World Health & Population
Urbanization and Health in Developing Countries: A Systematic Review
Abstract
Background: Future population growth will take place predominantly in cities of the developing world. The impact of urbanization on health is discussed controversially. We review recent research on urban-rural and intra-urban health differences in developing countries and investigate whether a health advantage was found for urban areas.
Methods: We systematically searched the databases JSTOR, PubMed, ScienceDirect and SSRN for studies that compare health status in urban and rural areas. The studies had to examine selected World Health Organization health indicators.
Results: Eleven studies of the association between urbanization and the selected health indicators in developing countries met our selection criteria. Urbanization was associated with a lower risk of undernutrition but a higher risk of overweight in children. A lower total fertility rate and lower odds of giving birth were found for urban areas. The association between urbanization and life expectancy was positive but insignificant. Common risk factors for chronic diseases were more prevalent in urban areas. Urban-rural differences in mortality from communicable diseases depended on the disease studied.
Conclusion: Several health outcomes were correlated with urbanization in developing countries. Urbanization may improve some health problems developing countries face and worsen others. Therefore, urbanization itself should not be embraced as a solution to health problems but should be accompanied by an informed and reactive health policy.
Introduction
More than half of the world's population inhabits urban areas (Dye 2008). The United Nations (UN) projects that the urban population will further increase from 3.3 billion to 4.9 billion worldwide by 2030 (UN 2007). Virtually all further population growth will take place in cities of the developing world, in which the rate of urbanization is faster than in developed countries (Alirol et al. 2011; Godfrey and Julien 2005).
Some argue that urbanization worsens the health status of the populations affected. If urbanization is unplanned and rapid, it is prone to producing informal settlements with insufficient housing, poor sanitary conditions and crowding, all of which can accelerate the spread of diseases (Godfrey and Julien 2005; Moore et al. 2003). Changes in the physical and social environment brought about by urbanization may increase the rate of mental disorders (Bhugra and Mastrogianni 2004; Penkalla and Kohler, forthcoming). Lifestyle changes may lead to an increase in accidents, violence-related disabilities and non-communicable diseases (NCDs) as causes of death (Bygbjerg 2012; Montgomery et al. 2003). The rapid upsurge in NCDs and NCD risk factors while low- and middle-income countries continue to deal with the problems of infectious disease and undernutrition causes a double burden of disease, which has been associated with urbanization (Marshall 2004; World Health Organization [WHO] 2013). With respect to the growing NCD burden, urbanization, economic growth, market integration, and foreign direct investment together have been described to correlate roughly three times stronger with long-term changes in the mortality rates of heart disease and chronic NCDs than population aging, particularly in low-income countries (Bygbjerg 2012; Stuckler 2008).
Others argue that infrastructure improvements such as better access to health services, education, sanitation and safe water supply through urbanization improve health (McDade and Adair 2001). Increased urbanization has been associated with greater malaria transmission reductions across countries and continents (Tatem et al. 2013). Access to information and communications technology, which is not yet widespread but fast-growing in developing countries, may increasingly influence disease prevention and health promotion opportunities in developing countries (Kohler 2013). However, the prior required increase in access to information and communications technology through urbanization in the developing world is already subject to debate (Chinn and Fairlie 2006, 2010).
This article reviews recent research on urban-rural and intra-urban health differences in developing countries as measured by some common health indicators.
Methods
Search Strategy
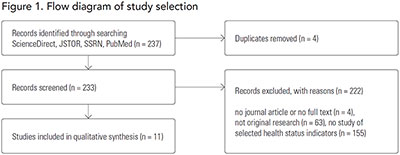
The databases JSTOR, PubMed, ScienceDirect and SSRN were searched from January 1, 2005 to October 23, 2012. The abstract, title or keywords had to include the terms urbanization, health and developing countries. Within PubMed, the MeSH-term urbanization was also searched in combination with the keywords child mortality, life expectancy, fertility, reproductive health, chronic disease and communicable disease (Figure 1).
Selection Criteria
We included studies in our review if they examined WHO health indicators of the leading causes of death or the general health status, and were original research, published in English as a journal article and available as full text. The 15 health indicators we selected cover five areas of health: general health (life expectancy, mortality rate); child health (under-five mortality, malnutrition); reproductive health (attended births, access to contraception, maternal mortality); prevalence of NCDs (hypertension, diabetes, obesity); and prevalence of communicable diseases (tuberculosis, HIV/AIDS, malaria, diarrhea, lower respiratory infections).
Studies were excluded if they investigated aspects of urbanization other than its influence on health, or health indicators different from the ones enumerated.
Data Extraction
We extracted data on the aims, country and population of the study, sample size, data source and time period studied, as well as health indicators. The health data we retrieved were deaths due to malaria, deaths due to diarrhea, occurrence of hypertension, diabetes and obesity, under-five mortality, childhood stunting, short stature, undernutrition and overnutrition, as well as fertility rates, the odds of giving birth within a year and life expectancy.
Results
A total of 11 studies met our inclusion criteria (Table 1). Two studies targeted several countries, while nine each focused on a single country.
| Table 1. Study characteristics | ||||||||
| Study | Country | Health indicator | Urbanization aspect | Study population | Study type | Data source | Study period | Sample size |
| Allender et al. 2011 | Sri Lanka | Chronic disease risk factors | Urban environment scale | Adults >18 years | Cross-sectional | Sri Lankan Diabetes and Cardio-vascular Study | 2007–2008 | 4,485 |
| Antai and Moradi 2010 | Nigeria | Under-five mortality | Urban socio-economic disadvantage | Children <5 years | Cross-sectional | Demographic and Health Survey | 2003 | 2,118 |
| Bergh and Nilsson 2010 | 92 countries | Life expectancy at birth | Globalization in 92 countries | Population | Longitudinal | Panel data set | 1970–2005 | 282–608 |
| Firestone et al. 2011 | Kanchanaburi, Thailand | Children's nutritional status | Urban and rural communities | Children 2–10 years | Cross-sectional | Kanchanaburi Demographic Surveillance System | 2004 | 4,610 |
| Fobil et al. 2011 | Accra, Ghana | Malaria or diarrhea mortality | Disparities in different neighbourhoods of Accra | Population | Cross-sectional | Ghanaian Vital Registry System | 1998–2002 | 1,001–1,292 |
| Niakara et al. 2007 | Ouagadougou, Burkina Faso | Hypertension risk | Exposure to rapid urbanization | Adults >35 years | Cross-sectional | Field research | 2004 | 2,044 |
| Sobngwi et al. 2004 | Cameroon | Stroke and myocardial infarct risk factors | Lifetime exposure to urban environment | Adults >25 years | Cross-sectional | Field research | NA | 1,726 |
| Van de Poel et al. 2007 | 47 developing countries | Children's health | Urban–rural differentials | Children <5 years | Cross-sectional | Demographic and Health Survey | 1994–2005 | 579–30,594 |
| Van de Poel et al. 2009 | Eight provinces in eastern China | Overweight and hypertension | Degree of urbanicity | Adults | Longitudinal | China Nutrition and Health Surveys | 1991–2004 | 6,197 –6,484 |
| Vorster et al. 2007 | North West Province of South Africa | Coronary heart disease risk factors | Socio-economic status during urbanization | Healthy adults >15 years | Cross-sectional | Field research | 1996–1998 | 1,854 |
| White et al. 2008 | Coastal Ghana | Fertility | Urbanization from 1997 to 2001 | Women 15–49 years | Cross-sectional | Population and Environment Survey | 2002 | 1,436 |
Communicable Diseases
One study assessed the prevalence of communicable diseases in relation to an urbanizing environment. Fobil et al. (2011) investigated mortalities from infectious diseases in spatially different neighbourhoods of a rapidly urbanizing city in Ghana. Data on neighbourhood environment quality were extracted from the census database of 2000. Data on the causes of death between 1998 and 2002 were obtained from the Vital Registration System in Ghana. A total of 1,292 deaths due to malaria and 1,001 deaths due to diarrhea were considered. Based on a principal component analysis of 65 environmental variables, the urban environment was classified as extremely, moderately or least deteriorated, representing worst, somewhat worse and good environmental conditions, respectively. Relative mortalities were evaluated using the least deteriorated zone as a reference. Malaria mortality frequently varied significantly with the urban environment for four assessed subcomponents of environmental quality; namely per capita waste generation, water supply and sanitation, hygiene facilities and housing conditions (p ≤ .061). Diarrhea mortality varied significantly with the urban environment for two of its four assessed subcomponents (p ≤ .036). The authors interpreted these findings as evidence for differences in malaria mortality across differing urban environment conditions.
Non-communicable Diseases
Coronary heart disease (CHD) stands out among the NCDs due to its high mortality rate (UN 2007). Five studies evaluated the association between urbanization and the CHD risk factors hypertension, obesity and diabetes (Tables 2a–c).
| Table 2a. Hypertension | ||||||||
| Study | Subgroup | N | Prevalence of hypertension (%) | OR and model | ||||
| 1 | 2 | |||||||
| Men | Women | Men | Women | Men | Women | |||
| Allender et al. 2011a | Low urbanicity | 1590 | 63.2 | 56.3 | 1 | 1 | 1 | 1 |
| Medium urbanicity | 1561 | 70.8 | 60.3 | 1.41 (1.11–1.79) | 1.18 (0.99–1.41) | 1.30 (1.02–1.66) | 1.06 (0.88–1.29) | |
| High urbanicity | 1334 | 67.1 | 57.9 | 1.19 (0.93–1.52) | 1.07 (0.88–1.29) | 1.05 (0.80–1.36) | 0.99 (0.81–1.22) | |
| Niakara et al. 2007b | Parceled-out areas | NA | 42.8 | 1 | ||||
| Non-parceled-out areas | 37.2 | 1.15 (0.99–1.34) | ||||||
| Sobngwi et al. 2004c | No EU | NA | 1 | 1 | ||||
| Residence urban | 2.46 (1.63–3.7) | 1.64 (1.09–2.47) | ||||||
| MN systolic | MN diastolic | |||||||
| Rural dwellers ≤2 years EU | 851 | 27.0 | 18.7 | 126 (21) | 120 (21) | 81 (15) | 77 (13) | |
| Rural dwellers >2 years EU | 234 | 123 (20) | 117 (17) | 81 (13) | 77 (11) | |||
| Urban dwellers ≤2 years EU | 29 | 42.1 | 25.1 | 130 (17) | 149 (28) | 81 (7) | 89 (14) | |
| Urban dwellers >2 years EU | 612 | 136 (23) | 125 (19) | 87 (13) | 80 (13) | |||
| Van de Poel et al. 2009d | Coefficient | Proportionate contribution | ||||||
| Top third 2004 | NA | 0.066 | 0.714 | |||||
| Top third 1991 | 0.026 | 0.198 | ||||||
| Vorster et al. 2007e | MN systolic | MN diastolic | ||||||
| Deep rural | 432 | 125 (122–127)zy | 126 (123–128)zyxs | 75 (74–77)zy | 77.1 (75–78)zyx | |||
| Farm workers | 239 | 125 (121–127)xw | 128 (124–131)wvu | 76 (73–78)x | 77 (75–79)w | |||
| Squatter camps | 272 | 131 (128–134)zxv | 130 (127–133)zwt | 80 (76–82)zx | 81 (79–83)zv | |||
| Urban | 472 | 128 (126–131)ywu | 130 (127–133)yvsr | 77 (76–79) | 81 (79–82)yu | |||
| Upper urban | 146 | 122 (117–126)vu | 117 (112–121)xutr | 79 (76–82)y | 73 (70–75)xwvu | |||
| Note: SD or 95% CI in parentheses. | ||||||||
| CI = confidence interval, EU = exposure to urban environment, MN = mean, NA = not available, OR = odds ratio, and SD = standard deviation. | ||||||||
| a Hypertension is defined as blood pressure >120 mmHg systolic or >80 mmHg diastolic. Model 1 is without adjustment. Model 2 adjusted for age and income. | ||||||||
| b Hypertension is defined as blood pressure ≥140 mmHG systolic or ≥90 mmHg diastolic for at least one arm, or use of hypertensive treatment. Prevalence is adjusted for age and gender. | ||||||||
| c Hypertension is defined as blood pressure ≥140 mmHG systolic or ≥90 mmHg diastolic. Model adjusted for age. Lifetime EU, socioprofessional category, alcohol intake, smoking status, and physical activity were not independently associated with hypertension. Age-adjusted four group comparison indicates difference of means for men (p < .00) and for women (p < .00). Age- and gender-adjusted four group comparison indicates difference of means for men and women jointly (p < .00). | ||||||||
| d Hypertension is defined as mean blood pressure ≥140 mmHG systolic or ≥90 mmHg diastolic after three measurements, or use of hypertensive treatment. Coefficient is from a linear probability model. Proportionate contribution is the contribution of the covariate to urbanicity-related inequality in hypertension relative to the concentration index for the respective risk factor. The prevalence of hypertension is 12%, 14%, 16%, 21% and 25%, respectively, in the least to most urban quintiles of an urbanicity index. Top third is significantly associated with urbanicity-related inequalities in hypertension in 2004 (p ≤ .1) and 1991 (p ≤ .01). | ||||||||
| e Means for each sex with the same symbol differ significantly (p ≤ .05). | ||||||||
| Table 2b. Overweight | ||||||||
| Study | Subgroup | N | Prevalence of overweight (%) | OR and model | ||||
| 1 | 2 | |||||||
| Men | Women | Men | Women | Men | Women | |||
| Allender et al. 2011a | Low urbanicity | 1590 | 19.6 | 30.7 | 1 | 1 | 1 | 1 |
| Medium urbanicity | 1561 | 27.7 | 35.7 | 1.56 (1.2–2.04) | 1.25 (1.04–1.52) | 1.42 (1.08–1.86) | 1.12 (0.92–1.37) | |
| High urbanicity | 1334 | 37.5 | 56.4 | 2.45 (1.88 3.2) | 2.92 (2.41–3.55) | 1.80 (1.41–2.48) | 2.47 (2.02–3.01) | |
| Niakara et al. 2007b | Parceled-out areas | 1072 | 39.6 | NA | ||||
| Non-parceled-out areas | 972 | 25.7 | ||||||
| Sobngwi et al. 2004c | No EU | NA | 9 | 17 | 1 | 1 | ||
| EU ≤10 years | 9 | 32 | 0.81 (0.36–1.84) | NS | ||||
| EU >10 years | 40 | 60 | 2.33 (1.00–4.99) | |||||
| Residence urban | 2.30 (1.09–4.87) | 5.56 (3.6–8.61) | ||||||
| Mean BMI | ||||||||
| Rural dwellers ≤2 years EU | 851 | 21.3 (2.8) | 22.0 (3.6) | |||||
| Rural dwellers >2 years EU | 234 | 21.6 (3.0) | 23.6 (3.9) | |||||
| Urban dwellers ≤2 years EU | 29 | 21.1 (2.2) | 25.8 (5.5) | |||||
| Urban dwellers >2 years EU | 612 | 24.7 (4.1) | 27.0 (5.2) | |||||
| Van de Poel et al. 2009d | Coefficient | Proportionate contribution | ||||||
| Top third 2004 | NA | 0.049 | 0.495 | |||||
| Top third 1991 | 0.079 | 0.489 | ||||||
| Vorster et al. 2007e | MN BMI | |||||||
| Deep rural | 432 | 20.9 (20.3–21.4)z | 25.8 (24.9–26.6)z | |||||
| Farm workers | 239 | 20.5 (19.8–21.3)y | 26.3 (25.1–27.4)y | |||||
| Squatter camps | 272 | 20.2 (19.6–20.9)xv | 26.5 (25.4–27.5)x | |||||
| Urban | 472 | 21.3 (20.6–21.8)cw | 28.2 (27.4–29.0)zyx | |||||
| Upper urban | 146 | 22.7 (21.8–23.7)zywv | 27.3 (25.9–28.7) | |||||
| Note: SD or 95% CI in parentheses. | ||||||||
| BMI = body mass index, CI = confidence interval, EU = exposure to urban environment, MN = mean, NA = not available, OR = odds ratio, and SD = standard deviation. | ||||||||
| a Overweight is defined as BMI >23 kg/m2. Model 1 is without adjustment. Model 2 adjusted for age and income. The female ORs 1.25, 1.12 and 2.47 were extracted from the study assuming they were mistakenly listed as the ORs for low physical activity in the original tabulation. The original article interpreted on of these values as an OR for increased BMI. | ||||||||
| b Overweight is defined as BMI >25kg/m2. Unadjusted prevalence differs between areas (p < .00). | ||||||||
| c Overweight is defined as BMI ≥25kg/m2. Prevalence data is extracted from a figure in the original article and may be imprecise. OR model adjusted for age and physical activity. Socioprofessional category, alcohol intake, and smoking status were not independently associated with overweight. Age-adjusted four group comparison indicates difference of means for men (p = .04) and women (p = .06). Age- and gender-adjusted four group comparison indicates difference of means for men and women jointly (p = .00) | ||||||||
| d Overweight is defined as BMI >25kg/m2. Coefficient is from a linear probability model. Proportionate contribution is the contribution of the covariate to urbanicity-related inequality in overweight relative to the concentration index for the respective risk factor. The prevalence of overweight is 10%, 12%, 17%, 25% and 26%, respectively, in the least to most urban quintiles of an urbanicity index. Top third is significantly associated with urbanicity-related inequalities in overweight in 2004 (p ≤ .01) and 1991 (p ≤ .01). | ||||||||
| e Means for each sex with the same symbol differ significantly (p ≤ .05). | ||||||||
| Table 2c. Diabetes and fasting serum glucose levels | ||||||||
| Study | Subgroup | N | Prevalence of diabetes (%) | OR and model | ||||
| 1 | 2 | |||||||
| Men | Women | Men | Women | Men | Women | |||
| Allender et al. 2011a | Low urbanicity | 1590 | 7.4 | 8.8 | 1 | 1 | 1 | 1 |
| Medium urbanicity | 1561 | 10.8 | 12.1 | 1.51 (1.02–2.23) | 1.43 (1.06–1.92) | 1.30 (0.86–1.98) | 1.27 (0.93–1.74) | |
| High urbanicity | 1334 | 16.3 | 16.7 | 2.44 (1.66 3.57) | 2.1 (1.58–2.80) | 2.05 (1.35–3.11) | 2.14 (1.58–2.91) | |
| Sobngwi et al. 2004b | No EU | NA | 10 | 8 | NS | 1 | ||
| EU ≤10 years | 13 | 9 | 1.40 (0.68–2.87) | |||||
| EU >10 years | 17 | 16 | 2.73 (1.69–4.39) | |||||
| MN fasting glucose level | ||||||||
| Rural dwellers ≤2 years EU | 851 | 12.0 | 7.7 | 4.7 (1.0) | 4.6 (0.7) | |||
| Rural dwellers >2 years EU | 234 | 4.9 (1.9) | 4.7 (1.1) | |||||
| Urban dwellers ≤2 years EU | 29 | 15.1 | 15.6 | 6.8 (6.0) | 5.0 (0.7) | |||
| Urban dwellers >2 years EU | 612 | 5.1 (1.8) | 5.0 (0.9) | |||||
| Vorster et al. 2007d | Deep rural | 432 | 5.0 (4.8–5.1)z | 4.9 (4.7–5.1)z | ||||
| Farm workers | 239 | 4.7 (4.5–5.0)y | 4.7 (4.5–5.0)y | |||||
| Squatter camps | 272 | 4.9 (4.7–5.1)x | 5.1 (4.9–5.4)x | |||||
| Urban | 472 | 4.9 (4.7–5.1)w | 4.7 (4.5–4.9)w | |||||
| Upper urban | 146 | 4.2 (3.8–4.5)zyxw | 4.1 (3.8–4.5)zyxw | |||||
| Note: SD or 95% CI in parentheses. | ||||||||
| CI = confidence interval, EU = exposure to urban environment, MN = mean, NA = not available, OR = odds ratio, OGGT = oral glucose tolerance test, and SD = standard deviation. | ||||||||
| a Diabetes is defined as fasting plasma glucose ≥7.0 mmol/l or 2h post-OGTT ≥11.1 mmol/l. Model 1 is without adjustment. Model 2 adjusted for age and income. | ||||||||
| b Diabetes or impaired fasting glycaemia, i.e., fasting blood glucose ≥5.6 mmol/l, or use of hypoglycemic treatment. Prevalence data is extracted from a figure in the original article and may be imprecise. Model adjusted for age. Urban residence, socioprofessional category, alcohol intake, smoking status, and physical activity were not independently associated with impaired fasting glycaemia or diabetes. Age-adjusted four group comparison indicates difference of means for men (p = .01) and women (p = .01). Age- and gender-adjusted four group comparison indicates difference of means for men and women jointly (p = .00) | ||||||||
| c Study measured fasting glucose in the serum. Means for each sex with the same symbol differ significantly (p ≤ .05). | ||||||||
Vorster et al. (2007) looked at newly assembled data from the Transition and Health during Urbanization of South Africans (THUSA) study. The study was conducted from 1996 to 1998 to examine the influence of urbanization on CHD risk factors of 1,854 apparently healthy adults in South Africa. Subjects were arranged into five levels of urbanization based on their place of residence and occupation. The five levels were deep rural, farm workers, informal settlements, urban and upper urban. Risk factors were evaluated through using questionnaires, measuring blood pressure, calculating body mass index (BMI) and analyzing blood. Mean risk factors of men and women were calculated separately. There were three main observations comparing blood pressure: Firstly, in both men and women there were no significant differences in the means of systolic and diastolic blood pressure among deep rural dwellers and farm workers. Secondly, informal settlement dwellers had the highest means of all groups in both systolic and diastolic blood pressure (p ≤ .05). Mean blood pressure in men was significantly lower for deep rural dwellers and farm workers. These means in women were significantly lower in upper urban dwellers and the deep rural group. Thirdly, upper urban men and women had the lowest systolic blood pressure, a finding that differed significantly from the means of all other groups, except for male rural dwellers and farm workers (p ≤ .05). Women of the upper urban group also had the lowest mean diastolic blood pressure compared with all other groups (p ≤ .05). Mean diastolic blood pressure of upper urban men was significantly higher than that of deep rural men (p ≤ .05), but it did not differ significantly compared with all other groups. The highest mean BMI was found among urban women and upper urban men and differed significantly from all other groups (p ≤ .05). The authors pointed out that, on average, urban groups were younger than rural groups. Therefore, they suggested that a higher mean BMI among urban groups was unlikely to be connected with increased risk due to age. Mean fasting serum glucose levels in both men and women were significantly lower among upper urban dwellers compared with all other levels of urbanization (p ≤ .05). No significant difference of mean serum glucose levels was observed within the other groups.
Sobngwi et al. (2004) examined the relationship between exposure to an urban environment (EU) and the prevalence of CHD risk factors. The factors studied were overweight, elevated fasting blood glucose and hypertension, as well as lifestyle aspects, such as sparse physical activity, smoking and alcohol intake. The EU was measured in total number of years or percentage of lifetime spent in urban areas. Cities with more than 100,000 inhabitants were classified as urban. The study sample included 1,726 randomly selected adults older than 25 years who were recruited from a rural and an urban area in Cameroon. The sample was divided into four subgroups: rural and urban dwellers with either less or more than two years of EU. The authors observed a higher prevalence of hypertension and diabetes in urban men and women. A longer lifetime EU was associated with significantly higher BMI and fasting blood glucose levels (p ≤ .00). Residing in an urban area was associated with higher odds of hypertension and higher odds of a BMI >25 kg/m2. Urban men were 2.46 (95% CI: 1.63–3.7) and urban women were 1.64 (95% CI: 1.09–2.47) times as likely to suffer from hypertension. Urban men had 2.3 (95% CI: 1.09–4.87) times the risk and urban women had 5.56 (95% CI: 3.6–8.61) times the risk to have a BMI >25 kg/m2.
Allender et al. (2011) investigated the relationship between urbanization and chronic diseases based on data from the cross-sectional Sri Lanka Diabetes and Cardiovascular Study (SLDCS) conducted from 2007 to 2008. The study population consisted of 4,485 subjects older than 18 years who were randomly recruited from seven out of nine provinces in Sri Lanka. The authors developed a multi-component scale that included population size and density, physical environment and infrastructure characteristics, as well as other items associated with an urban environment. The tertiles of the scale were used to divide the sample into three categories of urbanicity. The highest prevalence of overweight and diabetes mellitus were each among male subjects in the high urban category. The prevalence of hypertension was highest in the medium urbanicity group. In comparison with the low urbanicity category, men in the medium and high urbanicity categories had significantly higher odds of a BMI >23 kg/m2 (OR = 1.80, 95% CI: 1.41–2.48) and diabetes mellitus (OR = 2.05, 95% CI: 1.35–3.11), after adjusting for age and income differences. The highest prevalence of overweight and highest prevalence of diabetes mellitus for women also occurred in the high urbanicity category. By contrast, hypertension was most prevalent among women in the medium urbanicity category. After controlling for age and income differences, the women in the high and medium urbanicity categories had more than doubled their odds of a BMI >23 kg/m2 (OR = 2.47, 95% CI: 2.02–3.01) and diabetes mellitus (OR = 2.14, 95% CI: 1.58–2.91) compared to women in the low urbanicity category.
Niakara et al. (2007) examined the association between intra-urban disparities and the frequency of hypertension during rapid urbanization in Ouagadougou, Burkina Faso. A total of 2,087 inhabitants over 35 years old were sampled in a cross-sectional study in 2004. According to their type of housing, subjects were arranged in the subgroups of parcelled-out area and non-parcelled-out area. In parcelled-out areas, local authorities provided sanitation, electricity, infrastructure and access to public services, while non-parcelled-out areas were characterized by uncontrolled growth. Controlling for age and gender, the prevalence of hypertension was 42.8% in parcelled-out and 37.2% in non-parcelled-out areas, but the difference was not significant (OR = 1.15, 95% CI: 0.99–1.34). Risk factors for hypertension differed significantly between the subgroups (p ≤ .001). In non-parcelled-out areas, 25.7% of the sample had a BMI >25 kg/m2, compared to 39.6% in parcelled-out areas (p ≤ .001).
Van de Poel et al. (2009) examined changes in the prevalence of overweight and of hypertension in China from 1991 to 2004 and their association with the degree of urbanicity. Data were extracted from the longitudinal China Health and Nutrition Survey (CHNS). The authors evaluated eight provinces with a sample size of 6,484 subjects in 1991 and 6,197 subjects in 2004. They created an index of urbanicity using factor analysis with a set of community-level characteristics. Testing for robustness, they considered the index a reliable indicator of the degree of urbanicity. In 1991 and in 2004, the prevalence of BMI >25 kg/m2 and hypertension were each higher in the top third most urbanized communities (p ≤ .1). Urban environment characteristics accounted for 50% of the disparity in increased weight. While in 1991 these characteristics accounted for 20% of the urbanicity-related differences in hypertension, in 2004 they accounted for 62%. The rural-urban differences in the prevalence of overweight and in the prevalence of hypertension became smaller over time.
Child Health
Three studies of child health assessed under-five mortality and nutritional status (Table 3).
| Table 3. Child health indicators | |||||||
| Study | Subgroup | Health indicator | N | Prevalence (%) | OR and model | ||
| UADI | Child level | Mother level | |||||
| Antai and Moradi 2010a | Class I | Under-five mortality | 338 | 6 | 1 | 1 | 1 |
| Class II | 856 | 7 | 1.32 (1.19–1.54) | 1.32 (0.19–1.55) | 1.72 (0.91–3.29) | ||
| Class III | 490 | 13 | 1.39 (1.26–1.56) | 1.38 (0.26–1.56) | 1.78 (1.17–2.70) | ||
| Class IV | 43 | 8 | 1.76 (0.52–1.81) | 1.76 (0.52–2.11) | 2.03 (1.04–3.97) | ||
| Class V | 391 | 17 | 1.51 (0.65–1.72) | 1.49 (0.14–1.65) | 2.14 (1.11–4.12) | ||
| Firestone et al. 2011b | 1 | 2 | 3 | ||||
| Rural | Short stature | NA | 19.85 | 1 | 1 | Not significant | |
| Urban | 0.63 (0.42–0.94) | 0.92 (0.59–1.43) | |||||
| Rural | Underweight | 27.79 | 1 | 1 | Not significant | ||
| Urban | 0.64 (0.50–0.82) | 0.74 (0.55–1.00) | |||||
| Rural | Obesity | 8.26 | 1 | 1 | 1 | ||
| Urban | 2.66 (1.91–3.72) | 1.73 (1.21–2.48) | 1.03 (0.59–1.80) | ||||
| Van de Poel et al. 2007c | RR range | ||||||
| Urban | Under-five stunting | 47 | 0.09–0.47 (0.28) | 1 | |||
| Rural | 0.14–0.61 (0.43) | 1.00–2.60 (1.40) | |||||
| Urban | Under-five mortality | 47 | 0.04–0.20 (0.10) | 1 | |||
| Rural | 0.03–0.37 (0.14) | 0.72–1.80 (1.36) | |||||
| Note: Median or 95% CI in parentheses. | |||||||
| CI = confidence interval, UADI = urban area disadvantage index, NA = not available, OR = odds ratio, and RR = relative risk. | |||||||
| a Class I is assigned to the least disadvantaged, Class V to the most disadvantaged urban areas. Models accounted for community and mother-level random effects. Prevalence data is extracted from a figure in the original article and may be imprecise. The UADI model is without adjustment. The child-level model adjusted for child's sex, birth order and birth interval. The mother-level model adjusted in addition for mother's marital status, age, education, occupation, and a wealth index. | |||||||
| b Short stature (<2 SD height-for-age), underweight (<5th percentile BMI-for-age), obese (≥95th percentile BMI-for-age). Model 1 is without adjustment. Model 2 adjusted for household wealth, maternal education, household head occupation, child gender and age, maternal height or BMI, household size and ethnicity. Model 3 adjusted in addition for the community level variables wealth concentration, TV coverage and improved sanitation coverage that were found previously to be significant. | |||||||
| c Estimates of under-five stunting are statistically significant in 43 of 47 countries (p ≤ .1); estimates of the under-five mortality are statistically significant in 32 of 47 countries (p ≤ .1) | |||||||
Van de Poel et al. (2007) compared the under-five mortality and under-five stunting in urban and rural areas. A children′s height was defined as stunted if it fell two or more standard deviations below the median height of healthy counterparts. Data on child health were extracted from Demographic and Health Surveys (DHS) conducted between 1994 and 2005 in 47 developing countries. The authors used Poisson regression to estimate rural-urban relative risks. The median rural-urban relative risk ratio of all countries examined was 1.36 (0.72–1.80) for under-five mortality and 1.4 (1.00–2.60) for under-five stunting. There were significant rural-urban differences in under-five mortality and in stunting in 32 and 43 countries, respectively (p ≤ .1). The relative rural-urban risk of stunting and under-five mortality fell on average by 53% and 59% after adjusting for household wealth. Further adjusting for sociodemographic differences reduced the risk ratios by another 22% and 25%. Rural-urban disparities in stunting remained significant in 18 countries after controlling for household wealth and other covariates; the median risk ratio of stunting was reduced from 1.40 to 1.09. The median risk ratio of under-five mortality was reduced from 1.36 to 1.07 after controlling for all covariates the study measured, and the rural-urban under-five mortality disparities remained significant in 17 countries.
Firestone et al. (2011) examined short stature, undernutrition and the prevalence of obesity in 4,610 children living in Kanchanaburi, Thailand. Data were extracted from the Kanchanaburi Demographic Surveillance System (KDSS) in 2004. The authors described an urban advantage in the unadjusted odds of short stature (OR = 0.63, 95% CI: 0.42–0.94) and underweight (OR = 0.64, 95% CI: 0.50–0.82). After adjusting for household level differences in the education, height and BMI of the mother, household size and wealth, occupation of the household head, child's age and ethnicity, the urban area advantage in the odds of short stature and underweight was diminished and no longer significant. Household wealth was significantly and negatively associated with the odds of short stature and underweight. The authors concluded that household poverty accounted for child under-nutrition in this sample rather than community characteristics. After controlling for household level covariates, residence in urban areas was associated with greater odds of obesity (OR = 1.73, 95% CI: 1.21–2.48). Community wealth concentration, TV coverage and improved sanitation coverage could explain this rural-urban difference in obesity (OR = 1.03, 95% CI: 0.59–1.80).
Antai and Moradi (2010) measured the association between under-five mortality and a poor living standard in urban areas of Nigeria. They aimed to assess the influence of rapid urbanization on child health. Urban population pattern data were taken from the United Nations Department of Economics and Social Affairs. Population characteristics and child deaths were taken from the Demographic and Health Survey (DHS) in 2003. The study included 2,118 subjects. Urban areas were classified into five groups, using an urban area disadvantage index that was based on indicators of socio-economic disadvantage. Class I represented the least disadvantaged areas, whereas Class V stood for the most disadvantaged. Odds ratios were estimated in comparison with Class I. Covariates included were individual-level factors such as birth order, sex of child, occupation, education, age and marital status of mother, and a wealth index. The authors found significantly higher under-five mortality in the three most disadvantaged urban areas. Children in the most disadvantaged urban area faced more than twice the risk of dying below the age of five than did children in the least disadvantaged urban area (OR = 2.14, 95% CI: 1.11–4.12).
Fertility
White et al. (2008) evaluated the association between urbanization and fertility rates, conducting an event-history analysis of 1,436 women based on the 2002 Ghana Population and Environment Survey. Adjusting for age, the study reported, on average, a 24% lower odds of giving birth in any given year for women with urban residence (OR = 0.76, p ≤ .00). The effect size and its significance varied by the number of times a women had given birth. For all women and nulliparae, the negative association between urbanization and fertility could not be attributed to differences in age, education, the union or employment status of the mother. Net of these personal traits, urban women exhibited fertility odds that were, on average, 11% lower than those of rural women giving birth repeatedly and for the first time, respectively (p < .05).
Life Expectancy
Bergh and Nilsson (2010) investigated the relationship between life expectancy and globalization within a sample of 92 countries. Urbanization was examined as a covariate. The study found that globalization, urbanization, nutrition, education, public health measures and income were all positively related to life expectancy if significant (p ≤ .1). This result was reproduced for a subsample of less developed countries. Urbanization was positively but not significantly associated with life expectancy.
Discussion
Our aim was to give an overview of studies that investigated health in relation to aspects of urbanization across developing countries. We approached this broad research question by deciding on WHO health indicators to report on in our review. These were either connected to the 10 leading causes of death in developing countries or reflected a population's health status in general.
Summary of Main Results
Communicable and Non-communicable Disease
Malaria mortality appeared more strongly associated with urban environment characteristics than infectious diarrhea. An urban area disadvantage was observed for extremely deteriorated neighbourhoods. No clear pattern in the variation of the mortality risks due to environmental differences was found. Neither an overall effect of urbanization on the mortality from these diseases nor the influence of urbanization over time was assessed (Fobil et al. 2011).
The findings on NCDs varied across the studies examined. Studies either reported the values of blood pressure, BMI and fasting glucose levels, or their prevalence as CHD risk factors defined by cut-off values. Hypertension, overweight and diabetes were more prevalent under higher urbanization levels (Allender et al. 2011; Niakara et al. 2007; Sobngwi et al. 2004; Van de Poel et al. 2009). Both urban residence and lifetime exposure to urban environment were associated with greater odds of hypertension, diabetes and overweight (Sobngwi et al. 2004). The highest odds for hypertension were observed in the medium urbanicity group, whereas the highest odds of diabetes and overweight were found in the high urbanicity group (Allender et al. 2011). In another study, BMI but neither blood pressure nor fasting glucose increased, on average, with rising urbanization levels (Vorster et al. 2007). Several authors suggested that lifestyle changes occurring with urbanization, such as reduced physical activity or increased fat or protein intake, explain in part the urban concentration of NCD risk factors.
Child Health
Studies on child health reported lower under-five mortality and undernutrition for urban areas than for rural areas (Firestone et al. 2011; Van de Poel et al. 2007). Socioeconomic disadvantages on the household and community level were associated with under-five mortality and accounted for most of the rural-urban disparities in child health (Antai and Moradi 2010; Van de Poel et al. 2007). A higher prevalence of overweight in urban areas accompanied the positive effect of urban residence on undernutrition (Firestone et al. 2011).
Fertility and Life Expectancy
In developing countries, perinatal conditions have been considered to be among the leading contributors to the total burden of disease (Murray and Lopez 1997). In combination with other parameters, fertility rate is an important indicator for reproductive health and development. Urban residence was associated with lower fertility rates in Ghana (White et al. 2008).
Life expectancy is the most widely used indicator to measure a population's health status (OECD 2013). It takes into account length of life but not quality of life. Urbanization was not significantly associated with a higher life expectancy. In the same study, aspects that can be associated with urbanization, such as nutritional intake and the number of physicians, correlated positively with life expectancy (Bergh and Nilsson 2010).
Quality of Evidence
Nine studies reviewed were based on cross-sectional data, and two on longitudinal data. All controlled for some individual characteristics and some also for community-level or infrastructure characteristics. Suggestive associations between urbanization and health were described, but the evidence level for causal inference on the impact of urbanization on health is low.
Limitations and Ways Forward
The comparability of the studies reviewed and their findings is limited. The studies examined different countries, populations and time periods using different methods and study designs. The definitions of urbanization and diseases varied and rural-urban or intra-urban comparisons were investigated. Controlled trials were not among the results of our database search but are conceivable in future research within planned urbanization projects.
Additionally, weak health information systems may not be able to provide reliable disaggregated health statistics on a rural-urban or intra-urban basis, but aggregated data can mask rural-urban or intra-urban health differences if health determinants vary within the unit of data collection (Moore et al. 2003; WHO 2010). Collecting accessible and relevant data has consequently been considered necessary to better describe and quantify the relationships between health outcomes and the urban environment (Antai and Moradi 2010; Khan et al. 2013).
Conclusion
Implications for Research
Several health outcomes correlate with urbanization processes in developing countries. Urbanization has been associated with better and worse health status. Prospective research studies and continuing collection of reliable data are needed to assess the causal relationship between urbanization and health with more confidence. To improve our understanding of the different pathways through which urbanization affects health, the relationships between specific and general indicators of both need to be studied. In addition, future research should aim at assessing the overall impact of urbanization on the disease burden of developing countries to guide health policy and public health practitioners.
Implications for Practice
Measures that improve health in urban areas might be distinctively different from those in rural areas (Van de Poel et al. 2007). Urbanization can be expected to shift the disease pattern. Despite likely health improvements, urbanization also imposes new health problems on developing countries. Therefore, their progressing urbanization should be accompanied by an informed health policy that is able to anticipate and screen for health changes associated with urbanization.
Author Contributions
SE and SK jointly conceived the study. SE designed the study with advice from SK and acquired the data. SE drafted and SK revised the manuscript. Both authors analyzed and interpreted data.
About the Author(s)
Sophie Eckert, Institute for Social Medicine, Epidemiology and Health Economics, Charité University Medical Center, Berlin, Germany
Stefan Kohler, PhD, Institute for Social Medicine, Epidemiology and Health Economics, Charité University Medical Center, Berlin, Germany
Correspondence may be directed to: Stefan Kohler, Institute for Social Medicine, Epidemiology and Health Economics, Charité University Medical Center, Luisenstraße 57, 10117 Berlin, Germany, e-mail: Stefan.Kohler@charite.de.
References
Alirol, E., L. Getaz, B. Stoll, F. Chappuis and L. Loutan. 2011. "Urbanisation and Infectious Diseases in a Globalised World." The Lancet Infectious Diseases 11(2): 131–41. doi:10.1016/S1473-3099(10)70223-1.
Allender, S., K. Wickramasinghe, M. Goldacre, D. Matthews and P. Katulanda. 2011. "Quantifying Urbanization as a Risk Factor for Noncommunicable Disease." Journal of Urban Health: Bulletin of the New York Academy of Medicine 88(5): 906–18. doi:10.1007/s11524-011-9586-1.
Antai, D. and T. Moradi. 2010. "Urban Area Disadvantage and under-5 Mortality in Nigeria: The Effect of Rapid Urbanization." Environmental Health Perspectives 118(6): 877–83. doi:10.1289/ehp.0901306.
Bergh, A. and T. Nilsson. 2010. "Good for Living? On the Relationship between Globalization and Life Expectancy." World Development 38(9): 1191–1203. doi:10.1016/j.worlddev.2010.02.020.
Bhugra, D. and A. Mastrogianni. 2004. "Globalisation and Mental Disorders. Overview with Relation to Depression." The British Journal of Psychiatry 184(1): 10–20. doi: 10.1192/bjp.184.1.10
Bygbjerg, I.C. 2012. "Double Burden of Noncommunicable and Infectious Diseases in Developing Countries." Science (New York, N.Y.) 337(6101): 1499–501. doi:10.1126/science.1223466.
Chinn, M.D. and R.W. Fairlie. 2006. "The Determinants of the Global Digital Divide: A Cross-Country Analysis of Computer and Internet Penetration." Oxford Economic Papers 59(1): 16–44. doi:10.1093/oep/gpl024.
Chinn, M.D. and R.W. Fairlie. 2010. "ICT Use in the Developing World: An Analysis of Differences in Computer and Internet Penetration." Review of International Economics 18(1): 153–167. doi:10.1111/j.1467-9396.2009.00861.x.
Dye, C. 2008. "Health and Urban Living." Science (New York, N.Y.) 319(5864): 766–9. doi:10.1126/science.1150198.
Firestone, R., S. Punpuing, K.E. Peterson, D. Acevedo-Garcia and S.L. Gortmaker. 2011. "Child Overweight and Undernutrition in Thailand: Is There an Urban Effect?" Social Science and Medicine (1982) 72(9): 1420–1428. doi:10.1016/j.socscimed.2011.03.003.
Fobil, J.N., A. Kraemer, C.G. Meyer and J. May. 2011. "Neighborhood Urban Environmental Quality Conditions Are Likely to Drive Malaria and Diarrhea Mortality in Accra, Ghana." Journal of Environmental and Public Health. Epub 21 Jun 2011. doi:10.1155/2011/484010.
Godfrey, R. and M. Julien. 2005. "Urbanisation and Health." Clinical Medicine 5(2): 137–41. doi:10.7861/clinmedicine.5-2-137.
Harpham, T. 2009. "Urban Health in Developing Countries: What Do We Know and Where Do We Go?" Health and Place 15(1): 107–16. doi:10.1016/j.healthplace.2008.03.004.
Khan, F.S., I. Lotia-Farrukh, A.J. Khan, S.T. Siddiqui, S.Z. Sajun, A.A. Malik et al. 2013. "The Burden of Non-communicable Disease in Transition Communities in an Asian Megacity: Baseline Findings from a Cohort Study in Karachi, Pakistan." PloS One 8(2): e56008. doi:10.1371/journal.pone.0056008.
Kohler, S. 2013. "Can Internet Access Growth Help Reduce the Global Burden of Noncommunicable Diseases?" Online Journal of Public Health Informatics 5(2): 221. doi:10.5210/ojphi.v5i2.4667.
Marshall, S.J. 2004. "Developing Countries Face Double Burden of Disease." Bulletin of the World Health Organization 82(7): 556.
McDade, T.W. and L.S. Adair. 2001. "Defining the 'Urban' in Urbanization and Health: A Factor Analysis Approach." Social Science and Medicine 53(1): 55–70. doi:10.1016/S0277-9536(00)00313-0.
Montgomery, M.R., R. Stren, B. Cohen and H.E. Reed, eds. 2003. "Cities Transformed: Demographic Change and Its Implications in the Developing World." Washington, DC: National Academies Press.
Moore, M., P. Gould and B.S. Keary. 2003. "Global Urbanization and Impact on Health." International Journal of Hygiene and Environmental Health 206(4–5): 269–78. doi:10.1078/1438-4639-00223.
Murray, C.J. and A.D. Lopez. 1997. "Global Mortality, Disability, and the Contribution of Risk Factors: Global Burden of Disease Study." Lancet 349(9063): 1436–42. doi:10.1016/S0140-6736(96)07495-8.
Niakara, A., J. Fournet, J. Gary, M. Harang, L.V.A. Nébié and G. Salem. 2007. "Hypertension, Urbanization, Social and Spatial Disparities: A Cross-sectional Population-Based Survey in a West African Urban Environment (Ouagadougou, Burkina Faso)." Transactions of the Royal Society of Tropical Medicine and Hygiene 101(11): 1136–42. doi:10.1016/j.trstmh.2007.07.002.
OECD. 2013. Better Life Index: Health. Retrieved February 10, 2014. <http://www.oecdbetterlifeindex.org/topics/health/>.
Penkalla, A.M. and S. Kohler. "Urbanicity and Mental Health in Europe: A Systematic Review." European Journal of Mental Health forthcoming.
Sobngwi, E., J.-C. Mbanya, N.C. Unwin, R. Porcher, A.-P. Kengne, L. Fezeu et al. 2004. "Exposure over the Life Course to an Urban Environment and Its Relation with Obesity, Diabetes, and Hypertension in Rural and Urban Cameroon." International Journal of Epidemiology 33(4): 769–76. doi:10.1093/ije/dyh044.
Tatem, A.J., P.W. Gething, D.L. Smith and S.I. Hay. 2013. "Urbanization and the Global Malaria Recession." Malaria Journal 12(1): 133. doi:10.1186/1475-2875-12-133.
United Nations. 2007. State of World Population 2007: Unleashing the Potential of Urban Growth (p. 108). New York: United Nations Population Fund. Retrieved February 10, 2014. <https://www.unfpa.org/public/publications/pid/408>.
Van de Poel, E., O. O'Donnell and E. Van Doorslaer. 2007. "Are Urban Children Really Healthier? Evidence from 47 Developing Countries." Social Science and Medicine 65(10): 1986–2003. doi:10.1016/j.socscimed.2007.06.032.
Van de Poel, E., O. O'Donnell and E. Van Doorslaer. 2009. "Urbanization and the Spread of Diseases of Affluence in China." Economics and Human Biology 7(2): 200–16. doi:10.1016/j.ehb.2009.05.004.
Vorster, H.H., A. Kruger, C.S. Venter, B.M. Margetts and U.E. Macintyre. 2007. "Cardiovascular Disease Risk Factors and Socio-economic Position of Africans in Transition: The THUSA Study." Cardiovascular Journal of Africa 18(5): 282–9.
White, M.J., S. Muhidin, C. Andrzejewski, E. Tagoe, R. Knight and H. Reed. 2008. "Urbanization and Fertility: An Event-History Analysis of Coastal Ghana." Demography 45(4): 803–16. doi: 10.1353/dem.0.0035
World Health Organization. 2010. "Hidden Cities: Unmasking and Overcoming Health Inequities in Urban Settings." Geneva: World Health Organization. Retrieved February 10, 2014. <http://www.who.int/kobe_centre/publications/hidden_cities2010/en/>.
World Health Organization. 2013. Obesity and Overweight. WHO Fact Sheet No. 311. Retrieved February 10, 2014. <http://www.who.int/mediacentre/factsheets/fs311/en/>.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed