Healthcare Policy
A Cost-Effectiveness Analysis of Low Risk Deliveries: A Comparison of Midwives, Family Physicians and Obstetricians
Dylan Walters, Archna Gupta, Austin E. Nam, Jennifer Lake, Frank Martino and Peter Coyte
Abstract
Objective: To investigate the cost-effectiveness of in-hospital obstetrical care by obstetricians (OBs), family physicians (FPs) and midwives (MWs) for delivery of low-risk obstetrical patients.
Methods: Cost-effectiveness analysis from the Ministry of Health perspective using a retrospective cohort study. The time horizon was from hospital admission of a low-risk pregnant patient to the discharge of the mother and infant. Costing data included human resource, intervention and hospital case-mix costs. Interventions measured were induction or augmentation of labour with oxytocin, epidural use, forceps or vacuum delivery and caesarean section. The outcome measured was avoidance of transfer to a neonatal intensive care unit (NICU). Model results were tested using various types of sensitivity analyses.
Findings: The mean maternal age by provider groups was 29.7 for OBs, 29.8 for FPs and 31.2 for MWs – a statistically higher mean for the MW group. The MW deliveries had lower costs and better outcomes than FPs and OBs. FPs also dominated OB.s The differences in cost per delivery were small, but slightly lower in MW ($5,102) and FP ($5,116) than in OB ($5,188). Avoidance of transfer to an NICU was highest for MW at 94.0% (95% CI: 91.0–97.0), compared with 90.2% for FP (95% CI: 88.2–92.2) and 89.6% for OB (95% CI: 88.6–90.6). The cost-effectiveness of the MW group is diminished by increases in compensation, and the cost-effectiveness of the FP group is sensitive to changes in intervention rates and costs.
Conclusions: The MW strategy was the most cost-effective in this hospital setting. Given data limitations to further examine patient characteristics between groups, the overall conservative findings of this study support investments and better integration for MWs in the current system.
Introduction
Childbirth represents a significant share of total healthcare expenditures in Canada. In 2011–2012, there were over 373,000 childbirths in hospitals across the country (Canadian Institute of Health Information 2013). The majority of newborns are delivered by obstetrician/gynecologists (OBs) (69.6%), followed by family physicians/general practitioners (FPs) (14.6%), midwives (MWs) (4.3%), nurses or nurse practitioners (4.7%) and other (6.8%) (Public Health Agency of Canada 2009). Systematic reviews and cohort studies have shown that clinical effectiveness is comparable between these three groups (Birthplace in England Collaborative Group et al. 2011; Villar et al. 2001). However, a cost-effectiveness analysis (CEA) comparing the costs and outcomes of childbirths by the different providers could offer new information for healthcare decision-makers regarding the optimal management of low-risk obstetrical patients in the current fiscal climate.
Medical interventions such as epidurals, induction and augmentation of labour, assisted vaginal delivery techniques (vacuum and forceps delivery) and caesarian sections are increasingly being used during labour and delivery (Betran et al. 2007). However, prior studies have shown that the rates of medical intervention vary by provider. A retrospective chart review in Toronto, Ontario, showed that the intervention rates for artificial rupture of membranes, induction, augmentation, low forceps plus vacuum extraction, episiotomy and epidural anaesthesia were all higher in OB deliveries compared with FP (Reid et al. 1989). No difference was observed in the caesarean section or maternal and newborn outcome rates (Reid et al. 1989). A prospective cohort study in British Columbia showed that MW deliveries had lower rates of narcotic analgesia, episiotomy and artificial rupture of membranes, though no difference in adverse neonatal outcomes compared with physicians was detected (Janssen et al. 2007; Rosenblatt et al. 1997). A recent Cochrane review showed that MW patients were less likely to experience regional analgesia (epidural/spinal), and instrumental vaginal deliveries (vacuum/forceps), but there were no significant differences between groups for caesarean section or adverse neonatal outcomes (Sandall et al. 2013).
Different rates of intervention use between provider groups during labour and delivery could have cost implications where a fee-for-service payment scheme is used for physician services. Midwifery services are still in a nascent stage of development in the Canadian healthcare system. The scope of practice and payment scheme for this group varies across provinces and territories. In Ontario, MWs are remunerated for a course of care scheme instead of by fee-for-service. Despite recent investments in MWs as a low-cost provider, there are few Canadian cost-effectiveness studies on MW services and none that examine obstetrical care across OBs, FPs and MWs. Differences in intervention rates, remuneration schemes, scopes of practice and transfers of patient care from MWs or FPs to OBs present challenges when comparing the cost-effectiveness of the three provider groups or multiple sites and jurisdictions.
The objective of this study was to evaluate the cost-effectiveness of obstetrical care for low-risk women by OBs, FPs and MWs during the labour and delivery period in a hospital setting. The study used intervention rates and neonatal outcome rates (avoidance of transfer to the neonatal intensive care unit [NICU]) from a Canadian hospital. In-hospital costs were calculated from the provincial Ministry of Health perspective.
Methodology
Retrospective cohort study methods
A cost-effectiveness study was based on a retrospective cohort of low-risk deliveries from Brampton Civic Hospital (BCH) of the William Osler Health System located in the province of Ontario. BCH is a full-service community hospital with practicing privileges available to OBs, FPs and MWs. The retrospective data obtained through BCH for this study are part of the Better Outcomes Registry & Network Ontario (BORN) database, which collects information on every birth in Ontario. Research Ethics Board approval was granted in November 2013 for access to all the aggregated and anonymized BORN data specific to deliveries performed in-hospital at BCH from April 2012 to September 2013.
The exclusion criteria were based on the College of Midwives of Ontario indications for mandatory consultation and transfer of care (College of Midwives of Ontario 1999), and previous studies evaluating low-risk obstetrical care. Patients were considered high-risk and excluded from the study cohort if they met any of the following criteria: maternal pre-existing hypertension or diabetes (Janssen et al. 2007; Reid et al. 1989; Rosenblatt et al. 1997), gestational hypertension or diabetes (College of Midwives of Ontario 1999), greater than a singleton pregnancy (Janssen et al. 2007; Rosenblatt et al. 1997); previous caesarian section (Rosenblatt et al. 1997), previous stillbirth (Reid et al. 1989; Rosenblatt et al. 1997), placental abruption or placenta previa after 28 weeks' gestational age (GA) (College of Midwives of Ontario 1999), GA less than or equal to 36 weeks at the time of delivery (College of Midwives of Ontario 1999) or malpresentation of the baby at the time of the delivery (Janssen et al. 2007). Two investigators (A.G. and A.E.N.) independently applied the exclusion criteria to ensure data agreement and validity.
The retrospective cohort was stratified by the provider group under which the patient was admitted to compare intervention and neonatal outcomes rates. Maternal age, the only relevant patient-level characteristic with data available in the data set, was analyzed. Intervention variables analyzed were induction or augmentation of labour with oxytocin, epidural use, caesarean section, assisted vaginal delivery with forceps or vacuum and, finally, spontaneous vaginal delivery. These were the most common interventions with an effect on cost, and costing data readily available. Neonatal outcomes were defined by the avoidance of transfer to the NICU. As newborns admitted to the NICU are the most vulnerable and critically ill, transfers to the NICU provided a useful, albeit crude, marker to denote "healthy" versus "unhealthy" babies. Admission to NICU would capture infants who experienced other outcomes of interest such as low APGAR score at five minutes, need for resuscitation at birth or intubation (Janssen et al. 2007; Reid et al. 1989; Rosenblatt et al. 1997; Sutcliffe et al. 2012). Outcomes such as small for GA or low birth weight were not included, as they were not a direct consequence of labour and delivery, but more so of the entire pregnancy (Janssen et al. 2007; Reid et al. 1989; Sutcliffe et al. 2012; Villar et al. 2001). Maternal outcomes such as postpartum haemorrhage requiring hysterectomy and fourth-degree tears were analyzed but not included in the CEA owing to low prevalence and lack of statistically significant differences between providers. Two investigators (A.G. and A.E.N.) independently analyzed intervention and outcome rates for each provider group to ensure data agreement and validity.
All statistical analyses were conducted using SAS (version 9.4) software (SAS Institute Inc. 2013). Relative risks of interventions and neonatal outcomes in FPs and MWs were compared with OBs (the standard provider). A normal binomial distribution was assumed for all intervention and outcome variables.
Economic methods
This economic evaluation was conducted from the Ministry of Health perspective, which includes the overwhelming majority of hospital costs. The time horizon of analysis was hospital length of stay (time of admission of the pregnant patient to the time of discharge of mother and infant) to account for in-hospital decisions pertaining to care. Patient costs as well as intervention and outcome rates were attributed to the admitting provider (even for those patients transferred to OBs) to yield a conservative set of cost–outcome estimates. For example, if an FP or MW patient was transferred to an OB during the care process owing to a complication in labour, the interventions used by the OB and their costs were allocated to the admitting provider. This method was used to account for patient choice of provider regardless of subsequent transfers. TreeAge Pro (version 2015) was used to run the CEA decision tree model and sensitivity (TreeAge 2015).
Costs were obtained from two different sources. Human resource costs were micro-costed. Hospital costs were based on case costing. Human resource unit costs for interventions, labour and delivery were retrieved from the Ontario Schedule of Benefits for Physician Services (MOHLTC 2013), the Compensation Review of Midwifery (Courtyard Group 2010) and documents related to the current Association of Ontario Midwives, (AOM) lawsuit for pay equity (Durber 2013). Owing to the differences in payment methods between MWs (course of care for entire pregnancy) and fee-for-service for both groups of physicians, the cost for a MW attending delivery was calculated by allocating 48% of the total course of care fee. This was estimated by calculating a total cost of care for physicians (OBs and FPs) using the fee-for-service costs for the typical number of antepartum and postpartum visits in a healthy pregnancy and calculating the percentage of that total cost that was made up of attending delivery for the physician group (MOHLTC 2013). Time allocations for physician fees during time-dependent procedures like caesarean section (Petrou et al. 2001) and epidural maintenance (MOHLTC 2013) were based on clinical standards for the procedures.
Case costing is an accounting method that captures the full cost of specific procedures and episodes of care by calculating all direct and indirect costs. The Canadian Institute of Health Information (CIHI) maintains case-costing methodology called Case Mix Group (CMG+) (CIHI 2013). CMG+ categorizes acute care in-patients with similar clinical and resource-utilization characteristics, and is based on codes for the most responsible diagnosis and the primary procedure for each admission. It is often referred to as "patient-level costing" and is similar to the American Diagnosis-Related Groups methodology. CMG+ case costs for this study were provided directly from William Osler Health System – BCH 2012/2013 data. As there were a few BCH CMG+ case costs that were not available owing to Freedom of Information regulation – because there were fewer than five cases – data from the CIHI Patient Cost Estimator for all Ontario hospitals were used to supplement the CMG+ case costs (CIHI 2012). The CMG+ groups of interest within our study were: caesarean section with/without induction (#558–559), vaginal birth with/without anaesthetic and with/without non-major obstetrical interventions (#562–565), singleton delivery (#576) and caesarean delivery (#577). Additionally, the cost of newborn transfer to the NICU was calculated as a weighted average for all CMG+ groups indicating neonatal birth weight greater than 2,500 g with major complications (#589–599). Because the population was low-risk pregnancies, it was less likely to have a neonate <2,500 g. All unit costs and case costs were reported in 2013 Canadian dollars ($1.00 USD = $0.91 CAD) for this study (Bank of Canada 2014); therefore, no adjustment for inflation was necessary.
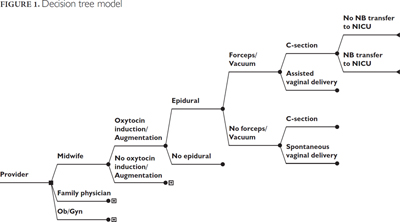
Within the variables selected for this study, a decision tree model was developed that outlined the possible combinations of human resources, interventions, method of delivery and outcomes associated with each provider group (Figure 1). The probabilities for interventions used in the model were obtained from the retrospective cohort (including oxytocin for induction and augmentation, epidural and forceps/vacuum) and method of delivery (caesarean section, spontaneous vaginal delivery and assisted vaginal delivery). Model costs were obtained from both the human resources costing and CMG+ groups described above. As the outcome of interest was defined as the avoidance of newborn transfer to the NICU, the model branches ending in a transfer to the NICU were assigned an effect equal to 0, and branches with no transfer to the NICU were assigned an effect equal to 1 (Sandall et al. 2013).
One-way sensitivity analyses were conducted for all three providers by varying case costs and probabilities at the 95% confidence intervals. Values for the sensitivity analysis of cost and probability variables were retrieved from the literature, provincial data and probability point-estimates (Aenhaim et al. 2007; CIHI 2012; Durber 2013; Janssen et al. 2007; Krikke and Bell 1989; MOHLTC 2013; Reid et al. 1989; Sandall et al. 2013). Additionally, the cost of MW attending birth was varied up to a high value equivalent to the compensation level requested by MWs in a current Ontario lawsuit (Association of Ontario Midwives [AOM] 2013). The results of the one-way sensitivity analyses of key variables for MWs are presented in an Incremental Cost-Effectiveness Ratio Tornado diagram, which demonstrated the influence of varying key costs and probabilities to high and low values from literature, provincial averages and a current labour dispute. Probabilistic sensitivity analyses (Drummond et al. 2005), using a Monte Carlo Simulation of 10,000 cases with means and standard deviations for all variables, were conducted for the MWs and FPs versus OBs. Costs were assigned a gamma distribution and probabilities were assigned a beta distribution (Briggs et al. 2001). An Incremental Cost Effectiveness Plot Report was used to determine the portion of scenarios cost-effective under $1,000 and $5,000 willingness-to-pay thresholds.
Results
Retrospective cohort study
A total of 4,693 low-risk deliveries were eligible for inclusion in this study. By provider, this included 3,601 (76.7%) births to mothers admitted by OBs, 844 (18.0%) admitted by FPs and 248 (5.3%) admitted by MWs. The mean maternal age for mothers was 29.7 for OBs (CI: 29.56, 29.88), 29.8 for FP (CI: 29.48, 30.89) and 31.2 for MW (CI: 30.72, 31.69). There was both a statistical difference in means between MW and other providers (p < 0.0001). From the overall low-risk birth cases, 15.1% (n = 708) delivered by caesarean section and 10.1% (n = 474) of newborns were transferred to the NICU. The intervention rates were reported as the following: induction with oxytocin at 12.8% (n = 601), augmentation with oxytocin at 41.7% (n = 1,959), epidural at 71.4% (n = 3,353) and forceps or vacuum delivery at 10.0% (n = 491). The comparative proportions of interventions and maternal and neonatal outcomes in the three providers are shown in Table 1.
| TABLE 1. Intervention and neonatal outcome rates in OBs/FPs/MWs and relative risk of interventions/ outcomes in FPs and MWs versus OBs | |||||
| Intervention/outcome | OB (n = 3,603) | FP (n = 845) | MW (n = 248) | FP vs. OB | MW vs. OB |
| % (95% CI) | % (95% CI) | % (95% CI) | RR (95% CI) | RR (95% CI) | |
| Induction and/or augmentation with oxytocin | 58.0 (56.4–60.0) | 48.1 (44.8–51.6) | 25.0 (19.6–33.4) | 0.83 (0.77, 0.89)* | 0.43 (0.35, 0.54)* |
| Epidural | 72.8 (71.3–74.2) | 75.1 (72.2–78.1) | 38.7 (32.7–44.8) | 1.03 (0.99, 1.08) | 0.53 (0.45, 0.62)* |
| Forceps and/or vacuum | 10.8 (9.8–11.8) | 10.3 (8.4–12.5) | 5.2 (2.5–8.0) | 0.95 (0.76, 1.19) | 0.48 (0.28, 0.83)* |
| Caesarean section delivery | 16.2 (15.0–17.4) | 12.4 (10.3–14.8) | 7.3 (4.0–10.5) | 0.77 (0.63, 0.93)* | 0.45 (0.29, 0.70)* |
| Spontaneous vaginal delivery | 75.1 (73.4–76.2) | 79.6 (76.3–81.8) | 87.1 (84.3–92.3) | 1.06 (1.02, 1.10) | 1.16 (1.10, 1.22)* |
| Neonatal outcomes** | 89.6 (88.6–90.6) | 90.2 (88.2–92.2) | 94.0 (91.0–97.0) | 1.01 (0.98–1.03) | 1.05 (1.01–1.08)* |
| *Statistically significant (ɑ = 0.05). | |||||
| **Avoided transfer to neonatal intensive care unit (NICU) | |||||
The relative risks (RR) of all interventions and outcomes in FP and MW compared with OB are also shown (Table 1). Patients in the FP group were more likely to experience spontaneous vaginal delivery (RR: 1.06; 95% CI: 1.02–1.10) and were less likely to receive induction/augmentation (RR: 0.83; 95% CI: 0.77–0.89) and caesarean section (RR: 0.77; 95% CI: 0.63–0.93). Patients in the MW group were more likely to experience spontaneous vaginal delivery (RR: 1.16; 95% CI: 1.10–1.22) and less likely to receive any of the interventions analyzed in this study: induction/augmentation (RR: 0.43; 95% CI: 0.35–0.54), epidural (RR: 0.53; 95% CI: 0.45–0.62), forceps/vacuum (RR: 0.48; 95% CI: 0.28–0.83) and caesarean section (RR: 0.45; 95% CI: 0.29–0.70). Newborns delivered in the FP group had comparable results in avoiding neonatal transfer to the NICU (RR: 1.01; 95% CI: 0.98–1.03), while the MW group showed a slight, but statistically significant, improvement (RR: 1.05; 95% CI: 1.01–1.08).
Costs
The decision tree model (Figure 1) assisted in determining the cost for each care pathway based on intervention, method of delivery and outcome variables attributed to each provider. According to the Ontario Schedule of Benefits (April 1, 2013), physician course of care cost was $1,025 (Table 2) for a low-risk obstetrical patient, including all antepartum and postpartum appointments as well as vaginal delivery (MOHLTC 2013). The portion of the course of care cost specified for vaginal delivery is 48%. Using the same portion, the cost for MWs attending a delivery was calculated at 48% of the course of care cost. Given that MWs have varying costs for courses of care depending on practice site (urban/rural) and seniority (Courtyard Group 2010), the course of MWs attending a delivery was calculated as $1,043 (0.48 × $2,147.50), with a range between $860 and $1,227 for the purposes of this CEA (Table 2). There was little difference in costs between FPs and OBs for the decision tree pathways, with the exception of caesarean section billings. For patients admitted under OBs who require caesarian sections, the OB fee for caesarean delivery (P018) plus a surgical assistant fee will be billed (P018B). However, for patients admitted under FPs, the FP fee for attendance at the delivery (P009) will be billed in addition to the OB fee for caesarean delivery (P018) but without a surgical assistant fee. Notably, in cases admitted under MWs requiring a caesarean delivery, each of the MWs course of care cost, the OB fee for caesarean delivery (P018) and surgical assistant fee (P018B) was attributed to the midwife branch. Additional costs for other interventions, referral, attendance by physicians, anaesthesia or a second MW were attributed to the admitting providers.
| TABLE 2. Cost variables | ||
| Description | Cost | Reference |
| Caesarean section with induction (case cost) | $5,639 | BCH CMG+ 558 |
| Caesarean section with no induction (case cost) | $3,461 | BCH CMG+ 559 |
| Vaginal delivery with anaesthetic and with non-major intervention (case cost) | $3,874 | BCH CMG+ 562 |
| Vaginal delivery with anaesthetic and without non-major intervention (case cost) | $2,938 | BCH CMG+ 563 |
| Vaginal delivery without anaesthetic and with non-major intervention (case cost) | $2,478 | BCH CMG+ 564 |
| Vaginal delivery without anaesthetic and without non-major intervention (case cost) | $1,936 | BCH CMG+ 565 |
| Newborn, singleton birth (case cost) | $790 | BCH CMG+ 576 |
| Newborn, caesarean birth (case cost) | $977 | BCH CMG+ 577 |
| Newborn, transfer to ICU (case cost) | $2,436 | BCH CMG+ 589–599 weighted average |
| Midwife costs for attending delivery | $1,043.68 | Prorated (48%) midwife course of care |
| Midwife second attending a birth | $214.00 | Ontario midwife compensation guide 2010 |
| Midwife referral for anaesthesia | $106.80 | Ontario physician schedule of benefits April 1, 2013 A816 |
| Midwife referral for physician assessment | $101.70 | Ontario physician schedule of benefits April 1, 2013 A813 |
| Physician costs for vaginal delivery | $498.70 | Ontario physician schedule of benefits April 1, 2013 P006 |
| Physician costs for forceps or vacuum delivery | $535.60 | Ontario physician schedule of benefits April 1, 2013 P020 |
| Physician costs for caesarean section delivery of a patient admitted by an obstetrician (time assumed to be one hour for assistant) | $700.20 | Ontario physician schedule of benefits April 1, 2013 P018 + P018B |
| Physician costs for caesarean section delivery of a patient admitted by a family physician | $1,078.50 | Ontario physician schedule of benefits April 1, 2013 P018 + P009 |
| Human resource cost of caesarean section delivery of patient admitted by midwife (time assumed to be one hour for assistant) | $1743.88 | Prorated (48%) midwife course of care + Ontario physician schedule of benefits April 1, 2013 P018 + P018B |
| Physician costs for induction or augmentation of labour with oxytocin | $67.75 | Ontario physician schedule of benefits April 1, 2013 P023 |
| Anaesthesia costs for inserting and maintenance of epidural (time assumed to be six hours [maximum]) | $270.18 | Ontario physician schedule of benefits April 1, 2013 P014C + P016C |
| Anaesthesia costs for attendance at caesarean section (time assumed to be one hour) | $165.11 | Ontario physician schedule of benefits April 1, 2013 P018C |
| Anaesthesia costs for attendance at caesarean section with no epidural (time assumed to be one hour) | $90.06 | Ontario physician schedule of benefits April 1, 2013 P013C |
Case costs for method of delivery at BCH ranged from a total average cost of $1,936 for vaginal delivery without anaesthetic and without non-major intervention to $5,639 for a caesarean section with induction (Table 2). In addition, the case costs for outcome ranged from $790 for singleton delivery to $2,436 for newborn transfer to the NICU. The BCH CMG+ costs varied from 19% (caesarean delivery) to 25% (vaginal delivery with anaesthetic and with non-major intervention) in comparison with the provincial averages.
Cost-effectiveness
In the CEA model, MW care dominated the other two providers, as it was both more effective (fewer NICU admissions) and less costly. As well, FPs dominated in relation to OBs. It is important to recognize that there are small differences in both the total cost per delivery by provider ($5,188 [OB], $5,116 [FP] and $5,102 [MW]) and the difference in NICU admissions (Table 3).
| TABLE 3. Cost-effectiveness analysis results | |||||||
| Ministry perspective | |||||||
| Provider | Cost | Incremental cost | Effectiveness | Incremental effectiveness | Incremental C/E | NMB | C/E |
| Midwife | $5,102 | 0.9395 | -5,102 | 5,431 | |||
| Family physician | $5,116 | 14 | 0.9018 | -0.0377 | -361 | -5,116 | 5,673 |
| Obstetrician | $5,188 | 86 | 0.8956 | -0.0439 | -1957 | -5,188 | 5,793 |
Sensitivity analysis
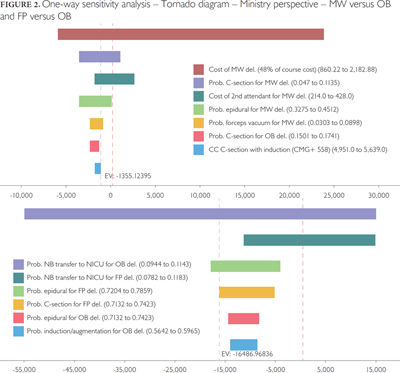
Results of the one-way sensitivity analysis for MW versus OB as well as FP versus OB are shown in a Tornado diagram (Figure 2). The Tornado diagram shows that MW and FP strategy has a positive cost-effectiveness relative to OB, but that varying certain costs and intervention rates to values from the literature or provincial estimates could reduce the difference between providers or eliminate all advantage. Most notably, varying the MW compensation to the increased level recommended by a pay equity consultant – a 75% compensation increase – for the AOM lawsuit (calculated as $2,182 for MW costs for attending delivery, which represents 48% of requested course of care fee) negated the MW dominance as a cost-effective strategy for low-risk births (Figure 2). This is an important finding because it demonstrates the impact of human resource costs in the model. The probability of receiving a caesarean section for a mother admitted by MW and the cost of the second attendant in MW deliveries also had an effect. Varying the probabilities of newborn transfer for both the FP and OB had a greater positive effect on FP cost-effectiveness compared with OBs.
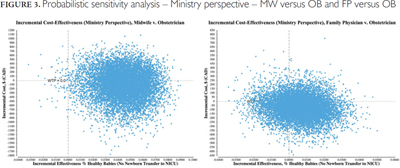
The results of the probabilistic sensitivity analysis show that the MW sample is stable with respect to effect size for the primary health outcome (Figure 3). Based on the variance around both the MW and OB group, the model has a 95% certainty that MW newborns are transferred less often than OB patients. However, the cost estimate has a large variance and the 95% confidence interval is −$900 (savings) and +$700 (increased costs). Overall, the MW strategy cost less than $5,000 per NICU transfer avoided in 80% of scenarios and less than $1,000 per NICU transfer avoided in 63% of scenarios compared with the OB strategy. Within the FP versus OB analysis, the model was sensitive to both cost and effect variations for this population.
Discussion
The model shows that MWs and FPs were more cost-effective than OBs in performing deliveries in low-risk obstetrical patients. Notably, MWs have demonstrated significantly lower intervention rates, which are accompanied by lower costs. The sensitivity analyses showed the MW model to be sensitive to increases in the compensation for attending the delivery. If MW compensation increases, they may no longer be the cost-effective strategy.
BCH was a model hospital for this study because all three groups provide obstetrical care in this institution and MWs have the capacity to practice to their full scope of practice (College of Midwives of Ontario 1999). In contrast to other hospitals in Ontario, the scope of MW practice includes managing the care of clients who have received an epidural or whose labour has been induced or augmented (Ontario Hospital Association et al. 2010), which enables MWs to continue as primary provider for a larger proportion of patients without transferring such patients to another provider. As all births in this study took place in BCH, this study did not include home births attended by MWs or deliveries at birthing centres.
Strengths and limitations
A strength of this study is that it was based on real data and included almost 5,000 patients. While the 248 MW births may appear small, the hospital has among the most MW-led deliveries for any institution in Ontario under the current limited scale of midwifery in the province. This model attributed all interventions and outcomes and their associated costs for a particular patient to the admitting provider instead of the providers who applied interventions, and this may have inflated intervention rates and associated costs for FP and MW providers. The strength of the CMG+ methodology is in its generalizability across Ontario; it is a good way to look at populations of patients within the same hospital or health system. The limitation is the use of an average cost; costs for providers who are not using resources such as nursing staff are overestimated, and costs for providers who use more resources are underestimated. For example, MWs may not have nursing staff present during labour and delivery, which may result in lower direct costs. Together, it is reasonable to suggest that these factors have resulted in even more conservative cost-effectiveness estimates in support of the MW strategy. It is uncertain whether higher-than-average CMG+ cost at BCH for case types is a reflection of being higher-than-average or rather simply a larger facility or having a concentration of specialists than other community-based health facilities.
The cost-effectiveness results should be viewed with caution, however, as costs and outcomes differed by narrow margins. It is also unknown whether the findings here are generalizable to MW care in other delivery settings such as homes and birth centres, as outcomes may vary (Grunebaum et al. 2014). A potential bias of the study is that lower-risk patients may have self-selected a MW. Previous studies showed that patients who choose a MW have a desire to avoid technology and intervention, while some women perceive childbirth as a process with inherent risks and are more likely to choose a physician and be more accepting of technology and intervention (Howell-White 1997), but this level of analysis is not possible using data from the comprehensive BORN database. Other than age of mothers, it was not possible to examine patient-level characteristics such as ethnicity, education level or socio-economic background, which may have influenced the types and number of interventions used during labour and delivery. Even though the mean maternal age was higher in the MW group by 1.5 years, this difference is not expected to change the results. It is conceivable that the slightly older MW patients resulted in a more conservative estimate for cost-effectiveness. Attributing costs, however, to the original provider helps to mitigate the potential bias of only having very healthy patients in the MW group. This model was designed to reflect, as closely as possible, the consequence of patients choosing their preferred provider for pregnancy care, labour and delivery.
The time frame selected for analysis was from hospital admission of the pregnant patient until discharge of mother and baby. The CEA only accounted for the costs of labour and delivery, as opposed to the entire course of care that typically also includes antenatal and postpartum care. This is relevant to MWs because they are paid in the form of one course of care fee for the entire pregnancy, in contrast to physicians who are paid by fee-for-service. Using a percentage of total MW costs for calculating the cost for attending delivery in our model was necessary to compare disparate funding models. Further assumptions made when costing specific interventions may also have led to some biases. With respect to physician costing, it was assumed that all instrumental deliveries were mid-cavity extractions and were priced at the premium delivery code of P020, as opposed to P006 (MOHLTC 2013), which increases the cost of delivery by $36.90. However, this only occurred in 10.2% of cases for FPs and 10.8% for OBs (Table 1) and, therefore, has a negligible effect on total cost. Furthermore, physician-led birth costs may have been underestimated because allowable evening/night/weekend premiums were not included.
Summary and future directions
This study shows that MWs are the most cost-effective provider group for low-risk obstetrical care during delivery in this hospital setting. All three provider groups were similar with respect to the cost per delivery. In November 2013, the AOM initiated legal action against the MOHLTC under the Human Rights Tribunal of Ontario, claiming systematic discrimination in MW remuneration on the basis of gender (Association of Ontario Midwives [AOM] 2013). Based on our findings, if compensation for MWs is increased to the levels recommended in the pay equity lawsuit, MWs would no longer be the most cost-effective provider group. Currently, MWs are only meeting 65% of the demand for their services (Ontario Hospital Association et al. 2010). This study's findings support greater integration and collaboration between MWs, FPs and OBs for providing obstetrical care in hospital settings under the current provider compensation schemes. Finally, the model developed may be used for future larger research studies across multiple settings and can inform governments on funding frameworks for obstetrical care.
Analyse coÛt-efficacité des accouchements à faible risque : comparaison entre sages-femmes, médecins de famille et obstétriciens
Résumé
Objectif : Étudier le rapport coÛt-efficacité des soins obstétricaux offerts à l'hôpital par les obstétriciens (OB), par les médecins de famille (MF) et par les sages-femmes (SF) pour les accouchements à faible risque.
Méthodes : Analyse coÛt-efficacité, selon l'angle du ministère de la Santé, au moyen d'une étude de cohorte rétrospective. La période de temps visée s'étendait de l'admission à l'hôpital d'une patiente enceinte à faible risque jusqu'à l'obtention du congé par la mère et l'enfant. Les données sur le calcul des coÛts comprenaient les ressources humaines, les interventions et les coÛts d'hospitalisation du groupe clients. Les interventions retenues pour les mesures étaient le déclenchement ou l'accélération du travail à l'aide de l'ocytocine, le recours à l'épidurale, l'emploi du forceps ou de la ventouse obstétricale et la césarienne. Le résultat mesuré était l'évitement d'un transfert vers l'unité de soins intensifs néonatals (USIN). Divers types d'analyses de la sensibilité ont été employés pour tester les résultats modélisés.
Résultats : L'âge moyen à l'accouchement, selon les groupes de fournisseurs de soins, était de 29,7 pour les OB, 29,8 pour les MF et 31,2 pour les SF – une moyenne statistiquement plus élevée pour le groupe des SF. Les accouchements avec SF présentaient des coÛts moins élevés et de meilleurs résultats que ceux avec les MF et les OB. En ce sens, les MF obtiennent de meilleurs résultats que les OB. La différence du coÛt par accouchement était peu marquée, mais légèrement plus petite pour les SF (5 102 $) et pour les MF (5 116 $) que pour les OB (5188 $). L'évitement du transfert à l'USIN était plus élevé chez les SF, soit à 94,0 % (95 % IC: 91,0–97,0), comparé aux MF avec 90,2 % (95 % IC: 88,2–92,2) et aux OB avec 89,6 % (95 % IC: 88,6–90,6). Le rapport coÛt-efficacité pour le groupe des SF est réduit grâce à l'accroissement des avantages. Le rapport coÛt-efficacité pour le groupe des MF est sujet à changement en raison des taux et coÛts des interventions.
Conclusions : La stratégie des SF présente le meilleur rapport coÛt-efficacité en milieu hospitalier. Malgré la limite des données permettant d'approfondir les caractéristiques des patientes selon les groupes, les résultats d'ensemble de cette étude appuient le financement des SF ainsi qu'une meilleure intégration des SF dans le système en place.
About the Author(s)
Dylan Walters, MA, Student Fellow, Canadian Centre for Health Economics, Institute of Health Policy, Management and Evaluation, University of Toronto, Toronto, ON
Archna Gupta, MD, CCFP, MPH, Family Physician, Department of Family Medicine, Brampton Civic Hospital, Brampton, ON
Austin E. Nam, MSc, Institute of Health Policy, Management and Evaluation, University of Toronto, Toronto, ON
Jennifer Lake, PharmD, Assistant Professor, Leslie Dan Faculty of Pharmacy, University of Toronto, Toronto, ON
Frank Martino, MD, CCFP(EM), FCFP, Chief of Family Medicine, William Osler Health System, Brampton, ON
Peter C. Coyte, PhD, Professor, Institute of Health Policy, Management and Evaluation, University of Toronto, Toronto, ON
Correspondence may be directed to: Dylan Walters, Canadian Centre for Health Economics, Institute of Health Policy, Management and Evaluation, University of Toronto, 155 College Street, 4th Floor, Toronto, ON M5T 3M6; tel.: (416) 999-7890; e-mail: dylan.walters@mail.utoronto.ca.
References
Aenhaim, H., M. Welt and R. Sabbah. 2007. "Obstetrician or Family Physician: Are Vaginal Deliveries Managed Differently?" Journal of Obstetrics and Gynecology Canada 20(10): 801–04.
Association of Ontario Midwives (AOM). 2013. "Ontario Midwives Application to the Human Rights Tribunal of Ontario: A Summary." Retrieved December 2, 2013. <http://www.ontariomidwives.ca/images/uploads/documents/Ontario_Midwives_Application_to_the_Human_Rights_Tribunal_of_Ontario_letterhead.pdf>.
Bank of Canada. 2014. "Exchange Rates: USD." Retrieved April 22, 2014. <http://www.bankofcanada.ca/rates/exchange/>.
Betran, A.P., M. Merialdi, J.A. Lauer, W. Bing-Shun, J. Thomas, P. Van Look et al. 2007. "Rates of Caesarean Section: Analysis of Global, Regional and National Estimates." Paediatric and Perinatal Epidemiology 21(2): 98–113. doi:10.1111/j.1365-3016.2007.00786.x.
Birthplace in England Collaborative Group, P. Brocklehurst, P. Hardy, J. Hollowell, L. Linsell, A. Macfarlane et al. 2011. "Perinatal and Maternal Outcomes by Planned Place of Birth for Healthy Women with Low Risk Pregnancies: The Birthplace in England National Prospective Cohort Study." BMJ (Clinical Research Ed.) 343: d7400. doi:10.1136/bmj.d7400.
Briggs, A., R. Goeree, G. Blackhouse and B. O'Brien. 2001. "Probabilistic Analysis of Cost-Effectiveness Models: Choosing between Treatment Strategies for Gastro-Esophageal Reflux Disease. Medical Decision Making 22(4): 290–308. doi: 10.1177/0272989X0202200408.
Canadian Institute of Health Information (CIHI). 2012. "Patient Cost Estimator." Retrieved November 28, 2013. <http://www.cihi.ca/CIHI-ext-portal/internet/en/applicationnew/spending+and+health+workforce/spending/cihi020209>.
Canadian Institute of Health Information (CIHI). 2013. Highlights of 2011–2012 Selected Indicators Describing the Birthing Process in Canada. Canadian Institute of Health Information. Ottawa, ON.
College of Midwives of Ontario. 1999. Indications for Mandatory Discussion, Consultation, and Transfer of Care. College of Midwives of Ontario. Toronto, ON.
Courtyard Group. 2010. Compensation Review of Midwifery on behalf of Ministry of Health and Long Term Care and Association of Ontario Midwives. Toronto, ON.
Drummond, M.F., M.J. Sculpher, G.W. Torrance, B.J. O'Brien and G.L. Stoddart. 2005. Methods for the Economic Evaluation of Health Care Programmes. Oxford: Oxford University Press.
Durber, P. 2013. Examining the Issue of Equitable Compensation for Ontario's Midwives. A report for the Association of Ontario Midwives, November 24, 2013. <http://www.ontariomidwives.ca/images/uploads/documents/Durber_Report_-Examining_the_Issue_of_Equitable_Compensation_for_Ontarios_Midwives_Nov._24,_2013_(C0928577).pdf>.
Grunebaum, A., L.B. McCullough, K.J. Sapra, R.L. Brent, M.I. Levene, B. Arabin et al. 2014. "Early and Total Neonatal Mortality in Relation to Birth Setting in the United States, 2006–2009." American Journal of Obstetrics and Gynecology 212(2): 250. doi: 10.1016/j.ajog.2014.10.005.
Howell-White, S. 1997. "Choosing a Birth Attendant: The Influence of a Woman's Childbirth Definition." Social Science & Medicine 45(6): 925–36.
Janssen, P.A., E.M. Ryan, D.J. Etches, M.C. Klein and B. Reime. 2007. "Outcomes of Planned Hospital Birth Attended by Midwives Compared with Physicians in British Columbia." Birth 34(2): 140–47. doi:10.1111/j.1523-536X.2007.00160.x.
Krikke, E. and N. Bell. 1989. "Relation of Family Physician or Specialist Care to Obstetric Interventions and Outcomes in Patients at Low Risk: A Western Canadian Cohort Study." CMAJ 140(6): 637–43.
Ministry of Health and Long-Term Care (MOHLTC). 2013. Schedule of Benefits: Physician Services under the Health Insurance Act. Toronto, ON.
Ontario Hospital Association, the College of Midwives of Ontario and the Association of Ontario Midwives. 2010. Resource Manual for Sustaining Quality Midwifery Services in Hospitals. Toronto, ON.
Petrou, S., J. Henderson and C. Glazener. 2001. "Economic Aspects of Caesarean Section and Alternative Modes of Delivery." Best Practice & Research in Clinical Obstetrics and Gynaecology 15(1): 145–63. doi:10.1053/beog.2000.0154.
Public Health Agency of Canada. 2009. What Mothers Say: The Canadian Maternity Experiences Survey. Ottawa: Public Health Agency of Canada.
Reid, A.J., J.C. Carroll, J. Ruderman and M.A. Murray. 1989. "Differences in Intrapartum Obstetric Care Provided to Women at Low Risk by Family Physicians and Obstetricians." CMAJ: Canadian Medical Association Journal 140(6): 625–33.
Rosenblatt, R.A., S.A. Dobie, L.G. Hart, R. Schneeweiss, D. Gould, T.R. Raine et al. 1997. "Interspecialty Differences in the Obstetric Care of Low-Risk Women." American Journal of Public Health 87(3): 344–51.
Sandall, J., H. Soltani, S. Gates, A. Shennan and D. Devane. 2013. "Midwife-Led Continuity Models Versus Other Models of Care for Childbearing Women." The Cochrane Database of Systematic Reviews. 8(CD004667). 1–107 doi: 10.1002/14651858.CD004667.pub3.
SAS Institute Inc. 2013. What's new in SAS 9.4. Cary, USA.
Sutcliffe, K., J. Caird, J. Kavanagh, R. Rees, K. Oliver, K. Dickson et al. 2012. "Comparing Midwife-Led and Doctor-Led Maternity Care: A Systematic Review of Reviews." Journal of Advanced Nursing 68(11): 2376–86. doi:10.1111/j.1365-2648.2012.05998.x.
TreeAge. 2015. TreeAge pro 2015 user's manual. TreeAge Software, Inc. Williamstown, MA, USA
Villar, J., G. Carroli, D. Khan-Neelofur, G. Piaggio and M. Gulmezoglu. 2001. "Patterns of Routine Antenatal Care for Low-Risk Pregnancy." The Cochrane Database of Systematic Reviews 4: CD000934. doi:10.1002/14651858.CD000934.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed