Healthcare Quarterly
Reflections on Knowledge Translation in Canadian NICUs Using the EPIQ Method
Abstract
The Canadian Neonatal Network conducted a trial of Evidence-Based Practice for Improving Quality (EPIQ) between 2002 and 2005. Improved neonatal intensive care unit (NICU) outcomes established credibility for quality improvement. We surveyed team members and physician leaders to examine critical success factors and barriers to improvement during EPIQ. Respondents agreed that EPIQ had a high utility, was effectively implemented and was a major learning opportunity. The collaborative nature of the project was key to success. Respondents identified the need for additional training and resources in quality improvement. Better communication between clinicians and senior leaders is required to support quality improvement in NICUs.
It has long been recognized that geographical outcome variation is associated with variation in practice and resource utilization (Fisher and Wennberg 2003; Lomas et al. 2005). While standardization and continuous quality improvement have enabled industry to vastly improve quality outcomes (Liker 2004), consistent execution of validated clinical strategies is slow and variable in healthcare, and notable clinical successes are often irreproducible at different locations. Clearly, context is critical in complex social interventions (Berwick 2008; Hillman et al. 2005; Pawson and Tilley 2007; Verhoef and Leis 2008). A variety of research methods may be required to triangulate the evidence required to understand not only what happened, but how (Sharek 2007).
Sankaran et al. (2002) and others (Chien et al. 2002; Evans et al. 2007; Marshall et al. 2005; Richardson et al. 2001; Tarnow-Mordi and Parry 1993) have shown risk-adjusted variation in mortality and morbidity in neonatal intensive care units (NICUs). Synnes et al. (2001) showed that variations in intraventricular hemorrhage rates in Canada were attributable to NICU practice differences. Clearly, opportunities for process improvement exist in many Canadian NICUs (Lee et al. 2000).
Neonatal care in Canada is highly regionalized. Tertiary neonatal care is provided by 30 NICUs that serve distinct geographical regions and coordinate care with a network of primary- and secondary-level facilities. The Canadian Neonatal Network (CNN) is a group of Canadian researchers, founded in 1995 by Dr. Shoo Lee, who collaborate on research issues related to neonatal care. CNN maintains a standardized NICU database that supports local benchmarking, epidemiological research and systems improvement on a national scale. Detailed clinical data are collected on each patient whose NICU stay is equal to or greater than 24 hours, or who dies or is transferred to another level-two or -three facility within 24 hours. All data are cleaned of patient identifiers prior to uploading to the coordinating centre for analyses. Individual patient consent for data collection is not sought. CNN presently includes 29 of 30 tertiary-level NICUs across Canada, though only 17 NICUs were members when the Evidence-Based Practice for Improving Quality (EPIQ) study began. In 2004, CNN received the first Canadian Institutes of Health Research (CIHR) award for knowledge translation.
Twelve CNN NICUs participated in the EPIQ project (Lee et al. 2009) from October 2002 to September 2005, while the other five NICUs acted as a comparison group. The 12 NICUs in this study were major tertiary-level regional NICUs representative of four geographical regions of Canada (two NICUs in British Columbia, four in Prairie provinces, four in Central Canada, two in Atlantic Canada), and included approximately half the tertiary NICU beds in Canada. All NICUs were academic centres. In each unit, an academic neonatologist, who was already affiliated with CNN, led the implementation of the study and established a multidisciplinary team for the purpose. Two NICUs were in stand-alone children's hospitals with independent boards and management; all others were programs or operational divisions of a regional health authority. All but one centre were co-located with obstetrical services. The size and composition of the healthcare team varied among centres and included professionals with a variety of educational backgrounds and countries of origin.
Methods
The primary goal of the EPIQ project was to improve neonatal outcomes in Canadian NICUs. We specifically addressed the incidence of nosocomial infection (NI) and bronchopulmonary dysplasia (BPD). These outcomes were chosen because they are associated with a significant burden of illness, they are clearly defined and their root causes have been extensively researched. We hypothesized that the implementation of the EPIQ method would decrease the incidence of NI and BPD in Canadian NICUs.
Intervention
We have previously demonstrated how multi-level modelling methods can be used to identify practice differences associated with outcome variation for targeted interventions and to quantify their attributable risks (MacNab et al. 2004). Building on these observations, we developed the EPIQ model. EPIQ is based on three pillars: (1) the use of evidence in the published scientific literature, (2) the use of data from participating hospitals to identify hospital specific practices for targeted intervention (gap analysis) and (3) the utilization of a national network to share quality improvement expertise. EPIQ recognizes the importance of local context, customizing interventions and implementation strategies to maximize improvement potential at each hospital, while providing leadership and peer support for ongoing improvement efforts through CNN.
The study intervention has previously been described in detail (Lee et al. 2009). Briefly, 12 participating NICUs were randomly divided into clusters of six. One cluster (the NI group) collaborated to reduce the incidence of NI; the other (the BPD group) collaborated to reduce the incidence of BPD. A third non-randomized comparison group of five NICUs was not involved in any intervention. During the one-year baseline period, education and systematic reviews were conducted; there was a two-year intervention period, during which the infection and pulmonary groups worked independently of each other. Intervention strategies were targeted toward the specific gaps in evidence-based practice found in each NICU; evidence included best practice as described in the literature as well as local data. Clinical data were collected throughout the study period. Each centre participating in this study obtained approval from the local research ethics board.
Investigating Organizational Factors
Based on the literature on change management and implementation of innovations in healthcare (Greenhalgh et al. 2004; Guldbrandsson 2008), a 57-item retrospective survey was developed to assess the perception of team members and physician leaders of the importance of recognized drivers of change during the EPIQ project, using a five-point Likert scale ranging from strongly disagree (one point) to strongly agree (five points). Qualitative comments were also invited. Following the conclusion of the intervention phase of the EPIQ study, consent was obtained to circulate the survey electronically to local investigators as well as to team members at each participating hospital, using Survey Monkey™. All data collection was anonymous. Identical surveys were circulated to local investigators and to other team members. Responses were rated by the degree of agreement with each statement. Attributes were then grouped into seven themes (utility, implementation, communication, teamwork, leadership, system support and competition) and aggregate scores were calculated for each attribute in each group.
Written consent was obtained from a subset of the site investigators for confidential telephone interviews. Focus questions were developed based on the literature, the survey results and input from the director of CNN. Semistructured interviews, lasting 30–45 minutes, were recorded and transcribed. Exploratory description (Speziale and Carpenter 2006) and naturalistic inquiry (Sandelowski 2006) were used to investigate emerging themes.
Funding
The parent study was supported by Grant MOP-53115 from CIHR. Additional funding was provided by individual centres and their foundations. Funding agencies had no role in the study design, data analysis, data interpretation or writing of the report.
Results
Changes in the Process of Care
The consensus lists of practice change strategies developed by the NI and BPD groups, and the prioritization of change strategies, have previously been described (Lee et al. 2009). Each hospital's approach was unique, guided by the gap analysis resulting from the literature review and local data.
Patient Outcomes
In the NI group, there was a significant (p < .01) decrease in the incidence of NI (32% decrease from baseline) during the intervention phase of the study. In the BPD group, there was a significant (p < .01) decrease in the incidence of NI (45% decrease from baseline), BPD (15% decrease from baseline) and death or BPD (12% decrease from baseline). There was no significant change in other secondary outcomes, nor was there any change in primary or secondary outcomes in the non-randomized comparison group.
Survey Results
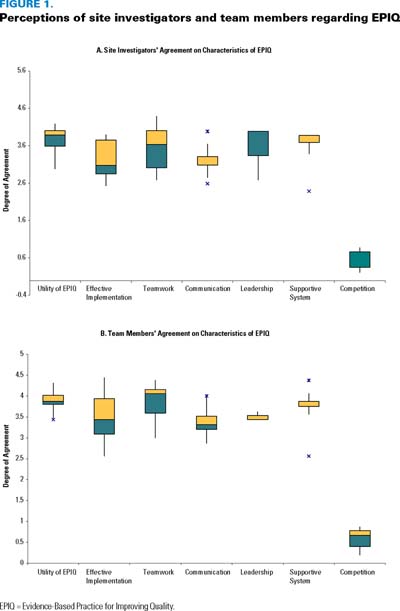
Two groups consisting of 11 site investigators and 16 team members, respectively, completed organizational surveys. Both groups had similar perceptions of the utility of the EPIQ method, effectiveness of implementation at their site, teamwork, communication, leadership, having a supportive organization and the existence of competition between centres. In general, there was moderate to strong agreement that EPIQ was a useful method and was effectively implemented. Respondents assigned low ratings to some drivers of innovation cited in the literature, including adequacy of the budget, the existence of "slack" (the capacity to take on improvement activities) in the unit, technical support and feedback from the coordinating centre, top-down implementation, homogeneity of staff and physicians, competition between centres and peer pressure from other investigators (Figure 1).
Interviews with Site Investigators
Six interviews were conducted with site investigators, all experienced academic neonatologists. Their previous experience with quality improvement varied from minimal to extensive. Two had never attended a quality workshop prior to the study.
Team Composition
While the study protocol provided some direction on the composition of the site teams, respondents reported that team composition was highly site specific. Team size varied from six to 12 people and was not correlated with hospital size. Teams consistently included neonatologists and a variety of nurses, including front-line and advanced practice nurses and nurse educators. Teams addressing NI included infection control personnel, infectious diseases specialists and/or a microbiologist; teams addressing BPD generally included a respiratory therapist. Quality improvement personnel, administrators, nutritionists, data abstractors, executives and residents were less frequent inclusions, and no team included a family member. The composition of some teams changed during the project as members developed different interests, were assigned different responsibilities or left the organization. All but one team confined their administrative input to those with direct responsibility for the NICU, typically the patient care manager or equivalent and the neonatal division head. One team included the chief nursing officer. Site investigators all identified one or more individuals within the team, as well as other front-line staff, who became champions for the project.
Team Learning
For many respondents, EPIQ was their first foray into quality improvement. Among their new insights were the difference between quality improvement and quality assurance, and the importance of an organized team, breaking the process into manageable steps, multiple change cycles, buy-in and visible feedback. Even those who were seasoned administrators indicated that EPIQ had helped them learn how to change the system. The following was among the comments of positive experiences:
"I learned how easy this can be when what you are doing is aligned with the mission and strategic direction of the board, which is sending messaging down to managers – when you have the right people on your team, when they can lead and make decisions and when your unit is not policy bound."
In contrast, another individual stated the following:
"We didn't have the skill set, tools or knowledge to really be effective. There was nobody on the team who had the authorization to make decisions about policy making or financial resources."
Other difficulties cited included the length of time taken to obtain the requisite approvals and the challenges associated with communicating with hundreds of staff. Some investigators were surprised by both the complexity of the system and that the process changes were so rapid:
"I felt that rather than having to push, there was a pull. Outcome changes were so dramatic."
Another investigator was surprised by the ability of a simple audit tool to change practice within a very short time. All respondents strongly felt that the EPIQ approach was helpful in achieving improvement. Specifically, they indicated that bringing different disciplines together "broadens your view of the world about things that physicians and nurses don't learn in their training," providing a "commonality of purpose" and "focusing the team and providing an impetus." Others appreciated the "support and experience of your colleagues across the country to draw on." It was felt that EPIQ helped people "see the possibilities, both as regards innovative processes and better outcomes. I do think it gets their competitive spirit going. When an initiative goes well, it makes the team really proud of their achievements, and that helps morale." "We've made lots of progress," stated another respondent.
Investigators developed an awareness of variation in the results of Plan-Do-Study-Act (PDSA) cycles, some proving effective, some not. They realized that the effectiveness of change management may have impacted outcomes. One noted that natural variation in local outcomes over time tended to mask these effects, making the combined efforts of many centres more valuable in seeing the big picture.
All respondents remarked on the importance of collecting process data that would not normally be collected in the course of clinical care. Indicators that proved useful in specific centres included the number of skin breaks, time between birth and surfactant administration, and number of days on a ventilator. Data were important at all levels:
"Indicators are important: people at the bedside should be aware of process and outcome indicators. We need to bring process measurement to the bedside."
"We had the ability to look at potential changes in a scientific framework."
"Until we got national data back, we didn't realize we didn't benchmark very well. The data provided fuel to go to administration, so they had no excuse not to help. I think those statistics should be in the public domain; and once we had data I would tell parents that we had a high risk of NI."
Inability to access data for timely feedback was seen as a barrier. Sustainability was felt to be a particular challenge for academic centres with a high turnover of trainees.
Drivers of Quality
Several respondents cited leadership, management and strategic directions of the organization:
"The region is very supportive of quality and safety. However, in neonatology, because of our involvement in EPIQ, we are way above other departments. Both administration and people at the bedside are very supportive."
"It was absolutely key that the board had set a new strategic direction on quality. The hospital devoted resources to measurement, and made all managers accountable for improvements in process and outcome in their areas. In this context, EPIQ was a win-win for everyone."
"A third driver was [the principal investigator's] visit. He met with the hospital executive and program leaders. He had great credibility, and this helped us as well as other programs."
Barriers to Quality
There were several comments on the importance of human resources for data collection, communication and administration of the project:
"We needed three things: resources to collect data, to analyze them and turn it into changes and policies and to educate. We got a grant from the foundation, but it was not enough, and to complete the project I was going to have to pay for it out of pocket; but eventually the data convinced the hospital to pay for it."
"Everybody is so work overloaded. A unit of this size merits somebody whose focus is [quality improvement]."
"It's a fairly time-consuming process overall but good value for money."
It became clear that the infrastructure and funding to support quality improvement are highly variable across Canadian NICUs. Respondents perceived that there was little excess capacity to take on quality improvements.
While some noted the importance of visionary leadership, cultural issues, including lack of professionalism, were seen as barriers. Respondents perceived that organizational readiness involved both leadership at the senior management level and an absence of internal barriers to improvement:
"Some units are just not ready for EPIQ. If they do not have the structure, or are policy-driven units, change is very difficult to implement. Some units have bureaucratic and autocratic obstructions to change. The best unit is one where everybody feels valued. Smaller units seem to really jump on it, while bigger units have difficulty."
Quality Management Systems in NICU
The availability of dedicated quality improvement support staff for the NICU varied widely, from none to 2.0 full-time positions. Quality improvement staff included quality improvement nurses, case reviewers reporting to risk management and abstractors. Some units had access to regional resources but did not generally depend on external quality improvement staff to support EPIQ. Some, but not all, NICUs had quality improvement committees, and some established them during the project. One investigator remarked on the paucity of infection control resources, which has been reported across Canada (Zoutman 2009).
Decision Support Tools
These investigators clearly viewed conventional sources of decision support tools as being inadequate to meet the requirements of continuous quality improvement:
"National clinical guidelines are not helpful because they are always out of date. So is the Cochrane Library. Even recent reviews may be out of date."
Few wish lists included complex electronic tools. Rather, they emphasized simple quality tools, timely process information, information exchange and educational tools:
"[We needed] timely reports that could identify the impact of change, the process results of improvement; …virtually no interval between acquisition of the data, analysis and interpretation; … many simple paper decision tools, for example, PDSA forms, skin break audit forms."
"Give people the tools they require to teach their juniors: create [quality improvement] modules for respiratory therapists, nurses and physicians. This teaches the teachers as well, for example, in how to make decisions about infection control."
Investigators reported many structural, process and cultural changes in their units as a result of the EPIQ project:
"There's a much higher level of consciousness about quality. It's discussed on ward rounds and handover rounds. We have a weekly morbidity meeting, Friday for half an hour. The issues are documented and filed for future reference."
"The unit has started using 12 indicators of good practice that are measured on every baby."
Respondents had many excellent suggestions for improvement of the EPIQ process. A major theme was education on quality improvement:
"Train people right from the outset. Physicians aren't taught the basis of quality care and resource utilization. The two go hand in hand; for example, when you order a white blood cell count and differential, the differential may not even be useful in a neonate, but someone in the laboratory spends 20 minutes counting those white cells, time that could be used for something else. Quality needs to be taught in the undergraduate and apprenticeship domains, and in a fundamental way. We make too many cognitive errors."
The importance of communication and data feedback was a common theme. Along with regular teleconferences, it was suggested that there be improved use of a variety of communication methods:
"Involve more nurses and allied health people. Listen to the needs of the stakeholders, and design communications that they need. Increase the rapidity of outcomes feedback. Establish a network of 'go to' people who can provide support for centres and teams who are having problems. Provide a showcase for teams to share their achievements. Use the web more effectively. Make the site more user friendly and use web conferencing and editable document sharing in repositories."
"[Focus groups] really made a difference to buy-in and stimulated dialogue."
Other respondents noted the need to incorporate resourcing of quality management systems into operational budgets and national standards, and the potential payback:
"We need education of the senior leadership team at hospitals so that they see this as a vital part of patient care. We need to get the concept of assessment of outcomes into the minds of people who are making decisions with tight budgets; for example, we've got to convince people that you need to spend 3% of that budget on measuring the outcomes of the other 97%."
"Targets are important, for example, the range of infection rates is A–X. We want to reduce the variation to B–Y nationally. Locally, we want to reduce it to Z."
"Think globally, act locally. Quality is so context sensitive that it cannot be 'controlled' by a national centre. Develop and publish a set of quality management standards for neonatal services. They would include, for example, having quality expertise on site. We could work with Accreditation Canada on this."
Networks
The respondents were unanimous that being part of a collaborative and supportive network of peers and mentors contributed to success:
"We need to build a well-established network of [quality] experts.
"There must be recognition by the local centres that we can't do it alone. It's a combined community project."
Discussion
The EPIQ project brought together teams from a large number of Canadian NICUs to examine the evidence and to identify and correct gaps in their own best practice; it resulted in significant improvement in patient outcomes. The changes made were predominantly process improvements rather than technological innovations. Prior to the study, all units had had opportunities to implement these improvements independently but had not done so. Units that were not involved in the intervention groups had no improvements in outcomes during the course of the study. We can infer, therefore, that involvement in the study itself was the catalyst for change.
In recent years, there has been increased interest in knowledge translation (Straus et al. 2009) and at least two systematic reviews of factors influencing diffusion, implementation and sustainability of innovation in healthcare organizations (Greenhalgh et al. 2004; Robert et al. 2009). It is clear that adoption, implementation and assimilation of change comprise both social and organizational processes. An evidence-based approach to change management must include the improvement of decision-making processes, increasing capacity to absorb new knowledge, ensuring a receptive organizational context for innovation and improving organizational readiness for the specific innovation (Robert et al. 2009). Management literature advocates a combination of strategies to increase organizational readiness, including highlighting the gap between current and desired performance, generating dissatisfaction with the status quo, creating an appealing vision of a desired future state and fostering confidence that the vision is achievable (Armenakis et al. 1993; Kotter 1996; O'Connor and Fiol 2006; Sweeney and Whitaker 1994). Many of these concepts are based on anecdotal experience and are not grounded in research. Weiner (2009) has developed a model of organizational readiness for change, which he defines as a shared psychological state in which organizational members feel committed to implementing an organizational change and confident in their collective abilities. Herscovitch and Meyer (2002) observed that staff can commit to implementing change for a variety of reasons: because they value the change, because they have no choice or because they feel an obligation to do so. Valuing the change reflects the highest commitment to organizational change. The EPIQ process is an appealing method of galvanizing academic physicians to lead change, grounded as it is in their explicit and implicit professional values of delivering evidence-based care.
Weiner (2009) notes that staff take into consideration the organization's structural assets and shortcomings in formulating judgments on the efficacy of change in the particular situation at hand. Change efficacy is higher when people share a sense of confidence that collectively they can implement a complex organizational change. Feedback from team members suggests that the EPIQ structure and process bolstered both teams' knowledge about quality improvement and confidence in their own abilities to effect change.
Insights from the surveys and interviews following the study suggest that many of the cultural drivers of innovation were present in the participating NICUs. The leadership and enthusiasm of staff were evident. However, several barriers were noted. First, neither dedicated expertise nor financial resources for quality were consistently available in Canadian NICUs. Where quality expertise was available, it facilitated improvement. Second, most site investigators were physicians who had received little or no training in quality improvement methods prior to this study. The learning associated with this study enabled them to develop from novices to leaders in quality. Third, the fact that few site investigators engaged senior executives in the project suggests that these physician leaders had a limited understanding of the considerable strategic importance of the EPIQ project to their own organizations, and of the potential benefits of having an ally on the senior management team. In a study of the relationship between information and influence in hospitals conducted in the 1980s, Provan (1991) noted that while physicians had a high degree of clinical autonomy, they were at the lower end of the information gradient with respect to management information, and had the least amount of influence compared with chief executive officers and the board. EPIQ increased physician and team knowledge on best practice, built competencies in quality improvement and change management and facilitated the ability of neonatologists to lead positive change within their units. Models such as EPIQ present excellent opportunities to foster physician leadership skills in quality improvement, which historically has often been viewed by physicians as the domain of other health professionals.
Gittell (2000) described relational coordination as a team competency required to work effectively in service operations that are highly uncertain, interdependent and time constrained, as NICUs typically are. Relational coordination is characterized by frequent, timely problem solving communication and by helping, shared goals, shared knowledge and mutual respect among workers. It is essentially a network of communication and relationship ties among workers and can be thought of as a form of organizational social capital likely to enhance organizational performance. Relational coordination improves service quality and clinical outcomes for patients while reducing lengths of stay (Gittell 2000). We speculate that involvement in EPIQ could increase relational coordination at sites. This is worthy of further study.
Gittell and Weiss (2004) studied networks within and across healthcare organizations and have developed a multi-level framework for intra- and inter-organizational design. They postulated that the elements of organizational design (e.g., routines, information systems, team meetings and boundary spanners) can improve quality and efficiency performance by strengthening networks both within and between organizations.
Lave and Wenger developed the concept of a community of practice (COP), which they defined as "a system of relationships between people, activities, and the world," stating, "developing with time, and in relation to other tangential and overlapping 'communities of practice' is an intrinsic condition of the existence of knowledge" (1991: 89). Wenger (1998) identified main characteristics of COPs and three key dimensions: (1) members interact with one another, establishing norms and relationships through mutual engagement; (2) members are bound together by an understanding of a sense of joint enterprise; and (3) members produce over time a shared repertoire of communal resources, including, for example, language, routines, artifacts and stories. As a long-standing and well-established research collaborative, CNN has contributed to relationship building and the exchange of ideas between investigators and between their sites for over a decade. The EPIQ project effectively leveraged the CNN into a COP.
Roberts (2006) notes that COPs can be applied in a wide variety of organizational settings. For business organizations to fully leverage their knowledge capacities, they must seek to harness COPs that straddle their organizational boundaries. COPs require cultivation if business organizations are to fully exploit their benefits. Roberts cautions that COPs are not stable, that the demise of a community in the social context does not bode well for the adoption of COP, that they may have difficulty developing when the pace of change is accelerating, and that the use of a COP as a tool of knowledge management is likely to be more successful in those regions and nations that have a strong community spirit. We speculate that the existence of a universal healthcare ethos may be conducive to effective use of a COP as a knowledge management tool in the Canadian context.
In a meta-analysis of knowledge transfer (KT) within and between organizations, van Wijk et al. (2008) reviewed 251 effects from 83 independent samples reported in 75 studies. They concluded that organizations and units may equally improve their innovative capacity by leveraging the skills of others through KT, that organizational size positively relates to KT, that ambiguity of knowledge hinders its subsequent transfer and that relational capital is arguably the most important network-level driver of organizational KT both within and across organizations. They recommended that organizations pursuing KT need to focus particularly on developing strong and trustworthy relations, especially within organizational boundaries. At the inter-organizational level, organizations must occupy a central position among many partners. Organizations need to carefully balance external structural and internal relational capital. Cognitive capital seems to be a critical element alongside structural and relational capital. Again, the strong relationships between CNN peers established over a decade were consistent with these drivers of knowledge translation. CNN is now embarking on a second, more advanced EPIQ project that will include both qualitative and quantitative assessments of organizational readiness for change and additional mentorship support for participating teams.
What are the lessons for Canadian healthcare leaders and managers? First, when knowledge translation is effectively implemented, there is tremendous potential for outcome improvement. Second, clinicians have a significant knowledge deficit in the areas of quality improvement and change management. Third, the local quality improvement resources available to Canadian NICUs are uneven and, in many cases, nonexistent. Fourth, a network or COP with effective physician involvement, leadership and well-developed relationships can be a driver of system improvement within and across organizations. Geography is no barrier to improvement. Fifth, lines of communication between clinicians and senior leaders must be strengthened.
Recommendations
Based on our experience, we make the following recommendations to support quality improvement in Canadian healthcare:
- Quality improvement education is required for clinicians of all disciplines and career stages, not just for managers. Physicians in particular need to be better equipped with the knowledge and leadership skills to support continuous improvement.
- Healthcare leaders must evaluate the business case for making significant investments in capacity building in quality improvement and clinician leadership at all levels within their organizations.
- Canadian healthcare organizations should develop, engage in, lead and evaluate outcomes of COPs focused on specific clinical populations. This is particularly important for highly specialized disciplines such as neonatal care, where provincial peer institutions may not exist.
Appendix. The Canadian Neonatal Network EPIQ Study Group
Principal investigator: Shoo K. Lee, MBBS, FRCPC, PhD1
Clinical group: Khalid Aziz, MBBS, FRCPC2; Nalini Singhal, MBBS, FRCPC3; Catherine M. Cronin, MD, MBA, FRCPC, FRCPI, FAAP4; Andrew James, MBChB, MBI, FRACP, FRCPC1; David S.C. Lee, MBBS, FRCPC5; Derek Matthew, MBBS, FRCPC6; Arne Ohlsson, MD, FRCPC, MSc1; Koravangattu Sankaran, MBBS, FRCPC7; Mary Seshia, MBChB, FRCPED4; Anne Synnes, MDCM, FRCPC, MHSc6; Robin Walker, MBChB, FRCPC8; and Robin Whyte, MBBS, FRCPC9
Research Methods Committee: Joanne Langley, MD, FRCPC, MSc9; Ying C MacNab, PhD10; Arne Ohlsson, MD, FRCPC, MSc1; Bonnie Stevens, PhD11; and Peter von Dadelszen, MBChB, DPhil, FRCSC12
Institutions: 1Departments of Paediatrics, University of Toronto, Toronto, Ontario; 2Memorial University, St John's, Newfoundland; 3University of Calgary, Calgary, Alberta; 4University of Manitoba, Winnipeg, Manitoba; 5University of Western Ontario, London, Ontario; 6University of British Columbia, Vancouver, British Columbia; 7University of Saskatchewan, Saskatoon, Saskatchewan; 8University of Ottawa, Ottawa, Ontario; 9Dalhousie University, Halifax, Nova Scotia; 10Department of Health Care and Epidemiology, University of British Columbia; 11Department of Nursing, University of Toronto; 12Department of Obstetrics and Gynecology, University of British Columbia.
About the Author(s)
Catherine Mary Gerard Cronin, MD, MBA, FRCPC, FRCPI, FAAP, is medical director, Perinatal and Child Health Network, at British Columbia's Interior Health.
G. Ross Baker, PhD, is a member of the Department of Health Policy, Management and Evaluation, University of Toronto.
Shoo K. Lee, MBBS, FRCPC, PhD, is a member of the Department of Paediatrics, University of Toronto, in Toronto, Ontario.
Arne Ohlsson, MD, FRCPC, MSc, is a member of the Department of Paediatrics at University of Toronto.
Douglas D. McMillan, MD, FRCPC, is a member of the Department of Pediatrics, Dalhousie University, Halifax, Nova Scotia
Mary M.K. Seshia, MBChB, FRCPED, is a member of the Department of Paediatrics and Child Health at the University of Manitoba.
Acknowledgment
We gratefully acknowledge Robert Liston, Jochen Moehr, Abraham Peliowski, Paul Thiessen and Elizabeth Whynot for their advice and insights; Claudio Martin and Robert Platt, who were members of the Data Monitoring and Safety Committee; and the staff of the Canadian Neonatal Network EPIQ Study Coordinating Center, Sukhy Mahl, Priscilla Chan and Phillip Ye, for their tireless and diligent work.
This study was supported by Grant MOP-53115 from the Canadian Institutes of Health Research. Additional funding was provided by the B.C. Children's Hospital Foundation; Calgary Regional Health Authority; Dalhousie University Neonatal-Perinatal Research Fund; Division of Neonatology, Children's Hospital of Eastern Ontario; Child Health Program, Health Care Corporation of St John's; The Neonatology Program, Hospital for Sick Children; Lawson Research Institute; Mount Sinai Hospital; Ontario Ministry of Health and Long-Term Care; Saint Boniface Hospital, Saint Joseph's Health Centre; University of Saskatchewan Neonatal Research Fund; University of Western Ontario; Victoria General Hospital; and Winnipeg Health Sciences Centre.
References
Armenakis, A.A., S.G. Harris and K.W. Mossholder. 1993. "Creating Readiness for Organizational Change." Human Relations 46(6): 681–703.
Berwick, D. 2008. "The Science of Improvement." Journal of the American Medical Association 299(10): 1182–84.
Chien, L.Y., R. Whyte, P. Thiessen, R. Walker, D. Brabyn, S.K. Lee et al. 2002. "SNAP-II Predicts Severe Intraventricular Hemorrhage and Chronic Lung Disease in the Neonatal Intensive Care Unit." Journal of Perinatology 22(1): 26–30.
Evans, N., J. Hutchinson, J.M. Simpson, D. Donoghue, B. Darlow and D. Henderson-Smart. 2007. "Prenatal Predictors of Mortality in Very Preterm Infants Cared for in the Australian and New Zealand Neonatal Network." Archives of Disease in Childhood – Fetal and Neonatal Edition 92: F34–40.
Fisher, E.S. and J.E. Wennberg. 2003. "Health Care Quality, Geographic Variations, and the Challenge of Supply-Sensitive Care." Perspectives in Biology and Medicine 46(1): 69–79.
Gittell, J.H. 2000. "Organizing Work to Support Relational Coordination." International Journal of Human Resource Management 11(3): 517–39.
Gittell, J.H. and L. Weiss. 2004. "Coordination Networks within and across Organizations: a Multi-level Framework." Journal of Management Studies 41(1): 127–53.
Greenhalgh, T., G. Robert, F. MacFarlane, P. Bate and O. Kyriakidou. 2004. "Diffusion of Innovations in Service Organizations: Systematic Review and Recommendations." Milbank Quarterly 82(4): 581–629.
Guldbrandsson, K. 2008. From News to Everyday Use: The Difficult Art of Implementation. Östersund, Sweden: Swedish National Institute of Public Health.
Herscovitch, L. and J.P. Meyer. 2002. "Commitment to Organizational Change: Extension of a Three-Component Model." Journal of Applied Psychology 87(3): 474–87.
Hillman, K., J. Chen, M. Cretikos, R. Bellomo, D. Brown, G. Doig et al. 2005. "Introduction of the Medical Emergency Team (MET) System: A Cluster Randomized Controlled Trial." Lancet 365(9477): 2091–97.
Kotter, J.P. 1996. Leading Change. Cambridge, MA: Harvard Business Press.
Lave, J. and E. Wenger. 1991. Situated Learning: Legitimate Peripheral Participation. Cambridge, UK: Cambridge University Press. Page 89.
Lee, S.K., D.D. McMillan, A. Ohlsson, M. Pendray, A. Synnes, R. Whyte et al. 2000. "Variations in Outcomes and Practices in the Canadian NICU Network: 1996–1997." Pediatrics 106(5): 1070–79.
Lee, S.K., K. Aziz, N. Singhal, C.M. Cronin, A. James, D.S.C. Lee et al. 2009. "Improving the Quality of Care for Infants: a Cluster Randomized Controlled Trial." Canadian Medical Association Journal 181(8): 469–76. DOI: 10.1503/cmaj.081727.
Liker, J.K. 2004. The Toyota Way: 14 Management Principles from the World's Greatest Manufacturer. New York: McGraw-Hill Professional.
Lomas, J., T. Culyer, C. McCutcheon, L. McAuley and S. Law. 2005. Conceptualizing and Combining Evidence for Health System Guidance. Ottawa, ON: Canadian Health Services Research Foundation.
MacNab, Y.C., Z.G. Qiu, P. Gustafson, C.B. Dean, A. Ohlsson and S.K. Lee. 2004. "Hierarchical Bayes Analysis of Multilevel Health Services Data: A Canadian Neonatal Mortality Study." Health Services and Outcomes Research Methodology 5: 5–26.
Marshall, G., J.L. Tapia, I. D'Apremont, C. Grandi, C. Barros, A. Alegria et al. 2005. "A New Score for Predicting Neonatal Very Low Birth Weight Mortality Risk in the NEOCOSUR South American Network." Journal of Perinatology 25: 577–82.
O'Connor, E.J. and C.M. Fiol. 2006. "Creating Readiness and Involvement." Physician Executive 32(1): 72–74.
Pawson, R. and N. Tilley. 2007. Realistic Evaluation. London: Sage Publications.
Provan, K.G. 1991. "Receipt of Information and Influence over Decisions in Hospitals by the Board, Chief Executive Officer and Medical Staff." Journal of Management Studies 28(3): 281–98.
Richardson, D.K., J.D. Corcoran, G.J. Escobar, S.K. Lee, for the Canadian NICU Network, the Kaiser Permanente Neonatal Minimum Data Set Wide Area Network et al. 2001. "SNAP-II and SNAPPE-II – Newborn Illness Severity and Mortality Risk Scores." Journal of Pediatrics 138: 92–100.
Robert, G., T. Greenhalgh, F. MacFarlane and R. Peacock. 2009. Organisational Factors Influencing Technology Adoption and Assimilation in the NHS: A Systematic Literature Review. Report for the National Institute for Health Research Service Delivery and Organization Programme. Cambridge, United Kingdom: Queen's Printer and Controller.
Roberts, J. 2006. "Limits to Communities of Practice." Journal of Management Studies 43(3): 623–39.
Sandelowski, M. 2000. "Whatever Happened to Qualitative Description?" Research in Nursing and Health 23(4): 334–40.
Sankaran, K., L.Y. Chien, R. Walker, M. Seshia, A. Ohlsson and S.K. Lee. 2002. "Variations in Mortality Rates among Canadian Neonatal Intensive Care Units." Canadian Medical Association Journal 166: 173–78.
Sharek, P.J., L.M. Parast, K. Leong, J. Coombs, K. Earnest, J. Sullivan et al. 2007. "Effect of a Rapid Response Team on Hospital-Wide Mortality and Code Rates Outside the ICU in a Children's Hospital." Journal of the American Medical Association 298(19): 2267–74.
Speziale, H.J. and D.R. Carpenter. 2006. Qualitative Research in Nursing: Advancing the Humanistic Imperative. Philadelphia: Lippincott.
Straus, S.E., J. Tetroe and I. Graham. 2009. "Defining Knowledge Translation." Canadian Medical Association Journal 181(3–4): 165–68.
Synnes, A.R., L.Y. Chien, A. Peliowski, R. Baboolal, S.K. Lee and the Canadian Neonatal Network. 2001. "Variations in Intraventricular Hemorrhage Incidence Rates among Canadian Neonatal Intensive Care Units." Journal of Pediatrics 138(4): 525–31.
Tarnow-Mordi, W.O. and G. Parry. 1993. "The CRIB Score." Lancet 342(8883): 1365.
Van Wijk, R., J.J.P. Jansen and M.A. Lyles. 2008. "Inter- and Intra-organizational Knowledge Transfer: A Meta-analytic Review and Assessment of Its Antecedents and Consequences." Journal of Management Studies 43(4): 830–53.
Verhoef, M.J. and A. Leis. 2008. "From Studying Patient Treatment to Studying Patient Care: Arriving at Methodologic Crossroads." Hematology Oncology Clinics of North America 22(4): 671–82, viii–ix.
Weiner, B.J. 2009. "A Theory of Organizational Readiness for Change." Implementation Science 4: 67. DOI:10.1186/1748-5908-4-67.
Wenger, E. 1998. Communities of Practice: Learning, Meaning and Identity. Cambridge, United Kingdom: Cambridge University Press.
Zoutman, D.E. and B.D. Ford. 2009. "A Comparison of Infection Control Program Resources, Activities, and Antibiotic Resistant Organism Rates in Canadian Acute Care Hospitals in 1999 and 2005: Pre- and Post-severe Acute Respiratory Syndrome." Canadian Journal of Infection Control 24(2): 109–15.
Footnotes
*See Appendix at http://www.longwoods.com/content/22539
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed