Healthcare Quarterly
New Mental Health Indicators Provide a Snapshot on Performance of the Mental Health System in Canada
Abstract
Although the general hospital remains an important place for stabilizing crises, most services for mental illnesses are provided in outpatient/community settings. In the absence of comprehensive data at the community level, data that are routinely collected from general hospitals can provide insights on the performance of mental health services for people living with mental illness or poor mental health. This article describes three new indicators that provide a snapshot on the performance of the mental health system in Canada: self-injury hospitalization rate, 30-day readmission rate for mental illness and percentage of patients with repeat hospitalizations for mental illness. Findings suggest a need for the early detection and treatment of mental illnesses and for optimal transitions between general hospitals and community services.
In Canada, as in many countries, mental illnesses are among the 20 leading causes of disability (World Health Organization 2008) and are associated with death by suicide (Public Health Agency of Canada [PHAC] et al. 2006). Mental illnesses often persist over time, and they affect people of all cultures and socio-economic statuses (Mental Health Commission of Canada 2009; PHAC 2006). They are also costly to the health system. In 2006, the economic burden of mental illnesses in Canada was estimated to be $52 billion, when taking into account the costs associated with the reduction in health-related quality of life, loss of productivity in the workplace and direct costs of mental health services and supports (Institute of Health Economics 2008).
In recent years, there have been calls for more information on mental health to inform the planning, management and evaluation of the mental health system (Canadian Institute for Health Information [CIHI] 2009; Kirby and Keon 2006; World Health Organization 2001). In response, CIHI developed new indicators related to mental health services to provide insight into the performance of the mental health system in Canada. Although these indicators are based on data from general hospitals, they can be interpreted as being closely related to outcomes associated with effective community-based care and supports in both treating persons age 15 years and older who are living with mental illnesses and in reducing unnecessary or avoidable hospitalizations.
This article describes the three new indicators: self-injury hospitalization rate, 30-day readmission rate for mental illness and percentage of patients with repeat hospitalizations for mental illness, and it summarizes the more detailed findings presented in Health Indicators 2011 (CIHI 2011).
Study Population
The population studied included Canadian residents age 15 years and older who were hospitalized in a general hospital for a mental illness or self-injury. (General hospital excludes all free-standing psychiatric institutions. See Health Indicators 2011 [CIHI 2011] for more details.) Mental illness was identified as the most responsible diagnosis upon discharge and included substance-related disorders, schizophrenia, mood disorders, anxiety disorders and personality disorders. Self-injury was identified as having a diagnosis code of intentional external cause of injury, regardless of whether a mental illness was recorded on the discharge. Data were from CIHI's Discharge Abstract Database (DAD), the Ontario Mental Health Reporting System, the National Ambulatory Care Reporting System and Fichier des hospitalisations MED-ÉCHO, ministère de la Santé et des Services sociaux du Québec. All records were selected based on the discharge date.
More details about the methodology used can be found at www.cihi.ca.
Methods
The self-injury hospitalization rate is a partial measure of the extent to which community-based services are accessible and effective in minimizing self-injury. Self-injury can be the result of suicidal or self-harming behaviours, or both. Hospitalization rates are expressed per 100,000 population and are age standardized to the 1991 Canadian population.
The 30-day mental illness readmission rate is a measure that reflects the coordination and continuity of services in the mental health system. It is the proportion of hospitalizations for mental illness that are readmitted to hospital within 30 days of the previous hospitalization for mental illness. (Hospitalizations are episodes of care, which include the first hospitalization to a general hospital and all consecutive transfers to other general hospitals.) Rates are risk-adjusted for age, sex, type of mental illness, being discharged against medical advice and having prior multiple hospitalizations for mental illness (all related to the initial hospitalization).
The percentage of repeat hospitalizations for mental illness is a proxy measure of the extent to which individuals are able to use and have access to appropriate community-based services. It is calculated as the number of individuals with three or more hospitalizations for mental illness over a one-year follow-up period, divided by the number of individuals with at least one hospitalization for mental illness during a given fiscal year. Results are risk adjusted for age, sex, type of mental illness and being discharged against medical advice (all related to the initial hospitalization).
Findings
Self-Injury Hospitalization Rate
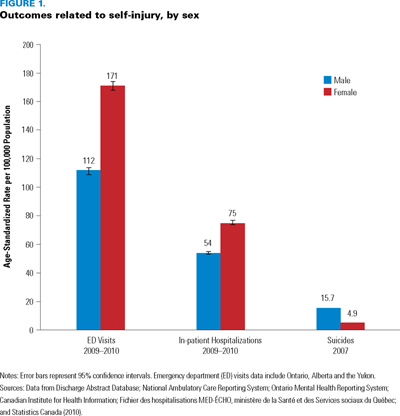
In 2009–2010, the self-injury hospitalization rate for Canada was 65 per 100,000 population (17,482 hospitalizations). About 70% of hospitalizations for self-injury included at least one diagnosis code for mental illness. Females had more emergency department visits and in-patient hospitalizations as a result of self-injury; however, data from Statistics Canada show that males are far more likely to die as a result of self-injury (Figure 1). Young women aged 15–19 were the most likely to be hospitalized for self-injury and had more than twice the rate for males of the same age (145 per 100,000 versus 61 per 100,000).
Thirty-Day Mental Illness Readmission Rate
In 2009–2010, 11.4% of hospitalizations for mental illnesses were followed by a readmission within 30 days (12,618 hospitalizations); 41% of readmissions occurred within seven days and 64% occurred within 14 days. In the risk-adjusted model, the strongest factors associated with a higher risk of readmission within 30 days (all for the initial hospitalization) were (1) being 20–34 years old (odds ratio [OR] 1.25, 95% confidence interval [CI] 1.15–1.36); (2) having a personality disorder (OR 1.18, 95% CI 1.08–1.28) or schizophrenia (OR 1.18, 95% CI 1.12–1.24); (3) having multiple prior hospitalizations (OR 3.14, 95% CI 3.01–3.28); and (4) being discharged against medical advice (OR 2.32, 95% CI 2.18–2.46).
Percentage of Repeat Hospitalizations for Mental Illness
In 2008–2009, 11% of all people hospitalized for mental illness were hospitalized at least three times over a one-year follow-up period (10,004 individuals). This represented 28% of all hospitalizations and 27% of the total number of patient days for these mental illnesses. In the risk-adjusted model, the strongest factors associated with having repeat hospitalizations for mental illness (all for the initial hospitalization) were (1) being 21–50 years old (OR 1.98, 95% CI 1.82–2.16); (2) having schizophrenia (OR 2.73, 95% CI 2.52–2.96); and (3) being discharged against medical advice(OR 1.52, 95% CI 1.40–1.64).
Discussion
This analysis showed that people in Canada use general hospitals for treatment and support related to mental illness. While not all self-injury hospitalizations could be linked to mental illness, 70% were, implying the need for early detection and treatment of mental illnesses. Almost two thirds of 30-day readmissions occurred within two weeks, suggesting opportunities for better coordination of services between hospital and community and among multiple service settings. Furthermore, over one in ten people hospitalized for mental illness are admitted to the hospital at least three times in one year. Not all hospitalizations are preventable; but having appropriate and accessible community services could reduce rates, improve clinical outcomes and, ultimately, affect the social functioning of individuals living with mental illnesses.
This analysis included only data from general hospitals, so it provides a partial view of hospital use for mental health issues in an acute setting. Identifying consensus descriptions for levels of care in hospitals across Canada would be helpful in this regard. Additionally, the ability to link data that are related to services received in both hospital and community settings would be important. More data are needed for further assessment.
These indicators provide a starting point for a discussion about measuring and improving mental health services in Canada. Regular reporting of these indicators can be useful to inform the planning, management and evaluation of the mental health system.
About the Author(s)
Carolyn Sandoval, MSc, was a project lead with the Health Indicators team at the Canadian Institute for Health Information (CIHI), in Toronto, Ontario until 2012. Carolyn has been involved in health indicator development and dissemination at CIHI since 2003.
Chantal Couris, MSc, PhD, is the manager of the Health Indicators team at CIHI, in Toronto. Chantal has extensive research experience using administrative data to promote quality of care and quality health policy decision-making.
Kira Leeb is the director of the Health System Performance branch at CIHI, in Toronto. Kira has been involved in many health services research reports since beginning her tenure at CIHI in 2000.
Acknowledgment
We thank Yue You, Jun Liang, Ling Yin and Kathy Nguyen, from the Health Indicators team at CIHI, for performing the analyses.
References
Canadian Institute for Health Information. 2009. Report from the Third Consensus Conference on Health Indicators. Ottawa, ON: Author.
Canadian Institute for Health Information. 2011. Health Indicators 2011. Ottawa, ON: Author.
Institute of Health Economics. 2008. How Much Should We Spend on Mental Health? Edmonton, AB: Author.
Kirby, M.J.L. and W.J. Keon. 2006. Out of the Shadows at Last: Transforming Mental Health, Mental Illness and Addiction Services in Canada. Ottawa, ON: Senate of Canada.
Mental Health Commission of Canada. 2009. Toward Recovery and Well-Being: A Framework for a Mental Health Strategy for Canada. Ottawa, ON: Author.
Public Health Agency of Canada, Mood Disorders Society of Canada, Health Canada, Statistics Canada and the Canadian Institute for Health Information. 2006. The Human Face of Mental Health and Mental Illness in Canada, 2006. Ottawa, ON: Minister of Public Works and Government Services Canada.
Statistics Canada. 2010. Deaths and Mortality Rate, by Selected Grouped Causes, Age Group and Sex, Canada, Annual. Ottawa, ON: Author. Retrieved March 9, 2011. <http://www5.statcan.gc.ca/cansim/pick-choisir?lang=eng&id=1020551&pattern=1020551&searchTypeByValue=1>.
World Health Organization. 2001. The World Health Report 2001: Mental Health: New Understanding, New Hope. Geneva, Switzerland: Author.
World Health Organization. 2008. The Global Burden of Disease: 2004 Update. Geneva, Switzerland: Author.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed