Healthcare Quarterly
Organizing Care across the Continuum: Primary Care, Specialty Services, Acute and Long-term Care
Abstract
Primary care networks (PCNs) facilitate integration of healthcare across the continuum. The Calgary Rural PCN implemented a community-based model where physicians and Alberta Health Services work together to deliver primary care addressing local population needs. This model is highly valued by physicians, decision-makers and providers, with early impacts on outcomes.
Introduction
Integration of the planning and delivery of services is an important component of healthcare systems. This paper describes the planning and implementation of a community-based model of primary care in the Calgary Rural Primary Care Network (CRPCN), a collaborative initiative between family physicians, Alberta Health Services – Calgary and Area managers and other stakeholders to ensure an integrated system across the continuum of care.
Background
Prior to the development of primary care networks (PCNs) in Alberta, the primary care system was isolated and functioned independently from other components of the healthcare system. Primary care consisted of disparate components; more specifically, the care provided by family physicians was disconnected from other primary care services and the system as a whole. This marginalized family physicians from their specialist colleagues and the healthcare system, resulting in poor or non-existent relationships with health authorities (Lester et al. 1998; Oelke et al. 2006).
Rural areas were also known to have additional, unique challenges impacting the delivery of healthcare services and realization of integration. These included geographical distance (Bolda and Seavy 2001; O'Meara 2003); lack of communication between providers and service organizations, often intensified by distance (O'Meara 2003); and animosity between communities (Hanlon 2001). Healthcare providers in rural settings were often regarded as second class by other providers. Rural health services tended to have higher case loads and fewer resources (e.g., support services, continuing education) than their urban counterparts (Halma et al. 2004; McCabe and Macnee 2002; Rogers 2003). On the other hand, rural settings exhibited a number of strengths. These included strong local leadership, a greater sense of community ownership, willingness to support local initiatives and the flexibility of small teams, where identification of needs and solutions can be expedited (Bolda and Seavy 2001).
The redesign of Alberta's primary care system has been a key response to these issues. Physician integration has been recognized as key to successfully integrated systems (Suter et al. 2007). Both the health system and physicians realize that integration is no longer an option but a necessity (Budetti et al. 2002; Gillies et al. 2001; Lester et al. 1998), considering the complexity of today's healthcare system (Alexander et al. 2001). In 2003, PCNs were initiated through a trilateral agreement (Alberta Medical Association 2003) between the Alberta Medical Association, Alberta Health and Wellness and regional health authorities. PCNs establish a formal relationship between physicians and the health region to collaboratively plan and deliver health services for a geographic area based on population needs. PCNs were developed to better integrate healthcare delivery across the continuum of care (e.g., specialty services, acute and long-term care). Objectives for PCNs include (Primary Care Initiative 2008):
- Improving coordination of primary health services with other healthcare services including hospitals, long-term care and specialty care services;
- Fostering a team approach to providing primary healthcare; and
- Family physicians work in cooperation with AHS to plan, coordinate and deliver care for patients (Primary Care Initiative 2008.).
The Calgary Rural PCN began its operations in February 2006. It covers a large geographic area southwest and southeast of Calgary and services approximately 110,000 residents. Currently, 100 physicians are registered with the CRPCN, with a physician participation rate of 100% in communities taking part in the initiative.
Intervention
Six local primary care team members across communities were interviewed. They described and articulated the model, successes and challenges and the impact on outcomes. Themes from these interviews provided the foundation for this paper.
Description of the Model
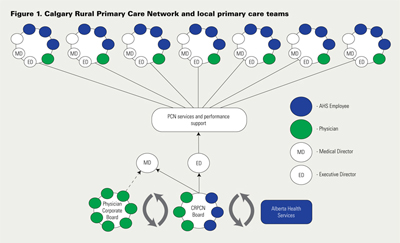
The CRPCN chose a community-based model; seven geographic communities each with a local primary care team. Each local primary care team consists of the community physician and Alberta Health Services – Calgary and Area managers accountable for various primary healthcare programs in that community (e.g., public health, continuing care). The model is illustrated in Figure 1.
The majority of CRPCN funding is distributed at the local level; therefore, each local primary care team sets its own priorities for service delivery based on local community needs as determined by the team, local community experts. More recently, population, healthcare utilization and evaluation data have been used in planning services. Provider interests, opportunities and long-term gaps have also been used to determine priorities for service delivery. This funding model allows "local autonomy that enables freedom and flexibility in a complex adaptive system" (interview participant) in planning and implementing primary care services for the population residing in that community.
The CRPCN Executive Director and Medical Director attend all local primary care team meetings. Other CRPCN physicians and staff and Alberta Health Services – Calgary and Area staff attend meetings, depending on agenda items. Local primary care team meetings are led by the co-chairs – the physician leader and a health system manager. Teams are characterized by collaborative decision making through discussion and consensus of team members. Because decisions are made locally, there is "greater buy-in and accountability for funding, performance measurement and improved health outcomes for patients" (interview participant).
The model has changed little over time, although relationships and services have evolved and ownership has been strengthened. While the same model is used across communities, the maturity of the model varies, with some teams being more integrated and collaborative than others.
Why Was This Model Chosen?
Initial CRPCN planning discussions "focused on community-based services to truly meet unmet health needs" (interview participant). Local solutions were highly valued by decision makers and providers, particularly family physicians. This was reinforced at a recent CRPCN retreat, where there was unanimous agreement that the local primary care model needed to be maintained. The model was chosen to facilitate "the integration that this type of model provides…an opportunity to work alongside physicians that we did not previously have" (interview participant) and to engage physicians. The model allows for services that address care and access specific to each community's population. Also, the community-based model was well aligned with rural culture.
Methodology, Change Process and Results
Local primary care teams meet monthly to plan and openly discuss ongoing issues in implementing primary care services in their communities. Having the CRPCN leadership at the table provides connection to other teams and the provincial vision and mandate. Learning across teams is facilitated by the participation of Alberta Health Services – Calgary and Area managers on more than one local primary care team. The model requires leadership and champions at the local level. Relationships are the foundation of the model and require time to develop, assisted by regular meetings and connections.
Impact of the Model
Early outcomes are described at the patient, provider and system levels.
Impact for Patients
There is a strong sense from members of local primary care teams that the quality of patient care has improved. Patients are receiving services locally that previously were not available or would have required travel to Calgary. Overall, care is more comprehensive for patients. For instance, chronic disease management (CDM) has been enhanced by adding pharmacists and CDM nurses in each community. From April to September 2008, CRPCN pharmacists had a total of 437 patient encounters involving 310 patients. Providers perceived a decrease in acute care admissions and increased self-care capacity for chronic disease patients. Although outcome data are not yet available, clinical indicators (e.g., HbA1C, BP [glycosylated hemoglobin, blood pressure]), utilization of healthcare services (emergency room admissions, in-patient admissions), quality of life, self-efficacy and patient satisfaction are being collected for future evaluation.
Each of the local primary care teams in the CRPCN has designated resources to a social worker (SW). SWs have been involved with a variety of patients through various PCN and AHS programs. One patient described the integration of services and providers organized by the SW as follows:
I wouldn't be where I am today if it wasn't for the social worker. Between the social worker and my doctor…the psychiatrist, the mental health people, all of that was because of the social worker. And so, truthfully, I don't know where I would be today if it wasn't for the social worker in my life.
With the introduction of community development and primary prevention initiatives, there is an increased focus on wellness. A teen and young-adult health clinic was initiated in one community early in the development of the PCN. Between September 2007 and September 2008, 1,002 clients were seen at the clinic, with an increase every six months since opening. In a sample of 124 new clients, 42% cited "the accessibility of the clinic" as their reason for choosing this clinic over another facility or provider. Four key themes were perceived by staff to increase accessibility of the clinic to youth: confidentiality of services; open attitudes of staff; multiple services provided (e.g., diagnosis, treatment and prevention of sexual health issues); and the connections to other services in the clinic (e.g., mental health, addiction, smoking cessation). The clinic has been so successful in providing access to teens and young adults, where previously there was no access to such services locally, that clinics have been initiated in two other communities in the CRPCN.
Impact for Providers
The community-based model has increased the satisfaction of health system managers, physicians and other healthcare professionals. There is a stronger working relationship between physicians and Alberta Health Services – Calgary and Area managers as well as physicians and other healthcare professionals. Decisions regarding services are based on discussions between these parties. The PCN initiatives have brought all providers into a closer working relationship, and regular meetings have provided a forum to enhance communication between providers. One manager stated that there is an increase in respect for physicians and valuing of their input. This proactive collaborative approach to meet the needs of their communities has resulted in increased provider satisfaction.
Impact on the System
The community-based model has promoted "a more integrated primary care system with enhanced collaboration between family physicians, public health, continuing care, social work, etc." (interview participant). Although the local primary care team was focused primarily on collaboration between physicians and the health system, increased collaboration between departments within the health system has also been realized. The enhanced collaboration between all components of the primary care system has increased the efficiency of service delivery and provided an opportunity to involve services that were previously absent.
Collaboration has moved beyond the primary care realm and has created linkages to acute care and seniors' care. This is evidenced by the "Blueberry Muffin" example. Monthly meetings initially organized by the PCN's pharmacist (where blueberry muffins were served, hence the name) to review patients' medications have broadened to include all patient issues. Interprofessional team members including the pharmacist, CDM nurse, physicians, home care staff and social worker are invited to review patients in a case conference format. Integration of primary care in a seniors' setting has created the opportunity for interprofessional collaboration and improved outcomes for residents.
The implementation of the social work role has been unique to each community to meet local needs. As an example of the integration of the social work role, one social worker has established a strong network with providers and programs in acute care, with physicians while they are doing rounds in the hospital, long-term care centres, community healthcare services (e.g., public health, home care, mental health services) and with other community organizations (e.g., the RCMP, Legal Aid, schools). The social worker attends various community meetings for the purposes of prevention/promotion activities, networking, community wellness education and advocacy.
A data-sharing agreement among clinic physicians, continuing care and emergency medical services (EMS), Alberta Health Services – Calgary and Area was developed in one community to enhance integration. Coupled with iPhone technology, home care nurses and EMS staff now have access to physician electronic medical records, providing better continuity of care for patients. The success of this program has resulted in its expansion to other communities.
The CRPCN community-based model fosters an environment of creativity in the delivery of primary care services. Community expertise facilitates local primary care teams in identifying local needs. Funding is managed locally and stakeholders all sit at the table, allowing for expedited decision- making with services "tailored to community needs" (interview participant). Both managers and physicians state that the CRPCN allows for "true innovation" in service delivery.
Discussion and Conclusion
Research identifies 10 characteristics found in successfully integrated systems (Suter et al. 2007). The CRPCN's community-based primary care model possesses a number of these characteristics, with early positive outcomes being realized for patients, providers and the healthcare system. First, the CRPCN is patient focused, with a community-needs-driven approach that is utilized by each local primary care team. The benefit is that local needs of patients and populations are being addressed. Services must be responsive to the changing needs of community members (Roberts 1996) in order to receive funding from the PCN, emphasizing accountability by each local primary care team. To date, community needs have largely been determined through local team expertise, but there is recognition that utilizing health services administrative and social district data from Alberta Health Services – Calgary and Area is necessary to better understand community needs.
Secondly, while still in the infancy stage, performance measurement, another characteristic of integrated systems (Suter et al. 2007), is a key focus of the CRPCN and its local primary care teams. Local teams are accountable for their finances as well as the outcomes for services delivered. Regular evaluation is carried out at the program and PCN levels, and data on ambulatory care sensitive conditions is being utilized in decision-making. This information is of benefit to each of the local teams to ensure that quality services are being delivered and the PCN continues to work on collecting further outcome data.
Third, the community-based model adopted by the CRPCN facilitates strong physician integration and leadership, essential at all levels of the healthcare system to ensure successful integration (Appleby et al. 1999; Coddington et al. 2001). Physicians are highly involved and have taken on a leadership role to deliver primary care services in partnership with Alberta Health Services – Calgary and Area management. Challenges continue to exist with differing philosophies and agendas regarding services and fund allocation, but these issues are being addressed by local primary care teams.
Fourth, utilization of interprofessional teams is highly evident in the CRPCN, ensuring communication among providers and facilitating continuity of care for patients. The PCN "has allowed us to explore all pieces of interprofessional practice" (interview participant). The right practitioners are doing the right things; territorial boundaries have been blurred and silos dismantled, even though standardized care delivery has not been a focus for teams. An additional benefit of the interprofessional practice has been the building of relationships between providers within the PCN and those in AHS.
The CRPCN has successfully created an integrated system for planning and implementation of service delivery at the community level. The CRPCN model shows significant integration within the primary care system in each rural community. Linkages have been initiated with other components of the health system (e.g., long-term care, acute care, EMS), but continued efforts will be required to ensure better integration across the continuum of care to further impact outcomes for patients.
About the Author(s)
Nelly D. Oelke, Research and Evaluation Consultant, Health Systems and Workforce Research Unit, Alberta Health Services - Calgary and Area. She is the evaluation lead for the Calgary Rural PCN. She can be reached at: nelly.oelke@albertahealthservices.ca.
Dr. Leslie Cunning, Medical Director, Calgary Rural PCN. Dr. Cunning has been with the PCN through initial development and implementation.
Kaye Andrews, Leader, Pharmacy Project Services, Calgary Rural PCN. Ms. Andrews has been instrumental in the development and integration of pharmacy services in the PCN.
Dorothy Martin, Manager, Continuing Care, Central Rural, Alberta Health Services - Calgary and Area. She has been a leader in programming for chronic disease in the PCN, as well as integrating PCN with home care and seniors' care.
Anne MacKay, Manager, Sexual and Reproductive Health, Sexual Assault Response Team, Domestic Violence Program, Alberta Health Services - Calgary and Area. As the past manager for public health, she was actively involved in leading one of the local primary care teams.
Katie Kuschminder. Ms. Kuschminder was previously employed as a Research Analyst in the Health Systems and Workforce Research Unit, Alberta Health Services - Calgary and Area responsible for the implementation of evaluation activities in the PCN.
Dr.Val Congdon, Regional Clinical Department Head, Rural Medicine, Alberta Health Services - Calgary and Area. Dr. Congdon has provided leadership in development and implementation of the Calgary Rural PCN and also practices as a family physician in the PCN.
References
Alberta Medical Association. 2003. Negotiations 2003 Detailed Summary. Edmonton: Alberta Medical Association.
Alexander, J. A., Waters, T. M., Burns, L. R., Shortell, S. M., Gillies, R. R., Budetti, P. P. et al. (2001). "The Ties That Bind: Interorganizational Linkages and Physician-system Alignment." Medical Care 39: 130-145.
Anderson, S.T. 1998. "How Healthcare Organizations Can Achieve True Integration." Healthcare Financial Management 52: 31-4.
Appleby, N.J., D. Dunt, D.M. Southern and D. Young. 1999. "General Practice Integration in Australia. Primary Health Services and Consumer Perceptions of Barriers and Solutions." Australian Family Physician 28: 858-63.
Bolda, E.J. and J.W. Seavy. 2001. "Rural Long-term Care Integration Developing Service Capacity." The Journal of Applied Gerontology 20: 426-57.
Budetti, P.P., S.M. Shortell, T.M. Waters, J.A. Alexander, L.R. Burns, R.R. Gillies et al. 2002. "Physician and Health System Integration." Health Affairs 21: 203-10.
Coddington, D.C., F.K. Ackerman Jr. and K.D. Moore. 2001. "Setting the Record Straight: Physician Networking Is an Effective Strategy." Healthcare Financial Management 55: 34-7.
Gillies, R.R., H.S. Zuckerman, L.R. Burns, S.M. Shortell, J.A. Alexander, P.P. Budetti et al. 2001. "Physician System Relationships: Stumbling Blocks and Promising Practices." Medical Care 39(7, S1): 92-106.
Halma, L., C. Mitton, C. Donaldson and B. West. 2004. "Case Study on Priority Setting in Rural Southern Alberta: Keeping the House from Blowing In." Canadian Journal of Rural Medicine 9: 26-36.
Hanlon, N.T. 2001. "Hospital Restructuring in Smaller Urban Ontario Settings: Unwritten Rules and Uncertain Relations." Canadian Geographer 45: 252-67.
Lester, R.S., M. Hundert, T.P. Dilworth, A. Blair and R. Crawford. 1998. "Physicians in Integrated Health Systems." Hospital Quarterly 1: 59-61.
McCabe, S. and C.L. Macnee. 2002. "Weaving a New Safety Net of Mental Healthcare in Rural America: a Model of Integrated Practice." Issues in Mental Health Nursing 23: 263-78.
Oelke, N.D. 2006. "Understanding Issues in Primary Care: Perspectives of Primary Care Physicians." Quality in Primary Care 14: 253-8.
O'Meara, P. 2003. "Would a Prehospital Practitioner Model Improve Patient Care in Rural Australia?" Emergency Medical Journal 20: 199-203.
Primary Care Initiative. 2008. About PCNs. Retrieved April 5, 2009. <http://www.albertapci.ca/AboutPCNs/Pages/default.aspx>.
Roberts, C.C. 1996. "Redefining the Healthcare Paradigm." Hospital Topics 74: 16-21.
Rogers, J. 2003. "Sustainability and Collaboration in Maternity Care in Canada: Dreams and Obstacles." Canadian Journal of Rural Medicine 8: 193-8.
Suter E., N.D. Oelke, C.E. Adair, C. Waddell, G.D. Armitage and L.A. Huebner. 2007. Health Systems Integration. Definitions, Processes and Impact: A Research Synthesis.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed