Healthcare Quarterly
"What's In, What's Out": Stakeholders' Views About the Boundaries of Medicare
Abstract
The Canada Health Act requires that provincial insurance plans provide universal coverage without co-payments for all "medically necessary" services delivered by hospitals and doctors, but allows care delivered by other providers in other locations to fall outside of the boundaries of medicare. Discussion about the sustainability of medicare at both the national and provincial levels has called for the revisiting of these boundaries.
The M-THAC (Medicare to Home and Community) Research Unit attempted to clarify the areas of consensus and controversy as to what key stakeholders thought should be "in" or "out" of medicare. Using a non-experimental, cross-sectional design, a self-administered survey (in both English and French, constructed in consultation with our partners) was distributed between January and April 2002 to policy elites of key stakeholder groups. The results are based on 2,523 responses.
Much of the current "debate" is mired in discussing issues where consensus already exists. We found strong support for in-hospital care. However, there is considerable resistance, across all groups, to full funding for similar services in private clinics or in the home, and almost no support for full funding for non-medical home-based services. The vision of many policy elites remains heavily linked to the current system of guaranteed public funding only for acute care in hospitals or by physicians. Successful reform will need to address, rather than assume, a broader view of healthcare.
Introduction
Medicare is widely seen as the most popular Canadian social program, but there is increasing questioning of its sustainability (Alberta Association of Registered Nurses et al. 2000; Berger 1999; Brimacombe et al. 2001; British Columbia Medical Association 2000b; Canadian Healthcare Association 1999, 2001; Canadian Health Services Research Foundation 2001; Canadian Medical Association 2001a, b; Canadian Public Health Association 2001a, b; Commission on the Future of Health Care in Canada 2002b; Donelan et al. 1999; Ekos Research Associates Inc. 1998; Ferguson 2001; Haddad 2001; Hay Group 1999; Medical Reform Group of Ontario 2001; National Forum on Health 1997a, b; Premier's Advisory Council on Health for Alberta 2001; Premier's Health Quality Council 2001; Quebec commission d'étude sur les services de santé et les services sociaux 2000; Rachlis et al. 2001; Stabile 2001). As the debate about the sustainability of medicare heightens, observers at both the national (Canadian Health Services Research Foundation 2002; Commission on the Future of Health Care in Canada 2002a; Flood and Choudhry 2002; Maxwell et al. 2002; Ramsay 2002; Shiell and Mooney 2002; Standing Senate Committee on Social Affairs, Science and Technology 2002a) and the provincial level (Armstrong 2002; British Columbia Medical Association 2000a; Premier's Advisory Council on Health for Alberta 2001; Quebec commission d'étude sur les services de santé et les services sociaux 2000) have called for updating the determination of what should be "in" or "out" of medicare. This debate has largely been based on rhetoric rather than on evidence. To help clarify the debate, the M-THAC (Medicare to Home and Community) Research Unit and its research partners undertook a national survey of policy elites from key stakeholder groups. Discovering areas of agreement may enable us to identify where we are ready to move beyond discussion to action. Areas of controversy, in contrast, require ascertaining the rationale for the contending views and seeing whether consensus may then be reached.
This paper presents the views of 2,523 policy elites, from across Canada on what should be "in" and "out" of the publicly funded system. The paper starts with a brief description of the M-THAC survey, presents the views of the policy elites and concludes with a discussion on the potential policy implications of the findings.
M-THAC Survey: Views on the Boundaries of Medicare
Using a non-experimental, cross-sectional design, the self-administered questionnaire was constructed in consultation with our research partners. As well, the sample was developed with the assistance of our research partners who identified individuals who met the sampling criteria. A complete list of the organizations/associations that participated in the survey is in the acknowledgement section of this paper.
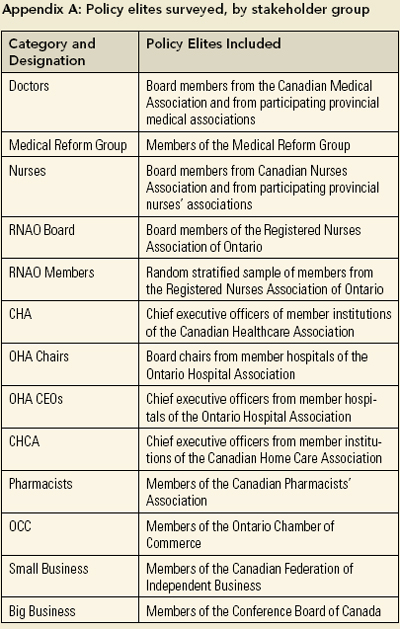
The questionnaire was distributed between January 2002 and April 2002 to policy elites from knowledgeable stakeholder groups involved in health policy discussions, either as providers or as businesses (who are often asked to pay the bills, both as taxpayers and as providers of employee benefits). We surveyed physicians (Canadian Medical Association, collaborating provincial medical associations and the Medical Reform Group), nurses (Canadian Nurses Association and collaborating provincial nurses' associations), hospital/health authorities (Canadian Healthcare Association and the Ontario Hospital Association), home care providers (Canadian Home Care Association), pharmacists (Canadian Pharmacists Association) and business (Conference Board of Canada, Canadian Federation of Independent Business and Ontario Chamber of Commerce). A complete list of who was included (by stakeholder group) is found in Appendix A. The policy elites include groups expected to be supportive (e.g., providers paid by the current system), plus those that are potentially suspicious of the government's role (e.g., business). The survey did not include the general public, because it was thought that too many questions were at a level of detail unlikely to be answerable by "lay persons" within the format of a mailed survey.
Timing of the questionnaire allowed the findings to be sent to the Romanow Commission and the Standing Senate Committee on Social Affairs, Science and Technology (the Kirby report).
The 12-page survey (available in English and French) included items about overall sustainability issues. This paper focuses on responses to a detailed question asking for views on coverage for a list of 48 potential services. We begin with the premise that there is no "right" answer, and that individuals may differ in their views about which costs should be "socialized." However, clarifying where consensus does or does not exist may assist in developing policies that can be implemented. We are employing the general framework of the "rational political model" (Wiktorowicz and Deber 1997), which stresses the importance of facts (the extent to which particular policy options are likely to achieve particular policy goals), values (the extent to which particular stakeholders support the policy goals) and institutions (the importance of the stakeholders in the given policy process). This paper contributes information to the values matrix, clarifying support for funding particular services. Respondents were accordingly asked whether each potential service should be:
Universal- falling under the same terms as the Canada Health Act; no user fees to insured persons
Partial coverage- public payment on a sliding scale only for those who cannot afford it, with others paying some or all of the cost, depending upon their incomes
Subsidized - partial public payment on another, non-means tested basis, such as capped payments with user fees allowed
Not included- no public payment; those who want it and/or their insurers pay the full cost themselves
Results
Currently, under the terms of the Canada Health Act (Government of Canada 1984), all medically necessary services delivered in hospitals and by physicians are guaranteed universal coverage with no co-payment. In addition to these insured services, provinces and territories opt to publicly insure additional services (prescription drugs, home-based nursing, etc.) but are not required to do so.
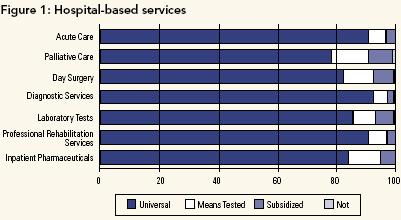
Hospital-Based Services
Hospital services still represent the largest category of total health expenditures (at about 32%) (Canadian Institute for Health Information 2002), but this share has fallen dramatically over the last 25 years. As Figure 1 demonstrates, there was overwhelming support across all groups for the continuation of full public payment for insured hospital services, which include: acute hospital care; palliative care in institutions; day surgery in hospitals; diagnostic services in hospitals; laboratory tests in hospitals; professional rehabilitation services in hospitals; in-patient pharmaceuticals.
We conclude that further debate on covering currently insured hospital-based services seems somewhat misplaced; all groups surveyed, including business, agreed that hospital services should continue to be "in" medicare.
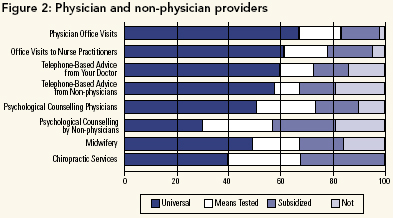
Physician and Non-Physician Providers
Physician services are also guaranteed full coverage under the Canada Health Act, and currently 99% of physician services are financed by the public sector. However, the views about public coverage for such insured medical services were more mixed than was the case for insured hospital services (see Figure 2). Several points are evident. First, the results revealed some support for allowing co-payments by insured persons, along with strong opposition to this idea from others. There were differences between respondent groups (data not shown), with stronger support for universal coverage of services among the groups on the "reform" side of the political spectrum (including nurses, home care organizations, Medical Reform Group), as well as by groups that offer a particular service and would like to ensure public payment. Second, with the exception of physicians, most groups did not distinguish between physician and non-physician providers for such services as office visits to nurse practitioners, telephone-based advice from non-physicians and midwifery.
When considering health reform, it is worth noting that services provided by non-physician providers in hospitals (e.g., nurses) are generally paid for from public funds through hospital budgets. Our respondents support continued public payment for hospital services, and so this would not change. However, much of this care can now be delivered outside hospital walls. Because services provided by non-physician providers (e.g., nurse practitioners) outside of the hospital setting are not required to be insured under the terms of the Canada Health Act, these shifts can result in the de-insuring of many services now covered by medicare.
One striking example is the role of mental health within the publicly funded system. Much of this care had been delivered within provincial psychiatric hospitals. As care shifted to the community, mental health has often fallen through the cracks. Some provinces will pay for psychological counselling by physicians, but most do not cover mental healthcare by psychologists or other non-physician providers. Among our respondents, only 51% wished full coverage for psychological counselling by physicians; this dropped to 30% if the service was performed by non-physicians. At the same time, it is becoming clear that untreated or under-treated mental health problems are major causes of mortality and morbidity, and various studies have repeatedly called for improvements (World Health Organization, 2001b; Global Business and Economic Roundtable on Addiction and Mental Health 2004). Our results suggest that the place of mental health needs urgent discussion and clarification as to the rationale among a sizeable proportion of providers for opposing such coverage.
Certain Services Currently out of Medicare
Medicine is not static, and innovation must be dealt with. We asked about certain services, not required to be funded, which could be categorized as either innovative or elective/unproven.
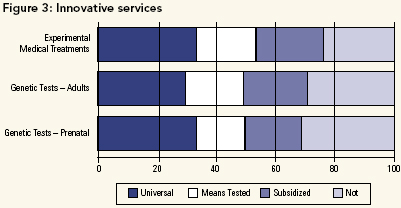
Innovative Services
As shown in Figure 3, there was some support for having a mechanism to include: experimental medical treatments; genetic test for adults (disease propensities); genetic test for prenatal screening. As technology advances, it seems essential to retain some flexibility in the ability to move these services "in" once they are deemed "medically necessary." Presumably, although we did not ask specifically, decisions about inclusion could be linked with evidence-based decision-making and other forms of technology assessment.
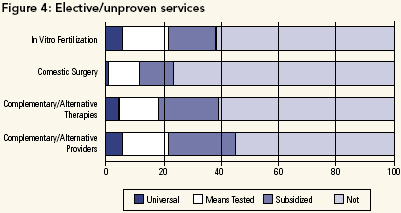
Elective/Unproven Services
In contrast, there was very little support for fully funding a second group of services characterized as either elective (i.e., medical, but voluntary) or unproven, which include: in vitro fertilization; cosmetic surgery; complementary/alternative therapies; complementary/alternative providers (see Figure 4). However, a significant minority did support partial coverage for these services. We interpret this as highlighting the tension between a "consumer-driven" and an "evidence-based" approach to determining public payment.
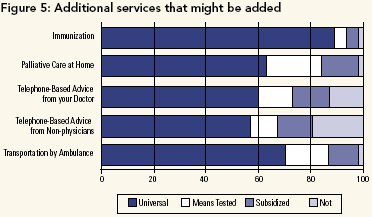
Additional Services That Might Be Added
There was fairly strong support for extending full public payment to certain services that are not currently required to be insured, which include: immunizations (e.g., polio, mumps, measles); palliative care at home; telephone-based advice from doctor(s); telephone-based advice from non-physician provider; transportation by ambulance for emergency care (see Figure 5). Little distinction was made between having telephone-based services provided by physicians and non-physicians. The Romanow (Commission on the Future of Health Care in Canada 2002) and Kirby (Standing Senate Committee on Social Affairs, Science and Technology 2002b) reports proposed incorporating immunizations, palliative care and telephone-based services into the basket of services. To the extent that regionalization is consolidating services into centres of excellence, many Canadians are faced with increased travel distances. Although transportation was identified by our respondents as a candidate for public funding, this has not yet reached the political agenda, and did not figure in the Kirby or Romanow reports.
More recently, the 2004 Federal Budget included funds to pay for nationwide immunization and for the Canada Health Infoway, which is supporting a variety of efforts to use technology to improve access to care (Department of Finance Canada 2004).
Thus, there appears to be some justification for moving debate into action and incorporating these services into the medicare basket of services.
Site of Care Matters
As noted above, the Canada Health Actcurrently guarantees universal coverage with no co-payment for all medically necessary services delivered in hospitals but does not extend this same guarantee to these same services delivered outside of the hospital walls. Health reformers often argue that these services should be treated in the same way, regardless of where they are located (National Forum on Health 1995). However, the results supported the view that the site of care matters when it comes to views about full public payment. We asked about provision of a number of the same services (day surgery, diagnostic services, laboratory tests, professional rehabilitation) in different locations: hospital (Figure 1) and private clinics.
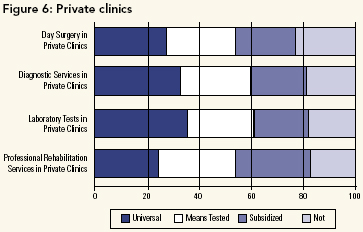
Private Clinics
Support for full public payment drops sharply when we ask about delivery in a private clinic (Figure 6). Compared to responses for the same services within hospitals (Figure 1), there was stronger support for some form of co-payment for these services; indeed, approximately 20% of the respondents indicated that they did not think private clinics should receive any public payment.
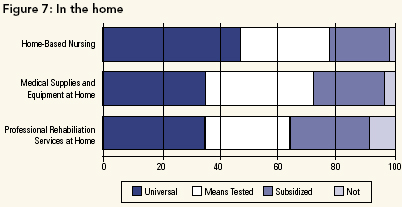
In the Home
We also asked about home-based delivery of several services that would be paid for if delivered in hospital - nursing, medical supplies/equipment and professional rehabilitation services (see Figure 7). Unlike the views on services delivered in private clinics, most respondents wished to ensure at least partial public payment for such services, even when delivered in the home. However, there was support for some form of co-payment at home, but not in the hospital. (See Figure 1 and Figure 7.)
Drug Coverage
Pharmaceuticals are a large and growing sector of healthcare. Currently, pharmaceutical costs (at 14.9% of total health expenditures now exceed costs for physician services (at 13.6%) (Canadian Institute for Health Information 2002). Again, the Canada Health Act requires full coverage for prescription drugs only if these are given in hospital. Figure 8 demonstrates that the majority of respondents support full public payment for in-patient prescription drugs but not for out patient prescription drugs. Support does exist for limited coverage of out patient prescription drugs, which is compatible with the recommendations made in the Romanow Commission's final report (Commission on the Future of Health Care in Canada 2002) and the Kirby report (Standing Senate Committee on Social Affairs, Science and Technology 2002b). There is little support for non-prescription drugs (on the same order as support for CAM), although there is some "consumer-driven" support for partial coverage. (See Figure 8.)
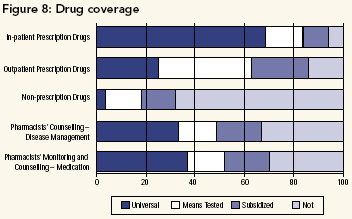
The issue of where pharmacists fit into the healthcare system was also very contentious. There is some support for seeing pharmacists as health professionals, with responsibility for better disease management and monitoring/ counselling (re medication). However, a minority of respondents support fully funding this role, although many appear willing to see at least partial payment. Further debate is clearly needed about the role of pharmacists: Are they private business people or healthcare team members?
Support for Long-Term Services
Individuals do not require only acute care. We asked about services offered on a long-term basis (e.g., institutional care) and about prevention/maintenance services often used to support individuals in their homes (see Figure 9). Our respondents felt that such services differed from those being fully funded under Canada Health Act terms and conditions. Overall, the consensus was that long-term care in institutions and home-based personal support services should involve user fees, although some groups (e.g., nurses and the Medical Reform Group) supported full public coverage. It is noteworthy that patterns of support for funding institutional care in long-term care facilities closely resembles views on paying for home-based personal support services; respondents feel that costs should be shared between the public and recipients of care. Similar patterns are evident for homemaking, supportive housing, community support (e.g., meals on wheels), adult day programs, transportation to receive care at an out-of-region centre, respite support for family caregiver and stipends to family caregiver, with variations in how respondents wish to balance public and private funding. Indeed, for some of the more social services, a sizeable minority rejects any public role, and very few wish full public payment. (See Figure 9.)
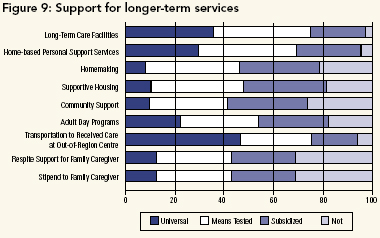
These results support the decision by policy-makers not to try to include these services within medicare, but to seek parallel programs with different terms and conditions. It is worth noting that the federal government has already acted on implementing some caregiver support; starting January 2004 (Department of Finance Canada 2003) an employment insurance compassionate family care leave benefit will entitle eligible individuals to care for their "gravely ill or dying child, parent or spouse" while receiving employment insurance benefits, assuming that provincial/territorial governments agree. Certain provincial governments are also examining home supports and expanding nursing home capacity.
Disease Prevention Services
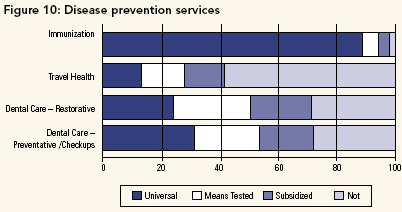
It has been recognized both nationally (Commission on the Future of Health Care in Canada 2002; National Forum on Health 1997b; Standing Senate Committee on Social Affairs, Science and Technology 2002b) and internationally (Glouberman 2001; World Health Organization 1984, 2001a) that measures such as disease prevention contribute greatly to health and well-being. (We did not ask about health promotion in this question.) Within healthcare, there was strong support for immunizations, but not for travel health (possibly on the grounds that those who could afford foreign travel could pay their own way) (see Figure 10). There was also minimal support for expanding support to dental services, for either restorative work (e.g., fillings) or prevention/checkups. One might argue that a number of these decisions exemplify "penny wise/pound foolish" policy making. Poor dental health is associated with considerable morbidity and may lead to other diseases (Health Canada 2004). The travel health decision seems even harder to defend, since imported diseases can be extremely expensive to Canadians.
Policy Implications of Our Findings
Many different factors influence the direction of healthcare reform including economic factors (the need to be more cost-effective), technological and pharmaceutical advancements (allowing for less invasive treatment outside of institutions), fiscal concerns (balancing budgets and the decisions how best to allocate funds among both governmental priorities in general and between healthcare priorities specifically) and political factors (the distribution of power and who gets to decide). For many others, healthcare policy has spoken to the need to shift from hospital-based care to the delivery of care in the community and the home.
An ongoing dilemma is why this shift in care has been so difficult to achieve. Although bed numbers have dropped (Canadian Institute for Health Information and Statistics Canada 2001), pressure on hospitals has remained intense. Our results demonstrated one potential reason why - the vision of many policy elites is still heavily linked to the current system of acute care delivery in hospitals by physicians. This cannot fully be written off to "vested interests." Clearly, healthcare providers believe that the services they offer are important and wish to ensure that they are funded. Yet, this belief does not necessarily translate into a desire for universal public funding. Indeed, to the extent that government controls costs, it may translate into a desire for allowing user charges; a proportion of our respondents tended to support such co-payments for physician and other ambulatory services. In addition, respondents gave answers for a list of 48 services, most of which would not be provided by their group. In addition, the business respondents were not providers at all, although they might be expected to pay for some care not provided universally.
The extent of consensus was accordingly striking. We found strong support for in-hospital care and resistance, across all groups, to similar services in private clinics. In addition, there is almost no support for full funding for home-based services, particularly if these involve non-medical care. It appears that this preference incorporated both the privileged character of hospital-based care (since support was lower for similar services at home or in private clinics), as well as the ongoing controversy about the advantages and disadvantages of for-profit delivery (Deber 2004).
What this survey has brought to the foreground is a discrepancy between current policy directions and the views of policy elites, including health providers and business. It is well recognized that, as technology enables care to shift from hospitals to home and community, "passive privatization" can result. To that end, both Romanow and Kirby have called for ensuring that coverage follows services, rather than location. However, a large proportion of our respondents do not fully agree. This may explain why reform has largely "stalled," as implementation has moved to expert panels and other consultation mechanisms, and away from the views of the public and experts, as solicited by the Romanow and Kirby processes.
Much of the current "debate" is mired in discussing issues where consensus already exists. In our view, the debate of what should be "in" and "out" of medicare needs to move on. Our findings suggest the need to examine and clarify areas where disagreement is evident. However, it also identifies areas where paths are clear and action is overdue.
About the Author(s)
Raisa B. Deber, PhD, is a professor in the Department of Health Policy, Management and Evaluation in the Faculty of Medicine at the University of Toronto.
Brenda J. Gamble, MSc, is a PhD candidate at the Institute of Medical Sciences in the Faculty of Medicine at the University of Toronto. Currently she is a part-time instructor at the School of Health Services Management at Ryerson University, Toronto.
Please direct correspondence to: Brenda Gamble, M-THAC Research Unit, Faculty of Medicine, University of Toronto, Department of Health Policy, Management and Evaluation, McMurrich Bldg, 2nd floor, 12 Queen's Park Cres. W., Toronto, ON M5B 1A8. Tel. 416-978-1406; Fax 416-978-7350; e-mail brenda.gamble@utoronto.ca
Acknowledgment
Previously published in Longwoods Review 2(4), 2004.Funding and support for this research project was provided by the M-THAC (Medicare to Home and Community) Research Unit and the project's partner organizations/associations. The M-THAC Research Unit brings together community partners and a wide variety of academic researchers from an eclectic assortment of disciplines to focus on the policy implications of the shift to home and community. M-THAC is funded by the Canadian Institutes of Health Research (CIHR). We would like to thank our co-investigators, Earl Berger and A. Paul Williams, for invaluable advice; any errors cannot be attributed to them. Cathy Bezic, Ann Pendleton and Jenny McInnes assisted with questionnaire distribution and data entry. We would particularly like to thank our research partners, who assisted us in identifying the sampling frame, encouraging responses, and partially funding questionnaire distribution: Canadian Medical Association; Newfoundland and Labrador Medical Association; Medical Society of Prince Edward Island; L'Association médicale du Québec; Saskatchewan Medical Association; Alberta Medical Association; British Columbia Medical Association; Yukon Medical Association; Canadian Nurses Association; Registered Nurses Association of British Columbia; Alberta Association of Registered Nurses; Registered Nurses Association of Ontario; Ordre des infirmières et infirmiers du Québec; Nurses Association of New Brunswick; Association of Nurses of Prince Edward Island; Yukon Registered Nurses Association; Canadian Pharmacists Association; Conference Board of Canada; Canadian Federation of Independent Business; Ontario Chamber of Commerce; Medical Reform Group; Canadian Home Care Association; Canadian Healthcare Association; and Ontario Hospital Association.
References
Alberta Association of Registered Nurses, Canadian Nurses Association, Ontario Nurses' Association, Registered Nurses Association of Ontario and United Nurses of Alberta. 2000. Towards a Sustainable, Universally Accessible Health-Care System: A Discussion Paper Prepared for the National Nursing Forum. May.
Armstrong, W. 2002. Jumping on the Alberta Bandwagon: Does B.C. Need This Kind of Assisted Living? Report published by the Consumers' Association of Canada.
Berger, E. 1999. The Berger Population Health Monitor: Policy Report Survey #20. With the Hay Health Care Consulting Group, October Survey.
Brimacombe, G.G., P. Antunes and J. McIntyre. 2001. The Future Cost of Health Care in Canada - 2000 to 2020: Affordability and Sustainability. Ottawa: Conference Board of Canada. May.
British Columbia Medical Association. 2000a. Establishing "Medically Required" and Core Services. Vancouver, BC: British Columbia Medical Association. April.
British Columbia Medical Association. 2000b. Turning the Tide - Saving Medicare for Canadians: Part II of II, a New Course for Health Care. Vancouver, BC: BCMA. A Discussion paper by BC's Physicians. May.
Canadian Healthcare Association. 1999. Framework for a Sustainable Healthcare System in Canada. Discussion paper. November. Retrieved June 2, 2004. < http://www.canadian-healthcare.org >.
Canadian Healthcare Association. 2001. A Responsive, Sustainable, Publicly Funded Health System in Canada: The Art of the Possible. Submission to the Romanow Commission on the Future of Health Care in Canada. October.
Canadian Health Services Research Foundation. 2001. "Myth: The Aging Population Will Overwhelm the Healthcare System."
Canadian Health Services Research Foundation. 2002. Medically Necessary: What Is It, and Who Decides? Ottawa: Commission on the Future of Health Care in Canada. Issue/survey paper prepared for the Commission on the Future of Health Care in Canada. July.
Canadian Institute for Health Information. 2002. National Health Expenditure Trends, 1975-2002. National Health Expenditure Database.
Canadian Institute for Health Information and Statistics Canada. 2001. Health Care in Canada. Ottawa: Statistics Canada. Retrieved 2001. < http://www.cihi.ca >.
Canadian Medical Association. 2001a. Getting the Diagnosis Right. Toward A Sustainable Future for Canadian Health Care Policy. Part One of a two-part brief to the Royal Commission on the Future of Health Care in Canada.
Canadian Medical Association. 2001b. In Search of Sustainability: Prospects for Canada's Health Care System. Discussion document. Retrieved June 2, 2004. < http://www.cma.ca >.
Canadian Public Health Association. 2001a. Creating Conditions for Health. Ottawa: Submitted to the Commission on the Future of Health Care in Canada. October.
Canadian Public Health Association. 2001b. The Future of Public Health in Canada. Ottawa: Board of Directors discussion paper. October.
Commission on the Future of Health Care in Canada. 2002a. Interim Report: Shape of the Future of Health Care. February.
Commission on the Future of Health Care in Canada. 2002b. Sustainability of Canada's Healthcare System. Policy Dialogue No. 8. University of Toronto. September 11.
Commission on the Future of Health Care in Canada (Roy J. Romanow, Commissioner). 2002. Building on Values: The Future of Health Care in Canada: Final Report. Ottawa: Queen's Printer.
Deber, R.B. 2004. "Delivering Health Care: Public, Not-for-Profit, or Private?" In G.P. Marchildon, T. McIntosh and P.-G. Forest, eds., The Fiscal Sustainability of Health Care in Canada (pp. 233-96). Toronto: University of Toronto Press.
Department of Finance Canada. 2003. Building the Canada We Want: The Budget in Brief 2003. Ottawa.
Department of Finance Canada. 2004. Budget 2004. Ottawa.
Donelan, K., R.J. Blendon, C. Schoen, K. Davis and K. Binns. 1999. "The Cost of Health System Change: Public Discontent in Five Nations." Health Affairs 18: 206-16.
Ekos Research Associates Inc. 1998. Rethinking Government IV. Presentation to the National Conference on Home Care. March 9.
Ferguson, B.S. 2001. Expenditure on Medical Care in Canada: Looking at the Numbers. Working paper prepared for the Atlantic Institute for Market Studies healthcare project Health Care's Hidden Face.
Flood, C.M. and S. Choudhry. 2002. Strengthening the Foundations: Modernizing the Canada Health Act. Discussion Paper No. 13. Commission on the Future of Health Care in Canada.
Global Business and Economic Roundtable on Addiction and Mental Health. 2004. Retrieved March 26, 2004. < http://www.mentalhealthroundtable.ca/aboutus.html >.
Glouberman, S. 2001. Towards a New Perspective on Health Policy. CPRN Study No. H/03. Ottawa, Ontario.
Government of Canada. 1984. Canada Health Act, Bill C-3. Statutes of Canada, 1984, 32-33 Elizabeth II (R.S.C. 1985, c. 6; R.S.C. 1989, c. C-6).
Haddad, H. 2001. Getting the Diagnosis Right: Toward a Sustainable Future for Canadian Health Care Policy. Part One of a two-part brief to the Royal Commission on the Future of Health Care in Canada by the Canadian Medical Association.
Hay Group. 1999. Public Behaviour, Perceptions and Priorities in the Health Sector: An Overview. The Health Services Restructuring Commission. January 14.
Health Canada. 2004. The Effects of Oral Health on Overall Health. It's Your Health. Retrieved May 16, 2004. < http://www.healthcanada.ca/iyh >.
Maxwell, J., K. Jackson, B. Legowski, S. Rosell, D. Yankelovich, P.-G. Forest and L. Lozowchuk. 2002. Report on Citizens' Dialogue on the Future of Health Care in Canada. Prepared for the Commission on the Future of Health Care in Canada. June.
Medical Reform Group of Ontario. 2001. Brief submitted to the Romanow Commission. October 26.
National Forum on Health. 1995. The Public and Private Financing of Canada's Health System. Ottawa: National Forum on Health, discussion paper.
National Forum on Health. 1997a. Canada Health Action: Building on the Legacy: Synthesis Reports and Issues Papers. (Vol. 2). Ottawa: National Forum on Health.
National Forum on Health. 1997b. Canada Health Action: Building on the Legacy: The Final Report of the National Forum on Health. (Vol. 1). Ottawa: National Forum on Health.
Premier's Advisory Council on Health for Alberta. 2001. A Framework for Reform. Report of the Premier's Advisory Council on Health. December.
Premier's Health Quality Council. 2001. Health Renewal - A Discussion Paper. New Brunswick. < www.gnb.ca >.
Quebec commission d'étude sur les services de santé et les services sociaux. 2000. Emerging Solutions: Report and Recommendations.
Rachlis, M., R.G. Evans, P. Lewis and M.L. Barer. 2001. Revitalizing Medicare: Shared Problems, Public Solutions. Vancouver: Tommy Douglas Research Institute. January.
Ramsay, C. 2002. A Framework for Determining the Extent of Public Financing of Programs and Services. Commission on the Future of Health Care in Canada, Discussion Paper No.16. August.
Shiell, A. and G. Mooney. 2002. A Framework for Determining the Extent of Public Financing of Programs and Services. Commission on the Future of Health Care in Canada, Discussion Paper No.6. July.
Stabile, M. 2001. Options for Health Care Reform in Ontario. Toronto: Ontario Hospital Association. December.
Standing Senate Committee on Social Affairs, Science and Technology. 2002a. The Health of Canadians: The Federal Role: Volume Four: Issues and Options. Interim report on the state of the healthcare system in Canada.
Standing Senate Committee on Social Affairs, Science and Technology. 2002b. The Health of Canadians: The Federal Role: Volume Six: Recommendations for Reform. Final report on the state of the healthcare system in Canada. October.
Wiktorowicz, M. and R.B. Deber. 1997. "Regulating Biotechnology: A Rational-Political Model of Policy Development." Health Policy 40: 115-38.
World Health Organization. 1984. Health Promotion: A Discussion Document on the Concept and Principles. Copenhagen: WHO Regional Office for Europe.
World Health Organization. 2001a. "Responsiveness: Level and Distribution." In World Health Organization, eds., Report of the Scientific Peer Review Group on Health Systems Performance Assessment (pp. 71-82). Copenhagen: World Health Organization.
World Health Organization. 2001b. The World Health Report 2001: Mental Health: New Understanding, New Hope. Geneva, Switzerland: World Health Organization.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed

