Healthcare Policy
A Survey of Health Equity Practices in Early Psychosis Intervention Programs: A Starting Point for Improvement
Avra Selick, Alexandra Lamoureux, Karen O'Connor and Janet Durbin
Abstract
Equity has been identified as a core component of quality healthcare in Ontario. However, translating policy into practice can be challenging. This paper reports results from a province-wide survey of early psychosis intervention programs to assess the extent to which equity has been incorporated into program delivery. All 56 programs (100%) completed the survey. Results found that while most programs perceive that they are meeting equity aims, they reported limited use of practices to support this aim, and few systematically collect information on performance. Strategies to improve equity in practice are discussed.
Background
Equity is an established priority and legal requirement of the Ontario healthcare system (e.g., Accessibility for Ontarians with Disabilities Act 2005; Excellent Care for All Act 2010; French Language Services Act 1990). Health equity is defined as the absence of disparities in the health outcomes of specific populations that are "not only unnecessary and avoidable, but in addition, are considered unfair and unjust" (Whitehead 1992: 433). A health equity strategy is intended to create opportunities for all individuals to experience good health, and reduce differences in the health outcomes of specific populations, for example, due to gender, sexual orientation, geography, ability, ethnicity or income. Importantly, a health equity approach is more than the absence of discrimination; it requires active steps be taken to counteract the existing disparities faced by vulnerable groups.
In recent years, positive steps have been taken in Ontario to put policy into practice. The Ministry of Health and Long-term Care (MOHLTC) developed the Health Equity Impact Assessment (HEIA), a tool that organizations can use to identify unintended impacts of policies and programs for marginalized populations and follow-up mitigation and monitoring strategies (MOHLTC 2013). Several Local Health Integration Networks (LHINs; regional health authorities) have implemented system-wide initiatives to expand and standardize socio-demographic data collection with the aim of improving health equity (e.g., Mississauga Halton LHIN 2016; Toronto Central LHIN and Mount Sinai Hospital 2016). Health Quality Ontario (HQO), a provincial agency that monitors the quality of healthcare, includes equity as one of six dimensions of quality care it monitors and reports annually as part of the Common Quality Agenda (Health Quality Ontario 2016a).
Despite these initiatives, health service providers have received limited direction on specific approaches to address health inequities in their programs. It remains mostly up to individual organizations to identify strategies to implement and set equity targets.
Early Psychosis Intervention (EPI) is one of a funded basket of services in the community mental health and addictions system in Ontario. EPI is an evidence-based model of care aimed at engaging young adults in treatment as soon as possible after their first episode of psychosis to minimize duration of untreated psychosis. The EPI model takes a holistic approach to treatment and, in addition to medication and therapy, focuses on active outreach, psychoeducation, re-engagement in education or work, physical health monitoring and family support (Bird et al. 2010).
Despite this emphasis on early engagement in care, research has shown that factors including race, ethnicity, gender, sexual orientation, income and immigration status are associated with compromised access to EPI programs, including negative pathways into care (i.e., access through justice or hospital) (Anderson et al. 2010; Bhui et al. 2003), higher dropout rates (Ouellet-Plamondon et al. 2015) and overall reduced help-seeking (Franz et al. 2010). Recognizing these issues, health equity is explicitly embedded in the Ontario EPI Program Standards (MOHLTC 2011). Standard 11, Barrier-Free Services, includes the expectation that individuals from all communities are able to access EPI services and that services are delivered in a manner sensitive to the backgrounds and experiences of different clients, considering language, customs, beliefs and other factors. The Standard lists strategies for programs to use to meet these aims; these pertain to both service quality (i.e., recruitment of diverse staff, use of interpreters, multilingual program materials, youth-friendly physical space) and access (i.e., self-referral, community early identification system).
After the EPI Program Standards were released, a committee was formed to support implementation. An initial task was a sector-wide key informant survey to learn about EPI program delivery in relation to the Standards. The present paper reports survey results for the Barrier-Free Standard, including the extent to which programs have incorporated health equity practices into service delivery, and available supports.
Method
Survey development
Two online surveys were developed as part of a larger project to obtain sector feedback on implementation of the EPI program Standards. Results from the first survey (Standards 1–6) are reported elsewhere (Durbin et al. 2016). The second survey on implementing Standards 7–13 asked about overall compliance, use of various implementation practices and availability of implementation supports. Survey development was supported by reviewing the literature and relevant policy documents, several iterations of feedback from Ontario EPI service providers on the clarity of survey questions and response options and on relevance of items to the Ontario system. The survey contained 85 questions in total.
Pertaining to the Barrier-Free Standard, there were 11 questions, both close-ended (Likert scale) and open-ended. Within these questions, programs were asked to rate: (1) overall compliance regarding the extent to which clients reflected the diversity of the local community and the extent to which the program was able to meet their treatment needs; (2) frequency of use of 14 strategies for incorporating a health equity approach into program delivery, with items based on Canadian and international equity policies and literature (e.g., Department of Health 2001; Registered Nurses' Association of Ontario 2007; Singh and Kunar 2010); (3) the extent to which additional supports were needed to promote the inclusion of 11 vulnerable groups, with groups based on the HEIA (MOHLTC 2013) and (4) the availability of administrative supports for this work (six items). In open-ended questions, respondents had the opportunity to elaborate on their responses and describe innovative practices.
Data collection
All 56 Ontario EPI programs were invited to complete the survey during February and March 2014. An invitation was sent to a contact person at each program, usually a manager or clinical lead, with follow-up e-mails and telephone calls to encourage completion.
Analysis
For the close-ended items, percentages were calculated of programs who indicated yes (vs. no), regularly (vs. not at all/rarely or sometimes) or a fair amount or great deal (vs. not at all/rarely or occasionally), as relevant. Results were calculated for the sample as a whole and then compared for small programs (two or fewer full-time equivalent [FTE] clinical staff) and large programs (greater than two clinical FTEs). Large programs typically serve urban catchment areas, whereas small programs serve rural or mixed urban/rural catchment areas (Durbin et al. 2016). Fisher's Exact tests were used to determine significance. Qualitative feedback from open-ended questions was summarized to distill key ideas.
Ethics approval for this study was obtained from the research team home institution.
Results
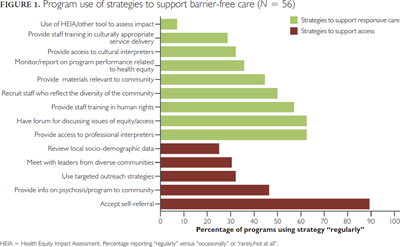
Fifty-six Ontario EPI programs participated in the survey, achieving a 100% response rate. Informant ratings of overall compliance with the Barrier-Free Standard were high, with the majority of programs (84%) reporting that they were able to meet the treatment needs of diverse clients a fair amount or great deal, and that the clients reflected the diversity of their local community. However, use of strategies to support equitable access and care was variable, with 10 of 14 assessed strategies used by fewer than half of programs (see Figure 1). Only one-third of programs reported regularly on their program performance related to health equity to their Board or LHIN; only 7% regularly used the HEIA or other equity assessment tools.
Regarding access for marginalized groups, almost 40% of programs identified First Nations, Inuit and Métis and 21–23% identified linguistic minorities and persons who are D/deaf, hard of hearing or visually impaired as communities for whom additional support was needed to engage and appropriately meet their needs (Figure 2). Although fewer programs requested additional support to engage individuals with developmental disabilities, qualitative results found that some programs felt challenged to provide care for this population.
Almost 60% of programs reported having leadership support to implement the Standard and almost half had a written policy. However, few programs reported having a designated support person (36%), an implementation plan (23%) or dedicated resources (18%), and few regularly evaluated their performance (21%) (Figure 3). A high number of respondents were uncertain whether or not supports were available. Qualitative responses provided more detail on implementation challenges including: limited resources to conduct outreach; insufficient staff training; difficulty recruiting staff reflective of the community and an inaccessible physical space.
There were generally no significant differences between large (n = 31) and small (n = 25) programs (not shown). The only exceptions were that small programs were more likely to meet with leaders from diverse communities (48% vs. 16%; p = 0.02) and large programs were more likely to provide access to interpreters (77% vs. 44%; p = 0.01).
Overall, the qualitative responses revealed that while some programs are using innovative and creative strategies to incorporate equity approaches into their programs, others identified significant barriers. Additionally, some respondents stated that they were unfamiliar with the term "health equity" and others gave responses indicating a misunderstanding of the concept, for example: "We are not excluding anyone from our program at this time." "Equity is not a concern in our small agency/small community. We do not discriminate against any minority group."
Discussion
This study found that most programs believed they were providing equitable care; however, use of practices to support this aim was limited. To enhance access, most programs accepted self-referrals but few reported regular use of other strategies (e.g., review of local socio-demographic data to identify underserved groups). To make care responsive, many programs offered access to language interpreters but few provided regular staff training on equity. Only one-third systematically monitored their performance and few used the HEIA or other tools to assess impact of program practices or changes on disadvantaged groups, though it is provincially recommended. The survey results suggest that despite the focus on equity at a policy level, there is a lack of understanding of health equity among some programs, low use of equity promoting strategies and a lack of resources and support for this work.
Our findings align with a broad literature showing the challenge of translating policy into practice and the need for active and sustained efforts to achieve practice change (Torrey et al. 2012; Wyatt et al. 2016). Our findings also echo other Ontario work. Public Health Ontario investigated the use of health equity tools and similarly found that the absence of resources and a shared understanding of equity were barriers to the uptake of the tools. They found that incorporating equity indicators into performance reporting was an important facilitator of success (Tyler et al. 2014). In their Health Equity Plan (2016b), HQO highlighted the need to build capacity for health equity through education and knowledge exchange, and the importance of ongoing generation of both provincial and local data to better understand what is needed.
Based on these findings, we suggest two strategies to support the dual aims of more equitable access and more equitable care in Ontario EPI programs that may be feasible to implement.
First, although most programs reported they were serving all members of their communities, few are systematically collecting and reviewing information to understand who is and who is not accessing services. EPI and other programs need a deliberate strategy for routinely collecting demographic data on their service population and comparing to community profiles. Effective collection and use of data for quality monitoring is a common challenge in community programs (Mental Health and Addictions Leadership Advisory Council 2015) and selecting a specific issue to address may be a good starting point. Socio-demographic equity indicators are starting to be monitored in provincial and regional reporting (e.g., Health Quality Ontario 2016a, LHIN service accountability agreements), so the data that programs collect can be used to meet broader accountability reporting, and also create an opportunity for comparing and learning from each other.
Efforts to track program access may be supported by work that has been done by the Toronto Central LHIN to define a minimum set of key socio-demographic variables, supported by eight standardized questions, for monitoring access to service (Toronto Public Health et al. 2013). Collecting these data is currently required in the 17 Toronto Central LHIN hospitals and the standardized questions are being recommended for inclusion in the Ontario Common Assessment of Need, a province-wide assessment tool in community mental health programs. Providing training to front-line staff on the aims of health equity, the value of this information and strategies for asking sensitive questions will be key (Toronto Public Health et al. 2013).
Second, programs may need additional direction, training and field coaching/supervision support on how to serve diverse groups. Regional bodies, such as the LHINs, and sector-specific networks, such as the Early Psychosis Intervention Ontario Network, can collaborate to identify needs and provide supports. These efforts also may identify policy gaps around mandates and admission criteria for serving more vulnerable groups. For example, in our survey, some EPI programs indicated a lack of clarity on their role in supporting young adults with developmental disabilities. Although programs recognized the importance of ensuring equitable treatment for this population, they were unclear on whether and how this could be achieved in EPI programs and what their role was in relation to other parts of the system (e.g., the social services sector). Policies at the regional or provincial level on how to include more complex populations would offer programs guidance and create consistency across the province. That said, there will still be a need for local adaptation given regional population differences and the unique needs and resources of local communities.
A key strength of this study is the high response rate, providing full provincial representation for this sector. However, the study did not include the perspective of clients and families, or the experience of those who have not been able to access services. Future work could examine clients' and families' perceptions on whether the assessed strategies could lead to reduced barriers to access, or what else might be helpful. Follow-up work could also explore factors that contribute to some organizations making equity a priority and devoting resources to it. It should be noted that the survey was confidential but not anonymous and it is possible that programs may have inflated their responses, suggesting that use of equity strategies in practice may be even lower than reported.
Although equity is a core component of the EPI Standards and has been clearly endorsed in Ontario healthcare policy, few programs have been able to implement specific and purposeful equity approaches in practice. Similar challenges may exist in other health services. A more active implementation approach at front-line program levels, that includes better information about who programs are serving and strategies to improve care for identified vulnerable populations, is necessary to achieve an equitable healthcare system.
Sondage sur les pratiques d'équité en santé dans les programmes d'intervention précoce pour le traitement de la psychose: un point de départ pour l'amélioration
Résumé
L'équité a été désignée comme composante centrale de la qualité des services de santé en Ontario. Cependant, transposer les politiques en pratiques présente un défi. Cet article fait état des résultats d'un sondage provincial mené auprès des programmes d'intervention précoce dans le traitement de la psychose, et ce, afin d'évaluer dans quelle mesure l'équité fait partie de la mise en œuvre du programme. L'ensemble des 56 programmes (100 %) ont répondu au sondage. Les résultats montrent que bien que la plupart des programmes ont la perception qu'ils atteignent les cibles en matière d'équité, ils rapportent avoir peu recourt aux pratiques qui soutiennent cet objectif, et peu de programmes recueillent systématiquement des données sur le rendement. L'article discute des stratégies visant à améliorer la équité dans la pratique.
About the Author(s)
Avra Selick, MA, Research Coordinator, Provincial System Support Program, Centre for Addiction and Mental Health, Toronto, ON
Alexandra Lamoureux, MSW, RSW, Equity and Engagement Coordinator, Provincial System Support Program, Centre for Addiction and Mental Health, Toronto, ON
Karen O'Connor, MED, RSW, Senior Director, Clinical Programs and Strategic Planning, Canadian Mental Health Association, Peel Dufferin Branch, Brampton, ON
Janet Durbin, PHD, Independent Scientist, Provincial System Support Program, Centre for Addiction and Mental Health, Toronto, ON
Correspondence may be directed to: Avra Selick, Research Coordinator, Provincial System Support Program, Centre for Addiction and Mental Health, 33 Russell Street, Toronto, ON M5S 2S1; tel.: 416-535-8501, ext. 30127; e-mail: avra.selick@camh.ca
Acknowledgment
This study was funded by the Early Psychosis Intervention Ontario Network, which, along with the Standards Implementation Steering Committee, supported survey implementation and made the data available to the researchers. Thank you to the Ontario Early Psychosis Intervention programs for their participation in this survey.
References
Accessibility for Ontarians with Disabilities Act. 2005. S.O. 2005, c. 11.
Anderson, K.K., R. Fuhrer and A.K. Malla. 2010. "The Pathways to Mental Health Care of First Episode Patients: A Systematic Review." Psychological Medicine 40: 1585–97. doi:10.1017/S0033291710000371.
Bhui, K.A., A. Standsfeld, S. Hull, S. Priebe, F. Mole and G. Feder. 2003. "Ethnic Variations in Pathways to and Use of Specialist Mental Health Services in the UK: Systematic Review." British Journal of Psychiatry 182: 105–16. doi:10.1192/bjp.182.2.105.
Bird, V., P. Premkumar, T. Kendall, C. Wittington, J. Mitchell and E. Kuipers. 2010. "Early Intervention Services, Cognitive-Behavioural Therapy and Family Intervention in Early Psychosis: Systematic Review." British Journal of Psychiatry 197: 350–56. doi:10.1192/bjp.bp.109.074526.
Department of Health. 2001. The Mental Health Policy Implementation Guide. London, UK: Author.
Durbin, J., A. Selick, D. Hierlihy, S. Moss and C. Cheng. 2016. "A First Step in System Improvement: A Survey of Early Psychosis Intervention Programmes in Ontario." Early Intervention in Psychiatry 10: 485–93.
Excellent Care for All Act. 2010. S.O. 2010, c. 14.
Franz, L., T. Carter, A.S. Leiner, E. Bergner, N.J. Thompson and M.T. Compton. 2010. "Stigma and Treatment Delay in First-Episode Psychosis: A Grounded Theory Study." Early Intervention in Psychiatry 4: 47–56. doi: 10.1111/j.1751-7893.2009.00155.x.
French Language Services Act, R.S.O. 1990, c. F.32
Health Quality Ontario (HQO). 2016a. Measuring Up 2016: A Yearly Report on How Ontario's Health System Is Performing. Toronto, ON: Queen's Printer for Ontario.
Health Quality Ontario (HQO). 2016b. Health Quality Ontario's Health Equity Plan. Toronto, ON: Queen's Printer for Ontario.
Mental Health and Addictions Leadership Advisory Council. 2015. Better Mental Health Means Better Health: Annual Report of Ontario's Mental Health & Addictions Leadership Advisory Council. Retrieved July 7, 2017. <http://www.health.gov.on.ca/en/common/ministry/publications/reports/bmhmbh/mental_health_adv_council.pdf>.
Ministry of Health and Long-Term Care (MOHLTC). 2011. Ontario Early Psychosis Intervention Program Standards. Toronto, ON: Author. Retrieved July 7, 2017. <http://www.health.gov.on.ca/english/providers/pub/mental/epi_program_standards.pdf>.
Ministry of Health and Long-Term Care (MOHLTC). 2013. Health Equity Impact Assessment. Toronto, ON: Author. Retrieved July 7, 2017. <http://www.health.gov.on.ca/en/pro/programs/heia/>.
Mississauga Halton LHIN. 2016. Partnering for a Healthy Community: Integrated Health Service Plan 2016–2019. Retrieved November 1, 2017. <http://www.mississaugahaltonlhin.on.ca/goalsandachievements/ihsp.aspx>.
Ouellet-Plamondon, C., C. Rousseau, L. Nicole and A. Abdel-Baki. 2015. "Engaging Immigrants in Early Psychosis Treatment: A Clinical Challenge." Psychiatric Services 66(7): 757–59. doi:110.1176/appi.ps.201300284.
Registered Nurses' Association of Ontario. 2007. Embracing Cultural Diversity in Health Care: Developing Cultural Competence. Toronto, ON: Author.
Singh, S.P. and S.S. Kunar. 2010. "Cultural Diversity in Early Psychosis" In P. French, J. Smith, D. Shiers, M. Reed and M. Rayne, eds. Promoting Recovery in Early Psychosis: A Practice Manual. Oxford, UK: Wiley-Blackwell, pp. 66–72.
Toronto Central LHIN and Mount Sinai Hospital. 2016. Measuring Health Equity Project. Retrieved July 7, 2017. <http://www.mountsinai.on.ca/about_us/human-rights/measuring-health-equity>.
Toronto Public Health, St. Michael's Hospital, Centre for Addiction and Mental Health, Mount Sini Hospital. 2013. We Ask because We Care: The Tri-Hospital and TPH Health Equity Data Collection Research Project Report. Retrieved November 1, 2017. <http://www.stmichaelshospital.com/quality/equity-data-collection-report.pdf>.
Torrey, W.C., G.R. Bond, G.J. McHugo and K. Swain. 2012. "Evidence-Based Practice Implementation in Community Mental Health Settings: The Relative Importance of Key Domains of Implementation Activity." Administration and Policy in Mental Health 39: 353–64. doi:10.1007/s10488-011-0357-9.
Tyler, I., H. Amare, B. Hyndman and H. Manson; Ontario Agency for Health Protection and Promotion (Public Health Ontario). 2014. Health Equity Assessment: Facilitators and Barriers to Application of Health Equity Tools. Toronto, ON: Queen's Printer for Ontario.
Whitehead, M. 1992. "The Concepts and Principles of Equity and Health." International Journal of Health Services: Planning, Administration, Evaluation 22(3): 429–45.
Wyatt, R., M. Laderman, L. Botwinick, K. Mate and J. Whittington. 2016. Achieving Health Equity: A Guide for Health Care Organizations. IHI White Paper. Cambridge, MA: Institute for Healthcare Improvement.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed