World Health & Population
Resource Allocation in Pakistan's Health Sector: A Critical Appraisal and a Path toward the Millennium Development Goals
Babar Tasneem Shaikh, Irum Ejaz, Arslan Mazhar and Assad Hafeez
Abstract
Pakistan is trying hard to sustain its progress toward the Millennium Development Goals. However, because of a lack of political commitment to innovative solutions to improve its financing mechanism, the health system is unable to provide even essential and basic services to the people. The country, with more than 70% of the population living on less than two US dollars a day, largely depends on direct taxes for its revenue. Because of inadequate financing, the quality of government services is inexcusably poor; therefore, a majority of people seek healthcare in the private sector. This has led to a horde of issues pertaining to equity, accessibility and fairness. High out-of-pocket expenses on health jeopardize a family's livelihood, pushing it into a vicious circle of poverty. In the wake of recent devolution, this paper presents options for future health financing that enables the provinces to exert their autonomy to safeguard the health of the most vulnerable in the country. Our recommendations follow the vision of the World Health Organization and the Commission on Macroeconomics and Health, to achieve universal health coverage and social protection for the poor.
Background
Healthcare embraces all the goods and services designed to promote health through promotive, curative and palliative care, whether directed to individuals or to populations. Providing a mix of services to a huge population is a challenge for most middle- and low-income countries with low budget allocations for health. Social and economic deprivation, compounded by issues such as gender, education, women's status, nutrition and sanitation, put immense pressure on the poor to seek medical care. Under such circumstances, the key milestones of a robust health system should encompass improving the health status of the population as well as cover the financial cost of treating illness. A well-functioning health system aims to lessen the financial burden on healthcare users (World Health Organization 2000). The widening coverage gap between rich and poor has decelerated the progress of health indicators under the Millennium Development Goals (MDGs). Communities must not experience financial hardship in accessing health services. To achieve this goal, the World Health Organization (WHO) also urged member states to modify healthcare financing systems within the sociocultural, macroeconomic and political context of the country and to develop sustainable financing mechanisms to manage their health systems (World health Organization 2000).
The total healthcare expenditure in a country is usually sourced through a mix of public and private spending, as shown in Figure 1 (Poullier et al. 2002). More reliance on private health expenditures without a mechanism to enforce regulations is likely to promote inequity, inaccessibility and financial hardship in healthcare seeking. Every year, 11% of the population in African and South Asian countries suffers severe financial hardship, and 5% falls below the poverty line. Inappropriate and inadequate financial mechanisms for public health expenditures and low income add an enormous burden on low-income quintiles. Coverage for social security protection in middle-income countries varies from 20% to 60%, compared with 5% to 10% in African and South Asian countries (World health Organization 2005). Since most low-income countries are not on track to achieve MDG targets, the developing an impetus to identify health financing mechanisms that address the coverage gaps for universally accessible health services is critical.
Figure 1. Sources of public and private expenditure in a health sector

With this background and state of affairs, we performed a critical appraisal of financing in Pakistan's health sector. Furthermore, in this paper we attempt to shed light on feasible options of improving health sector financing and allocations in the post-devolution period, wherein provinces are autonomous in making their own strategic decisions.
Health Financing in Pakistan
Pakistanis a low-income country in South Asia with a slow progression on the Human Development Index, where it currently stands 125th among 169 countries (United Nations Development Program 2010). Population growth, with an epidemiological transition i.e. changing disease patterns during the last decade, did not allow policy makers to develop mechanisms for financing health, therefore rendering a larger segment of population bereft of essential healthcare packages. About 0.6% of GDP and 5.1% to 11.6% of development expenditure on health is financed by the Government of Pakistan (Ahmed and Shaikh 2008; Nishtar 2006), contrary to the WHO recommendation to allocate at least 5% of GDP spending on health (World health Organization 2000). Notably, member countries of the Organisation of Economic Cooperation & Development (OECD) spend more than 8% of their GDP on health (OECD 2011). The health sector in Pakistan has received increments in budgetary allocations over the last few years, but they were not adjusted for inflation, population growth and burden of disease, leading to unresolved issues for social protection and health for all. Moreover, three-fifths of budgetary allocations are consumed by non-development purposes such as salaries, thus leaving a meagre share to deliver efficient, equitable and quality service. The public sector in Pakistan has shown weak capacity in the context of delivery and management of health services, resulting in a number of quality, competence and coverage issues (Nishtar 2010). The need to develop appropriate systems for allocating resources from the central to lower administrative levels has always been critically felt at the policy level.
Resource generation can be from taxes, employee contributions, the community, private insurance and out-of-pocket expenditures. In Pakistan, the most common modes of health financing are through general taxation and out-of-pocket payments. The Government of Pakistan is responsible for health spending in the public sector, where the capital investment through general taxation is channelled in annual development plans, inclusive of external funding from bilateral and multilateral donors (Ghaffar et al. 2000). Most revenue is collected by the central finance ministry and then redistributed vertically between the federal and provincial governments and horizontally among the provinces. A positive note is that about 80% of the financial resources in the public sector are provided by the Government of Pakistan. Pakistan's per capita spending on health is around 22 US dollars, of which the government's share is 6.4 dollars and 1.3 dollars are contributed by development partners. Obviously, the dependency factor is not very worrisome, as Official Developmental Assistance has been quite variable over the past few years and has depended on international and local political priorities. Of total health expenditures, out-of-pocket expenses constitute the largest share and have to be borne mostly by the poor, even when seeking care at government facilities, for instance, while purchasing medicine. Provincial governments' allocations have been even more skewed toward the non-development side, with a considerable share given to tertiary hospitals in all the provinces (Mohammad et al. 2007).
Current health insurance schemes in Pakistan cover only 5% of the population (Asian Development Bank 2005). Likewise, Zakat (the Islamic concept of a luxury tax on 2.5% of dormant wealth over a certain amount unused for a year, collected and used in specified categories), Bait-ul-Maal (a treasury of an Islamic government, used to provide income for the needy, including the poor, elderly, orphans, widows and the disabled) and private health insurance are the other financing mechanisms, catering to a very small proportion of the population.
Alarmingly, private (out-of-pocket) expenditures on health have increased to as high as 80%, thus pushing more people below the poverty line (World Health Organization 2011). Local evidence shows this expense as high as 73% as shown in Figure 2. Because of these high costs, the gap in access to health services by the poorest and wealthiest quintiles has been growing for years. Soaring healthcare costs have burdened poor households with crushing expenditures, aggravating their poverty. Therefore, there is an urgent need to provide them with protection against the impoverishing blows of ill-health (Belay et al. 2010).
Figure 2. Health expenditure coverage in Pakistan

Resource allocation is the distribution of resources among competing groups of people, programs or geographical areas. It refers to fair financing, one of the six building blocks of health systems (World Health Organization 1996). Resource allocation formulas have an essential role to play in the public sector in directing resources to underserved geographic areas, underprivileged population groups and underfunded programs. It is imperative that resource allocation to developmental and non-developmental health plans is evenly distributed across the federation and provinces. Low spending on health is not the only impeding factor in the provision of equitable, accessible and efficient services; there is also an issue of imbalance in allocation of resources to developmental and non-developmental annual plans. Over the years, non-developmental health spending has remained high, compared to the developmental projects' budget. Notably, the provinces spend 70% to 80% of their health expenditures on non-developmental and recurrent expenses, including salaries (Government of Pakistan 2005). Expansion of developmental health plans in the provinces has not factored in population growth, leading to unsatisfactory coverage and substandard quality of public health services, particularly in rural Pakistan. At present, financing mechanisms to reduce out-of-pocket payments and increase the pooling of general taxation are missing. Yet there are opportunities to plan and promote various modes of health system financing.
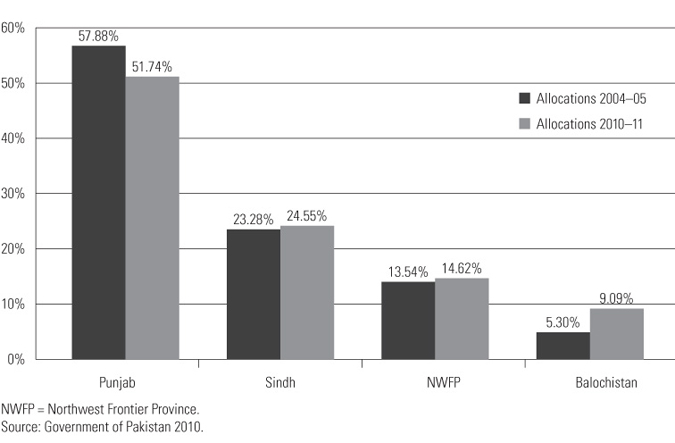
There are federal, provincial and district levels for generation and allocation of public health expenditures in Pakistan. While total funding for the health sector is important, it is instructive to see how it is spent by the respective tiers of government. From the federal level, resources include revenue shares, grants, straight transfers and loans that are transferred to the provincial level, based on a resource allocation formula. The National Finance Commission (NFC) recommends distribution of specified taxes and duties between the federation and provinces and disbursement of grants to provincial governments, and decides on the borrowing powers to be exercised by the federation and provinces (Ahmed et al. 2007). The provincial divisible pool consists of federal tax assignments, straight transfers and provincial tax receipts. Priority expenditures comprise pensions, subsidies, debt servicing and priority programs and are subtracted from the gross divisible pool to arrive at a net divisible pool. The provincial divisible pool is then further divided into a provincial retained amount and a provincial allocable amount, which are 45% and 55%, respectively (Government of Sindh 2004). Population had been the sole criterion for the NFC's formula for distribution to the provinces since the inception of the federation, in 1947. However, in 2010 the NFC adopted a more equitable and fair allocation formula, considering the relative weight of population, level of development, provincial revenue and inverse population density. Consequently, shares were more responsive to the provinces' population needs, as shown in Figure 3 (Government of Pakistan 2010).
Figure 3. Provincial allocations by the National Finance Commission Award in 2004-05 and 2010-11.
Ministry of Finance, Islamabad
Devolution and Health Financing
Pakistan's health system has experienced two major political transitions: the local Government Ordinance in 2001 and, recently, the promulgated 18th constitutional amendment. As a result of devolution of the social and health sector under the latter reform, provincial bodies are now autonomous for administrative and financial decisions. This shift in decision making and health services planning to the provincial bodies opens up many prospects for developing effective financing mechanisms for the health sector. Other countries have sustained reforms and faced financial hardships, yet kept health as a national priority; for example, Cuba sustained political transitions and improved its maternal and child health indicators, with an elevated allocation of 7% of GDP for health spending, matching that of the OECD countries (Pan American Health Organization 2011). Under the seventh NFC award in 2011, there are financial increments for the health and the social sector in each province. This opportunity, with amplified benefits to the health sector, makes the case for generation of broader and sustained financing mechanisms in provincial health systems. Nevertheless, the new arrangement must ensure the diminution of inequities in healthcare utilization (Nishtar 2011).
Although the government's health budget has been gradually increasing over the last few years, no absolute increase has been observed in terms of percentage of GDP, which has remained stagnant at or below 1%, as shown in Figure 4 (Ahmed and Shaikh 2008). Devolution has come with many opportunities as well as some risks in the management of heath financing in the provinces.
Figure 4. Health allocation of government as percentage of GDP over the years

The Government of Pakistan has a history of investing 85% of the health budget for curative care, while primary health services, which cater to 80% of the population, receive only 15% (Nishtar 2010). The provinces' enhanced autonomy after the 18th amendment allows them to manage the pooling and purchasing arrangements for health (World Bank 1998). Now, provinces bear the responsibility of ensuring fair financing in the health system. Accountability mechanisms at the provincial level need to be strengthened to improve performance and transparency in healthcare financing. Another risk is the limited capacity of provinces in managing financing mechanisms. Successful decentralization is critically determined by the local health system's managerial capacity (Spedo et al. 2009). At this time, interim technical support from the federation is desirable not only for swift transfer of financing to the provinces, but also to enable them to build capacity to manage and sustain their own resources.
Health Financing Opportunities with Devolution
It must be ensured that poorer health systems have sufficient funds to scale up the equitable modes of health financing. Low-income countries need to spend at least 35 dollars per capita by 2015 to attain MDGs through universal coverage (World Health Organization 2005). Financial incentives under the last NFC award are well recognized by the provinces, as the new custodians of the health and social sector. Provincial reservations and conflicts over budgetary allocations seem to have been resolved by the 18th amendment. The following recommendations are proposed to create effective health financing mechanisms in the provinces to serve poor segments of the population.
1. Reprioritization of Provincial Budgets
For any health system to function efficiently, it is imperative to set priorities for resource allocation, health services delivery, human resources for health, and a supply of medicine and equipment in various geographical areas. To catch up to MDG targets, provinces must strive to double current health sector allocations (World Health Organization 2011). A transparent and accountable decision-making process is needed to bring evidence-based change. Instead of wasting the already meagre resources, it is high time that we redirect them to high-priority needs. Steps for the health financing decision-making process must include creating a vision and completing a situational analysis, a financial and constraints assessment, development and implementation of proposed strategies, and monitoring and evaluation (World Health Organization 2005). Pakistan's epidemiological and political transition requires that the provinces undertake these steps to revamp health financing mechanisms. The major share of the health budget that is consumed in the non-developmental accounts should be reviewed (Ahmed and Shaikh 2008; World Health Organization 2011). Provinces are now in a position to reallocate finances for developmental and non-developmental sectors, directing an additional benefit to the health and social sector. En route, sufficient allocations will have to be made to incentivize existing human resources as well as fill current vacancies across healthcare delivery levels, from primary to tertiary and across the vertical programs. It may be worthwhile to spend the allocation on public health and essential curative services, leaving the rest to be financed by the private sector perhaps, but mediated through private or social insurance (World Bank 1993). It is an opportune time to give maternal and child health services their due priority, because they serve the most vulnerable segments of the population (Mazhar and Shaikh 2012).
2. Efficient Revenue Collection
Extensive tax and contribution collection capacity is usually observed in the formal economies i.e. having a well structured tax system with registered tax payers, whereas in Pakistan, the informal sector is predominant and accounts for less than 20% of GDP toward general taxation (Nishtar 2010). The federation and provinces must make every effort to collect direct taxation from the formal sector. Likewise, necessary amendments to the present law related to tax collection must be implemented in their true letter and spirit. For broadening the tax collection base, a transparent accountability mechanism must ensure the involvement of the informal sector and other revenue-generating sectors such as agriculture. This will instil greater public confidence in the government's initiatives. The revamped general taxation system of Indonesia, with added benefits to health, accomplished these goals (World Health Organization 2005). Reallocation of a proportion of taxes by the provinces for public health activities would be invaluable for achieving the MDGs by 2015.
3. Social Protection for Health
Social health insurance (SHI) is provided in more than 60 countries around the world (World Bank 2006). Thailand introduced its 30 Baht scheme to promote universal coverage. This novel mode of financing reduced the financial burden on consumers and subsequently discouraged out-of-pocket payments, which occur mostly in the private health sector (Sreshthaputra and Indaratna 2001). Pakistan's current scenario of devolution is ideal for assessing and testing the feasibility of SHI on a small scale (Abrejo and Shaikh 2008). Prepaid vouchers and conditional cash transfers have also been advocated to improve access for the poor to health services and enhance the appropriate service utilization trends (Bellows et al. 2011; Doetinchem et al. 2008). Such modalities have the potential to save households from the health shocks and catastrophic expenditures that push them into the hardships of poverty. Provinces must ensure their stewardship role, which has been defined with multiple facets, from providing a vision for the health of the nation to managing and guaranteeing a just distribution of resources across the health sector (Saltman and Ferroussier-Davis 2000). Pakistan is facing a double burden of disease i.e. a mix of communicable and non-communicable diseases, and today it reflects almost equal shares of both types of diseases. Chronic diseases, which need expensive treatment and hospitalization, must be covered by safety nets designed for vulnerable segments of the population. Provinces have financial autonomy, following the 2011 reforms, and thus it is an opportune time to devolve these powers further to the districts. At the district level, administration is more manageable and poverty indices more easily calculated to identify the actual population to be covered (Mazhar and Shaikh 2012). With the bureaucratic bottlenecks inherent in a federally run system removed, issues can now be effectively addressed in a devolved system and at the district level. A district social security system has already been proposed as part of the government's policy framework (Planning Commission 2005).
4. Innovative Modes of Financing Health
This is an ideal time to envision innovative ways of financing health and enhancing allocations to the health sector. Globally, there is a dire need to explore options for domestic fundraising through direct and indirect taxation. Indirect taxation can be efficiently channelled through increased taxes, for example, on air fare, foreign exchange transactions and other luxuries (World Health Organization 2005). Higher taxes on products hazardous to health, such as tobacco, would benefit the health system by improving the health of the population as well as increasing tax revenue. However, such innovative health-financing mechanisms demand political commitment from the federation as well as from the provinces. Now that provincial stakeholders have an augmented financial share, they ought to make every effort to test alternative modes of health financing. Furthermore, the federation has a pivotal role in developing the technical and managerial capacity of provinces to lay out innovative health financing strategies that will also create an environment of harmony among provinces. Although cost-sharing programs and co-financing schemes have been tested across the country, serious efforts to scale up such innovative schemes are needed. Community financing to mobilize resources for healthcare has been found very effective in reaching a large number of low-income populations who would otherwise have no financial protection against the cost of illness (Ekman 2004). In the wake of the constitutional amendment, provincial governments must strategize to ensure fair financing for facilitating access to healthcare, especially for maternal and child healthcare services (Mazhar and Shaikh 2012).
5. Donor Contributions for Developmental Assistance
Pakistan's unstable macroeconomic indicators and uneven economic growth have resulted in a sizable proportion of the population living in poverty. Although the Government of Pakistan embarked on a poverty reduction strategy that aimed to create jobs, alleviate poverty and improve social indicators (Government of Pakistan 2007), the available finances in a poor country such as Pakistan have not been sufficient to meet MDG targets. To bridge the gap, it is imperative to augment domestic fundraising by seeking enhanced donor contributions for developing countries. It would be worthwhile to tap into the potential of some credible international non-governmental organizations and development partners to help increase the allocation of the health budget (Ejaz et al. 2011). Global solidarity is essential to help low-income countries assuage poverty and increase investment in development plans of the health sector. Under Official Developmental Assistance commitments, high-income countries are pledged to develop the financial capacity of middle- and low-income countries (World Health Organization 2005). This would allow the state to spend more on development plans compared to non-development ones, which would be a fundamental prerequisite for meeting the 35 US dollar per capita spending on health needed to attain the MDGs (World Health Organization 2001). Although Pakistan's health sector has never been entirely dependent on donor financing for health, except for some vertical programs, weaning ourselves off that proportion of funding should be the eventual goal.
Conclusion
Taking stock of healthcare financing in Pakistan provides some critical conclusions: insufficient allocations from tax revenue for the health sector; unjustifiably high amounts spent on tertiary care concentrated in urban areas; visible inequities in access to healthcare and, most serious of all, inefficient distribution of funds and low utilization that result in exclusion of the poor from the health system. Progression toward the MDGs will necessitate extensive political and economic reforms in the civil service and governance structures, and a fair allocation of resources to the health sector (Shaikh 2008; United Nations 2011). Devolution of administrative and financial powers to the provinces in Pakistan should be seen as an opportunity. The provinces must strategize to empower the districts to build their local managerial capacity and accountability mechanisms. The health sector of Pakistan is yearning for a transformational strategy to deliver just and fair financing with a pro-poor approach. Devolution empowers provinces to develop efficient and innovative financing mechanisms that are needed immediately to diminish the overwhelming influence of the private health sector and minimize out-of-payments. Support from the federal government, development partners and training institutions during this transition will enhance technical capacity of provinces and even the districts to experiment with innovative modes of financing.
About the Author(s)
Babar Tasneem Shaikh, MBBS, MBA, MPH, PhD, FRCP Edin, Associate Professor, Health Systems & Policy, Health Services Academy, Islamabad, Pakistan
Irum Ejaz, MBBS, MSc Health Policy & Management, Consultant, Health Services Academy, Islamabad, Pakistan
Arslan Mazhar, MBBS, MPH, Instructor, Health Systems, Health Services Academy, Islamabad, Pakistan
Assad Hafeez, MBBS, FCPS, PhD, Professor, Public Health, Health Services Academy, Islamabad, Pakistan
Correspondence may be directed to: Dr. Babar Tasneem Shaikh, Room B-205, Health Services Academy, Park Road, Chak Shahzad, Islamabad, 44000 Pakistan; Tel.: +92-51-9255590-94, ext. 102; E-mail: shaikh.babar@gmail.com.
References
Abrejo, F.G. and B.T. Shaikh. 2008. "Social Health Insurance: Can We Ever Make a Case for Pakistan?" Journal of Pakistan Medical Association 58(5): 267–70.
Ahmed, I., U. Mustafa and M. Khalid. 2007. National Finance Commission Awards in Pakistan: A Historical Perspective. Pakistan Institute of Development Economics, Islamabad.
Ahmed, J. and B.T. Shaikh. 2008. "An All Time Low Budget for Healthcare in Pakistan." Journal of College of Physicians and Surgeons of Pakistan 18(6): 388–91.
Asian Development Bank. 2005. Technical Assistance to the Islamic Republic of Pakistan for the Developing Social Health Insurance Project. TAR: PAK 37359. Islamabad.
Belay, T., A. Couffinhal, I. Haq, S. Kazi and B. Loevinsohn. 2010. Delivering Better Health Services for Pakistan's Poor. Islamabad: World Bank.
Bellows, N.M., B.W. Bellows and C. Warren. 2011. "The Use of Vouchers for Reproductive Health Services in Developing Countries: Systematic Review." Tropical Medicine and International Health 16(1): 84–96.
Doetinchem, O., K. Xu and G. Carrin. 2008. Conditional Cash Transfers: What's in It for Health? World Health Organization, Geneva.
Ejaz, I., B.T. Shaikh and N. Rizvi. 2011. "NGOs and Government Partnership for Health Systems Strengthening: A Qualitative Study Presenting Viewpoints of Government, NGOs and Donors in Pakistan." BMC Health Services Research 11(1): 122.
Ekman, B. 2004. "Community-Based Health Insurance in Low-Income Countries: A Systematic Review of the Evidence." Health Policy & Planning 19(5): 249–70.
Ghaffar, A., B.M. Qazi and M. Salman. 2000. "Healthcare Systems Transition III. Pakistan, Part I. An Overview of the Healthcare System in Pakistan." Journal of Public Health Medicine 22(1): 38–42.
Government of Pakistan. 2005 Midterm Development Framework 2005–2010. Islamabad: Ministry of Health.
Government of Pakistan. 2007. Ensuring a Demographic Dividend: Unleashing Human Potential in a Globalized World. Poverty Reduction Strategy Paper–II. Islamabad: Ministry of Finance, Islamabad.
Government of Pakistan. 2010. National Finance Commission Award 2010. Islamabad: Ministry of Finance.
Government of Sindh. 2004. Report and Recommendations of the Provincial Finance Commission. Karachi: Provincial Finance Secretariat.
Mazhar, A. and B.T. Shaikh. 2012. "Reforms in Pakistan: Decisive Times for Improving Maternal and Child Health." Healthcare Policy 8(1): 24–32.
Mohammad, K.B., A. Hafeez and S. Nishtar. 2007. "Public Sector Health Financing in Pakistan: A Retrospective Study." Journal of Pakistan Medical Association 57(6): 311–7.
Nishtar, S. 2006. The Gateway Paper–Health Systems in Pakistan – A Way Forward. Islamabad: Heartfile.
Nishtar, S. 2010. Choked Pipes. Reforming Pakistan's Mixed Health System. Karachi: Oxford University Press.
Nishtar, S. 2011. Health and the 18th Amendment: Retaining National functions in Devolution. Retrieved December 20, 2011. < http://www.heartfile.org/pdf/HEALTH_18AM_FINAL.pdf>.
Organization of Economic Cooperation & Development. 2011. OECD Health Data 2011. Retrieved July 21, 2012. <http://www.oecd.org/health/healthdata>.
Pan American Health Organization. 2011. Country Health Profile: Cuba. Retrieved July 21, 2012. <http://www.paho.org/english/sha/prflcub.htm>.
Planning Commission. 2005. Medium-Term Development Framework 2005–10. Islamabad: Government of Pakistan, Federal Ministry of Health.
Poullier, J.P., P. Hernandez, K. Kawabata and W.D. Savedoff. 2002. Patterns of Global Health Expenditures: Results for 191 Countries. EIP/HFS/FAR, Discussion Paper No. 51. World Health Organization: 2002. Retrieved June 17, 2012. <http://www.who.int/healthinfo/paper51.pdf>.
Saltman, R.B. and O. Ferroussier-Davis. 2000. "The Concept of Stewardship in Health Policy." Bulletin of the World Health Organization 78(6): 732–9.
Shaikh, B.T. 2008. "Marching toward the Millennium Development Goals: What about Health Systems, Health-Seeking Behaviours and Health Service Utilization in Pakistan?" World Health & Population 10(2): 44–52. Retrieved July 20, 2012. <http://www.longwoods.com/content/19960>.
Spedo, S.M., O.Y. Tanaka and N.R. Pinto. 2009. "The Challenge of Decentralization of the Unified National Health System in Large Cities: The Case of Sao Paulo, Brazil." Cadernos de Saúde Pública 25(8):1781–90.
Sreshthaputra, N. and K. Indaratna. 2001. The Universal Coverage Policy of Thailand: An Introduction. Asia-Pacific Health Economics Network (APHEN), Bangkok.
United Nations. 2011. The Millennium Development Goals Report 2011. We Can End Poverty. New York: United Nations.
United Nations Development Program. 2010. Human Development Report 2010. The Real Wealth of Nations: Pathways to Human Development. New York: United Nations Development Program.
World Bank. 1993. World Development Report 1993. Investing in Health. Washington, DC: World Bank.
World Bank. 1998. Pakistan – towards a Health Sector Strategy. Washington DC: World Bank, Health, Nutrition and Population Unit, South Asia Region (Report No. 16695-PAK).
World Bank. 2006. "Healthcare Financing in Low-Income Countries." In: Health Financing Revisited. Washington, DC: World Bank.
World Health Organization. 1996. Investing in Health and Development. Report of the ad hoc committee on health research relating to future intervention options. Geneva: World Health Organization. Retrieved June 20, 2011. <http://whqlibdoc.who.int/hq/1996/TDR_GEN_96.2.pdf>.
World Health Organization. 2000. World Health Report 2000. Health Systems: Improving Performance. Geneva: World Health Organization.
World Health Organization. 2001. Macroeconomics and Health: Investing in Health for Economic Development. Geneva: World Health Organization, Report of the Commission on Macroeconomics and Health.
World Health Organization. 2005. Sustainable health financing, universal coverage and social health insurance. Geneva: World Health Organization, Resolution WHA58.33: Fifty-eighth World Health Assembly.
World Health Organization. 2010. Health Systems Financing: The Path to Universal Coverage. World Health Report 2010. Geneva: World Health Organization.
World Health Organization. 2011. World Health Statistics 2011. Geneva: World Health Organization.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed


