Healthcare Quarterly
Integrated Complex Care Model: Lessons Learned from Inter-organizational Partnership
Eyal Cohen, Cindy Bruce-Barrett, Shauna Kingsnorth, Krista Keilty, Anna Cooper and Stacey Daub
Abstract
Providing integrated care for children with medical complexity in Canada is challenging as these children are, by definition, in need of coordinated care from disparate providers, organizations and funders across the continuum in order to optimize health outcomes. We describe the development of an inter-organizational team constructed as a unique tripartite partnership of an acute care hospital, a children's rehabilitation hospital and a home/community health organization focused on children who frequently use services across these three organizations. Model building and operationalization within the Canadian healthcare system is emphasized. Key challenges identified to date include communication and policy barriers as well as optimizing interactions with families; critical enablers have been alignment with policy trends in healthcare and inter-organizational commitment to integrate at the point of care. Considerations for policy developments supporting full integration across service sectors are raised. Early indicators of success include the enrolment of 34 clients and patients and the securing of funds to evaluate and expand the model to serve more children.
Medical and technological advances continue to reduce childhood mortality rates, resulting in a dramatic increase in the prevalence of children with medical complexity (CMC) (Cohen et al. 2011; Wise 2004). Examples vary and include children with congenital or acquired brain injuries and significant medical and neuro-developmental sequelae, as well as children with multi-system conditions and associated feeding, respiratory and developmental health issues. CMC form a vulnerable group characterized by substantial health needs and complex and/or chronic underlying conditions that require highly specialized care and services over many years by multiple providers in many different settings.
Imperative to Change
Although CMC represent a small minority, they use exceedingly disproportionate and growing amounts of healthcare spending. In a large sample of American children's hospitals in 2006, these children accounted for 10% of admissions, 26% of hospital days, 40% of hospital charges and 73–92% of different forms of technology assistance (e.g., gastrostomy and tracheostomy tubes; Simon et al. 2010). CMC now account for more than half of childhood deaths from medical causes outside the perinatal period (Feudtner et al. 2002).
While the amount of care these children receive is substantial, the quality of care delivered is largely suboptimal. Many CMC are subject to prolonged and multiple hospitalizations and are often readmitted to hospital for the same underlying problem (Berry et al. 2011). The scope of their healthcare needs places extraordinary stress on caregivers (Raina et al. 2005). In one study, over half of parental caregivers reported that a family member had quit their job because of their child's health demands (Kuo et al. in press). Coordination of care in concert with the needs of these children and their families is extremely challenging (Dosa et al. 2001; Matlow et al. 2006) and, if not done well, leads to untimely delays, fragmented communication, medical errors (Sacchetti et al. 2000; Slonim et al. 2003), dissatisfied patients and families, poor health outcomes (Kelly et al. 2002; Srivastava et al. 2005) and inefficient and costly use of health resources (Gordon et al. 2007).
Focus on Integration
Traditional paradigms of complex care management have focused on a single community-based primary care provider. This provider, usually a pediatrician or family physician, is responsible for all aspects of primary care as well as the coordination of referrals to community and hospital specialists. It is now generally accepted that the notion of a single provider being armed with sufficient knowledge and access to systems of healthcare, social services and educational supports for CMC may be unrealistic and misguided (King and Meyer 2006). While primary care reform initiatives across Canada have aimed to provide a team-based orientation to the care of patients, these models have not concentrated on the unique needs of children, in particular those with complex health needs (Miller et al. 2004). Given the frequent interface of CMC with the entire continuum of care (i.e. acute, home, primary and rehabilitation care sectors), it is imperative to promote integration that allows families to navigate the complex labyrinth of services and providers, creates value, reduces costs and ultimately improves child and family outcomes.
The promise of integrated care is substantial (Table 1). This premise was fundamental to the creation of the Integrated Complex Care Model (ICCM) and has revealed some positive outcomes as observed in practice during the early stages of model implementation.
| TABLE 1. Benefits and observations of the Integrated Complex Care Model | ||
| Target | Proposed Benefits | Observations in Practice |
| Child and family | Seamless care, better outcomes, less time-consuming, less stressful |
Active engagement in goal setting and care planning Better alignment and timing of interactions at key transition points (i.e., home to hospital, hospital to home, hospital to hospital) Child- and family-centred approach focused on health needs versus diagnosis |
| Front-line provider | Ability to work across traditional professional/organizational boundaries, better job satisfaction |
Opportunities for ongoing team building and education Coaching and mentorship to build skill and capacity Improved communication (i.e., provider to child/family, provider to provider) |
| Organization | Alignment of organizational goals, coordinating targets, activities and processes |
Improved efficiency of care and service delivery Optimized process and resource use Collective vision and demonstrable support for integration efforts impacting quality of care |
| Funder | Developing system-wide solutions based primarily on leveraging existing system resources, clear accountabilities about system performance and evaluation |
Improved cost-effectiveness by maximizing resources across the continuum Opportunity to leverage existing information systems and technology (e.g., Ontario's electronic Child Health Network) |
| Policy maker | Promoting and enabling effective service models and surrounding these with appropriate incentive and funding models | Local policy and practice changes to better support seamless integration (i.e., information management, confidentiality, sharing of health records) |
ICCM: Creation
In 2009, the Toronto Central Local Health Integration Network (TC-LHIN), one of the 14 regional health networks in Ontario, launched a strategic initiative titled Integrated Care for Complex Populations. The initiative's mandate was to improve system sustainability by focusing on integrated care for select high-risk populations in the system. CMC, specifically medically fragile or technology-dependent children, was the sole pediatric population identified among five target populations. In order to develop a feasible, sustainable integration model for CMC within the TC-LHIN, an innovative and voluntary partnership was established engaging three organizations involved in providing care and service for this vulnerable population. These organizations included a children's hospital (The Hospital for Sick Children), a pediatric rehabilitation hospital (Holland Bloorview Kids Rehabilitation Hospital) and a key organization that connects children to home care and other community services (Toronto Central Community Care Access Centre). Over the course of six months, team members across each partner organization sought input from a wide variety of stakeholders (e.g., primary care physicians, nursing agencies, patients and their families etc.) in order to develop the ICCM, which focused on integration at the point of care for CMC.
Specifically, the overarching goals of the ICCM were the following:
- Improved co-operation between organizations
- Better coordination across settings and levels of care
- Greater focus on children's health needs as opposed to medical conditions
- Maximized accessibility and minimized duplication of services and resources
- Enhanced outcomes for children with complex, chronic health issues
ICCM: Operationalization
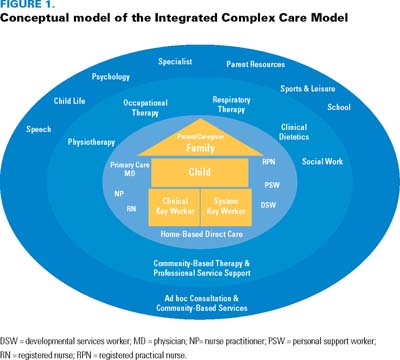
The ICCM creates a circle of partnerships that surround the child and family, providing holistic care that is "accessible, continuous, comprehensive, compassionate, coordinated, family-centred and culturally effective" (Homer et al. 2008: e922). Through inter-professional assessments, the coordination of relevant investigations, the sharing of information, the setting of mutual goals and the execution of treatment plan options in varied sectors and settings (Figure 1), the child and family are encouraged to participate and contribute in the design and plan of care based on changing needs and concerns. This approach promotes more collaborative care management among providers and also helps build the child's and family's confidence and capacity for managing care.
The model is formulated around the concept of a "key worker"' for the child and family, acknowledging the need for a lead who assumes responsibility for ensuring coordination, communication and follow-through with the plan of care. Without such a lead, assumptions may be made as to roles and accountabilities, leaving the child and family at risk of "falling through the cracks." The key worker acts as the family's single point of contact within healthcare and across other systems (education, social services, financial resources, recreation, transportation, etc).
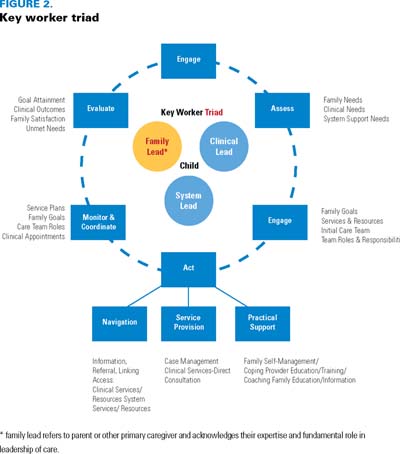
Previous iterations of key workers in complex care models focused on either a single clinician, such as a nurse practitioner (Cohen et al. 2010; Rahi et al. 2004), or a community-based case manager (King and Meyer 2006). However, the end result of the ICCM partnership between hospitals and the community required the realignment of existing resources and led to the articulation of a two-person key worker team functioning with a family lead as part of a triad (Figure 2). In this model, a clinical key worker (CKW), who has a prominent focus on clinical needs, and a system key worker (SKW), who concentrates primarily on the system needs including community resources, work together with a family member who has the most direct knowledge and responsibility for meeting the child's health needs.
The CKW is a pediatric nurse with advanced skills and education in the provision of holistic care for this population of patients. Serving as a critical guide in helping lead the clinical care of the complex child, the CKW has comprehensive knowledge and understanding of various disease processes and the subsequent effects on these children. The CKW carries out many responsibilities including performing telephone triage, making clinical decisions, coordinating healthcare and assisting families to plan for key transitions. The CKW also ensures that there is an "interface" between the child, family, providers and key services and organizations, working in concert with the SKW.
The SKW is a community care coordinator designated to provide case management services to children with complex care needs. The SKW coordinates cross-sectoral services, makes referrals, secures relevant resources and assists families to plan and navigate the system. The SKW works with the CKW to provide ongoing collaborative support.
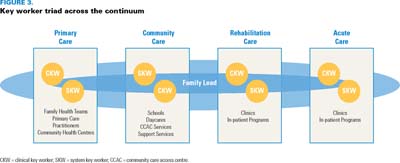
Key workers are expected to work independently, meeting regularly with each other. One key worker may assume a more prominent role at different times across the child and family's continuum of care (Figure 3), but the family is always involved in leading care planning, decision-making and coordination. The key workers are not co-located – both are housed in their own employment setting. Their communication can be conducted in person, via the telephone, by secure e-mail or through an electronic portal.
The frequency of key workers' contact with the child and family is individualized based on the goals and service needs. The key worker team is expected to formally connect with each other in the following situations:
- A transition is anticipated, such as an agency admission or discharge, a move to the adult system, entrance to school or daycare, a move to another LHIN, a change of primary care practitioner etc.
- There is a change in the child or family's situation or health status that requires a review of the goals, services or care team.
- There is an admission to hospital (planned or unexpected).
- The family requests a care conference.
- A scheduled review of the child and family's plan or services has been pre-determined.
Other operational components and guiding principles of the ICCM are summarized in Table 2.
| TABLE 2. Components of the Integrated Complex Care Model | ||
| Components | Rationale | |
| Shared care | The right people, with the right information, doing the right things, in the right order, at the right time. This principle recognizes that no one organization, discipline or provider can adequately meet all the needs of the chronically ill child and family. It also acknowledges that inefficiencies commonly occur when multiple organizations independently try to tackle complex health problems in a child. For these reasons, this component speaks to the need to promote complex medical support in a variety of settings including acute care hospitals, transitional care settings and the community. | |
| Team-based care | This component envisions a multidisciplinary team that uses the unique skills of team members; involving expertise from a number of different disciplines (e.g., nursing, occupational therapy, physiotherapy, medicine, dietetics, respiratory therapy, education, social work and personal support) across organizations and sectors. It recognizes that not every team member needs to be involved in the care of every child. Sufficient flexibility needs to be developed in the construction of the team to ensure that each child receives appropriate care delivery:
|
|
| Joint accountability | This component removes the traditional barriers of silos to integrated care that occur when providers are accountable to a single organization (e.g., a hospital, or a community agency). A successful model allows (and promotes) the movement of team members with the child to the multiple locations of care wherever it is provided; and that partnering organizations facilitate this by sharing resources for the seamless provision of care. This component requires innovative partnership between hospitals, community care access centres and other providers/agencies. | |
| Electronic care plans | Co-created by family and key workers, this document contains salient medical and psycho-social information including an updated list of medications, care providers and appointments as well as goals of care. Copies of the care plan will be provided to families and placed in the health record and will be accessible to providers in a both community and hospital settings through an existing platform – the Ontario Electronic Child Health Network. | |
ICCM: Evaluative Framework
The Institute for Healthcare Improvement (IHI) believes that optimization of the health system must consider the simultaneous pursuit of three aims: a better care experience for individuals, better health for defined populations and reduced, or at least controlled, per capita cost of care. This framework, referred to as the IHI Triple Aim (IHI 2011), serves as a basis for the ICCM evaluation, which includes a combination of quantitative and qualitative methods to collect data for analysis. The impact of the ICCM is being evaluated based on the effectiveness of healthcare quality with respect to family centredness of care, family function and quality of life (parental and child); the efficiency of health resource use as measured by emergency department visits, hospitalization days and use of rehabilitation services; and care coordination experience as measured by interviews with families and clinical staff and care plan reviews. Thirty-four children and families have been enrolled in the model and will be contributing to the evaluation.
ICCM: Reflections on Model Building
Enablers
The sustainability of the model is facilitated by a number of important enablers, including alignment with policy priorities and integration at the point of care.
Alignment with Policy Priorities
High-level integration of care across organizations and across the cycle of care has been recognized as an important health policy priority for complex client populations. In particular, the creation of true value for clients and families is now increasingly being driven by incentives to find system efficiencies. Aspects of the ICCM have already been espoused by other LHINs in Ontario (e.g., Champlain [Ottawa]), and there is a strong interest in expanding into other jurisdictions as well.
Integration at the Point of Care
A cardinal feature of the ICCM is a unique and voluntary integration of multiple partners across the healthcare continuum (hospital to community; hospital to hospital) who are motivated to develop a useful and sustainable model of care for CMC and replace existing models that have been perceived as suboptimal. The ICCM has been designed with the aim to enable children, families and healthcare providers to cross traditional organizational barriers, and to create a new cadre of empowered advocates to promote and sustain integrated care.
Opportunities
Many of the barriers encountered in the care of CMC have served as the impetus for change and ongoing development of the ICCM. A number of challenges remain; however, concerted efforts have been directed toward leveraging opportunities for improvement, specifically related to information management, infrastructure, scalability and family centredness.
Communication Strategies
Given the number of providers, sectors and levels of care involved in effectively managing CMC, the tools and technology required to support communication and collaboration are key to enabling the seamless coordination of care. Information management has been the biggest challenge for the key worker team and represents an issue that is common to all integration initiatives. Efforts are being directed to overcome this, leveraging existing systems and technology both from within and across the partner organizations (e.g., Ontario's electronic Child Health Network). Key learnings from model implementation can help inform and influence the implementation of a comprehensive, information-management solution with broad utility for providers, patients and families.
Policy Barriers
Policy barriers that are real, perceived or potential pose a threat to the delivery of coordinated, family-centred care and service. Privacy associated with integration and information management, limited use of non-regulated providers, a lack of family-directed funding models, capitation to available services, shortages of pediatric home care providers and outdated coverage by insurance carriers have been noted as barriers impacting the ability to extend the level of community-based care that is required to keep CMC at home and in their own community. As well, engagement of broader team members and resources beyond the key workers has been identified as critical in order to achieve the level of seamless integration required for this population (i.e., service providers, primary care, inter-professional teams, community resources and agencies). The next phase of ICCM operationalization will concentrate on the engagement of the broader team to advance integration beyond the key worker dyad and a robust evaluation that will reveal specific policy and process issues impacting CMC to inform policy directions at local and provincial levels.
Interfacing with Families
The ICCM has identified the need for more creative strategies to engage CMC and their families (i.e., via e-mail, telephone, coordinating with other appointments, telemedicine) in goal setting and planning care at key transition points in healthcare over time (e.g., preschool to school age) and place (e.g., hospital to home). Past models and interventions built within traditional paradigms, where the focus has been on family meetings, are no longer sufficient, particularly when families are not available for a home visit due to work, school and real-life limitations. As a result, the key workers endeavour to maximize opportunities for collaboration with children and families during existing visits and activities (i.e., at home, school, hospital), at critical points of transition (discharge, admission, transfer) and through interactions by telephone, teleconference and tele–home care.
Conclusions and Future Projections
The "system" of healthcare is currently somewhat of a misnomer because of silos that continue to impede the delivery of seamless, comprehensive child- and family-centred care. The ICCM is a promising model highlighting the potential of a true system to effectively integrate complex care delivery across organizational structures, service sectors and regional boundaries.
A predicted growth in numbers of CMC, combined with concerns of escalating costs and "balkanization" across essential interfacing sectors (health, education and social services), provides the impetus for a continued evolution of systems to provide value across the entire cycle of care from the hospital to the community (Porter 2009). The TC-LHIN remains committed to integrative care efforts and has approved the expansion and ongoing evaluation of the ICCM to include 50 children by the end of 2011. This commitment, along with the foundational principles established by the ICCM, bodes well for further development and replication of the model to facilitate delivery of care as close to home as possible for diverse populations whenever integration is essential to optimal health outcomes.
About the Author(s)
Eyal Cohen, MD, MSc, FRCP(C), is a member of the Division of Pediatric Medicine at The Hospital for Sick Children and the Departments of Pediatrics and Health Policy, Management and Evaluation, University of Toronto, in Toronto, Ontario. Dr. Cohen can be reached at 416-813-7654, ext. 2626, or by e-mail at eyal.cohen@sickkids.ca.
Cindy Bruce-Barrett, RN, BScN, MN, PMP, works in corporate strategy and performance at The Hospital for Sick Children, in Toronto, Ontario.
Shauna Kingsnorth, PhD, is a member of the Bloorview Research Institute, Holland Bloorview Kids Rehabilitation Hospital, in Toronto, Ontario.
Krista Keilty, MN, NP-Paeds, works as a nurse practitioner at The Hospital for Sick Children, University of Toronto in Toronto, Ontario.
Anna Cooper, RN, MN, works in client services at the Toronto Central Community Care Access Centre (CCAC), in Toronto, Ontario.
Stacey Daub, MA, MBA, is chief executive officer of the Toronto Central CCAC, in Toronto, Ontario.
Acknowledgment
We wish to thank Betty Winsor-Stallan, Mary French May, Suzanne Breton and the other members of the ICCM project team for their contributions to the development of the model and the ideas expressed in this paper.
The evaluation of the ICCM is being supported by the Norman Saunders Complex Care Initiative through the SickKids Foundation and from the Value and Affordability Task Force in Pediatrics through the Toronto Central LHIN.
References
Berry, J.G., D.E. Hall, D.Z. Kuo, E. Cohen, R. Agrawal, C. Feudtner et al. 2011. "Hospital Utilization and Characteristics of Patients Experiencing Recurrent Readmissions within Children's Hospitals." Journal of the American Medical Association 305(7): 682–90.
Cohen, E., D. Kuo, R. Agrawal, J. Berry, T. Simon, S. Bhagat et al. 2011. "Children with Medical Complexity: An Emerging Population for Clinical and Research Initiatives." Pediatrics 127(3): 529–38.
Cohen, E., J.N. Friedman, S. Mahant, S. Adams, V. Jovcevska and P. Rosenbaum. 2010. "The Impact of a Complex Care Clinic in a Children's Hospital." Child Care Health and Development 36(4): 574–82.
Dosa, N., N. Boeing and R. Kanter. 2001. "Excess Risk of Severe Acute Illness in Children with Chronic Health Conditions." Pediatrics 107(3): 499–504.
Feudtner, C., M.J. Silveira and D.A. Christakis. 2002. "Where Do Children with Complex Chronic Conditions Die? Patterns in Washington State, 1980–1998." Pediatrics 109(4): 656–60.
Gordon, J., H. Colby, T. Bartelt, D. Jablonski, M. Krauthoefer and P. Havens. 2007. "A Tertiary Care-Primary Care Partnership Model for Medically Complex and Fragile Children and Youth with Special Health Care Needs." Archives of Pediatric and Adolescent Medicine 161(10): 937–44.
Homer, C.J., K. Klatka, D. Romm, K. Kuhlthau, S. Bloom, P. Newacheck et al. 2008. "A Review of the Evidence for the Medical Home for Children with Special Health Care Needs." Pediatrics 122(4): e922–37.
Institute for Healthcare Improvement. 2011. The IHI Triple Aim. Cambridge, MA: Author. Retrieved June 2011. <http://www.ihi.org/offerings/Initiatives/TripleAim/Pages/default.aspx>.
Kelly, A.M., B. Kratz, M. Bielski and P.M. Rhinehart. 2002. "Implementing Transitions for Youth with Complex Chronic Conditions Using the Medical Home Model." Pediatrics 110(6): 1322–27.
King, G. and K. Meyer. 2006. "Service Integration and Co-ordination: A Framework of Approaches for the Delivery of Co-ordinated Care to Children with Disabilities and Their Families." Child Care Health and Development 32(4): 477–92.
Kuo, D., E. Cohen, R. Agrawal, J.G. Berry and P. Casey. In press. "National Profile of Caregiver Challenges of More-Complex Children with Special Health Care Needs." Archives of Pediatric and Adolescent Medicine.
Matlow, A., J. Wright, B. Zimmerman, K. Thomson and M. Valente. 2006. "How Can the Principles of Complexity Science Be Applied to Improve the Coordination of Care for Complex Pediatric Patients?" Quality and Safety in Health Care 15(2): 85–88.
Miller, A.R., M.A. Recsky and R.W. Armstrong. 2004. "Responding to the Needs of Children with Chronic Health Conditions in an Era of Health Services Reform." Canadian Medical Association Journal 171(11): 1366–67.
Porter, M.E. 2009. "A Strategy for Health Care Reform – Toward a Value-Based System." New England Journal of Medicine 361(2): 109–12.
Rahi, J.S., I. Manaras, H. Tuomainen and G.L. Hundt. 2004. "Meeting the Needs of Parents around the Time of Diagnosis of Disability among Their Children: Evaluation of a Novel Program for Information, Support, and Liaison by Key Workers." Pediatrics 114(4): e477–82.
Raina, P., M. O'Donnell, P. Rosenbaum, J. Brehaut, S. Walter, D. Russell et al. 2005. "The Health and Well-Being of Caregivers of Children with Cerebral Palsy." Pediatrics 115(6): e626–36.
Sacchetti, A., C. Sacchetti, C. Carraccio and M. Gerardi. 2000. "The Potential for Errors in Children with Special Health Care Needs." Academy of Emergency Medicine 7(11): 1330–33.
Simon, T.D., J. Berry, C. Feudtner, B.L. Stone, X. Sheng, S.L. Bratton et al. 2010. "Children with Complex Chronic Conditions in Inpatient Hospital Settings in the United States." Pediatrics 126(4): 647–55.
Slonim, A., B. LaFleur, W. Ahmed and J. Joseph. 2003. "Hospital-Reported Medical Errors in Children." Pediatrics 111(3): 617–21.
Srivastava, R., B. Stone and N. Murphy. 2005. "Hospitalist Care of the Medically Complex Child." Pediatric Clinics of North America 52: 1165–87.
Wise, P.H. 2004. "The Transformation of Child Health in the United States: Social Disparities in Child Health Persist Despite Dramatic Improvements in Child Health Overall." Health Affairs 23(5): 9–25.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed