Healthcare Quarterly
CIHI Survey: Waiting in the Emergency Department for an In-Patient Bed: Variations by Hospital Type, Season and Day
Abstract
More than one million Canadians are admitted to hospitals each year via emergency departments (EDs). The time that admitted patients waited in the ED for an in-patient bed following the decision to admit them is influenced by many factors including in-patient bed capacity, the size and staffing of EDs and hospitals, hospital operational patterns and changes in the demand for hospital services (Bagust et al. 1999; Chan et al. 2001; Forster et al. 2003; Rathlev et al. 2007). Based on analyses included in Understanding Emergency Wait Times: Access to Inpatient Beds and Patient Flow by the Canadian Institute for Health Information (CIHI 2007), this article provides information on how long patients waited for a bed in large community and teaching hospitals. It also highlights variations by season and day of the week.
Data Sources and Methods
The analyses presented in this article were based on a sample of 58 large community and teaching hospitals in Canada. Admissions from these 58 hospitals account for 39% of all admissions via the ED in Canada (outside Quebec). Hospitals were identified as large community hospitals (those with 200 or more acute care beds, n = 34) and teaching hospitals (n = 24) based on CIHI's Comparison of Hospital Activity Program peer groups. The data were obtained from CIHI's Discharge Abstract Database for patients who were admitted via the ED to an in-patient acute care bed in the same hospital, in 2005. This analysis focuses on large community and teaching hospitals, where ED wait times tend to be the longest.
Bed Wait Time by Hospital Type
Half of the patients who were admitted via the ED to large community and teaching hospitals waited 2.2 hours or less to access an in-patient bed once the decision to admit them from the ED had been made (Table 1). There was variation in bed wait times in the ED between individual hospitals, with median bed wait times in the ED ranging from zero to 4.8 hours for these hospitals.
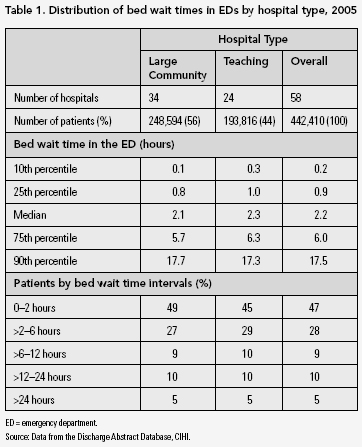
Ten percent of patients (with the shortest bed wait times in the ED) waited less than 11 minutes to access an acute care bed. In contrast, 10% of patients (90th percentile) with the longest bed wait times in the ED had a wait time of more than 17 hours, with a range of 1.9-44 hours among individual hospitals. Five percent of patients waited over 24 hours.
Bed Wait Time by Season
Hospitals are typically busier during fall and winter but see fewer patients during the summer. Researchers suggest a number of potential reasons for this phenomenon, including that admissions due to cardiovascular or respiratory conditions (e.g., influenza) tend to peak during fall and winter (Frost et al. 2002; Fullerton and Crawford 1999; Menec et al. 1999). In contrast, they found that during the summer months, elective admissions may be reduced because of staff scheduling and other factors that may affect the number of beds staffed and available.
Bed wait times in the ED also show seasonal patterns. For example, the 90th percentile for bed wait times in the ED were longer during the winter months (20.4 hours, 21.5 hours and 20 hours in the months of January, February and March) and shortest during summer months (14.1 hours in July and August and 14.5 hours in September) (Figure 1).
Bed Wait Time by Day of Week
Studies have shown that ED wait times and patient volume fluctuate throughout the week (Fatovich et al. 2005; Physician Hospital Care Committee 2006; Proudlove et al. 2003; Schull et al. 2002). This research suggests that these patterns may be influenced by the availability of resources to meet the demand for in-patient beds via the ED and the coordination of hospital operations in relation to emergency and elective admissions and discharge.
Based on our analysis, the median bed wait times in the ED during 2005 tended to be shorter on weekends than weekdays. When a decision to admit occurred on Saturday or Sunday, 50% of patients waited two hours or less, while at mid-week the median bed wait time in the ED was longer (2.4 hours). We observed slightly different patterns for the 90th percentile, with the shortest wait times on Fridays and Saturdays (14.5 and 15.7 hours, respectively) (Figure 2).
Conclusion
Given the variation in ED wait times among the hospitals, there may be opportunities for some hospitals to improve their coordination and planning for the demand for the in-patient beds. This may include better allocation of resources during the busiest months and days of the week.
About the Author(s)
Greg Webster, MSc, is director of research and indicator development at CIHI. In this role, he is responsible for providing vision, leadership and direction for CIHI's health services research, health indicator, hospital standardized mortality ratio and primary healthcare programs.
Heather Dawson, MHA, is manager of health services research at CIHI. In this role, she oversees the development and production of health services research initiatives and analytic reports. She has previously worked in leadership roles in hospitals and health planning and advocacy organizations in Ontario.
Raymond Przybysz, MSc, is project lead of health services research at CIHI. He is responsible for coordination and implementation of project plans and provides support in the field of analytical methods and research techniques. He has previously worked with several research institutes in Ontario and Quebec.
References
Bagust, A., M. Place and J.W. Posnett. 1999. "Dynamics of Bed Use in Accommodating Emergency Admissions: Stochastic Simulation Model." BMJ 319(7203): 155-8.
Canadian Institute for Health Information. 2007. Understanding Emergency Department Wait Times: Access to Inpatient Beds and Patient Flow. Ottawa: Author.
Chan, B., M. Schull and S. Schultz. 2001. Emergency Department Services in Ontario. Toronto: Institute for Clinical Evaluative Sciences.
Fatovich, D.M., Y. Nagree and P. Sprivulis. 2005. "Access Block Causes Emergency Department Overcrowding and Ambulance Diversion in Perth, Western Australia." Emergency Medicine Journal 22(5): 351-4.
Forster, A.J., I. Stiel, G. Wells, A.J. Lee and C. van Walraven. 2003. "The Effect of Hospital Occupancy on Emergency Department Length of Stay and Patient Disposition." Academic Emergency Medicine 10(2): 127-33.
Frost, L., S.P. Johnsen, L. Pedersen, S. Husted, G. Engholm, H.T. Sorensen and K.J. Rothman. 2002. "Seasonal Variation in Hospital Discharge Diagnosis of Atrial Fibrilation: A Population-Based Study." Epidemiology 13(2): 211-5.
Fullerton, K.J. and V.L. Crawford. 1999. "The Winter Bed Crisis - Quantifying Seasonal Effects on Hospital Bed Usage." QJM: Monthly Journal of the Association of Physicians 92(4): 199-206.
Menec, V.H., N.P. Roos, D.L. Nowicki, L. MacWilliam, G. Finlayson and C. Black. 1999. Seasonal Patterns of Winnipeg Hospital Use. Winnipeg: Manitoba Centre for Health Policy and Evaluation.
Physician Hospital Care Committee. 2006. Improving Access to Emergency Care: Addressing System Issues. Toronto: Ontario Hospital Association, Ontario Medical Association, Ontario Ministry of Health and Long-Term Care.
Proudlove, N.C., K. Gordon and R. Boaden. 2003. "Can Good Bed Management Solve the Overcrowding in Accident and Emergency Departments?" Emergency Medicine Journal 20: 149-155.
Rathlev, N.K., J. Chessare, J. Olshaker, D. Obendorfer, S.D. Mehta, T. Rothenhaus, S. Crespo, B. Magauran, K. Davidson, R. Shemin, K. Lewis, J.M. Becker, L. Fisher, L. Guy, A. Cooper and E. Litvak. 2007. "Time Series Analysis of Variables Associated with Daily Mean Emergency Department Length of Stay." Annals of Emergency Medicine 49(3): 265-71.
Schull, M., P.M. Slaughter and D.A. Redelmeier. 2002. "Urban Emergency Department Overcrowding: Defining the Problem and Eliminating Misconceptions." Canadian Journal of Emergency Medicine 4(2): 76-83.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed

