Healthcare Quarterly
Utilization Management in Inpatient Psychiatry
Abstract
The purpose of this article is to outline a utilization management strategy for inpatient psychiatry that improves patient care, reduces the readmission rate and increases accessibility to limited beds/resources. This strategy will enhance the capacity of the inpatient team to meet the growing demand for their specialized services. It increases accountability for the use of limited resources and reduces unnecessary delays in service provision, while unifying a consistent treatment approach across the service.
Background
In the past, hospitals responded to increased demand for services by augmenting their budgets to meet that demand. However, as the demand for healthcare services grows, hospitals are left to initiate innovative methods to improve efficiency and measure corresponding outcomes objectively. Accountability is paramount. Anecdotal comments received at Peterborough Regional Health Centre included complaints regarding no access to inpatient beds, poor discharge planning and inconsistent treatment practices. There were also concerns in lag time for response to internal referrals and lack of coordinated teamwork. Many hospitals are turning to concurrent utilization management as a strategy to address issues, recommend changes and realize efficiencies.
Concurrent utilization management in the hospital sector is a relatively new phenomenon in Canada and can take many forms. Principally, utilization management strives to ensure that patients get the right service, in the right bed, at the right time based on their medical (clinical) needs. Our proactive management strategy monitors patients as they move through the hospital system. The strategy respects each patient's unique health problems and monitors the severity of the illness, the appropriate course of treatment and anticipates future needs by promoting sound discharge planning. It is individually based rather than by a diagnostic group or cluster. It enables a healthy balance between quality care and cost-effective (feasible) service delivery. This utilization strategy holds clinicians of all disciplines accountable and provides real-time information to support appropriate clinical/treatment decision-making and administrative program change.
To date, there is no published literature on the strategic introduction of concurrent utilization management in inpatient psychiatry. Published articles emphasize best practice, theoretical and clinical advancements and outcome studies of case mix groups (Durbin et al. 1993). The information in these articles must be incorporated into best practices in order to provide leading-edge treatment. Peer review journals are rich with research to enhance knowledge and understanding of every kind of health-related disorder. Peer review and retrospective data analysis demonstrate trends in treatment and measure outcomes of best practice techniques. These must not be ignored.
Kalant et al. (2000) describe a comparative analysis of three
concurrent utilization tools and their application as the sole
basis for deciding the appropriateness of days in hospital. Goldman
et al. (1997)studied the validity and reliability of available
utilization tools and found "few differences in the validity" of
the tools as they related to mental health.
Historically, efforts to improve efficiency relied upon
retrospective data analysis (Goel et al. 1996) and projected
benefits of new technology, medication and treatments. Our
concurrent utilization management strategy is a defined process in
which each patient's need for admission to acute care and the
subsequent treatment plan is critically appraised daily. It is then
compared to an objective tool for coding - InterQual ISD-AC
(1999).
There are a variety of utilization management tools (standards) available. However, for psychiatry the process is as equally important as the objective tool. Through the review process, the treatment team is encouraged to objectively evaluate the patient's condition and treatment plan. Additionally, the process would enable a systematic review and documentation of internal and external barriers to discharge and/or gaps in community services that would otherwise facilitate discharge.
Other utilization tools such as "clinical pathways" or "care maps" have been useful in standardizing procedural-based interventions with predictable recovery patterns (i.e., knee replacement surgery). Utilization improvements on inpatient psychiatric units have been thought to be significantly more difficult, as there is a subjective component to assessment and treatment of psychiatric disorders. The management team was committed to long-term change and clearly understood that investing in a good process with strategic forethought would lead to successful measurable outcomes.
Goal
The goal was to determine if a concurrent utilization management review process would improve access to limited inpatient psychiatric beds/resources, enhance patient care and reduce the need for readmission, while at the same time reduce the number of unnecessary delays in service and potentially avoidable days of care.Method
Introducing concurrent utilization management in inpatient psychiatry is a long-term process of change and may take two to three years of work before sustained change can be observed. The overall process can be divided into three distinct phases. First, there is a preliminary phase of organizing and gaining administrative and physician support for such a process. Second, data is compiled into a baseline report to show a realistic picture of the team's functioning and current utilization practices. Phase three is a proactive phase in which there is critical appraisal of the patient's need for admission, the treatment plan and the coordination of discharge planning.Preliminary Phase
In order for this concurrent utilization management strategy to succeed, appropriate resources and long-term support must be allocated. This requires administrative and medical buy-in and commitment. Our management team was prepared to back this process and commit itself to long-term change. The strategy was not expected to be a temporary solution. It was an investment in shifting and focusing the goals, purposes and processes of this acute care psychiatric unit.Full team participation was essential. As part of the strategy, "team building" meetings were conducted, and multidisciplinary ward rounds were modified to include all team members. A tone was set by the management team about everyone's responsibility to participate in improving the whole service. Resistance was anticipated and met with a neutral response that acknowledged that teamwork was more effective than isolated individual practice. All inpatient team members, including the psychiatrists, participate in reviewing all patients. This aspect of shifting the organization took six months of planning and meetings with the team. During this phase the InterQual ISD-AC tool was selected as the criteria set from which to work. The hospital was already licensed to use the tool, and it was therefore economical to proceed with this criteria system.
Resources were designated to recruit, train and support a full-time "Patient Resource Coordinator" (PRC) and a "Physician Reviewer" for inpatient psychiatry.
Baseline Phase
Phase two of this implementation strategy involved the PRC auditing each patient chart, collecting data and following patients through the inpatient service for three months. During this phase the PRC used the InterQual ISD-AC tool to determine the "Severity of Illness" of the patient, the "Intensity of Services" and the "Discharge Screen" based on information solely in the patient chart. Each inpatient chart was reviewed daily, and data were then reviewed regularly with the Physician Reviewer for final coding and designation. During this phase the PRC and the Physician Reviewer refined the use of the tool, developed a consistent interpretation of the tool and established a baseline framework from which to evaluate the effectiveness of the overall strategy. No proactive interventions were initiated during this period despite the inpatient team being aware of the process.This was also a time for the PRC to develop credibility on the unit as an integral part of the inpatient team. This was done in a non-threatening manner by demonstrating clinical knowledge and understanding of patient care and an appreciation of the current mental health system. It was important to be in tune to the interpersonal dynamics between the inpatient team members and respond in a neutral manner. Effective interpersonal skills of the PRC are essential.
Delays in response to internal turnaround times, such as social work and psychology referrals and other systemic delays, were noted, including physician discharge order delays. A "potentially avoidable day" of care was designated when the PRC and the Physician Reviewer determined there was evidence in the chart that the patient met the InterQual ISD-AC discharge criteria.
At the completion of the baseline phase, data were then aggregated and presented to the inpatient team for their information and reflection. The data were presented by the PRC and Physician Reviewer in a neutral fashion as "the facts" in terms of reflecting back to the team their current utilization practices. The data were met with a variety of anticipated responses, both positive and negative. Some responses were dismissive, while others wanted to argue with the validity of the data. Other team members left the meeting determined to change their current practice. The strategic action at this point was to remain neutral to these rebuttals and inform the team that these aspects of utilization would continue to be monitored in the proactive phase.
Proactive Phase
In this phase, the InterQual ISD-AC tool was used to audit patient charts on a daily basis as per the baseline phase. In the proactive phase, however, the PRC would ask pertinent team members informal questions of clarification based on the InterQual ISD-AC criteria system regarding the patient's progress and plan of care. Since documentation was critical in the process, staff and physicians were encouraged to be clear and concise regarding treatment progress and discharge plans. The PRC would identify patients who no longer met the criteria for acute care and/or those patients who were potential discharge challenges and would review these cases with the Physician Reviewer.At the multidisciplinary team ward rounds, open critical appraisal of the treatment plan was encouraged, and each discipline was invited to give its own assessment. Patients who no longer met the criteria for acute care were discussed openly in relation to their need for continued inpatient care. Clinical debates in a healthy format afforded team members of each discipline the opportunity to consult with colleagues and fellow team members. This type of critical appraisal and direct questioning would lead to more comprehensive assessments, clearly stated treatment plans and appropriate pre-discharge planning. Patients who required readmission would benefit from the whole team's input and the team would provide support and back-up. Psychiatrists would consult with each other regarding psychopharmacological interventions, and the nurses, social workers, occupational therapist and psychologists would participate in the development of the treatment plan.
The team began to function more effectively and cooperatively
with clear common goals. Turnaround time for internal referrals was
monitored, and new processes were introduced to enable social work
and psychology referrals to be processed more quickly and action
taken expediently. A greater sense of ownership developed as these
types of internal changes were generated and initiated and
implemented by the staff. The general culture on the unit began to
shift as individuals on the team responded to their personal
respon-
sibility as a team member.
Throughout this utilization strategy, it was clear to the team that the final decisions on clinical issues would be based on clinical judgment and not on the data generated with the InterQual ISD-AC tool. The InterQual ISD-AC criteria system does not usurp sound clinical decisions of the team members or direct the actual care of patients. Open, objective critical appraisal of each patient's treatment plan holds physicians and all team members accountable for their role in providing this specialized treatment.
Outcomes
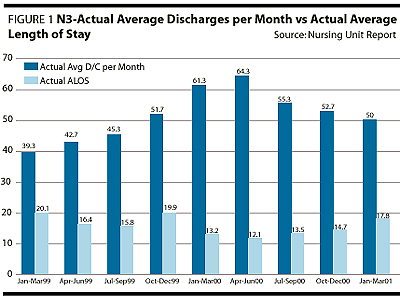
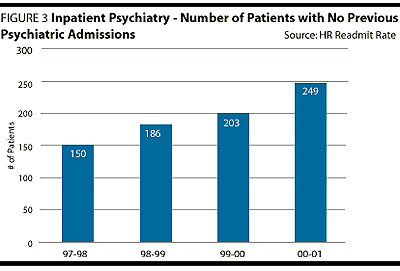
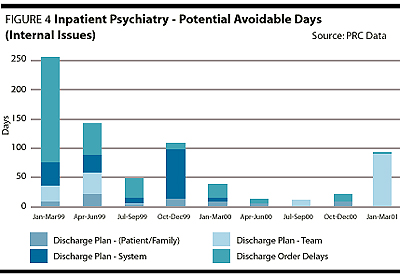
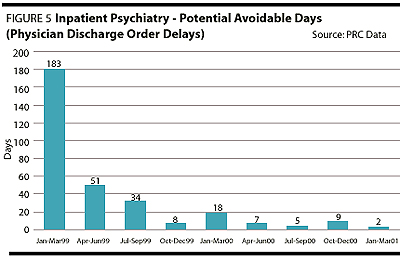
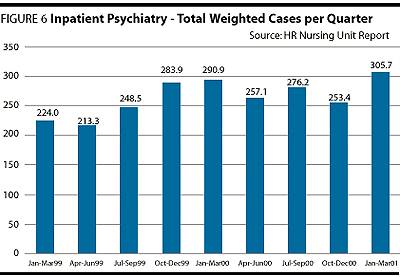
As a result of the concurrent utilization management strategy outlined, there have been rippling influences across the service. Subjectively, there is clear improvement in team collaboration, open dialogue about patient care and improvements in documentation regarding goals of each admission, daily progress and discharge planning. The team defines when a patient no longer requires an acute level of care, and there is greater collective accountability for the use of hospital resources.Objectively, there have been significant changes to note. The number of patient separations has increased (Figure 1), the average length of stay has been reduced by approximately three days (Figure 1), the readmission rate is lower (Figure 2) and the service is more accessible to new patients who have had no previous inpatient psychiatric history (Figure 3). There is also a significant drop in the number of "potential avoidable days" (Figure 4) and discharge order delays (Figure 5). The average RIW (Resource Intensity Weight) has not dramatically changed. More patients are being treated with essentially the same human and fiscal resources. The acuity level on the unit is higher as measured by the increase in "total weighted cases"(Figure 6).

Conclusion
This concurrent utilization management strategy impacts clinicians of all disciplines and holds each accountable for their contribution to patient treatment. Each admission and treatment plan is scrutinized and critically appraised, thus raising quality of care and setting consistent standards regarding stated goals and plan for admission and treatment. Clear and concise documentation on a daily basis assists the whole team. Discharge planning begins at the time of admission, and preplanned discharges are essential for successful discharges and to allow for appropriate follow-up to be arranged.The concurrent utilization management process maintains accountability to the patient and the organization for effective use of limited resources. A collective sense of responsibility is emphasized, and clinical necessity as the driving force behind patient length of stay is crucial. The intangible benefits of this process are many and include team collaboration and healthy collegial dialogue and discussion. This utilization management strategy will work for long-term change and help shift a culture of practice to include everyone's personal responsibility as a team member. It requires investment, commitment and patience. However, the payback will be tremendous. It is in the strategic process of introducing concurrent utilization management that achievable and sustainable results can be realized in inpatient psychiatry.
About the Author(s)
Mike VandenBroek, M.S.W. R.S.W. is the Patient Resource Coordinator - Mental Health Services at Peterborough Regional Health Centre.
Dr. F.G. McNestry, FRCP(C) is Medical Director - Mental Health Services, Chief of Psychiatry and a Physician Reviewer for Utilization at Peterborough Regional Health Centre.
Ann Dobby, R.N., B.Sc.N, M.Sc. Appl. is the Manager of the Inpatient Unit - Mental Health Services at Peterborough Regional Health Centre.
References
Durbin, J., P. Goering, G. Pink and M. Murray. 1993. "Classifying Psychiatric Inpatients: Seeking Better Measures." Medical Care 37(4): 415-23.
Goel, V., J. Williams, G. Anderson, P. Blackstien-Hirsh, C. Fooks and D. Naylor. 1996. "Patterns of Health Care in Ontario." The ICES Practice Atlas, 2nd ed. Ottawa: Canadian Medical Association.
Goldman, R.,C. Weir, C. Turner, and C. Smith. 1997. "Validity of Utilization Management Criteria for Psychiatry." American Journal of Psychiatry 154: 349-54.
InterQual ISD-AC. 1999. Marlborough (MA) Access Health Inc.
Kalant, N., M. Berlinguet, J. Diodati, L. Dragatakis and F. Marcotte. 2000. "How Valid Are Utilization Review Tools in Assessing Appropriate Use of Acute Care Beds." Canadian Medical Association Journal 162(13): 1809-25.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed

