Healthcare Policy
Structural Facilitators and Barriers to Access to and Continuity of French-Language Healthcare and Social Services in Ontario’s Champlain Region
Jacinthe Savard, Kate Bigney, Lucy-Ann Kubina, Sébastien Savard and Marie Drolet
Abstract
Purpose: The purpose of this article is to examine access to and continuity of French-language healthcare and social services in Ontario's Champlain region through an analytical framework that incorporates people seeking care, their caregivers and the linguistic component of care into a health and social service system bounded by community, organizational, political and symbolic structures.
Methods: Experiences of French-speaking seniors seeking care and those of health and social service providers and managers from two qualitative exploratory studies are used to describe trajectories through the system.
Results: Participants exposed how, together with community vitality, issues within each of the system's symbolic, political or regulatory and organizational structures influence these trajectories.
Conclusions: To meet the needs of francophone seniors, additional work is needed to increase French-language services coordination within the organizational, regulatory and policy structures of the health and social service system.
Introduction
Living in a linguistic minority context has been identified as a social determinant of health (Bouchard et al. 2012). People in such contexts face major barriers when health and social services are only provided in the majority language (Bowen 2015; De Moissac and Bowen 2017; Lapierre et al. 2014). Language affects the development of a trusting relationship between the person and the provider, and the sense of comfort within that relationship, both of which are fundamental to person-centred services (Drolet et al. 2014; Irvine et al. 2006). Numerous studies outline the consequences of not receiving these services in one's chosen language (Bowen 2015; De Moissac and Bowen 2019; Flores et al. 2012; Madoc-Jones 2004). Even in the case of bilingual individuals, one cannot assume that when dealing with affectively laden health and social issues, the person's linguistic competence is identical in both languages (Castaño et al. 2007; Pavlenko 2012).
Canada has two official languages, English and French. Within many provinces, legislative and policy provisions exist to ensure services to official language minority communities (OLMCs). Among Ontario's population of 14 million, 622,415 are francophone (Office of the French Language Services Commissioner 2018a). Following the enactment of the province's 1986 French Language Services Act (1990), in 2010, oversight of French-language health service delivery in designated areas of the province was assigned to six French-language health planning entities, working in conjunction with the local health integration networks (LHINs). Organizations or agencies are not automatically designated to offer health and social services in French; rather, the LHIN or the entities can identify an organization, or an organization can self-identify to begin the designation process. The steps are numerous, and many identified institutions are aiming for partial designation, that is, they may have committed to offer some services in French and not others (Office of the French Language Services Commissioner 2018b). The province's planning entities have endorsed the principle of Active Offer in French-Language Service (FLS) provision (Regroupement des entités de planification des services de santé en français de l'Ontario et Alliance des Réseaux Ontariens de santé en français 2015), that is, a written or verbal invitation to communicate in the person's preferred official language, preceding the request for services (Bouchard et al. 2012). Yet, obtaining healthcare and social FLS in Ontario is still reported as difficult by many: although there is regional variation, 40% reported that obtaining healthcare in French was very difficult or impossible, and only 33% of francophones in Ontario communicate in French with their family doctor (Gagnon-Arpin et al. 2014).
The purpose of this study is to examine facilitators and barriers to access to and continuity of French-language healthcare and social services in an OLMC: the Champlain region in Ontario. It presents a new analysis of a data subset from two interrelated qualitative studies: one examining care trajectories described by francophone seniors and their caregivers, as well as parents of children, living in the Champlain region1 (Drolet et al. 2015, 2017), and the second exploring facilitators and barriers in FLS access and continuity in the Champlain region and in Winnipeg, Manitoba, with a wider diversity of actors – health and social service managers, providers, physicians, seniors and caregivers (Kubina et al. 2018). Data were analyzed with the help of an analytical framework inspired by models and concepts previously found in the literature. This analytical framework is outlined below, followed by a description of methods and results for the present analysis.
Analytical Framework
An analytical framework (Savard et al. 2020) was designed to organize our data and identify levers of action for improving FLS. It is inspired by Champagne and colleagues (2005), who proposed that health and social services are an organized system of actions, delimited by various structures. The system is intended to reduce illness intensity and duration. It comprises autonomous and interdependent structures (e.g., physical structures, including buildings, technical platforms and budgets; organizational structures or governance; and symbolic structures, including values and collective norms) within which actors, namely, professionals, managers, policy makers and vendors, interact to achieve the system's goals. The framework was adapted to the context of OLMCs by multiple iteration with our data: the structures influencing the provision of FLS include laws and regulations to promote linguistic rights (Foucher 2017), the organization of health and social services (Forgues and Bahi 2017) as well as the community structure and its vitality (Bouchard et al. 2006). These structures provide the actors with playing rules that guide their interaction along the care trajectories.
With a growing emphasis on person-centred care, the person seeking care plays an active role in the trajectory. As highlighted by Wagner and colleagues (1996) in the Chronic Care Model and its variations, health or social service providers, and the senior and the senior's caregivers, are central partners collaborating in the management of health conditions (Bodenheimer et al. 2002). Ideally, professionals are proactive, open to networking and to a multipronged approach. Seniors and their caregivers are better informed and empowered to initiate behaviour and lifestyle changes (Wagner et al. 2001). When surrounded by community resources and public policies conducive to health, professionals and seniors' interactions produce better outcomes (Barr et al. 2003; McCurdy et al. 2008).
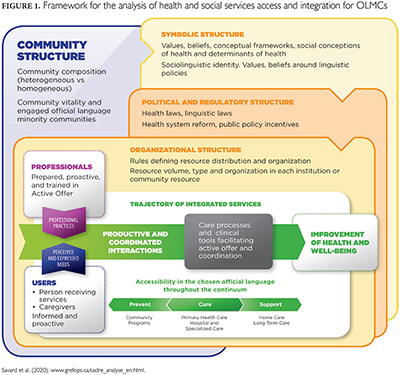
Integration of these concepts is illustrated in Figure 1. At the centre of the illustration is the service trajectory consisting of the encounter(s) of one or more service providers and the person seeking care, supported by one or more caregivers. These actors evolve in a social space influenced by the following structures:
- a symbolic structure, comprising values, beliefs, social representations, perceptions around equity, bilingualism and francophone identity and perception of healthcare and social services;
- a political and regulatory structure, comprising laws, regulations, health and social service government policies and each province's or territory's official language policies;
- an organizational structure, comprising rules that determine resource distribution and organization and the volume and type of resources in each facility; and
- a community structure, including institutions, organized representations, support groups and community services that complement services offered from formal institutions.
The system also includes processes by which the resources are mobilized and used by actors to work toward the system's goals (Champagne et al. 2005). To ensure continuity of FLS during a care trajectory, the processes should include integration mechanisms such as coordination between service organizations (Couturier et al. 2013; Leutz 1999) and supports or resources to facilitate Active Offer (Savard et al. 2017).
Method
The present analysis used a data subset from two previous studies: (1) care trajectories of francophones in the Champlain region (Drolet et al. 2015; Dorlet et al. 2017) and (2) integration of services for francophone seniors in Eastern Ontario and Manitoba (Kubina et al. 2018), the subset consisting of the senior participants in the Champlain region. The region includes many health and social service providers designated under the Ontario French Language Services Act (Champlain LHIN 2014). Both studies and the data subset analysis followed a general qualitative design using content analysis. Methods are presented in more detail in three previous publications (Drolet et al. 2015, 2017; Kubina et al. 2018) and are summarized below. Both studies received ethics approval from appropriate research ethics boards and the participants' written informed consent.
Participants
Participants retained from the first study consisted of nine dyads, each having accessed at least one health and/or social FLS and comprising a francophone senior (65 years or older) living with a chronic illness affecting their communication skills, and their principal caregiver. Chosen for the complexity of their care trajectories, the seniors were living with dementia (n = 4), stroke (n = 4) or Parkinson's (n = 1). Participants' ages ranged from 51 to 94 years (seniors: 60–94; caregivers: 51–81). Seniors or caregivers predominantly self-identified as francophone, with varying degrees of comfort while communicating in English, from very little to fluently bilingual.
From the second study, we included four types of participants from four Champlain region areas (rural, urban and low- and high-density French-speaking populations): (1) service managers (n = 19); (2) health and social service providers who, formally or informally, offered services in French (n = 24); (3) physicians (n = 3); and (4) seniors or caregivers who preferred receiving services in French (n = 23).
Data collection
In the first study, information on care trajectories was collected through two in-depth, semi-structured interviews (Seidman 2006) with seniors and caregivers, covering participants' trajectories through health and social services and their experiences in receiving linguistically appropriate services. The second interview allowed for member checking of previously collected data. The third author conducted all interviews in French from 2012 to 2014, and these were audio-recorded and transcribed verbatim.
In the second study, questions and case studies depicting complex situations inspired by data from the first study were formulated to encourage discussions of integrated practices in general, and in French, in individual interviews or focus groups with managers, providers and physicians. Current collaboration between actors and organizations as well as favourable moments for FLS integration were also addressed. Focus groups with seniors and caregivers focused on FLS access facilitators, service navigation and communication of personal information along the service trajectory. Interviews and focus groups were co-conducted by two team members (Lucy-Ann Kubina and Jacinthe Savard or Lucy-Ann Kubina and Sébastien Savard) from 2015 to 2016, in French or English, audio-recorded and transcribed verbatim. Saturation of data was achieved in this study.
Analysis
For both studies, we performed transcript content analysis to identify code categories and emerging themes (Paillé and Mucchielli 2012). Research team consensus and code validation were obtained. Interrater agreement was sought on 20% of the coded transcripts (Huberman and Miles 2002). The remaining data were coded using this validated list, while allowing for the emergence of new codes.
For the first study, we transposed each interview's findings onto a schematic diagram depicting both the chronology and the complexity of the senior's service utilization, illustrating general and linguistic service discontinuities. In the second study, we explored factors leading to service continuity or discontinuity.
Finally, multiple iterative comparisons of the data from both studies with the evolving analytical framework were done to analyze systemic barriers to and opportunities for service provision in a linguistic minority context within the current health and social service system.
Means to increase trustworthiness included data triangulation (consistent questions posed to different sources: managers, care providers, seniors and their caregivers), data saturation, some member checking and peer debriefing at many points during analysis.
Results
Analysis of care trajectories from the first study shed light on instances of service discontinuity, some inherent to the healthcare and social service system's limited resources and others specific to limited access to FLS. The second study provided a more varied perspective to explain the barriers related to FLS.2 Results are presented according to our analytical framework.
Regarding the service trajectory, participants living in the highly bilingual eastern part of the Champlain region were frequently able to access FLS, such as family physicians, geriatric assessment clinic, diabetic clinic, seniors' day program and a university rehabilitation clinic operating in French. A positive encounter between a senior or a caregiver empowered to request services in French and a proactive provider aware of available resources can lead to a satisfactory service trajectory.
An Anglophone called me. I told her I was Francophone and preferred things in French, and she said, "I will give your name to a Francophone here right away." And [a Francophone] called me back in 5 minutes to chat. (RO-1, caregiver)
However, the opposite was also the case. Even in the presence of bilingual personnel, the environment may not be conducive to providing services in French. One senior reported being spoken to in English by a francophone provider, suggesting a lack of awareness of Active Offer.
Instances of FLS access variability occurred with acute care, in- and outpatient rehabilitation, community-based home support, community or peer support groups and respite services. This inconsistent access along the trajectory was manifested within the various structures, illustrating where access to FLS could be improved.
In the symbolic structure, values and beliefs influence both the demand for and offer of FLS. Several participants reflected on their reluctance to request services in French.
I don't think I have ever asked for service in French, because I don't want to be too demanding. I don't want to start with anything negative with the doctor or the physiotherapist. (RO-80, senior)
Some seniors did request services in French, which usually increased FLS access. Yet, this access is mediated by service availability; thus, highly valuing services in French alone is insufficient. This is illustrated by one participant, whose ability to comprehend and speak English was significantly diminished by illness. The participant reported insisting on services in French but having to accept services in English, such as home-based physiotherapy services and driving evaluation.
Another barrier to requesting services in French is the perception that service will be delayed. Several participants noted that they were unwilling to wait for FLS, preferring to be seen more quickly in the language of the majority.
I'm not ready to go with a delay. If I have a problem, since I can manage in English, I'd as much have the treatment as soon as possible. (RO-87, senior)
This perception may not hold true for a particular service: at the symbolic level, it may reflect past experiences. Or it may be real for the requested service, and thus be a barrier within the organizational structure.
Yet, despite not always asking for FLS, some participants highlighted the difficulty of expressing themselves in English.
It's harder to speak English. … I don't find the words anymore. It's harder and harder as you get older. (RO-85, caregiver)
Some managers were unaware of these difficulties; one stated that francophones their organization serves are bilingual and, therefore, do not require services in French. When provided with examples drawn from actual health and social service encounters, she grasped the connection between linguistically appropriate services and values such as safety and quality of care.
You brought forward in my mind some things I haven't really thought about that much, you know, especially your stories that you … that you told. It's like, oh, awareness is the first step, right? (RO-31, manager)
With respect to the political and regulatory structure, participants' encounters reflected Ontario's FLS legislative framework. In the first study's detailed trajectory analysis, services from fully designated institutions were almost always received in French. In contrast, in partially designated institutions, participants almost always experienced some disruptions in the supply of FLS, whether these services were available in French at certain times or days and not others, or that some services were offered in French and not others. However, the choice to go to a designated facility is often not within the control of the senior or the referring provider. Some services are not available in designated facilities. For example, during a cerebrovascular accident, one participant went to the designated hospital, where treatments required for hemorrhagic stroke were unavailable. The participant was transferred to a partially designated hospital; there, neurology services were not offered in French.
A designated institution also serves the surrounding community, without priority for those with a linguistic preference. Instances of francophones being denied access to existing designated institutions or programs occurred for emergency care as well as in outpatient rehabilitation as demonstrated in the following cases.
I had to go to the emergency room by ambulance, and I said "I want to go to the Montfort (a designated hospital), I want to go to the Montfort," and he said, "No. The Montfort is too busy. We will take you …" They took me to the [non-designated hospital]. (RO-66, senior)
She [the doctor] had sent the request to the Montfort because she knows it's important to me, services in French. But Montfort, they said they had reached their quota. (RO-65, senior)
Me, it's my physiotherapy issue that I specified [I wanted the Montfort] and they called me back to send me to [a non-designated hospital in the city's West end]. And they told me they do a geographic triage. (RO-66, senior)
These examples highlight how designation and regional policies, or institution-specific practices, can interact to produce a disruption in FLS access.
In addition, many respondents turned to private services or community organizations to meet needs that are unmet in the publicly funded system. These services appear less likely to request designation, although some that are owned or operated by francophones do offer FLS. Nonetheless, participants reported that searching for French service providers was challenging, and many respondents had no choice but to accept services in English, such as private night help, private physiotherapy, respite accommodation and personal care, even when this caused some difficulty.
With respect to the organizational structure and care processes, study participants identified specific gaps in FLS access such as a lack of programs in certain geographic areas and access to specialists, fewer of whom speak French.
Managers and providers noted difficulty hiring French-speaking and bilingual personnel. This shortage of linguistically competent resources creates significant communication barriers for those seeking care.
… the secretaries [at the neurologist's office] … speak English and want nothing to do [with French]. They don't even want to let us talk. I understand that the neurologist doesn't have time to talk to every patient, but when you don't speak English, what do you do? (RO-77, senior)
Participants also suggest insufficient formal structural mechanisms to facilitate FLS access. In one underserved region, there had been a recent increase in bilingual physicians. Participants noted no increased access to these physicians. There seemed to be no intentional pairing of bilingual physicians with francophones. When the pairing did occur, it appeared to be due to proactive providers rather than structural mechanisms.
There's no difference. They don't say, that's a Francophone, we'll put the Francophones with the bilingual doctor. No. (RO-93, senior)
… for my francophone clients, we have here [at the community health centre] francophone physicians, and I direct them to the French. Even if I often hear [from staff] "yes, but she [client] understands English," I say: "No, you don't understand. Once again, I tell you, when I am in pain, I am in pain in my first language." (RO-35, provider)
Furthermore, referring francophones to francophone providers was limited by the absence of a comprehensive directory of francophone providers, or unfamiliarity with existing directories.
We need better lists of what's available [in French] and I think that's lacking sometimes (…) that's unfortunate, because when we don't know, we can't offer or we can't recommend. (RO-28, manager)
If the provider does not facilitate FLS continuity, the burden is placed on the senior, as in the case of one senior who was provided with a list of English-speaking physiotherapists by a francophone physician, and told to "look in the phone book" to find a French-speaking therapist.
The community structure can play an important role in FLS access. Community support groups act as networking sites for francophone seniors and caregivers, providing them with peer support and information.
We have meetings [in French], and there we talk, we chat … of our problems, so it helps. (…) It gives you courage to carry on longer. [And] if there is something new, we are [made] aware. (RO-13, caregiver)
Even when a support group is conducted in English, francophone members will seek and connect with francophones in the group. Participants underscored how such groups can offer them opportunities to exchange information regarding available FLS.
Formal health and social service organizations can also link with community groups to increase the visibility of FLS.
So, we go into the buildings … there's a large population of seniors, [our service] will enter and do a general presentation of the care program, services in their community, and they reach more francophones (…) it's a smaller francophone population here [Ottawa West], but there are more there [in the buildings]. (RO-25, manager)
The presence of institutions in the community is also an asset that can facilitate the recruitment of French-speaking or bilingual personnel, as explained by RO-16, manager:
The University of Ottawa now offers the dietician program in French. Now, we easily recruit a dietician. It makes a big difference.
Discussion
In this study, we sought to characterize disruptions in health and social service access and continuity within an official language minority context. As described by study participants, an uninterrupted care and service trajectory in French requires collaboration between the person seeking care, their caregivers and the service providers, and is facilitated by the health and social service system's organizational, political and regulatory as well as symbolic structural contexts.
As found previously (Drolet et al. 2015, 2017), this interaction will be positive when, on the one hand, service providers are proactive and capable of offering services in French or can direct the person to an appropriate resource. On the other hand, individuals and caregivers are sensitive to the importance of communication for quality and safe health and social services and affirm their need to obtain certain services in their preferred language. However, some were reluctant to do so. Being part of a minority culture can lead to feelings of inferiority (Drolet et al. 2017; Forgues and Landry 2014), triggering concerns that the relationship with the health provider could be jeopardized by requesting services in French.
Individuals seeking care and service providers do not operate in a vacuum. Consistent with previous studies, community vitality, including both formal and informal resources such as a local university or support groups, emerged as a factor supporting both supply and demand of FLS. Community vitality enhances communities' capacities to not only compensate for service gaps and facilitate information sharing but also articulate service requests to decision-makers (Bouchard et al. 2006). This is illustrated by the francophone community's response to threats to their institutions: Montfort in 1995 and Office of the French Language Services Commissioner in 2018 (Assemblée de la francophonie de l'Ontario 2018). Community vitality contributes to a sense of pride in an individual's cultural and linguistic community (Forgues and Landry 2014) and to providers' sensitivity to the importance of speaking one's preferred language. Thus, the community and symbolic structures mutually influence each other.
Study participants reported difficulty accessing French-language providers, which reflects a general shortage of such providers (Drolet et al. 2014). However, the number of French-speaking providers does not always translate into FLS, as mechanisms to pair francophones with French-speaking providers are inefficient and often left to the initiative of proactive individuals. The public hardly understands the designation process and which services to expect in partially designated institutions. Such flaws previously identified by service users (Drolet et al. 2015, 2017) were, in this analysis, confirmed by service providers.
Providers supported by their organizations will find it easier to implement Active Offer principles (Savard et al. 2017). In this sense, the French Language Services Act's designation mechanisms seem to affirm providers' FLS offer. In this study, receiving care from a fully designated institution ensured better access to and continuity of care in French, in contrast to non-designated or partially designated institutions. Although generalization would be premature, an examination of designation policies found few mechanisms to ensure that conditions present at the time of designation are maintained over time (Office of the French Language Services Commissioner 2018b).
Furthermore, with the increase in chronic diseases, individuals are more likely to juggle interventions from several social and health service providers from various institutional and community networks. For such a trajectory to be seamless, collaboration and coordination mechanisms among several service providers must not only be present but also account for the linguistic variable (Tremblay et al. 2012). In Ontario, the LHIN is mandated to coordinate services from various provider organizations (OMHLTC 2017a); in collaboration with the entity, they work to identify which agencies should aim for designation to ensure a greater range of FLS (OMHLTC 2017b). This is certainly a positive development, but further coordination is needed.
The findings of this analysis led to some recommendations. Strategies for intentional pairing of francophones to French-speaking providers should be explored within both the organizational and regulatory structures. There is a need for further policies including systematic collection of service users' linguistic preference to facilitate service planning according to francophones' identified needs,3 referral mechanisms that account for linguistic needs and greater communication between health and social services. Policies limiting francophones' access to designated institutions (such as geographic triage or quota) should, when no other FLS are available, be eliminated. Another important strategy includes adequate training in Active Offer of FLS, which includes reinforcing awareness of the link between linguistically appropriate services and current values such as safety and quality of care (Bowen 2015). This training can be left to individual organizations or could be mandated by a governing body. Services in the official language of choice throughout the continuum of care cannot be the responsibility of a single individual or organization; both organizational and policy and regulatory structures must facilitate this coordination.
We acknowledge that linguistic barriers may compromise access to quality healthcare and social services for others whose first language is not the same as the one commonly used in their living area and institutions. However, only English and French are protected by Canadian language laws, thus favouring creation or improvement of FLS. Health and social service professionals have access to resources to learn both official languages, professional training programs offered in both French and English, support from OLMC institutions, etc. Solutions for other linguistic minority communities will differ, opening a range of research possibilities.
Study limitations
The choice to present the results by structure allowed to bring attention to the multiple levers of action for improving FLS. This classification may only be imperfect, as there are interactions between each structural element. Another limitation comes from the data subset: it refers to the Champlain region only and service users of age 65 years and older. Some facilitators and barriers to FLS continuity may be specific to this geographic area or population group. The 65 years and older population is one that presents more complex needs, increasing the importance of improving service access for them. Difficulties in access to linguistically appropriate services has been reported for a different population (Tempier et al. 2015), in other Canadian provinces (Carter 2012; De Moissac et al. 2015; De Moissac and Bowen 2017; Forgues and Landry 2014) and other countries with two official languages such as Wales in the UK (Madoc-Jones 2004; Martin et al. 2018; Roberts and Burton 2013) or Finland (Eriksson-Backa 2008). The proposed framework could be used in future studies for national or international comparison of access to and continuity of health and social services for OLMCs.
Conclusion
Examining the health and social services system's structures revealed complex and unexpected ways in which health policy and institution-specific resource allocation interact to create disruptions in FLS continuity. Our analysis highlights possible points of action for implementing Active Offer principles and health and social service continuity in the official language of choice.
The designation of individual institutions is a good starting point to increase the provision of FLS. However, it does not ensure continuity of FLS for seniors with complex needs requiring many providers. Including service accessibility in the official language of choice as a feature of integrated health services would help meet their needs. It would require additional actions to increase FLS coordination within each of the organizational, regulatory and policy structures of the regional or provincial health and social service system.
Conflict of Interest
The authors have no conflicts of interests to declare. Funding agencies were not involved in data collection and analysis.
Facilitateurs et obstacles structurels à l'accès et à la continuité en français des services sociaux et de santé dans la région ontarienne de Champlain
Résumé
Objectifs : Examiner l'accès aux services sociaux et de santé en français, ainsi que leur continuité, dans la région de Champlain en Ontario, à l'aide d'un cadre d'analyse qui inclut la personne qui demande des services, ses proches aidants et la composante linguistique des services, dans un système de services sociaux et de santé encadré par des structures communautaire, organisationnelle, politique et règlementaire, et symbolique.
Méthode : Les expériences de francophones ayant besoin de services, ainsi que celle de fournisseurs et de gestionnaires de services, tirées de deux études qualitatives exploratoires menées par notre équipe, sont utilisées pour décrire des trajectoires dans le système.
Résultats : Les participants démontrent comment chacune des structures symbolique, politique et règlementaire, organisationnelle, et communautaire influence ces trajectoires.
Conclusion : Pour répondre aux besoins des ainés francophones en situation minoritaire, la coordination des services sociaux et de santé offerts en français devrait être améliorée, tant au sein de la structure organisationnelle que de la structure politique et règlementaire.
About the Author(s)
Jacinthe Savard, PhD, OT REG (ONT), Associate Professor, Occupational Therapy Program, School of Rehabilitation Sciences, University of Ottawa, Research Chair, University of Ottawa and Institut du savoir Montfort, Member, Groupe de recherche sur la formation et les pratiques en santé et service social en contexte francophone minoritaire (GReFoPS), University of Ottawa, Ottawa, ON
Kate Bigney, PhD, Postdoctoral Fellow, GReFoPS, University of Ottawa and Institut du savoir Montfort, Senior Policy Analyst, Agriculture and Agri-Food Canada, Ottawa, ON
Lucy-Ann Kubina, MSC, Former Occupational Therapist, Research Associate, GReFoPS, University of Ottawa, Ottawa, ON
Sébastien Savard, PhD, Full Professor, School of Social Work, University of Ottawa, Member, GReFoPS, University of Ottawa, Member, Institut du savoir Montfort-Recherche, Ottawa, ON
Marie Drolet, PhD, RSW, Full Professor, School of Social Work, University of Ottawa, Founding Member, GReFoPS, University of Ottawa, Project Manager, LE CAP – Centre d'appui et de prévention, Ottawa, ON
Correspondence may be directed to: Jacinthe Savard, PhD, OT Reg (Ont), School of Rehabilitation Sciences, Faculty of Health Sciences, University of Ottawa, 451, Smyth Road, Room 3071, Ottawa, ON K1H 8M5. She can be reached by e-mail at jsavard@uottawa.ca or by phone at (613) 562-5800 x 8065.
Acknowledgment
The authors wish to thank all the seniors, caregivers, service providers and managers who participated in this research.
This work was supported with grants from ARIMA (a Social Sciences and Humanities Research Council–funded partnership) and from the Consortium national de formation en santé (CNFS) Secrétariat national and Volet Université d'Ottawa (funded by Health Canada under the Roadmap for Canada's Official Languages 2013–2018: Education, Immigration, Communities). Opinions expressed in this article are those of the authors and do not necessarily reflect the views of Health Canada or any other funding agency.
References
Assemblée de la francophonie de l'Ontario. 2018. Nouvelles de l'Assemblée: On the First Anniversary of the Université de l'Ontario français, the AFO Announces that It Has Hired Its Legal Team. Retrieved December 18, 2018. <https://monassemblee.ca/en/on-its-first-anniversary-the-universite-de-lontario-francais-announces-that-it-has-hired-its-legal-team/>.
Barr, V.J., S. Robinson, B. Marin-Link, L. Underhill, A. Dotts, D. Ravensdale et al. 2003. The Expanded Chronic Care Model: An Integration of Concepts and Strategies from Population Health Promotion and the Chronic Care Model. Healthcare Quarterly 7(1): 73–82. doi:10.12927/hcq.2003.16763.
Bodenheimer, T., E.H. Wagner and K. Grumbach. 2002. Improving Primary Care for Patients with Chronic Illness. JAM. 288(14): 1775–79. doi:10.1001/jama.288.14.1775.
Bouchard, L., A. Gilbert, R. Landry and K. Deveau. 2006. Social Capital, Health, and Francophone Minorities. Canadian Journal of Public Healt. 97: S16–20. doi: 10.1007/bf03405368.
Bouchard, L., M. Beaulieu and M. Desmeules. 2012. L'offre active de services de santé en français en Ontario: Une mesure d'équité. Reflets: Revue d'intervention sociale et communautair. 18(2): 38–65. doi:10.7202/1013173ar.
Bowen, S. 2015. The Impact of Language Barriers on Patient Safety and Quality of Care. Société Santé en français. Retrieved March 11, 2016. <http://www.santefrancais.ca/wp-content/uploads/2018/11/SSF-Bowen-S.-Language-Barriers-Study-1.pdf>.
Carter, J. 2012. Quel avenir pour les services sociaux et de santé des communautés anglophones du Québec? In R. Bourhis, ed. Déclin et enjeux des communautés de langue anglaise du Québec. Patrimoine Canadien, p. 229–62.
Castaño, M.T., J.L. Biever, C.G. González and K.B. Anderson. 2007. Challenges of Providing Mental Health Services in Spanish. Professional Psychology: Research and Practic. 38(6): 667–73. doi:10.1037/0735-7028.38.6.667.
Champagne, F., A.-P. Contandriopoulos, J. Picot-Touché, F. Béland and H. Nguyen. 2005, September. Un cadre d'évaluation globale de la performance des systèmes de services de santé: Le modèle EGIPSS. Groupe de recherche interdisciplinaire en santé de l'Université de Montréal.
Champlain LHIN. 2014. Health Services Available in French. Retrieved December 12, 2016. <http://www.champlainlhin.on.ca/AboutUs/GetConnectedwithCare.aspx>.
Couturier, Y., D. Gagnon, L. Belzile and M. Salles. 2013. La coordination des services, concepts et méthodes pour le travail social gérontologique. Presses de l'Université de Montréal.
De Moissac, D. and S. Bowen. 2017. Impact of Language Barriers on Access to Healthcare for Official Language Minority Francophones in Canada. Healthcare Management Foru. 30(4): 207–12. doi:10.1177/0840470417706378.
De Moissac, D. and S. Bowen. 2019. Impact of Language Barriers on Quality of Care and Patient Safety for Official Language Minority Francophones in Canada. Journal of Patient Experience 6(1): 24–32. doi:10.1177/2374373518769008.
De Moissac, D., F. Giasson and M. Roch-Gagné. 2015. Accès aux services sociaux et de santé en français: l'expérience des Franco-Manitobains. Minorités linguistiques et société 6: 42–65. doi: 10.7202/1033189ar.
Drolet, M., I. Arcand, J. Benoît, J. Savard, S. Savard and J. Lagacé. 2015. Agir pour avoir accès à des services sociaux et de santé en français: des Francophones en situation minoritaire nous enseignent quoi faire! Canadian Social Work Review/Revue canadienne de service socia. 32(1–2): 5–26. doi: 10.7202/1034141ar.
Drolet, M., J. Savard, J. Benoît, I. Arcand, S. Savard, J. Lagacé et al. 2014. Health Services for Linguistic Minorities in a Bilingual Setting: Challenges for Bilingual Professionals. Qualitative Health Researc. 24(3): 295–305. doi:10.1177/1049732314523503.
Drolet, M., J. Savard, S. Savard, J. Lagacé, I. Arcand, L.A. Kubina et al. 2017. The Experience of Francophones in Eastern Ontario: The Importance of Key Facilitators (Service Users and Providers) and the Influence of Structures Supporting the Health and Social Services System (Chap. 6). In M. Drolet, P. Bouchard and J. Savard eds., Accessibility and Active Offer: Health Care and Social Services in Linguistic Minority Communities (pp. 125–47). University of Ottawa Press.
Eriksson-Backa, K. 2008. Access to Health Information: Perceptions of Barriers among Elderly in a Language Minority. Information Research 13(4): 368. Retrieved January 20, 2020. <http://InformationR.net/ir/13-4/paper368.html>.
Flores, G., M. Abreu, C.P. Barone, R. Bachur and H. Lin. 2012. Errors of Medical Interpretation and Their Potential Clinical Consequences: A Comparison of Professional versus Ad Hoc versus No Interpreters. Annals of Emergency Medicine 60(5): 545–53. doi:10.1016/j.annemergmed.2012.01.025.
French Language Services Act, R.S.O. 1990, c. F.32. Government of Ontario. Retrieved July 6, 2020. <https://www.ontario.ca/laws/statute/90f32>.
Forgues, É. and R. Landry. 2014. L'accès aux services de santé en français et leur utilisation en contexte francophone minoritaire. Institut canadien de recherche sur les minorités linguistiques (ICRML).
Forgues, É. and B. Bahi. 2017. Offering Health Services in French: Between Obstacles and Favourable Factors in Anglophone Hospital Settings. In: M. Drolet, P. Bouchard and J. Savard, eds., Accessibility and Active Offer : Health Care and Social Services in Linguistic Minority Communities (pp. 149–83). University of Ottawa Press.
Foucher, P. 2017. French-Language Health Services in Canada: The State of the Law. In: M. Drolet, P. Bouchard and J. Savard, eds., Accessibility and Active Offer : Health Care and Social Services in Linguistic Minority Communities (pp. 65–83). University of Ottawa Press.
Gagnon-Arpin, I., L. Bouchard, A. Leis and M. Bélanger. 2014. Accès et utilisation des services de santé en langue minoritaire. In R. Landry, ed., La vie dans une langue officielle minoritaire au Canada. Presses de l'Université Laval.
Huberman, A.M. and M.B. Miles. 2002. The Qualitative Researcher's Companion: Classic and Contemporary Readings. SAGE Publications.
Irvine, F.E., G.W. Roberts, P. Jones, L.H. Spencer, C.R. Baker and C. Williams. 2006. Communicative Sensitivity in the Bilingual Healthcare Setting: A Qualitative Study of Language Awareness. Journal of Advanced Nursing 53(4): 422–34. doi:10.1111/j.1365-2648.2006.03733.x.
Kubina, L.A., D. de Moissac, J. Savard, S. Savard, F. Giasson and other collaborators. 2018. Health and Social Services for Francophone Seniors in Eastern Ontario and Manitoba: Guidelines to Improve Continuity of French Language Services. Research Report. GReFoPS, University of Ottawa. Retrieved November 30, 2018. <http://www.grefops.ca/uploads/7/4/7/3/7473881/intégral__services_sociaux_santé_pa_francophones_grefops.pdf>.
Lapierre, S., C. Coderre, I. Côté, M.-L. Garceau and C. Bourassa. 2014. Quand le manque d'accès aux services en français revictimise les femmes victimes de violence conjugale et leurs enfants. Reflets: Revue d'intervention sociale et communautair. 20(2): 22–51. doi:10.7202/1027585ar.
Leutz, W.N. 1999. Five Laws for Integrating Medical and Social Services: Lessons from the United States and the United Kingdom. The Milbank Quarterly 77(1): 77–110. doi:10.1111/1468-0009.00125.
Madoc-Jones, I. 2004. Linguistic Sensitivity, Indigenous Peoples and the Mental Health System in Wales. International Journal of Mental Health Nursin. 13(4): 216–24. doi:10.1111/j.1440-0979.2004.00337.x.
Martin, C., B. Woods and S. Williams. 2018. Language and Culture in the Caregiving of People with Dementia in Care Homes – What Are the Implications for Well-Being? A Scoping Review with a Welsh Perspective. Journal of Cross-Cultural Gerontolog. 34(1): 67–114. doi:10.1007/s10823-018-9361-9.
McCurdy, B., C. MacKay, E. Badley, P. Veinot and C. Cott. 2008, April. A Proposed Evaluation Framework for Chronic Disease Prevention and Management Initiatives in Ontario. Arthritis Community Research & Evaluation (ACREU) – University Health Network. Retrieved December 31, 2014. <http://www.acreu.ca/pdf/pub5/08-02.pdf>.
Office of the French Language Services Commissioner. 2018a. 2017–2018 Annual Report: Looking Ahead, Getting Ready. Retrieved November 30, 2018. <https://csfontario.ca/wp-content/uploads/2018/07/OFLSC-283633-Annual-Report-2017-2018_ENG.pdf>.
Office of the French Language Services Commissioner. 2018b, March. Special Study – Designation: [Re]Vitalize French Language Services. Retrieved November 30, 2018. <https://csfontario.ca/wp-content/uploads/2018/03/OFLSC-275398-Special-Report_2018_03_06_EN-FINAL.pdf>.
Ontario Ministry of Health and Long-Term Care (OMHLTC). 2017a. Local Health Integration Networks. Retrieved November 30, 2018. <http://health.gov.on.ca/en/common/system/services/lhin/default.aspx>.
Ontario Ministry of Health and Long-Term Care (OMHLTC). 2017b. French Language Health Services: French Language Health Planning Entities under the Local Health System Integration Act. 2006 and Regulation 515/09. Retrieved November 30, 2018. <http://www.health.gov.on.ca/en/public/programs/flhs/planning.aspx>.
Paillé, P. and A. Mucchielli. 2012. L'analyse qualitative en sciences humaines et sociales. Armand Colin.
Pavlenko, A. 2012. Affective Processing in Bilingual Speakers: Disembodied Cognition? International Journal of Psycholog. 47(6): 405–28. doi:10.1080/00207594.2012.743665.
Regroupement des entités de planification des services de santé en français de l'Ontario et Alliance des Réseaux Ontariens de santé en français. 2015. Énoncé de position commune sur l'offre active des services de santé en français en Ontario. Retrieved November 25, 2016. <http://rssfe.on.ca/upload-ck/Enonce_OffreActive_10mars15_FR.pdf>.
Roberts, G.W. and C.R. Burton. 2013. Implementing the Evidence for Language-Appropriate Health Care Systems: The Welsh Context. Canadian Journal of Public Health 104(6 Suppl 1): S88–90. doi:10.17269/cjph.104.3496.
Savard, J., L. Casimiro, P. Bouchard and Benoît, J. 2017. Behaviours Demonstrating Active Offer: Identification, Measurement, and Determinants. In M. Drolet, P. Bouchard and J. Savard, eds., Accessibility and Active Offer: Health Care and Social Services in Linguistic Minority Communitie. (pp. 281–317). University of Ottawa Press.
Savard, J, S. Savard, M. Drolet, D. de Moissac, L.A. Kunina, S. van Kemenade et al. 2020. Framework for the Analysis of Health and Social Services Access and Integration for Official Language Minority Communities. Retrieved April 29, 2020. <http://www.grefops.ca/uploads/7/4/7/3/7473881/cadre_explication_pour_site_web_ang_avril2020.pdf>.
Seidman, I. 2006. Interviewing as Qualitative Research: A Guide for Researchers in Education and the Social Sciences. Teachers College Press, Columbia University.
Tempier, R., E.M. Bouattane and J.P. Hirdes. 2015. Access to Psychiatrists by French-Speaking Patients in Ontario Hospitals: 2005 to 2013. Healthcare Management Forum 28(4): 167–71. doi:10.1177/0840470415581244.
Tremblay, S., D. Angus and B. Hubert. 2012. Étude exploratoire en matière de services de santé intégrés pour les communautés francophones: Rapport présenté au Réseau des services de santé en français de l'Est de l'Ontario. PGF Consultants Inc. Retrieved June 1, 2016. <https://d3n8a8pro7vhmx.cloudfront.net/coopontariofr/pages/46/attachments/original/1510261561/Etudeexploratoireenmatieredeservicesdesanteintegrespourlescommunautesfrancophones.pdf?1510261561>.
Wagner, E.H., B.T. Austin, C. Davis, M. Hindmarsh, J. Schaefer and A. Bonomi. 2001. Improving Chronic Illness Care: Translating Evidence into Action. Health Affairs 20(6): 64–78. doi:10.1377/hlthaff.20.6.64.
Wagner, E.H., B.T. Austin and M.V. Korff. 1996. Organizing Care for Patients with Chronic Illness. The Milbank Quarterl. 74(4): 511–44. doi:10.2307/3350391.
Footnotes
1. The Champlain region is in Eastern Ontario. See http://www.champlainlhin.on.ca/AboutUs/GeoPopHlthData/Geography.aspx.
2. The present analysis focuses on the structural factors influencing access to and continuity of FLS. Previous descriptions of the care trajectories and the way key facilitators (caregivers or professional service providers) had solved problems around obstacles have already been published (Drolet et al. 2015, 2017). See also http://www.grefops.ca/uploads/7/4/7/3/7473881/les_trajectoires.pdf for the schematic representation of the nine service trajectories studied in more detail (in French) and http://www.grefops.ca/complementary-results.html for more citations and citations in the original French where applicable.
3. At the time of writing, a motion was voted by Ontario Legislature asking the government to add linguistic identity to the data contained in the Ontario Health Insurance Plan (OHIP) card. See Office of the French Language Services Commissioner (October 5, 2018). Linguistic variable for patients: the OHIP card could become smart! Retrieved November 28, 2018. <https://csfontario.ca/en/articles/6554>.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed