Books
Background
In 2007, the British Columbia (BC) government released the Primary Health Care Charter, setting the direction, targets and outcomes to support the creation of a strong, sustainable, accessible and effective primary healthcare system in the province (BC Ministry of Health 2007). The report highlights the importance of partnerships with patients to achieve these goals, and calls for infrastructure supports to sustain both the philosophy and policy of patients as partners in efforts to bring about large-scale health system change.
The Patients as Partners program, created in 2008, is a partnership among the BC Ministry of Health, patients, healthcare providers, universities, healthcare not-for-profit organizations and non-governmental organizations. These partners work together to include the patient voice, choice and representation in healthcare improvement initiatives. The aim of Patients as Partners is to achieve better health outcomes and to improve the experience of professionals and patients at a sustainable cost – recognized as the Triple Aim.
Patient Engagement
The Patients as Partners philosophy is guided by three quality improvement charters developed collaboratively with patients, healthcare stakeholder organizations and the BC Ministry of Health. The charters focus on engagement at various levels of the system, including individual care; program and community services; and system redesign. Together, the charters provide the overall vision and strategic direction for the work. The partners involved in Patients as Partners collaborate to set the program’s goals and systematically undertake healthcare improvement efforts.
“Nothing about me without me” is the principle driving change at Patients as Partners. Patients are partners when they are supported and encouraged to “participate in decision-making about their own care at the level they choose and in quality improvement and healthcare redesign in ongoing and sustainable ways” (McQuillen et al. 2013). The Patients as Partners Partnership Framework (Figure 1) illustrates the bottom-up and top-down collaborative approach that is central to the program. Patient members, recruited through partner networks, including the BC Family Caregivers Network, intercultural Online Network, Patient Voices Network (PVN) and the Chronic Disease Self‑Management Program, are involved in all Patients as Partners committees.
Supporting self-management
Patients as Partners collaborates with its partners across the province to bring chronic disease self-management principles and strategies to within people’s own communities in BC. The Centre for Collaboration, Motivation and Innovation (CCMI) provides Brief Action Planning (BAP), a structured, patient-centred, stepped-care, evidence-based self-management support tool to help patients engage in positive behaviour change. The University of Victoria’s Chronic Disease Self-Management Program delivers group-based programs (adapted from the Stanford University Chronic Disease Self-Management Program) in chronic disease self-management and diabetes (in English, Chinese and Punjabi); chronic pain, arthritis/fibromyalgia and active choices (in English); and an online chronic disease self-management program (in English). The University of Victoria’s Chronic Disease Self-Management Program has trained 4,843 program leaders and has reached 27,259 people with chronic health conditions across the province.
The interCultural Online Health Network (iCON) is a community-driven health promotion initiative that helps multicultural communities, patients and caregivers across BC optimize chronic disease prevention and management in a way that respects traditional and cultural values. iCON is funded by Patients as Partners and implemented by the University of British Columbia Faculty of Medicine eHealth Strategy office. iCON has been successfully working with South Asian and Chinese communities since 2007 and with Aboriginal communities since 2010 to offer greater access to up-to-date, culturally relevant and translated health information on a variety of health topics (e.g., diabetes, heart disease, dementia, liver disease, mental health), as well as provide information on health system navigation to help patients become more informed users of the healthcare system. In addition, health information is shared at public health forums and workshops, via webcasts and a website (iconproject.org), and through special media projects (television and radio programming) (iCON 2016).
Figure 1: Patients as Partners Partnership Framework
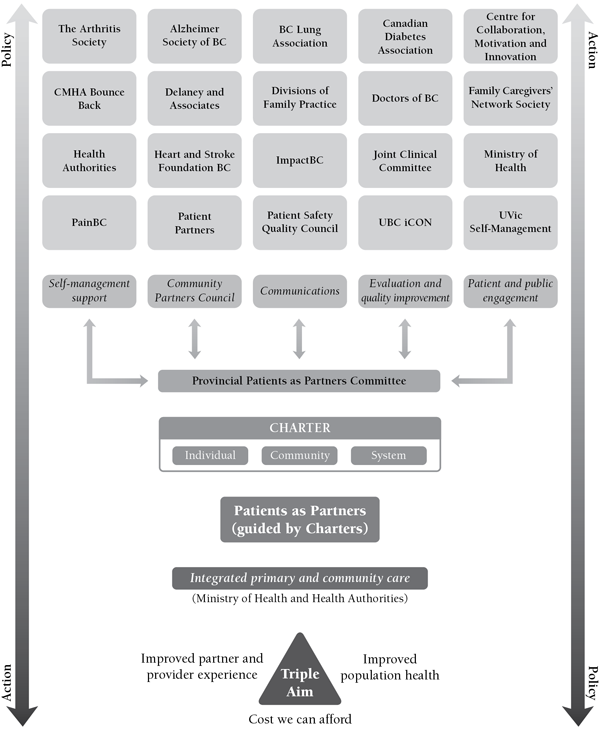
Supporting patient and public engagement in system redesign
Patients as Partners also supports capacity building to design meaningful engagement opportunities within existing healthcare settings. Key to the culture shift has been the five days of training in patient and public engagement for both staff and patients. Patients as Partners has used the International Association of Public Participation (IAP2) curriculum and tailored engagement approaches to focus on BC healthcare system case studies. Training in patient and public engagement (PPE) has been key to the shift towards a Patients as Partners culture in BC. Participants value learning together to begin improvement work based on a common understanding of the proposed roles and mechanisms of engagement.
The PVN is one of several networks within Patients as Partners. This network matches patients with healthcare providers seeking to include the patient voice in decision-making associated with specific initiatives. The PVN recruits patients to become part of a volunteer pool. All patients must undergo an orientation session and are afforded ongoing skill-building opportunities, coaching and information support from PVN staff. Patients are also matched with healthcare providers who seek to include the patient voice within their decision-making processes. In this role of facilitating connections between patients and providers, the PVN ensures that expectations of both providers and patients are managed to ensure meaningful participation of patients.
Key Strategies to Support Patient and Provider Engagement
Infrastructure support
The BC government recognized that large-scale health system change would require new partnerships with patients. By identifying patients as partners as a philosophy within its Primary Health Care Charter and by supporting infrastructure to operationalize this philosophy, the provincial government led the implementation of infrastructure to support the expression of the philosophy in specific contexts. This adaptability facilitated the culture shift.
Patients as Partners equips both patients and providers with the supports necessary to enter into meaningful partnerships. The program serves as a facilitator, connecting patients and organizations or initiatives seeking the participation of patients to ensure meaningful engagement. PVN encourages patients to participate at the level that they choose, affording the flexibility to meet individual patient needs. Further, Patients as Partners manages the expectations of providers by ensuring the purpose and level of engagement are appropriate for the improvement initiative and that patients are matched accordingly. Centralization of these infrastructure supports brought a degree of standardization to engagement efforts across the province, while building a shared base of knowledge and expertise (BC Ministry of Health 2013).
Collaborative approach
The BC Ministry of Health supports a distributed leadership approach. Recommendations set forth in the Primary Health Care Framework created an expectation for change and accountability at the most senior level of leadership. The work of Patients as Partners is guided by a provincial Patients as Partners Committee, whose membership includes representatives from the Ministry of Health, regional health authorities, healthcare organizations, providers and not-for-profit organizations, as well as patients, families and caregiver members. Patients have been involved since the inception of Patients as Partners, sitting on all six Ministry of Health Patients as Partners subcommittees to ensure the program maintains its focus: enabling end-users to be active partners in healthcare.
Measurement focus
Influenced by the need to measure research, accountability and quality improvement, Patients as Partners’ measurement strategy has evolved. The Provincial Patients as Partners Committee has developed a provincial measurement strategy that includes a variety of instruments to gauge individual and community engagement as well as elements of system design (McQuillen et al. 2013).
Impact
Over 30,000 patients in BC are currently engaged in the Patients as Partners program. “The culture in BC is shifting to value and expect the patient voice at all tables,” noted Caryl Harper, the director of Patients as Partners. For example, through the PVN, patients are now sitting on complex advisory tables, such as the provincial surgical executive committee and UBC’s reallocation subcommittee. Patients are also included in committees’ terms of reference.
The PVN is also gaining attention beyond the province. For example, recognizing the value of engaging patients in system redesign, the Government of New Brunswick recommended the implementation of a PVN in its 2012 Primary Healthcare Framework (Government of New Brunswick 2012). Patients as Partners program evaluation results from a March 2014 stakeholder meeting demonstrate a high degree of confidence that participants “believe in the direction that Patients as Partners and patient-centred care is headed” (BC Ministry of Health 2014). Through the iCon program, meanwhile, there is strong evidence that participants are becoming more active in managing their own health. Using an adapted patient activation measure (PAM), iCON participants are demonstrating increased PAM scores following training (Harper 2015: personal communication). Notably, attendees at a Punjabi language forum and workshop reported a statistically significant change in patient activation levels: 75 per cent of participants expressed the intention to make a positive health behaviour change as a result of attending an iCON event.
Summary
The Patients as Partners program aims to achieve better health outcomes and improve the experience of professionals and patients at a sustainable cost through partnerships with patients. The work of Patients as Partners is guided by three quality improvement charters that focus on engagement at various levels of the system, including individual care, program and community services and system redesign. Key to its success has been the infrastructure support to centralize engagement efforts and build a collective body of knowledge and expertise. The distributed leadership approach has given rise to many core champions who work collectively toward the shared goals of patient partnership. Since this case study was written, oversight and administration of the PVN has changed and, as of December 2015, resides with the BC Patient Safety & Quality Council.
This case study was researched and written in 2015 as part of research commissioned by the Federal Advisory Panel for Healthcare Innovation to inform their report: Unleashing Innovation: Excellent Healthcare for Canada (https://www.healthycanadians.gc.ca/publications/health-system-systeme-sante/report-healthcare-innovation-rapport-soins/index-eng.php)
About the Author(s)
Christine Maika, BSc, MPH (candidate), Improvement Lead, Canadian Foundation for Healthcare Improvement, Ottawa, ON
Caryl Harper, MSN (candidate), Former Director, Patients as Partners, BC Ministry of Health, Victoria, BC
Maria Judd, BScPT, MSc, Senior Director, Canadian Foundation for Healthcare Improvement, Ottawa, ON
References
BC Ministry of Health. 2007. Primary Health Care Charter: A Collaborative Approach. Retrieved February 16, 2016. <http://www.health.gov.bc.ca/library/publications/year/2007/phc_charter.pdf>.
BC Ministry of Health. 2013. Patients as Partners: The Patient and Health Care Provider Experience: 2012–2013 Annual Report. Retrieved February 13, 2015 from: <http://www2.gov.bc.ca/assets/gov/health/about-bc-s-health-care-system/primary-health-care/patients-as-partners-annual-report-2012-2013.pdf>.
BC Ministry of Health. 2014. Patients as Partners 2014: Provincial Dialogue Event Summary. Retrieved February 18, 2016. <http://www2.gov.bc.ca/assets/gov/health/about-bc-s-health-care-system/primary-health-care/patients-as-partners-event-summary-2013.pdf>.
Government of New Brunswick. 2012. A Primary Health Care Frame Work for New Brunswick. Retrieved February 9, 2016. <http://www.gnb.ca/0053/phc/pdf/2012/8752_EN%20Web.pdf>.
Harper, C. 2015 (January 29). Personal communication.
InterCultural Online Health Network (iCON). 2016. Project Overview. Retrieved February 13, 2015. <http://www.iconproject.org/dnn_icon/aboutus/projectoverview>.
McQuillen K., C.L. Davis, K. Ho, P. McGowan, J. Resin, K. McEwan et al. 2013. “Challenges in Measuring Patient Participation: Case Studies from British Columbia’s Patients as Partners Initiative.” Journal of Participatory Medicine 5: e10. Retrieved February 19, 2016. <http://www.jopm.org/evidence/case-studies/2013/02/27/challenges-in-measuring-patient-participation/>.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed


