Healthcare Quarterly
Impact of the COVID-19 Pandemic on the Health Workforce in Canada
Healthcare workers are the foundation that keep our healthcare systems running. The recent COVID-19 pandemic has placed unprecedented demands on Canada's health workforce. The Canadian Institute for Health Information has compiled data and information to help inform how the pandemic has impacted healthcare workers and the care Canadians received.
This article deliberates on the many challenges of the pandemic, such as safety and access to personal protective equipment, faced by healthcare workers along with its impact on health workers and the healthcare system. The article also shares how the system responded to protect the health workforce and boost capacity by expanding provider roles and adapting new ways of delivering services, including quickly adapting to virtual care.
Background
Healthcare workers are the foundation of our healthcare systems. From testing and caring for COVID-19 patients to maintaining levels of care in the community and vaccinating people, the COVID-19 pandemic has highlighted the importance of the health workforce in all aspects of care delivery. The Canadian Institute for Health Information (CIHI) has compiled data and information on Canada's health workforce to investigate how it was impacted by the COVID-19 pandemic.
Supply of Health Workforce
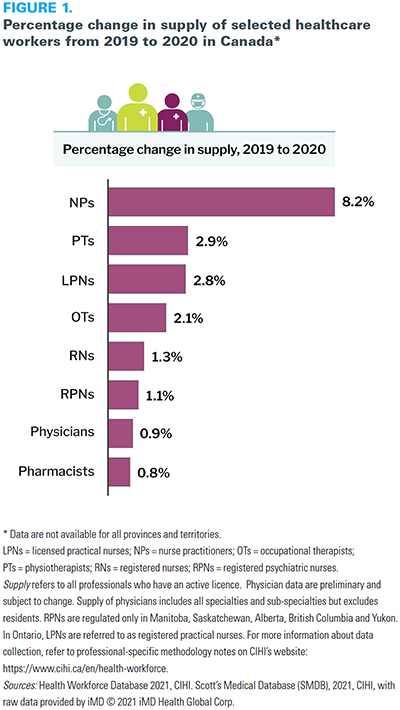
From 2019 to 2020, Canada saw an increase in the supply of selected healthcare workers, including physicians (0.9%), regulated nursing professionals (1.8%), pharmacists (0.8%), physiotherapists (2.9%) and occupational therapists (2.1%) (Figure 1). More than 90% of these healthcare workers (excluding physicians) were working in a role related to their profession. Of those, about 9 out of 10 worked in direct patient care roles.
As the number of COVID-19 cases increased, jurisdictions examined different approaches to maintain staffing levels, including tapping into the supply of retired or non-practising healthcare workers. Many regulatory bodies waived or modified licence reinstatement requirements, allowing these individuals to rapidly return to their profession during the time of need. Based on data obtained from Canada's professional regulatory bodies, nearly 6,000 non-practising nurses, occupational therapists, physiotherapists and pharmacists responded to the call to provide support across the country in 2020. Despite the increase in supply, healthcare worker infections and exposure to the virus contributed to staffing shortages.
Expanding Health Workforce Roles
As the pandemic continued, the needs for COVID-19 testing and vaccination placed additional demands on Canada's health workforce. By June 1, 2021, more than 34 million COVID-19 tests had been performed in Canada, and upwards of 24 million vaccines had been administered (Government of Canada 2020).
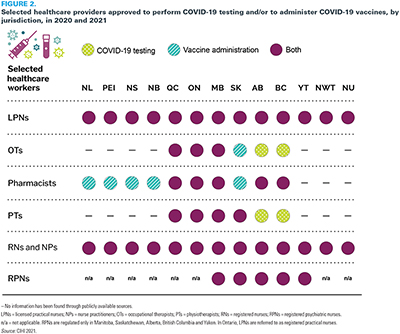
Each jurisdiction looked to different professions to meet these demands. For example, Quebec authorized midwives, chiropractors, occupational therapists, optometrists, ambulance technicians and those practising within a health and social services institution to perform COVID-19 testing. Across the country, many provinces and territories also expanded the list of healthcare workers approved to administer COVID-19 vaccines to accelerate the process in order to protect Canadians. Figure 2 provides a snapshot of publicly available data captured in CIHI's COVID-19 Intervention Scan (CIHI 2022), showing different types of healthcare workers approved to administer COVID-19 tests or vaccinations across Canada.
Adapting to Virtual Care
The COVID-19 pandemic has altered how Canadians engage with healthcare systems. As cases surged across the country, access to in-person healthcare services was restricted. Canada's healthcare workers quickly adapted to the virtual service delivery approach to maintain continuity of care.
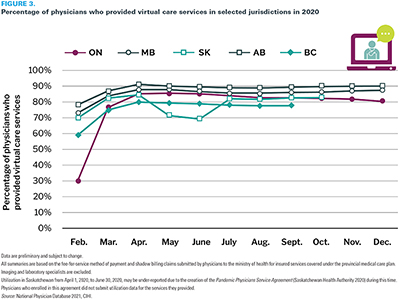
In February 2020, for the provinces where data were available, 48% of physicians had provided at least one virtual care service. By April 2020, this had increased to 85.3% (Figure 3).
For those same five provinces, Canadians accessing physician services also experienced a significant change: the proportion of patients who received at least one virtual care service jumped from 6% to 56% between February and September 2020.
The pandemic promoted the introduction of new virtual care guidelines and best practices for many other professions across the country (CIHI 2022). Understanding which healthcare professionals are using virtual care to provide services and how will be important for filling data gaps around equity in access and outcomes.
Challenges for Long-Term Care Workers
Several types of healthcare professionals work in long-term care (LTC). A recent CIHI report found that by August 31, 2020, a total of 12,005 LTC workers had contracted COVID-19 (CIHI 2021). The implementation of infection prevention and control measures remained critical to protecting both healthcare workers and patients in LTC. Early in the pandemic, Canada's provinces and territories rapidly mobilized plans to secure personal protective equipment for the health workforce, especially for harder hit sectors, such as LTC. However, factors such as issues with supply chains posed many challenges in the process.
Analysis of data from a 2020 crowdsourced survey sheds some light on experiences of individuals working in healthcare settings (Statistics Canada 2020). Of the respondents who worked in LTC, 51% reported challenges in always having access to respirators (e.g., N95 masks). Additionally, 25% stated that equipment such as face shields and goggles were not always available when needed (Statistics Canada 2020).
Formal investigations that have taken place with regard to COVID-19 in LTC recommend that increased staffing levels and better infection control measures are needed to reduce the risk of infections, outbreaks and deaths (CIHI 2021).
Long-Term Impacts
Healthcare workers have continued to provide care for patients despite exhaustion, personal risk of infection, fear of transmission to family members and the loss of patients and colleagues. The long-term effects of the pandemic on Canada's health workforce, including those on mental health, remain to be seen.
CIHI continues to collect and analyze health workforce data to understand the impacts of the pandemic, including looking at how burnout might impact the supply of healthcare workers in the years to come. Standardized pan-Canadian health workforce data will be key for the planning and management of the health workforce as health systems begin to recover from the COVID-19 pandemic.
About the Author(s)
Amanda Tardif, MSc, is a senior analyst with the Health Workforce Information team at CIHI in Ottawa, ON. She can be reached at atardif@cihi.ca
Babita Gupta, BSc, MBA, is a program lead with the Health Workforce Information team at CIHI in Ottawa, ON.
Lynn McNeely, BScN, is the manager of the Health Workforce Information team at CIHI in Ottawa, ON.
Walter Feeney, BSc, is a program lead with the Physician Information team at CIHI in Ottawa, ON.
References
Canadian Institute for Health Information (CIHI). 2021, March 30. The Impact of COVID-19 on Long-Term Care in Canada: Focus on the First 6 Months. Retrieved June 3, 2021. <https://www.cihi.ca/sites/default/files/document/impact-COVID-19-long-term-care-canada-first-6-months-report-en.pdf>.
Canadian Institute for Health Information (CIHI). 2022, January 13. COVID-19 Intervention Scan. Retrieved April 1, 2022. <https://www.cihi.ca/en/COVID-19-intervention-scan>.
Government of Canada. 2020, March 3. Public Health Infobase – Data on COVID-19 in Canada. Retrieved June 3, 2021. <https://open.canada.ca/data/en/dataset/261c32ab-4cfd-4f81-9dea-7b64065690dc>.
Saskatchewan Health Authority. 2020. Pandemic Agreement. Retrieved April 1, 2022. <https://www.saskdocs.ca/pandemic-physician-agreement-submission/>.
Statistics Canada. 2020, November 25. Impacts of COVID-19 on Health Care Workers: Infection Prevention and Control (ICHCWIPC). Retrieved January 25, 2022. <https://www.statcan.gc.ca/en/survey/household/5340>.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed