Healthcare Policy
System Integration and Clinical Utilization of the Advanced Clinician Practitioner in Arthritis Care (ACPAC) Program–Trained Extended Role Practitioners in Ontario: A Two-Year, System-Level Evaluation
Abstract
Background: The Advanced Clinician Practitioner in Arthritis Care (ACPAC) program was developed in 2005 to prepare experienced physical and occupational therapists to function as extended role practitioners (ERPs) within models of arthritis care across Ontario, Canada.
Purpose: To examine the system-level integration and clinical utilization of the ACPAC program–trained ERP.
Method: A longitudinal survey was administered to all ACPAC graduates over a two-year period (n=30).
Results: The majority of ERPs were physical therapists working in urban settings. Family physicians or physician specialists referred the majority of patients. The longest median wait time to access ERPs' services was 22 days. Half of the ERPs triaged patients, and most of those who did triage (75%) worked under medical directives. Approximately half (51.6%) of the patients seen had a diagnosis of osteoarthritis, followed by rheumatoid arthritis (14.7%).
Conclusion: Understanding the system-level impact of this unique human resource can help to shape healthcare planning and delivery of care.
Arthritis and musculoskeletal disorders are among the most common chronic health conditions in Canada, affecting more than 4.6 million people (Bombardier et al. 2011). Together, they are a leading cause of morbidity, disability and healthcare utilization. These conditions affect people of all ages, being most prevalent among seniors but also affecting children and working-age adults. The most common arthritis conditions, those with the greatest impact on the healthcare system, and those expected to increase to approximately 2% of the population in the next 30 years, are osteoarthritis (OA) and rheumatoid arthritis (RA) (Bombardier et al. 2011).
In order to help address the growing arthritis burden, the Advanced Clinician Practitioner in Arthritis Care (ACPAC) program was developed in 2005 to prepare experienced physical therapists and occupational therapists for extended practice roles and to promote the development of innovative models of arthritis care across diverse clinical settings in Ontario, Canada. Graduates of the ACPAC program represent a new cadre of extended role practitioner (ERP), having received significant additional training with formal evaluation to establish competency in advanced assessment, diagnosis and management of select arthritis conditions described elsewhere (Lundon et al. 2011). The ACPAC program is a unique clinical and academic training program offered in Toronto, Ontario. It focuses on the advanced assessment, diagnosis, triage and independent management of select musculoskeletal (orthopaedic) and arthritis-related (rheumatological) disorders (Lundon et al. 2008, 2009, 2011). Between 2005 and 2011, five cohorts (37 practitioners) of trainees have successfully completed the ACPAC program.
A need was identified to evaluate the impact of the ERPs as the graduates of the ACPAC program began to develop and implement new roles at their various institutions. The purpose of this study was to evaluate the system-level impact of ACPAC program–trained ERPs working within various models of arthritis care in diverse clinical settings across Ontario. The specific objectives were to (a) measure the extent to which ACPAC program–trained ERPs are delivering integrated and timely healthcare for patients with musculoskeletal and arthritis-related disorders throughout the province of Ontario, (b) describe the role utilization of the ACPAC program–trained ERP and (c) describe the clinical performance of the ACPAC program–trained ERP with respect to patient volumes, referral sources and diagnoses of patients seen by the ERPs.
Methods
The balanced scorecard approach (Kaplan and Norton 1996) was chosen as a framework for evaluation. This framework was used to provide stakeholders of the ACPAC program (faculty, students, graduates, healthcare organizations, policy makers) with feedback regarding performance measurement and to permit continuous improvement and strategic healthcare planning. In the province of Ontario, the Hospital Report: Rehabilitation series (Cott et al. 2005) has modeled four quadrants from the original balanced scorecard approach using the following nomenclature: (a) client perspectives, (b) clinical utilization and outcomes, (c) system integration and change and (d) financial performance and condition. This nomenclature was chosen for the ACPAC system-level evaluation, with the exception that "client perspectives" was renamed "patient and stakeholder perspectives." This study reports on the results from the system integration and change (SIC) and the clinical utilization and outcomes (CUO) quadrants.
The evaluation of the SIC and CUO quadrants consisted of a longitudinal electronic survey of all ACPAC program–trained graduates (n=30) working in Ontario over a two-year period. Data were collected quarterly for the fiscal (April 1 to March 31) years 2009/2010 and 2010/2011 using SurveyMonkey® software (www.surveymonkey.com). The current cohort of ACPAC trainees (n=7) was excluded from this study. The survey consisted of indicators related to the SIC and CUO quadrants developed by a committee of ACPAC graduates and faculty. Feedback regarding selected indicators was sought from patients and parents of paediatric patients who had been recipients of healthcare provided by ACPAC program–trained ERPs and from healthcare administrators, who were familiar with or had ACPAC program–trained ERPs reporting to them. The questionnaire was then pilot tested with the ERPs on three separate occasions. ERPs were asked to provide feedback regarding face and content validity, clarity, relevance and format of the indicators included in the questionnaire. The indicators were further refined based on the feedback from each pilot. Table 1 defines the indicators related to the SIC and CUO quadrants. Variables relating to the ERP demographics were derived from the ACPAC graduate database, and from provincial and federal government websites.
| TABLE 1. System integration and change (SIC) and clinical utilization and outcomes (CUO) indicator definitions | |
| Indicator | Definition |
| System Integration and Change | |
| Access to care | |
| Wait times | The number of days from the date of referral to the date the ERP first saw the patient. The average wait time was calculated as the total wait time for all new patients seen during the fiscal quarter divided by the number of new patients seen during the fiscal quarter. Weekends and holidays were included in this calculation. |
| Integration of extended role practice | |
| Extended role practice | Working in a professional capacity that uses competencies beyond entry-to-practice-level competencies and which may be achieved through delegation or medical directives in either all or part of a full-time equivalent position. |
| Full-time equivalent (FTE) | The proportion of a full-time equivalent position employed as an ERP. |
| Title | Job title used at the ERP's primary place of employment at the time the quarterly questionnaire was completed. |
| Medical directives | Medical directives are defined as "indirect physician orders, used to expedite patient care by competent health professionals" (Hospital for Sick Children 2012). Elements of medical directives include the specifics of the procedure, safety conditions, the types of patient to which the directive applies and the types of professional that are authorized to implement the procedure (College of Physiotherapists of Ontario 2008). |
| Integration with the healthcare system | |
| Referral to services | The number of patients referred to institutional or community healthcare services and resources. |
| Communication | The number of dictations and letters completed that were related to the ERP role. |
| Clinical Utilization and Outcomes | |
| Volumes | |
| New consultations | The number of patients seen face-to-face for the first time by the ERP, regardless of whether this was in an initial consultation or triage capacity |
| Follow-ups | The number of patient encounters seen in follow-up for either consultation or treatment. If the same patient was seen more than once, the visit was counted on each occasion |
| Triage | Paper triage of faxed or electronic referrals (patients triaged during a face-to-face consultation were captured as "new consultations") |
| Referral sources | |
| Referral sources | The number of patients who were referred from the following sources: self-referral; family doctor; nurse practitioner; physician specialist; other allied health; and other |
| Diagnoses | |
| Diagnoses | Based on International Classification of Diseases ICD-10 (World Health Organization 2010) categories related to arthritis and musculoskeletal disorders. Diagnosis was based on the ERP's assessment findings. If the patient had more than one diagnosis, the most responsible diagnosis was used. For paediatric diagnoses related to arthritis and musculoskeletal disorders, the International League of Associations for Rheumatology (ILAR) classification was used (Petty et al. 2004) |
Data were downloaded from SurveyMonkey® into Excel 2003, and all analyses were conducted using SAS version 9.1. Data analysis consisted of descriptive and univariate statistics to describe the variables related to demographics and the above indicators. This study received approval from the St. Michael's Hospital Research Ethics Board.
Results
A total of 30 ACPAC program–trained ERPs who graduated from the program received an electronic questionnaire each quarter during the 2009 and 2010 fiscal years. The mean response rate was 91.3% over the two-year data collection period. The quarterly response rate varied from 83.3% to 96.7%. Throughout the 2009 and 2010 fiscal years, the majority of ACPAC program–trained ERPs were physical therapists, working in urban settings and focused on adult populations. See Table 2.
| TABLE 2. Description of ACPAC-trained ERPs | |
| Variable | n (%) |
| Professional Designation | |
| Physical Therapist | 25 (84%) |
| Occupational Therapist | 5 (16%) |
| Geographic Location of Place of Employment | |
| Urban | 23 (76.7%) |
| Rural | 7 (23.3%) |
| Academic Status of Place of Employment | |
| Academic | 5 (50%) |
| Non-academic | 5 (50%) |
| Population Served | |
| Adult | 26 (86.7%) |
| Paediatric | 4 (13.6%)* |
| * Percentages may not add up to 100% due to rounding. | |
System integration
The indicators to describe the system integration of the ACPAC program–trained ERP included access to care, integration of extended role practice and integration with the healthcare system.
Access to care
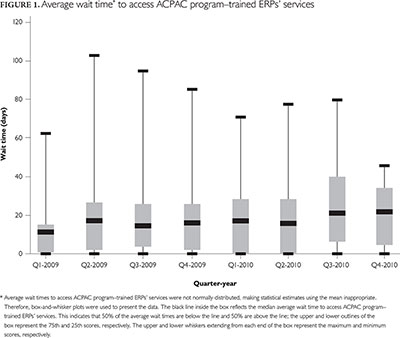
Three-quarters of ACPAC program–trained ERPs reported an average wait time of no longer than 39 days from the date when the referral was received to the date the patient was actually seen by the ERP. Over the two-year period, the longest median wait time to access ACPAC program–trained ERPs' services was 22 days. See Figure 1.
Integration of the extended role practice
Over the 2009 fiscal year, a mean of 89.7% (n=24) of ERPs reported practising in an extended role. A similar pattern was found in the 2010 fiscal year (86.4%). Reasons for not practising in the role included lack of funding for the role, being on an extended leave of absence (including parental leave) or a change of position (for example, promotion to a management position).
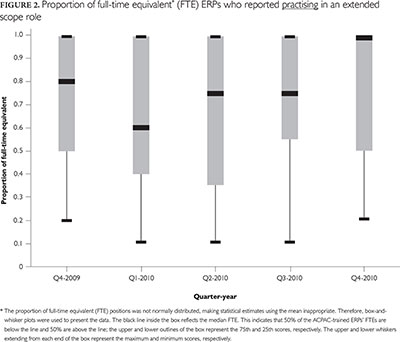
There was wide variation among ACPAC ERPs regarding the proportion of their time dedicated to the extended practice role. As illustrated in Figure 2, this varied from as little as 0.1 of a full-time equivalent (FTE) (i.e., a half-day per week in a regular 40-hour work week) to as much as 1.0 FTE. However, 50% of the ACPAC ERPs reported working in a position dedicated to extended role practice at least 0.6 of a FTE.
ERPs used a variety of titles to describe their role. Overall, there were 25 reported titles being used throughout 2009 and 2010. Some examples include "advanced practice physiotherapist," "advanced clinical practitioner in arthritis care," "physiotherapist," "practitioner in rheumatology" and "advanced physiotherapist practitioner." Similar variation existed for occupational therapists.
With respect to the specific activities being performed under medical directives, the majority of ACPAC ERPs reported ordering lab tests (64.3%) and X-rays (82.1%) either on a daily, weekly or monthly basis during the 2009 fiscal year. A similar and slightly increased trend was observed in 2010 with respect to these specific medical directives. Approximately 40% of ERPs reported ordering diagnostic ultrasound and bone density tests over the 2009 and 2010 fiscal years.
Furthermore, about 70% of ACPAC ERPs recommended medication changes, dosage changes or both to either the patient or the referring physician, and approximately 4% of ERPs were able to make these changes under a medical directive. Similarly, 90% of ACPAC ERPs recommended joint injections to either the patient or the referring physician, with approximately 5% of ERPs having performed joint injections under a medical directive.
Integration with the healthcare system
Approximately one-third of patients seen by ACPAC program–trained ERPs were referred for X-ray, laboratory and other services. These were followed by referral to allied health services (20%) and referral to specialists (7%). Consultation letters were dictated for a third of patients. Less than 5% of patients required letters for schools, insurance agencies or Ontario Drug Benefit programs, or were related to adult transitional care.
Clinical utilization
The clinical utilization indicators included patient volumes, referral sources and patient diagnoses.
Patient volumes
ERPs saw 4,032 and 4,679 new consultations in 2009 and 2010, respectively. The majority of the ERPs (75%) reported as many as 55 to 80 new consultations across each fiscal quarter.
With respect to patients seen in a follow-up capacity, ACPAC ERPs saw between 25% and 50% more patients for follow-up than they were seeing for new consultations. In 2009, they saw 6,563 patients for follow-up, and in 2010, 9,141 patients for follow-up.
Half of the ERPs reported being involved in triage. In 2009, 2,119 patients were triaged, and 3,506 in 2010. Of those who were actively triaging patients, the majority (75%) of ERPs triaged approximately 50 patients per quarter.
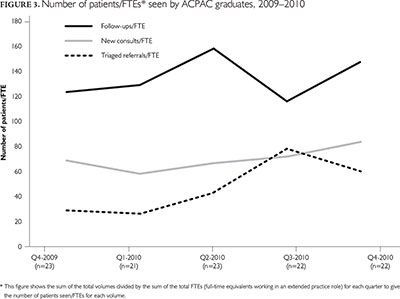
There was an overall increase in the number of patients seen per FTE for new consultations, follow-ups and patients triaged (see Figure 3). Specifically, new consultations ranged from 58 to 85 patients per FTE across the quarters; follow-ups ranged from 118 to 160 patients per FTE across the quarters, and triaged referrals ranged from 27 to 79 patients per FTE across the quarters.
The distribution of overall patient volumes over the two-year data collection period was similar with respect to the proportion of new consultations, follow-ups and triages that made up the ERPs' caseloads. Approximately half of the ERPs' caseloads were dedicated to follow-up patients.
Referral sources
In 2009, the greatest number of referrals came from family physicians (43.9%), followed by physician specialists (35.8%). In 2010, the reverse was the case (51.5% and 37.3%, respectively). Self-referral and referrals from nurse practitioners, allied health professionals and other sources comprised the remaining referrals.
Diagnoses
Most patients had non-inflammatory disorders (61.9% in 2009 and 60.1% in 2010). Approximately half of all patients seen had a diagnosis of osteoarthritis. Other common diagnoses included rheumatoid arthritis (15%) and juvenile idiopathic arthritis (10%).
Discussion
This system-level evaluation describes the integration and clinical utilization of ACPAC program–trained ERPs within the Ontario healthcare system over a two-year period. The results of this study indicate there is an opportunity to maximize the use of the ACPAC ERP, given that half of respondents reported working less than a full-time equivalent position at the end of the study period. It has been well established that there is a physician shortage throughout the province of Ontario, in terms of family physicians and medical specialists (including rheumatologists and orthopaedic surgeons) (OMA 2007; Badley et al. 2007, 2008). Given this shortage, there is a need for alternative models of healthcare delivery. Greater utilization of the ERP could (a) assist in the delivery of healthcare in geographic areas where there is lack of specialized care for specific patient populations, (b) help to improve access to care where wait times may be long, (c) enhance interprofessional care, (d) help to improve patient outcomes and (e) increase capacity for care for patients with arthritis. Further investigation into these potential system-level impacts by the ACPAC-trained ERP is warranted.
Clearly, there was no consensus among ERPs or their institutions regarding the assigned title of extended practice roles for physical therapists and occupational therapists working with people with musculoskeletal and arthritis-related disorders. The implications of multiple titles used to describe the ERP could potentially lead to difficulty in role promotion. Furthermore, consumers and colleagues from other healthcare professions may have difficulty clarifying the role. Despite foreseeable challenges, which include existing titles that have been designated through various human resources departments, as well as regulatory body restrictions that protect professional titles, the wide variation of terminology used to describe ERP roles illustrates the need for standardization of title for ERPs.
The Physiotherapy Act, 1991 was recently amended to include a number of acts that were previously beyond scope of practice (Government of Ontario 2011). However, the majority of ERPs are working under medical directives as they practise in institutions governed by the Public Hospitals Act. Furthermore, expectations of increased clinical responsibilities in the extended practice role include performing the initial assessment of a patient with undiagnosed arthritis (inflammatory or non-inflammatory), initiating orders for laboratory testing or diagnostic imaging, interpreting laboratory or diagnostic imaging test results, giving a differential diagnosis and independently managing and monitoring the follow-up for patients with an array of arthritic conditions. As an example, the practitioner is expected to identify "red flags" generated from taking a detailed history and initiate laboratory investigations based on systemic symptoms such as fever and weight loss; multisystem disease involving skin, lung, gastrointestinal and neurological symptoms; and muscle weakness. The practitioner is expected to interpret abnormal laboratory findings based on complete blood count (CBC), high erythrocyte sedimentation rate (ESR), c-reactive protein (CRP), abnormal urinalysis, liver function tests (LFT), creatine kinase (CK) elevation and abnormal proteins, all in the context of polyarthritis. With the exception of communicating a diagnosis, the additional acts do not reflect typical musculoskeletal and arthritis-related practice and therefore, many of the roles currently undertaken by ACPAC program–trained EPRs remain beyond scope, and continue to fall under the auspices of delegation or medical directive to perform. Thus, the utilization of medical directives may assist ERPs in providing comprehensive care, such as ordering appropriate investigations in a timely manner and providing efficient and effective management of musculoskeletal and arthritis-related conditions. Moreover, the use of medical directives may have the potential to help reduce unnecessary visits to specialists and may help to ensure early identification of need for specialist intervention.
Introduction of the ACPAC ERP role has demonstrated a positive impact on access to care for patients with musculoskeletal and arthritis-related disorders. The results of this evaluation showed that the longest median wait time to see an ACPAC ERP was less than three weeks. Access to appropriate healthcare is a priority for the Ontario Ministry of Health and Long-Term Care to ensure that patients are seen by the right healthcare professional, in the right place, at the right time (MOHLTC 2008). In 2007, the mean reported wait time to see a rheumatologist for non-urgent inflammatory arthritis was 13.4 weeks in the province of Ontario (Badley et al. 2008). It has been suggested that healthcare professionals working in extended roles could facilitate the early identification of inflammatory arthritis and thereby provide effective and timely intervention for this patient population (Jamal et al. 2011). Similarly, the current wait times target for orthopaedic hip and knee joint replacement surgeries in the province of Ontario is 26 weeks (MOHLTC 2011). Although orthopaedic wait times have improved in urban areas of the province, other, more rural areas still have lengthy wait times (MOHLTC 2011). The results of this evaluation indicate that the use of ERPs has the potential to improve access to healthcare professionals who specialize in arthritis care, as they are able to see patients in a timely manner, thereby facilitating early detection and early intervention for patients with inflammatory and non-inflammatory arthritis.
The rise in patient volumes over the two-year study period likely demonstrates an increase in utilization of ERPs as their referral sources adapted to this new role. To date, there has been no benchmark set for the number of patients that should be seen in either a consultative or follow-up capacity. However, according to our findings, not all ERPs working in the province of Ontario were being utilized to their full capacity. With appropriate role promotion, the volumes of patients managed by ERPs are expected to increase over time. Further study is warranted to determine appropriate benchmarks related to patient volumes for ACPAC ERPs.
The majority of patients seen by ERPs had a diagnosis of OA. This could be attributed to the fact that the prevalence of OA (affecting 13% of Canadians), a non-inflammatory arthritis, is much greater than that of inflammatory arthritis (affecting 0.9% of Canadians) (Bombardier et al. 2011). Furthermore, the initiative of the Ontario Ministry of Health and Long-Term Care to improve access to hip and knee replacement surgery funded a number of ACPAC program–trained ERPs to develop triage programs for hip and knee replacement surgery (MOHLTC 2007). These initiatives have increased the number of patients, especially with osteoarthritis, seen by ERPs. Based on the above findings, there may be opportunities to further augment the ERP's role in improving access to care for people with inflammatory arthritis.
Limitations
This study was the first iteration of a balanced scorecard approach to measuring the impact of ACPAC program–trained ERPs on the healthcare system. As such, a number of limitations should be addressed.
First, the lack of benchmarks makes interpretation of the data difficult. A recent systematic review of Canadian and international advanced practice physiotherapists (APPs) (similar to physiotherapists and occupational therapists working in extended roles) working with patients with musculoskeletal disorders mainly examined clinical and patient satisfaction outcomes (Desmeules et al. 2012). Unfortunately, very few studies included in this review examined system-level outcomes, thus making it difficult to draw comparisons to our study. One recent study that did examine system-level outcomes, not included in the above systematic review, examined the APP role within a specialty shoulder clinic located in Ontario (Razmjou et al. 2012). This paper reports significantly shorter wait times from date of referral to date of consultation of advanced practice physical therapists compared to surgeons. The authors report a mean wait time of 147 days to be seen by the APP for shoulder consultation, compared to our finding of an average wait time of no longer than 39 days to be seen by ACPAC program–trained ERPs.
The second limitation to be acknowledged is the heterogeneity of the cohort, which makes comparisons of clinical utilization difficult, as ACPAC graduates are working in various capacities in terms of client base and clinical setting. While we have demonstrated significant pre–post change in advanced skills and knowledge and, thus, competency of the ACPAC program trainee (Lundon et al. 2011), a comparison of pre–post change in workforce measures is restricted by a relatively small cohort (n=30 ACPAC graduates) and dissimilar workplace settings that limit meaningful comparisons at this time.
Third, the unique training and system integration of ACPAC program–trained ERPs restricts the findings of this study to this particular group at this time, making the results difficult to generalize to other healthcare professionals working in alternative roles (e.g., nurse practitioner or physician assistant).
Fourth, the ACPAC program has generated a relatively small cohort of ACPAC ERP graduates since its inception (n=37). This volume reflects the extremely labour-intensive nature of this training initiative as its success relies upon establishing the necessary associations with a range of preceptors including rheumatologists, orthopaedic surgeons and other physician specialists. This is the rate-limiting step restricting the program from processing larger numbers of practitioners on an annual basis. While there is pan-Canadian interest in this program and its graduates, incorporation of this initiative at a broader academic level and across multiple sites remains at a developmental stage.
Lastly, ERPs who were consulted in the development of the indicators used in this evaluation also took part in the study. Their inclusion potentially could have led to some bias in the results. However, one could argue that the contribution of the ERPs may have actually strengthened the indicators because of a better understanding of context reflecting diverse practice settings. Moreover, administrative and physician stakeholders, as well as patients, were included in the development of the indicators to help eliminate any issues of bias.
Conclusion
Overall, this two-year, system-level evaluation yielded detailed information regarding how ACPAC program–trained ERPs are providing integrated and timely care for Ontarians with arthritis, particularly those with OA. These practitioners reported unique roles in triaging patients and working under medical directives.
Intégration dans le système et utilisation clinique des praticiens aux fonctions élargies formés dans le cadre du programme Advanced Clinician Practitioner in Arthritis Care (ACPAC) en Ontario : évaluation de deux ans au niveau du système
Résumé
Contexte : Le programme Praticiens cliniques avancés dans le traitement de l'arthrite (Advanced Clinician Practitioner in Arthritis Care, ACPAC) a été créé en 2005 pour préparer des physiothérapeutes et des ergothérapeutes expérimentés à remplir le rôle de praticiens aux fonctions élargies (PFE) au sein de modèles de traitement de l'arthrite en Ontario, Canada.
Objet : Examiner l'intégration au niveau du système et l'utilisation clinique des PFE formés dans le cadre du programme ACPAC.
Méthode : Nous avons mené une enquête longitudinale auprès de tous les diplômés de l'ACPAC pendant une période de deux ans (n=30).
Résultats : La majorité des PFE étaient des physiothérapeutes qui travaillaient dans des établissements urbains. La majorité des patients y étaient acheminés par des médecins de famille ou des spécialistes. La plus longue médiane pour le temps d'attente avant d'accéder aux services d'un PFE était de 22 jours. La moitié des patients qui ont été dirigé par triage par un PFE, et la plupart de ceux qui ont effectué le triage (75 %), ont travaillé sous direction médicale. Environ la moitié (51,6 %) des patients traités avaient reçu un diagnostic d'ostéo-arthrite, suivi de l'arthrite rhumatoïde (14,7 %).
Conclusion : Mieux comprendre l'impact, à l'échelon du système, de cette ressource humaine unique peut aider la planification de services de santé et la prestation des soins.
About the Author(s)
Laura A. Passalent, MHSc, ACPAC, Physiotherapist Practitioner, Toronto Western Hospital, Lecturer, Department of Physical Therapy, University of Toronto, Toronto, ON
Carol Kennedy, MSc, Research Associate, Mobility Program Clinical Research Unit, St. Michael's Hospital, Research Associate, Institute for Work & Health, Lecturer, Department of Physical Therapy, University of Toronto, Toronto, ON
Kelly Warmington, OCT, BeD, MEd, Research Coordinator, Mobility Program Clinical Research Unit,, Keenan Research Centre, St. Michael's Hospital, Toronto, ON
Leslie J. Soever, MSc, ACPAC, Advanced Practice Physiotherapist, Mt. Sinai Hospital, Lecturer, Department of Physical Therapy, University of Toronto, Toronto, ON
Katie Lundon, MSc, PhD, ACPAC Program, St. Michael's Hospital, Department of Medicine, University of Toronto, Toronto, ON
Rachel Shupak, MD, Rheumatologist and ACPAC Program Director, St. Michael's Hospital, Director of Education, The Martin Family Centre for Arthritis Care and Research, St. Michael's Hospital, Associate Professor, Department of Medicine, University of Toronto, Toronto, ON
Sydney Lineker, PhD, Director of Research, The Arthritis Society, Ontario Division, Toronto, ON
Rayfel Schneider, MD, MBBCh, Rheumatologist, Associate Chair of Education, Paediatrics, Hospital for Sick Children, Toronto, ON
Correspondence may be addressed to: Laura A. Passalent, e-mail: laura.passalent@uhn.ca.
Acknowledgment
Other authors of this paper include Sydney Lineker, PhD, Director of Research, The Arthritis Society, Ontario Division, Toronto, ON, and Rayfel Schneider, MD, MBBCh, Rheumatologist, Associate Chair of Education, Paediatrics, Hospital for Sick Children, Toronto, ON.
References
Badley, E.M., P. Veinot, H. Ansari and C. MacKay. 2008. "2007 Survey of Rheumatologists in Ontario." Arthritis Community Research and Evaluation Unit (ACREU). Retrieved April 12, 2013. <http://www.acreu.ca/pdf/pub5/08-03.pdf>.
Badley, E.M., P. Veinot, J. Tyas, M. Canizares, C. MacKay, A. Davis and N. Mahomed. 2007. "2006 Survey of Orthopaedic Surgeons in Ontario." Arthritis Community Research and Evaluation Unit (ACREU). Retrieved April 12, 2013. <http://www.acreu.ca/pdf/pub5/07-03.pdf>.
Bombardier, C., G. Hawker and D. Mosher. 2011. "The Impact of Arthritis in Canada: Today and Over the Next 30 Years." Arthritis Alliance of Canada. Retrieved April 12, 2013. <http://www.arthritisnetwork.ca/downloads/20111022_Impact_of_arthritis.pdf>.
College of Physiotherapists of Ontario. 2008. "Performing Controlled Acts: Guide to the Standards of Professional Practice." Retrieved April 12, 2013. <http://www.collegept.org>.
Cott, C., S. Jaglal, I. McKillop, A. Brown, P. Blackstien-Hirsch, M. Canizares et al. 2005. "Hospital Report 2005: Rehabilitation." Joint Initiative of the Ontario Hospital Association and the Government of Ontario. Toronto: Hospital Report Research Collaborative, University of Toronto.
Desmueles, F., J. Roy, J.C. MacDermid, F. Champagne, O. Hinse and L.J. Woodhouse. 2012. "Advanced Practice Physiotherapy in Patients with Musculoskeletal Disorders: A Systematic Review." BMC Musculoskeletal Disorders 13: 107. doi: 10.1186/1471-2472-13-107.
Government of Ontario. 2011. Physiotherapy Act, 1991. Retrieved April 12, 2013. <http://www.e-laws.gov.on.ca/html/statutes/english/elaws_statutes_91p37_e.htm>.
Hospital for Sick Children. 2012. "Definition of Medical Directives." Retrieved April 12, 2013. <http://www.sickkids.ca/medicaldirectives/101/definition/index.html>.
Jamal, S., M.H. Shabbir, E.M. Badley and C. Bombardier. 2011. "Time to Treatment for New Patients with Rheumatoid Arthritis in a Major Metropolitan City." Journal of Rheumatology 38(7): 1282–88.
Kaplan, R.S. and D.P. Norton. 1996. Translating Strategy into Action: The Balanced Scorecard. Boston: Harvard Business School Press.
Lundon, K., R. Shupak, S. Reeves, R. Schneider and J. McIlroy. 2009. "The Advanced Clinician Practitioner in Arthritis Care Program: An Interprofessional Model for Transfer of Knowledge for Advanced Practice Practitioners." Journal of Interprofessional Care 23(2): 198–200.
Lundon, K., R. Shupak, R. Schneider and J. Herold McIlroy. 2011. "Development and Early Evaluation of Interprofessional Post-Licensure Education Programme for Extended Practice Roles in Arthritis Care." Physiotherapy Canada 63(1): 94–103.
Lundon, K., R. Shupak, L. Sunstrum-Mann, D. Galet and R. Schneider. 2008. "Leading Change in the Transformation of Arthritis Care through Development of an Interprofessional Academic Clinical Education Training Model." Healthcare Quarterly 11(3): 62–68.
Ministry of Health and Long-Term Care (MOHLTC). 2007. "Hip and Knee Replacement Program." Retrieved April 12, 2013. <http://www.ontla.on.ca/library/repository/mon/20000/274844.pdf>.
Ministry of Health and Long-Term Care (MOHLTC). 2008. "Health Care Priorities." Retrieved April 12, 2013. <http://www.health.gov.on.ca/english/public/updates/archives/hu_08/health_care_priorities_20080424.html>.
Ministry of Health and Long-Term Care (MOHLTC). 2011. "Wait Times Provincial Trends." Retrieved April 12, 2013. <http://www.waittimes.net/Surgerydi/en/Type.aspx>.
Ontario Medical Association (OMA). 2007. "Ontario Physician Shortage." Retrieved April 12, 2013. <http://www.oma.org/Mediaroom/Backgrounders/Pages?OntarioPhysicianShortage2007.aspx>.
Petty, R.E., T.R. Southwood, P. Manners, J. Baum, D.N. Glass, J. Goldenberg et al. 2004. "International League of Associations for Rheumatology Classification of Juvenile Idiopathic Arthritis: Second Revision, Edmonton, 2001." Journal of Rheumatology 31: 390–92.
Razmjou, H., S. Robarts, D. Kennedy, C. McKnight, A.M. MacLeod and R. Holtby. 2012. "Evaluation of an Advanced-Practice Physical Therapist in a Specialty Shoulder Clinic: Diagnostic Agreement and Effect on Wait Times." Physiotherapy Canada. doi: 10.3138/ptc.2011-56.
World Health Organization (WHO). 2010. "Chapter XIII: Diseases of the Musculoskeletal System and Connective Tissue (M00–M99)." International Classification of Diseases and Related Health Problems (10th rev.). Retrieved April 12, 2013. <http://apps.who.int/classifications/icd10/browse/2010/en#/XIII>.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed