Healthcare Quarterly
Seniors and Alternative Level of Care: Building on Our Knowledge
Abstract
There is ongoing concern that acute care beds in Canada are occupied by seniors who are waiting to be discharged to a more appropriate level of care. These individuals, who no longer require acute care services, are commonly designated as alternative level of care (ALC) patients. In this study, the authors examined the characteristics of patients transitioning from acute care to home care or residential care.
 There is ongoing concern that acute care beds in Canada are occupied by seniors who are waiting to be discharged to a more appropriate level of care (ALC Expert Panel 2006). These individuals, who no longer require acute care services, are commonly designated as alternative level of care (ALC) patients.
There is ongoing concern that acute care beds in Canada are occupied by seniors who are waiting to be discharged to a more appropriate level of care (ALC Expert Panel 2006). These individuals, who no longer require acute care services, are commonly designated as alternative level of care (ALC) patients.
ALC is an important challenge for individuals and for the health system (Ontario Association of Community Care Access Centres 2006). Seniors awaiting placement may experience a decline in their overall health and well-being (Covinsky et al. 2003; Graf 2006). Traditionally, people have viewed this issue as one resulting from persons waiting for placement in residential care. However, there has been a recent shift in thinking to focus on increasing the capacity of the community care sector to meet these needs (LHIN Collaborative 2011). Health planners and policy makers are interested in understanding the transitions of people between hospitals and other sectors of the healthcare system in order to explore the potential to divert demand from residential care to home care settings.
The majority of seniors want to remain at home, and evidence suggests that providing care at home is a cost-effective alternative (Weissert et al. 2003). Projections show that the proportion of seniors in Canada's population will nearly double in the next few decades, from 15% in 2011 to 25% in 2036 (Statistics Canada 2010); the number of ALC patients is therefore expected to increase as well (Walker 2011). This shifting demographic may increase the pressure on both acute care and residential care facilities unless demands can be shifted to other community-based settings to help address the ALC challenge (Walker 2011).
In this article, we briefly discuss the findings of a study that we performed to examine the characteristics of patients transitioning from acute care to home care or residential care.
Data Sources and Methods
The study linked data from the Canadian Institute for Health Information (CIHI) Continuing Care Reporting System, Home Care Reporting System and Discharge Abstract Database for four fiscal years, 2007–2008 through to 2010–2011. The data for this report focused on newly admitted long-stay home care clients and residential care clients, age 65 years and older, who had been discharged from an acute care facility between April 2007 and September 2011.
The final linked dataset included 90,507 transitions from acute care to either home care (61,047 in Nova Scotia, Ontario and Yukon) or residential care facilities (29,460 in British Columbia, Manitoba [Winnipeg Regional Health Authority], Newfoundland and Labrador, Ontario and Yukon).
Findings
As expected, the majority of transitions found in this analysis were from acute care to home care. However, ALC days were much more common in transitions to residential care. A greater proportion of clients recently admitted to residential care (four in five) had ALC days as compared with recently admitted long-stay home care clients (one in five). In addition, seniors waiting for discharge to residential care waited much longer (26 days compared with seven days for those discharged to home care).
Multiple factors were associated with ALC status among persons discharged from acute care. Logistic regression models were developed to determine the combination of factors that best predicted the presence of ALC days in the populations transitioning home and to residential care.
Predicting ALC Days among Persons Admitted to Home Care
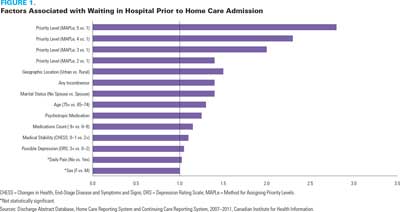
The results of the logistic regression for persons admitted to home care are shown in Figure 1. The Method for Assigning Priority Levels (MAPLe) algorithm (Hirdes et al. 2008) identifies people more likely to have a distressed caregiver and to enter residential care. After controlling for other factors, the odds of having ALC days were almost three times higher for persons with a very high MAPLe score than for persons with a low MAPLe score. This suggests that persons at higher risk of caregiver distress and institutionalization are more likely to have ALC days prior to home care admission while waiting for adequate supports to be put in place at home.
Factors associated with having ALC days extend beyond the clinical characteristics of the individual. For example, both geographical location (urban) and marital status (no spouse) are related to waiting in hospital prior to discharge.
Predicting ALC Days among Persons Admitted to Residential Care
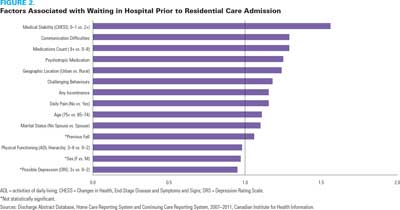
Medical stability, as measured by the Changes in Health, End-Stage Disease and Symptoms and Signs (CHESS) scale (Hirdes et al. 2003), was the strongest predictor of ALC days among those admitted to residential care (Figure 2). This may suggest challenges around residential care admission practices. After controlling for other factors, the odds of having ALC days in acute care (versus having no ALC days) were one and a half times higher for persons who were medically stable (lower CHESS scores) than for persons with moderate to severe medical instability. Consistent with the literature, dementia-type symptoms such as challenging behaviours and communication difficulties were also strong predictors of ALC days.
The odds of having ALC days were higher for persons taking greater than nine medications, or those taking one or more psychotropic medications. These findings suggest that persons who require considerable medication monitoring are more likely to wait prior to admission to residential care.
Discussion
The data presented in this report shed light on the growing ALC challenge in Canada's healthcare system. The models presented account for many of the clinical differences between seniors with and without ALC days. However, given that the presence of ALC days is not well explained by clinical differences, health system–level factors may be important in shedding light on delayed transitions to the community, particularly for those going to residential care. For example, there are differences in the availability of and admission policies to residential care beds, as well as the availability of alternative discharge settings within and between jurisdictions (Penney and Henry 2008). The resources that have been allocated to home support services and the programs put in place to support informal caregivers vary widely and may have a significant effect on policies and decisions related to discharge planning (Weissert et al. 2003).
This analysis also identified a subgroup of clients – those who were medically stable and had symptoms associated with dementia – who were more likely to wait before being admitted to residential care. The needs of these individuals may require further consideration in order to facilitate transition out of acute care, and have been noted in recent initiatives in a number of provinces to allocate resources to behavioural support or other specialized care (Ontario Local Health Integration Network 2012).
It is well documented in the literature that waiting in an acute care bed for placement may lead to a decline in the health of the individual (Covinsky et al. 2003; Graf 2006). Waiting is also very costly and resource-intensive for the healthcare system since a bed is being occupied by a person who no longer requires acute services (Walker 2011). Facilitating a successful transition home, or to another community setting, requires careful consideration of resource availability, costs, risks and benefits to the individual and the health system as a whole.
These findings and others are described in detail in a recent CIHI publication, Seniors and Alternate Level of Care: Building on our Knowledge (2012). This report is available free of charge at www.cihi.ca.
About the Author(s)
Norma Jutan, PhD, is a senior analyst on the Home and Continuing Care team at Canadian Institute for Health Information (CIHI). She supports health system decision-making through training and analyses focusing on emerging issues in the healthcare system.
Lacey Langlois, MSc, is a team lead on the Home and Continuing Care team at CIHI. She leads analytical and reporting activities related to home and continuing care.
Natalie Damiano, PT, MSc, is the manager for Integrated eReporting at CIHI. At the time of this writing, she was the Manager for Home and Continuing Care Data Management and was responsible for managing all activities related to home and continuing care data, analysis and reporting, as well as stakeholder engagement to support the uptake and use of data.
References
ALC Expert Panel. 2006. Appropriate Level of Care: A Patient Flow, System Integration and Capacity Solution. Ministry of Health and Long-Term Care. Retrieved November, 2012. <Link>.
Canadian Institute for Health Information. 2012. Seniors and Alternate Level of Care: Building on our Knowledge. Ottawa, ON: Author.
Covinsky, K.E., R.M. Palmer, R.H. Fortinsky, S.R. Counsell, A.L. Stewart, D. Kresevic et al. 2003. "Loss of Independence in Activities of Daily Living in Older Adults Hospitalized with Medical Illnesses: Increased Vulnerability with Age." Journal of the American Geriatrics Society 54: 451–58.
Graf, C. 2006. "Functional Decline in Hospitalized Older Adults." American Journal of Nursing 106: 58–67.
Hirdes, J.P., D.H. Frijters and G.F. Teare. 2003. "The MDS-CHESS Scale: A New Measure to Predict Mortality in Institutionalized Older People." Journal of the American Geriatrics Society 51: 96–100.
Hirdes, J.P., J. Poss and N. Curtin-Telegdi. 2008. "The Method for Assigning Priority Levels (MAPLe): A New Decision-Support System for Allocating Home Care Resources." BMC Medicine 6: 9.
LHIN Collaborative. 2011. Home First: Implementation Guide and Toolkit. Toronto, ON: Author.
LHIN Collaborative. 2006. Alternate Level of Care – Challenges and Opportunities. Toronto, ON: Author. Ontario Local Health Integration Network. 2012. Behavioural Supports Ontario. Retrieved November, 2012. <http://www.akeresourcecentre.org/BSO>.
Penney, C. and E. Henry. 2008. "Improving Performance Management for Delivering Appropriate Care for Patients No Longer Needing Acute Hospital Care." Journal of Health Services Research and Policy 13(Suppl. 1): 30–34.
Statistics Canada. 2010. Population Projections for Canada, Provinces and Territories (Catalogue No. 91-520-XWE). Ottawa, ON: Author.
Walker, D. 2011. Caring for Our Aging Population and Addressing Alternate Level of Care. Toronto, ON: Ontario Ministry of Health and Long-Term Care.
Weissert, W., M. Chernew and R. Hirth. 2003. "Titrating versus Targeting Home Care Services to Frail Elderly Clients: An Application of Agency Theory and Cost-Benefit Analysis to Home Care Policy." Journal of Aging and Health 15: 99–123.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed