pdf>.
Verreault, L. 2011, October 13. "Un Réseau, Une Vision, Une Gouverne." Unpublished Allocution. Summary found at <http://www.aqesss.qc.ca/1852/Archives_2011.aqesss>. Retrieved December 1, 2011.
Footnotes
1For a full description of the six Stages of the future Ambulatory EMRAM score, see: HIMSS Analytics EMR Adoption Model: http://www.himssanalytics.org/hc_providers/emr_adoption.asp.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed