Healthcare Quarterly
Canada’s Evolving Medicare: Patient-Centred Care
Terrence Montague, Joanna Nemis-White, John Aylen, Emily Torr, Lesli Martin and Amédé Gogovor
Abstract
Canada's universal healthcare program, medicare, continues to evolve. An area of care that has gained increasing attention over the past several years is the general concept and specific components of patient centricity in healthcare delivery. This paper compares key measures of patient-centred care practices recorded in the 2013 and 2016 Health Care in Canada (HCIC) surveys, with the most recent preferences of the public and health professionals obtained in the 2018 HCIC survey, including priorities for improved future care. Timely access and caring care were the public's top-supported components of patient-centred care in the 2013 and 2016 HCIC surveys. In the 2018 HCIC survey, the Canadian public's overwhelming choice as the top-priority component of patient-centred care continued to be care readily and timely accessed, provided in a caring and respectful environment and based on need versus the ability to pay. In contrast, the public's lesser-supported option in all surveys was measurement and stakeholder feedback of actual care and outcomes. Among professionals in 2018, timely access and caring care were also rated as the top characteristics of patient-centred care, followed by care supported by research and expert opinion. Also similar to the public, Canadian healthcare professionals in 2018 rated measurement and feedback of delivered care and outcomes at the bottom of their support list. When the public and professionals were asked in the 2018 survey to prioritize their implementation choices for enhanced patient-centred care going forward, both stakeholder groups chose timely access as their first priority. Measurements and feedback of care and outcomes were rated at the lower end of choices in both groups in 2018. In summary, among key stakeholders, healthcare that is not readily and timely accessed remains the perceived greatest impediment to achievement of patient-centred care in contemporary Canadian medicare. The continued reality of undue delay in accessing healthcare in Canada is disturbing. A companion risk going forward is that all other components of patient-centred care will retreat to a level of irrelevance. Measurement and feedback of care, particularly its timeliness of access and outcomes, are necessary to monitor progress, stimulate innovation and ensure the success of Canadian medicare. Things can be better.
Introduction
Closing healthcare gaps in Canada is a challenging and ongoing proposition (Montague 2004). To facilitate key impediments to optimal care and their potential solutions, 13 sequential Health Care in Canada (HCIC) surveys from 1998 to 2018 have measured and reported the public's and professionals' views of the evolving status of key aspects of Canada's universal healthcare system, medicare (Nemis-White et al. 2014). This paper provides an overview of stakeholders' recently measured perceptions regarding the concept and evolving performance of patient-centred care in contemporary medicare, focusing on key components and implementation priorities as measured in the 2018 HCIC survey and compared to previous HCIC survey measures (Gogovor et al. 2016).
HCIC Members and Data Acquisition
Current HCIC survey members include Canadian Cancer Society, Canadian Home Care Association, Canadian Hospice Palliative Care Association, Canadian Medical Association, Canadian Nurses Association, Canadian Pharmacists Association, Constance Lethbridge Rehabilitation Centre/Centre for Interdisciplinary Research in Rehabilitation, McGill University, Health Charities Coalition of Canada, HealthCareCAN, Innovative Medicines Canada, Institute of Health Economics, Studer Group Canada, Merck Canada, Strive Health Management and CareNet Health Management Consulting.
The principal data used for this analytic review were the findings of the 2013, 2016 and 2018 HCIC surveys. Data sources for each survey were representative samples of the Canadian adult public and a broad spectrum of clinical and administrative health professionals. In the 2013 and 2016/2018 surveys, the public sample sizes were 1,000 and 1,500, respectively. The professional samples averaged 100 each for doctors, nurses, pharmacists, administrators and other healthcare providers (including nutritionists, dietitians, occupational therapists, physical therapists, psychologists and social workers). The sample sizes provide an estimated margin of error of ±2.5% for the public's responses and ±9.8% for each professional group (excluding "other professionals," which does not have an estimated margin of error).
Stakeholders' Levels of Support for Components of Patient-Centred Care
In recent HCIC surveys, the adult public's support for various components of patient-centred care has been remarkably consistent. As outlined in Figure 1, timely access to care and care provided in a caring and respectful manner are, and have consistently been over recent years, the top two choices to enhance patient-centred care in Canada.
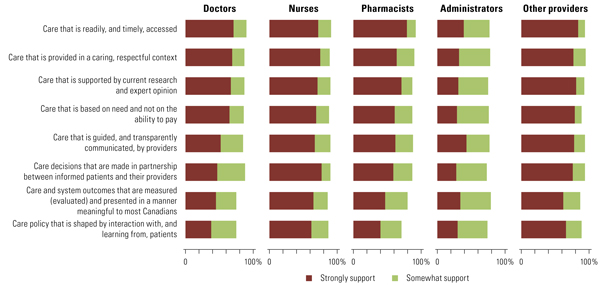
As illustrated in Figure 2, the spectrum of healthcare professionals' recent opinions largely mirrors the views of the public. In particular, care that is readily and timely accessed and care provided in a caring manner were also their top-ranked choices.
Equally consistent, support for measurement and feedback of care practices and outcome results remain at the bottom end of support among both the public and professional stakeholders (Figures 1 and 2).
Figure 1. The Canadian adult public's (n = 1,500) responses when asked in the 2018 Health Care in Canada survey to indicate the extent they oppose or support widespread implementation of each attribute as an effective contribution to enhance patient-centred care, using a scale from 1 to 10, where 1 means they would "strongly oppose" and 10 means they would "strongly support"
Figure 2. Healthcare professionals' responses when asked in the 2018 Health Care in Canada survey to indicate the extent they oppose or support widespread implementation of each attribute as an effective contribution to enhance patient-centred care, using a scale from 1 to 10, where 1 means they would "strongly oppose" and 10 means they would "strongly support" (doctors [n = 100], nurses [n = 99], pharmacists [n = 99], administrators [n = 100], other providers [n = 99])
General Level of Support for Enhancing Patient-Centred Care: Professional Perceptions
A consistent finding in previous HCIC surveys has been the dichotomy of respondents' rankings of support for, versus priority for implementation of, specific therapeutic options. This phenomenon was also apparent in the 2018 survey.
In reply to questions regarding level of support, many choices achieved near-equal and high-level ratings among both public and professional respondents. In contrast, when asked to prioritize patient-centred care attributes for practical clinical implementation, value differentiation among the multitude of choices became more apparent among all respondents. The public's top-priority implementation choices were timely and readily accessed care and care based on need and not on ability to pay (Figure 3). Among healthcare professionals, timely care access also ranked as their first implementation priority, followed by care supported by current research and expert opinion (Figure 4).
Figure 3. Left: The Canadian adult public's hierarchal priorities for enhancing patient-centred care in 2018 when asked: "Which three attributes would you most strongly support?" Right: The average degree of priority for each attribute in the 2013 and 2016 Health Care in Canada surveys
Figure 4. Canadian healthcare professionals' hierarchal priorities for enhancing patient-centred care in the 2018 Health Care in Canada survey when asked: "Which three attributes would you most strongly support?"
Of note, measurement and feedback of care and outcomes to stakeholders remained near the bottom of priorities to improve patient-centred care among both public (Figure 3) and professional (Figure 4) constituencies.
Medicare's Most Lacking Aspect: Stakeholders' Views
To further define stakeholders' priorities regarding future options to improve patient-centred care, respondents in the 2018 HCIC survey were asked to identify which single healthcare attribute is most lacking in contemporary patient-centred care.
The results were remarkably concordant among the public and the majority of healthcare professionals. Briefly, care that is readily and timely accessed was rated first by the public (38%) and professional stakeholders (average 44%, ranging from 58% among physicians to 2% among administrators).
In summary, key stakeholders in the practical day-to-day evolution and implementation of patient-centred care in Canada believe that the dominant issue impeding optimal patient-centred care was, and remains, lack of timely access to care.
Previous analyses of HCIC data reveal that this most-lacking component in real-world healthcare delivery is not evenly distributed within the patient population. Multivariate analyses indicate that it has a particularly high prevalence among younger individuals, especially young women, those living alone and those with chronic diseases (Chan et al. 2018).
The bottom line, however, for all segments of the population is that it remains a major challenge to moving medicare forward.
Going Forward
Looking to the future, acquisition of timely access, although difficult to achieve, appears critical to future success in optimizing patient-centred healthcare as a key component of medicare. However, if non-timely care access persists, a companion realization may arise among stakeholders in its absence. All other companion contributors to patient centricity in healthcare may begin to appear, in the reality of practice, as irrelevant.
In this complex dynamic of searching for patient centricity in healthcare, a companion imperative for medicare to successively move forward is that partnership, measurement and pan-stakeholder feedback of care practices and outcomes are fostered in order to recognize common risks and opportunities and to ensure that best evidence-based therapies are being applied, resulting in predicted optimal outcomes. Measurement and feedback of practice patterns to patients and practitioners work to close care gaps and improve outcomes (Montague 2004, 2013, 2017, 2018).
Things can be better.
About the Author(s)
Terrence Montague, CM, CD, MD, is the principal at CareNet Health Management Consulting and adjunct professor of Medicine at the University of Alberta, Edmonton, AB.
Joanna Nemis-White, BSc, PMP, is the principal at Strive Health Management Consulting Inc., Halifax, NS.
John Aylen, MA, is the president of John Aylen Communications, Montréal, QC.
Emily Torr, BPHE, MSc, is a consultant in healthcare research and knowledge translation, Toronto, ON.
Lesli Martin, BA, is the vice-president of public affairs at Pollara Strategic Insights, Toronto, ON.
Amédé Gogovor, DVM, MSc, PhD, is a research assistant at McGill University and a postdoctoral fellow at Laval University, QC.
References
Chan, C.W.T., A. Gogovor, M.-F. Valois and S. Ahmed. 2018. "Age, Gender, and Current Living Status Were Associated with Perceived Access to Treatment Among Canadians Using a Cross Sectional Survey." BMC Health Services Research 18: 471. doi:10.1186/s12913-018-3215-6.
Gogovor, A., J. Nemis-White, E. Torr, J. Aylen, L. Marshall, S. Ahmed et al., for the 2013–2014 Health Care in Canada Survey Members. 2016. "Patient-Centred, Evidence-Based and Technology-Facilitated Health Care." Retrieved August 6, 2016. <https://www.mcgill.ca/hcic-sssc/files/hcic-sssc/hcic_patient-centred_evidence-based_technology-facilitated_2015.pdf>.
Montague, T. 2004. Patients First: Closing the Health Care Gap in Canada. Mississauga, ON: John Wiley & Sons Canada.
Montague, T., J. Nemis-White, B. Cochrane, J. Meisner and T. Trasler. 2013. "Partnership and Measurement: The Promise, Practice and Theory of a Successful Health Social Networking Strategy." Healthcare Quarterly 16(1): 31–37. doi:10.12927/hcq.2013.23316.
Montague, T., A. Gogovor, J. Aylen, L. Ashey, S. Ahmed, L. Martin, et al. 2017. "Patient-Centred Care in Canada: Key Components and the Path Forward." Healthcare Quarterly 20(1): 50–56. doi:10.12927/hcq.2017.25136.
Montague, T., B. Cochrane, A. Gogovor, J. Aylen, L. Martin and J. Nemis-White. 2018. "Healthcare in Canada: Choices Going Forward." Healthcare Quarterly 21(1): 13–18. doi:10.12927/hcq.2018.25522.
Nemis-White, J., E. Torr, A. Gogovor, L. Marshall, S. Ahmed, J. Aylen et al. for the Health Care in Canada Survey Members. 2014. "Stakeholder Surveys of Canadian Healthcare Performance: What Are They Telling Us? Who Should Be Listening? Who Should Be Acting, and How?" Healthcare Quarterly 17(4): 22–27. doi:10.12927/hcq.2015.24113.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed