Healthcare Policy
Active Referral: An Innovative Approach to Engaging Traditional Health Providers in TB Control in Burkina Faso
Abstract
Background and objective: The involvement of traditional healthcare providers (THPs) has been suggested among strategies to increase tuberculosis case detection. Burkina Faso has embarked on such an attempt. This study is a preliminary assessment of that model.
Methods: Qualitative data were collected using unstructured key informant interviews with policy makers, group interviews with THPs and health workers, and field visits to THPs. Quantitative data were collected from program reports and the national tuberculosis (TB) control database.
Results and analysis: The distribution of tasks among THPs, intermediary organizations and clinicians is appealing, especially the focus on active referral. THPs are offered incentives based on numbers of suspected cases confirmed by health workers at the clinic, based on microscopy results or clinical assessment. The positivity rate was 23% and 9% for 2006 and 2007, respectively. The contribution of the program to national case detection was estimated at 2% for 2006. Because it relied totally on donor funding, the program suffered from irregular disbursements, resulting in periodic decreases in activities and outcomes.
Conclusions: The study shows that single interventions require a broader positive policy environment to be sustainable. Even if the active referral approach seems effective in enhancing TB case detection, more complex policy work and direction, domestic financial contribution and additional evidence for cost-effectiveness are needed before the approach can be established as a national policy.
Healthcare in any country consists of several subcomponents that enjoy different levels of support from public health authorities. According to Arthur Kleinmann, pluralist healthcare systems are characterized by the coexistence of three different sectors of healthcare: the professional sector, the popular sector and the folk sector (cited in Helman 2007). The professional sector consists of scientific, allopathic medicine practitioners; the popular sector comprises families, friends and other useful reference people from whom a patient can seek advice; and the folk sector is represented by practitioners of non-Western medicine who specialize in curing or caring for various physical or spiritual problems.
In most African countries, this folk sector is large and known as traditional medicine. Prior to the emergence of the HIV epidemic, public health policies remained ambiguous as to the role this sector had to play in healthcare. However, since early 2000, the situation has changed as many governments and international agencies realized that countries needed multisectoral responses to the epidemic (Burford et al. 2000; Liverpool et al. 2004). Traditional medicine and its practitioners started to be seen as resources that policy makers needed to capitalize upon. Interventions of different kinds were initiated to assess the role of this sector in addressing diverse disease-specific issues (Sorsdahl et al. 2009).
From the point of view of global health policy, increased recognition during the end of the last decade by The Global Fund (for tuberculosis and HIV, specifically) of the role of civil society and local non-governmental organizations (NGOs) in the delivery of preventive and treatment services led many principal recipients of funds to consider involving local organizations in their programs. This recognition culminated in the introduction of so-called dual-track financing, which has been an important policy development at The Global Fund (2012). Dual-track financing allows countries to enable civil society and the private sector to become principal recipients. This approach was seen as an innovation, given that grants management in some countries had become a monopoly of large international organizations, and ministries of health in other countries.
With regard to global efforts to control tuberculosis (TB), increasing success in case detection and treatment has been the critical goal of every TB control program since 1991, when the World Health Assembly set targets of a 70% case detection rate and an 85% treatment success rate by 2000 (the target year was later reset to 2005). Globally, Africa has the lowest case detection rate compared to other world regions. Several approaches to increase case detection have been tried, including systematic engagement of private providers. In African settings, numerous initiatives to involve providers of traditional medicine have been attempted (Banerjee et al. 2004; Chakaya et al. 2008; Colvin et al. 2003; Wilkinson et al. 1999). However, many of these remain largely undocumented, turning sometimes useful experiences into simple local, inconsequential events, despite interesting policy challenges and lessons that could be drawn from them.
The World Health Organization's Stop TB Department has embarked on a process of identifying and documenting many of these initiatives in order to allow cross-country learning and exchanges, as well as to inform development of policy guidance for national disease control programs. Lessons from these examples could elucidate several high-level policy challenges, ranging from health systems–related issues (e.g., human resources, linking community and clinical services, national stewardship) to issues related to the impact of global health financing mechanisms. It is against this background that the Burkina Faso experience of involving traditional health practitioners in TB case finding might be worthy of exploration.
Burkina Faso is a landlocked country in West Africa, with a population of over 15 million. The TB incidence rate is estimated at 57 (48–66) per 100,000 population. TB notification data in 2011 indicated a total of 5,543 cases, of which 3,450 (68%) were smear-positive. With 5,286 TB cases detected out of 9,700 cases estimated, the detection rate – which indicates the percentage of reported cases against the estimated number of cases occurring – is low in Burkina Faso, at 55% (uncertainty interval, 47%–65%) (WHO 2011). This low rate indicates a significant gap, meaning that many TB cases are still missed. Improving this rate has been the central goal of the Burkina Faso TB control community, under the coordination of the national TB control program. One initiative has consisted of an attempt to systematically engage traditional healthcare practitioners (THPs) in TB case finding. The initiative has been implemented since 2006 within the framework of the Programme d'appui au monde associatif et communautaire (PAMAC; "community and associative sector support program") owned and run by the United Nations Development Program (UNDP).
It is estimated that there are about 30,000 THPs in Burkina Faso, compared to the 9,000 nurses and physicians available in the country (Professor Nikiéma, Head of the Unit for Promotion of Traditional Medicine, Ministry of Health, Burkina Faso, personal communication, 2008). Burkina Faso has a national association of THPs, the ANAPHARM (Association nationale des acteurs de la pharmacopée et de la médecine).
Features of the Burkina Faso TB Control Program Model
Multiple intermediaries' roles
Intermediary organizations included all the various institutions that act as facilitators between health facilities and the National Tuberculosis Program (NTP) (i.e., representatives of the Ministry of Health) on one side and individual THPs on the other. The foremost intermediary was the UNDP through PAMAC, an arrangement that ensured the overall coordination and liaising function at the national level, including financial management, monitoring and evaluation (the centralization of reports). The UNDP was responsible for the program vis-à-vis the NTP and the country coordination mechanism that assumes countrywide coordination and policy advocacy.
The second level was a network of community support organizations (called structures pivots). This is a stronger association with substantial capacity in managing projects and in monitoring its own and smaller partners' projects. Such an organization was selected to partner with PAMAC, utilizing the latter's capacity in data collection and research, and in maintaining working relationships with health authorities at the district and provincial levels. The chosen organization had to be specialized in information, education and communication (IEC) activities at the community level as well as in community care and/or advocacy for people living with HIV/AIDS and TB. Such organizations might operate in a large area, such as a region or province. To be selected for the TB program, an organization had to submit an action plan that was consistent with the NTP's and PAMAC's objectives and that took into consideration the needs and activities of the implementing member associations at the grassroots level.
A third level of intermediary organization was the one made of providers' associations: these associations allow THPs to have a unified voice vis-à-vis the health facilities, other organizations and PAMAC. Such associations were responsible for training their members, and for dealing with all issues and processes related to payment of incentives to or compensation of their members for their participation. The associations are generally responsible for limited sub-areas within a district.
The role assigned to individual THPs
Finally, individual THPs were selected by their organizations. The task assigned to THPs according to the model was limited to referral of suspected cases to the nearest health facility. THPs were not formally involved in IEC activities, e.g., community mobilization. Neither were they involved in TB treatment supervision, known as directly observed treatment (DOT).
Operational steps in engagement of THPs
At the preparatory stage, PAMAC interacted with provincial and district health facilities to select a potential network of organizations (the structures pivots) to work with. When this network was selected, viable THP associations were identified among the membership or the partners of the network, and later individual THPs were identified. The following steps were essential in the operational process of working with THPs.
- Training: A number of THPs were selected by their associations and trained by the health district staff on TB, its symptoms and management according to the NTP's guidelines.
- Active referral: THPs were encouraged, whenever possible, to personally ensure they accompanied patients to the TB clinic, beyond providing them with a written referral form.
- Feedback collection: Every month, the president or coordinator of the THPs' association contacted the TB clinic to collect feedback papers.
- Monthly meetings with the TB clinic staff: The purpose of these was to discuss the progress of the collaboration and solve any identified problems.
- Quarterly reporting and payment of incentives: Feedback documents were compiled every quarter, and referring THPs were reimbursed 1,000 CFA francs (2.5 USD) per suspected case referred and confirmed by the clinicians (and therefore tested for TB), irrespective of whether the patients were found to be infected with TB.
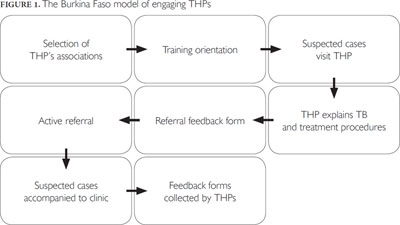
Figure 1 illustrates this process.
This paper is a preliminary evaluation of the approach used in this initiative to engage THPs in the capital, Ouagadougou, and Bobo Dioulasso, the country's second largest city. Analysis of the operational features of the model, of the main perceptions of the key parties involved and the policy environment surrounding it is likely to help identify some critical elements that could contribute to enhancing the success of such endeavours in Burkina Faso and beyond, especially in countries with a high TB burden and a significant presence of traditional medicine practitioners.
Aim of the Study
The aim of this study was to assess the contribution of a model of involvement of THPs to TB case finding in Burkina Faso and explore the perceptions of key stakeholders (THPs, nurses, policy makers) involved in its implementation.
Methods
Data collection
Both qualitative and quantitative data were used to explore THPs' involvement in TB case finding in Burkina Faso. The qualitative part included unstructured interviews with key informants that were held with three high-level officers of the National Tuberculosis Program (including the NTP manager). In addition, two group interviews with THPs in Ouagadougou were held (with over 20 participants each time) and one with health workers (five participants) in a TB clinic. Field visits (two) were paid to traditional practitioners involved in the collaboration, to see their working environment in the community. Available quantitative data were collected from the UNDP-supported program (PAMAC) that oversaw the involvement of THPs in TB control in the country. All the data were collected during a visit to Burkina Faso in June 2008.
The interview guide, used both for key informants and for group interviews, was generic and focused on key issues such as how THPs and health workers described their collaboration with the clinic, how the NTP perceived the whole initiative of working with THPs, the challenges experienced by each group of participants in the initiative and how they thought these could best be addressed. The qualitative interviews were basically aimed to facilitate understanding of participants' feelings about their experiences and of the dynamics of the program in order to interpret the quantitative data generated by the program and to identify trends. In other words, the qualitative interviews aimed at understanding the processes from different actors' perspective as well as the overall policy framework, whereas the quantitative data focused on the outcomes as reported in the program's documents. The qualitative data were recorded through minutes taken by the author, who was assisted by one or two PAMAC employees who helped clarify any issues that came up in the discussions.
Data analysis
The qualitative information was summarized under themes such as the roles of THPs, the nature of relationships between THPs and the supervising local NGO, the nature of interactions among THPs, NGOs and the NTP (and other services within the Ministry of Health), the role of UNDP in the context and so on. The quantitative data were entered in Excel and analyzed using SPSS Version 20.
Results
Policy context surrounding THPs' engagement in TB control
The engagement of THPs started in 2005 with the HIV control program. The Global Fund's grant round 4 included a substantial community engagement component that required UNDP to set up PAMAC. The engagement of THPs became part of this generic program, which was initially aimed at supporting the National AIDS Commission in involving community and civil society organizations in scaling up prevention, voluntary counselling and testing (VCT) and community-based care for AIDS patients. In 2006, the NTP requested PAMAC to take charge of the community component of its program.
Findings from the interviews with policy makers indicated that despite the Ministry of Health's general policy on promoting traditional medicine and its practitioners, the policy had no explicit implementation direction in relation to specific disease control efforts. The content of the policy was unknown even to highly placed policy makers outside the Ministry's sector in charge of those questions. It appeared, therefore, that THPs' participation in TB case finding was a short-lived, standalone program, disconnected from the broader policy in which it should have been embedded. Another indication of this lack of alignment was that the intervention had no relation with any other initiative involving THPs in other health provision services (HIV, malaria, maternal health, etc.).
Stakeholders' perceptions of the intervention
NATIONAL TUBERCULOSIS PROGRAM
NTP officers appeared satisfied with the UNDP-sponsored program, and indicated they had given it their full support and mandate to care for the community involvement component of the national response to control TB. However, their attitude indicated a kind of detachment, as if they would not invest time and resources in this endeavour should UNDP not accept responsibility for it. The absence of a clear, or even tentative, vision of plans to scale up this intervention beyond the two major cities of Ouagadougou and Bobo Dioulasso was another indication that the intervention was seen as a temporary one.
UNDP/PAMAC
The owners of the program appeared satisfied with its progress and achievements. What mattered most to them was to ensure optimal program performance, that funding was available and that there were no major problems between the THP associations and health facilities. Long-term issues of program sustainability or program alignment with other disease control programs beyond TB, or with broader health system constraints, were not of concern.
A strong focus of the owners' support to other actors in the program's implementation was on monitoring and evaluation (M&E), to ensure that all data were recorded and the report transmitted. This M&E focus was reflected in the fact that intermediaries at lower levels of the implementation network (the structures pivots) were properly equipped with computers and software, enabling them to produce progress reports at any time.
NURSES
The nurses described their experiences of working with THPs and the THP organizations as fruitful, responsive and characterized by mutual respect. Nurses reported no major difficulties with this collaboration. They highly valued the contribution of THPs to TB case finding in the community. Nurses wanted to see THPs take on even more responsibilities in relation to TB care, including, for example, supervision of TB treatment, instead of just case finding.
Nurses saw also in THPs a huge potential with respect to efforts to control other diseases (HIV, malaria, etc.). Nurses expressed their satisfaction in relation to THPs' performance, especially regarding the proper assessment of suspected TB cases.
TRADITIONAL HEALTH PRACTITIONERS
THPs were generally satisfied with their interactions with staff at TB clinics. They were rather surprised that the work had gone so smoothly, and that they were respectfully received by health workers at the centres. THPs also thought that the task assigned to them of identifying suspected TB cases was minimal, as they believed they were capable of doing much more. They referred, among other things, to training opportunities they had attended (each THP could show at least five certificates). They hoped that this initiative would be a pilot for more comprehensive involvement in healthcare.
The compensation that the model provided was seen as a positive incentive that many THPs appreciated. Some pointed out, however, that the incentive was meagre in some circumstances, such as when a THP lived far from the health facility and needed to pay travel expenses for him/herself and his/her patients.
Another dimension in which THPs would call for improvement is the role assigned to their professional organizations. These associations' role was also very reduced, limited to selecting THPs before initial involvement and training and periodically for collecting and distributing compensation. THPs thought that their associations could play a bigger role in liaising with UNDP/PAMAC and with the NTP, which was not the case. It was rather the structures pivots, the network of organizations, that interacted with UNDP and the NTP, for the sake of monitoring program activities.
Outcome Data in 2006 and 2007
Referral and detection of suspected TB cases
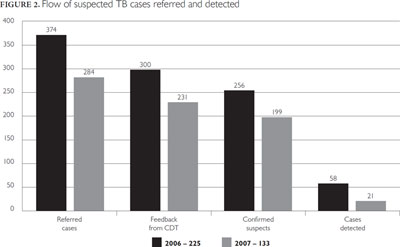
The project was initiated in Ouagadougou and Bobo Dioulasso in 2006. It has so far been limited to a few health districts in these two cities. Figure 2 provides an overview of the number of suspected cases referred and detected.
Analysis of lost cases and positivity ratios
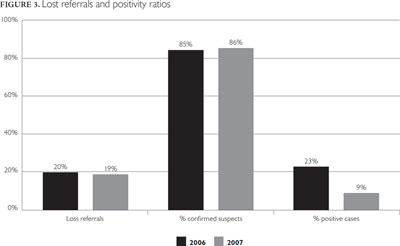
Figure 3 is based on Figure 2 and suggests more details on proportions of lost suspected and detected cases. Confirmed suspected cases represent the proportion of cases referred by THPs that were, after first consultation, deemed by the clinician to be serious; the higher the proportion, the higher the level of consistency between clinicians' and THPs' assessments.
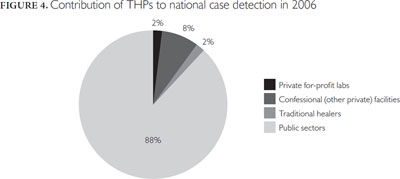
Contribution to national TB detection
Given the national figures of new smear-positive cases detected for 2006, the contribution of THPs was assessed and compared to that of other major private providers involved in collaboration with the National Tuberculosis Program (Figure 4).
Discussion
THPs have been recognized as important pillars in healthcare in several communities in sub-Saharan Africa. Major national disease-specific programs have increasingly called for, and attempted, involving these providers to increase accessibility and acceptability of health services (Banerjee et al. 2004; Kayombo et al. 2005; King and Homsy 1997; Magassouba et al. 2007). THPs' involvement has even been called for and tested in respect to non-communicable disease management (Mbeh et al. 2010).
This experience from Burkina Faso indicates that in the health sector, as in other social policy areas, policy development is complicated because it is informed by many aspects that go well beyond individual interventions. In other words, the existence of clear and pressing needs (e.g., TB case detection) and effective interventions does not always lead to quick fixes in term of policy formulation. Efficacy of a standalone intervention is not enough to trigger major policy shifts unless other policy context specificities are acted upon. Policy making is complex, time-consuming and not necessarily rational (Watt 2004). Such policy-related complexities probably explain why the dream of realizing a harmonious involvement of THPs in healthcare has not so far been achieved. In relation to THPs' involvement in healthcare provision, a major impediment has always been the absence of a sectorwide policy orientation regulating collaboration between conventional medicine practitioners and THPs.
In TB control, as in other disease control efforts, one of the critical impediments to constructive involvement of THPs in healthcare has been the lack of a generic model of engagement of these providers. This has resulted in the application of small-scale and contextual models, which in turn has complicated replication and comparison of initiatives. The Burkina Faso approach discussed in this paper appears to be an interesting model from which lessons can be learned.
The most attractive feature of this model is the "active referral" concept, i.e., encouraging THPs to accompany their patients on visits to health facilities for TB screening. This activity presupposes that THPs should be convinced of the seriousness of the case, and that they must be equipped with the necessary skills to convince patients of the need to take a TB test. Furthermore, the receptivity of health facility personnel is another key factor that determines whether THPs will tend only to refer patients with suspected TB or will escort them to the clinic. In the case of the Burkina Faso study, THPs reported positive attitudes and interactions with the health workers at TB clinics. Thus, the model needs to build on this positive groundwork, including not only training of THPs but, most importantly, the sensitization of health professionals at the facility level. The Burkina Faso model is innovative in that it goes beyond the traditional "training fallacy," i.e., a focus on the training of THPs as the sole means to involve them in healthcare. The Burkina Faso model provides for a mix of roles for actors and organizations, including incentives to THPs.
The distribution of tasks between participating partners, despite being minimalist, seems appropriate; this is another important component in such collaborative frameworks. THPs refer, their associations take care of the incentive reimbursements and health facilities manage the medical issues. This structure of task distribution appears acceptable, given that the epidemiological situation of TB, HIV and TB/HIV co-infection in the country is moderate. What was remarkable in this study was the call from nurses recommending increased involvement of the THPs, whom they considered to be performing well. Increased tasks would imply wider focus and, therefore, greater impact.
The fact that the THPs' role was limited to referrals implies that supporters of the initiative (i.e., UNDP/PAMAC and NTP) made no value judgment regarding other healthcare-related operations in which THPs might be involved. One could argue that the Burkina Faso model built on an instrumental approach to involving THPs as opposed to an idealist approach. The lack of any role for the national associations of THPs that might promote traditional medicine more broadly, as well as the lack of any mention in national policy for promoting traditional medicine, are evidence of this instrumental and disease-specific perspective. Broader promotion of traditional medicine would significantly increase support for the THPs' associations, mostly through capacity-building initiatives well beyond the mere monitoring of the TB project's outputs. Such an ambitious agenda would demand stronger national ownership.
A survey of the TB project's quantitative outcomes indicates that the model might be effective. The positivity ratio of 23% in 2006 and 9% in 2007 means that THPs' pre-screening assessment of suspected TB cases was as accurate as that of qualified clinicians. The initiative's contribution to national TB case detection is as effective as that of formal private laboratories involved in public–private collaboration in the country. This finding indicates a largely untapped opportunity, considering the huge population of uninvolved THPs.
Because this program has so far been implemented only in urban settings, nothing can be said about the feasibility of active referral in rural areas. Transportation difficulties might constitute the main obstacle to active referrals in such settings. Also, collaboration has so far involved only public facilities. It is uncertain whether so-called confessional facilities (private clinics) would be equally keen to work with THPs.
One potentially controversial aspect in the Burkina Faso initiative is the reimbursement of incentives to THPs. To me, these incentives are not only acceptable, but also equitable and insignificant in terms of cost to the program. The problem is the project's dependence on foreign funding. In fact, the declining trends observed in 2007 were due to decreases in global funding and a consequent reduction in activities. Stable funding is thus critical to the program's sustainability and scalability.
One limitation of this study is that it has not been possible to compare program outcomes with TB case-finding data from previous years in these geographic regions. Such data were unavailable at the health centres, and could not be retrieved from central data at the NTP level. For this reason, the information discussed in this paper relates only to the project implementation period.
Policy Implications
The key message of this paper is the importance of policy environment rather than simple outcome statistics. What are the policy options, and how may countries derive greater benefit from their traditional healthcare sectors? Four dimensions, in particular, demand attention.
1. Strategic policy direction
This dimension, essential to success, was found to be weak in Burkina Faso as there was no policy framework backing the intervention. The Ministry of Health unit in charge of traditional medicine should play a role in ensuring that interventions are firmly embedded in policy so that results can, in turn, feed into policy formulation. Otherwise, interventions turn into isolated phenomena.
2. National ownership of intervention
Ownership here is different from the nationality of the operational agent. The Burkina Faso intervention was fully run by domestic actors (national program, national health facilities, etc.), but funding was fully external. Consequently, once funding was delayed, the project nearly closed down. One might even wonder if the intervention was more motivated by the imperative of disbursing financial surpluses from international donors than by meeting genuine public health needs. This is not to say that such was the case in Burkina Faso, but fluctuation in the project's activities suggests the need to spend available excess resources. Sustainability would be better served if such initiatives were included in the national budget. Such inclusion would indicate policy makers' seriousness with regard to incorporating the traditional medicine sector.
3. Cost-effectiveness studies
Preliminary assessment seems to indicate the viability of this approach in enhancing active detection of TB cases. However, cost-effectiveness studies would reinforce the evidence base. Cost-effectiveness analyses covering longer periods are called for before active referral approaches can be scaled up and their replication recommended.
4. Broader integration vs. disease-specific collaboration
Broader integration of THPs within the spectrum of public healthcare activities would be more advantageous than relying on multiple, short-lived and ad hoc interventions initiated by specific disease control programs. From the perspective of public health policy and strengthening health systems, broader integration is a more demanding approach but would signal how committed policy makers are to including THPs in comprehensive healthcare.
Conclusion
Active referral by THPs might be an option in enhancing TB case finding. However, viability of such interventions requires more high-level policy work in terms of strategic direction and the broader needs and imperatives of the public health sector. Also, dependence on foreign funding will remain a serious threat to program sustainability as long as national budgets fail to bear a significant portion of the costs.
L'orientation active : une démarche novatrice pour favoriser la participation des prestataires de soins de santé traditionnels dans le contrôle de la tuberculose au Burkina Faso
Résumé
Contexte et objectif : La participation des prestataires de soins de santé traditionnels (PST) a été proposée comme stratégie pour accroître la détection de cas. Le Burkina Faso a mis cette stratégie à l'essai. La présente étude est une évaluation préliminaire de ce modèle.
Méthodes : Les données qualitatives ont été recueillies par : des entrevues non-structurées auprès d'informateurs clés, notamment des responsables de politiques; des entretiens de groupes avec des PST et des travailleurs de la santé; et des visites pour rencontrer les PST sur le terrain. Les données quantitatives proviennent des rapports du programme ainsi que de la base de données nationales sur le contrôle de la tuberculose.
Résultats et analyse : La distribution des tâches entre les PST, les organisations intermédiaires et les cliniciens est intéressante, particulièrement l'accent mis sur l'orientation active. Les PST reçoivent des incitatifs en fonction du nombre de cas suspects confirmés par les professionnels de la clinique, à l'aide des résultats de microscopie et des évaluations cliniques. Les taux positifs étaient de 23 % et 9 % respectivement pour 2006 et 2007. L'apport du programme à la détection de cas à l'échelle nationale a été estimé à 2 % pour 2006. Puisqu'il repose entièrement sur le financement de donateurs, le programme souffre de versements irréguliers, ce qui a causé un déclin des activités et des résultats.
Conclusions : L'étude montre que la durabilité des interventions est tributaire d'un environnement politique plus favorable. Même si la démarche de l'orientation active semble efficace pour accroître la détection de cas de tuberculose, il faudra mettre en place des politiques complexes, assurer une contribution financière intérieure et obtenir plus de données sur le rapport coût-efficacité avant d'implanter la démarche à l'échelle nationale.
About the Author(s)
Berthollet Bwira Kaboru, PhD, Senior Lecturer, School of Health and Medical Sciences, Örebro University, Örebro, Sweden
Correspondence may be directed to: Berthollet Bwira Kaboru, PhD, Senior Lecturer, School of Health and Medical Sciences, Örebro University, 701 82 Örebro, Sweden; tel.: +46 (0) 19 30 11 84; e-mail: Berthollet.Kaboru@oru.se.
Acknowledgment
I am grateful to Dr. Mathurin Dembele, Manager of NTP Burkina Faso, and Dr. Fodé Simaga, Director of PAMAC, for their support during the collection of the data for this study. I also wish to thank the THPs, TB clinic personnel and the staff of the Kasabati Association for facilitating my field visits and taking part in the interviews.
References
Banerjee, A., B.V. Sharma, A. Ray, N.K. Kannuri and T.V. Venkateswarlu. 2004. "Acceptability of Traditional Healers as Directly Observed Treatment Providers in Tuberculosis Control in a Tribal Area of Andhra Pradesh, India." International Journal of Tuberculosis and Lung Disease 8(10): 1260–65.
Burford, G., G. Bodeker, D. Kabatesi, B. Gemmill and E. Rukangira. 2000. "Traditional Medicine and HIV/AIDS in Africa: A Report from the International Conference on Medicinal Plants, Traditional Medicine and Local Communities in Africa (a parallel session to the Fifth Conference of the Parties to the Convention on Biological Diversity, Nairobi, Kenya, May 16–19, 2000)." Journal of Alternative and Complementary Medicine 6(5): 457–71.
Chakaya, J., M. Uplekar, J. Mansoer, A. Kutwa, G. Karanja, G., V. Ombeka et al. 2008. "Public–Private Mix for Control of Tuberculosis and TB-HIV in Nairobi, Kenya: Outcomes, Opportunities and Obstacles." International Journal of Tuberculosis and Lung Disease 12(11): 1274–78.
Colvin, M., L. Gumede, K. Grimwade, D. Maher and D. Wilkinson. 2003. "Contribution of Traditional Healers to a Rural Tuberculosis Control Programme in Hlabisa, South Africa." International Journal of Tuberculosis and Lung Disease 7(9 Suppl. 1): S86–91.
Helman, C.G. 2007. Culture, Health and Illness (5th ed.). Oxford: Hodder Arnold.
Kayombo, E.J., Z.H. Mbwambo and M. Massila. 2005. "Role of Traditional Healers in Psychosocial Support in Caring for the Orphans: A Case of Dar-es Salaam City, Tanzania." Journal of Ethnobiology and Ethnomedicine 1, 3. doi: 10.1186/1746-4269-1-3.
King, R. and J. Homsy. 1997. "Involving Traditional Healers in AIDS Education and Counselling in Sub-Saharan Africa: A Review." AIDS 11 (Suppl. A): S217–25.
Liverpool, J., R. Alexander, M. Johnson, E.K. Ebba, S. Francis and C. Liverpool. 2004. "Western Medicine and Traditional Healers: Partners in the Fight against HIV/AIDS." Journal of the National Medical Association 96(6): 822–25.
Magassouba, F.B., A. Diallo, M. Kouyate, F. Mara, O. Mara, O. Bangoura et al. 2007. "Ethnobotanical Survey and Antibacterial Activity of Some Plants Used in Guinean Traditional Medicine." Journal of Ethnopharmacology 114(1): 44–53. doi: 10.1016/j.jep.2007.07.009.
Mbeh, G.N., R. Edwards, G. Ngufor, F. Assah, L. Fezeu and J.C. Mbanya. 2010. "Traditional Healers and Diabetes: Results from a Pilot Project to Train Traditional Healers to Provide Health Education and Appropriate Health Care Practices for Diabetes Patients in Cameroon." Global Health Promotion 17(2 Suppl.): 17–26. doi: 10.1177/1757975910363925.
Sorsdahl, K., J.C. Ipser and D.J. Stein. 2009. "Interventions for Educating Traditional Healers about STD and HIV Medicine." Cochrane Database of Systematic Reviews 4, CD007190. doi: 10.1002/14651858.CD007190.pub2.
The Global Fund. 2012. "Information Note: Global Fund Engagement with Civil Society." Retrieved September 27, 2013. <http://www.theglobalfund.org/en/partners/civilsociety/>.
Watt, G. 2004. Health Policy: An Introduction to Process and Power. Johannesburg: Witwatersrand University Press and Zed Books.
Wilkinson, D., L. Gcabashe and M. Lurie. 1999. "Traditional Healers as Tuberculosis Treatment Supervisors: Precedent and Potential." International Journal of Tuberculosis and Lung Disease 3(9): 838–42.
World Health Organization (WHO). 2011. Tuberculosis Country Profiles. "Burkina Faso." Retrieved September 27, 2013. <http://www.who.int/tb/country/data/profiles/en/>
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed