Healthcare Policy
Wait Time Management Strategies for Scheduled Care: What Makes Them Succeed?
Marie-Pascale Pomey, Pierre-Gerlier Forest, Claudia Sanmartin, Carolyn De Coster and Madeleine Drew
Abstract
Objectives: To assess experts' perceptions of the contextual and local factors that promote or inhibit the implementation of waiting time management strategies (WTMS) in Canadian healthcare organizations.
Methods: We conducted 16 semi-structured interviews and one focus group with individuals involved in WTMS at the federal, provincial or organizational level.
Results: The most frequently cited local factor was physicians' participation. Physicians' leadership made the greatest difference in bringing resistant physicians on board. To be effective, however, local leadership had to be supported by senior management. Alignment of financial incentives between the contextual and local levels was also frequently cited, and interviewees stressed the importance of tools used to design, monitor, evaluate and prioritize WTMS.
Conclusions: Finding the right balance between supportive resources and tools and an effective management system is a tough challenge. But achieving this balance will help reconcile contradictions between top-down and bottom-up WTMS.
For over a decade, industrialized countries around the world have struggled to solve the problem of long wait times for scheduled medical care (Siciliani and Hurst 2003). Canada's recent history in the matter is a study in paradoxes. On the one hand, Canadian decision-makers appear to have agreed that the answer to the problem of waiting lists and wait times lies at the federal and provincial levels, and recent Canadian wait time initiatives have consistently looked to centralized programs as their solution (Health Council of Canada 2007; Health Canada 2004; SCC 2005; Prime Minister of Canada 2007). On the other hand, recent findings suggest that the success or failure of a given wait time management strategy (WTMS) depends less on federal or provincial policy than on how the strategy is implemented in healthcare organizations (HCOs) themselves. The results of Ontario's Wait Times Strategy initiative, for example, reveal that HCOs were the key players in the program's success, and it was only after a significant investment of time, attention and resources that organizations adopted an accountability framework that allowed them to execute the program and meet the provincial government's objectives (Trypuc, Hudson et al. 2006; Trypuc, Hudson et al. 2007). It seems clear, then, that we must pay closer attention to the factors that facilitate or impede the implementation of WTMS in HCO (Ferlie and Shortell 2001). For that reason, this paper describes what WTM experts from different levels of Canada's healthcare system perceive as factors in the success or failure of WTMS, and how they feel these factors interact to facilitate or impede the implementation of WTM programs within HCOs.
Methods
We conducted 16 one- to two-hour interviews and one focus group with prominent thinkers and managers in the field of wait time management. The focus group was conducted at the request of a person whom we had contacted for an interview: this person felt that it would be useful for us to meet the entire wait time management team. The interviews took place between October 2005 and August 2006, and the focus group took place in October 2005. All interviews and the focus group were taped and transcribed. In order to solicit a variety of insights, we interviewed two groups of respondents. The first group comprised individuals who had been involved in wait time strategies at the federal or provincial level within the prior few years ("federal/provincial respondents"). These select individuals were among the most frequently consulted experts on WTM in Canada, and their views reflected decades of experience (Table 1). The second group of respondents (Table 2) consisted of senior leaders from eight healthcare organizations (HCOs). This latter group included respondents who
- represented provinces from different regions of the country (BC, AB, SK, MB, ON, QC, NS);
- represented a range of professions (physicians, surgeons and managers);
- addressed different domains of WTMS (cancer care, cardiac surgery, general surgery, broad initiatives, eye care, joint replacement and medical imaging);
- were familiar with different types of WTMS (active management strategies, benchmarks, information technology and wait list management, central booking systems, clinical assessment [prioritization] tools and clinical appropriateness guidelines); and
- had been active in WTMS in an HCO (a regional health authority or a hospital) over the past three years.
| TABLE 1. Federal/provincial respondents | |
| Province | Organization |
| Manitoba | Winnipeg Regional Health Authority, Federal Advisor on Waiting Times |
| British Colombia | Provincial Health Services Authority (PHSA) |
| Quebec | Montreal Regional Health Authority |
| Ontario | Institute for Clinical Evaluative Sciences |
| Ontario | Ontario Wait Times Strategy |
| Saskatchewan | Saskatchewan Health |
| Ontario | Canadian Association of Radiologists |
| Saskatchewan and Ontario | Saskatchewan Surgical Care Network and Ontario Wait Times Strategy |
| Ontario | Ontario provincial wait time information system |
| TABLE 2. Healthcare organization respondents | ||
| Organization | Interviewee's title | Waiting time strategy |
| Alberta Bone & Joint Health Institute, AB | Surgeon, Vice Chair of the Alberta Bone & Joint Health Institute | Joint replacement Pathway design, new coordinating entities |
| Calgary Health Region, AB | Physician, Medical Director | Joint replacement Pathway design; new coordinating entities |
| CSSS Alma, QC | Physician President of the Doctors', Dentists' and Pharmacists' Committee |
General surgery Pathway design, collection system, centralized booking system |
| Kingston General Hospital, ON | Manager, President and CEO | General surgery and cancer care Software, registries |
| QEII Health Sciences Centre (HI Site), NS | Surgeon, Head of Department of Surgery | General surgery and joint replacement Software, operations research, prioritization tool, increased capacity |
| St. Boniface General Hospital, MB | Surgeon, Department of Surgery | General surgery Registry, prioritization tool, website, increased capacity, pathway, operations research |
| Total Joint Network, ON | Manager, Project Manager | Joint replacement Pathway, prioritization tool |
| Vancouver Coastal Health Authority, BC | Managers, Focus group with five managers from the Services Planning Project | General surgery Prioritization tool, registry, performance target |
To elicit diverse aspects of respondents' experiences with WTMS, we selected a semi-structured interview approach that allowed us to explore trends in the implementation of WTMS within and across organizations, discuss respondents' views of the factors that facilitated or inhibited WTMS at the organizational level, and probe respondents' impressions of the influence of external elements.
This study was not intended as a comprehensive evaluation of WTMS in HCOs. Although our sample of individuals and organizations is broad-based, we made no attempt to represent all perspectives on this issue. Nor did we intend to collect rigorous and unbiased data. Rather, we sought qualitative data that would illuminate the situation as it now stands. Furthermore, given the exploratory nature of our study and the expertise of our respondents, it was not our intent to reach saturation. Nonetheless, certain themes in our respondents' perspectives emerged after the first 10 or so interviews. Insofar as the accuracy of our conclusions is concerned, the great experience of our expert respondents provides an excellent basis. Finally, to validate our findings, we presented them at several venues, including Taming of the Queue (CPRN 2009).
Framework
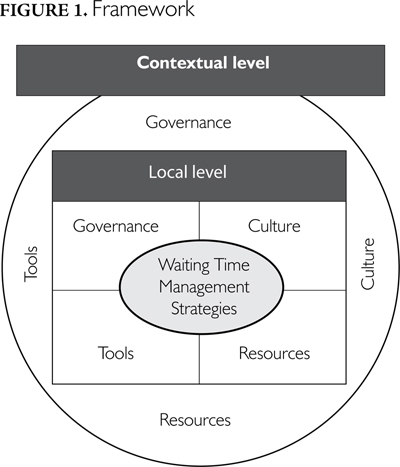
We used Parsons' (1977) social system action theory to evaluate how different factors interact and affect outcomes at the local and contextual levels. The Parsonian perspective corresponds to a structuro-functionalist view of organizations and focuses on the four functions required by organizations to survive: goal attainment, environmental adaptation, production and culture. We transposed these functions into four categories of factors relevant to the implementation of WTMS (Figure 1):
- governance factors (goal attainment and environmental adaptation), defined as "the conduct of collective action from a position of authority" (Hatchuel 2000);
- cultural factors (culture), defined as "underlying beliefs, values, norms and behaviors" (Shortell et al. 1995);
- resource factors (production), whether human, financial, infrastructural or informational; and
- tools (production), i.e., the instruments or procedures seen as helpful for implementing a strategy. An example is industrial engineering techniques such as queue management and patient flow processes.
We chose this framework because of its robust nature. Over the course of the past 50 years, the framework has been used in disciplines as diverse as sociology, administration and management and in organizational contexts of all kinds (industry, health and more). In our case, it allowed us to consider not only such factors as resources and tools that are commonly taken into account, but also political and cultural factors that are often overlooked.
We constructed an interview guide that organized questions according to our four categories (Table 3). More specifically, we asked how contextual-level and local-level factors in each category promoted or inhibited the implementation of a given WTMS. By contextual-level factors, we referred to factors that were present in the organization's environment, such as provincial and national legislation and policies (a governance factor) and economic conditions or provincial/national human resources shortages (resource factors). We defined local-level factors as factors that form part of a HCO: for example, the organization's ethical norms (a cultural factor), its protocols for the attraction and retention of staff (a tool), its human, financial and infrastructure resources (a resource factor) and its self-care process (a governance factor). The study was approved by the Ethics Committee of the University of Ottawa. To respect confidentiality respondents' quotations are identified only by institutional affiliation: federal/provincial respondents (FPR) or healthcare organization respondents (HOR).
| TABLE 3. Interview questions |
|
Case studies Factors
Documents |
Findings: Success Factors and Failure Factors in the Implementation of Wait Time Management Strategies
Research on organizational innovation has shown that specific factors promote or encourage innovation ("success factors"), while other factors inhibit it ("failure factors") (Greenhalgh et al. 2004). In this section, we explore respondents' perceptions of success and failure factors in the implementation of WTMS.
Local-level factors
GOVERNANCE FACTORS
Effective organizational leadership was mentioned by eight of 17 respondents, all of whom felt it to be key. Some respondents expressed this by identifying the lack of internal leadership as an impediment, while others emphasized the importance of a leader with credibility and vision. Still others stated that local-level wait time projects could not move forward without the support of senior management: "You need obvious organizational commitment. You need support from the senior leadership and the CEO for WTM" (FPR).
Local-level partnerships were another factor felt to be important, particularly in the field of orthopaedic surgery, where partnerships manifest as collaboration among various segments of the continuum of care (acute, rehabilitation and home care), collaboration between hospitals or collaboration among surgeons (some of whom had coordinated an orthopaedic "blitz"). For example, one respondent explained, "To prevent bed cuts, the physicians' leaders started to develop partnerships between the various stakeholders, to work on change before the government cut any beds" (HOR).
CULTURAL FACTORS
All respondents spoke of how pivotal physicians were to the success of WTMS. Seven of 10 organizational-level interviewees brought up physicians' support: "It's crucial to get the surgeons on side. The person implementing the initiative has to have the respect and trust of the surgeons" (HOR). In many cases, surgeons' leadership was cited as decisive. In Ontario and Nova Scotia, for example, surgeons confident about a computerized tracking system were central in bringing the other doctors on board: "At the beginning I had to convince my colleagues but when they understood how this could help their clinical practice with patients, they trusted me" (HOR).
Most organizational-level respondents also emphasized that involving doctors in the planning process from the outset was central to securing their support for federal and provincial strategies; they even suggested that general practitioners should take part in deciding the overall direction of the strategy. Respondents stressed, however, that local physician leadership was ineffective without the support of senior management. It was also clear that while certain strategies benefited from the dedication of a number of doctors, most physicians resisted change, and many actually hindered the implementation of wait time strategies. Respondents in three provinces (QC, MB and NS) attributed this phenomenon to the professional autonomy to which surgeons are accustomed, an autonomy that can act as a hurdle to the implementation of centralized lists.
Another cultural factor identified by our respondents consisted of the existence of subcultures within an organization. In most cases, subcultures were seen as an obstacle to the introduction of WTMS. Organizational-level respondents pointed out that the most successful initiatives took place in organizations dominated by a culture of innovation, one with opportunities to create team identity and a climate that promoted success. Among other cultural factors, one interviewee attributed his hospital's efficiency to its culture of data collection, on the grounds that better information allows for better decisions. In his view, however, the success of better data-collection initiatives depended on a non-punitive approach: "Originally there were some concerns about whether this would be used to measure performance and individuals and so on. But as time went on, people have found it useful to be able to know what exactly has been going on. And so trust was earned" (HOR). Contrary to this position, another interviewee expressed scepticism of the evidence-based culture, saying that "physicians and nurses are not data-driven. They pretend they are but they are not" (FPR). This opinion notwithstanding, several respondents felt that better data allowed more thorough evaluations, which soliciting the interest and collaboration of organizations, in turn. This occurred in the case of Greater Toronto's Total Joint Network.
RESOURCE FACTORS
All four kinds of resources (financial, human, infrastructural and informational) were identified as factors at the organizational level. Insofar as financial resources were concerned, "seed money" or "kick start" funds for wait time projects were mentioned as a factor in three successful initiatives, while in two other projects, insufficient funds had detrimental impacts. Transparency in the allocation of funds was also cited. Five participants explained how strategies at the local level were helped by financial incentives, such as extra compensation for physicians who provided the strategy with specified information. Few resources were mobilized for the implementation of initiatives undertaken by HCOs: "We didn't need a lot of money to launch our strategy" (HOR). Instead, local initiatives tended to deploy existing resources in new ways.
Among other types of resources mentioned, several respondents cited dedicated human resources as a beneficial factor and two identified personnel shortages as a barrier. Infrastructure resources were sometimes but not always an issue. General surgery in Winnipeg, for example, had adequate capacity, but patient distribution was not maximized as two surgeons had too many patients and other surgeons were underused. One of the orthopaedic surgeons interviewed, however, cited the availability of operating room space and hours as a major factor inhibiting the reduction of wait times. Information resources such as data collection and improved analysis were also mentioned by interviewees, who felt that these were critical if actors were to publicize the status of wait times and evaluate the implementation of WTMS.
TOOL FACTORS
Our respondents identified a number of local-level tools: patient care tools (such as referral criteria using a referral template); prioritization tools, often developed at the provincial level; clinical guidelines; patient pathways with target lengths of stay; and protocols for operating room use or postoperative treatment. Information technology was also cited as allowing better information sharing among clinical parties. One of the four respondents who touched on this point explained that the development of demand forecast modelling and the publication of comparative data on the Internet helped to "hold administration accountable" (FPR). Another stressed the importance of offering simple and relevant information technology solutions to secure buy-in from physicians. Leaving information technology aside, one interviewee felt that evaluation tools such as patient satisfaction surveys, staff satisfaction surveys and case-cost comparisons were useful.
It is revealing that federal/provincial respondents exhibited complete ignorance of the tools used by HCOs. Only one federal/provincial respondent mentioned those tools at all: "For example, the Kingston General Hospital has a database that captures all surgery" (FPR). In contrast, all organizational-level respondents spoke of tools as essential.
Contextual-level factors
GOVERNANCE FACTORS
While governance-related issues were identified as an important contextual factor in 10 of 17 interviews, the importance that respondents accorded governance in the implementation of WTMS depended on whether the respondent hailed from the federal/provincial level or from the organizational level (HCOs). Only four of nine organizational-level respondents felt that contextual-level governance (i.e., the governance of Canada's healthcare system overall) was a significant factor. These respondents cited provincial health ministries' creation of a committee (BC) and of a network (ON) as the element that brought stakeholders together: "The provincial spotlight on wait times gave credibility to the project" (HOR). Similarly, an organizational-level respondent described how the centralization of general surgery referrals in Manitoba was temporarily abandoned after higher-level authorities failed to make it a priority. In contrast to this weak showing among organizational-level respondents, all federal/provincial respondents regarded contextual-level governance as essential. Successful initiatives, they claimed, had two characteristics: (1) they had been prioritized by political and administrative stakeholders (i.e., government, physicians' representatives and organizations' top management) and (2) they had experienced strong collaboration among all parties: "You need allies in all the different groups, at all the different levels" (FPR).
In Ontario, for example, one initiative succeeded after its implementation strategy had been made a priority for stakeholders from both federal/provincial and organizational levels, and organizational proactivity had been encouraged by Ontario's Innovation Fund. Conversely, local initiatives faced challenges when unsupported by provincial policy (see MB example, above). Four federal/provincial-level respondents also felt that a neutral committee (AB) or a neutral and respectful person in a leadership position (ON, SK) enhanced collaboration: "They are outside players that help the process" (FPR); "I see myself as a broker" (HOR). In a number of top-down initiatives, the credibility of the leader or that of the structure established to launch the strategy was another key factor. For example, Ontario respondents systematically acknowledged the role of the leader of the Ontario Wait Times Strategy, whose clinical and administrative experience gave him credibility at the same time that his independence from government and hospitals caused him to appear objective.
CULTURAL FACTORS
Eight interviewees cited the culture of Canada's healthcare system as a key contextual-level factor. One physician suggested that "a fee-for-service model is a major cultural impediment to moving forward. Every action affects physicians' income" (HOR). With respect to provincial initiatives, participants hailing mainly from the federal/provincial level emphasized the benefits of a participative approach and the development of a culture of evaluation, communication or rapid decision-making about WTMS in order to publicize progress made. All Ontario interviewees esteemed a culture of accountability, and one mentioned sustainability: "If many … initiatives fail, it is because they don't build a sustainability culture" (FPR). Participants talking about provincial initiatives also emphasized the benefits of communicating with the public about wait time durations (to increase accountability) and about wait time strategies (to publicize progress made). In terms of negative cultural factors, three organizational-level interviewees mentioned a history of adversity among stakeholders and a context of mistrust between hospitals and the ministry of health: "The most important obstacle to change is culture, the culture of opposition within the healthcare system" (FPR).
RESOURCE FACTORS
Eight participants pointed out that financial resources were a necessary success factor, but that financial incentives had to be carefully planned, aligned and linked to efficiencies – for example, "special funds were dedicated to help physicians field the data" (FPR). Respondents also highlighted disincentives such as global budgets and the unavailability of overtime salary, and mentioned that national- and provincial-level strategies implemented at the local level required significant financial resources in order to secure stakeholder participation. Two federal/provincial-level participants also referred to human resources shortages in Canada, and six organizational-level participants spoke of operating capacity: "There are real limitations with operating room space and the hours available for operations" (HOR).
TOOL FACTORS
The tools cited by our respondents were mainly used to collect data and follow or rank patients. For example, one respondent mentioned Quebec's System to Manage Access to Care, which helps Quebec organizations rank the weight and urgency of cases in tertiary cardiology and radio-oncology.
Discussion: Balancing Governance, Culture, Resources and Tools
Achieving a balance between supportive resources and tools and an effective management system is a challenge for any WTMS and a key to the strategy's success. The findings of this study point to several key lessons whose importance is underlined by the fact that they are echoed in the evidence from the literature. Looking at organizational-level factors, we can say that where cultural factors are concerned, involving physicians from the outset is key. Using clinical leaders to get other doctors on board is an essential cultural success factor. Physicians' attention needs to be drawn to how the WTMS will improve their practice and help them provide better care. Studies have systematically found that involving physicians early facilitates the implementation and diffusion of WTMS down the road (Appleby et al. 2004; Glynn 2006; Frank et al. 2006). But at the same time, physicians need managers to help them redesign the patient pathway. Mobilizing a clinical governance model (Pomey et al. 2008) that shares responsibility between physicians and managers allows the parties to align their objectives. However, the relationship between the world of management and the world of practice is often characterized by conflict (Appleby et al. 2004). Furthermore, physicians are often active participants in access management strategies but are excluded from the decision-making process (Glynn 2006). In addition, an organizational culture open to innovation and teamwork (Frank et al. 2006) is more inclined to implement successful WTMS. Such strategies require that problems be met with collaborative solutions and not blame, and can achieve their full potential only when there is collaboration between HCOs and higher levels, as noted in the reports of Appleby and colleagues (2004).
A WTMS can been seen as a quality management process and in consequence needs to mobilize quality methods and professional expertise (McNulty and Ferlie 2002; Ham et al. 2003; Rachlis 2005). Different strategies have been implemented and can mobilize operations research (Patrick and Puterman 2008; Walley et al. 2006), priority scoring systems (Noseworthy et al. 2003) and guidelines (McGurran et al. 2002; WCWL 2008). Managers play an important role in helping evaluate the impacts and in adopting an open management style that develops staff and engages them in quality enhancement activities (Walley et al. 2006; McLeod et al. 2003; ACAHO 2006). The ability to monitor the impact of the strategies requires an investment in an information management system (Vanostenberg 2006). Data collection keeps actors accountable, and has to be considered as a normal part of doing business. Data collection also results in transparency, which facilitates discussion and improves collaboration among stakeholders both upstream and downstream from HCOs (Federal Advisor on Wait Times 2006; Collins-Nakaï et al. 2006). As part of the quality enhancement process, an evaluation of the impact of WTMS on other initiatives and procedures has to be taken into account (Carruthers 2006).
In addition, we saw in our interviews that it is difficult to launch a WTMS without earmarked funds (Bellan 2004). Seed money helps to smooth the introduction of sometimes difficult changes (Greenhalgh et al. 2004; Baker and Schwartz 2005; Pearson and Meyer 1996). Finally, the alignment between high-level policies and local strategies is essential and rarely discussed in the literature. It is in the top-down initiative's interests to take organizational constraints into account (Frank et al. 2006); a third party—an independent organization, for example—can work with the organization to alleviate or address obstacles and facilitate implementation.
Conclusion
These reflections are the fruit of the experience of expert Canadians working at different levels of the healthcare system. They constitute the strength of this study, the first to plumb seasoned viewpoints of the factors that promote or inhibit the implementation of WTMS. Furthermore, this is the first time that these factors have been grouped in a landscape that includes not only federal/provincial strategies but also, critically, organizational strategies, and considers how these strategies interact. This exercise has allowed us to discern the synergy between different levels of decision-making and to grasp the importance of considering those levels simultaneously. It also makes our analytical model of great use to those involved in WTMS: for the first time, managers and policy makers have at their disposal a tool that includes all principal factors and demonstrates their interdependence. As complex as this may seem, improving patients' access to appropriate and timely care is "worth the wait."
Les stratégies contre les temps d'attente pour les soins électifs : qu'est ce qui fait leur succès?
Résumé
Contexte : Cette étude porte sur la perception d'experts sur les facteurs, au niveau local ou contextuel, qui favorisent ou empêchent l'implantation de stratégies contre les temps d'attente dans les établissements de santé au Canada.
Méthodes : Nous avons réalisé 16 entretiens semi-structurés et un groupe de discussion avec des personnes sélectionnées par leur implication aux niveaux fédéral et provincial, ou au niveau des établissements de santé (ES), dans la mise en œuvre de stratégies contre les temps d'attente.
Résultats : Le facteur le plus souvent cité a été celui de la participation des médecins au niveau des ES. Nous avons trouvé qu'un fort leadership médical dans un ES permettait de faire participer les autres médecins à la mise en œuvre d'une stratégie. Cependant pour être efficace, ce leadership doit être aidé par les gestionnaires. La congruence des incitatifs financiers aux niveaux local et contextuel est aussi un autre facteur souvent cité. Les interviewés ont aussi mis en évidence l'importance des outils qui aident à redessiner, suivre, évaluer et prioriser les stratégies contre les temps d'attente.
Conclusions : Ces résultats permettent de mettre en tension la nécessité non seulement d'avoir des ressources et des outils mais aussi d'avoir une culture et une gestion adéquate, ce qui est souvent difficile à réaliser. La capacité d'arriver à cet équilibre permet de réconcilier des initiatives qui peuvent être locales ou contextuelles.
About the Author(s)
Marie-Pascale Pomey, MD, PHD, Associate Professor, Department of Health Administration, Groupe de recherche et d'intervention sociale de Montréal (GRIS), Faculty of Medicine, University of Montreal, Montreal, QC
Pierre-Gerlier Forest, PHD, President, Trudeau Foundation, Montreal, Adjunct Professor, University of Montreal, Montreal, QC
Claudia Sanmartin, PHD, Statistics Canada and University of Calgary, Calgary, AB
Carolyn De Coster, RN, PHD, Senior Researcher, Calgary Health Region, Assistant Professor, Department of Community Health Sciences, University of Manitoba, Winnipeg, MB
Madeleine Drew, MHA, School of Management, University of Ottawa, Ottawa, ON
Correspondence may be directed to: Marie-Pascale Pomey, MD, PhD, Associate Professor, Department of Health Administration, GRIS, Faculty of Medicine, University of Montreal, CP 6128, Succ. Centre Ville, Montreal, QC H3C 3J7; tel.: 514-343-6111, ext. 1-1364; fax: 514-343-2448; e-mail: marie-pascale.pomey@umontreal.ca.
Acknowledgment
This research was supported by the Canadian Institutes of Health Research grant #KSY-73928. Marie-Pascale Pomey is supported in part by career awards from the Canadian Institutes of Health Research. We would like to thank the interview participants for having contributed their experience and insights. We would also like to thank Jennifer Petrela for her editorial contribution.
References
Appleby J., S. Boyle, N. Devlin, M. Harley, A. Harrison, L. Locock and R. Thorlby. 2004. Sustaining Reductions in Waiting Times: Identifying Successful Strategies. Final report to the Department of Health. London: King's Fund. Retrieved January 5, 2010. <http://www.library.nhs.uk/HealthManagement/ViewResource.aspx?resID=70785>.
Association of Canadian Academic Healthcare Organizations (ACAHO). 2006 (March). Wait Watchers II: Measuring Progress of Wait Time Management Strategies across ACAHO Members. An ACAHO Member Survey. Ottawa: Author. Retrieved January 5, 2010. <http://www.acaho.org/docs/pdf_2006_wait_watchers_II_final_report.pdf>
Baker, G.R. and F. Schwartz. 2005. "Innovation and Access to Cancer Care Services in Ontario." Healthcare Quarterly 8(2 Suppl.): 2–12.
Bellan, L. 2004. "The Impact of Allocation of Additional Resources on the Waiting Time for Cataract Surgery." Healthcare Quarterly 7(4): 54–56.
Canadian Policy Research Network (CPRN). 2009. Waiting List Management (Taming of the Queue). Retrieved January 5, 2010. <http://www.cprn.org/theme.cfm?theme=43&l=en>.
Carruthers, C. 2006. "Sustaining the Wait Time Strategy." HealthcarePapers 7(1): 51–54.
Collins-Nakaï, R., O. Adams and M. Saulnier. 2006. "A Prescription for Ontario's Wait Time Strategy." HealthcarePapers 7(1): 46–50.
Federal Advisor on Wait Times. 2006. Final Report of the Federal Advisor on Wait Times. Ottawa: Health Canada.
Ferlie, E.B. and S.M. Shortell. 2001. "Improving the Quality of Health Care in the United Kingdom and the United States: A Framework for Change." Milbank Quarterly 7(2): 281–315.
Frank, C., D. Dick, D. Smith, T. Wasylak, K. Gooch and R. Zernicke. 2006. "The Alberta Bone and Joint Health Institute: Creating Sustainable Accountability through Collaboration, Relevant Measurement and Timely Feedback." HealthcarePapers 7(1): 34–39.
Glynn, P.A. 2006. "Sustaining Change: The Imperative for Patient Access Strategies." HealthcarePapers 7(1): 55–57.
Greenhalgh, T., G. Robert, F. Macfarlane, P. Bate and O. Kyriakidou. 2004. "Diffusion of Innovations in Service Organizations: Systematic Review and Recommendations." Milbank Quarterly 82(4): 581–629.
Ham, C., R. Kipping and H. McLeod. 2003. "Redesigning Work Processes in Health Care: Lessons from the National Health Service." Milbank Quarterly 81(3): 415–39.
Hatchuel, A. 2000. Prospective et gouvernance : quelle théorie de l'action collective ? In E. Heurgon and J. Landrieu, eds., Prospective pour une gouvernance démocratique (pp. 29–42). La Tour d'Aigues, France: Éditions de l'Aube.
Health Canada. 2004. First Ministers' Meeting on the Future of Health Care. A 10-Year Plan to Strengthen Health Care. Retrieved January 5, 2010. <http://www.hc-sc.gc.ca/hcs-sss/delivery-prestation/fptcollab/2004-fmm-rpm/index_e.html>.
Health Council of Canada. 2007. Wading through Wait Times: What Do Meaningful Reductions and Guarantees Mean? Retrieved January 5, 2010. <http://healthcouncilcanada.ca/en/index.php?option=com_content&task=view&id=202&Itemid=10>.
McGurran, J., T. Noseworthy and the Steering Committee of the Western Canada Waiting List Project. 2002 (Spring). "Improving the Management of Waiting Lists for Elective Healthcare Services: Public Perspectives on Proposed Solutions." Hospital Quarterly 5(3): 28–32. Retrieved January 5, 2010. <http://www.wcwl.org/media/pdf/library/published_papers.5.pdf>.
McLeod, H., C. Ham and R. Kipping. 2003. "Booking Patients for Hospital Admissions: Evaluation of a Pilot Programme for Day Cases." British Medical Journal 327: 1147–50.
McNulty, T. and E. Ferlie. 2002. Reengineering Health Care. The Complexities of Organizational Transformation. Oxford: Oxford University Press.
Noseworthy, T.W., J.J. McGurran, D.C. Hadorn and the Steering Committee of the Western Canada Waiting List Project. 2003. "Waiting for Scheduled Services in Canada; Development of Priority-Setting Scoring Systems." Journal of Evaluative Clinical Practice 9: 23–31.
Parsons, T. 1977. Social Systems and the Evolution of Action Theory. New York: Free Press.
Patrick, J. and M.L. Puterman. 2008. "Reducing Wait Times through Operations Research: Optimizing the Use of Surge Capacity." Healthcare Policy 3(3): 75–88.
Pearson, K. and H. Meyer. 1996. "Wait Times: The Search for Equitable Solutions." Australian Health Review 9(4): 93–99.
Pomey, M.-P., J.-L. Denis and A.-P. Contandriopoulos. 2008. "Un cadre conceptuel d'analyse de la gouvernance clinique dans les établissements de santé." Pratiques et Organisations des Soins 39(3): 183–94. Retrieved January 5, 2010. <http://www.ameli.fr/l-assurance-maladie/statistiques-et-publications/la-revue-pratiques-et-organisation-des-soins/les-articles-de-la-revue/pratiques-et-organisation-des-soins-2008-n-3/sommaire-du-numero-3-2008.php>.
Prime Minister of Canada. 2007 (April 4). "Canada's New Government Announces Patient Wait Times Guarantees." Retrieved January 5, 2010. <http://pm.gc.ca/eng/media.asp?id=1611>.
Rachlis, M. 2005. "Public Solutions to Health Care Wait Lists." Ottawa: Canadian Centre for Policy Alternatives. Retrieved January 5, 2010. <http://www.policyalternatives.ca/publications/commentary/public-solutions-health-care-wait-lists>.
Shortell, S.M., J.L. Levin, J.L. O'Brien and E.F. Hughes. 1995. "Assessing the Evidence of CQI: Is the Glass Half Empty or Half Full?" Hospital & Health Services Administration 40(1): 4–24.
Siciliani, L. and J. Hurst. 2003. "Tackling Excessive Wait Times for Elective Surgery: A Comparative Analysis of Policies in 12 OECD Countries." Health Policy 572(2): 201–15.
Supreme Court of Canada (SCC). 2005 (June 9). Chaoulli v. Quebec (Attorney General), 2005 SCC 35, [2005] 1 SCR 791. Retrieved January 5, 2010. <http://scc.lexum.umontreal.ca/en/2005/2005scc35/2005scc35.html>.
Trypuc, J., A. Hudson and H. Macleod. 2006. "Ontario's Wait Time Strategy: Part 1." Healthcare Quarterly 9(2): 44–51.
Trypuc, J., H. MacLeod and A. Hudson. 2006. "Developing a Culture to Sustain Ontario's Wait Time Strategy." HealthcarePapers 7(1): 8–24.
Vanostenberg, P. 2006. "Quality Measurement across Borders: Need and Options." World Hospital Health Services 42(1): 19–22.
Walley, P., K. Silvester and R. Steyn. 2006. "Knowledge and Behaviour for a Sustainable Improvement Culture." Healthcare Quarterly 7(1): 26–33.
Western Canada Waiting List (WCWL) Project. 2008. List of Published Papers. Retrieved January 5, 2010. <http://www.wcwl.org/library/published_papers/?id=published_papers.5>.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed