Healthcare Policy
The Use of Registered Nurses to Perform Flexible Sigmoidoscopy Procedures in Ontario: A Cost Minimization Analysis
Sarah E. Costa, Peter C. Coyte, Audrey Laporte, Laura Quigley and Shannon Reynolds
Abstract
Rationale: Rates of colorectal cancer (CRC) are on the rise in Canada. Flexible sigmoidoscopy (FS) is an initial screening test for CRC primarily used in adults aged 50 years and older at average risk for the disease. Physicians and registered nurses have been shown to have the same effectiveness in performing a FS procedure. This paper presents an analysis of the use of registered nurses (RN) compared to physicians in Ontario to assess costs to the healthcare system.
Objectives: To evaluate whether FS performed by RNs is a less costly alternative to increase access to CRC screening capacity in Ontario.
Methodology: A cost minimization analysis was conducted from a health system perspective.
Discussion: RN-performed FS is a viable alternative for increasing CRC screening capacity in Ontario. Remuneration schedules for on-call physicians must be taken into consideration if policies are developed for the implementation of RN screening procedures.
Results: The findings suggest that the use of RNs may be cost saving compared to physician-performed FS procedures, depending on physician remuneration.
Ontario has one of the highest rates of colorectal cancer (CRC) in the world (MOHLTC 2010a). According to the Canadian Cancer Society, one in 13 men and one in 16 women will develop CRC during their lifetime, with CRC being the fourth most common cancer behind breast, prostate and lung cancers (Canadian Cancer Society 2011a,b). Increasing age can lead to greater prevalence of and mortality from CRC; considering the rise in Canada's aging population, the number of individuals eligible for screening for this disease will only increase over time (Canadian Cancer Society et al. 2008).
CRC has a long pre-malignant phase, which is both easily identified and treated, making it an ideal candidate for screening (Schultz et al. 2004). The chances of survival and cure for colorectal cancer greatly increase the earlier the cancer is detected – for instance, the chances of survival rise to nearly 90% when caught in earlier stages compared to just 10% in later stages of disease progression (Cancer Care Ontario 2008). Therefore, it is important that access to CRC screening is made available for average-risk individuals in Ontario, that is, persons aged 50 years or older with no family history of the disease (Kielar and El-Maraghi 2008; Schoenfeld 1999; Schoenfeld et al. 1999a,b,c; Wong 1999).
Healthcare interventions targeted at prevention and early detection have the potential to yield positive benefits for the healthcare system by mitigating future treatment costs, enhancing population health and assisting in health system sustainability. Flexible sigmoidoscopy offers a practical approach to increasing screening capacity for CRC. In Ontario, four procedures are available for screening, three of which are invasive: flexible sigmoidoscopy (FS), colonoscopy and double-barium contrast enema (Madlensky et al. 2003). The fourth is the non-invasive faecal occult blood test (FOBT) (Clemen and Lacke 2001).
Flexible sigmoidoscopy is endorsed by the Canadian Task Force on Preventive Health Care as an initial screening test for CRC in men and women at average risk, as well as supported in consensus guidelines by the American Cancer Society, the US Multisociety Task Force on Colorectal Cancer and the American College of Radiology (Levin et al. 2008). Although colonoscopy as a screening strategy is often considered the "gold standard," it has not yet been demonstrated to be more effective than FS in reducing mortality through detection of CRC (Neugut and Lebwohl 2010).
A recent large, randomized trial in the United Kingdom found that the cumulative reduction in distal colon cancer incidence and mortality was 50% after one-time FS screening, with some case-control studies reporting this reduction to be as high as 70% (Atkin et al. 2010). The most serious complication during FS is perforation of the colon, which would usually require surgical repair (Horton et al. 2001); however, the rates of these complications are very low, at about one perforation per 10,000 procedures (Johnson 1999). The procedure requires less time to prepare for and perform than a colonoscopy, is safer owing to decreased risk of perforation as compared to colonoscopy, is less costly and can be undertaken without anaesthesia (NC Cancer Partnership 2007).
According to the Canadian Credentialing Guidelines for Flexible Sigmoidoscopy, developed by the Canadian Association of Gastroenterology (CAG), colonoscopy is recommended if one or more adenomas are found, regardless of their size, or if a polyp is found that is greater than 1 centimetre in size (Enns et al. 2008). The removal of polyps smaller than 1 centimetre discovered during the FS procedure requires that the sigmoidoscopist be trained to biopsy the polyp. This requirement was addressed for the nurse FS project, a pilot project initiated in 2006 with the MOHLTC and Cancer Care Ontario, the first initiative of its kind in Canada.
The project was launched in various cancer centres around the province to assess the impact and acceptability of this procedure as a method of CRC screening as performed by registered nurses (Green et al. 2010). At the time, the Ontario Task Force on Large Bowel Endoscopic Services determined that the Ontario Regulated Health Professions Act and the Nursing Act allowed biopsied polyps "by RNs (general class), for the purpose of assessment, to be within their scope of practice" (Dobrow 2007). According to the Canadian Partnership Against Cancer's (2010) watching brief on flexible sigmoidoscopy, criteria are still needed for referral to colonoscopy of persons in whom one or more polyps are found. Considerations – including physician supervision and availability, and malpractice issues – have not yet been completely resolved by regulatory bodies (Dobrow et al. 2007; CPAC 2010; OMA 2007).
There is evidence to suggest that other healthcare practitioners, including registered nurses, may be trained to perform FS safely and competently (Lal et al. 2004; Rabeneck and Paszat 2003). The effectiveness of RNs in performing FS has also been shown in the United States with the Colon Cancer Prevention Program at the Kaiser Permanente Center for Health Research, in the United Kingdom with the National Health Service National Endoscopy Project and in Canada (Dobrow et al. 2007; Shapero et al. 2007). Schoenfeld and colleagues (1999b) found that there was no difference in detection of adenamatous polyps between nurse endoscopists and gastroenterologists. Complication rates for both endoscopists and RNs that have been appropriately trained have been found to be similar (Goodfellow 2006; Schoenfeld et al. 1999b). Experienced nurse endoscopists may perform screening FS as safely and as effectively as gastroenterologists (Schoenfeld et al. 1999b). Internationally, flexible sigmoidoscopy, along with FOBT and colonoscopy, is seen as an appropriate screening modality for CRC because it is a safe and well-endured procedure and can be performed by non-physician endoscopists (O'Brien et al. 2003; Terhaar Sive Droste et al. 2006; Winawer et al. 1990). Members of the nursing profession have successfully assumed this role in various jurisdictions, and have been supported by professional guidelines from both nursing bodies (Society of Gastroenterology Nurses and Associates Practice Committee in the United States) and medical societies (British Society of Gastroenterology Endoscopy Section Working Party) (O'Brien et al. 2003; Terhaar Sive Droste et al. 2006; Winawer et al. 1990; Arumugam et al. 2000; Basnyat et al. 2000; Goodfellow 2006).
The issue of RN-performed FS is a timely one for Ontario for multiple reasons. First, recent investments by the provincial government, such as the ColonCancerCheck program (a mutual partnership between the Ministry of Health and Long-Term Care and Cancer Care Ontario), are aimed at increasing access to CRC screening; however, there is a risk that there are insufficient hospital-based resources to meet present needs (OMA 2007). Second, Health Force Ontario announced its commitment to the establishment of a new healthcare professional role – the registered nurse–performed flexible sigmoidoscopy (RNFS) – as a part of its health human resources strategy intended to help meet the province's screening objectives (OMA 2007). Pilot projects are underway in various cancer centres throughout Ontario, where nursing professionals, after receiving specialized education and participating in training procedures, perform flexible sigmoidoscopy procedures on eligible patients under physician supervision. Physician-related issues such as malpractice coverage, physician reimbursement for training and back-up and medical directives that allow RNs to perform the procedures still need to be addressed beyond the current pilot study setting (CPAC 2010). An on-call physician fee was incorporated into the model for this analysis to address these as of yet unresolved issues.
Notwithstanding human resource constraints throughout the healthcare system, including the supply of nurses, we examine whether RN-performed flexible sigmoidoscopy is a viable option to increase the screening capacity in the province. Our study compares the cost of FS conducted by RNs relative to physicians (i.e., gastroenterologists, general surgeons, internists and family physicians) in Ontario.
Methods
We conducted a cost minimization analysis from a health system perspective. The results were intended to demonstrate whether the use of registered nurses, in addition to current practice providers (i.e., physicians), can contribute to the current screening capacity while remaining fiscally responsible.
Cost data
Salary ranges for RNs were obtained from the 2008 Ontario Nurses' Association Collective Agreement (ONA 2008). The hourly salary rate was multiplied by 1.20 for employer-based benefits (Annual Earnings Data 2001; Chan et al. 1996), and further multiplied by 1.13 (52/46) to account for vacation days and holidays (Guerriere et al. 2010). Reimbursement rates for the FS procedures for physicians were based on the 2010 Ontario Health Insurance Plan (OHIP) Schedule of Benefits obtained from the Ministry of Health and Long-Term Care (2010b).
Flexible sigmoidoscopy was defined as endoscopy up, but not beyond, the splenic flexure (Schultz et al. 2007). There are three fee schedule codes associated with a FS procedure, including Z555 (colonoscopy of sigmoid to descending colon); E740 (colonoscopy to splenic flexure); and Z580 (endoscopy using 60-centimetre flexible endoscope). It was decided that the most appropriate fee schedule code to use in our study was Z555 + E740 (Schultz et al. 2007). Fee schedule codes for polyp removal were dependent on size and method, including Z570 (fulguration of first polyp through colonoscope) ± E719 (each additional polyp – maximum of four); or Z571 (excision of first polyp ≥3 millimetres through colonoscope) ± E720 (each additional polyp ≥3 millimetres – maximum of two). In our analysis, we used Z571 for the cost of polyp removal to provide a conservative estimate. Procedure times were derived from the literature and ranged from eight to 10 minutes for an experienced endoscopist (Schoenfeld et al. 1999c), whereas less experienced endoscopists may take over 20 minutes to complete the procedure (Schoenfeld et al. 1999b; Spiegel 1995). For this study, we used a conservative estimate of 20 minutes as the procedure time for conducting the FS procedure. This estimate is comparable to procedure times of registered nurses who have recently completed their training, though procedure times are expected to decline with experience. The highest available wage rate for RNs with 25 or more years of service was used for the analysis in order to provide an estimate of the maximum costs of RN-performed FS (ONA 2008). Consequently, this study used an hourly RN wage of $40 (or $18.09 for each 20-minute FS procedure when fringe benefits and vacation time are included).
Physician remuneration
Various remuneration cases are examined for physicians, depending on whether a polyp is detected and the procedure code billed by physicians through OHIP. In addition, because a physician needs to be on-site in case of situations that require intervention beyond the scope of practice for RNs (e.g., polyp removal or complications), the option of an on-call fee was considered. Because the issue of medical directives differs among hospital sites, various physician on-call fees are considered in this analysis. These on-call fees are defined in proportion to the full OHIP fee for a physician-performed FS procedure. Consequently, in the absence of physician intervention, physicians would still be reimbursed for the on-call supervision of the RN-performed FS procedure. Set-up costs for the procedure are assumed to be identical independent of the provider performing the FS. Our analysis does not include anything beyond the initial screening procedure, regardless of whether or not a polyp is detected.
The base case, or case 1, considers the cost of the RN and a range of on-call physician fees, ranging from 0% to 100% of the physician-performed FS fee schedule code (Z555 [$57.70] + E740 [$57.70], at $115.40) (Table 1). In case 2, we consider the situation in which a polyp is detected and a physician intervenes to remove it. In this case, in addition to the RN cost and the physician on-call fee (using the range previously used under case 1), the physician also bills for polyp removal (code Z571, at $150.15) and for the performance of FS (Z555 + E740, at $115.40) (Table 1). Finally, in case 3 we consider the situation where a polyp is detected, the physician intervenes to remove it and the physician bills only for the polyp removal (Z571, at $150.15) without billing for a full FS procedure, because he or she did not perform it. However, case 3 results in the same cost differential between registered nurses and physicians as case 1; therefore, only cases 1 and 2 are reported here.
| Table 1. Description of costing cases | ||
| Case | Description for Registered Nurses | Description for Physicians |
| Case 1 (base case) | Physician on-call fee accounts for a range of 0%, 25%, 50%, 75% and 100% of the OHIP Z555 + E740 billing for flexible sigmoidoscopy. Cost per procedure performed by an RN is $18.09. | Cost per procedure performed by a physician is $115.40 (code Z555 + E740). |
| Case 2 | Physician on-call fee accounts for the range of OHIP Z555 + E740 billing as outlined in case 1, full billing of the flexible sigmoidoscopy procedure (Z555 + E740, at $115.40) and full billing of the polyp removal fee schedule code (Z571, $150.15). Cost per procedure performed by an RN is $18.09. | Cost per procedure performed by a physician is $115.40 (code Z555 + E740). Cost for polyp removal is $150.15 (code Z571). |
Cost minimization analysis
The base case (case 1) is expected to be the most common outcome, as the intention is to screen asymptomatic individuals at average risk. We conducted our analysis, applying this case against all patients who would be considered for screening purposes. In these situations, both the physician and the RN would refer the patient for colonoscopy. As previously stated, this scenario is not included because the subsequent colonoscopy costs are identical for both physician- and RN-performed FS.
A cost minimization analysis was conducted by comparing the costs of a physician-performed FS with that of a RN-performed FS. The cost of a physician-performed FS was calculated based on the code for flexible sigmoidoscopy in case 1, and included the addition of polyp removal in case 2 (see Table 1). The cost of a RN-performed FS was calculated for each of the five possible physician remuneration scenarios (0%, 25%, 50%, 75% or 100% of the OHIP fee schedule) for case 1 and case 2. A cost minimization analysis was conducted in which we applied cases 1 and 2 in 75% and 25% of all cases, respectively. Therefore, for a population of 100 individuals, it was calculated that 25 average-risk individuals would require intervention from a physician. Thus, 75% of the case 1 cost and 25% of the case 2 cost were combined to provide an overall cost for each on-call fee. The cost of a RN-performed flexible sigmoidoscopy was then compared to the cost of a physician-performed procedure.
Results
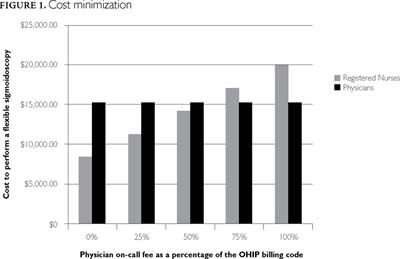
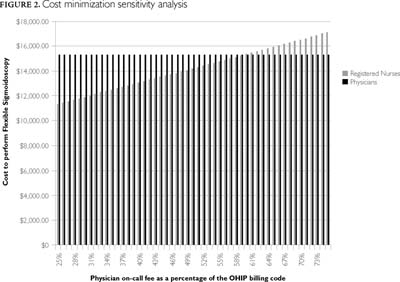
Cost minimization was calculated for each of the on-call rates and compared against physicians' fees at a polyp detection rate of 25% (Table 2 and Figure 1). The cost for physician-performed flexible sigmoidoscopy per 100 patients is $15,293.75. The results show that RN-performed FS minimizes costs when the physician on-call fee is less than 75%. More specifically, for screening FS procedures, the sensitivity analysis (Figure 2) indicates that RNs are less costly compared to physicians with an on-call fee of up to $69.24 (at an on-call rate of 60%) for physicians.
| Table 2. Cost minimization analysis | |||
| On-Call Fee | Case 1 (75%) | Case 2 (25%) | Total |
| Cost for Registered Nurses | |||
| 0% | $18.09 | $283.64 | $8,447.45 |
| 25% | $46.94 | $312.49 | $11,332.45 |
| 50% | $75.79 | $341.34 | $14,217.45 |
| 75% | $104.64 | $370.19 | $17,102.45 |
| 100% | $133.49 | $399.04 | $19,987.45 |
| Cost for Physician-Performed FS | |||
| $115.40 | $265.55 | $15,293.75 | |
Discussion
Implementation of RN-performed flexible sigmoidoscopy is a viable alternative to physician-performed FS. RN-performed FS is as effective as physician-performed FS (Schoenfeld et al. 1999b). RN-performed FS is also less costly than physician-performed FS when a reasonable on-call remuneration fee for physicians is used. However, physician remuneration must be considered when policies are developed for the implementation of RN-performed FS, as this influences the relative cost savings associated with the use of RNs rather than physicians.
Regardless of the setting considered for RN-performed FS, potential barriers exist to the broadening of the role of RNs, for example, the nurse sigmoidoscopist. The referral rate of RNs for FS may be low and could severely limit the potential to increase screening capacity. The nurse FS training program in Ontario identified low patient referral by physicians to RNs as a barrier to the achievement of program objectives (Dobrow et al. 2007). Other important considerations for the successful integration of alternative healthcare providers in providing the screening procedures concern scope-of-practice issues, especially those associated with the proper identification of polyps and adherence to protocols, and patient safety. The inclusion of FS within the RN's scope of practice provides one less barrier to further implementation.
There are several limitations to the current study. First, the assumptions used to perform the cost minimization analysis do not currently represent actual practice patterns. There is a paucity of Canadian studies concerning current patterns of practice regarding RN-performed FS. As most studies are based on practice in the United States and the United Kingdom, assumptions used in our study were based on practices described in the literature. Second, the cost estimates used may differ among physicians owing to differing billing practices and the use of alternative billing codes for colon screening. These effects are minimal because of the small variation in costs among codes. For instance, the OHIP database, which identifies information on all physician fee-for-service billings, does not differentiate among types of physician and the specificity of procedures billed. Third, time considerations were not taken into account in the present analysis. For instance, Schoenfeld and colleagues (1999a) found that RNs took on average 8.3 minutes, surgeons 7.6 minutes and gastroenterologists 6.8 minutes to complete the procedure (Schoenfeld et al. 1999a). Thus, while approximately equal volumes of procedures can be performed by each provider (not accounting for potential differences in setup times among providers), minor variations with respect to this parameter are not included. Fourth, training costs will need to be considered for the implementation of RN-performed FS. For this study, training costs for Ontario were not available to the researchers; however, it is recommended that for future studies, training costs be factored into a cost minimization or cost-effectiveness or return-on-investment analysis. Finally, the findings from this study will vary in their applicability to various settings. For instance, varying methods of procedure billing will affect the results of the potential cost savings. The scope of practice for RNs in the United States is greater than in Canada and hence, may result in more physician willingness to share responsibilities for sigmoidoscopy screening. However, within the Ontario Ministry of Health and Long-Term Care, this is a major treatment option that is being considered, as evidenced by HealthForceOntario's designation and the pilot projects. Therefore, this study contributes valuable findings to answer the question of whether this is a viable policy option.
Conclusions
The literature indicates that RN-performed FS is a safe, feasible and cost-effective option to increase CRC screening capacity in Ontario. The literature also indicates that nurses and physicians have equal effectiveness rates in polyp detection. This study shows that RN-performed FS is a cost-saving option to increase the screening capacity of the health system in Ontario. Remuneration considerations for on-call physicians are crucial to the implementation of RN screening procedures, because the cost minimization of RN-performed FS is inversely related to such on-call fees.
Given that concerns about the adequate supply of RNs as well as physicians are likely to continue as the population ages, it will be increasingly important to evaluate ways in which we can utilize the existing stock of healthcare professionals in new and more efficient ways. Based on the implications of these findings, future studies should also consider training costs and the number of RNs that would be required to provide appropriate coverage for increased CRC screening as part of overall human resource planning for FS procedures.
Sigmoïdoscopie flexible effectuée par les infirmières autorisées en Ontario : analyse de minimisation des coûts
Résumé
Contexte : Au Canada, les taux de cancer colorectal (CCR) sont à la hausse. La sigmoïdoscopie flexible (SF) est un test initial de dépistage du CCR principalement utilisé chez les adultes de 50 ans et plus qui présentent un risque moyen de développer la maladie. Il a été démontré que les médecins et les infirmières autorisées présentent la même efficacité pour effectuer les procédés de FS. Cet article présente une analyse de comparaison entre les infirmière autorisées et les médecins en Ontario afin d'en évaluer les coûts pour le système de santé.
Objectifs : Évaluer dans quelle mesure la SF effectuée par les infirmières autorisées est un choix moins coÛteux pour accroître l'accès au dépistage du CCR en Ontario.
Méthodologie : Une analyse de minimisation des coûts a été effectuée selon l'angle du système de santé.
Discussion : La FS effectuée par les infirmières autorisées afin d'accroître les capacités de dépistage du CCR en Ontario est une option viable. Les barèmes de rémunération des médecins sur appel doivent être reconsidérés si on souhaite élaborer des politiques de mise en place de procédés de dépistage par les infirmières autorisées.
Résultats : Les résultats font voir que, par rapport aux médecins, l'utilisation des infirmières autorisées pour effectuer les procédés de SF peut permettre des économies, dépendamment de la rémunération des médecins.
About the Author(s)
Sarah E. Costa, MSc Institute of Health Policy, Management and Evaluation, University of Toronto, Toronto, ON
Peter C. Coyte, PhD Professor, Health Economics and CHSRF/CIHR Health Services Chair Institute of Health Policy, Management and Evaluation, University of Toronto, Toronto, ON
Audrey Laporte, PhD Associate Professor, Health Economics Institute of Health Policy, Management and Evaluation, University of Toronto, Toronto, ON
Laura Quigley, MSc Faculty of Medicine, University of Toronto, Toronto, ON
Shannon Reynolds, BHSC Institute of Health Policy, Management and Evaluation Health System Performance Research Network, University of Toronto, Toronto, ON
Correspondence may be directed to: Dr. Peter Coyte, PhD, Professor, Full SGS Member, CHSRF/ CIHR Health Services Chair, Health Policy, Management and Evaluation, Faculty of Medicine, University of Toronto, Health Sciences Building, 4th Floor, 155 College Street, Suite 425, Toronto, ON M5T 3MS; Tel.: 416-978-8369; e-mail: peter.coyte@utoronto.ca.
References
"Annual Earnings Data." 2001. The Economist 361: 8245.
Arumugam, P.J., G.N. Rao, J. West, M.E. Foster and P.N. Haray. 2000. "The Impact of Open Access Flexible Sigmoidoscopy: A Comparison of Two Services." Journal of the Royal College of Surgeons of Edinburgh 45(6): 366–68.
Atkin, W.S., R. Edwards, I. Kralj-Hans, K. Wooldrage, A.R. Hart et al. UK Flexible Sigmoidoscopy Trial Investigators. 2010. "Once-Only Flexible Sigmoidoscopy Screening in Prevention of Colorectal Cancer: A Multicentre Randomised Controlled Trial." The Lancet 375(9726): 1624–33.
Basnyat, P.S., J. West, P.S. Davies and M.E. Foster. 2000. "The Nurse Practitioner Endoscopist." Annals of the Royal College of Surgeons of England 82(5): 331–32.
Canadian Cancer Society. 2011a. "Colorectal Cancer Statistics at a Glance." Retrieved December 15, 2011. <http://www.cancer.ca/Canada-wide/About cancer/Cancer statistics/Stats at a glance/Colorectal cancer.aspx?sc_ lang=en>.
Canadian Cancer Society. 2011b. "Cancer Statistics Figures." Retrieved December 15, 2011. <http://www.cancer.ca/canada-wide/about%20cancer/cancer%20statistics/powerpoint%20slides.aspx?sc_lang=en>.
Canadian Cancer Society, National Cancer Institute of Canada, Statistics Canada, Provincial/Territorial Cancer Registries and Public Health Agency of Canada. 2008. "Canadian Cancer Statistics."
Canadian Partnership Against Cancer (CPAC). 2010 (June 3). Flexible Sigmoidoscopy Watching Brief. 2nd Iteration of Expert Panel Report. Toronto: Author.
Cancer Care Ontario. 2008. "Colon Cancer Check 2008 Program Report." Retrieved December 15, 2011. <https://www.cancercare.on.ca/common/pages/UserFile.aspx?fileId=75573>.
Chan, B., P. Coyte and C. Heick. 1996. "Economic Impact of Cardiovascular Disease in Canada." Canadian Journal of Cardiology 12(10): 1000–6.
Clemen, R.T. and C.J. Lacke. 2001. "Analysis of Colorectal Cancer Screening Regimens." Health Care Management Science 4: 257–67.
Dobrow, M.J., M.A. Cooper, K. Gayman, J. Pennington, J. Matthews and L. Rabeneck. 2007. "Referring Patients to Nurses: Outcomes and Evaluation of a Nurse Flexible Sigmoidoscopy Training Program for Colorectal Cancer Screening." Canadian Journal of Gastroenterology 21(5): 301–8.
Enns, R., J. Romagnuolo, T. Ponich, J. Springer, D. Armstrong and A.N. Barkun. 2008. "Canadian Credentialing
Guidelines for Flexible Sigmoidoscopy." Canadian Journal of Gastroenterology 22(2): 115–19.
Green, E., I. LeClaire, G. Pasut, D. Claus, J. Gilbert et al. 2010. "Forging a New Role in the Cancer System: RN Performed Flexible Sigmoidoscopy Model." Canadian Partnership Against Cancer: Cancer Workforce Symposium. Retrieved December 15, 2011. <http://www.cancerview.ca/idc/groups/public/documents/webcontent/hhr_symp_pres_rnpfsproject.pdf>.
Goodfellow, P.B. 2006. "Flexible Sigmoidoscopy Performed by Nurses." Endoscopy 38(6): 624–26.
Guerriere, D.N., B. Zagorski, K. Fassbender, L. Masucci, L. Librach and P.C. Coyte. 2010. "Cost Variations in Ambulatory and Home-Based Palliative Care." Palliative Medicine 24(5): 523–32.
Horton, K., A. Reffel, K. Rosen and F.A. Farraye. 2001."Training of Nurse Practitioners and Physician Assistants to Perform Screening Flexible Sigmoidoscopy." Journal of the American Academy of Nurse Practitioners 13(10): 455–59.
Johnson, B.A. 1999. "Flexible Sigmoidoscopy: Screening for Colorectal Cancer." American Family Physician 59(6): 1537–46.
Kielar, A.Z. and R.H. El-Maraghi. 2008. "Canadian Colorectal Cancer Screening Initiatives and Barriers." Journal of the American College of Radiology 5(9): 951–57.
Lal, S.K., A. Barrison, T. Heeren and P.C. Schroy III. 2004. "A National Survey of Flexible Sigmoidoscopy Training in Primary Care Graduate and Postgraduate Education Programs." American Journal of Gastroenterology 99(5): 830–36.
Levin, B., D.A. Lieberman, B. McFarland, R.A. Smith, D. Brooks, K.S. Andrews et al. for the American Cancer Society Colorectal Cancer Advisory Group, the US Multi-Society Task Force and the American College of Radiology Colon Cancer Committee. 2008. "Screening and Surveillance for the Early Detection of Colorectal Cancer and Adenomatous Polyps." CA: A Cancer Journal for Clinicians 58: 130–60.
Madlensky, L., J. McLaughlin and V. Goel. 2003 (July). "A Comparison of Self-Reported Colorectal Cancer Screening with Medical Records." Cancer Epidemiology, Biomarkers and Prevention 12: 656.
Ministry of Health and Long-Term Care (MOHLTC). 2010a. ColonCancerCheck – Health Care Professionals. Retrieved December 15, 2011. <http://www.health.gov.on.ca/en/pro/programs/coloncancercheck>.
Ministry of Health and Long-Term Care (MOHLTC). 2010b. Schedule of Benefits for Physician Services Under the Health Insurance Act. Retrieved December 15, 2011. <http://www.health.gov.on.ca/english/providers/program/ohip/sob/physserv/physserv_mn.html>.
Moayyedi, P. 2007. "The Promises and Perils of Nurse-Led Flexible Sigmoidoscopy Screening." Canadian Journal of Gastroenterology 21(5): 280–82.
North Carolina (NC) Cancer Partnership. 2007 (December). Colorectal Cancer White Paper. Raleigh: Author.
Neugut, A.I. and B. Lebwohl. 2010. "Colonoscopy vs. Sigmoidoscopy Screening: Getting It Right." Journal of the American Medical Association 304: 461–62.
O'Brien, K., B.F. Sweeney, N. Conger, J.R. Fischer and K.A. Lang. 2003. "Prevalence of Proximal Adenomas After an Adenoma Is Found on Flexible Sigmoidoscopy." Cancer Detection and Prevention 27: 259–65.
Ontario Medical Association (OMA). 2007. "The Ontario Medical Association's Statement on Nurse Sigmoidoscopist." Retrieved December 15, 2011. <https://www.oma.org/Resources/Documents/2007NurseSigmoidoscopist.pdf>.
Ontario Nursing Association (ONA). 2008. Collective Agreement. Retrieved December 15, 2011. <http://www.ona.org/documents/File/onanews/Draft_HospitalCentralAgreement_20140331.pdf>.
Rabeneck, L. and L.F. Paszat. 2003. "Colorectal Cancer Screening in Canada: Why Not Consider Nurse Endoscopists?" Canadian Medical Association Journal 169(3): 206–7.
Schoenfeld, P. 1999. "Flexible Sigmoidoscopy by Paramedical Personnel." Journal of Clinical Gastroenterology 28(2): 110–16.
Schoenfeld, P.S., B. Cash, J. Kita, M. Piorkowski, D. Cruess and D. Ransohoff. 1999a. "Effectiveness and Patient Satisfaction with Screening Flexible Sigmoidoscopy Performed by Registered Nurses." Gastrointestinal Endoscopy 49(2): 158–62.
Schoenfeld, P., S. Lipscomb, J. Crook, J. Dominguez, J. Butler, L. Holmes et al. 1999b. "Accuracy of Polyp Detection by Gastroenterologists and Nurse Endoscopists During Flexible Sigmoidoscopy: A Randomized Trial." Gastroenterology 117(2): 312–18.
Schoenfeld, P., M. Piorkowski, J. Allaire, R. Ernst and L. Holmes. 1999c. "Flexible Sigmoidoscopy by Nurses: State of the Art 1999." Gastroenterology Nursing 22(6): 254–61.
Schultz, S., L. Rabeneck and C. Vinden. 2004. Use of Large Bowel Procedures in Ontario. Toronto: ICES Research Atlas.
Schultz, S.E., C. Vinden and L. Rabeneck. 2007. "Colonoscopy and Flexible Sigmoidoscopy Practice Patterns in Ontario: A Population Based Study." Canadian Journal of Gastroenterology 21(7): 431–34.
Shapero, T., J. Hoover, L. Paszat, E. Burgis, E. Hsieh et al. 2007. "Colorectal Cancer Screening with Nurse-Performed Flexible Sigmoidoscopy: Results from a Canadian Community-Based Program." Gastrointestinal Endoscopy 65(4): 640–45.
Spiegel, T. 1995. "Flexible Sigmoidoscopy Training for Nurses." Gastroenterology Nursing 18(6): 206–9.
Terhaar Sive Droste, J.S., G.D. Heine, M.E. Craanen, H. Boot and C.J. Mulder. 2006. "On Attitudes about Colorectal Cancer Screening among Gastrointestinal Specialists and General Practitioners in the Netherlands." World Journal of Gastroenterology 12(32): 5201–4.
Winawer, S.J., J. St. John, J. Bond, J.D. Hardcastle, O. Kronborg, B. Flehinger et al. 1990. "Screening of Average-Risk Individuals for Colorectal Cancer. WHO Collaborating Centre for the Prevention of Colorectal Cancer." Bulletin of the World Health Organization 68(4): 505–13.
Wong, R.C.K. 1999. "Screening Flexible Sigmoidoscopy by Nonphysician Endoscopists: It's Here to Stay, But Is It the Right Test to Do?" Gastrointestinal Endoscopy 49(2): 262–64.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed