Nursing Leadership
Advanced Practice Nursing in Canada: Overview of a Decision Support Synthesis
Abstract
The objective of this decision support synthesis was to identify and review published and grey literature and to conduct stakeholder interviews to (1) describe the distinguishing characteristics of clinical nurse specialist (CNS) and nurse practitioner (NP) role definitions and competencies relevant to Canadian contexts, (2) identify the key barriers and facilitators for the effective development and utilization of CNS and NP roles and (3) inform the development of evidence-based recommendations for the individual, organizational and system supports required to better integrate CNS and NP roles into the Canadian healthcare system and advance the delivery of nursing and patient care services in Canada. Four types of advanced practice nurses (APNs) were the focus: CNSs, primary healthcare nurse practitioners (PHCNPs), acute care nurse practitioners (ACNPs) and a blended CNS/NP role.
We worked with a multidisciplinary, multijurisdictional advisory board that helped identify documents and key informant interviewees, develop interview questions and formulate implications from our findings. We included 468 published and unpublished English- and French-language papers in a scoping review of the literature. We conducted interviews in English and French with 62 Canadian and international key informants (APNs, healthcare administrators, policy makers, nursing regulators, educators, physicians and other team members). We conducted four focus groups with a total of 19 APNs, educators, administrators and policy makers. A multidisciplinary roundtable convened by the Canadian Health Services Research Foundation formulated evidence-informed policy and practice recommendations based on the synthesis findings.
This paper forms the foundation for this special issue, which contains 10 papers summarizing different dimensions of our synthesis. Here, we summarize the synthesis methods and the recommendations formulated at the roundtable.
Introduction
Nurse practitioners (NPs) and clinical nurse specialists (CNSs) have existed in Canada for about four decades. Both are considered advanced practice nurses (APNs), defined internationally as registered nurses (RNs) who have acquired the expert knowledge base, complex decision-making skills and clinical competencies for expanded practice (International Council of Nurses 2008). Advanced nursing practice, according to the national framework developed by the Canadian Nurses Association (CNA), is
… an umbrella term describing an advanced level of clinical nursing practice that maximizes the use of graduate educational preparation, in-depth nursing knowledge and expertise in meeting the health needs of individuals, families, groups, communities and populations. It involves analyzing and synthesizing knowledge; understanding, interpreting and applying nursing theory and research; and developing and advancing nursing knowledge and the profession as a whole (CNA 2008: 10).
Core advanced practice nursing roles include direct patient care, research, education, consultation, collaboration and leadership activities.
Despite the 40-year existence of APNs, the implementation of their roles in Canada has been sporadic and dependent on the changing political agendas shaping the healthcare system. Given the instability of the roles, the Office of Nursing Policy of Health Canada and the Canadian Health Services Research Foundation (CHSRF) commissioned a decision support synthesis. It aimed to develop evidence-informed policy and practice recommendations for optimizing the contributions of NPs and CNSs in meeting Canadians' healthcare needs. A decision support synthesis seeks to address a policy-relevant question through a deliberative process involving the engagement of decision makers, distillation of published and grey literature, data collection from key stakeholders and, finally, integration and analysis of the data to develop policy and management recommendations (CHSRF 2010).
This special issue of the Canadian Journal of Nursing Leadership focuses entirely on the synthesis, beginning with this paper, which summarizes the methods and resulting recommendations. The following nine papers focus on various dimensions of the APN role in Canada. They include a historical account (Kaasalainen et al. 2010), an examination of educational issues (Martin-Misener et al. 2010), detailed summaries of the status of primary healthcare NPs (Donald et al. 2010b), acute care NPs (Kilpatrick et al. 2010) and CNSs (Bryant-Lukosius et al. 2010), the role of nursing leadership in integrating APN roles (Carter et al. 2010), an examination of title confusion and lack of role clarity as barriers to role implementation (Donald et al. 2010a), factors enabling role integration (DiCenso et al. 2010c) and, finally, examples of innovative models that utilize NPs to increase patient access to primary healthcare (DiCenso et al. 2010a).
Types of APNs
In Canada, APNs include primary healthcare NPs (PHCNPs), acute care NPs (ACNPs), CNSs and CNS/NPs (a blended role). The nurse anesthetist role is just emerging and was not addressed in this synthesis. NPs are
registered nurses with additional educational preparation and experience who possess and demonstrate the competencies to autonomously diagnose, order and interpret diagnostic tests, prescribe pharmaceuticals and perform specific procedures within their legislated scope of practice (CNA 2009b: 1).
PHCNPs, also known as family or all-ages NPs, typically work in the community in settings such as community health centres, primary healthcare teams and long-term care. Their main focus is health promotion, preventive care, diagnosis and treatment of acute minor illnesses and injuries, and monitoring and management of stable chronic diseases. ACNPs, also known as specialty or specialist NPs as well as adult, pediatric and neonatal NPs, provide advanced nursing care across the continuum of acute care services for patients who are acutely, critically or chronically ill, often with multiple and complex morbidities. These ACNPs might work in settings such as neonatology, nephrology and cardiology. Titling of NP roles is in transition. For the purposes of our synthesis, we refer to NPs who practise in community settings with a focus on families and all ages as PHCNPs. We refer to those who work in hospital in-patient or ambulatory settings with a focus on specialized populations as ACNPs.
CNSs are RNs with a graduate degree in nursing who have expertise in a clinical nursing specialty and perform a role that includes practice, consultation, collaboration, education, research and leadership. They contribute to the development of nursing knowledge and evidence-based practice and address complex healthcare issues for patients, families, other disciplines, administrators and policy makers (CNA 2009a). CNSs specialize in a specific area of practice that may be defined in terms of a population, setting, disease or medical subspecialty, type of care or type of problem.
There are also APNs who combine the CNS and NP roles (Pinelli 1997). The blended CNS/NP role was first introduced in Ontario in tertiary-level neonatal intensive care units (NICUs) in the late 1980s (Hunsberger et al. 1992). At the time, the blended CNS/NP title was chosen to protect time for the nonclinical dimensions of advanced practice. However, current CNS/NP practice is consistent with the ACNP role involving the clinical care of complex medical problems and patient care planning and coordination, in addition to leadership, consultation and research. Given that nonclinical role dimensions have been proposed as essential components of all advanced practice nursing roles, there is no longer a need for a separately titled CNS/NP role, and most of these APNs now are known as ACNPs.
Numbers of APNs in Canada
Between 2004 and 2008, the number of licensed NPs in Canada more than doubled, increasing from 800 to 1,626 (Canadian Institute for Health Information [CIHI] 2010). This figure, however, is an underestimate of the NP workforce as the numbers do not include ACNPs from all Canadian jurisdictions. Until recently, in some provinces ACNPs have not been licensed, and therefore it is not currently possible to determine how many exist in Canada. It is also difficult to ascertain the exact number of CNSs in Canada because there is no protected titling or standard credentialling mechanism. Based on self-reported CNS data, the number of CNSs decreased between 2000 and 2008 from 2,624 to 2,222, accounting for about 1% of the Canadian nursing workforce (CIHI 2010; CNA 2006).
Effectiveness of APNs
There is abundant research demonstrating the safety and effectiveness of PHCNPs, ACNPs and CNSs. In preparation for our decision support synthesis, we conducted searches for all randomized controlled trials ever published internationally comparing APNs to usual care in terms of patient, provider and/or health system outcomes. While our search was not as comprehensive as one would do for a formal systematic review, we found a total of 78 trials: 28 of PHCNPs, 17 of ACNPs, 32 of CNSs and one of CNS/NPs. Findings consistently showed that care by APNs resulted in equivalent or improved outcomes. The complete listing of studies and their findings is included in an appendix to our full decision support synthesis report, found on the CHSRF website (DiCenso et al. 2010b).
A systematic review of NPs in primary care found that patients receiving NP care had higher satisfaction and better quality of care than those receiving physician care, with no difference in health outcomes (Horrocks et al. 2002). A recent study of four primary healthcare delivery models in Ontario found high-quality chronic disease management was associated with the presence of a PHCNP (Russell et al. 2009). Comparisons of ACNP care with usual care showed either no differences in outcomes such as mortality, morbidity/complications and length of hospital stay or an improvement in outcomes favouring the ACNP role (e.g., Dawes et al. 2007; Krichbaum 2007).
In their annotated bibliography of 70 studies, Fulton and Baldwin (2004) found that CNSs were associated with reductions in hospital length of stay, readmissions, emergency room visits and costs, as well as improvements in staff nurse knowledge, functional performance, mood state, quality of life and patient satisfaction. Mitchell-DiCenso et al. (1996) found that CNS/NPs functioning in the blended role in NICUs were equivalent to pediatric residents with respect to neonatal morbidity and mortality, parent satisfaction, costs and incidence of long-term developmental delays.
Synthesis Objective
The objective of this decision support synthesis was to identify and review published and grey literature and to conduct stakeholder interviews to (1) describe the distinguishing characteristics of CNS and NP role definitions and competencies relevant to Canadian contexts, (2) identify the key barriers and facilitators for the effective development and utilization of CNS and NP roles and (3) inform the development of evidence-based recommendations for the individual, organizational and health system supports required to better integrate CNS and NP roles into the Canadian healthcare system and advance the delivery of nursing and patient care services in Canada. In this paper, we outline the detailed methods of our synthesis that form the foundation for the papers that follow in this special issue.
Methods
We received ethics approval from the McMaster University Research Ethics Board on July 15, 2008. The synthesis included a number of elements: (1) an advisory board, (2) a scoping review of the literature, (3) key informant interviews and focus groups and (4) a multidisciplinary roundtable to formulate recommendations from the synthesis findings. Each of these elements is described below.
Advisory Board
We formed a 23-member multidisciplinary (administrators, policy makers, practitioners, educators, regulators and researchers) and multijurisdictional (international, federal, provincial and territorial) advisory board. Via teleconferences and an all-day face-to-face meeting, advisory board members helped identify relevant documents and key informant interviewees, develop interview questions and formulate implications based on the findings.
Scoping Review of the Literature
We conducted a scoping review using established methods (Arksey and O'Malley 2005; Anderson et al. 2008) to summarize the literature on advanced practice nursing role definitions, competencies and utilization in the Canadian healthcare system, identify the policies influencing the development and integration of these roles and explore the gaps and opportunities for their improved deployment. Like systematic reviews, scoping reviews use rigorous and transparent methods to comprehensively search for all relevant literature and to analyze and interpret the data. However, a scoping review differs from a systematic review in three ways. First, a scoping review is exploratory in nature and seeks to "map" all the relevant literature on a broad topic and identify recurring themes, while a systematic review addresses a highly specific research question and focuses strictly on empirical studies. Second, in a scoping review, the criteria for exclusion and inclusion are based not on the quality of the studies, but on relevance. Because scoping reviews are exploratory, all papers on a topic are included, be they studies or narrative and commentary pieces such as editorials and essays. Third, all information from the included papers is charted, and themes and key issues are identified. Because of the broad inclusion criteria, many themes emerge that can inform gaps in the existing research.
We concentrated on Canadian literature of all types to capture context-free, context-sensitive and colloquial evidence (CHSRF 2010). In keeping with the tenets of scoping reviews, we did not exclude articles based on methodological quality. To guide our work, we developed a framework to capture the structure, process and outcome dimensions and descriptors of advanced practice nursing roles. Structure-related dimensions included role description, numbers, types, education, competencies, regulation, scope of practice, practice settings, union membership and liability coverage. Process-related dimensions included barriers and facilitators associated with role implementation and practice patterns. Outcome-related dimensions included patient, provider and health system outcomes.
We searched MEDLINE, CINAHL and EMBASE using applicable Mesh headings and free text keywords pertinent to CNSs, NPs and CNS/NPs, and we performed a citation search using the Web of Science database and 10 key papers that directly addressed structure, process and outcome dimensions of advanced practice nursing roles. We scanned the reference lists of all relevant papers and searched websites of Canadian professional organizations and national, provincial and territorial governments. The four journals yielding the greatest number of relevant articles, Canadian Journal of Nursing Leadership, Journal of Advanced Nursing, Canadian Nurse and Clinical Nurse Specialist, were hand searched from May 2008 to January 2009 to avoid omitting papers published after the original database search. Advisory board and research team members contributed relevant papers from their personal files.
Papers included in the synthesis met the following criteria:
- All Canadian papers including primary studies, literature and policy reviews, reports, editorials, essays, commentaries and descriptive accounts (any date of publication)
- International review papers published between 2003 and 2008
- International non-review papers only if of unique relevance to the synthesis or if little Canadian literature existed on the topic
- Written in French or English
- Addressing structure, process and/or outcome dimensions of one or more advanced practice nursing roles
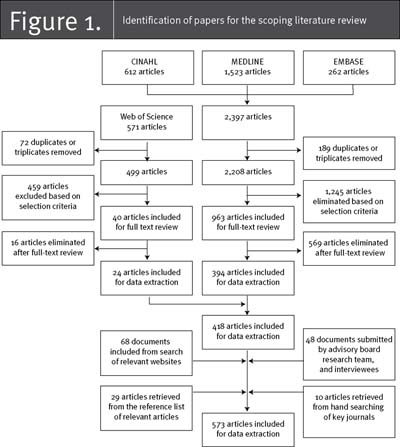
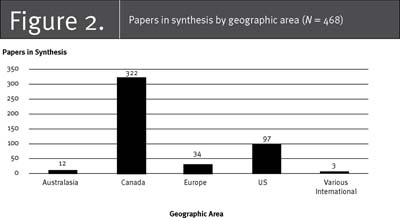
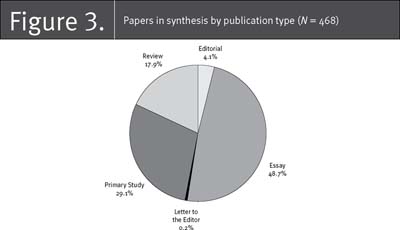
The search yielded 2,397 papers (Figure 1). They were divided among three teams of two researchers for title and abstract review (researchers had participated in training to ensure consistency across reviews). We resolved within-team disagreements by having a third team member review the disputed titles and abstracts. If a paper was deemed relevant after title and abstract review, one team member reviewed the full text, using our inclusion criteria. We identified 573 relevant papers for data extraction. The team was divided into triads, and each triad reviewed and extracted data from literature pertinent to a specific advanced practice nursing role (e.g., CNSs). During this stage, 105 papers failed to meet our inclusion criteria, leaving 468 papers in the synthesis. Figure 2 summarizes the country of origin of the 468 papers. They represent all Canadian papers but only recent reviews from other countries, hence the large proportion of Canadian papers (69%). Figure 3 provides the breakdown by publication type, showing that about half the papers represent primary studies and reviews and half represent essays and editorials. Table 1 describes the Canadian papers by type of APN, publication type and publication year. The majority of papers (70%) have been written since 2000, with 17% focused on ACNPs, 47% on PHCNPs, 8% on NPs (type unspecified), 3% on CNS/NPs, 10% on CNSs and 15% on APNs (type unspecified).
| Table 1. Canadian papers by type of APN and publication year | ||||||||||||
| Type of APN | 1970 to 1999 | 2000 to 2009 | Overall (1970 to 2009) | |||||||||
| Primary study or review | Editorial or essay | Total | % | Primary study or review | Editorial or essay | Total | % | Primary study or review | Editorial or essay | Total | % | |
| ACNP | 7 | 3 | 10 | 9.5 | 15 | 34 | 49 | 20.1 | 22 | 37 | 59 | 16.9 |
| PHCNP | 27 | 34 | 61 | 58.1 | 61 | 43 | 104 | 42.6 | 88 | 77 | 165 | 47.3 |
| General NP | 2 | 3 | 5 | 4.8 | 11 | 12 | 23 | 9.4 | 13 | 15 | 28 | 8.0 |
| CNS/NP | 1 | 3 | 4 | 3.8 | 2 | 4 | 6 | 2.5 | 3 | 7 | 10 | 2.9 |
| CNS | 2 | 7 | 9 | 8.6 | 13 | 12 | 25 | 10.2 | 15 | 19 | 34 | 9.7 |
| General APN | 4 | 12 | 16 | 15.2 | 13 | 24 | 37 | 15.2 | 17 | 36 | 53 | 15.2 |
| Total | 43 | 62 | 105 | 115 | 129 | 244 | 158 | 191 | 349a | |||
| ACNP = acute care nurse practitioner; APN = advanced practice nurse; CNS = clinical nurse specialist; NP = nurse practitioner; PHCNP = primary healthcare nurse practitioner. | ||||||||||||
| a Total exceeds the number of Canadian papers in Figure 2 because some papers fit into more than one publication type category. | ||||||||||||
To analyze the extracted data, we used a combination of descriptive tables, narrative syntheses (Mays et al. 2005) and team discussions. Each member of each triad independently summarized the data she had extracted. Each triad then met to discuss the tabulated data and their summaries. Three researchers (AD, IB and KK) attended all triad meetings to enable cross-triad continuity. At the triad meetings, the summaries prepared by team members were discussed to compare and contrast themes and to formulate conclusions. The entire team then met to discuss the results of the triad meetings and aggregate data across triads.
Key Informant Interviews and Focus Groups
In consultation with our advisory board, we used purposeful sampling to identify key informants with a wide range of perspectives on advanced practice nursing issues in Canada and internationally. The advisory board also assisted in developing a semi-structured interview guide, which was piloted on four participants. Feedback from the pilot indicated that the questions were clear and comprehensive and that the length of the interview was appropriate. All key informants were asked the same set of questions, focusing on all types of APNs. The questions included, for example, reasons for introducing the role(s) in their organizations, region or province/territory; how the role(s) were implemented; key factors facilitating and hampering their full integration at the individual, organizational and system levels; the nature of their collaborative relationships; their impact; success stories and recommendations for fully integrating the role(s). Individual interviews were conducted by telephone or in person in English or French. We also conducted four focus groups. All individual and focus group interviews were audio recorded, transcribed and checked for accuracy.
Data collection occurred between August 2008 and February 2009. We interviewed 62 key stakeholders (Table 2) including CNSs (n = 9; five from three provinces in Canada and four from the United States [US]); PHCNPs (n = 8; five from three provinces and two territories in Canada, two from the US, and one PHCNP–researcher from the United Kingdom [UK]); ACNPs (n = 5; four from four provinces in Canada and one from the US); health administrators (n = 11 from five provinces); provincial government policy makers (n = 6 from five provinces; five in chief-nursing-officer or nursing-policy-analyst positions and one without a nursing background); nursing regulators (n = 7; six from Canada representing seven provinces/territories [one regulator represented two territories] and one from Australia); educators (n = 5; three from Canada representing three provinces and two from the US); physicians (n = 7; three family physicians and four specialists from five provinces); and four healthcare team members from three provinces, including two RNs, one pharmacist and one respiratory therapist. Four of the interviews were conducted in French and the remainder in English. The 62 interview participants came from Canada (51), the US (9), the UK (1) and Australia (1). Of the 51 from Canada, 14 were from the Western provinces, 18 were from Ontario, 8 from Quebec, 8 from the Atlantic provinces and 3 from the three territories.
| Table 2. Key informant interviews (n = 62) | ||
| Type | Number | Location |
| Clinical nurse specialists | 9 | 5 – Canada (3 provinces) 4 – United States |
| Primary healthcare nurse practitioners | 8 | 5 – Canada (3 provinces and 2 territories) 2 – United States 1 – United Kingdom |
| Acute care nurse practitioners | 5 | 4 – Canada (4 provinces) 1 – United States |
| Health administrators | 11 | 11 – Canada (5 provinces) |
| Provincial government policy makers | 6 | 6 – Canada (5 provinces) |
| Nursing regulators | 7 | 6 – Canada (5 provinces and 2 territories) 1 – Australia |
| Educators | 5 | 3 – Canada (3 provinces) 2 – United States |
| Physicians | 7 | 7 – Canada (5 provinces) |
| Healthcare team members | 4 | 4 – Canada (3 provinces) |
Three of the focus groups were a convenience sample of attendees at the International Council of Nurses (ICN) International Nurse Practitioner/Advanced Practice Nursing Network (INP/APNN) conference in Toronto in September 2008. An invitation to attend the focus group was included in the conference package. A total of 15 individuals participated, representing all types of APNs, as well as educators, administrators and policy makers. The majority of participants were from Canada; others were from the US and Australia. Each focus group had three to six participants and was conducted by two members of our research team, one as interviewer and the other as recorder and observer. The fourth focus group was a purposively selected sample of ACNPs (previously known as CNS/NPs) from Ontario (four participants) who worked in the same setting.
In the interest of having as diverse and representative a sample as possible, we chose to continue interviewing even after data saturation was achieved. In total, through focus groups and interviews, we collected data from 81 individuals: four focus groups with 19 attendees and 62 interviewees.
An initial coding structure of emergent themes from the interviews was developed by the interviewer and one team member (IB). This draft coding structure was then integrated by three team members (DBL, IB and AD) into a broader, theoretically informed framework based on two papers describing factors influencing advanced practice nursing role integration (Bryant-Lukosius and DiCenso 2004; Bryant-Lukosius et al. 2004). A spreadsheet was created to summarize codes, themes and data from each transcript. Three team members (DBL, IB and AD) and the four individuals who would be coding used the framework to independently code one transcript and discussed their coding. Two team members (JA and KK) and two research assistants then used the framework to code all the transcripts, following which they prepared summaries according to type of stakeholder. Themes were compared across stakeholder type. Canadian and international interviews were summarized separately. A French-speaking team member (KK) coded French interviews.
In summarizing the results, we integrated findings from the scoping review and interviews examining similarities and differences in themes and common patterns and trends (Erzberger and Kelle 2003). For barriers and facilitators associated with advanced practice nursing role integration, we concentrated on Canadian papers written since 1990, because barriers or facilitators identified pre-1990 could be outdated. This was especially likely given the implementation of regionalization throughout Canada beginning about 1990.
Multidisciplinary Roundtable
Once we completed the synthesis and worked with our advisory board to derive the implications of our findings, CHSRF convened a multidisciplinary roundtable that included representatives from key nursing, medical, government, regulatory and professional associations to develop pragmatic recommendations for policy, practice and research (DiCenso et al. 2010b).
Discussion
Roundtable Recommendations
Roundtable participants made 11 key recommendations (DiCenso et al. 2010b). They are grouped below according to which of the key players in our healthcare system would likely assume a leadership role for action or implementation.
For the Nursing Community (and Partners)
- The CNA should lead, in collaboration with other health professional stakeholder groups (particularly the Canadian Medical Association and the College of Family Physicians of Canada), the creation of vision statements that clearly articulate the value-added role of CNSs and NPs across settings, with close attention paid to roles in the delivery of primary healthcare. These vision statements should include specific, yet flexible, role descriptions pertinent to specific healthcare contexts, which would help to address implementation barriers deriving from lack of role clarity.
For Senior Decision Makers (Policy and Practice)
- A pan-Canadian multidisciplinary task force involving key stakeholder groups should be established to facilitate the implementation of advanced practice nursing roles.
- Health human resources planning by federal, provincial and territorial ministries of health should consider the contribution and implementation of advanced practice nursing roles based on a strategic and co-ordinated effort to address population healthcare needs.
- A communication strategy should be developed (via collaboration with government, employers, educators, regulatory colleges and professional associations) to educate nurses, other healthcare professionals, the Canadian public and healthcare employers about the roles, responsibilities and positive contributions of advanced practice nursing.
- Advanced practice nursing positions and funding support should be protected following implementation and demonstration initiatives to ensure some stability and sustainability for these roles (and the potential for longer-term evaluation) once they have been incorporated into the healthcare delivery organization/structure.
- In order to facilitate provider mobility in response to population healthcare needs and improve recruitment and retention to advanced practice nursing roles, a pan-Canadian approach should be taken, in collaboration with regulators, to standardize advanced practice nursing regulatory standards, requirements and processes.
For Educators
- In order to facilitate provider mobility in response to population healthcare needs and improve recruitment and retention to advanced practice nursing roles, a pan-Canadian approach should be taken, in collaboration with educators, to standardize advanced practice nursing educational standards, requirements and processes.
- The curriculum across all undergraduate and postgraduate health professional training programs should include components that address inter-professionalism, in order to familiarize all health professionals with the roles, responsibilities and scopes of practice of their collaborators.
For the Research and Research Funding Community
- Further research should be conducted to quantify the impact of advanced practice nursing roles on healthcare costs. The contexts of education, effectiveness and length of career should be addressed within this research.
- 10. The focus of advanced practice nursing role effectiveness research should shift away from replacement models and illustrate the "value added" of these roles as compared to other nursing roles.
- 11. The CNS role in the Canadian context requires further study and should be the focus of future academic work.
Strengths and Limitations
We used a variety of strategies to ensure comprehensive identification of published papers and grey literature. As a result, we reviewed and retained in the synthesis close to 500 papers representing English- and French-language published and unpublished literature written about APNs in Canada as well as international reviews published in the past five years. We used an electronic program to systematically extract the information from the papers, with training and pilot testing of data extractors. While we identified many relevant keywords to guide the searches, we may have missed papers that used different keywords.
We conducted 62 interviews (four in French) and four focus groups with a breadth of key informants, including all types of APNs, health administrators, nursing regulators, educators, policy makers, physicians and members of the healthcare team, most from Canada but also from the US, the UK and Australia. While these are more interviews than we had proposed to conduct, the number is still relatively small when considering the vastness of Canada and the different constituencies represented. However, many of the themes arose repeatedly across informant groups and were consistent with the literature. We interviewed at least one key informant from each province and territory (with one interviewee speaking about both Nunavut and the Northwest Territories). The inclusion of French-language literature and French-speaking key informants (interviewed in French) minimized the English-language bias and enabled a fuller exploration of the issues throughout all of Canada.
While we interviewed seven physicians, we conducted only four interviews of other members of the healthcare team: two RNs, a pharmacist and a respiratory therapist. The APN relationship with these and other healthcare team members (e.g., social workers) should be studied further. When our advisory board reviewed the findings, they indicated that some of the data provided by key informants may have been incorrect or incomplete, based perhaps on a limited awareness of the issue; for example, some informants indicated that CNSs did not provide direct patient care. This misperception reinforces the themes that emerged from our synthesis regarding lack of role clarity and title confusion.
The collection of data from patient informants was beyond the mandate and scope of this review. As new models of care emerge in the future, it will be important to involve patients and families to identify their unmet needs.
Our interview data provide a snapshot of key issues identified from diverse informant types across a variety of jurisdictions about different advanced practice nursing roles. Most reviews of advanced practice nursing conducted in Canada to date have focused on one APN type exclusively (e.g., PHCNPs). While the breadth of this decision support synthesis has allowed us to examine issues across APN types, it may have compromised depth of exploration of key issues for specific roles. For example, we were not able to sample APNs from all sectors in which they work.
The advisory board assisted with identifying relevant jurisdictional and organizational grey literature, reviewing the interview guide and suggesting key informants to interview. To ensure comprehensiveness and objectivity in the interpretation of our findings, the board also reviewed our report, provided constructive feedback and assisted in identifying implications based on our findings.
Dissemination Plans
The full report of the decision support synthesis is available in English and French on the CHSRF website (DiCenso et al. 2010b). In addition to this special issue of the Canadian Journal of Nursing Leadership, manuscripts that target relevant topics for international and healthcare professional audiences will be submitted to journals such as the Journal of Advanced Nursing and the Canadian Medical Association Journal. We have presented our findings at key national conferences and will continue to seek out these opportunities. We have shared the findings with the provincial/territorial nurse advisors across Canada. The Organisation for Economic Co-operation and Development (OECD) surveyed 12 countries about APNs in 2009, and the Canada-specific responses to the survey were largely informed by the decision support synthesis findings (Delamaire and Lafortune 2010).
Tailored briefing notes that emphasize action plans will be prepared for provincial/territorial Ministers and Deputy Ministers of Health, the Advisory Committee on Health Delivery and Human Resources (ACHDHR), employers and program managers. We will collaborate with key organizations such as the CNA, the Canadian Association of Advanced Practice Nurses (CAAPN), the Canadian Association of Schools of Nursing (CASN), the Academy of Canadian Executive Nurses (ACEN), the Canadian Healthcare Association (CHA), the Canadian Medical Association (CMA) and the College of Family Physicians of Canada (CFPC) to identify strategies for targeted information exchange with the nursing and medical communities and to identify medical and nursing champions to disseminate synthesis findings and recommendations to internal groups and committees of their professional associations and educational/regulatory bodies.
Conclusion
APNs have been part of the Canadian healthcare system for almost 40 years. Their presence has expanded and contracted based on factors such as physician shortages and surpluses and hospital budgets. Three existing significant reports have examined advanced nursing practice (CNA 2006) and more specifically NPs (Canadian Nurse Practitioner Initiative 2006) and extended nursing roles such as NPs in primary care from a Canadian perspective (Advisory Committee on Health Human Resources & The Centre for Nursing Studies in collaboration with The Institute for the Advancement of Public Policy, Inc. 2001). Our synthesis differs from these earlier works by providing an examination of CNS, ACNP and PHCNP roles through a systematic scoping review of Canadian and international literature and by conducting interviews and focus groups with national and international key informants from a variety of stakeholder groups.
The findings of our synthesis demonstrate (1) the yet unfulfilled or unrealized contributions APNs could make to address important gaps in maximizing the health of Canadians through equitable access to high-quality healthcare services, (2) the important interplay and influence of dynamic and often competing values, beliefs and interests of provincial and national governments, healthcare administrators and health professions on the policies and politics that shape the education, regulation and ad hoc deployment of advanced practice nursing roles, and (3) the continued vulnerability of advanced practice nursing roles to changes in health policies and economic conditions. The papers in this special issue both consolidate and augment our current knowledge base about advanced practice nursing. These papers provide readers with a comprehensive understanding of topics such as Canada's historical journey in integrating APNs into our healthcare system; the inconsistencies in educational requirements for PHCNPs across the country and limited access to CNS-specific graduate education; the central issues and challenges to the full integration of PHCNPs, ACNPs and CNSs in Canada; the important role leaders play in supporting advanced practice nursing; and innovative PHCNP-related approaches to increasing patient access to healthcare.
About the Author(s)
Alba DiCenso, RN, PhD, CHSRF/CIHR Chair in Advanced Practice Nursing (APN), Director, Ontario Training Centre in Health Services & Policy Research, Professor, Nursing and Clinical Epidemiology & Biostatistics, McMaster University, Hamilton, ON
Ruth Martin-Misener, NP, PhD, Associate Professor & Associate Director, Graduate Programs, School of Nursing,, Dalhousie University, Halifax, NS, Affiliate Faculty, CHSRF/CIHR Chair Program in APN
Denise Bryant-Lukosius, RN, PhD, Assistant Professor, School of Nursing & Department of Oncology, McMaster University, Senior Scientist, CHSRF/CIHR Chair Program in APN, Director, Canadian Centre of Excellence in Oncology Advanced Practice Nursing (OAPN) at the Juravinski Cancer Centre, Hamilton, ON
Ivy Bourgeault, PhD, CIHR/Health Canada Research Chair in Health Human Resource Policy, Scientific Director, Population Health Improvement Research Network and Ontario Health Human Resources Research Network, Professor, Interdisciplinary School of Health Sciences, University of Ottawa, Ottawa, ON
Kelley Kilpatrick, RN, PhD, Postdoctoral Fellow, CHSRF/CIHR Chair Program in APN, Professor, Department of Nursing, Université du Québec en Outaouais, St-Jérôme, QC
Faith Donald, NP-PHC, PhD, Associate Professor, Daphne Cockwell School of Nursing, Ryerson University, Toronto, ON, Affiliate Faculty, CHSRF/CIHR Chair Program in APN
Sharon Kaasalainen, RN, PhD, Associate Professor, School of Nursing, McMaster University, Career Scientist, Ontario Ministry of Health and Long-Term Care, Affiliate Faculty, CHSRF/CIHR Chair Program in APN, Hamilton, ON
Patricia Harbman, NP-PHC, MN/ACNP Certificate, PhD(c), University of Toronto, Graduate student in CHSRF/CIHR Chair Program in APN, Oakville, ON
Nancy Carter, RN, PhD, CHSRF Postdoctoral Fellow, Junior Faculty, CHSRF/CIHR Chair Program in APN, McMaster University, Hamilton, ON
Sandra Kioke, RN, PhD student, University of Victoria, Graduate student in CHSRF/CIHR Chair Program in APN, Courtenay, BC
Julia Abelson, PhD, Professor, Clinical Epidemiology & Biostatistics, McMaster University, Director, Centre for Health Economics & Policy Analysis (CHEPA), Hamilton, ON
R. James McKinlay, BPhEd, Research Coordinator, CHSRF/CIHR Chair Program in APN, McMaster University, Hamilton, ON
Dianna Pasic, BAH (Psychology), Senior Research Coordinator, Centre for Health Economics and Policy Analysis (CHEPA), McMaster University, Hamilton, ON
Brandi Wasyluk, BSc, Research Assistant, CHSRF/CIHR Chair Program in APN, McMaster University, Hamilton, ON
Julie Vohra, MSc, Program Coordinator, CHSRF/CIHR Chair Program in APN, McMaster University, Hamilton, ON
Renee Charbonneau-Smith, RN, MSc, Knowledge Exchange Specialist, CHSRF/CIHR Chair Program in APN, McMaster University, Hamilton, ON
Acknowledgment
The synthesis from which this work was derived was made possible through joint funding by the Canadian Health Services Research Foundation and the Office of Nursing Policy of Health Canada. We thank the librarians who conducted searches of the electronic databases, Tom Flemming at McMaster University and Angella Lambrou at McGill University. Chris Cotoi and Rick Parrish in the Health Information Research Unit (HIRU) at McMaster University created the electronic literature extraction tool for the project. We thank all those who took time from their busy schedules to participate in key informant interviews and focus groups. Special thanks go to our advisory board, roundtable participants and Dr. Brian Hutchison for their thoughtful feedback and suggestions.
References
Advisory Committee on Health Human Resources & The Centre for Nursing Studies in collaboration with The Institute for the Advancement of Public Policy, Inc. 2001. Final Report: The Nature of the Extended/Expanded Nursing Role in Canada. Retrieved January 12, 2009. <http://www.cns.nf.ca/research/finalreport.htm>.
Anderson, S., P. Allen, S. Peckham and N. Goodwin. 2008. "Asking the Right Questions: Scoping Studies in the Commissioning of Research on the Organisation and Delivery of Health Services." Health Research Policy and Systems 6(1): 7.
Arksey, H. and L. O'Malley. 2005. "Scoping Studies: Towards a Methodological Framework." International Journal of Social Research Methodology 8(1): 19–32.
Bryant-Lukosius, D., N. Carter, K. Kilpatrick, R. Martin-Misener, F. Donald, S. Kaasalainen, P. Harbman, I. Bourgeault and A. DiCenso. 2010. "The Clinical Nurse Specialist Role in Canada." Canadian Journal of Nursing Leadership 23(Special Issue December): 140–66.
Bryant-Lukosius, D., A. DiCenso, G. Browne and J. Pinelli. 2004. "Advanced Practice Nursing Roles: Development, Implementation and Evaluation." Journal of Advanced Nursing 48(5): 519–29.
Bryant-Lukosius, D. and A. DiCenso. 2004. "A Framework for the Introduction and Evaluation of Advanced Practice Nursing Roles." Journal of Advanced Nursing 48(5): 530–40.
Canadian Health Services Research Foundation. 2010. Decision Support Synthesis Program. Ottawa, ON: CHSRF. Retrieved December 31, 2010. <http://www.chsrf.ca/Programs/PastPrograms/DecisionSupportSynthesisPrograms.aspx>.
Canadian Institute for Health Information. 2010. Regulated Nurses in Canada: Trends of Registered Nurses. Ottawa, ON: CIHI. Retrieved March 21, 2010. <http://secure.cihi.ca/cihiweb/products/regulated_nurses_2004_2008_en.pdf>.
Canadian Nurses Association. 2006. Report of 2005 Dialogue on Advanced Nursing Practice. Ottawa, ON: CNA. Retrieved March 2, 2009. <http://www.cna-aiic.ca/CNA/documents/pdf/publications/Report_2005_ANP_Dialogue_e.pdf>.
Canadian Nurses Association. 2008. Advanced Nursing Practice: A National Framework. Ottawa, ON: CNA. Retrieved January 12, 2009. <http://www.cna-aiic.ca/CNA/documents/pdf/publications/ANP_National_Framework_e.pdf>.
Canadian Nurses Association. 2009a. Position Statement: Clinical Nurse Specialist. Ottawa, ON: CNA. Retrieved September 17, 2009. <http://www.cna-aiic.ca/CNA/documents/pdf/publications/PS104_Clinical_Nurse_Specialist_e.pdf>.
Canadian Nurses Association. 2009b. Position Statement: The Nurse Practitioner. Ottawa, ON: CNA. Retrieved April 5, 2010. <http://www.cna-aiic.ca/CNA/documents/pdf/publications/PS_Nurse_Practitioner_e.pdf>.
Canadian Nurse Practitioner Initiative. 2006. Nurse Practitioners: The Time Is Now. A Solution to Improving Access and Reducing Wait Times in Canada. Ottawa, ON: Canadian Nurse Practitioner Initiative. Retrieved January 12, 2009. <http://www.cna-nurses.ca/CNA/documents/pdf/publications/cnpi/tech-report/section1/01_Integrated_Report.pdf>.
Carter, N., R. Martin-Misener, K. Kilpatrick, S. Kaasalainen, F. Donald, D. Bryant-Lukosius, P. Harbman, I. Bourgeault and A. DiCenso. 2010. "The Role of Nursing Leadership in Integrating Clinical Nurse Specialists and Nurse Practitioners in Healthcare Delivery in Canada." Canadian Journal of Nursing Leadership 23(Special Issue December): 167–85.
Dawes, H.A., T. Docherty, I. Traynor, D.H. Gilmore, A.G. Jardine and R. Knill-Jones. 2007. "Specialist Nurse Supported Discharge in Gynaecology: A Randomised Comparison and Economic Evaluation." European Journal of Obstetrics Gynecology and Reproductive Biology 130(2): 262–270.
Delamaire, M-L. and G. Lafortune. 2010. Nurses in Advanced Roles: A Description and Evaluation of Experiences in 12 Developed Countries. OECD Health Working Paper No. 54. Retrieved July 12, 2010. <http://www.oecd-ilibrary.org/social-issues-migration-health/nurses-in-advanced-roles_5kmbrcfms5g7-en>.
DiCenso, A., I. Bourgeault, J. Abelson, R. Martin-Misener, S. Kaasalainen, N. Carter, P. Harbman, F. Donald, D. Bryant-Lukosius and K. Kilpatrick. 2010a. "Utilization of Nurse Practitioners to Increase Patient Access to Primary Healthcare in Canada – Thinking Outside the Box." Canadian Journal of Nursing Leadership 23(Special Issue December): 239–59.
DiCenso, A., D. Bryant-Lukosius, I. Bourgeault, R. Martin-Misener, F. Donald, J. Abelson, S. Kaasalainen, K. Kilpatrick, S. Kioke, N. Carter and P. Harbman. 2010b. Clinical Nurse Specialists and Nurse Practitioners in Canada: A Decision Support Synthesis. December 31, 2010. <http://www.chsrf.ca/SearchResultsNews/10-06-01/b9cb9576-6140-4954-aa57-2b81c1350936.aspx>.
DiCenso, A., D. Bryant-Lukosius, R. Martin-Misener, F. Donald, J. Abelson, I. Bourgeault, K. Kilpatrick,N. Carter, S. Kaasalainen and P. Harbman. 2010c. "Factors Enabling Advanced Practice Nursing Role Integration in Canada."Canadian Journal of Nursing Leadership 23(Special Issue December): 211–38.
Donald, F., D. Bryant-Lukosius, R. Martin-Misener, S. Kaasalainen, K. Kilpatrick, N. Carter, P. Harbman, I. Bourgeault and A. DiCenso. 2010a. "Clinical Nurse Specialists and Nurse Practitioners: Title Confusion and Lack of Role Clarity." Canadian Journal of Nursing Leadership 23(Special Issue December): 189–210.
Donald, F., R. Martin-Misener, D. Bryant-Lukosius, K. Kilpatrick, S. Kaasalainen, N. Carter, P. Harbman, I. Bourgeault and A. DiCenso. 2010b. "The Primary Healthcare Nurse Practitioner Role in Canada." Canadian Journal of Nursing Leadership 23(Special Issue December): 88–113.
Erzberger, C. and U. Kelle. 2003. "Making Inferences in Mixed Methods: The Rules of Integration." In A. Tashakkori and C. Teddlie, eds., Handbook of Mixed Methods in Social and Behavioral Research pp. 457–88. Thousand Oaks, CA: Sage Publications.
Fulton, J. S. and K. Baldwin. 2004. "An Annotated Bibliography Reflecting CNS Practice and Outcomes." Clinical Nurse Specialist 18(1): 21–39.
Horrocks, S., E. Anderson and C. Salisbury. 2002. "Systematic Review of Whether Nurse Practitioners Working in Primary Care Can Provide Equivalent Care to Doctors." British Medical Journal 324(7341): 819–23.
Hunsberger, M., A. Mitchell, S. Blatz, B. Paes, J. Pinelli, D. Southwell, S. French and R. Soluk. 1992. "Definition of an Advanced Nursing Practice Role in the NICU: The Clinical Nurse Specialist/Neonatal Practitioner." Clinical Nurse Specialist 6(2): 91–6.
International Council of Nurses. 2008. The Scope of Practice, Standards and Competencies of the Advanced Practice Nurse. Geneva, Switzerland: ICN.
Kaasalainen, S., R. Martin-Misener, K. Kilpatrick, P. Harbman, D. Bryant-Lukosius, F. Donald, N. Carter and A. DiCenso. 2010. "A Historical Overview of the Development of Advanced Practice Nursing Roles in Canada." Canadian Journal of Nursing Leadership 23(Special Issue December): 35–60.
Kilpatrick, K., P. Harbman, N. Carter, R. Martin-Misener, D. Bryant-Lukosius, F. Donald, S. Kaasalainen, I. Bourgeault and A. DiCenso. 2010. "The Acute Care Nurse Practitioner Role in Canada." Canadian Journal of Nursing Leadership 23(Special Issue December): 114–39.
Krichbaum, K. 2007. "GAPN Postacute Care Coordination Improves Hip Fracture Outcomes." Western Journal of Nursing Research 29(5): 523–44.
Martin-Misener, R., D. Bryant-Lukosius, P. Harbman, F. Donald, S. Kaasalainen, N. Carter, K. Kilpatrick and A. DiCenso. 2010. "Education of Advanced Practice Nurses in Canada." Canadian Journal of Nursing Leadership 23(Special Issue December): 61–84.
Mays, N., C. Pope and J. Popay. 2005. "Systematically Reviewing Qualitative and Quantitative Evidence to Inform Management and Policy-Making in the Health Field." Journal of Health Services Research & Policy 10(Suppl. 1): 6–20.
Mitchell-DiCenso, A., G. Guyatt, M. Marrin, R. Goeree, A. Willan, D. Southwell, S. Hewson, B. Paes, P. Rosenbaum, M. Hunsberger and A. Baumann. 1996. "A Controlled Trial of Nurse Practitioners in Neonatal Intensive Care." Pediatrics 98(6): 1143–8.
Pinelli, J. M. 1997. "The Clinical Nurse Specialist/Nurse Practitioner: Oxymoron or Match Made in Heaven?" Canadian Journal of Nursing Administration 10(1): 85–110.
Russell, G., S. Dabrouge, W. Hogg, R. Geneau, L. Muldoon and M. Tuna. 2009. "Managing Chronic Disease in Ontario Primary Care: The Impact of Organizational Factors." Annals of Family Medicine 7(4): 309–18.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed