Healthcare Policy
Non-Official Language Concordance in Urban Canadian Medical Practice: Implications for Care during the COVID-19 Pandemic
Abstract
Language barriers can reduce access to medical and virtual care. Although the topic of healthcare professionals and linguistic minorities has been studied in Canada, it has mainly been done for official languages (i.e., English and French). Non-official languages (NOLs) have not been explored previously in the healthcare system at the pan-Canadian level. The objective of this study is to determine to what extent NOLs spoken by physicians relate to those of Canadian ethnic groups and are an enabler of access to care. Using data from the Canadian Institute for Health Information (CIHI) and Statistics Canada, we found an imbalance in the physician-to-population NOL ratios in Montreal and, to a lesser extent, Vancouver.
Introduction and Background
Poor language proficiency and inadequate communication are potential barriers to access to medical care. International studies note that miscommunications in the healthcare sector can sometimes lead to life-threatening results (Meuter et al. 2015). The COVID-19 pandemic has made access to medical care more problematic and may compound the existing language and communication issues, given the disproportionate toll of COVID-19 on immigrant populations. Although immigrants, refugees and other newcomers make up just over 25% of the Ontario population, they accounted for 43.5% of all COVID-19 cases (Guttmann et al. 2020).
Physician service imbalances based on language ability have long been considered in the context of official language minorities, mostly francophones, in Canada (Bowen 2000; Federal, Provincial and Territorial ACPH 1999; Lepage and Lavoie 2017; Ngwakongnwi et al. 2012; Timony et al. 2016). Research on language barriers and Indigenous access to healthcare is also growing (Office of the Languages Commissioner of Nunavut 2015; Webster 2018).
Poor language facility and thus poor physician–patient communication can represent a non-trivial barrier to access to high-quality care (Bowen 2001). Recent immigrants lack information about health systems, have different cultural expectations or experience discrimination as visible minorities. This analysis focuses on proficiency in either official language for doctors and patients, particularly the one dominant provincially. According to the 2016 census, about 23% of the population has a mother tongue that is a non-official language (NOL), slightly higher than the 21.4% of the population with French as their official mother tongue.
Preliminary data from Santé Montreal (2020) and Toronto's (DeClerq 2020) public health offices, among others, have shown COVID-19 incidence and mortality rates to be higher in ethnic communities where a large number of residents speak an NOL. Guttmann et al. (2020) noted lower rates of COVID-19 testing for recent immigrants and refugees in Ontario, with a lack of English or French language ability associated with lower testing. Moreover, those who ended up being tested had higher positivity rates. Data from 10 US cities show that the impact of COVID-19 is about three to nine times higher in poor and non-White counties (Adhikari et al. 2020). Assuming that being non-White is a proxy for NOL proficiency, the impact of COVID-19 is therefore associated with poverty and poor official language ability.
As a result of the COVID-19 pandemic, all jurisdictions have promoted and expanded virtual care (VC) measures to enhance the safety and efficacy of the medical workforce. They have created new/temporary fee codes and/or repurposed existing fee codes for telephone or video consultation services. Details are provided by CIHI (2020a), which monitored and compiled the changes made to jurisdictional fee schedules and billing codes. While VC has many benefits, it can be challenging for ethnic minorities, who are more likely to be NOL speakers and might barely speak/understand English or French.
COVID-19 can compound the existing structural and societal inequalities in health status among immigrant or ethnic minority populations (van Dorn et al. 2020). With more VC, communication problems due to lack of language facility can be compounded by absence of body language (in the case of telephone consultation) or poorly interpreted facial signals and body language, as has been noted in the case of video conferencing (Jiang 2020).
Because VC can be delivered across a wide region, it can quantitatively increase access to care during a pandemic, but quality and equity aspects should also be considered. VC is less effective if the people most impacted by the pandemic have limited proficiency in English or French and lack access to physicians with NOL facility. A better understanding of the situation can inform whether additional measures are required to reduce health disparities due to linguistic/cultural barriers.
Objective, Research Question and Contribution to the Literature
This research can inform medical and health system management response, decision making and planning within and across Canadian jurisdictions. The question addressed is as follows: To what extent do foreign languages spoken by physicians in Canadian urban areas relate to those of ethnic minorities? Given the current Canadian physician distribution, we expect some NOL discordance across jurisdictions. If a mismatch is indeed found, this analysis could prompt decision makers to provide incentives for improving physician access via adjustments in language and communication services. This can improve the uptake and efficiency of virtual consultations, which is becoming more crucial for the Canadian healthcare system in the context of the pandemic.
Ethnicity and utilization of healthcare providers have been studied in the context of single and multiple ethnic groups. Wang et al. (2008) found preference among mainland Chinese survey respondents for Chinese-speaking family physicians in the Toronto Census Metropolitan Area (CMA). De Mossaic and Bowen (2019) explored the experience of minority francophones living in four Canadian provinces; they found that language barriers contribute to poorer patient assessment, misdiagnosis, delayed treatment and incomplete understanding of patient condition. McKeary and Newbold (2010) found that refugees or recent immigrants speaking neither English nor French faced problems accessing primary care and were more likely to report problems in accessing specialists. Waibel et al. (2018) studied multiple ethnic groups (adults who spoke English, French, Mandarin, Cantonese or Punjabi) and multiple geographic areas (British Columbia, Manitoba and Quebec), focusing on the impact of language barriers on healthcare experiences. While the research examining the effects of language on healthcare patterns and use is abundant (Lepage and Lavoie 2017; Ngwakongnwi et al. 2012; Rawal et al. 2019; Timony et al. 2016), only one study, to our knowledge, has examined the capacity of medical care providers to offer services in the most common NOLs in Canada. Sears et al. (2013) looked at patient–physician language discordance for the top five NOLs (Chinese, Italian, Punjabi, Portuguese and Spanish) in each census division (CD) of Ontario. They found that there were at least five CDs with a non-English/non-French population speaking a NOL without any primary care physician proficient in that NOL.
We pair self-reported physician proficiency in NOL with that of the population to illuminate physician supply and demand matches for most Canadian provinces. We contribute by examining the indicators of both the capacity of medical staff to provide services in a foreign language and the demand of the population for these services in the major CMAs, using more NOLs and updated data.
Method
Scott's Medical Database (SMDB) 2018 data from CIHI (2020b) are used to track the top 10 NOLs spoken by family and specialist physicians in the seven largest CMAs. Physicians are defined as anyone with an MD degree and a valid postal code, which includes family physicians as well as specialists. Self-reported professional proficiency in other languages (other than the one used for correspondence) is one of the variables collected, and these data are publicly accessible by making a custom data request to CIHI. Each physician with proficiency in one or more NOLs is assigned to a CMA (with a population of 100,000 inhabitants or more) based on their mailing address in SMDB. The mailing address typically reflects the geographic region where physicians practise, providing a reasonable indication of the access to medical care available to the region's population. Data for any given region with a count of less than five physicians are suppressed. Each physician with NOL proficiency was also assigned to an urban non-metropolitan area (with a minimum of 10,000 inhabitants) and a rural/remote area (with less than 10,000 inhabitants). However, the issue of low occurrence in these areas prevented doing the analysis at these levels.
Data from the 2016 Census of Statistics Canada (2017) were used to track the number of persons reporting various NOLs (persons with a NOL as mother tongue, which might also be the language spoken most often at home) by CMA.1 The top 10 NOLs spoken in the population and reported by Statistics Canada are as follows: Chinese (including Mandarin and Cantonese), Punjabi, Tagalog (Filipino), Spanish, Arabic, Italian, German, Urdu, Portuguese and Persian (Farsi). These represent 62% of the NOLs spoken in Canada, and 14% of the total population of Canada speaks one or more of these NOLs. About 67 Aboriginal languages were reported in the 2016 census, but people reporting an Aboriginal language as their mother tongue represent 0.6% of the Canadian population. Even the most common ones in this category – Cree, Inuktitut and Ojibway – suffer from the low occurrence issue for physicians with NOL proficiency. Only four physicians reported speaking one of the three most common Aboriginal languages at the national level. Therefore, physicians with Aboriginal language proficiency could not be included in this analysis.
We assume that patients wishing to receive medical services in their mother tongue are willing to travel or receive VC within their CMA – known as a "container-based" approach (Langford et al. 2016). This approach computes a supply-to-demand ratio within the boundaries of a fixed geographic space with no interaction across boundaries. Other approaches to understanding primary care utilization patterns include the "distance-based" or "floating catchment area" (FCA) approach (Guterman et al. 2011; Langford et al. 2016; Luo and Wang 2003; Stukel et al. 2013). For other patient attribution methods, see the studies by McCoy et al. (2018) and Peckham et al. (2018). The nature of the studied characteristic (accessibility based on NOL) does not lend itself to the FCA method in all the CMAs because low occurrence hampers the analysis in many cases. Hence, we use the "container-based" method, as the boundaries coincide with the CMA and are large and geographically inclusive enough that cross-CMA interaction is unlikely to happen, thus supporting the choice of this method. It is commonly believed that virtual or distance care could potentially expand access to services because patients are not limited to the physicians in their immediate vicinity. However, adults seeking routine care have a preference for services within a 30-minute drive, making the CMA a good geographic study choice (Yen 2013).
These CMAs must have a critical mass of physicians speaking one of the top 10 NOLs. Critical mass was defined as more than 200 physicians for each CMA to ensure adequate sample size. Seven CMAs fit this criterion: Montreal, Ottawa, Toronto, Winnipeg, Calgary, Edmonton and Vancouver. The percentage of physicians speaking a NOL are compared to the percentage of the population speaking that language. Physician–population ratios by NOL and CMA are also provided, with imbalances based on the observed gaps.
The physician-to-population NOL ratio is an important indicator and can be defined as the number of physicians who speak a NOL in a given area divided by the number of people who speak the same NOL in that area and multiplied by 1,000. A very large gap (defined as ±50% of the total physician–population ratio) can indicate a perceived surplus or deficit.
Results
Counts of NOL speakers among physicians
The top 10 NOLs reported by physicians in SMDB are Chinese, Arabic, Spanish, Punjabi, Urdu, Afrikaans, German, Hindi, Italian and Farsi/Persian. They also correspond to the top 10 NOLs spoken by the population, except for Afrikaans and Farsi/Persian, which are replaced by Tagalog (Filipino) and Portuguese. Table 1 provides the number of physicians speaking one of these languages in the seven largest CMAs in Canada. Percentages are reported in brackets.
The top 10 NOLs spoken by physicians largely vary among CMAs. For example, Spanish was the most common NOL spoken by physicians in Montreal and Ottawa (at about 2.3%), while it was Chinese in Toronto and Vancouver (at about 5.0%), Arabic in Edmonton (4.0%) and Urdu in Calgary (3.3%).
Counts of NOL speakers among the general population and concordance with physicians
In the general population, the variation in NOL speakers among the CMAs is low. Chinese is the most common NOL spoken in all the seven largest CMAs (5.4%), except in Montreal and Winnipeg, where the most common are Spanish and Punjabi, respectively. They were spoken by 2% of the population in these CMAs (Table 2).
Comparing the percentages in Tables 1 and 2 can inform us on the level of concordance of NOL speakers among physicians and the general population. It varies with the CMAs. The proportion of NOL-speaking physicians outweighed that of the NOL-speaking population for most CMAs, which means the NOL capacity is generally adequate. However, Montreal had the lowest proportion of Arabic-speaking physicians (0.2%), but it ranks the second-highest in the proportion of its Arabic-speaking population (1.9%). Similarly, the proportion of Chinese- and Punjabi-speaking physicians in Vancouver is much lower than that of the population itself.
| Table 1. Number and percentage (in brackets) of physicians speaking one of the top 10 NOLs in the seven largest Canadian CMAs (both sexes) in 2018 | ||||||||
| Top 10 NOLs | Montreal | Ottawa | Toronto | Winnipeg | Calgary | Edmonton | Vancouver | Total seven CMAs2 |
| N(%) | 11,032 (12.3) | 4,336 (4.8) | 15,596 (17.4) | 2,335 (2.6) | 4,539 (5.0) | 4,116 (4.6) | 6,920 (7.7) | 48,874 (54.4) |
| Afrikaans | 0 (0.0) | 8 (0.2) | 35 (0.2) | 12 (0.5) | 92 (2.0) | 60 (1.5) | 65 (0.9) | 272 (0.6) |
| Arabic | 26 (0.2) | 57 (1.3) | 393 (2.5) | 42 (1.8) | 80 (1.8) | 166 (4.0) | 36 (0.5) | 800 (1.6) |
| Chinese1 | 13 (0.1) | 46 (1.1) | 730 (4.7) | 25 (1.1) | 126 (2.8) | 141 (3.4) | 349 (5.0) | 1,430 (2.9) |
| German | 48 (0.4) | 44 (1.0) | 118 (0.8) | 29 (1.2) | 53 (1.2) | 55 (1.3) | 74 (1.1) | 421 (0.9) |
| Hindi | 9 (0.1) | 27 (0.6) | 301 (1.9) | 22 (0.9) | 100 (2.2) | 76 (1.8) | 68 (1.0) | 603 (1.2) |
| Italian | 103 (0.9) | 36 (0.8) | 222 (1.4) | 5 (0.2) | 19 (0.4) | 23 (0.6) | 22 (0.3) | 430 (0.9) |
| Persian/Farsi | 7 (0.1) | 15 (0.3) | 213 (1.4) | 13 (0.6) | 40 (0.9) | 27 (0.7) | 69 (1.0) | 384 (0.8) |
| Punjabi | 4 (0.0) | 26 (0.6) | 315 (2.0) | 29 (1.2) | 116 (2.6) | 86 (2.1) | 142 (2.1) | 718 (1.5) |
| Spanish | 259 (2.3) | 105 (2.4) | 330 (2.1) | 40 (1.7) | 87 (1.9) | 64 (1.6) | 88 (1.3)1 | 973 (2.0) |
| Urdu | 7 (0.1) | 31 (0.7) | 453 (2.9) | 30 (1.3) | 149 (3.3) | 117 (2.8) | 74 (1.1) | 861 (1.8) |
| Total 10 NOLs2 | 476 (4.3) | 395 (9.1) | 3,110 (19.9) | 247 (10.5) | 862 (19.0) | 815 (19.8) | 987 (14.3) | 6,892 (14.1) |
| 1. Chinese includes Mandarin and Cantonese. 2 Numbers or percentages may not exactly add up to total 10 NOLs and total seven CMAs due to rounding Source: CIHI 2020b. |
||||||||
| Table 2. Number (1,000) and percentage (in brackets) of people speaking one of the top 10 NOLs in the seven largest Canadian CMAs (both sexes) in 2016 | ||||||||
| Top 10 NOLs | Montreal | Ottawa | Toronto | Winnipeg | Calgary | Edmonton | Vancouver | Total seven CMAs2 |
| N (%) | 3,784.2 (10.8) | 921.6 (2.6) | 5,321.9 (15.1) | 647.1 (1.8) | 1,294.3 (3.7) | 1,235.3 (3.5) | 2,252.5 (6.4) | 15,456.9 (44.0) |
| Afrikaans | 0.0 (0.0) | 0.0 (0.0) | 0.3 (0.0) | 0.0 (0.0) | 0.5 (0.0) | 0.3 (0.0) | 0.5 (0.0) | 1.6 (0.0) |
| Arabic | 73.0 (1.9) | 19.1 (2.1) | 45.0 (0.8) | 2.8 (0.4) | 11.0 (0.9) | 10.6 (0.9) | 8.7 (0.4) | 170.2 (1.1) |
| Chinese1 | 56.5 (1.5) | 20.5 (2.2) | 380.6 (7.2) | 11.7 (1.8) | 46.0 (3.6) | 31.8 (2.6) | 283.9 (12.6) | 830.9 (5.4) |
| German | 1.6 (0.0) | 0.6 (0.1) | 3.6 (0.1) | 1.5 (0.2) | 1.5 (0.1) | 2.3 (0.2) | 2.9 (0.1) | 14.0 (0.1) |
| Hindi | 1.5 (0.0) | 1.3 (0.1) | 24.0 (0.5) | 1.2 (0.2) | 4.1 (0.3) | 5.1 (0.4) | 11.2 (0.5) | 48.4 (0.3) |
| Italian | 32.4 (0.9) | 2.5 (0.3) | 51.9 (1.0) | 1.0 (0.1) | 1.3 (0.1) | 1.4 (0.1) | 4.0 (0.2) | 94.3 (0.6) |
| Persian/Farsi | 18.3 (0.5) | 4.1 (0.4) | 67.3 (1.3) | 1.3 (0.2) | 6.5 (0.5) | 3.2 (0.3) | 27.4 (1.2) | 128.0 (0.8) |
| Punjabi | 8.8 (0.2) | 2.2 (0.2) | 116.0 (2.2) | 13.2 (2.0) | 29.1 (2.2) | 20.7 (1.7) | 104.9 (4.7) | 294.9 (1.9) |
| Spanish | 76.7 (2.0) | 6.1 (0.7) | 70.4 (1.3) | 3.3 (0.5) | 17.5 (1.4) | 10.9 (0.9) | 18.3 (0.8) | 203.2 (1.3) |
| Urdu | 7.1 (0.2) | 2.2 (0.2) | 78.1 (1.5) | 1.7 (0.3) | 11.1 (0.9) | 5.1 (0.4) | 5.2 (0.2) | 110.4 (0.7) |
| Total 10 NOLs22 | 275.8 (7.3) | 58.7 (6.4) | 837.1 (15.7) | 37.7 (5.8) | 128.6 (9.9) | 91.3 (5.4) | 466.9 (20.7) | 1,896.0 (12.3) |
| 1. Chinese includes Mandarin and Cantonese. 2 Numbers or percentages may not exactly add up to total 10 NOLs and total seven CMAs due to rounding Source: Statistics Canada 2017. |
||||||||
Physician-to-population NOL ratio
The more concise indicator physician-to-population NOL ratio is presented in Table 3. Note that Afrikaans is omitted from now on due to the virtually insignificant number of people speaking this NOL in the population.
| Table 3. Physician-to-population NOL ratio (per 1,000) for the top nine NOLs in the seven largest CMAs | ||||||||
| Top nine NOLs | Montreal | Ottawa | Toronto | Winnipeg | Calgary | Edmonton | Vancouver | Total seven CMAs |
| Arabic | 0.4 | 3.0 | 8.7 | 14.8 | 7.3 | 15.7 | 4.1 | 4.7 |
| Chinese1 | 0.2 | 2.2 | 1.9 | 2.1 | 2.7 | 4.4 | 1.2 | 1.7 |
| German | 30.3 | 70.4 | 32.9 | 19.7 | 34.4 | 23.8 | 25.6 | 30.0 |
| Hindi | 6.1 | 20.9 | 12.5 | 18.3 | 24.2 | 14.9 | 6.1 | 12.5 |
| Italian | 3.2 | 14.3 | 4.3 | 5.2 | 15.0 | 16.4 | 5.6 | 4.6 |
| Persian/Farsi | 0.4 | 3.7 | 3.2 | 10.4 | 6.2 | 8.4 | 2.5 | 3.0 |
| Punjabi | 0.5 | 11.8 | 2.7 | 2.2 | 4.0 | 4.2 | 1.4 | 2.4 |
| Spanish | 3.4 | 17.2 | 4.7 | 12.1 | 5.0 | 5.9 | 4.8 | 4.8 |
| Urdu | 1.0 | 14.0 | 5.8 | 17.7 | 13.5 | 22.9 | 14.3 | 7.8 |
| Total (Top NOL) | 1.7 | 6.7 | 3.7 | 6.6 | 6.7 | 8.9 | 2.1 | 3.6 |
| Total (Population) | 2.7 | 3.8 | 2.6 | 3.0 | 3.3 | 3.1 | 2.8 | 2.8 |
| 1. Chinese includes Mandarin and Cantonese. Source: Authors' calculations using data from CIHI (2020b) and Statistics Canada (2017). |
||||||||
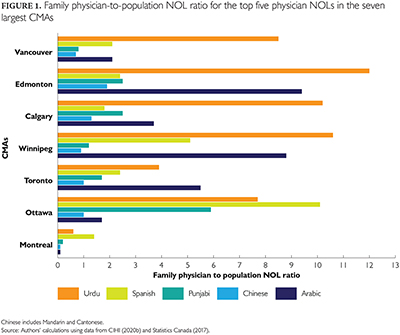
The general physician-to-population ratio varies between 2.6 and 3.8 among the seven CMAs (last row), suggesting that for most languages and CMAs, the physician-to-population NOL ratio compares favourably to that of the general population. However, this has not been the case for Montreal and Vancouver. In Montreal, the physician-to-population NOL ratio is much lower than that of the general population for Arabic, Chinese, Persian, Punjabi and Urdu. In the case of Vancouver, this indicator is lower only for Chinese and Punjabi. Otherwise, these ratios are not perceived as a constraint or are even generally higher than that of the population. Because primary care is a critical and voluminous component of the medical services provided by family physicians, the case for this specialty should be considered specifically. We have chosen to do so in Figure 1 for the top five physician NOLs.
Based on the general family physician-to-population ratio among the seven CMAs, which ranges from 1.2 to 2.1, we can also imply that for most languages and CMAs, the family physician-to-population NOL ratio compares favourably to that of the general population. For specific languages and CMAs, the pattern is about the same as that for physicians in general.
General Discussion, Policy Implications and Limitations
General discussion
For CMAs such as Montreal and Vancouver, the physician-to-population NOL ratio is lower than that of the general population for Chinese and Punjabi. On the other hand, this indicator is higher for Edmonton. Where the physician-to-population NOL ratio is much lower than that of the general population, there may be a larger impact on access to health services and health status, with a greater reliance on VC in the wake of COVID-19. While access concerns could be mitigated with increased physician workloads in affected areas, such an approach can come with lifestyle and equity issues with respect to workload.
The impact of this imbalance could be all the more important, given that among these communities, some people speak neither English nor French (the two official languages in Canada), which is more likely so for women. The percentage of people not speaking either Canadian official language is higher in Vancouver and Toronto (5.6% and 4.4%, respectively) and lower in Montreal, Ottawa, Winnipeg and Edmonton (Statistics Canada 2017). This makes the need to address the issue somewhat less critical in the latter cities. Also, there is a consistently higher proportion of women than men who do not speak any of the two official languages (for example, 6.4% vs 4.7% in Vancouver). Based on the principles of equity, diversity and inclusion, addressing this issue specifically in the case of Vancouver and Toronto would also reduce gender and ethnic imbalance.2
Policy implications
Traditionally, physicians are self-regulated, with a high level of professional autonomy. Solutions for access issues due to poor language proficiency and poor communication need to reflect this reality. In addition, ascertaining an ideal physician-to-population NOL ratio and using it as a policy target is a challenging exercise for improving access for NOL populations. For example, in Canada, the urban and rural physician-to-population ratios were 2.6 and 1.1, respectively (Ariste 2018), which means the rural ratio represents about 40% of the urban.3 A physician-to-population NOL ratio that represents the same as that of the rural population seems "reasonable" as an initial measurement benchmark. This target could be used to provide incentives to attract physicians in CMAs or regions with a deficiency. While rural areas are generally recognized as underserviced, we want to be conservative in the case of NOL and still choose them as a policy benchmark target for accessible services. Approaches used to remedy rural and remote service deficiencies may apply here.
Having provincial health ministries establish a special incentive payment to physicians agreeing to provide services in a certain NOL via VC might be helpful, especially when it comes to specialists. It might take the form of additional fee codes to be used when seeing NOL patients within a given census division. The exact form would of course need to be developed in consultation with the physician community. Provincial health ministries may wish to work with the federal government to secure additional funding for such an initiative. Furthermore, another way of adding to the stock of physicians with NOL proficiency is encouraging NOL-speaking international medical graduates (IMGs) who independently desire to immigrate to Canada to settle in areas where NOL services are needed. However, there is no need to set a NOL module as part of the medical school training as it is not realistic to expect medical students to acquire enough proficiency in a new language to be comfortable enough to deliver services in that language. Moreover, the current diversity of available physicians already provides a suitable stock of NOL capacity. The issue is the distribution and availability of that capacity to specific populations and that can be addressed with the aforementioned incentive payments. It might also be possible to recruit medical students with NOL proficiency in placement drives and assign them in regions where there is a need. Evidence suggests that rural exposure during medical training can improve the recruitment and retention of physician services in underserviced areas, such as remote rural areas, though challenges remain (Bosco and Onandson 2016; Holst 2020).
Another option might be to extend and improve interpreter services for NOL populations. For example, the Winnipeg Regional Health Authority employs trained health interpreters, who provide face-to-face and telephone interpreter services in 32 and 200 languages, respectively (WRHA n.d.). Additionally, there are commercial services that provide telephone translation in multiple languages (https://www.alllanguages.com/; Provincial Health Services Authority 2021).
Limitations
Our inability to report on other communities is a limitation. Still, it is not a major one because CMAs are the home for more than 90% of newcomers in Canada since the early 1990s (Statistics Canada 2015), and some of these newcomers are likely to be NOL speakers. The variable on professional proficiency in NOLs is self-reported by physicians. Yet, substantial data quality checks have been implemented, and the data for the past few years have been deemed fit for use. While the proportion of IMGs in Canada in 2018 was 26.4%, the percent of physicians who reported having proficiency in one or more NOL was 17%, which is a majority (about two thirds), as one would expect. Also, the number of physicians who reported having proficiency in a NOL in SMDB is at least on par with that for provinces with administrative data on publicly available NOL as reported by College of Physicians and Surgeons of Ontario (CPSO 2019) and the College of Physicians and Surgeons of British Columbia (CPSBC 2021).
Besides, SMDB groups physicians neither by their place of residence nor location of practice but based on the place they receive their mail (a valid mailing address). This does not represent a serious limitation for physicians practising in urban areas, as they typically have a mailing address that is close (or corresponds) to their workplace. Finally, data on languages spoken at the population level cannot account for people who are multilingual or for the level of proficiency in the official language spoken. That is beyond this study's scope.
Conclusion
The data suggest higher diversity and frequency of NOLs spoken among physicians than the general population, especially for European languages such as Spanish, German and Italian. NOL discrepancy is most relevant when the percentage of NOL-speaking physicians is much lower than that of the general population, as is the case in Vancouver and Montreal for languages such as Chinese (Mandarin and Cantonese), Punjabi and Arabic. Addressing these discrepancies and their potential impact on access to healthcare and services is an important issue. Potential solutions include targeted incentives to physicians and recent medical graduates as well as improvement in interpreter services.
Concordance des langues non officielles dans la pratique médicale en milieu urbain au Canada : implications pour les soins pendant la pandémie de COVID-19
Résumé
Les barrières linguistiques peuvent réduire l'accès aux soins médicaux en personne ou virtuels. Bien que la question des professionnels de la santé et des minorités linguistiques ait été étudiée au Canada, cela concernaient principalement les langues officielles (anglais et français). La question des langues non officielles (LNO) n'a pas été explorée dans le système de santé au niveau pancanadien. L'objectif de cette étude est de déterminer dans quelle mesure les LNO parlées par les médecins concordent avec celles des groupes ethniques au Canada et permettent de faciliter l'accès aux soins. À l'aide des données de l'Institut canadien d'information sur la santé et de Statistique Canada, nous observons un déséquilibre dans le rapport des LNO entre les médecins et la population à Montréal et, dans une moindre mesure, à Vancouver.
About the Author(s)
Ruolz Ariste, PhD, Adjunct Professor, Department of Operations and Decision Systems, Laval University, Québec, QC
Livio di Matteo, PhD, Professor, Department of Economics, Lakehead University, Thunder Bay, ON
Correspondence may be directed to: Ruolz Ariste, Adjunct Professor, Department of Operations and Decision Systems, Laval University, Pavillon Palasis-Prince 2325, rue de la Terrasse, Québec, QC G1V 0A6. He can be reached by phone at 418-656-2098 and by e-mail at ruolz.ariste@fsa.ulaval.ca
Acknowledgment
The authors would like to thank Deborah McCartney, Hetal Dave and Chardé Morgan for their work during the data processing and request that supported the development of this analysis. However, the views expressed in this document are those of the authors and do not represent those of any institution or other individual.
References
Adhikari, S., N.P. Pantaleo, J.M. Feldman, O. Ogedegbe, L. Thorpe and A.B. Troxel. 2020. Assessment of Community-Level Disparities in Coronavirus Disease 2019 (COVID-19) Infections and Deaths in Large US Metropolitan Areas. JAMA Network Open 3(7): e2016938. doi:10.1001/jamanetworkopen.2020.16938.
Ariste, R. 2018. Availability of Health Workforce in Urban and Rural Areas in Relation to Canadian Seniors. The International Journal Health Planning and Management 34(2): 510–20. doi:10.1002/hpm.2712.
Bosco, C. and I. Onandson. 2016, January. Review of Family Medicine within Rural and Remote Canada: Education, Practice, and Policy. Retrieved June 27, 2020. <https://portal.cfpc.ca/resourcesdocs/uploadedFiles/Publications/News_Releases/News_Items/ARFM_BackgroundPaper_Eng_WEB_FINAL.pdf>.
Bowen, S. 2000, September. Certain Circumstances Issues in Equity and Responsiveness in Access to Health Care in Canada: Part I Equity in Access to Health Care. Government of Canada. Retrieved April 11, 2020. <https://www.canada.ca/en/health-canada/services/health-care-system/reports-publications/health-care-accessibility/certain-circumstances-issues-equity-responsiveness.html#part1tc1>.
Bowen, S. 2001, November. Language Barriers in Access to Health Care. Government of Canada. Retrieved April 11, 2020. <https://www.canada.ca/en/health-canada/services/health-care-system/reports-publications/health-care-accessibility/language-barriers.html>.
Canadian Institute for Health Information (CIHI). 2020a. Physician Billing Codes in Response to COVID-19. Retrieved September 26, 2020. <https://www.cihi.ca/en/physician-billing-codes-in-response-to-COVID-19>.
Canadian Institute for Health Information (CIHI). 2020b. Supply, Distribution and Migration of Physicians in Canada, 2019: Methodology Notes. Retrieved August 28, 2020. <https://www.cihi.ca/sites/default/files/document/supply-distribution-migration-of-physicians-in-canada-2019-methodology-notes-en.pdf>.
College of Physicians and Surgeons of British Columbia (CPSBC). 2021. Registrant Directory. Retrieved August 29, 2020. <https://www.cpsbc.ca/registrant_search>.
College of Physicians and Surgeons of Ontario (CPSO). 2019. Doctor Search (Advanced). Retrieved August 29, 2020. <https://doctors.cpso.on.ca/?search=general>.
DeClerq, K. 2020, May 5. Toronto to Begin Tracking Racial and Socio-Economic Data in COVID-19 Patients. CP24. Retrieved September 26, 2020. <https://www.cp24.com/news/toronto-to-begin-tracking-racial-and-socio-economic-data-in-COVID-19-patients-1.4926450>.
de Mossaic, D. and S. Bowen. 2019. Impact of Language Barriers on Quality of Care and Patient Safety for Official Language Minority Francophones in Canada. Journal of Patient Experience 6(1): 24–32. doi:10.1177/2374373518769008.
Federal, Provincial and Territorial Advisory Committee on Population Health (ACPH). 1999, September. Toward a Healthy Future: Second Report on the Health of Canadians. Government of Canada. Retrieved April 11, 2020. <http://publications.gc.ca/collections/Collection/H39-468-1999E.pdf>.
Guterman, S., S.C. Schoenbaum, K. Davis, C. Schoen, A.-M.J. Audet, K. Stremikis et al. 2011, April. High Performance Accountable Care: Building on Success and Learning from Experience. The Commonwealth Fund. Retrieved November 21, 2020. <https://www.commonwealthfund.org/sites/default/files/documents/___media_files_publications_fund_report_2011_apr_1494_guterman_high_performance_accountable_care_v3.pdf>.
Guttmann, A., S. Gandhi, S. Wanigaratne, H. Lu, L.E. Ferriera-Legere, J. Paul et al. 2020, September. COVID-19 in Immigrants, Refugees and Other Newcomers in Ontario: Characteristics of Those Tested and Those Confirmed Positive, as of June 13, 2020. IC/ES. Retrieved November 21, 2020. <https://www.ices.on.ca/Publications/Atlases-and-Reports/2020/COVID-19-in-Immigrants-Refugees-and-Other-Newcomers-in-Ontario>.
Holst, J. 2020. Increasing Rural Recruitment and Retention through Rural Exposure during Undergraduate Training: An Integrative Review. International Journal of Environmental Research and Public Health 17(17): 6423. doi:10.3390/ijerph17176423.
Jiang, M. 2020, April 22. The Reason Zoom Calls Drain Your Energy. BBC. Retrieved July 23, 2020. <https://www.bbc.com/worklife/article/20200421-why-zoom-video-chats-are-so-exhausting>.
Langford, M., G. Higgs and R. Fry. 2016. Multi-Modal Two-Step Floating Catchment Area Analysis of Primary Health Care Accessibility. Health & Place 38: 70–81. doi:10.1016/j.healthplace.2015.11.007.
Lepage, J.-F. and E. Lavoie. 2017, January 6. Ethnicity, Language and Immigration Thematic Series: Health Care Professionals and Official-Language Minorities in Canada, 2001 and 2011. Statistics Canada. Retrieved April 11, 2020. <https://www150.statcan.gc.ca/n1/pub/89-657-x/89-657-x2017002-eng.htm>.
Luo, W. and F. Wang. 2003. Measures of Spatial Accessibility to Health Care in a GIS Environment: Synthesis and a Case Study in the Chicago Region. Environment and Planning B: Planning and Design 30(6): 865–84. doi:10.1068/b29120.
McCoy, R.G., K.S. Bunkers, P. Ramar, S.K. Meier, L.L. Benetti, R.E. Nesse et al. 2018. Patient Attribution: Why the Method Matters. American Journal of Managed Care 24(12): 596–603.
Meuter, R.F.I, C. Gallois, N.S. Segalowtize, A.G. Ryder and J. Hocking. 2015. Overcoming Language Barriers in Healthcare: A Protocol for Investigating Safe and Effective Communication When Patients or Clinicians Use a Second Language. BMC Health Services Research 15: 371. doi:10.1186/s12913-015-1024-8.
McKeary M. and B. Newbold. 2010. Barriers to Care: The Challenges for Canadian Refugees and their Health Care Providers. Journal of Refugee Studies 23(4): 523–45. doi:10.1093/jrs/feq038.
Ngwakongnwi, E., B.R. Hemmelgarn, R. Musto, K.M. King-Shier and H. Quan. 2012. Language Barriers: Use of Regular Medical Doctors by Canada's Official Language Minorities. Canadian Family Physician 58(12): e709–16.
Office of the Languages Commissioner of Nunavut. 2015, October. Systemic Investigation Report: Investigation into the Qikiqtani General Hospital's Compliance with the Official Languages Act, R.S.N.W.T. 1988: Final Report. Retrieved July 24, 2020. <https://langcom.nu.ca/sites/langcom.nu.ca/files/QGH%20-%20Final%20Report%20EN.pdf>.
Peckham, A., D. Rudoler, D. Bhatia, S. Fakim, S. Allin, G. Marchildon. 2018, November. Rapid Review 9. Accountable Care Organizations and the Canadian Context. Retrieved September 26, 2020. <https://ihpme.utoronto.ca/wp-content/uploads/2018/11/NAO-Rapid-Review-9_EN.pdf>.
Provincial Health Services Authority. 2021. Spoken Language Interpreting Services. Retrieved February 6, 2021. <http://www.phsa.ca/health-professionals/professional-resources/interpreting-services>.
Rawal, S., J. Srighanthan, A. Vasantharoopan H. Hu, G. Tomlinson and A.M. Cheung. 2019. Association between Limited English Proficiency and Revisits and Readmissions after Hospitalization for Patients with Acute and Chronic Conditions in Toronto, Ontario, Canada. JAMA 322(16): 1605–07. doi:10.1001/jama.2019.13066.
Santé Montreal. 2020. CORONAVIRUS COVID-19: About COVID-19. Retrieved June 20, 2020. <https://santemontreal.qc.ca/en/public/coronavirus-COVID-19/>.
Sears, J., K. Khan, C.I. Ardern and H. Tamim. 2013. Potential for Patient–Physician Language Discordance in Ontario. BMC Health Services Research 13: 535. doi:10.1186/1472-6963-13-535.
Statistics Canada. 2015, November 30. Analysis of Results: Ethnocultural Diversity within Census Metropolitan Areas (CMAs) [archived]. Retrieved September 26, 2020. <https://www150.statcan.gc.ca/n1/pub/91-551-x/2010001/ana-eng.htm#a3>.
Statistics Canada. 2017, August 31. Proportion of Mother Tongue Responses for Various Regions in Canada, 2016 Census. Retrieved April 20, 2020: <https://www12.statcan.gc.ca/census-recensement/2016/dp-pd/dv-vd/lang/index-eng.cfm#chrt-dt-tbl>.
Stukel, T.A., R.H. Glazier, S.E. Schultz, J. Guan, B.M. Zagorski, P. Gozdyra et al. 2013. Multispecialty Physician Networks in Ontario. Open Medicine 7(2): e40–55.
Timony, P.E., A.P. Gauthier, S. Serresse, N. Goodale and J. Prpic. 2016. Barriers to Offering French Language Physician Services in Rural and Northern Ontario. Rural and Remote Health 16(2): 3805.
van Dorn, A., R.E. Cooney and M.L. Sabin. 2020. COVID-19 Exacerbating Inequalities in the US. The Lancet.395(10232): 1243–44. doi:10.1016/S0140-6736(20)30893-X.
Waibel, S., S.T. Wong, A. Katz, J.-F. Levesque, R. Nibber and J. Haggerty. 2018. The Influence of Patient–Clinician Ethnocultural and Language Concordance on Continuity and Quality of Care: A Cross-Sectional Analysis CMAJ Open 6(3): E276–E284. doi:10.9778/cmajo.20170160.
Wang, L., M. Rosenberg and L. Lo. 2008. Ethnicity and Utilization of Family Physicians: A Case Study of Mainland Chinese Immigrants in Toronto, Canada. Social Science & Medicine 67(9): 1410–22. doi:10.1016/j.socscimed.2008.06.012.
Webster, P. 2018, May 30. Language Barriers Restricting Access to Health Care for Indigenous Populations. CMAJ News. Retrieved June 20, 2020. <https://cmajnews.com/2018/05/30/language-barriers-restricting-access-to-health-care-for-indigenous-populations-cmaj-109-5613/>.
Winnipeg Regional Health Authority (WRHA). n.d. Language Access Currently Employs Trained Health Interpreters Providing Face-to-Face Interpreter Services in 36 Languages. Retrieved November 13, 2020. <https://professionals.wrha.mb.ca/old/professionals/language/index.php>.
Yen, W. 2013, April. How Long and How Far Do Adults Travel and Will Adults Travel for Primary Care? Washington State Health Services Research Project: Research Brief No. 70. Retrieved April 11, 2020. <https://www.ofm.wa.gov/sites/default/files/public/legacy/researchbriefs/2013/brief070.pdf>.
Footnotes
Notes
1. Statistics Canada intercensal estimate of the population does not report counts by ethnic characteristics or NOLs spoken. Therefore, it was not possible to use 2018 population data.
2. It is likely that there is also a generational imbalance because seniors in ethnic minorities tend to be overrepresented among those not speaking any of the official languages, and they could be more at risk during a pandemic. However, that would be a topic for a separate study.
3. This percentage varies considerably among jurisdictions. For example, it is only 17% in Ontario but 44% in Quebec, suggesting that rural/remote areas in some jurisdictions are more underserved than others.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed