Healthcare Policy
Evaluation of Rheumatology Workforce Supply Changes in Ontario, Canada, from 2000 to 2030
Abstract
Rheumatology workforces are increasingly challenged by too few physicians in face of the growing burden of rheumatic and musculoskeletal diseases (RMDs). Rheumatology is one of the most frequent non-surgical specialty referrals and has the longest wait times for subspecialists. We used a population-based approach to describe changes in the rheumatology workforce, patient volumes and geographic variation in the supply of and access to rheumatologists, in Ontario, Canada, between 2000 and 2019, and projected changes in supply by 2030. Over time, we observed greater feminization of the workforce and increasing age of workforce members. We identified a large regional variation in rheumatology supply. Fewer new patients are seen annually, which likely contributes to increasing wait times and reduced access to care. Strategies and policies to raise the critical mass and improve regional distribution of supply to effectively provide rheumatology care and support the healthcare delivery of patients with RMDs are needed.
Introduction
Rheumatic and musculoskeletal diseases (RMDs) represent a multitude of degenerative, inflammatory and autoimmune conditions affecting millions of people worldwide (Al Maini et al. 2015). RMDs have one of the largest impacts on population health in terms of death and disability (GBD 2013 Mortality and Causes of Death Collaborators 2015; Global Burden of Disease Study 2013 Collaborators 2015). The costs associated with RMDs are significant. For example, tumour necrosis factor inhibitors (TNFis), now a therapeutic mainstay in rheumatology, gastroenterology and dermatology, remain the costliest therapeutic category in Canada, costing public drug plans $801.4 million in 2016; yet, only 0.5% of beneficiaries use these drugs (CIHI 2018). TNFis also accounted for 55% of growth in public spending on prescription drugs between 2007 and 2012 (CIHI 2012). There is potential to avoid these costly interventions, as advances in early diagnoses and treatment strategies for inflammatory arthritis have revolutionized patient care. Improving early access to rheumatologists for diagnosis and treatment with disease-modifying anti-rheumatic drugs (such as methotrexate in rheumatoid arthritis), could result in savings of almost $39 billion over the next 30 years (Bombardier et al. 2011). Thus, while rheumatologists represent a small subspecialty, they have the potential to influence a large and growing segment of healthcare spending.
It is well established that rheumatology specialty care is vital to the timely and accurate diagnosis and treatment of RMDs and to improving health outcomes of various RMD-affected populations (Gossec et al. 2016; Keeling et al. 2018; Monti et al. 2015). Currently, Canadian healthcare for RMDs is suboptimal, indicating barriers to accessing rheumatology specialty care and timely treatment (Barber et al. 2020; Lacaille et al. 2005; Widdifield et al. 2016b). Rheumatology is one of the most frequent non-surgical specialty referrals (Liddy et al. 2017) and has the longest wait times for subspecialists (Jaakkimainen et al. 2014; Shadd et al. 2011), far exceeding established benchmarks for timely care (Barber et al. 2020; Widdifield et al. 2016a, 2016b). High-volume rheumatology practices have been reported as a barrier to providing guideline-concordant care (Haraoui et al. 2012). Restricted availability of rheumatology services may create barriers to optimal care, contributing to suboptimal outcomes, increased healthcare costs and reduced quality of life (Barnabe et al. 2015; Feldman et al. 2013; Haraoui et al. 2012; Harris et al. 2013; Pease et al. 2010; Widdifield et al. 2016a, 2016b, 2017a, 2017b; Yazdany and MacLean 2008; Yazdany et al. 2014). There are increasing concerns over the rapidly rising prevalence of RMDs in aging populations placing greater demands on rheumatology services (Al Maini et al. 2015). Furthermore, smaller subspecialties, such as rheumatology, are especially sensitive to minor changes in physician supply. Thus, understanding rheumatology supply is vital for developing sound health human resource policies.
Within Canada, the number of rheumatologists has increased over time, but remains inadequate compared to the numbers in other Organisation for Economic Co-operation and Development countries. As of 2018, there were approximately 400 rheumatologists practising in Canada (Barber et al. 2017), leaving an estimated deficit of 200 rheumatologists, with all provinces failing to meet the Canadian Rheumatology Association recommendation of one rheumatologist per 75,000 population (Barber et al. 2017). This Canadian recommendation may underestimate population demand requirements for rheumatologists, as a recent international systematic review estimated that approximately two rheumatologists per 100,000 adults are needed (Dejaco et al. 2016). Despite the discrepancy in the ratio of rheumatology supply recommendations, international reports have identified major demographic and geographic changes that are significantly impacting rheumatology workforces, including baby boomer retirements, a millennial predominance and an increase in female and part-time providers (Battafarano et al. 2018). In addition, the major advancements in medication (biologics and small molecules) and diagnostic tools have made it increasingly difficult for primary care physicians to provide comprehensive care to the RMD-affected population due to the growing array of advanced services used in rheumatology (Isaacs 2015).
To date, previous Canadian rheumatology workforce studies have involved physician surveys, which may be incomplete and do not evaluate trends over time (Barber et al. 2017; Brophy et al. 2016; Kur and Koehler 2011). Ontario, being the most populous Canadian province, contains the largest Canadian rheumatology workforce, and while rheumatology supply differs across Canada, changing workforce characteristics in Ontario are likely to be generalizable to the Canadian rheumatology workforce as a whole. Ontario also contains a validated physician registry linkable to health services data, whereas, in many other Canadian provinces, there is no identifier to distinguish rheumatologists from internists in their provincial administrative data sets (Barber et al. 2020), making it difficult to evaluate health services use by patients of rheumatologists.
The purpose of this study is to describe changes in the Ontario rheumatology workforce and activity over the past 19 years. In addition, we sought to quantify provincial and practice-level patient volumes and geographic variation in the supply of and access to rheumatologists.
Method
We conducted a population-based study using linked health administrative databases in Ontario from 2000 to 2019. Rheumatologists and their characteristics were identified using the ICES Physician Database, which is constructed and routinely validated using the Ontario Health Insurance Plan (OHIP) Corporate Provider Database, Ontario Physician Human Resources Data Centre and physicians' OHIP billings. We included active rheumatologists defined as those with fee-for-service claims during each fiscal year. Pediatric rheumatologists were not included. We identified all patients 18 years and older with rheumatology encounters by linking the OHIP claims history database and the Registered Persons Database (RPDB). Annual population denominators were derived from the RPDB, including all living OHIP beneficiaries who had had contact with the healthcare system in the past seven years.
We identified the annual number of rheumatologists overall by clinical full-time equivalents (FTEs) classification and by healthcare planning region. Using annual fee-for-service billing claims, physicians below the 40th percentile of total billings were classified as providing less clinical activity (<1 FTE), 40th to 60th percentile were classified as 1 FTE, and >60th percentile as >1 FTE (Alberta Medical Association 2015). Practice volumes (defined as the median number of patient visits per year) and practice sizes (defined as the median number of unique patients per year) were assessed according to clinical FTE classification. To identify new patients, we applied a three-year washout period to identify individuals with no prior rheumatology contacts. Regional rheumatology supply, patient encounter rates, and access measures were assessed across 14 Local Health Integration Networks (LHINs). Measures of cross-boundary flow across LHINs assessed the local service rate and regional outflow rate. We used geographic information systems to map patient encounter rates across 76 sub-regions and the locations of rheumatology practices for 2019 as well as primary practice locations and maps of patients' inflow and outflow across LHINs.
Descriptive statistics were used to analyze characteristics of rheumatologists and their patients by fiscal year. Per capita rheumatology supply is expressed as per 75,000 residents, and provider-level rheumatology volume rates are expressed per 1,000 population.
A traditional stock-and-flow projection model was developed to project the provincial supply of rheumatologists by 2030. This was done by using the most current data available in 2019 and accounting for the addition of the rheumatology residents entering the practising rheumatology population, and the subtraction of the retiring rheumatologist population. Estimated practice entry cohort numbers were ascertained from the Canadian Post-M.D. Education Registry (CAPER 2019). Two alternative assumptions were made on the annual number of new rheumatologists entering the workforce, including a high scenario (assuming growth trends over time, with one additional trainee entering the workforce per year on top of the 15 new rheumatologists reported in 2019) and a low scenario (assuming the practice entry cohort remained constant). Both projected estimates assumed all graduates of Ontario training programs remained to practise in Ontario.
Results
There were 146 active rheumatologists in 2000, which increased to 230 rheumatologists by 2019 (Table 1). More female rheumatologists and more international graduates entered the workforce over this time. There was a shift in workforce demographics, with 66% male rheumatologists in 2000 compared to 48% in 2019. The overall workforce is aging, with an increasing proportion of rheumatologists aged 60 and older (16% in 2000 vs. 25% in 2019). More male rheumatologists were identified as high-volume providers across each time point (Table 1). There was a significant reduction in the median (interquartile range [IQR]) days providing patient care, from 220 (178–243) days in 2000 to 172 (136–210) days in 2019.
| TABLE 1. Demographics and clinical activity of the Ontario rheumatology workforce | |||
| Year | |||
| Demographics | 2000 | 2008 | 2019 |
| Total number of rheumatologists | 146 | 155 | 230 |
| Female, n (%) | 50 (34.3%) | 59 (38.1%) | 119 (51.7%) |
| Number of >1 FTE rheumatologists | 89 | 94 | 139 |
| Female1, n (%) | 24 (16.4%) | 29 (18.7%) | 65 (28.3%) |
| Male1, n (%) | 65 (44.5%) | 65 (41.9%) | 74 (32.2%) |
| Age, mean (SD) <40 years of age, n (%) 41 to 60 years of age, n (%) >60 years of age, n (%) |
48.5 (10.6) 34 (23.3%) 88 (60.3%) 24 (16.4%) |
51.5 (10.9) 31 (20.0%) 94 (60.6%) 30 (19.4%) |
49.1 (12.7%) 69 (30.0%) 102 (45.2%) 57 (24.8%) |
| Urban location2, n (%) | 105 (71.9%) | 145 (93.6%) | 218 (94.8%) |
| Canadian medical graduate, n (%) | 108 (74.0%) | 118 (76.1%) | 129 (56.1%) |
| High volume provider: >10 patient encounters/day on >209 days in the year3 Both sexes, n (%) Male rheumatologists, n (%) Female rheumatologists, n (%) |
43 (29.5%) 36 (37.5%) 7 (14.0%) |
38 (24.5%) 33 (34.4%) 5 (8.5%) |
45 (19.6%) 31 (27.9%) 14 (11.8%) |
| Number of days with patient assessments in the year4, median (IQR) | 220 (178–243) | 189 (143–224) | 172 (136–210) |
| Number of rheumatologists with hospital encounters5 n (%) | 127 (87.0) | 129 (83.2) | 151 (65.7%) |
| 1 Denominator is the total number of rheumatologists. 2 Urban location defined using the rurality index of Ontario. 3 209 days is a proposed benchmark for FTE (26). 4 Based on the number of days on which a physician provided at least one claim for an assessment during the fiscal year. 5 Based on the number of rheumatologists with at least one OHIP C fee code. |
|||
We observed a noticeable difference in rheumatology practice volumes and practice sizes according to clinical FTE classification (Table 2, available here). Median patient volumes and practice sizes per rheumatologist were the lowest in 2019, and there was a reduction in the median number of new patients seen per rheumatologist over the years.
Despite the growth to the workforce between 2000 and 2019, the percentage of the Ontario population seen by an Ontario rheumatologist remained constant at <3% (Table 3). Patients of rheumatologists were predominately female (68%), with an increasing proportion of older adults across time.
| Table 3. Characteristics of patients with rheumatology encounters | |||
| Year | |||
| Patient characteristics | 2000 | 2008 | 2019 |
| Number of Ontarians who visited a rheumatologist | 245,486 | 280,072 | 326,814 |
| Percentage of Ontarians under rheumatology care 1 | 2.7% | 2.8% | 2.8% |
| Age, years median (IQR) | 58 (46, 70) | 59 (48, 71) | 61 (49, 72) |
| Males (all ages) n (%) | 76,691 (31.2%) | 88,275 (31.5%) | 105,265 (32.2%) |
| 18 to 34 years, n (%) | 6,969 (9.1%) | 6,621 (7.5%) | 9,448 (9.0%) |
| 35 to 64 years, n (%) | 42,344 (55.2%) | 48,812 (55.3%) | 51,281 (48.7%) |
| 65 to 84 years, n (%) | 25,052 (32.7%) | 29,377 (33.3%) | 39,245 (37.3%) |
| >85 years, n (%) | 2,326 (3.0%) | 3,465 (3.9%) | 5,291 (5.0%) |
| Females (all ages), n (%) | 168,795 (68.8%) | 191,797 (68.5%) | 22,1549 (67.8%) |
| 18 to 34 years, n (%) | 13,299 (7.9%) | 12,401 (6.5%) | 18,663 (8.4%) |
| 35 to 64 years, n (%) | 94,724 (56.1%) | 106,812 (55.7%) | 109,661 (49.5%) |
| 65 to 84 years, n (%) | 55,154 (32.7%) | 63,972 (33.4%) | 81,117 (36.6%) |
| >85 years, n (%) | 5,618 (3.3%) | 8,612 (4.5%) | 12,108 (5.5%) |
| Ratio (females/males) | 2.2 | 2.2 | 2.1 |
| 1 18 years and older for population denominator. IQR = interquartile range. |
|||
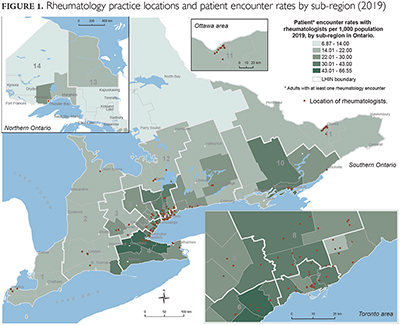
In 2019, the provincial per capita rheumatology supply was 0.9 FTEs per 75,000 residents. There was a large regional variation in rheumatology supply and access (Table 4, available here ; Figure 1), ranging from 4.8% of residents in Hamilton seeing a rheumatologist compared to 0.8% in the North East LHIN (the latter of whom travelled a mean distance of 354 km to see a rheumatologist). There was also a strong linear correlation between regional rheumatology supply and volume rates.
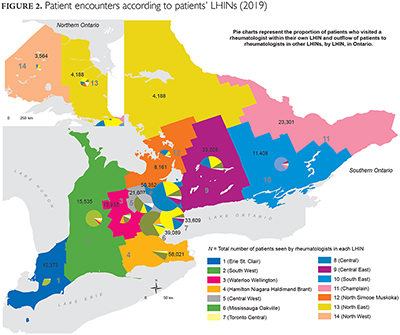
We also observed significant cross-boundary flow with some patients travelling long distances to see rheumatologists in other areas of the province (Table 4 , available online at longwoods.com/content/26428; Figure 2). Collectively, four LHINs (Hamilton Niagara, Mississauga Halton, Toronto Central, and Central [comprising Newmarket, North York, Richmond Hill]) provide rheumatology services to 66% of all of Ontario's rheumatology patient population (Table 4 and Figure A1, available online at longwoods.com/content/26428).
In our projection of the rheumatology workforce by 2030 – accounting for the incoming rheumatology workforce and the outflow of retiring rheumatologists – our high scenario (continued growth model) predicted a total of 363 Ontario rheumatologists by 2030, comprising 218 clinical FTEs. Based on our low scenario, a projected workforce by 2030 would comprise a total of 308 rheumatologists, of which 185 would be clinical FTEs.
Interpretation
Our findings provide baseline information on the state of rheumatology supply in Ontario for developing sound health human resource policies. Over the past two decades, several important rheumatology workforce changes took place, which were identified in this study. We discuss these changes and their implications on the future supply of and access to rheumatologists to inform considerations for workforce policy development.
The first notable trend is the growth in the total number of rheumatologists in Ontario. However, the overall clinical workforce remains low, with only 139 rheumatologists practising at or above one clinical FTE as of 2019. We project a modest increase by 2030. Despite the growth, changes in the demographic characteristics of the workforce – including increasing age of workforce members and more female rheumatologists over time (Table 1) – are unlikely to sustain the same level of patient volumes and services as previously. On average, studies have reported that female physicians work fewer hours than male physicians (Bae et al. 2016; Fisher et al. 2014; Pelley et al. 2016; Spector et al. 2014) and on a part-time basis (Pearse et al. 2001; Spector et al. 2014), and are more likely to take periods of leave (Bae et al. 2016), which could result in reduced workforce clinical capacity to meet population needs. Indeed, we found that there were twice as many male rheumatologists practising as at least one FTE or as a high-volume provider compared to the number of female rheumatologists. The declining number of annual days providing clinical service may also be reflective of generational effects as younger physicians (under 35 years) in the US and Canada report working fewer hours than previous generations (The Royal College of Physicians and Surgeons of Canada 2009; Deal et al. 2007; The College of Family Physicians of Canada et al. 2019). We also identified that average practice volumes and sizes were the lowest in 2019. Generational effects alone may not be the only cause for declining service capacity. Other factors – including additional administrative workloads, such as the migration to electronic medical records, drug authorization approvals and insurance form completion, greater demands for continuing medical education and research activity – could be impacting clinical capacity.
The complexity of care is also increasing among this patient population, which may also impact workforce capacity. The aging patient demographic and complexity of care management involved with comorbid illnesses in aging populations is placing greater demands on rheumatology services (Al Maini et al. 2015; Roubille et al. 2015). Due to the chronic nature of RMDs and high co-occurrence of multimorbidity and disability, patients require complex medication regimens and consistent, longitudinal interaction with rheumatology care. We have previously shown changes over time to the composition of patients under rheumatology care, with fewer patients being seen with non-inflammatory conditions (e.g., osteoarthritis and self-limiting musculoskeletal conditions) in recent years (Widdifield et al. 2020). A separate Ontario study identified that 17% of rheumatology referrals did not result in a rheumatology consultation (Widdifield et al. 2016b). In the present study, the proportion of the Ontarians under rheumatology care remained constant (2.7%) during our study period, despite a rising burden of RMDs in the population (Eder et al. 2019; O'Donnell et al. 2011; Widdifield et al. 2013) and growth in rheumatology supply. Taken together, these findings are likely a reflection of rheumatologists adapting to prioritize patients with systemic inflammatory conditions in light of a strained rheumatology supply. Other areas of Canada have similarly reported the prioritization of systemic inflammatory conditions in rheumatology care and the triage of patients as a means to improve access to care (Delaurier et al. 2012; Hazlewood et al. 2016).
Furthermore, Ontario rheumatology practice sizes and patient volumes (Table 2) appear to be in excess of those reported for both American (Raffoul et al. 2016) and Canadian family physicians, who have a median number of 1,025 to 1,400 patients (Ministry of Health and Long-Term Care 2011). There is evidence from primary care that the quality of care, access to services and continuity of care delivered decreases when physicians care for large practice panels (Campbell 1996; Hogg et al. 2009; Hudon et al. 2004; Murray et al. 2007; Russell et al. 2009; Wilkin and Metcalfe 1984). As clinics become saturated with patients requiring chronic care, rheumatologists' ability to provide services to new patients declines. Despite the growth in workforce size, on average, fewer new patients per rheumatologist are being seen. Moreover, as a large number of rheumatologists in the workforce are currently exiting the workforce (n = 72 nearing retirement), new rheumatologists entering the workforce are not necessarily increasing patient access, as they are taking over existing established rheumatology practices, which already contain a high case-load of patients requiring chronic care.
Finally, our findings highlight significant regional disparities in rheumatology supply, which have persisted during the study period. We observed a lower proportion of area residents seen by rheumatologists in areas with lower rheumatology supply. Thus, many areas in Ontario are insufficiently serviced, creating inequitable access to care. Regional maldistribution of rheumatology supply is also necessitating long travel times (and potentially long wait times) for patients looking to access a rheumatologist. Evidence suggests that more attention is needed on the distribution of physicians and not simply the absolute supply of physicians (Goodman 2004). Considering that RMDs often impair mobility, which hampers patients' ability to participate in society and in seeking medical care, barriers to rheumatology care also need to be understood using an ethical paradigm (MacKenzie et al. 2005; Rom et al. 2007). Early diagnosis of RMDs is critical in lessening disability, permanent organ system damage, potential disfigurement, poor health outcomes including premature mortality and excessive and unsustainable prescription drug costs (van Nies et al. 2014). Thus, ensuring this vulnerable patient population receives accurate and timely care is of great concern. In addition, as two-thirds of the rheumatology patient population are female, the inequitable access to care is disproportionally affecting women.
Our results are concordant with previous Canadian research on an insufficient rheumatology supply and maldistribution of rheumatologists across Canada (Barber et al. 2017; Brophy et al. 2016). A comprehensive US workforce study reported a ratio of provider per 100,000 patients as 3.1 in the northeast to 1.3 in the southwest in 2015 (Battafarano et al. 2018). The US rheumatology workforce also projected major demographic and geographic changes that will significantly impact the supply of the future workforce in parallel with an increased demand for adult rheumatology care due to the growing and aging US population (Battafarano et al. 2018).
Ontario rheumatologists practise using the fee-for-service model and currently there is no specific funding allocated for physiotherapists, occupational therapists, nurse practitioners (NPs), physician assistants (PAs), administrative overhead and nursing staff who are essential to supporting rheumatologists caring for people with RMDs. In order to support a sustainable rheumatology workforce, a competent health workforce is required to support the effective implementation of models of care and the associated models of service delivery (Chehade et al. 2016). While clinical service capacity may be increased by models of care that integrate the work of multidisciplinary teams – thereby shifting work flow, responsibilities and access to programs – the impact on workforce capacity arising from the implementation of alternative service delivery models has not been comprehensively studied in Canada (Chehade et al. 2016). Expanding the rheumatology workforce capacity, by incorporating well-trained allied health practitioners, NPs and PAs, has been a viable option in the US and England (Hooker 2008; Solomon et al. 2014). However, rheumatologists remain a vital component of all models of care involving systemic RMDs (Arthritis Alliance of Canada 2014; Keeling et al. 2018; Smolen et al. 2017). These multidisciplinary care models may also be associated with superior patient clinical outcomes (Solomon et al. 2015) and improving access to care and treatment for patients with RMDs (Ahluwalia et al. 2020). While multidisciplinary care funding models exist in some areas of Canada (Martin 2015; Stewart and Teo 2014), stable funding in Ontario would increase the ability of rheumatologists to provide more comprehensive care to a larger volume of patients, and improve earlier access to care. Health budgets would likely benefit from a reduction in health costs through avoidance of inappropriate delays to care, unnecessary investigations and a reduction in complications resulting from inadequately or inappropriately treated disease. However, the cost-effectiveness of models of care and multidisciplinary care funding models in the context of rheumatology is an area in need of future study.
Strengths of this study include the use of population-based data from a large single-payer jurisdiction, which has the strength of being relatively complete for rheumatology billing claims and population coverage. Moreover, Ontario has a validated physician registry, whereas in other provinces it is difficult to accurately distinguish rheumatologists from internists in administrative data. Although the use of administrative data represents an advantage to this study, we were unable to assess the totality of physician activity (e.g., time spent with patients). Another caveat is that some rheumatologists practise in multiple locations, and we were only able to identify each physician's primary practice location. In addition, supply projections are dependent upon assumptions that do not take into account transfers between provinces or international medical graduates. Further research is needed to predict the demand for supply taking into account population needs.
In summary, Ontario rheumatology supply falls below the national benchmark of one FTE per 75,000 population, and many regions are without equitable access to care. Changing workforce demographics is further compounding service capacity. The implications of our work should drive policies related to improving distribution and not merely supply of rheumatologists. The increase in the absolute number of rheumatologists in Ontario also needs to be viewed in the context of the changes occurring within the workforce, including the increasing proportion of female rheumatologists, generational effects and that rheumatology practices may be operating at an unsustainable capacity. Strategies and policies to raise the critical mass to effectively provide rheumatology care and support healthcare delivery to patients with RMDs across Ontario are urgently needed.
Funding
This study was funded by an operating grant from the Canadian Initiative for Outcomes in Rheumatology Care. This study was supported by ICES that is funded by an annual grant from the Ontario Ministry of Health and Long-Term Care (MOHLTC). Parts of this material are based on data and information compiled and provided by the MOHLTC. The opinions, results and conclusions reported in this paper are those of the authors and are independent from the funding and data sources. No endorsement by ICES or the Ontario MOHLTC is intended or should be inferred. Widdifield receives support from the Arthritis Society Stars Career Development Award (STAR-19-0610). Barber receives support from the Arthritis Society Stars Career Development Award funded by the Canadian Institutes of Health Research (CIHR) Institute of Musculoskeletal Health and Arthritis (STAR-19-0611/CIHR SI2-169745). Bernatsky holds a career award from the Fonds de la recherche en santé du Québec.
Évaluation des changements dans l'offre de main-d'œuvre en rhumatologie en Ontario, au Canada, de 2000 à 2030
Résumé
La main-d'œuvre en rhumatologie est de plus en plus confrontée au manque de médecins et au fardeau croissant des maladies rhumatismales et musculosquelettiques (MRM). La rhumatologie constitue l'une des spécialités non chirurgicales vers lesquelles on aiguille le plus fréquemment des patients, et les délais d'attente pour consulter un surspécialiste y sont les plus longs. Nous avons utilisé une méthode axée sur la population pour décrire les changements dans la main-d'œuvre en rhumatologie, le volume de patients ainsi que la variation géographique de l'offre et de l'accès aux rhumatologues, en Ontario, au Canada, entre 2000 et 2019; avec une projection des changements de l'offre d'ici à 2030. Au fil du temps, nous avons observé une plus grande féminisation de l'effectif et une augmentation de l'âge de la main-d'œuvre. Nous avons observé une grande variation régionale dans l'offre en rhumatologie. Moins de nouveaux patients sont vus chaque année, ce qui contribue probablement à l'augmentation des temps d'attente et à une réduction de l'accès aux soins. Il est nécessaire de mettre au point des stratégies et des politiques pour accroître la masse critique et pour améliorer la distribution régionale de l'offre de main-d'œuvre, et ce, afin de fournir efficacement des soins de rhumatologie et afin de soutenir la prestation de soins de santé aux patients atteints de MRM.
About the Author(s)
Jessica Widdifield, PhD Scientist, Sunnybrook Research Institute Holland Bone & Joint Program Assistant Professor, University of Toronto Institute of Health Policy, Management & Evaluation Toronto, ON Scientist, ICES Toronto, ON
Sasha Bernatsky, MD, FRCPC, PhD Rheumatologist and Scientist Research Institute of the McGill University Health Centre Associate Professor Department of Epidemiology, McGill University Montreal, QC
Janet E. Pope, MD, FRCPC, MPH Rheumatologist, St Joseph's Health Care London Professor of Medicine Epidemiology and Biostatistics Schulich School of Medicine & Dentistry, Western University London, ON
Bindee Kuriya, MD, FRCPC, SM Rheumatologist, Sinai Health System Assistant Professor Department of Medicine, University of Toronto Toronto, ON
Claire E.H. Barber, MD, FRCPC, PhD Rheumatologist, Assistant Professor University of Calgary Calgary, AB Research Scientist Arthritis Research Canada Richmond, BC
Lihi Eder, MD, PhD Rheumatologist, Clinician Scientist Women's College Research Institute Toronto, ON
Vandana Ahluwalia, MD, FRCPC Rheumatologist, William Osler Health System Brampton, ON
Vicki Ling, MSc Analyst, ICES Toronto, ON
Peter Gozdyra, MA Medical Geographer, ICES Toronto, ON
Catherine Hofstetter Patient Ambassador, Ontario
Anne Lyddiatt Patient Ambassador, Ontario
J. Michael Paterson, MSc Scientist, ICES Toronto, ON Assistant Professor Department of Family Medicine, McMaster University Hamilton, ON Assistant Professor, University of Toronto Institute of Health Policy, Management & Evaluation Toronto, ON
Carter Thorne, MD, FRCPC Rheumatologist, Southlake Regional Health Centre Newmarket, ON Assistant Professor of Medicine University of Toronto Toronto, ON
Correspondence may be directed to: Jessica Widdifield, Holland Bone and Joint Research Program, Sunnybrook Research Institute, MG 352 – 2075 Bayview Avenue, Toronto, ON M4N 3M5. She can be reached by phone at (416) 480-6100 x89436 or by e-mail at jessica.widdifield@utoronto.ca
Acknowledgment
The authors wish to thank Sue Schultz and Alex Kopp for their expertise.
References
Ahluwalia, V., S. Lineker, R. Sweezie, M.J. Bell, T. Kendzerska, J. Widdifield et al. 2020. The Effect of Triage Assessments on Identifying Inflammatory Arthritis and Reducing Rheumatology Wait Times in Ontario. The Journal of Rheumatology 47(3): 461–67. doi:10.3899/jrheum.180734.
Alberta Medical Association. 2015, December. A Physician's Guide to the Physician Compensation Committee and Individual Fee Review Process. Retrieved July 2020. <https://www.Albertadoctors.Org/physician-guide-to-pcc-and-individual-fee-review-process.Pdf>.
Al Maini, M., F. Adelowo, J. Al Saleh, Y. Al Weshahi, G.R. Burmester, M. Cutolo et al. 2015. The Global Challenges and Opportunities in the Practice of Rheumatology: White Paper by the World Forum on Rheumatic and Musculoskeletal Diseases. Clinical Rheumatology 34: 819–29. doi:10.1007/s10067-014-2841-6.
Arthritis Alliance of Canada. 2014, April. A Pan-Canadian Approach to Inflammatory Arthritis Models of Care. Retrieved July 2020. <http://www.arthritisalliance.ca/images/PDF/eng/20140430-2030-IA-MOCFINAL.pdf>.
Bae, G., M. Qiu, E. Reese, V. Nambudiri and S. Huang. 2016. Changes in Sex and Ethnic Diversity in Dermatology Residents Over Multiple Decades. JAMA Dermatology 152(1): 92–4. doi:10.1001/jamadermatol.2015.4441.
Barber, C.E.H., L. Jewett, E.M. Badley, D. Lacaille, A. Cividino, V. Ahluwalia et al. 2017. Stand Up and Be Counted: Measuring and Mapping the Rheumatology Workforce in Canada. The Journal of Rheumatology 44(2): 248–57. doi:10.3899/jrheum.160621.
Barber, C.E.H., D. Lacaille, P. Faris, D. Mosher, S. Katz, J.N. Patel, et al. 2020. Evaluating Quality of Care for Rheumatoid Arthritis for the Population of Alberta Using System-Level Performance Measures. The Journal of Rheumatology. doi:10.3899/jrheum.200420.
Barnabe, C., Y. Sun, G. Boire, C.A. Hitchon, B. Haraoui, J.C. Thorne et al. 2015. Heterogeneous Disease Trajectories Explain Variable Radiographic, Function and Quality of Life Outcomes in the Canadian Early Arthritis Cohort (Catch). PLoS One 10(8): e0135327. doi:10.1371/journal.pone.0135327.
Battafarano, D.F., M. Ditmyer, M.B. Bolster, J.D. Fitzgerald, C. Deal, A.R. Bass et al. 2018. 2015 American College of Rheumatology Workforce Study: Supply and Demand Projections of Adult Rheumatology Workforce, 2015–2030. Arthritis Care and Research (Hoboken) 70(4): 617–26. doi:10.1002/acr.23518.
Bombardier, C., G. Hawker and D. Mosher. 2011. The Impact of Arthritis in Canada: Today and Over the Next 30 Years. Retrieved July 2020. <https://www.arthritisalliance.ca/images/PDF/eng/Initiatives/20111022_2200_impact_of_arthritis.pdf>.
Brophy, J., D.A. Marshall, E.M. Badley, J.G. Hanly, H. Averns, J. Ellsworth et al. 2016. Measuring the Rheumatology Workforce in Canada: A Literature Review. The Journal of Rheumatology 43(6): 1121–9. doi:10.3899/jrheum.151174.
Chehade, M.J., T.K. Gill, D. Kopansky-Giles, L. Schuwirth, J. Karnon, P. McLiesh et al. 2016. Building Multidisciplinary Health Workforce Capacity to Support the Implementation of Integrated, People-Centred Models of Care for Musculoskeletal Health. Best Practice and Research Clinical Rheumatology 30(3): 559–84. doi:10.1016/j.berh.2016.09.005.
Campbell, J.L. 1996. The Reported Availability of General Practitioners and the Influence of Practice List Size. The British Journal of General Practice 46(409): 465–68.
Canadian Institute for Health Information (CIHI). 2012. Prescribed Drug Spending in Canada, 2012: A Focus on Public Drug Programs. Retrieved July 2020. <https://docplayer.net/9627344-Prescribed-drug-spending-in-canada-2012-a-focus-on-public-drug-programs.html>.
Canadian Institute for Health Information (CIHI). 2018, November. Prescribed Drug Spending in Canada. Retrieved July 2020. <https://www.Cihi.Ca/en/prescribed-drug-spending-in-canada>.
Canadian Post-M.D. Education Registry (CAPER). 2019. Annual Census of Post-M.D. Trainees 2018–2019. Retrieved September, 2020. <https://caper.ca/sites/default/files/pdf/annual-census/2018-19-CAPER_Census_en.pdf>.
Deal, C.L., R. Hooker, T. Harrington, N. Birnbaum, P. Hogan, E. Bouchery et al. 2007. The United States Rheumatology Workforce: Supply and Demand, 2005–2025. Arthritis and Rheumatism 56(3): 722–29. doi:10.1002/art.22437.
Dejaco, C., A. Lackner, F. Buttgereit, E.L. Matteson, M. Narath and M. Sprenger. 2016. Rheumatology Workforce Planning in Western Countries: A Systematic Literature Review. Arthritis Care and Research (Hoboken) 68(12): 1874–82. doi:10.1002/acr.22894.
Delaurier, A., S. Bernatsky, M. Baron, J. Légaré and D.E. Feldman. 2012. Wait Times for Rheumatology Consultation: Is Rheumatoid Arthritis Prioritized? Journal of Clinical Rheumatology 18(7): 341–44. doi:10.1097/RHU.0b013e31826d6408.
Eder, L., J. Widdifield, C.F. Rosen, R. Cook, K.-A. Lee, R. Alhusayen et al. 2019. Trends in the Prevalence and Incidence of Psoriasis and Psoriatic Arthritis in Ontario, Canada: A Population-Based Study. Arthritis Care and Research (Hoboken) 71(8): 1084–91. doi:10.1002/acr.23743.
Feldman, D.E., S. Bernatsky, M. Houde, M.E. Beauchamp and M. Abrahamowicz. 2013. Early Consultation with a Rheumatologist for RA: Does It Reduce Subsequent Use of Orthopaedic Surgery? Rheumatology (Oxford) 52(3): 452–59. doi:10.1093/rheumatology/kes231.
Fisher, J.M., M. Garside, K. Hunt and N. Lo. 2014. Geriatric Medicine Workforce Planning: A Giant Geriatric Problem or Has the Tide Turned? Clinical Medicine 14(2): 102–06. doi: 10.7861/clinmedicine.14-2-102.
GBD 2013 Mortality and Causes of Death Collaborators. 2015. Global, Regional, and National Age-Sex Specific All-Cause and Cause-Specific Mortality for 240 Causes of Death, 1990–2013: A Systematic Analysis for the Global Burden of Disease Study 2013. The Lancet 385: 117–71. doi:10.1016/S0140-6736(14)61682-2.
Global Burden of Disease Study 2013 Collaborators. 2015. Global, Regional, and National Incidence, Prevalence, and Years Lived with Disability for 301 Acute and Chronic Diseases and Injuries in 188 Countries, 1990-2013: A Systematic Analysis for the Global Burden of Disease Study 2013. The Lancet 86(9995): 743–800. doi:10.1016/S0140-6736(15)60692-4.
Goodman, D.C. 2004. Twenty-Year Trends in Regional Variations in the U.S. Physician Workforce. Health Affairs (Millwood) 2004: VAR90-7. doi:10.1377/hlthaff.var.90.
Gossec, L., J.S. Smolen, S. Ramiro, M. de Wit, M. Cutolo, M. Dougados et al. 2016. European League against Rheumatism (Eular) Recommendations for the Management of Psoriatic Arthritis with Pharmacological Therapies: 2015 Update. Annals of the Rheumatic Diseases 75(3): 499–510. doi:10.1136/annrheumdis-2015-208337.
Haraoui, B., W. Bensen, L. Bessette, S. Le Clercq, C. Thorne and J. Wade. 2012. Treating Rheumatoid Arthritis to Target: A Canadian Physician Survey. The Journal of Rheumatology 39(5): 949–53. doi:10.3899/jrheum.111134.
Harris, J.A., V.P. Bykerk, C.A. Hitchon, E.C. Keystone, J.C. Thorne, G. Boire et al. 2013. Determining Best Practices in Early Rheumatoid Arthritis by Comparing Differences in Treatment at Sites in the Canadian Early Arthritis Cohort. The Journal of Rheumatology 40(11): 1823–30. doi:10.3899/jrheum.121316.
Hazlewood, G.S., S.G. Barr, E. Lopatina, D.A. Marshall, T.L. Lupton, M.J. Fritzler et al. 2016. Improving Appropriate Access to Care with Central Referral and Triage in Rheumatology. Arthritis Care and Research (Hoboken) 68: 1547–53. doi:10.1002/acr.22845.
Hooker, R.S. 2008. The Extension of Rheumatology Services with Physician Assistants and Nurse Practitioners. Best Practice and Research Clinical Rheumatology 22(3): 523–33. doi:10.1016/j.berh.2007.12.006.
Hogg, W., S. Dahrouge, G. Russell, M. Tuna, R. Geneau, L. Muldoon et al. 2009. Health Promotion Activity in Primary Care: Performance of Models and Associated Factors. Open Medicine 3(3): e165–73.
Hudon, E., M.D. Beaulieu and D. Roberge. 2004. Integration of the Recommendations of the Canadian Task Force on Preventive Health Care: Obstacles Perceived by a Group of Family Physicians. Family Practice 21: 11–17. doi:10.1093/fampra/cmh104.
Isaacs, J.D. 2015. Decade in Review-Clinical Rheumatology: 10 Years of Therapeutic Advances in the Rheumatic Diseases. Nature Reviews Rheumatology 11: 628–30. doi:10.1038/nrrheum.2015.138.
Jaakkimainen, L., R. Glazier, J. Barnsley, E. Salkeld, H. Lu and K. Tu. 2014. Waiting to See the Specialist: Patient and Provider Characteristics of Wait Times from Primary to Specialty Care. BMC Family Practice 15: 16. doi:10.1186/1471-2296-15-16.
Keeling, S.O., Z. Alabdurubalnabi, A. Avina-Zubieta, S. Barr, L. Bergeron, S. Bernatsky et al. 2018. Canadian Rheumatology Association Recommendations for the Assessment and Monitoring of Systemic Lupus Erythematosus. The Journal of Rheumatology 45(10): 1426–39. doi:10.3899/jrheum.171459.
Kur, J. and B. Koehler. 2011. Rheumatologist Demographics in British Columbia: A Looming Crisis. BCMJ 53: 128–31.
Lacaille, D., A.H. Anis, D.P. Guh and J.M. Esdaile. 2005. Gaps in Care for Rheumatoid Arthritis: A Population Study. Arthritis and Rheumatism 53: 241–48. doi:10.1002/art.21077.
Liddy, C., S. Arbab-Tafti, I. Moroz and E. Keely. 2017. Primary Care Physician Referral Patterns in Ontario, Canada: A Descriptive Analysis of Self-Reported Referral Data. BMC Family Practice 18(1): 81. doi:10.1186/s12875-017-0654-9.
MacKenzie, C.R., F.G. Miller and J.J. Fins. 2005. Justice and Health Care in the Rheumatic Diseases. HSS Journal 1(1): 58–63. doi:10.1007/s11420-005-0108-0.
Martin, L. 2015. Academic Alternative Relationship Plan at the University of Calgary. CRAJ 25(3): 12–13.
Ministry of Health and Long-Term Care. 2011. Annual Report of the Office of the Auditor General of Ontario: Funding Alternatives for Family Physicians. Retrieved July 2020. <http://www.longwoods.com/blog/wp-content/uploads/2012/05/306en11.pdf>.
Monti, S., C. Montecucco, S. Bugatti and R. Caporali. 2015. Rheumatoid Arthritis Treatment: The Earlier the Better to Prevent Joint Damage. RMD Open 1: e000057. doi:10.1136/rmdopen-2015-000057.
Murray, M., M. Davies and B. Boushon. 2007. Panel Size: Answers to Physicians' Frequently Asked Questions. Family Practice Management 14(4): 44–51.
O'Donnell, S., C. Lagace, L. McRae and C. Bancej. 2011. Life with Arthritis in Canada: A Personal and Public Health Challenge. Chronic Diseases and Injuries in Canada 31(3): 135–56.
Pearse, W.H., W.H. Haffner and A. Primack. 2001. Effect of Gender on the Obstetric-Gynecologic Work Force. Obstetrics & Gynecology 97(5 Pt. 1): 794–7. doi: 10.1016/s0029-7844(01)01191-7.
Pease, C., J.E. Pope, C. Thorne, B.P. Haraoui, D. Truong, C. Bombardier et al. 2010. Canadian Variation by Province in Rheumatoid Arthritis Initiating Anti-Tumor Necrosis Factor Therapy: Results from the Optimization of Adalimumab Trial. The Journal of Rheumatology 37(12): 2469–7. doi:10.3899/jrheum.091447.
Pelley, F., A. Danoff, D.S. Cooper and C. Becker. 2016. Female Physicians and the Future of Endocrinology. The Journal of Clinical Endocrinology and Metabolism 101(1): 16–22. doi:10.1210/jc.2015-3436.
Raffoul, M., M. Moore, D. Kamerow and A. Bazemore. 2016. A Primary Care Panel Size of 2500 Is Neither Accurate nor Reasonable. Journal of the American Board of Family Medicine 29(4): 496–99. doi:10.3122/jabfm.2016.04.150317.
Rom, M., J.J. Fins and C.R. Mackenzie. 2007. Articulating a Justice Ethic for Rheumatology: A Critical Analysis of Disparities in Rheumatic Diseases. Arthritis and Rheumatism 57(8): 1343–45. doi:10.1002/art.23110.
Roubille, C., V. Richer, T. Starnino, C. McCourt, A. McFarlane, P. Fleming et al. 2015. Evidence-Based Recommendations for the Management of Comorbidities in Rheumatoid Arthritis, Psoriasis, and Psoriatic Arthritis: Expert Opinion of the Canadian Dermatology-Rheumatology Comorbidity Initiative. The Journal of Rheumatology 42(10): 1767–80. doi:10.3899/jrheum.141112.
Russell, G.M., S. Dahrouge, W. Hogg, R. Geneau, L. Muldoon and M. Tuna. 2009. Managing Chronic Disease in Ontario Primary Care: The Impact of Organizational Factors. Annals of Family Medicine 7(4): 309–18. doi:10.1370/afm.982.
Shadd, J., B.L. Ryan, H. Maddocks and A. Thind. 2011. Patterns of Referral in a Canadian Primary Care Electronic Health Record Database: Retrospective Cross-Sectional Analysis. Informatics in Primary Care 19(4): 217–23. doi:10.14236/jhi.v19i4.816.
Smolen, J.S., R. Landewé, J. Bijlsma, G. Burmester, K. Chatzidionysiou, M. Dougados et al. 2017. Eular Recommendations for the Management of Rheumatoid Arthritis with Synthetic and Biological Disease-Modifying Antirheumatic Drugs: 2016 Update. Annals of the Rheumatic Diseases 76(6): 960–77. doi:10.1136/annrheumdis-2016-210715.
Solomon, D.H., A. Bitton, L. Fraenkel, E. Brown, P. Tsao and J.N. Katz. 2014. Roles of Nurse Practitioners and Physician Assistants in Rheumatology Practices in the US. Arthritis Care and Research (Hoboken) 66(7): 1108–13. doi:10.1002/acr.22255.
Solomon, D.H., L. Fraenkel, B. Lu, E. Brown, P. Tsao, E. Losina et al. 2015. Comparison of Care Provided in Practices with Nurse Practitioners and Physician Assistants versus Subspecialist Physicians Only: A Cohort Study of Rheumatoid Arthritis. Arthritis Care and Research (Hoboken) 67(12): 1664–70. doi:10.1002/acr.22643.
Spector, N.D., W. Cull, S.R. Daniels, J. Gilhooly, J. Hall, I.B. Horn I et al. 2014. Gender and Generational Influences on the Pediatric Workforce and Practice. Pediatrics 133(6): 1112–21.
Stewart, J.C. and M.M. Teo. 2014. Rheumatology Perspectives: On Working with a Nurse. CRAJ 24(3): 15.
The College of Family Physicians of Canada, CMA, and Royal College of Physicians and Surgeons of Canada. 2019. National Physician Survey: 2014 National Results by Sex and Age Group – All Results. Retrieved July 2020. <http://nationalphysiciansurvey.ca/>.
The Royal College of Physicians and Surgeons of Canada. 2009. NPS Primer, June, 2009: Work Hours. Authors.
van Nies, J.A., A. Krabben, J.W. Schoones, T.W. Huizinga, M. Kloppenburg and A.H. van der Helm-van Mil. 2014. What Is the Evidence for the Presence of a Therapeutic Window of Opportunity in Rheumatoid Arthritis? A Systematic Literature Review. Annals of the Rheumatic Diseases 73(5): 861–70. doi:10.1136/annrheumdis-2012-203130.
Widdifield, J., J.M. Paterson, S. Bernatsky, K. Tu, J.C. Thorne, V. Ahluwalia et al. 2013. The Rising Burden of Rheumatoid Arthritis Surpasses Rheumatology Supply in Ontario. Canadian Journal of Public Health 104: e450–55. doi:10.17269/cjph.104.4115.
Widdifield, J., C.S. Moura, Y. Wang, M. Abrahamowicz, J.M. Paterson, A. Huang et al. 2016a. The Long-Term Effect of Early Intensive Treatment of Seniors with Rheumatoid Arthritis: A Comparison of 2 Population-Based Cohort Studies on Time to Joint Replacement Surgery. The Journal of Rheumatology 43(5): 861–68. doi:10.3899/jrheum.151156.
Widdifield, J., S. Bernatsky, J.C. Thorne, C. Bombardier, R.L. Jaakkimainen, L. Wing et al. 2016b. Wait Times to Rheumatology Care for Patients with Rheumatic Diseases: A Data Linkage Study of Primary Care Electronic Medical Records and Administrative Data. CMAJ Open 4(2): E205–12. doi:10.9778/cmajo.20150116.
Widdifield, J., K. Tu, J.C. Thorne, C. Bombardier, J.M. Paterson, R.L. Jaakkimainen, et al. 2017a. Patterns of Care among Patients Referred to Rheumatologists in Ontario, Canada. Arthritis Care and Research (Hoboken) 69(1): 104–14. doi:10.1002/acr.22910..
Widdifield, J., M. Paterson, A. Huang, M. Abrahamowicz and S. Bernatsky. 2017b. Early Treatment with Methotrexate Improves All-Cause and Cardiovascular Survival among an Inception Cohort of Seniors with Rheumatoid Arthritis. Annals of the Rheumatic Diseases 76(2): 749.
Widdifield, J., S. Bernatsky, J.E. Pope, V. Ahluwalia, C.E.H. Barber, L. Eder L et al. 2020. Encounters with Rheumatologists in a Publicly Funded Canadian Healthcare System: A Population-Based Study. The Journal of Rheumatology 47(3): 468–76. doi:10.3899/jrheum.190034.
Wilkin, D. and D.H. Metcalfe. 1984. List Size and Patient Contact in General Medical Practice. British Medical Journal (Clin Res Ed) 289(6457): 1501–505. doi:10.1136/bmj.289.6457.1501.
Yazdany, J. and C.H. MacLean. 2008. Quality of Care in the Rheumatic Diseases: Current Status and Future Directions. Current Opinion in Rheumatology 20(2): 159–66. doi:10.1097/BOR.0b013e3282f50ec4.
Yazdany, J., L. Trupin, G. Schmajuk, P.P. Katz and E.H. Yelin. 2014. Quality of Care in Systemic Lupus Erythematosus: The Association between Process and Outcome Measures in the Lupus Outcomes Study. BMJ Quality and Safety 23(8): 659–66. doi:10.1136/bmjqs-2013-002494.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed