Healthcare Policy
Inequity in Access to Guideline-Recommended Colorectal Cancer Treatment in Nova Scotia, Canada
André R. Maddison, Yukiko Asada, Robin Urquhart, Grace Johnston, Frederick Burge and Geoff Porter
Abstract
Cancer continues to be one of the heaviest burdens of disease in Canada, and assessing potential inequities in access to cancer care may serve as a barometer of the health of Canadian health systems. This study tackled three limitations of the current literature by clearly differentiating between inequality and inequity, by assessing inequity in receipt of care and wait times for care, and by taking advantage of inequity indices to enhance comparability of inequities between studies and populations. We measured income-, age-, sex- and distance-related inequities among colorectal cancer (CRC) patients in Nova Scotia by accounting for clinical guidelines and patient need. Results reveal statistically significant inequity in access to chemotherapy and radiotherapy for CRC by age, sex and distance, but not income. This study demonstrates the importance of carefully examining inequity in access to cancer care and highlights one method to report and compare inequities with conceptual clarity.
Colorectal cancer (CRC) is the third most common cancer in Canada, with an estimated 22,200 new cases in 2011 (Canadian Cancer Society 2011). Incidence is approximately equal for men and women, and five-year relative survival rates average 63% (Canadian Cancer Society 2011). Surgery is the primary treatment for CRC in conjunction with adjuvant chemotherapy and neo-adjuvant radiotherapy, depending on disease site and tumour stage. Although early diagnosis and survival rates of CRC have improved over the past decade (Canadian Cancer Society 2011), studies continue to identify variations in access to CRC services by, for example, patients' income, age and geographic location (Cree et al. 2009; Singh et al. 2010; Winget et al. 2010). Ensuring equitable access – equal access for equal need – is of particular importance for CRC care given its complexity and time sensitivity. Delays in access to services along the continuum of care affect the progression of treatment and are linked to negative patient outcomes (Berrino et al. 2007; Cheung et al. 2009; Gatta et al. 2000; Hershman et al. 2006). The complexity and multidisciplinary nature of cancer treatment makes provision of equitable care a challenge and necessitates a clear understanding of where along the continuum of care inequity occurs. Identification of inequities along the CRC continuum of care is a critical step in planning clinical interventions and policies to reduce inequities.
There is a distinction between inequity and inequality. Inequality in access to healthcare implies that there are individual differences in access to services. Inequity in access, on the other hand, means that variations in access to care are ethically problematic or of social concern. The distinction between inequality and inequity is often made based on the factors that contribute to the variation in access to care. Inequalities in access are caused by both need factors (those that reasonably influence an individual's access) and non-need factors (those that should not influence an individual's access). In contrast, inequities in access to healthcare are caused by non-need factors, after controlling for all need factors.
This study reports income-, age-, sex- and distance-related inequities in access to chemotherapy and radiotherapy among CRC patients in Nova Scotia, Canada, using a rich, population-based administrative data set containing tumour stage information. Our inequity analysis addresses the following three limitations of previous studies:
- Receipt of care and wait time represent different dimensions of care and often show different magnitudes of inequity, yet are rarely examined together (Maddison et al. 2011). In this study, we separately assessed inequity in receipt of chemotherapy and radiotherapy and wait time for radiotherapy.
- The current literature does not clearly distinguish between inequalities and inequities in access to care, thereby making it difficult to identify whether access is simply unequal or is ethically problematic. In this study, we made the distinction clear by incorporating clinical practice guidelines into our analyses and adjusting for need factors – factors whose influence on patients' access to care is generally considered reasonable (e.g., tumour stage and co-morbidities). Our approach extended a need-standardization method – an established method for equity analysis in population-based studies – to clinical data.
- Current studies examining inequity in access to cancer care have yet to take advantage of inequity indices that an increasing number of population-based analyses employ to enhance comparability of the degree of inequities between studies and populations (Allin 2008; van Doorslaer et al. 2006; Wagstaff et al. 1991). We calculated the Horizontal Inequity Index (HI) (van Doorslaer et al. 2006), a widely used index in population-based inequity analyses, to compare inequities in CRC care between receipt of chemotherapy and radiotherapy and wait time for radiotherapy across different dimensions of inequity (i.e., income, age, sex and distance).
Methods
Data and study population
Data for this study came from the ACCESS (Access to Colorectal Cancer Services in Nova Scotia) data set, a five-year, population-based linked administrative data set in Nova Scotia, Canada (n=3,501) (Urquhart and Grunfeld 2010). The core database for ACCESS, from which all linkages took place, was the Nova Scotia Cancer Registry (NSCR). Personnel from the NSCR identified all individuals diagnosed with CRC between January 1, 2001 and December 31, 2005. Collaborative staging was applied to all patients within the NSCR (Collaborative Stage Data Collection System 2010). Excluded from the ACCESS data set were (a) individuals who had non-invasive/collaborative stage zero CRC and (b) cases that were diagnosed by death certificate or autopsy only.
Clinical, demographic and socio-economic information for these individuals was derived from 15 administrative databases, including the NSCR, anonymously linked at the individual level. Specifically, the NSCR and Oncology Patient Information System (OPIS) provided demographic, tumour and death data; hospital discharge abstracts provided information on all hospital admissions and discharges throughout the province; and the 2001 Census in Canada provided socio-economic data at the enumeration level, which were linked to the individuals in the ACCESS data set through the Postal Code Conversion File (Wilkins 2005). Data on chemotherapy referrals, visits and receipt were obtained from OPIS, the Medical Services Insurance physicians' billing database and a comprehensive chart review to obtain complete population-based chemotherapy data. Specifically, we reviewed charts of all individuals for whom chemotherapy was guideline-recommended, but there was no indication of receipt in the administrative data files; further details related to this review are reported elsewhere (Urquhart et al. 2011). Data on radiotherapy referrals, visits and receipt were obtained from OPIS.
The population for this study was a subset of 1,094 individuals from the ACCESS data set of 3,501 new CRC cases in Nova Scotia. We included all adults (≥ 20 years) who were diagnosed with stage II or III rectal or stage III colon cancer and who underwent surgical resection. We selected resected stage II/III rectal cancer and resected stage III colon cancer because of the existence of clinical practice guidelines regarding neo-adjuvant treatments for these populations.
Variables
Access to chemotherapy and radiotherapy
We created measures of receipt of chemotherapy and radiotherapy and wait time for radiotherapy. The receipt variable was binary: whether or not the individual received chemotherapy and/or radiotherapy. We used clinical practice guidelines established by Cancer Care Ontario (Figueredo et al. 1997, 2003) and accepted in Nova Scotia for the years 2001–2008. These guidelines recommend that patients with resected stage II or III rectal cancer receive neo-adjuvant or adjuvant radiotherapy, as well as adjuvant chemotherapy. Similarly, these guidelines recommended that patients with resected stage III colon cancer receive adjuvant chemotherapy. Therefore, if patients did not receive chemotherapy and/or radiotherapy, depending on their disease site, they were considered to have not met guidelines. Therapies were captured in the six months prior to surgery (neo-adjuvant radiotherapy) and 12 months post-surgery (adjuvant radiotherapy and adjuvant chemotherapy). We excluded radiotherapy provided with palliative intent (i.e., when "intent" was palliative or the number of fractions was ≤ 20), but were not able to ensure that the chemotherapy provided in the year following surgery was for adjuvant versus palliative reasons.
For those rectal cancer patients who received the clinically recommended radiotherapy, we created the wait time variable. The wait time variable was also binary: whether or not the individual who received radiotherapy met the 14-day benchmark set by the Canadian Association of Radiation Oncology from referral to radiation oncology to consultation (Wait Time Alliance 2005). Inequity in wait times for chemotherapy was not examined in this study owing to intrinsic challenges of assessing time intervals for chemotherapy.
Factors that influence access to chemotherapy and radiotherapy
We selected both need and non-need factors as explanatory variables for our analyses of inequities in receipt of chemotherapy and radiotherapy and wait time for radiotherapy. Need factors are those whose influence on access to care is typically judged to be reasonable (e.g., health status). Non-need factors are those that should not influence access to care (e.g., patient income).
We used a previous cancer diagnosis (yes or no) and co-morbidities as need factors, which we judged should appropriately influence receipt of care and wait time variables. A previous cancer diagnosis may prevent a patient from receiving subsequent radiotherapy because of prior exposure. In addition, multiple co-morbidities may hinder an individual's ability to receive or recover from chemotherapy or radiotherapy. Using the Elixhauser list of co-morbidities (Elixhauser et al. 1998), we tabulated a co-morbidity score by computing the sum of all recorded co-morbid conditions, excluding cancer, in the two years prior to the date of diagnosis and the 30 days following diagnosis (score range = 0–28). Co-morbid conditions were retrieved as diagnostic codes from hospital discharge abstracts; these codes include all diagnoses recorded as the cause(s) of the hospital admission as well as all diagnoses that affected the patient's resource consumption or length of stay. We identified previous cancer-related conditions from records captured in NSCR/OPIS.
As non-need factors, we included the patients' income, sex, age at diagnosis, year of diagnosis, distance to the nearest cancer centre, health district, tumour site and tumour stage. Ethically, these factors should not affect access, but the literature has demonstrated that they are associated with access to cancer care (Baldwin et al. 2008; Cree et al. 2009; Paszat et al. 1998). Patient income, sex, year of diagnosis and geographic factors are commonly used non-need factors and clearly should not influence an individual's access to care (e.g., age at diagnosis is considered a non-need factor because differences in health status by age have been adjusted by controlling for co-morbidities). Tumour stage was considered a non-need factor because we included only those patients (stage II/III rectal; stage III colon) for whom clinical practice guidelines recommend therapy.
We measured distance as the driving distance from the patient's area of residence (based on postal code) to the nearest cancer centre (i.e., Halifax or Sydney) using Google Maps (Zdeb 2010). We used the average median household income from the neighbourhood of each patient as a proxy for the patient's income. Specifically, the average median household income was measured at the enumeration level of the 2001 Census in Canada and linked to the individual using patient residential postal codes on the date of diagnosis.
Measure of inequity
Our measure of inequity is the Horizontal Inequity Index. The HI is based on the assumption that access is equitable when people with equal need have equal access after adjustment for need (O'Donnell et al. 2007). It uses the concept of the concentration curve that describes whether access is concentrated among the advantaged sub-population (e.g., the rich) or among the disadvantaged sub-population (e.g., the poor). Such pro-advantaged or pro-disadvantaged relationship can be summarized by an index that takes values between –1 and +1. Using income as an example, a value of 0 indicates that each individual has equal access regardless of income; a value between 0 and +1 suggests those with greater income have better access (pro-advantaged); and a value between –1 and 0 indicates that those with smaller income have better access (pro-disadvantaged). When access is examined without need adjustment, the index is called the Concentration Index (CI), which reports inequality.
We used income, sex, age and distance as attributes with which to examine inequities in receipt of chemotherapy and radiotherapy and wait time for radiotherapy. Calculation of the HI requires subcategories to be ranked from the disadvantaged to the advantaged. Ranking of income subcategories was straightforward, from the smallest income of the disadvantaged to the greatest income of the advantaged. For sex, age and distance, based on the literature, we considered younger age, being male and travelling a shorter distance to a cancer centre as advantaged characteristics. Accordingly, we ranked these attributes from disadvantaged to advantaged as follows: for age, 80+, 70–79, 60–69 and < 60 years; for sex, female or male; and for distance, 125+km, 75–124.99km, 15–74.99km and 0–14.99km to the nearest cancer centre.
Analysis
Our analytical approach extended a need-standardization method, a widely used method for analyses of inequity in access to healthcare in population-based studies (O'Donnell et al. 2007). Such analysis, regardless of the clinical or population setting, asks whether healthcare use systematically deviates from standard healthcare use according to need for care (Asada and Kephart 2011). In an ideal world, well-specified, evidence-based clinical guidelines identify standard healthcare that should be offered to patients with a specific need profile. In the real world, such clinical guidelines exist only in limited settings. Population-based inequity studies, thus, typically employ a need-standardization method, which statistically estimates the average healthcare use based on need in the population and considers systematic deviation as inequitable. Our analytical approach included a need-standardization method by accounting for evidence-based clinical guidelines in receipt of chemotherapy and radiotherapy and wait time for radiotherapy, as well as patient need. Despite need-adjustment, patient choices remain unadjusted and may influence inequity results.
We examined income-, sex-, age- and distance-related inequity separately for receipt of guideline-recommended care and wait time for such care. Each analysis took the following four steps:
- Using logistic regression, we modelled observed use according to guidelines by all need and non-need factors. Modelling in this first step provided initial assessments of impact of need and non-need factors on observed use according to guidelines.
- We predicted need-expected use according to guidelines for each individual in the data set by purging the influence of non-need factors (i.e., holding them constant at the most frequent subcategory of each non-need factor). This second step accounted for acceptable reasons for not meeting the clinical guidelines.
- We estimated the guideline need-standardized use for each individual by subtracting the need-expected use from the observed use according to the guidelines and adding the average use of the population.
- In the final step, we calculated an HI separately for income, age, sex and distance in relation to the distribution of guideline need-standardized use.
We conducted all analyses using Stata 11. Our data included all CRC patients in Nova Scotia in the specified study period and, thus, did not require sample weights. Data access was approved by the Capital District Health Authority and Dalhousie University research ethics boards.
Results
Just over half of the study cohort (53.2%) received the guideline-recommended chemotherapy, radiotherapy or both (Table 1). Notably, those diagnosed with colon cancer were more likely to receive guideline-recommended treatment (i.e., chemotherapy) compared to individuals diagnosed with rectal cancer (i.e., chemotherapy and radiotherapy). Among rectal cancer patients who received guideline-recommended care, 53.5% met the 14-day benchmark from radiation oncology referral to consultation.
| TABLE 1. Study population characteristics | ||
| Variable | N (n=1,094) | % |
| Receipt of clinically recommended treatment* | ||
| All (rectal and colon) cancer patients (n=1,094) | 582 | 53.2 |
| Rectal cancer patients (n=503) | 250 | 49.7 |
| Colon cancer patients (n=591) | 332 | 56.2 |
| Wait time within clinical benchmark** (n=250) | ||
| No | 116 | 46.5 |
| Yes | 134 | 53.5 |
| Need factors | ||
| Previous cancer diagnosis | ||
| No | 976 | 89.2 |
| Yes | 118 | 10.8 |
| Co-morbidities (number) | ||
| 0 | 670 | 61.2 |
| 1 | 207 | 18.9 |
| 2+ | 217 | 19.9 |
| Non-need factors | ||
| Sex | ||
| Men | 605 | 55.3 |
| Women | 489 | 44.7 |
| Age at diagnosis (years) | ||
| < 60 | 277 | 25.3 |
| 60–69 | 265 | 24.2 |
| 70–79 | 316 | 28.9 |
| 80+ | 236 | 21.6 |
| Mean (standard deviation) | 68.4 | (12.4) |
| Disease site | ||
| Rectum | 503 | 54.0 |
| Colon | 591 | 46.0 |
| Stage at diagnosis for rectal cancer | ||
| II | 222 | 44.1 |
| III | 281 | 55.9 |
| Year of diagnosis | ||
| 2001 | 219 | 20.0 |
| 2002 | 211 | 19.3 |
| 2003 | 202 | 18.5 |
| 2004 | 219 | 20.0 |
| 2005 | 243 | 22.2 |
| Region of Nova Scotia** | ||
| Capital District Health Authority | 407 | 37.2 |
| Cape Breton District Health Authority | 194 | 17.7 |
| Annapolis Valley, South Shore and South West Health Authorities | 287 | 26.2 |
| Colchester East Hants, Pictou County and Guysborough Antigonish Straight Health Authorities | 206 | 18.9 |
| Distance to the nearest cancer centre (km) | ||
| 0–14.99 | 277 | 25.2 |
| 15–74.99 | 285 | 26.1 |
| 75–124.99 | 249 | 22.8 |
| 125+ | 283 | 25.9 |
| Income (Canadian dollars) | ||
| < $30,000 | 244 | 22.3 |
| $30,000–$44,999 | 502 | 45.9 |
| $45,000+ | 325 | 29.7 |
| Missing | 23 | 2.1 |
| * Clinically recommended treatment for rectal cancer is adjuvant or neo-adjuvant radiotherapy and chemotherapy, and clinically recommended treatment for colon cancer is chemotherapy. | ||
| ** Wait time is from radiation oncology referral to consultation within the 14-day benchmark, and the wait time includes only those who received clinically recommended treatment, chemotherapy in addition to neo-adjuvant or adjuvant radiotherapy. | ||
The modelling of observed use according to guidelines indicated that the likelihood of receiving guideline-recommended care and of meeting the radiation oncology wait time benchmark were not solely determined by need (Table 2). Multiple logistic regression analysis demonstrates a statistically significant greater likelihood of receiving guideline-recommended care when the subject was male, younger than 60 years, received care in Cape Breton District Health Authority, lived less than 15 km from the nearest cancer centre, had no co-morbidities and was diagnosed with colon cancer. Notably, among all individuals in this study, those 70–79 years old had odds of 0.20 (95% CI: 0.13–0.30), and individuals 80+ years old had odds of 0.02 (95% CI: 0.013–0.039), of receiving guideline-recommended care compared to those aged 60 years or younger. The likelihood of meeting the wait time benchmark was statistically significant when associated only with health district: patients from Cape Breton District Health Authority had 4.07 times greater odds of meeting the benchmark compared to those from Capital District Health Authority (95% CI: 1.80–9.20).
| TABLE 2. Effects of need and non-need factors on receipt of clinically recommended care and wait time within clinical benchmark | ||||
| Variable | Receipt of Clinically Recommended Care* | Wait Time within Clinical Benchmark** | ||
| OR§ | (95% CI§§) | OR§ | (95% CI§§) | |
| Need factors | ||||
| Previous cancer diagnosis | ||||
| No | 1.00 | 1.00 | ||
| Yes | 0.84 | (0.53, 1.35) | 0.72 | (0.24, 2.17) |
| Co-morbidities (number) | ||||
| 0 | 1.00 | 1.00 | ||
| 1 | 0.80 | (0.53, 1.20) | 1.27 | (0.62, 2.63) |
| 2+ | 0.33 | (0.21, 0.50) | 1.42 | (0.58, 3.46) |
| Non-need factors | ||||
| Sex | ||||
| Men | 1.00 | 1.00 | ||
| Women | 0.61 | (0.45, 0.83) | 0.91 | (0.55, 1.50) |
| Age at diagnosis (years) | ||||
| <60 | 1.00 | 1.00 | ||
| 60–69 | 0.64 | (0.42, 0.97) | 0.95 | (0.36, 2.51) |
| 70–79 | 0.20 | (0.13, 0.30) | 0.72 | (0.27, 1.87) |
| 80+ | 0.02 | (0.01, 0.04) | 0.92 | (0.36, 2.36) |
| Disease site | ||||
| Colon | 1.00 | |||
| Rectum | 0.39 | (0.29, 0.54) | ||
| Year of diagnosis | ||||
| 2001 | 1.00 | 1.00 | ||
| 2002 | 0.71 | 0.44–1.15 | 0.85 | 0.38–1.90 |
| 2003 | 1.07 | 0.66–1.72 | 1.01 | 0.45–2.26 |
| 2004 | 1.39 | 0.86–2.25 | 0.95 | 0.44–2.06 |
| 2005 | 0.97 | 0.61–1.54 | 1.27 | 0.58–2.78 |
| Region of Nova Scotia | ||||
| Capital District Health Authority | 1.00 | 1.00 | ||
| Cape Breton District Health Authority | 5.12 | (2.99, 8.76) | 4.07 | (1.80, 9.20) |
| Annapolis Valley, South Shore and South West Health Authorities | 1.58 | (0.88, 2.86) | 0.63 | (0.23, 1.68) |
| Colchester East Hants, Pictou County and Guysborough Antigonish Straight Health Authorities | 1.62 | (0.89, 2.93) | 0.76 | (0.28, 2.02) |
| Distance to the nearest cancer centre (km) | ||||
| 0–14.99 | 1.00 | 1.00 | ||
| 15–74.99 | 0.74 | (0.47, 1.16) | 1.14 | (0.57, 2.27) |
| 75–124.99 | 0.63 | (0.34, 1.18) | 0.97 | (0.36, 2.59) |
| 125+ | 0.46 | (0.24, 0.89) | 0.89 | (0.30, 1.90) |
| Income (Canadian dollars) | ||||
| < $30,000 | 1.00 | 1.00 | ||
| $30,000–$44,999 | 1.19 | (0.80, 1.78) | 0.99 | (0.52, 1.89) |
| $45,000+ | 1.45 | (0.91, 2.31) | 1.28 | (0.62, 2.64) |
| Missing | 2.71 | (0.84, 8.74) | 1.08 | (0.26, 4.44) |
| Note 1: All odds ratios are adjusted for other variables listed in the table. | ||||
| Note 2: Bold indicates statistical significance at 5%. | ||||
| * Clinically recommended treatment for rectal cancer is adjuvant or neo-adjuvant radiotherapy and chemotherapy, and clinically recommended treatment for colon cancer is chemotherapy. | ||||
| ** Wait time is from radiation oncology referral to consultation within 14 days, and the number includes only those who received clinically recommended treatment, chemotherapy in addition to neo-adjuvant or adjuvant radiotherapy. | ||||
| § Odds ratio | ||||
| §§ Confidence interval | ||||
Consistent with the results from the logistic regression analyses reported in Table 2, the HIs suggested statistically significant age-, sex- and distance-related inequities in receipt of guideline-recommended care but no statistically significant inequities in wait time within the clinical benchmark (Table 3). The magnitude of inequity was greatest for age-related inequity in receipt of guideline-recommended care (HI: 0.22, 95% CI: 0.19–0.25). We observed no income-related inequity in receipt of such care or wait time to receive care.
| TABLE 3. Inequities in access to guideline-recommended care | ||||
| Dimension of inequity | Receipt of clinically recommended treatment* | Wait time within clinical benchmark** | ||
| HI§ | (95% CI§§) | HI§ | (95% CI§§) | |
| Income | 0.01 | (–0.02, 0.04) | 0.00 | (–0.06, 0.06) |
| Age | 0.22 | (0.19, 0.25) | –0.01 | (–0.07, 0.05) |
| Sex | 0.05 | (0.02, 0.08) | 0.02 | (–0.04, 0.08) |
| Distance | 0.05 | (0.02, 0.09) | 0.05 | (–0.01, 0.11) |
| Note 1: Bold indicates statistical significance at 5%. | ||||
| * Clinically recommended treatment for rectal cancer is adjuvant or neo-adjuvant radiotherapy and chemotherapy, and clinically recommended treatment for colon cancer is chemotherapy. | ||||
| ** Wait time is from radiation oncology referral to consultation within 14 days, and the number includes only those who received clinically recommended treatment, chemotherapy in addition to neo-adjuvant or adjuvant radiotherapy. | ||||
| § Horizontal Inequity Index | ||||
| §§ Confidence interval | ||||
Discussion
Using population-based linked administrative databases, this study examined income-, age-, sex- and distance-related inequity in access to chemotherapy and radiotherapy among CRC patients in Nova Scotia. We found indications of age-, sex- and distance-related inequities in access to guideline-recommended care. Our study went beyond regression analyses by describing the degree of inequity by the HI, an increasingly popular inequity index in population-based analyses. One can examine inequities by looking at odds ratios for each subcategory (e.g., for age, 60–69, 70–79 and 80+ compared to < 60), but the HI summarizes these odds ratios for each dimension (e.g., the HI expressing the degree of age-related inequity). Using this approach facilitated comparison of degrees of inequity across dimensions, types of services and study populations, as opposed to comparing all odds ratios. Moreover, the use of the HI also enhances comparability of results from studies that use different subcategories for the same dimension. For example, age can be categorized as < 60, 60–69, 70–79 and 80+, or as < 65 and 65+. One can still examine effect sizes of each of these subcategories, but with the use of the HI, comparison is clearer in terms of the degree of age-related inequity.
Lower rates of access to chemotherapy and radiotherapy with increasing age have been well documented in the literature. Even after controlling for health status, older individuals were significantly less likely to receive adjuvant treatment (Carsin et al. 2008; Cree et al. 2009; Golfinopoulos 2006; Newcomb and Carbone 1993; Potosky et al. 2002). Previous studies have demonstrated that older patients were less likely to be given chemotherapy and radiotherapy as treatment options by physicians and less likely to be referred to medical and radiation oncologists (Newcomb and Carbone 1993; Weeks 1994), despite evidence of the effectiveness of these treatments in elderly patients (Pignon et al. 1997; Zachariah et al. 1997). Consistent with this literature, our analysis identified age-related inequity in receipt of clinically recommended treatment. However, there may be differences in patient wishes for care related to age, which no existing population-based databases in Nova Scotia capture. Further investigation is necessary to identify factors that contribute to the age-related inequity, especially distinguishing health system and patient factors, such as lower physician referral rates, lower understanding of or comfort with the health system among the elderly, or greater logistic challenges (e.g., transportation to a cancer centre) among older patients.
The indication of pro-male inequity in receipt of guideline-recommended care was unexpected and not in agreement with previous studies (Ayanian 2003; Cree et al. 2009; Johnston et al. 2004). Reasons for this finding are unclear and require further investigation. It may be possible that there are fewer or less severe barriers for men to receive radiotherapy and chemotherapy. For example, women may have greater difficulty than men in repeatedly travelling to a cancer centre owing to family or work commitments.
We found no statistically significant income-related inequity in receipt of care or in wait times. This finding was not unexpected, as a 2011 literature review reported inconsistent income-related inequality in access to CRC care in Canada (Maddison et al. 2011). Our regression analyses indicated a trend of greater access for those with higher income, yet this trend did not result in a statistically significant income-related inequity in the calculation of an HI.
Our analysis showed no inequity in the likelihood of meeting the 14-day benchmark from radiation oncology referral to consultation. However, we must interpret this finding with caution. Our wait time analyses had a smaller sample size (n=582) than those for the receipt analyses (n=1,094). In addition, we selected the time interval between radiation oncology referral to consultation to maximize our ability to differentiate between inequality and inequity. Such a focused time interval should potentially reduce the number and impact of potentially confounding factors, but it also diminishes the likelihood of identifying variations. In rectal cancer, intervals that begin at radiation oncology referral (or consultation) and end at start of radiotherapy treatment must account for receipt of concurrent or prior therapies (e.g., chemotherapy). Moreover, these longer intervals might be more influenced by patient choice (particularly in a province where radiotherapy services are centralized and many patients must coordinate regular transportation and/or lodging for a prolonged period) and other need factors that cannot be captured. Nonetheless, the interval we selected may not be a good proxy for actual receipt of treatment. The interval "ready-to-treat to start of radiotherapy treatment" (now measured by most Canadian jurisdictions) may prove a better interval to examine inequity because the ready-to-treat date is meant to represent the date at which the patient is medically, physically, personally and psychologically prepared to begin radiotherapy. We did not examine the ready-to-treat to treatment interval in this study owing to considerable missing data in one of the fields required for this measurement.
In addition to identification of inequities, a further concern may be that only 53.2% of individuals received the guideline-recommended chemotherapy and/or radiotherapy. Moreover, among those who received care according to guidelines, only 53.5% then met wait time goals for care. Although these rates may seem lower than might be expected or hoped for, they must be interpreted carefully, as they are unadjusted. A proportion of patients that did not meet guidelines would have failed to do so because of valid contraindications or personal choice. Notably, a 2009 study reported that 53% of individuals diagnosed with stage III colon cancer or stage II/III rectal cancer in Alberta, Saskatchewan and Manitoba received guideline-recommended care (Cree et al. 2009).
Need-standardization is imperative for measuring inequity. Even when clinical practice guidelines and wait time benchmarks exist, there are occasions when it is reasonable for providers and patients not to follow them. The common challenge of determining the variables that should be included as need factors in the analysis in population-based studies (Hutchison et al. 2000) also applies to clinical studies like ours. The rich, linked administrative database used in this study allowed us to include objectively measured contraindications for care and health status as need factors. However, contraindications, measured by the number of co-morbidities, were likely underreported. We measured co-morbidities in the two years prior to the date of CRC diagnosis as recorded in the hospital discharge abstracts, and hence, our co-morbidity calculation may have missed less severe conditions or those managed by a family physician. Also, a measure of contraindication for clinically recommended treatment for CRC should ideally be more specific than a co-morbidity count or a previous cancer diagnosis, which were the two measures we used in this study. For example, a previous cancer diagnosis indicates a possible contraindication to radiotherapy because of prior exposure to radiotherapy. However, such diagnosis does not imply that the patient in fact received radiotherapy, or that the radiotherapy was directed to the pelvic region (the rationale for the contraindication being that the pelvic region is the target of radiotherapy for a rectal cancer).
In addition, our need-standardization could not account for patient choice regarding care. Patient choice likely plays an important role in examining whether age-related and distance-related variations in care are inequitable. Furthermore, our methods assume that observed access, measured by whether clinical guidelines were followed in consideration of patient need, is appropriate. This assumption may not hold for all cases, and there might be situations where we should consider a failure to treat or a failure to follow appropriate clinical guidelines. Taken together, the HI results should be interpreted with the caveat that, although we made attempts to level patient need for care, the remaining variation may include some degree of unmeasured patient need and/or may not be entirely ethically problematic.
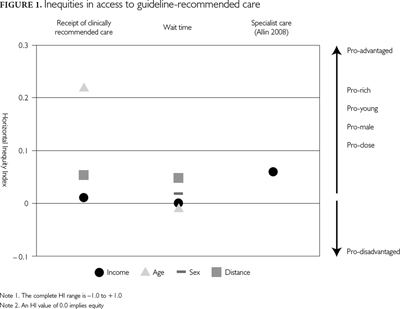
The use of the HI facilitated comparison between inequities in receipt of care and wait time for care and across different dimensions of inequity, but the novelty of its use brought challenges. The HI values are not intuitively interpretable, and it is not clear which values we should consider clinically significant. To our knowledge, our study is the first to use this index in cancer health services research, and we cannot compare the HI values we calculated to other cancer equity studies. Comparison to studies examining inequity in use of specialist health services in Canada, however, may be useful (Figure 1). Both Allin (2008) and van Doorslaer and colleagues (2006) examined income-related inequity in use of specialist visits using the HI and reported pro-rich inequity of the HI values of 0.055 and 0.06, respectively. These HI values for specialist services are greater than the HI values that we reported for receipt of chemotherapy and radiotherapy. As the usefulness of the HI improved with its increased use in population-based equity studies, the promise of the application of the HI in cancer health services research might follow a similar path in future.
Conclusion
Inequities exist in access to chemotherapy and radiotherapy for CRC patients in Nova Scotia. By incorporating clinical practice guidelines and benchmarks, adjusting for patients' need for care and applying the HI, we moved beyond measuring inequalities in care by relying only on regression analyses. For academic researchers, this study demonstrates the importance of carefully examining inequity in access to care and wait times for care across the cancer continuum through using clinical guidelines and need-standardization. For policy makers, this study highlights one method to report and compare inequities with conceptual clarity and methodological rigour. It also points to target areas that require further investigation, such as possible age-related inequity. Such knowledge may eventually call for designing and implementing clinical or policy interventions, or both, to reduce inequities.
Iniquité d'accès au traitement du cancer colorectal recommandé par les directives en Nouvelle-Écosse, Canada
Résumé
Le cancer demeure l'un des plus grands fardeaux en termes de maladies au Canada. L'évaluation des iniquités d'accès au traitement du cancer peut servir de baromètre pour connaître l'état des systèmes de santé au Canada. Cette étude cerne trois obstacles liés à la littérature actuelle, et ce, en faisant clairement la différence entre inégalité et iniquité, en évaluant l'iniquité dans les soins et les temps d'attente et en tirant profit des indices d'iniquité pour accroître la comparabilité des iniquités dans les études et dans la population. Nous avons mesuré les iniquités liées au revenu, à l'âge, au sexe et à la distance chez les patients traités pour un cancer colorectal (CCR) en Nouvelle-Écosse, en tenant compte des directives cliniques et des besoins des patients. Les résultats révèlent l'existence d'iniquités statistiquement significatives en termes d'accès à la chimiothérapie et à la radiothérapie pour le traitement du CCR, et ce, en fonction de l'âge, du sexe et de la distance, mais non pas en fonction du revenu. Cette étude démontre l'importance d'examiner soigneusement les iniquités d'accès au traitement du cancer et fait valoir une méthode pour rendre compte des iniquités et les comparer entre elles, avec une précision conceptuelle.
About the Author(s)
André R. Maddison, MSc, Graduate Student, Faculty of Medicine, Dalhousie University, Halifax, NS
Yukiko Asada, PhD, Associate Professor, Community Health & Epidemiology, Dalhousie University, Halifax, NS
Robin Urquhart, MSc, Cancer Outcomes Research Program, Cancer Care Nova Scotia, Halifax, NS
Grace Johnston, PhD, Professor, School of Health Administration, Dalhousie University, Halifax, NS
Frederick Burge, MSc, MD, Professor, Department of Family Medicine, Dalhousie University, Halifax, NS
Geoff Porter, MSc, MD, Professor, Division of General Surgery, Dalhousie University, Halifax, NS
Correspondence can be directed to: André R. Maddison, andre.maddison@dal.ca.
Acknowledgment
The authors would like to thank Martha Cox and Vickey Bu for their assistance with providing the data. Funding for this study was provided by the Canadian Institutes of Health Research, Cancer Care Nova Scotia, Nova Scotia Department of Health and Wellness, Capital District Health Authority, Dalhousie University Faculty of Medicine and the Dalhousie Medical Research Foundation. Yukiko Asada is the recipient of a Canadian Institutes of Health Research New Investigator Award.
References
Allin, S. 2008. "Does Equity in Healthcare Use Vary across Canadian Provinces?" Healthcare Policy 3(4): 83–99.
Asada, Y. and G. Kephart. 2011. "Understanding Different Methodological Approaches to Measuring Inequity in Health Care." International Journal of Health Services 41(2): 195–207.
Ayanian, J. 2003. "Use of Adjuvant Chemotherapy and Radiation Therapy for Colorectal Cancer in a Population-Based Cohort." Journal of Clinical Oncology 21(7): 1293–300.
Baldwin, L.M., Y. Cai, E.H. Larson, S.A. Dobie, G.E. Wright, D.C. Goodman et al. 2008. "Access to Cancer Services for Rural Colorectal Cancer Patients." Journal of Rural Health 24(4): 390–99.
Berrino, F., R. De Angelis, M. Sant, S. Rosso, M. Bielska-Lasota, J.W. Coebergh et al. 2007. "Survival for Eight Major Cancers and All Cancers Combined for European Adults Diagnosed in 1995–99: Results of the EUROCARE-4 Study." Lancet 8: 773–83.
Canadian Cancer Society. 2011. "Canadian Cancer Society's Steering Committee: Canadian Cancer Statistics 2011." Toronto: Author.
Carsin, A.E., L. Sharp, D.P. Cronin-Fenton, A.O. Céilleachair and H. Comber. 2008. "Inequity in Colorectal Cancer Treatment and Outcomes: A Population-Based Study." British Journal of Cancer 99(2): 266–74.
Cheung, W.Y., B.A. Neville and C.C. Earle. 2009. "Etiology of Delays in the Initiation of Adjuvant Chemotherapy and Their Impact on Outcomes for Stage II and III Rectal Cancer." Diseases of the Colon and Rectum 52(6): 1054–64.
Collaborative Stage Data Collection System. 2010. Collaborative Stage Data Collection System Coding Instructions. Retrieved September 15, 2012. <http://www.cancerstaging.org/cstage/manuals/csmanual-p1s1.pdf>.
Cree, M., J. Tonita, D. Turner, Z. Nugent, R. Alvi, R. Barss et al. 2009. "Comparison of Treatment Received versus Long-Standing Guidelines for Stage III Colon and Stage II/III Rectal Cancer Patients Diagnosed in Alberta, Saskatchewan and Manitoba in 2004." Clinical Colorectal Cancer 8(3): 141–45.
Elixhauser, A., C. Steiner, R.D. Harris and R.M. Coffey. 1998. "Comorbidity Measures for User with Administrative data." Medical Care 36(1): 8–27.
Figueredo, A., S. Fine, J. Maroun, C. Walker-Dilks and S. Wong. 1997. "Adjuvant Therapy for Stage III Colon Cancer After Complete Resection. Provincial Gastrointestinal Disease Site Group." Cancer Prevention and Control 1(4): 304–19.
Figueredo, A., L. Zuraw, R. Wong, O. Agboola, R.B. Rumble, V. Tandan and Cancer Care Ontario's Program in Evidence-Based Care's Gastrointestinal Cancer Disease Site Group. 2003. "The Use of Preoperative Radiotherapy in the Management of Patients with Clinically Resectable Rectal Cancer: A Practice Guideline." BMC Medicine 1(1).
Gatta, G., R. Capocaccia, M. Sant, C.M. Bell, J.W. Coebergh, R.A. Damhuis et al. 2000. "Understanding Variations in Survival for Colorectal Cancer in Europe: A EUROCARE High Resolution Study." Gut 47: 533–38.
Golfinopoulos, V., G. Pentheroudakis and N. Pavlidis. 2006. "Treatment of Colorectal Cancer in the Elderly: A Review of the Literature." Cancer Treatment Reviews 32(1): 1–8.
Hershman, D., M.J. Hall, X. Wang, J.S. Jacobson, R. McBride, V.R. Grann et al. 2006. "Timing of Adjuvant Chemotherapy Initiation After Surgery for Stage III Colon Cancer." Cancer 107(11): 2581–88.
Hutchison, B., J. Hurley, S. Birch, J. Lomas, S.D. Walter, J. Eyles et al. 2000. "Needs-Based Primary Medical Care Capitation: Development and Evaluation of Alternative Approaches." Health Care Management Sciences 3(2): 89–99.
Johnston, G.M., V.L. MacGarvie, D. Elliott, R.A. Dewar, M.M. MacIntyre and M.C. Nolan. 2004. "Radiotherapy Wait Time for Patients with a Diagnosis of Invasive Cancer, 1992–2000." Clinical and Investigative Medicine 3: 142–56.
Maddison, A.R., Y. Asada and R. Urquhart. 2011. "Inequity in Access to Cancer Care: A Review of the Canadian Literature." Cancer Causes Control 22: 359–66.
Newcomb, P.A. and P.P. Carbone. 1993. "Cancer Treatment and Age: Patient Perspectives." Journal of the National Cancer Institute 85(19): 1580–84.
Paszat, C.I., W.J. Mackillop, P.A. Groome, J. Zhang-Salomons, K. Schulze and E. Holowaty. 1998. "Radiotherapy for Breast Cancer in Ontario: Rate Variation Associated with Region, Age and Income." Clinical and Investigative Medicine 21(3): 125–34.
Pignon, T., J.C. Horiot, M. Bolla, H. van Poppel, H. Bartelink, F. Roelofsen et al. 1997. "Age Is Not a Limiting Factor for Radical Radiotherapy in Pelvic Malignancies." Radiotherapy and Oncology 42: 107–20.
Potosky, A.L., L.C. Harlan, R.S. Kaplan, K.A. Johnson and C.F. Lynch. 2002. "Age, Sex and Racial Differences in the Use of Standard Adjuvant Therapy for Colorectal Cancer." Journal of Clinical Oncology 20(5): 1192–202.
O'Donnell, O., E. van Doorslaer, A. Wagstaff and M. Lindelow. 2007. "Analyzing Health Equity Using Household Survey Data: A Guide to Techniques and Their Implementation." Washington, DC: The World Bank.
Singh, H., C. De Coster, E. Shu, K. Fradette, S. Latosinsky, M. Pitz et al. 2010. "Wait Time from Presentation to Treatment for Colorectal Cancer: A Population-Based Study." Canadian Journal of Gastroenterology 24(1): 33–39.
Urquhart, R. and E. Grunfeld. 2010. "Building Tools to Measure and Improve Access to and Quality of Colorectal Cancer Care in Nova Scotia." Canadian Journal of Gastroenterology 24 (Supplement SA).
Urquhart, R., D. Rayson, G. Porter and E. Grunfeld. 2011. "Quantifying Limitations in Chemotherapy Data in Administrative Health Databases: Implications for Measuring the Quality of Colorectal Cancer Care." Healthcare Policy 7(1): 32–40.
van Doorslaer, E., C. Masseria, X. Koolman and OECD Health Equity Research Group. 2006. "Inequalities in Access to Medical Care by Income in Developed Countries." Canadian Medical Association Journal 174(2): 177–83.
Wagstaff, A., P. Paci and E. van Doorslaer. 1991. "On the Measurement of Inequalities in Health." Social Science and Medicine 33(5): 545–57.
Wait Time Alliance. 2005. "No More Time to Wait: Towards Benchmarks and Best Practices in Wait-Time Management." Retrieved September 15, 2012. <http://www.waittimealliance.ca/images/report_times_up.pdf>.
Weeks, J. 1994. "Preferences of Older Cancer Patients: Can You Judge a Book by Its Cover?" Journal of the National Cancer Institute 86(23): 1743–44.
Wilkins, R. 2005. "Automated Geographic Coding Based on the Statistics Canada Postal Code Conversion Files." Catalogue no. 82F0086-XDB. Ottawa: Statistics Canada.
Winget, M., S. Hossain, Y. Yasui and A. Scarfe. 2010. "Characteristics of Patients with Stage III Adenocarcinoma Who Fail to Receive Guideline-Recommended Treatment." Cancer 116: 4849–56.
Zachariah, B., L. Balducci, G.V. Venkattaramanabalaji, L. Casey, H.M. Greenberg and J.A. Del Regato. 1997. "Radiotherapy for Cancer Patients Aged 80 and Older: A Study of Effectiveness and Side Effects." International Journal of Radiation Oncology 39(5): 1125–29.
Zdeb, M. 2010. "Driving Distances and Times Using SAS and Google Maps." SAS Global Forum 2010 Proceedings. Retrieved September 15, 2012. <http://support.sas.com/resources/papers/proceedings10/050-2010.pdf>.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed