Healthcare Quarterly
Equity-Mobilizing Partnerships in Community (EMPaCT): Co-Designing Patient Engagement to Promote Health Equity
Abstract
Equity-Mobilizing Partnerships in Community (EMPaCT) is a novel approach to patient engagement that centres diverse lived experiences and promotes equity-oriented and inclusive partnerships. As an independent community table, EMPaCT is made up primarily of patients/diverse members of community. Researchers and other decision makers come to this table with their projects to learn how to make their project more inclusive and equitable. In this paper, we detail how we used participatory co-design to define, build and grow EMPaCT as an innovative and scalable patient partnership model that promotes bottom-up action for health equity.
Key Points
|
Introduction
With the maturing of patient engagement, the demand to include a more diverse set of perspectives has grown. Equity-Mobilizing Partnerships in Community (EMPaCT) is a novel approach to engaging with diverse and structurally seldom-heard population groups by partnering on terms and projects that are prioritized by members of community themselves. Through this process of co-design, EMPaCT has grown to become an independent community-led and community-driven table made up primarily of patients/diverse members of community. Members of EMPaCT meet regularly every month to provide Health Equity Assessments (HEAs) through the lens of their collective lived experience to project decision makers.
EMPaCT exists as an expert advisory group independent of any specific project. We have co-produced our engagement structures and policies. Since our establishment in January 2021, we have consulted on several projects brought to us by decision makers, policy influencers and research teams seeking to learn from diverse lived experiences, enhance the inclusivity of their work and reduce health inequities. By centring the diverse lived experiences of community members, we are building capacity for impactful outcomes by mobilizing community knowledge on issues related to health equity and translating them into tangible recommendations for projects.
EMPaCT is housed at the Women's College Hospital (WCH) Institute for Health System Solutions and Virtual Care (WIHV). Designed as a scalable model of equitable patient engagement, it has received the Engaging Multi-stakeholders for Patient Oriented-research Wider Effects and Reach (EMPOWER) Award from the Ontario Strategy for Patient-Oriented Research (SPOR) SUPPORT Unit (OSSU). In this paper, we share the participatory co-design journey that led to EMPaCT. Participatory co-design refers to partnership with members of community who have relevant lived experiences and the involvement of all members in the co-production of processes and collaborative decision making toward a unified goal (Palmer et al. 2019). Documenting the co-design process is increasingly recognized as an important way to understand the linkages among participatory action, project outcomes and associated impacts (O'Brien et al. 2021; Palmer et al. 2019).
Conceptual Approach to Co-Design
We have applied an equity-oriented approach (engaging with those who are least likely to be included with the greatest amount of outreach; Sayani et al. 2021) to the co-design of EMPaCT. As such, we recognize that health inequities have been created by the historical and systematic disempowerment of communities through interlocking structures of sexism, colonialism and racism resulting in the unjust and unfair distribution of power, privilege and prestige, which determine opportunities to be healthy and health outcomes (Hankivsky and Christoffersen 2008; McGibbon and McPherson 2011; Raphael and Bryant 2015; Sayani 2019). As a consequence, groups experiencing the most marginalization by society (based on the intersections of gender, race, income, etc.) are the most likely to be left out of decision making unless proactive outreach is done and relationships rooted in trust are built (Sayani et al. 2021).
We have grown as a community by applying an equity-oriented and trauma-informed (nurturing relationships of trust that recognize structures and systems of oppression) approach to engagement (Sayani et al. 2021). We have taken a stepwise approach to enhance diversity, equity and inclusivity using the ConNECT Framework (Alcaraz et al. 2017) in the following ways:
- Integrating CONtext: recognizing the intersections among structural oppression, the COVID-19 pandemic and the heightened need to integrate structurally seldom-heard diverse voices into policies that can shape action for health equity;
- Fostering a Norm of inclusion: co-designing our process of engagement, ensuring compensation for members unless they choose to decline it and not using predefined labels to describe people;
- Ensuring Equitable diffusion of innovations: facilitating real-world benefit for all by leveraging lived experiences and integrating community priorities into the design and implementation of research, policies and plans;
- Harnessing Communication technology: prioritizing digital equity and deliberately supporting digital participation for all members of EMPaCT; and
- Prioritizing specialized Training: maximizing participation through mutual co-learning, in which each member of EMPaCT is both a learner and a teacher, and identifying future learning needs that may be serviced by outside providers.
Co-Designing a Sustainable and Scalable Model of Equitable Patient Partnerships
Three key issues have hindered effective action to improve health inequities across sectors:
- Absence of a conceptual framework that makes explicit the linkages among social, political and economic inequalities and health outcomes (Ndumbe-Eyoh and Moffatt 2013);
- Lack of social participation to the degree that communities experiencing the most inequities have little influence in decision making (WHO 2010); and
- A failure to take considerations of scalability and sustainability into program design (WHO 2010).
We have described our conceptual underpinning earlier; now in this section, we describe how we have applied the Institute for Healthcare Improvement (IHI) Framework of Going to Full Scale (Barker et al. 2016) to co-design EMPaCT as a scalable and sustainable model of diverse patient engagement (Figure 1).
It is important to note that the foundation of our co-design work rests on relationships (Figure 1). Some relationships existed prior to beginning this project, and many more have been built along the way. As a fundamental value, relationships are core to our existence, and relationships take priority over any processes and outcomes we may wish to achieve as a group. EMPaCT's foundational blocks include institutional buy-in and supportive structures (legal, finance, strategic direction and senior scientists) and the availability of resources such as time and grant funds.
Scale-up idea
We have expanded on the IHI Framework of Going to Full Scale (Barker et al. 2016) by including an additional section on the scale-up idea at the start. We define a scale-up idea as a learning health system innovation that results from engaging in dialogue about the possibilities for change that can be packaged as a solution and implemented across settings. As a patient-partnered project, it is important to detail how we co-designed the idea for EMPaCT.
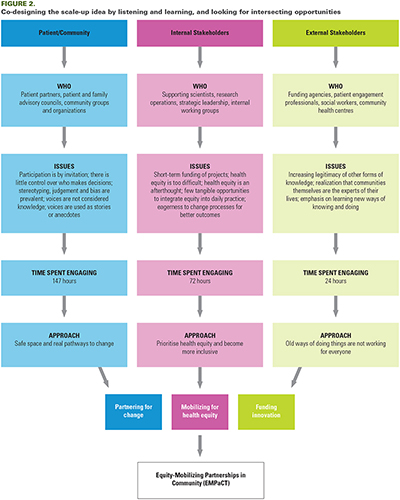
In May 2020, members of a patient-oriented research team (AS, JM, EN, JP, SH, GB and AL) realized that their work lacked the diversity of perspectives needed to appropriately inform their study on lung cancer screening. Participation in lung cancer screening is influenced by barriers such as discrimination, historical injustice and stigma, particularly for Indigenous populations, recent immigrants and those living in conditions of poverty and precarious housing, for whom smoking and access to care are shaped by social and structural inequality. To appropriately proceed with the lung cancer screening study, it was first important to partner with patients with the relevant lived experiences. Engaging patients who bring diverse perspectives particularly from structurally underserved communities is a recognized challenge in patient engagement. This sparked a broader engagement with patients, community members and institutional stakeholders and ultimately the co-initiation of EMPaCT. AS and AM began by listening and learning about the barriers to diverse patient engagement through formal and informal conversations with a variety of different stakeholders (June 2020–December 2020). Using integrated knowledge translation (iKT; Jull et al. 2017), we specifically looked for intersecting opportunities that could be channelled into actionable steps. The details of this step, including the hours of engagement per stakeholder group, key themes and opportunities, are outlined in Figure 2.
Set up groundwork for success
Set up refers to the preparation needed to seed a scale-up idea (Barker et al. 2016). This includes an initial test site to nurture and promote an idea and give it space to grow. WIHV is an innovation lab where team members collaborate to generate solutions to emerging health issues. In an organization committed to equity, we identified early adopters (supporting scientists, JS and AL) who were ready to fund and engage with members of EMPaCT on the terms set by members of EMPaCT. The institutional champions for change (peers, the WIHV Equity-Advisory Committee, research operations and strategic leadership for WIHV) all collaborated to meet the needs and priorities of EMPaCT as it formed with early members that included AS and AM.
Co-develop a scalable unit
A "scalable unit" is defined as a microsystem of key infrastructure and relationships needed for full scale (Barker et al. 2016). For EMPaCT, we have grown as a community one relationship at a time (from two members in December 2020 to 15 members in March 2022, 12 of whom are patients/diverse members of community). We devote half our monthly meeting time to nurturing our relationships and co-designing the next steps. Meetings are steered by AS and AM, and members take turns to lead and reflect on different activities. This process has built trust as a group, sustained engagement over time and refined our collective vision. We see ourselves as advocates for change unified by our desire to push for health system changes to promote health equity. We are disseminating knowledge concepts related to health equity, patient partnerships and pathways to change in the form of a digital library containing co-presented videos and webinars. We have co-designed a consultation process whereby we conduct HEAs. Traditionally, most HEAs are conducted by scientific experts, academics and policy administrators. The EMPaCT HEAs are based on the expertise of the members' diverse lived experiences brought to the process as a collective analytical lens. To our understanding, we are the first community of those with diverse lived experiences to offer and conduct HEAs. The strategic location of EMPaCT in an innovation hub has allowed us to navigate exclusionary institutional policies that create barriers to diverse patient engagement, including modifications to financial and legal agreements between institutions and community members.
As a scalable unit, EMPaCT is an expert advisory group existing independent of any specific project. Project decision makers (policy makers, health/social service administrators and research collaborators) are referred to as "impact partners". They engage with EMPaCT to learn and co-create knowledge/policy/practice solutions that advance health equity. The impact partners request to meet with EMPaCT. As part of the intake process, AS and AM coach impact partners for engagement with EMPaCT. This includes refining scope and communication skills so that the consultation results in authentic dialogue for co-learning. During EMPaCT consultations, members engage with project teams to help them understand how different communities might be impacted by a decision, what unintended outcomes may occur and how equity in health can be better addressed for the communities involved. Impact partners receive a written report validated by all members containing recommendations from the consultation process. Impact partners provide feedback on how they modified their project based on the findings of the report. They also provide feedback on the process of engagement. The community uses this to continuously improve how we do things. This relationship is the "impact partnership" between EMPaCT and decision makers.
Test of scale-up and potential for impact
To date, EMPaCT has engaged in a variety of impact partnerships, including research and hospital policy for four hospitals in Ontario, Canada. We have disseminated knowledge through a variety of platforms and received a provincial award as a scalable model of equitable patient engagement. Table 1 shows the impact categories for EMPaCT based on the Canadian Academy of Health Sciences Framework (CAHS) (CAHS 2009).
| TABLE 1. Impact from EMPaCT based on the CAHS Framework for measuring impact from research investments | |||||
| Building capacity | Advancing knowledge | Informing decisions | |||
| Members of EMPaCT | 14 | Publications | 3 | Impact partnerships | 7 |
| Sources of funding | 3 | Presentations | 6 | Impact partners engaged | 20 |
| Awards | 1 | Workshops | 2 | Decision makers engaged* | 9 |
| Digital videos | 3 | Hospitals served | 4 | ||
| Technical reports | 8 | ||||
| Source: CAHS 2009 | |||||
| *One senior vice president, two hospital vice presidents, one hospital medical director and five research principal investigators. | |||||
Key Learnings
We have learned from our projects that there is much demand for EMPaCT as an expert group to guide health system stakeholders to improve health equity in their projects. We are hopeful that many small actionable steps taken across the system are the start of a bottom-up community movement promoting health equity.
We have also learned that our health systems are structured to be exclusionary and discriminatory. The terms of patient engagement should be directed by members of community, safe spaces need to be built on relationships of trust and power hierarchies must be blurred so that each person occupies the role of both teacher and learner. This includes impact partners who receive preliminary coaching to scope and prepare for their consultation with EMPaCT.
Finally, a key learning has been that a willing host organization committed to adapting institutional policies and procedures to support a community is essential. EMPaCT has been able to grow and sustain itself because of the change makers at WCH who have believed in its value and supported its development.
In parallel with our scale-up, we have initiated a project evaluation loop where we are collecting anonymous feedback from the members of EMPaCT and impact partners to understand their experiences and perspectives on EMPaCT. We will analyze these findings together as a community to co-design better processes in the future.
Conclusion
The current processes of patient engagement within an already deeply hierarchical healthcare system reinforce the structures and policies that perpetuate inequalities and create barriers. Transformative change striving to improve health outcomes across the population requires innovative models of partnership centred around public participation and citizen empowerment. The involvement of patients and community members in decision making can contribute to the design of a patient-responsive healthcare system. We have described how we have co-designed EMPaCT as a patient partnership model that promotes bottom-up action for health equity. This community-driven model has potential for impact across multiple sectors and is rooted in a framework to promote social justice and health equity.
About the Author(s)
Ambreen Sayani, MD, MSc, PhD, is a Transition to Leadership Stream postdoctoral fellow in Patient-Oriented Research at the Women's College Research Institute at WCH in Toronto, ON, and co-initiator of EMPaCT. Ambreen can be contacted by e-mail at ambreen.sayani@wchospital.ca.
Alies Maybee, BA, is an independent patient partner, co-initiator of EMPaCT and co-founder of the Patient Advisors Network (PAN) in Toronto, ON.
Jackie Manthorne, BA, BEd, is the president and chief executive officer of the Canadian Cancer Survivor Network in Toronto, ON.
Erika Nicholson, MHSc, is vice president, Cancer Control at the Canadian Partnership Against Cancer in Toronto, ON. She works with pan-Canadian partners to drive progress toward the goals of the Canadian Strategy for Cancer Control.
Gary Bloch, MD, CCFP, is a family physician with St. Michael's Hospital and Inner City Health Associates and an associate professor at the University of Toronto in Toronto, ON. His clinical, educational, program development, research and advocacy interests focus on the intersection among primary care, health inequities and the social determinants of health.
Janet A. Parsons, BScPT, MSc, PhD, is a research scientist at the Applied Health Research Centre, Li Ka Shing Knowledge Institute of St. Michael's Hospital and an associate professor with the Department of Physical Therapy and the Rehabilitation Sciences Institute, University of Toronto in Toronto, ON. She is a qualitative methodologist who conducts health services and policy research, with expertise in health and social equity, patient and community engagement and participatory approaches to research and knowledge translation.
Stephen W. Hwang, MD, MPH, FRCPC, is the chair of Homelessness, Housing, and Health; director of the MAP Centre for Urban Health Solutions at St. Michael's Hospital; and a professor of Medicine at the University of Toronto in Toronto, ON.
James A. Shaw, PT, PhD, is an assistant professor in the Department of Physical Therapy at the University of Toronto with cross-appointment to the Institute of Health Policy, Management and Evaluation at the University of Toronto in Toronto, ON. He serves as a research director of Artificial Intelligence (AI), Ethics & Health at the University of Toronto's Joint Centre for Bioethics and is an adjunct scientist at the WCH Institute for Health System Solutions and Virtual Care.
Aisha Lofters, MD, PhD, CCFP, is a clinician scientist with the Department of Family and Community Medicine at the University of Toronto and chair in Implementation Science at the Peter Gilgan Centre for Women's Cancers at WCH in Toronto, ON. Her research focuses on cancer screening and prevention with a health equity lens.
Members of EMPaCT
The members of EMPaCT are Emily Cordeaux, Ryan Hinds, Tara JejiP, Omar KhanP, Bee LeeP, Alies MaybeeP, Desiree MensahP, Linda MonteithP, Mursal MusawP, Marlene RathboneP, Jill RobinsonP, Staceyan SterlingP, Ambreen Sayani and Dean WardakP.
References
Alcaraz, K.I., J. Sly, K. Ashing, L. Fleisher, V. Gil-Rivas, S. Ford et al. 2017. The ConNECT Framework: A Model for Advancing Behavioral Medicine Science and Practice to Foster Health Equity. Journal of Behavioral Medicine 40(1): 23–38. doi:10.1007/s10865-016-9780-4.
Barker, P.M., A. Reid and M.W. Schall. 2016. A Framework for Scaling Up Health Interventions: Lessons from Large-Scale Improvement Initiatives in Africa. Implementation Science 11(1): 12. doi:10.1186/s13012-016-0374-x.
Canadian Academy of Health Sciences (CAHS). 2009. Making an Impact: A Preferred Framework and Indicators to Measure Returns on Investment in Health Research. Retrieved July 11, 2016. <https://www.cahs-acss.ca/wp-content/uploads/2011/09/ROI_FullReport.pdf>.
Hankivsky, O. and A. Christoffersen. 2008. Intersectionality and the Determinants of Health: A Canadian Perspective. Critical Public Health 18(3): 271–83. doi:10.1080/09581590802294296.
Jull, J., A. Giles and I.D. Graham. 2017. Community-Based Participatory Research and Integrated Knowledge Translation: Advancing the Co-Creation of Knowledge. Implementation Science 12(1): 150. doi:10.1186/s13012-017-0696-3.
McGibbon, E. and C. McPherson. 2011. Applying Intersectionality & Complexity Theory to Address the Social Determinants of Women's Health. Women's Health and Urban Life 10(1): 59–86.
Ndumbe-Eyoh, S. and H. Moffatt. 2013. Intersectoral Action for Health Equity: A Rapid Systematic Review. BMC Public Health 13(1): 1056. doi:10.1186/1471-2458-13-1056.
O'Brien, J., E. Fossey and V.J. Palmer. 2021. A Scoping Review of the Use of Co-Design Methods with Culturally and Linguistically Diverse Communities to Improve or Adapt Mental Health Services. Health and Social Care in the Community 29(1): 1–17. doi:10.1111/hsc.13105.
Palmer, V.J., W. Weavell, R. Callander, D. Piper, L. Richard, L. Maher et al. 2019. The Participatory Zeitgeist: An Explanatory Theoretical Model of Change in an Era of Coproduction and Codesign in Healthcare Improvement. Medical Humanities 45(3): 247–57. doi:10.1136/medhum-2017-011398.
Raphael, D. and T. Bryant. 2015. Power, Intersectionality and the Life-Course: Identifying the Political and Economic Structures of Welfare States that Support or Threaten Health. Social Theory & Health 13(3–4): 245–66. doi:10.1057/sth.2015.18.
Sayani, A. 2019. Social Class and Health Inequalities. In D. Raphael, T. Bryant and M.H. Rioux, Eds., Staying Alive: Critical Perspectives on Health, Illness and Healthcare (3rd edition) (pp. 171–98). Canadian Scholars' Press Inc.
Sayani, A., A. Maybee, J. Manthorne, E. Nicholson, G. Bloch, J.A. Parsons et al. 2021. Building Equitable Patient Partnerships during the COVID-19 Pandemic: Challenges and Key Considerations for Research and Policy. Healthcare Policy 17(1): 17–24. doi:10.12927/hcpol.2021.26582.
World Health Organization (WHO). 2010. Intersectoral Action to Tackle the Social Determinants of Health and the Role of Evaluation. Retrieved June 30, 2021. <https://apps.who.int/iris/bitstream/handle/10665/70579/WHO_ETH_10.1_eng.pdf>.
Footnotes
P = Patient partner.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed