Healthcare Policy
Abstract
Optometric labour market projections are provided. First, population growth and ageing-based estimates of the rate of increase of eye-care services in Ontario from 2011 to 2036 are presented, holding the age–sex structure of utilization constant. Then, using data on the 2011 supply and working hours of Ontario's optometrists, the number of optometrists needed to keep the level of optometric services per age–sex-adjusted person comparable over time is estimated. The projections suggest that the number of Ontario optometrists should grow by approximately 30–40 full-time equivalents per year; to offset retirements and account for decreasing work hours, this suggests 77–90 new practitioners are required each year. However, in recent years, the number of Ontario optometrists has been growing faster than this, suggesting either that demand has exceeded supply and/or surpluses will accumulate if this trend continues.
Introduction
Optometric eye care is becoming increasingly important with an ageing population, while, simultaneously, the supply side of the market is altering markedly as practice patterns evolve. Given that the labour market is regulated and that it is not competitive in a neoclassical economic sense for this and other reasons, it is important to take stock of the expected changes on both sides of the optometric labour market as an input into discussions regarding its ongoing operation. This paper therefore provides projections of both utilization and the supply of optometric services over 25 years from 2011 to 2036.
A methodologically similar, though larger, exercise was undertaken for a large range of physician specialties by Denton et al. (2009), and a relevant single-specialty analysis more conceptually similar to this one was conducted for ophthalmology by Bellan and Buske (2007) amid concerns of a looming shortage of ophthalmologists. More recently, however, Bellan et al. (2013) found that ophthalmologist-to-population ratios have stabilized due to an increased number of graduates, declining retirement rates and declining emigration to the US. Bellan et al. (2013), therefore, predicted that, by 2030, the ratio of ophthalmologists to population will increase slightly from current levels, although the number of full-time equivalents (FTEs) will see a small decline. Worldwide, Resnikoff et al. (2012: 783) predicted shortages and suggest that it is "necessary to aggressively train eye care teams now."
There is little evidence regarding the labour market for Canadian optometrists, who are complements to, and sometimes substitutes for, ophthalmologists. Although not quantitative, Dreezer (1996) provided recommendations from the Committee on Optometric Human Resources, which are aimed at balancing the provision of adequate optometric services to the Canadian population with government's desire to manage costs. A section of this report discusses the issue of human resource management for Ontario, including the fact that even if influencing the number of optometrists graduating in Ontario were feasible, interprovincial and international migration can more than offset local initiatives.
Jin and Trope (2011) used the 2005 Canadian Community Health Survey (CCHS) to provide estimates of eye-care demand by age and gender (i.e., demand for both ophthalmology and optometric services). On the supply side, the Canadian Institute for Health Information (CIHI 2010) provided Canadian labour force estimates for optometrists from 2000 to 2009. But, to the best knowledge of the authors, there are no recent estimates of the extent to which the Canadian supply of optometrists will be adequate to keep pace with the growing and ageing Canadian population. This paper aims to partially fill that void by examining the case of Ontario.
Internationally, work similar to this has been conducted for the US and Australia. For the US, both Lee et al. (1995) and White et al. (2000) predicted an excess supply of optometrists relative to projected demand. Horton et al. (2006: 229) found that the number of optometrists was "adequate to meet the needs of the Australian population." By 2009, however, the same authors found that the supply was "more than adequate" (Kiely et al. 2010: 330).
Methods
Increases in utilization for optometric services in Ontario caused by an ageing and growing population are projected of the 25-year period from 2011 to 2036. Estimated utilization rates by age and gender are first obtained from the 2010 CCHS, and these age–sex cell rates are projected forward using Statistics Canada's population growth estimates.1 This allows a more accurate estimate of future utilization than does simply providing optometrist-to-population ratios, as the former accounts for the fact that an ageing and growing population uses more services than one that is merely growing.
Although some factors under study are commonly associated with one or the other side of the market (e.g., population ageing with the demand side, and the number of new optometry graduates with the supply side), in no sense is either a demand or supply curve estimated in this exercise. Rather, extrapolations of utilization observed in a base year are presented. If the market is in equilibrium, then the model projects this equilibrium level of service forward, allowing only for exogenous changes in the population's size and age distribution.2 Potential other future shocks to the equilibrium are addressed in a set of sensitivity tests. If the market was in disequilibrium in the base year, then modest perturbations from the steady state are likely covered by the sensitivity tests, but large deviations would need to be identified in a more extensive data collection and analysis process than that undertaken here. Some labour market studies address clinical "need," which is frequently defined as the hypothesized optimal level of service provision as determined by clinical experts for a population presenting with particular characteristics.3 Clearly, it is neither reasonable to claim that the market equilibrium reflects need, nor that all needs are appropriately met (with positive or negative deviations possible) in the base year. Akin to the disequilibrium case, assessing need would be a much larger exercise than that undertaken in this analysis, which has a more limited scope.4 In this analysis, utilization growth projections are used to ask the following question:
To what extent would Ontario's supply of optometrists be required to grow, and how many annual graduates would be necessary, to keep the level of service constant in each age–sex cell?
Supply-side estimates are based on the stock of Ontario optometrists and their working behaviours as estimated using data from the Health Professionals Database (HPDB) for 2011. The HPDB is a census of practitioners collected annually by the Ontario Ministry of Health and Long-term Care (MoHLTC) from regulatory colleges and is used for health human resource planning. Assuming that optometrists from a given age–gender category will continue to work similar annual hours into the future (that is, for example, a 35-year-old female optometrist in 2016 through 2031 is assumed to work, on average, the same number of hours as a 35-year-old female optometrist in 2011), the study estimates the annual number of new optometrists (new graduates and/or net geographic mobility into the province) that will be required to provide the required service volumes.
Results
Eye-care service utilization
First, the utilization of optometric services in Ontario is estimated. The CCHS asks, "Have you visited an eye specialist, such as an ophthalmologist or optometrist (about your physical, emotional or mental health)?" Respondents who reply affirmatively are then asked the number of times they have visited in the past 12 months. Appendix A provides responses from these questions by age and gender. Youths aged 19 and below are relatively heavy users of eye-care services, but this tapers off with the onset of adulthood. Then, not surprisingly, use increases steadily from about age 20, and the elderly are the most likely to make use of eye-care services. Women visit eye-care specialists slightly more than men.
Note, importantly, that the survey data are unable to distinguish whether the respondent visited an ophthalmologist or an optometrist. In the projections to follow, one must therefore assume that the mix between ophthalmologic and optometric services remains fairly constant going forward and that it is stable across age–gender categories. While there are several reasons that this mix could change, there is no obvious direction for it to take. Sensitivity analysis below examines "high" and "low" utilization of optometry scenarios, which encompass possible changes to the mix between ophthalmology and optometry.
Appendix B provides "medium growth" estimates from Statistics Canada of the population in Ontario over the next 25 years (i.e., each five years from 2011 to 2036). As is well-understood, the population is both increasing in overall size (estimated to increase by 6.4% by 2016 and 33.1% by 2036) and ageing, suggesting that those who make the greatest use of optometric services (the elderly) are likely to see the greatest increases in population.
In Table 1 (details in Appendix C), the results from Appendices A and B are combined to project required optometric services into the future. To do so, the assumption is made that the utilization of services by each age–gender category will remain constant into the future. That is, for example, it is assumed that the average 83-year-old woman will visit an optometrist/ophthalmologist 1.11 times in 2036, just as they do in 2010. However, if the improving health of 83-year-olds means that in reality they visit eye-care providers less than now, the analysis is unable to capture this change. Similarly, changes in technology that could change the needs for services are unaccounted for. However, in the sensitivity analysis, estimates are provided for low- and high-utilization growth scenarios, which should accommodate such changes.
| Table 1. Projection of eye specialist visits (Ontario) | ||
| Year | Total anticipated eye specialist visits | Percentage growth since 2011 |
| 2011 | 6,629,924 | |
| 2016 | 7,206,738 | 8.7 |
| 2021 | 7,857,461 | 18.5 |
| 2026 | 8,565,575 | 29.2 |
| 2031 | 9,282,885 | 40.0 |
| 2036 | 9,947,730 | 50.0 |
| Source: Authors' calculations based on Appendices A and B (see Appendices A and B). Detailed breakdown is available in Appendix C. | ||
Supply of services
CURRENT SUPPLY OF OPTOMETRIC SERVICES
The supply of optometric services is now described. The first set of columns in Table 2 shows the average number of weeks worked by practicing optometrists in the past year by age and gender. Data are from the HPDB, which captures all registered Ontario optometrists. At all ages, males work more weeks on average in the year than females, although these differences are quite small at ages above 45 years. Women under 35 years of age work an average of 3.5 fewer weeks than men of the same age, while women aged 35–44 work 2.5 fewer weeks than their male counterparts. These are quite likely consequences of women of child-bearing age being more likely to take maternity and/or parental leave, and have implications for the number of required optometrists. The second set of columns in Table 2 shows the average number of weekly hours worked over the past year. Women work an average of about 6 hours per week less than men. A gap is apparent at all ages, although the difference is small for those over 55 years of age.
| Table 2. Working time by Ontario optometrists | ||||||||||||
| Average weeks worked in 2011 | Average hours per week | Active optometrists | Full-time equivalents (FTEs) | |||||||||
| Male | Female | Total | Male | Female | Total | Male | Female | Total | Male | Female | Total | |
| <35 years | 43 | 39.5 | 40.6 | 37.4 | 31.6 | 33.4 | 174 | 390 | 564 | 177.8 | 308.7 | 486.4 |
| 35–44 years | 47.3 | 44.8 | 46 | 37.4 | 28.9 | 33 | 264 | 291 | 555 | 296.8 | 239.6 | 536.4 |
| 45–54 years | 46.5 | 45.8 | 46.2 | 38 | 31.2 | 34.9 | 240 | 203 | 443 | 269 | 184.4 | 453.4 |
| 55–64 years | 45.8 | 44.7 | 45.6 | 35.7 | 33 | 35.1 | 226 | 61 | 287 | 234.7 | 57.1 | 291.8 |
| 65 years and older | 44.4 | – | 44.2 | 28.9 | – | 29.2 | 57 | 4 | 61 | 46.5 | 4 | 50.5 |
| Total | 45.8 | 42.8 | 44.3 | 36.6 | 30.8 | 33.7 | 961 | 949 | 1,910 | 1,024.2 | 794.3 | 1,818.5 |
| Source: 2011 HPDB | ||||||||||||
Table 2, on the left-hand side of the lower panel, shows the number of active optometrists for 2011 registered in the HPDB. In total, Ontario had 1,910 active optometrists roughly evenly split between males and females. However, this apparent gender balance masks large differences by age category. Older optometrists are far more likely to be male than female, whereas the younger optometrists are substantially more likely to be female.
Finally, the lower-right set of columns in Table 2 shows the number of FTE male and female optometrists at various ages. "Full-time" is arbitrarily defined as 35 hours per week and 45 weeks per year, or a total of 1,575 annual hours. As women work, on average, less than one FTE, the number of FTE women is less than the number of individuals. Men's count, on the other hand, stays roughly constant. This calculation suggests that the 2011 population of 1,910 optometrists is working the hours of roughly 1,818 full-time, full-year workers.
PROJECTED SUPPLY OF OPTOMETRIC SERVICES
Given the projected increases in utilization from the first section, it is assumed that the number of FTE optometrists would need to grow at a similar rate to keep the service level constant. The third row of Table 3 therefore shows the number of FTEs required to keep the age–sex-adjusted optometric services constant at the baseline level. For example, in 2016, to provide a comparable level of service to that in 2011, the number of FTE optometrists would need to rise by 8.7%, from 1,818 to 1,976. This is an average increase of about 32 FTE optometrists per year, as shown in the fourth column of Table 3. Overall, the annual increase in the number of FTE optometrists is gradual and is always between 32 and 39. Next, the number of new graduates that would be required to bring the total number of FTEs to the desired level is modelled. To do so, five simplifying assumptions are made, with sensitivity tests subsequently undertaken to ascertain their importance.
| Table 3. Summary estimate of future supply required to maintain 2011 service levels | ||||||
| 2011 | 2016 | 2021 | 2026 | 2031 | 2036 | |
| Panel A: Baseline estimate of optometry supply | ||||||
| Anticipated utilization | 6,629,924 | 7,206,738 | 7,857,461 | 8,565,575 | 9,282,885 | 9,947,730 |
| % Growth since 2011 | – | 8.70 | 18.50 | 29.20 | 40.00 | 50.00 |
| FTEs required | 1,818 | 1,976 | 2155 | 2,349 | 2,545 | 2,728 |
| Annual increase in FTEs | – | 32 | 36 | 39 | 39 | 36 |
| Anticipated active optometrists | 1,910 | 2,091 | 2,293 | 2,512 | 2,732 | 2,929 |
| Annual new recruits required | – | 77 | 77 | 87 | 92 | 92 |
| Panel B: Sensitivity of annual new recruits required to changes in assumptions | – | |||||
| Low growth scenario (low demand) | – | 73 | 71 | 77 | 81 | 80 |
| High growth scenario (high demand) | – | 80 | 83 | 97 | 104 | 104 |
| Increasing new graduate male:female ratio to 2/1 | – | 75 | 74 | 82 | 86 | 85 |
| Decreasing percentage male graduates to zero | – | 79 | 81 | 92 | 98 | 100 |
| Steadily declining work hours | – | 100 | 101 | 108 | 110 | 108 |
| Decreasing retirement age to 63 | – | 97 | 90 | 93 | 98 | 99 |
| Increasing retirement age to 67 | – | 68 | 77 | 87 | 92 | 92 |
| Source: Authors' calculation. Assumptions discussed in text. | ||||||
NEW RECRUITS WILL CONTINUE TO BE APPROXIMATELY 33% MALE AND 67% FEMALE
Recently, new graduates have been approximately two-thirds female (Table 2). It is assumed that this ratio will stay constant. If the percentage of males were to increase (decrease), the number of required optometrist graduates would decrease (increase), as males work more hours per year, especially at younger ages.
OPTOMETRISTS OF A GIVEN AGE–GENDER CATEGORY WILL CONTINUE TO WORK THE SAME NUMBER OF ANNUAL HOURS AS CURRENTLY
Naturally, if optometrists change their work habits to work more (fewer) hours, less (more) new graduates will be required to meet the projected utilization increases. It is unlikely, however, that these patterns will change dramatically, particularly the fact that women of child-bearing age work fewer annual hours on average.
EVERYBODY RETIRES AT AGE 65 AND WILL CONTINUE TO DO SO
For simplicity of analysis, it is assumed that all optometrists will retire at the age of 65. This is, in fact, the approximate mean age of retirement, as seen in the HPDB, although there is really a distribution of retirement ages. To the extent that the average retirement age increases (decreases), fewer (more) new graduates would be required to meet projected utilization of services. Furthermore, what we are classifying as "retirement" also captures other reasons for ceasing to practice in Ontario. Therefore, changes to the retirement age should be understood to mean changes in the mean age at which practitioners leave the occupation for any reason (e.g., death or emigration).
THE RATIO OF FTE OPTOMETRISTS TO SERVICES IN 2011 IS THE RATIO TO AIM FOR GOING FORWARD
As discussed above, no claim is made regarding knowledge of the optimal number of optometrists (e.g., a measurement of need). Rather, the question asked is, "How many new annual graduates would be required to maintain approximately the same level of service as provided in 2011?" To the extent that one believes the number of optometrists in the base year is too large (too small), the number of required new graduates will be too high (too low).
Given these assumptions, the number of optometrists who would still be working at each five-year interval is estimated. For example, in 2016, it is assumed that the number of males between ages 45 and 54 will be half what it was in 2011 plus half the number of males aged 35–44 in 2011 (as everybody ages five years). Given their new ages and expected working time, it is then determined how many new graduates it would take to bring the total number of FTEs to the numbers required in the third row of Table 3. The results are in the final row of Panel A of Table 3 (details in Appendix C); it is estimated that for the next 10 years, adding 77 new optometrists per year would keep the total number of optometrists growing at a similar rate to the growth in projected utilization. After 2021, the number of annual new graduates required would increase to 87 until 2026, and 92 thereafter.
CURRENT GROWTH AND SOURCES OF GRADUATES
It is estimated that Ontario will need approximately 77 new optometrists per year. In fact, in the past two years, the number of optometrists in Ontario has been growing by more than 100 per year: from 1,695 in 2009 to 1,795 in 2010, and to 1,910 in 2011, according to the HPDB. This suggests that the number of optometrists is growing at a faster rate than the projected increases in utilization of services holding age–sex-adjusted per-person utilization constant.
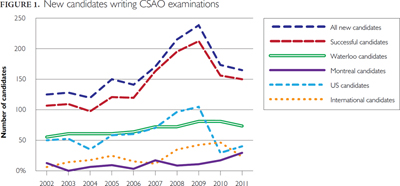
Examined next are some of the sources of new graduates to the Canadian stock of optometrists. As graduates from each of these sources are free to register in the province of their choosing, it should be understood that some percentage of them will locate in Ontario, although numbers may change from year to year. Figure 1 shows the numbers of graduates writing the CSAO (Canadian Standard Assessment in Optometry; as of 2011 replaced by the CACO, Canadian Assessment of Competency in Optometry) examinations in the past decade. The total number of candidates passing the CSAO examination has increased from just over 100 per year in the early 2000s to just over 200 in 2009. It has subsequently fallen somewhat in 2010 and 2011 to about 150 candidates. While the number of domestically trained optometrists (from the only two Canadian programs at the Universities of Waterloo and Montréal) has increased slowly and steadily during this period, the variation in growth comes from both US and other internationally trained optometrists. The decline in applicants between 2009 and 2010 is entirely due to fewer applicants from US schools. There is some anecdotal evidence that this is due to applicants bypassing the CSAO examination by registering in provinces which accept alternative entry-to-practice examinations, although the extent of this is unknown and is outside of the scope of this report. Once registered in any province by any route, however, optometrists can subsequently move to other provinces.
International graduates become eligible to work in Canada by passing the International Optometric Bridging Program (IOBP), and then writing the CASO examinations and registering with their provincial regulator. The IOBP currently enrols an annual number of about 30–35 students, and annual enrolment is capped at 40. Although the number of international candidates writing the CSAO declined in 2011,5 Figure 1 shows that it has otherwise grown steadily since 2007. For a number of reasons, however, the actual number of international graduates practising as optometrists may be smaller than the number writing the CACO indicated in Figure 1. The entry of those studying abroad and wanting to enter Canada, and its effect on the total number of optometrists, has the potential to become an important and political issue, as it did in the case of doctors several years ago. See, for example, Thomson and Cohl (2011a, 2011b) for a discussion of the issues related to international medical graduates.
It must be remembered that for each of these sources, graduates are free to register in any province upon graduation, and thus do not all locate in Ontario. Nevertheless, as described previously, enough new graduates are remaining in Ontario to cause the Ontario stock of optometrists to be rapidly increasing.
SENSITIVITY ANALYSIS
A sensitivity analysis is conducted to measure what effect changes in the main assumptions would have on the number of annual recruits required. The results are presented in the lower panel of Table 3. On the demand side, both Statistics Canada's high and low population growth rates are examined, and it is found that the number of required new recruits would drop to 71–81 in the case of the low growth rate, while it would rise to 80–104 in the case of the high growth rate. Clearly, these changes only make a small difference to the number of required new graduates. These estimates could also be used to consider other possible changes emanating from the demand side, for example, a shift in the ratio of services between ophthalmology and optometry.
On the supply side, the following are examined: the male-to-female ratio of new recruits, optometrists' work habits and their retirement age. For the new recruits' male–female ratio, if the ratio gradually increases from 1/2 to 2/1 by 2036, the number of new recruits required annually declines to 74–85, as male optometrists work more hours than female ones. If the percentage of male graduates gradually decreases to zero by 2036, that is all new recruits are female by 2036, then the number of new recruits required annually ranges from 79 to 100.
The most dramatic of the assumptions is about working habits where extreme trends are allowed for. If the working hours of optometrists reduces at a decreasing rate (5% for the first five years, 4% for the second and 1% by the end of 2036), the number of required new recruits increases to 100–110 per year. It is not surprising, however, that a cumulative decline in working hours of more than 10% per optometrist for the total stock of practitioners results in the need for substantially more new graduates.
Finally, changes to the expected retirement age are examined. If the assumed retirement age increases to age 67, the number of required new recruits declines to 68–92, while the number rises to 90–99, if the retirement age decreases to age 63. Again, retirement can be taken as a proxy for increases or decreases in optometrists leaving the Ontario profession for any reason.
Discussion
Increases in Ontario's requirements for optometric services over the next 25 years have been estimated based on a growing and ageing population, holding age–sex-adjusted utilization constant at 2010 levels. It is found that the quantity of required services will likely grow by 8.7 per cent by 2016 and by 50 per cent by 2036. In 2011, there were 1,910 active optometrists in Ontario, and it is projected that this number would need to grow by about 32–39 FTEs per year over our study period. Including replacement and accounting for the fact that many optometrists do not provide exactly one FTE in service provision, this implies that approximately 77 new optometrists are needed each year until 2021 (rising gradually to 92 in the following years).
In fact, however, the stock of Ontario optometrists has been rising more quickly than this, as the total number of active Ontario optometrists has increased by more than 100 in each of the past two years. If anything, the number of new graduates appears likely to continue to increase. This suggests a rate of growth that will increase the supply of optometrists relative to current utilization levels in the coming years.
Sensitivity tests suggest that these projections of the number of new optometrists required are not particularly sensitive to reasonable changes in the assumptions about utilization growth or optometrists' working time. Furthermore, the current growth in the number of optometrists of more than 100 per year in Ontario is at or beyond the outer limit of any single perturbation in the sensitivity tests. The conclusion that the current growth of optometric labour supply is likely faster than the projected growth in utilization as defined would only be overturned if multiple utilization-increasing scenarios such as those presented in Panel B of Table 3 occurred simultaneously with no countervailing influences. While possible, this is unlikely.
It is important to consider that this analysis begins with measures of utilization (i.e., the current numbers of optometrist visits by age and gender). Importantly, utilization is the (potentially constrained) intersection of demand and supply, and is not in itself a measure of need. While the CCHS estimates regarding visits appear to be roughly in line with the clinical practice guidelines from the Canadian Ophthalmological Society: Clinical Practice Guideline Expert Committee (2007), it is possible that there exists current need/demand for services which is not being met. The finding that supply is growing faster than demand may therefore mean two different things: either the level of any unmet need/demand will be lower in the future or there will be an oversupply of optometrists relative to the need/demand.
Finally, it is worth mentioning that, while the analysis has been conducted only for Ontario, it has implications Canada-wide, as optometrists are largely free to move from one province to another to set-up practice. To date, however, Ontario appears to be among the provinces that have seen the highest growth in numbers of optometrists (see, for example, CIHI, 2010).
Services d'optométrie en Ontario: facteurs liés à l'offre et facteurs liés à la demande, de 2011 à 2036
Résumé
Les prévisions sur le marché du travail pour l'optométrie sont connues. Premièrement, nous considérons la croissance de la population ainsi qu'une estimation de l'accroissement des services oculaires en Ontario, de 2011 à 2036, tenant compte du vieillissement tout en maintenant la structure d'utilisation selon l'âge et le sexe. Ensuite, nous estimons, selon les données de 2011 sur l'offre et les heures de travail des optométristes en Ontario, le nombre d'optométristes nécessaire pour maintenir au cours du temps un niveau comparable de services d'optométrie en fonction de l'âge et du sexe. Ces projections font voir que le nombre d'optométristes en Ontario devrait croître d'environ 30 à 40 équivalents temps plein par année; pour pallier aux retraites et tenir compte d'une diminution des heures de travail, de 77 à 90 nouveaux praticiens par année seraient nécessaires. Cependant, au cours des dernières années, le nombre d'optométristes en Ontario s'est accru plus rapidement, ce qui laisse croire que la demande a dépassé l'offre et/ou qu'il y aura accumulation de surplus si la tendance se maintient.
About the Author(s)
Philip S.J. Leonard, PhD, Post-Doctoral Fellow, Department of Economics, McMaster University, Hamilton, ON
Arthur Sweetman, PhD, Professor, Ontario Research Chair in Health Human Resources, Department of Economics, CHEPA (McMaster University) and IZA, Hamilton, ON
Xue (Helen) Zhang, MA, PhD Student, Department of Economics, McMaster University, Hamilton, ON
Correspondence may be directed to: Philip S.J. Leonard, PhD, Post-Doctoral Fellow, Department of Economics, McMaster University, Hamilton, ON; e-mail: philipsjleonard@hotmail.com.
Acknowledgment
Analyses using Statistics Canada's CCHS were conducted in the Research Data Centre at McMaster University and the authors thank the staff for their assistance.
Funding was provided through a grant from the Ontario MOHLTC's HSRF program, and data access was funded by the Ontario Association of Optometrists. The opinions in this paper are those of the authors and do not necessarily reflect those of Statistics Canada or the Province of Ontario.
References
Bärnighausen, T. and D.E. Bloom. 2011. "The Global Health Workforce." In P. Smith and S. Glied, eds., Oxford Handbook of Health Economics. New York, NY: Oxford University Press.
Bellan, L. and L. Buske. 2007. "Ophthalmology Human Resource Projections: Are We Heading for a Crisis in the Next 15 Years?" Canadian Journal of Ophthalmology [Journal Canadien d'Ophtalmologie] 42(1): 34–38. doi:10.3129/can.
Bellan, L., L. Buske, S. Wang and Y.M. Buys. 2013. "The Landscape of Ophthalmologists in Canada: Present and Future." Canadian Journal of Ophthalmology [Journal Canadien d'Ophtalmologie] 48(3): 160–66. doi:10.1016/j.jcjo.2013.01.017.
Canadian Ophthalmological Society: Clinical Practice Guideline Expert Committee, C. 2007. "Canadian Ophthalmological Society Evidence-Based Clinical Practice Guidelines for the Periodic Eye Examination in Adults in Canada." Canadian Journal of Ophthalmology [Journal Canadien d'Ophtalmologie] 42: 39–45. doi:10.3129/can.
Canadian Institute for Health Information (CIHI). 2010. Canada's Health Care Providers, 2000 to 2009 - A Reference Guide. Ottawa, ON: Author. Retrieved August 14, 2014. <https://secure.cihi.ca/estore/productFamily.htm?locale=en&pf=PFC1661>.
Denton, F.T., A. Gafni and B.G. Spencer. 2009. "Users and Suppliers of Physician Services: A Tale of Two Populations." International Journal of Health Services 39(1): 189–218. doi:10.2190/HS.39.1.i.
Dreezer, S. 1996. Report of the Committee on Optometric Human Resources. Toronto, ON: Ontario Ministry of Health.
Horton, P., P.M. Kiely and J. Chakman. 2006. "The Australian Optometric Workforce 2005." Clinical and Experimental Optometry: Journal of the Australian Optometrical Association 89(4): 229–40. doi:10.1111/j.1444-0938.2006.00048.x.
Jin, Y.-P. and G.E. Trope. 2011. "Eye Care Utilization in Canada: Disparity in the Publicly Funded Health Care System." Canadian Journal of Ophthalmology [Journal Canadien d'Ophtalmologie] 46(2): 133–38. doi:10.3129/i10-120.
Kiely, P.M., P. Horton and J. Chakman. 2010. "The Australian Optometric Workforce 2009." Clinical and Experimental Optometry 93(5): 330–40. doi:10.1111/j.1444-0938.2010.00506.x.
Lee, P.P., C.A. Jackson and D.A. Relles. 1995. "Estimating Eye Care Workforce Supply and Requirements." Ophthalmology 102(12): 1964–71; discussion 1971–72. doi:10.1016/S0161-6420(95)30767-1.
Resnikoff, S., W. Felch, T.-M. Gauthier and B. Spivey. 2012. "The Number of Ophthalmologists in Practice and Training Worldwide: A Growing Gap Despite More Than 200,000 Practitioners." British Journal of Ophthalmology 96(6): 783–87. doi:10.1136/bjophthalmol-2011-301378.
Thomson, G. and K. Cohl. 2011a. IMG Selection: Independent Review of Access to Postgraduate Programs by International Medical Graduates in Ontario, Volume 1: Findings and Recommendations. Submitted to the Ontario Ministry of Health and Long-Term Care and the Council of Ontario Universities.
Thomson, G. and K. Cohl. 2011b. IMG Selection: Independent Review of Access to Postgraduate Programs by International Medical Graduates in Ontario, Volume 2: Analysis and Background. Submitted to the Ontario Ministry of Health and Long-Term Care and the Council of Ontario Universities.
White, A., T. Doksum and C. White. 2000. "Workforce Projections for Optometry." Optometry 71(5): 284–300.
Footnotes
1. Statistics Canada, CANSIM, table 052-0005.
2. An equilibrium would likely not be a simple intersection of a supply and a demand curve. In part, this is because there is a derived demand for optometric services, as the fundamental demand is for vision health, not optometric services per se. However, more directly, the market's institutions make it likely that any equilibrium would be complicated, and quite possibly constrained. Key market institutions and characteristics potentially influencing the equilibrium include the structure of optometry regulation in each province, the actions of various professional associations and education/training institutions, the array of public and private insurance programs paying for optometric services that introduce a gap between the patient and provider, the asymmetric information common in healthcare and Canada's immigration system.
3. For optometry, see the Canadian Ophthalmological Society: Clinical Practice Guideline Expert Committee (2007), which is addressed in the discussion section.
4. For a discussion of these and related issues, see Bärnighausen and Bloom (2011) and the references therein.
5. Eligibility rules were changed in 2011 to require more years of education before becoming eligible to apply to the IOBP. Thanks to Dr. Murray Turnour for helpful discussions.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed