Healthcare Policy
The Impact of the Ontario Fertility Program on Duplicate Fertility Consultations
Angela Assal, Claire Ann Jones, Tamas Gotz and Baiju R. Shah
Abstract
Objectives: The Ontario Fertility Program (OFP) funds 5,000 annual in vitro fertilization (IVF) cycles. We hypothesized that after introduction of the OFP, there would be an increase in duplicate infertility consultations by patients attempting to increase chances at obtaining publicly funded IVF through enlisting at multiple fertility clinics.
Methods: This retrospective observational study included women eligible for healthcare services in Ontario from 2014 to 2016 and compared infertility consultations pre- and post-initiation of the OFP.
Results: Post-OFP, the average number of consultations per patient and the proportion of patients with more than one consult increased (1.04 vs. 1.05, p = 0.015 and 3.8% vs. 4.2%, p = 0.027, respectively). Total consultations for infertility increased from 24,565 to 27,714 post-OFP. The OFP had the largest impact in the Greater Toronto Area (GTA).
Conclusion: The OFP resulted in a statistically significant increase in duplicate consultations, although unlikely to be of clinical relevance. The disproportionate impact seen in the GTA highlights the inequitable access to fertility care in Ontario.
Introduction
Infertility is defined clinically as a disease of the reproductive system characterized by the inability to achieve a pregnancy after 12 months of regular intercourse (Zegers-Hochschild et al. 2009). Approximately one in six couples in Ontario will experience infertility and require assisted reproductive technology (ART) to achieve pregnancy (Greenblatt 2015). ART can include controlled ovarian hyperstimulation, intrauterine insemination (IUI), in vitro fertilization (IVF) and intracytoplasmic sperm injection. In Ontario, 1%–2% of live births are achieved with ART (Greenblatt 2015). As more people delay childbearing, and given the documented decline in fertility with age, a growing number of people are turning to IVF as a means of achieving a pregnancy. IVF is also used by single individuals and many lesbian, gay, bisexual, transgender, and queer (LGBTQ) people to achieve pregnancy, and a growing number of couples are also using ART for the purpose of preimplantation genetic diagnosis to prevent the transmission of known genetic conditions to offspring.
The Ontario Health Insurance Plan (OHIP) initially covered all fertility treatments until 1994. In 1994, IVF was delisted from OHIP requiring individuals to pay out of pocket, apart from persons with bilateral tubal obstructions who remained covered under OHIP until 2015 (Ikonomidis and Dickens 1995). A cycle of IVF typically costs upwards of CAD$15,000 for treatment and medication, making cost a major barrier to access.
On July 24, 2014, the Ontario Legislature passed The Building Opportunity and Securing Our Future Act promising to expand fertility coverage (Sousa 2014). The goal was to increase access to fertility treatments to all Ontarians, regardless of gender, sexual orientation or ability to pay (McGuinty 2007). In keeping with these goals, the Ministry of Health and Long-Term Care (MOHLTC) launched the Ontario Fertility Program (OFP) on December 21, 2015 (Ontario MOHLTC 2015a). The OFP introduced $70 million of funding annually for fertility treatments including cycle monitoring with IUI and IVF (Ontario MOHLTC 2015b). The program is limited to 5,000 IVF cycles per year, with capped cycles per year allocated to each fertility clinic based on their historical demand (Ontario MOHLTC 2015a). However, historical demand was primarily based on patients accessing private IVF, and thus, the increase in demand observed for publicly funded IVF is much greater than the supply, resulting in long wait lists reported up to 1.5 years at the onset of the program (Blackwell 2016). The average wait time for publicly funded OFP in the 2017/2018 fiscal year was 12 months (personal communication, OFP Team 2019). Under the OFP, each person under the age of 43 with a uterus and a valid OHIP card is entitled to one funded cycle, regardless of gender, sexual orientation or presence of a medical diagnosis of infertility (Ontario MOHLTC 2015b). A person is entitled to an additional cycle of IVF if she is acting or has acted as a gestational carrier (Ontario MOHLTC 2015a). There continues to be an option for privately funded IVF with no age restriction, for patients able to afford it, which creates a two-tiered system. Physician consultations at fertility clinics have continued to be covered under OHIP with no restrictions.
At the time of data collection in 2016, there were 51 fertility clinics participating in the OFP: 18 received funding for IVF cycles, whereas the other 33 sites were provided with funding for IUI only. However, many of these non-IVF sites are associated with IVF clinics, and thus, patients from these non-IVF sites could be entered on their affiliated centre's IVF wait list. Currently, in 2019, there are 50 fertility clinics participating in the OFP, with 18 providing IVF (Ontario MOHLTC 2018a). With a limited number of publicly funded cycles available to each of the IVF clinics in Ontario, they have been required to determine their own strategies for resource allocation. No principles of prioritization were suggested by the MOHLTC, and there is no standardization across the province, except for prioritization of cancer patients for fertility preservation. To see a fertility specialist who performs IVF, patients must be referred by another physician and wait for a scheduled consultation before they will have the opportunity to be placed on the clinic's funded IVF wait list. Some clinics post information about their wait list process on their websites, but most patients must wait for their first consultation to learn the clinic's process. Individuals benefit differently based on the fertility clinic's allocation strategy, and most patients would not know which clinic is best suited for them or that discrepancies exist. For example, a younger patient would benefit from attending a clinic that prioritizes successful outcomes versus one that prioritizes women approaching the maximum age for funding under the OFP. Without knowing a clinic's allocation method, a patient cannot choose a clinic with their most advantageous outcome, and it is likely that their family physician is also not aware of these discrepancies between clinics.
When fertility clinics were surveyed in 2016, eight clinics reported using first come, first served, two using lottery and 11 using multiple factors, some of which favoured younger patients and some that favoured older patients, to determine publicly funded IVF allocation (Gotz and Jones 2017). In the 2017/2018 fiscal year, most clinics also reported using a first come, first served wait list policy, often with some additional clinical considerations (e.g., priority for patients requiring fertility preservation) (personal communication, OFP Team 2019).
Given the lack of transparency of IVF wait list prioritization and differing methods of prioritization at different fertility clinics, we hypothesized that patients would be motivated to attend multiple, different clinics to be placed on several waiting lists at the same time. When the OFP was announced, media outlets reported on people attending multiple consultations at different fertility clinics and placing their names on multiple wait lists, trying to maximize their chances of receiving funded IVF as quickly as possible (Zlomislic 2015). The goal of the study was to assess whether there was an increase in the number of multiple consultations per patient by different fertility specialists in Ontario, following the introduction of the OFP. This study aims to obtain relevant information for healthcare policy makers to improve the function of the OFP and inform development of similar programs in the future.
Methods
This was a retrospective observational study. Residents of Ontario who were eligible for OHIP from 2014 to 2016 were included in this analysis. Eligible subjects were women under the age of 43 receiving consultations for infertility in Ontario. Women are defined as individuals who identify as a woman on their Ontario health cards.
Fertility clinics were identified from the OFP's website, which listed all 51 participating clinics at the time. Fertility specialists were identified through a comprehensive search strategy. Fertility clinics' websites were reviewed to determine the names of practicing physicians at their site, regardless of speciality. When this information was not available online, individual clinics were called. Any physician who stated they were a fertility specialist with access to ART was included. Gynaecologic Reproductive Endocrinology and Infertility (GREI)-certified physicians were also identified through searching on the College of Physicians and Surgeons of Ontario (CPSO) online directory. CPSO numbers for all physicians identified through this comprehensive search were obtained from the CPSO.
Consultations by specialists who work at OFP-associated fertility clinics were ascertained by examining the OHIP physician billing claims for the identified physicians. Infertility consultations were identified as claims with a diagnosis code of 628 and a fee code of A205 (OBGYN consultation), A935 (OBGYN special surgical consultation), A135 (internal medicine consultation), A005 (family medicine consultation), A905 (family medicine limited consultation) and A285 (medical biochemistry consultation). These speciality codes were used in accordance with the specialists identified as providing fertility care.
The government announced the OFP implementation plans in October 2015 prior to its initiation on December 21, 2015. The data were analyzed, eliminating the October–December 2015 period when the OFP was introduced and implemented to avoid overestimating the results solely because of the hype of the OFP announcement. Thus, the total number of consultations for infertility by OFP-associated specialists and the average number of consultations by different specialists per patient were compared between January 1, 2016 and December 31, 2016 and the year prior, October 1, 2014 to September 30, 2015. Subgroup analyses of patients aged 40–42 and those living in the Greater Toronto Area (GTA) were performed for the same parameters.
Secondary outcomes were the per cent of repeat consultations over 180-day increments. In each quarter between April 2014 and December 2016, the number of women who had their first consultation was determined, and then, the proportion who had a second consultation with a different specialist within 180 days was assessed. A subgroup analysis looking specifically at women who live within the Toronto, Halton, Peel, York and Durham regions was performed to assess whether duplicate consultations were a phenomenon specific to the GTA.
A logistic regression model was performed looking for relationships between duplicate consults and the following factors: age, income, rurality of locale and pre- or post-OFP implementation period. Effect modification of GTA residence on duplicate consults pre- and post-OFP implementation was tested using an interaction term.
Approval for the study was obtained from the Sunnybrook Health Sciences Research Ethics Board.
Results
The comprehensive search resulted in 129 physicians identified as practicing GREI in Ontario with access to ART, of which 122 hold billing numbers. Table 1 demonstrates the average number of consultations pre- and post-OFP, and the proportion of duplicate consultations. There was an overall increase in total number of consults (24,565 vs. 27,714). Out of all women who had a consult, there was a statistically significant increase in the average number of consultations per patient (1.04 ± 0.21 vs. 1.05 ± 0.23, p = 0.015), and a statistically significant increase in the per cent of patients with more than one consultation (3.8 vs. 4.2%, p = 0.027). Pre-OFP, the absolute number of duplicate consultations was 933 out of a total of 24,565 consultations. Post-OFP, the absolute number of duplicate consultations was 1,164 out of a total of 27,714 consultations. If the 3.8% rate stayed constant, there would have only been 1,053 duplicate consults; thus, an extra 111 duplicate consults were performed. The absolute increase in duplicate consultations was 231.
| Table 1. Assessment for duplicate consultation eliminating the announcement period and subgroup analysis | ||||||||
| Subgroup | Period | Patients with consults* | Number of consults per patient† | Patients with multiple consults§ | ||||
| Mean | SD | p | Total number | % | p | |||
| All patients | Oct 2014–Sep 2015 | 24,565 | 1.04 | 0.21 | 935 | 3.8 | ||
| Jan 2016–Dec 2016 | 27,714 | 1.05 | 0.23 | 0.015 | 1,160 | 4.2 | 0.027 | |
| Age 40–42 | Oct 2014–Sep 2015 | 2,277 | 1.05 | 0.24 | 110 | 4.8 | ||
| Jan 2016–Dec 2016 | 2,919 | 1.06 | 0.26 | 0.3 | 152 | 5.2 | 0.54 | |
| GTA | Oct 2014–Sep 2015 | 15,008 | 1.04 | 0.21 | 555 | 3.7 | ||
| Jan 2016–Dec 2016 | 16,848 | 1.05 | 0.74 | <0.0001 | 767 | 4.6 | 0.0001 | |
| * Consults outside each period not counted. Patients can appear in both periods. §,† Consults with different GREI physicians. |
||||||||
Subgroup analyses were performed for older age and GTA locale (Table 1). When looking at the 40–42 aged subgroup, there was an increase in overall number of consults, but no significant increase in the per cent of multiple consultations (4.8% vs. 5.2%, p = 0.54). Looking at the GTA subgroup, there was an increase in the overall number of consults and a significant increase in the per cent of multiple consultations (3.7% vs. 4.6%, p = 0.0001).
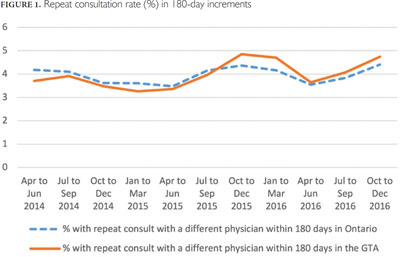
The number of patients who had a repeat consult 180 days after their first consult with a different physician was counted. Results were similar from April 2014 to December 2016 with minimal variability (Figure 1). The same 180-day increments were analyzed for individuals living in the GTA (Figure 1).
OFP implementation did not influence the likelihood of duplicate consultation after adjusting for age, income, rurality of residence and other factors (Table 2). However, GTA residence was a statistically significant effect modifier on this relationship (p = 0.0016). The odds ratio (OR) for duplicate consultation comparing pre- and post-OFP implementation was 1.102 (95% confidence interval = 0.926–1.312) for GTA residents and 0.942 (95% confidence interval = 0.873–1.016) for non-GTA residents. In 2016 there were a total of 10,866 consultations outside the GTA, out of 7,520,454 residents (0.14%). In comparison, there were a total of 16,848 consults in the GTA, out of 5,928,040 residents (0.28%) (Statistics Canada 2016).
| Table 2. Factors associated with duplicate consultations | ||||||
| N | % | OR | LCL | UCL | ||
| Age | <= 29 | 8,875 | 19.4% | Ref | ||
| 30–34 | 16,344 | 35.7% | 1.287 | 1.110 | 1.491 | |
| 35–39 | 15,137 | 33.1% | 1.445 | 1.247 | 1.675 | |
| 40–43 | 5,436 | 11.9% | 1.621 | 1.358 | 1.935 | |
| Income | Lowest | 7,823 | 17.1% | Ref | ||
| 2nd | 8,676 | 18.9% | 0.965 | 0.820 | 1.135 | |
| Mid | 9,254 | 20.2% | 1.029 | 0.879 | 1.205 | |
| 4th | 10,765 | 23.5% | 0.937 | 0.802 | 1.095 | |
| Highest | 9,030 | 19.7% | 1.172 | 1.004 | 1.368 | |
| Missing | 244 | 0.5% | 1.143 | 0.566 | 2.307 | |
| Rurality | Urban | 38,701 | 84.5% | Ref | ||
| Semi-urban | 5,380 | 11.7% | 1.135 | 0.981 | 1.312 | |
| Rural | 1,537 | 3.4% | 1.147 | 0.886 | 1.486 | |
| Missing | 174 | 0.4% | 1.187 | 0.525 | 2.686 | |
| Time period | Pre | 22,594 | 49.3% | Ref | ||
| Post | 23,198 | 50.7% | 1.073 | 0.975 | 1.180 | |
| LCL – lower confidence limit UCL – upper confidence limit |
||||||
Discussion
Funding IVF in Ontario allows for more equitable access to IVF services for people in Ontario. A US study showed that state-mandated insurance coverage for IVF resulted in a threefold increase in IVF utilization compared with states without insurance coverage (Jain et al. 2002). This suggests that in states without coverage, there may be a large number of people who would seek IVF if financial barriers were not present (Jain and Hornstein 2005). Compared with countries where IVF is subsidized, the US has much lower rates of IVF utilization, reflecting that cost is a barrier to access, and when this is eliminated, the actual need is demonstrated (Jain and Hornstein 2005). Similarly, when IVF funding was brought into effect in Quebec in 2010, the number of new consultations for secondary infertility treatment doubled from 14% to 29% immediately post-policy change and remained similar at 8 months at 30%. This could indicate that the availability of funding encouraged patients to seek ART (Tulandi et al. 2013). The increase in demand was so great that the Quebec provincial budget went over estimates by CA$40 million, resulting in discontinuation of the program in 2015 (Hendry 2015). In general, women who utilize ART are more likely to be older, richer, more educated and white (Tulandi et al. 2013). After the Quebec policy change, there were more patients with incomes below the Canadian median (CA$65,000) (47.4% vs. 36.7%, p = 0.02) and more likely to be unemployed (11.6% vs. 3.6%, p < 0.001). Thus, there is evidence that public funding may increase equitable distribution of ART and work towards minimizing barriers such as cost.
By introducing the OFP, the goal was to increase access to IVF for people in Ontario, rather than to promote population growth: "Ontario is committed to supporting people who are trying to start or expand a family by making IVF treatments more accessible regardless of sex, gender, sexual orientation or family status. Women under the age of 43 will be eligible for IVF funding, if a healthcare provider determines this is the most appropriate family-building option for them" (Ontario MOHLTC 2015b). Thus, an explicit goal of this funding program was to expand access to fertility care. After introduction of the OFP, we saw an increase in the number of annual consultations for infertility pre- versus post-OFP implementation (24,565 vs. 27,714, respectively). This suggests that by introducing publicly funded IVF, more people were seeking care for infertility, as patients who previously could not afford IVF could now consider it as an option. The increase in demand can affect access, as there will be increased strain on the system resulting in longer wait times and delays to accessing care. With any change in health policy, there can be unintended negative consequences. Physicians and health administrators were concerned that there would be an increase in the number of duplicate consultations with the introduction of the OFP as an attempt by individuals to obtain IVF as soon as possible, especially among older women attempting to access a funded IVF cycle before the 43-year-old age cut-off. The heterogeneous prioritization methods among fertility clinics are relevant for all patients, but particularly for those who run the risk of aging above the thresholds set for funding eligibility. Author AA reviewed all available clinic websites at the time of publication, and only one clinic publicized their prioritization strategies, which was first come, first served. Thus, for the vast majority of clinics, patients would be unsure of their likelihood of accessing a funded IVF cycle within a specific time frame.
There was a small but statistically significant increase in the rate of duplicate consultations. Although it is unlikely to be clinically relevant, the MOHLTC should consider the cost of duplicate consultations and the associated extra costs, such as repeated diagnostic tests, in the annual budget calculations.
There are many possible hypotheses why a large increase in duplicate consultations did not occur. There is a lack of published data on reasons for lack of duplicate consultations in a publicly funded healthcare program. Thus, the authors have developed proposed theories discussed here. The process by which patients were placed on a funded IVF cycle wait list may have been confusing for patients and family physicians to navigate, and it is possible that a greater increase in duplicate consults was not seen because patients were not aware that they could request multiple consultations at different clinics and that there were different criteria for prioritizing patients at different clinics. Patients may have been generally trusting in the healthcare system to have a fair process. When questioned, patients assumed funds were distributed by a centralized, standardized process and felt the allocation process was not transparent (Assal et al. 2019, manuscript submitted). It is also possible that fertility specialists declined consultations from patients who were already seen at another fertility clinic or that family physicians were not willing to send patients to multiple different doctors for the same medical problem, and thus were acting as good gatekeepers of our medical system whether they had intended to or not. We also speculate that patients may have heard from word of mouth that the wait lists at all fertility clinics were similar and that there would be no advantage to taking the time to attend multiple different clinics. This may be because of a well-distributed number of funded IVF cycle allotments at each fertility clinic, making each clinic's wait list short enough for patients to be satisfied with. A further understanding of the study findings is a future research goal.
Subgroup analyses of women aged 40–42 demonstrated that women in this age group were already at a higher likelihood of receiving multiple consultations. The introduction of the OFP did not affect the rate of duplicate consultations in this group, although this study may have been underpowered to detect a difference in this age group. One would expect that this group of women would be the most likely to seek out duplicate consultations, as they are more likely to age out of eligibility for a funded IVF cycle. The lack of statistical significance may reflect short enough wait times for patients desiring an OFP-funded IVF cycle at fertility clinics, making it not worthwhile to take the time to seek out multiple fertility consultations, or the fact that the wait lists were too long at all clinics for some of these women to be eligible for a funded IVF cycle at any clinic before aging out of the system. Although the wait time was in months to years, this is typical in the Canadian healthcare system. For example, 2018 data from the MOHLTC indicate that the average wait time for a hip replacement in Ontario is 253 days (MOHLTC 2018b). Thus, the wait time for IVF may have been more readily acceptable to patients.
The OFP had a greater impact on the rate of duplicate consultations in the GTA compared with outside the GTA. This is likely because of the higher concentration of fertility clinics in this region making it more accessible to seek out multiple consultations: currently within the GTA, there are 34 fertility clinics, 14 of which provide IVF (MOHLTC 2018a). Outside the GTA, there are currently 16 fertility clinics, four of which provide IVF (MOHLTC 2018b); these four clinics are in London, Burlington, Ottawa and Kingston. There are no fertility clinics offering funded IVF in Northern Ontario, and thus, patients from Northern Ontario typically travel far to access these services in the GTA, demonstrating the inequitable access to IVF services based on geographical location. Thus, people living in the GTA have a greater opportunity to obtain consultations at different clinics. In this study, the greater proportion of consultations seen in the GTA (0.28%) compared with that outside the GTA (0.14%) further demonstrates the inequality of care.
The strengths of this study include taking advantage of a natural experiment caused by a policy change and observing the effects in the population. The use of population-based data allows for complete data and no loss to follow-up. The methods used in this study are subject to certain limitations. People already being followed by a fertility clinic and then seeking a new consultation would not be captured as a duplicate if the initial consultation was prior to October 2014. In addition, if a different diagnostic or billing code was utilized, it would not be captured in this analysis. However, the decision to limit the analysis to consultation billing codes only for infertility was chosen to increase specificity and avoid including women who were not being seen for IVF and could be viewed as a strength of this study. Similarly, there may be fertility physicians who were missed, and thus, their consultation data would be missing. Furthermore, this analysis was limited to female consultations, as the majority of patients seeking IVF are female. However, same-sex male couples seeking fertility consultations for IVF using a donor egg and a gestational carrier would be missed, as these consults are paid for privately by the couple, as well as female-to-male transgender individuals for whom the health card status was designated as male, although this is a small proportion of patients seeking IVF services and likely would not affect overall findings of the study.
Having a centralized system to process IVF funding for patients seems substantively fair, and we hypothesized that it would result in cost savings by eliminating duplicate consultations. However, the data do not support this theory, as the increase in duplicate consultations was not clinically relevant, nor did it result in substantial increased costs to OHIP. Since the data were obtained for this study, wait lists have begun to shorten at individual fertility clinics, averaging one year in Ontario, and more clinics have been moving to a first come, first served model, making the differentiators between clinics less relevant over time (personal communication, OFP Team 2019). This study prompted the researchers to next examine the patients' perspectives on what factors should be considered important in deciding who should receive publicly funded fertility treatments to help guide the MOHLTC and fertility physicians on how to best allocate the limited funded IVF cycles in Ontario in the future.
Conclusion
The OFP introduced publicly funded IVF to a limited number of Ontarians per year with a goal of increasing access to fertility treatments for Ontarians. There is a lack of transparency and standardization of allocation of fertility funding across the province of Ontario. After introduction of the OFP, an increase in overall number of infertility consultations was observed together with a modest increase in OHIP duplicate consultation costs, which was lower than expected in response to the introduction of the OFP. The lack of duplicate consultations outside the GTA may reflect the lack of fertility clinics in these regions, highlighting the need for fertility clinics outside the GTA to provide equitable access to Ontarians.
The results of this study are relevant to healthcare policy makers. When developing similar programs introducing public funding for non—OHIP-covered services, an increase in total number of physician consultations to access the service should be expected. However, the cost of duplicate consultations would not be as high as anticipated, as demonstrated in this study.
Impact du Programme de procréation assistée de l'Ontario sur les demandes d'un second avis en consultation
Résumé
Objectif : Le Programme de procréation assistée de l'Ontario (PAO) permet de financer, chaque année, 5000 cycles de FIV. Notre hypothèse est qu'afin d'accroître les chances d'obtenir une FIV financée par les deniers publics, il y aurait un accroissement des demandes d'un second avis pour les consultations en infertilité suite à la mise en œuvre du PAO, ce qui augmenterait les coûts pour le système de santé publique.
Méthode : Cette étude observationnelle rétrospective porte sur des femmes admissibles aux services de santé ontariens entre 2014 et 2016 et compare le nombre de consultations en infertilité avant et après la mise en œuvre du PAO.
Résultats : Après la mise en œuvre du PAO, le nombre moyen de demandes de règlement pour les patientes qui ont obtenu plus d'une consultation s'est accru (1,04 contre 1,05; p=0,015 et 3,8% contre 4,2%; p=0,027, respectivement). Le nombre total de consultations en infertilité est passé de 24 565 à 27 714 après la mise en œuvre du PAO. L'impact le plus important du PAO touche la Région du Grand Toronto (RGT).
Conclusion : La mise en place du PAO a donné lieu à un faible, quoique statistiquement significatif, accroissement des demandes d'un second avis en consultation. La disproportion observée dans la RGT met en évidence l'iniquité d'accès aux services de fertilité en Ontario.
About the Author(s)
Angela Assal, MD, MHSC, Endocrinologist, Division of Endocrinology and Metabolism, Sunnybrook Health Sciences Centre, Toronto, ON
Claire Ann Jones, MD, GREI Specialist, Department of Obstetrics and Gynaecology, Mount Sinai Fertility, Sinai Health System, Toronto, ON
Tamas Gotz, MD, GREI Specialist, Department of Obstetrics and Gynaecology, Mount Sinai Fertility, Sinai Health System, Toronto, ON
Baiju R. Shah, MD, PhD, Endocrinologist, Division of Endocrinology and Metabolism, Sunnybrook Health Sciences Centre, Institute for Clinical Evaluative Sciences, Toronto, ON
Correspondence may be directed to: Angela Assal, Endocrinology and Metabolism, Clinical Associate, Sunnybrook Health Sciences Centre, H121–2075 Bayview Ave, Toronto, ON M4N 3M5; fax: 416-480-5122; e-mail: angela.assal@sunnybrook.ca
References
Assal, A., N. Chauhan, E. Shin, K. Bowman and C. Jones. 2019. "Perspectives on Resource Allocation of Publicly-Funded Fertility Treatments in Ontario: A Focus Group Study". CMAJ Open (in press).
Blackwell, T. 2016. "'Huge' Demand for IVF Treatment in Ontario – Where It's Fully Funded – Has Wait Lists Stretching to 2018." The National Post. Retrieved December 18, 2018. <https://nationalpost.com/health/huge-demand-for-ivf-treatment-in-ontario-where-its-fully-funded-has-wait-lists-stretching-to-2018>.
Gotz, T. and C. Jones. 2017. "Prioritization of Patients for Publicly Funded IVF in Ontario: A Survey of Fertility Centres." The Journal of Obstetrics and Gynaecology Canada 39(3): 138–44. doi: 10.1016/j.jogc.2016.11.011.
Greenblatt, E. 2015. "Advisory Process for Infertility Services Key Recommendations Report." Retrieved February 6, 2018. <http://health.gov.on.ca/en/public/programs/ivf/docs/ivf_report.pdf>.
Hendry, L. 2015. "New Quebec IVF Treatment Restrictions Leave Couples 'Devastated'". CBC News. Retrieved February 11, 2019. <http://www.cbc.ca/news/canada/montreal/ivf-treatment-funding-quebec-bill-20-muhc-1.3317591>.
Ikonomidis, S. and B. Dickens. 1995. "Ontario's Decision to Defund In Vitro Fertilization Treatment Except for Women with Bilateral Fallopian Tube Damage." Canadian Public Policy 21(3): 379–81.
Jain, T., B.L. Harlow and M.D. Hornstein. 2002. "Insurance Coverage and Outcomes of In Vitro Fertilization." The New England Journal of Medicine, 347: 661–66. doi: 10.1056/NEJMsa013491.
Jain, T. and M.D. Hornstein. 2005. "Disparities in Access to Infertility Services in a State with Mandated Insurance Coverage." Fertility and Sterility, 84(1): 221–23. doi: https://doi.org/10.1016/j.fertnstert.2005.01.118.
McGuinty, D. 2007. "Moving Forward Together: The Ontario Liberal Plan, 2007". Ontario Liberal Party. Retrieved February 8, 2018. <https://www.ontariotrails.on.ca/assets/files/pdf/member-newsletters/2007%20Liberal%20Platform%20Document.pdf>.
OFP Team. January 11, 2019. Personal communication.
Ontario Ministry of Health and Long-Term Care (MOHLTC). 2015a. "Ontario Announces 50 Clinics Offering Government-Funded Fertility Treatments: Helping Ontarians Grow their Families." Retrieved February 6, 2018. <https://news.ontario.ca/mohltc/en/2015/12/ontario-announces-50-clinics-offering-government-funded-fertility-treatments.html>.
Ontario Ministry of Health and Long-Term Care (MOHLTC). 2015b. "Ontario Fertility Program: Fertility Services." Retrieved February 9, 2019. <http://www.health.gov.on.ca/en/pro/programs/fertility/>.
Ontario Ministry of Health and Long-Term Care (MOHLTC). 2018a. "Fertility Services: Participating Clinics in the Fertility Program." Retrieved December 14, 2018. <http://health.gov.on.ca/en/public/programs/ivf/pub_clinics.aspx>.
Ontario Ministry of Health and Long-Term Care (MOHLTC). 2018b. "Surgery and Diagnostic Imaging Results." Retrieved May 25, 2018. <http://www.ontariowaittimes.com/Surgerydi/en/Service_Data.aspx?View=0&Type=0&Modality=2&ModalityString=2&ModalityType=3&ModalityTypeString=3&LHIN=7&city=&pc=&dist=0&hosptID=0&str=&period=0>.
Sousa, C. 2014. "Bill 14: The Building Opportunity and Securing Our Future Act (Budget Measures)." Printed by the Legislative Assembly of Ontario. Ontario, Canada.
Statistics Canada. 2016. Census Profile, 2016 Census. Retrieved January 3, 2019. <https://www12.statcan.gc.ca/census-recensement/2016/dp-pd/prof/details/page.cfm?Lang=E&Geo1=CMACA&Code1=535&Geo2=PR&Code2=35&Data=Count&SearchText=Caledon%20East&SearchType=Begins&SearchPR=01&B1=All>.
Tulandi, T., K. King and P. Zelkowitz. 2013. "Public Funding of and Access to In Vitro Fertilization." The New England Journal of Medicine 368(20): 1948–49. doi: 10.1056/NEJMc1213687.
Zegers-Hochschild, F., G.D. Adamson, J. de Mouzon, O. Ishihara, R. Mansour, K. Nygren et al. 2009. "International Committee for Monitoring Assisted Reproductive Technology and the World Health revised glossary of ART terminology." Fertility and Sterility 92(5): 1520–24. doi: 10.1016/j.fertnstert.2009.09.009.
Zlomislic, D. 2015. "How Government Funded IVF is Turning into a Baby Lottery." The Toronto Star. Retrieved January 28, 2018. <https://www.thestar.com/life/health_wellness/2015/12/16/how-government-funded-ivf-is-turning-into-a-baby-lottery.html>.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed