Healthcare Quarterly
Primary Prevention - Recent Developments in Policy and Support
Mary Spayne, Linda Rabeneck, Loraine Marrett and Alice Peter
Abstract
The focus of Cancer Care Ontario (CCO)'s renewed prevention strategy is to provide evidence-based support and policy advice for risk factor reduction and cancer prevention. As cancer shares several key modifiable risk factors with other major chronic diseases, CCO's prevention efforts also benefit the goals of chronic disease prevention. CCO's ability to successfully provide policy advice is dependent on timing and the ability to respond to current and emerging policy and legislative issues.
| LIST OF ACRONYMS | |
| Acronym | Description |
| CCO | Cancer Care Ontario |
| RCCs | Regional Cancer Centres |
| MOHLTC | Ministry of Health and Long-Term Care |
| PTCC | Program Training and Consultation Centre |
| CoP | Communities of practice |
| PSQI | Prevention System Quality Index |
| CSQI | Cancer System Quality Index |
Background
Primary prevention, which focuses on reducing exposure to risk factors and targets the well population before they are diagnosed with cancer, is an essential component of a cancer control strategy. Cancer shares several key modifiable risk factors – meaning that they can be affected by intervention or behaviour change – with other major chronic diseases including cardiovascular disease, chronic respiratory disease and diabetes. Because of this overlap, prevention initiatives at Cancer Care Ontario (CCO) also benefit the goals of chronic disease prevention.
Ideally, prevention activities are embedded throughout the cancer system and are reflected in the operations of Regional Cancer Programs and in efforts to drive quality improvement and health-system sustainability. Key to CCO's primary prevention role is its ability to provide scientific, evidence-based advice to support the effective development and implementation of policy, leading to initiatives that promote action on prevention, increase the effectiveness of the prevention system and work towards health equity. CCO's capacity to generate new knowledge, interpret and summarize existing evidence and measure and report on progress in risk factor reduction is central to its strategic approach.
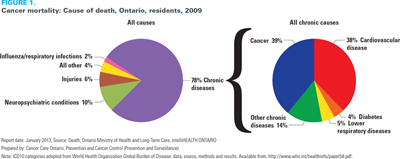
Cancer and other chronic diseases are common in Ontario, as they are in other provinces and around the world; cancer and cardiovascular disease together account for almost 80% of deaths in Ontario (Figure 1). In addition to causing premature death and affecting quality of life, cancer and chronic diseases also place a heavy burden on the healthcare system and increase health disparity (World Health Organization 2008).
Four key modifiable risk factors in the development of cancer are shared by other major chronic diseases – tobacco use, alcohol consumption, physical inactivity and unhealthy eating. A significant number of Ontarians engage in these behaviours or activities – 20% of Ontario adults smoke, 53% are overweight or obese, 9% drink alcohol in excess of cancer prevention recommendations, close to half are physically inactive or spend many of their leisure hours on the computer or watching television and almost two-thirds of Ontario adults consume fruit and vegetables less than five times per day (Cancer Quality Council of Ontario 2014).
Research has shown that one-third of cancers could be prevented if nobody smoked or was exposed to tobacco, and roughly another 20% by maintaining a healthy weight, consuming alcohol at or below cancer prevention guidelines and following healthy patterns of diet and physical activity (World Cancer Research Fund 2010). In addition, the four modifiable risk factors mentioned above are recognized as the most effective targets in reducing the burden of chronic disease at a population level (United Nations 2011). This article discusses CCO's renewed prevention mandate, describes the approach recommended for chronic disease reduction in Ontario by the 2012 policy document Taking action to prevent chronic disease: recommendations for a healthier Ontario ("Taking Action") (Cancer Care Ontario/Public Health Ontario 2012) and highlights CCO's current evidence-based prevention initiatives.
The Ontario Cancer Plan III - A Renewed Prevention Mandate
CCO's primary prevention mandate – to develop evidence-based recommendations and initiatives with CCO partners that promote and support action on chronic-disease prevention – enables the organization to play a unique role in prevention activities in the province. In 2011, the Ontario Cancer Plan III was released (Cancer Care Ontario 2011). This plan for the cancer system outlined six goals; one of which specifically identified lessening Ontarians' risk of developing cancer. In addition, prevention is one of the five pillars of CCO's corporate strategy, and CCO has renewed its commitment to prevention by dedicating approximately $1 million yearly to the organization's prevention work. The mandate's emphasis on providing policy advice is supported by CCO's experience in measurement and public reporting and its ability to maximize and leverage partnerships to achieve a common goal.
It is important to note that the impact of cancer prevention efforts/work/activity requires a long view. Many cancers take a long time to develop and even the most successful prevention initiatives may not demonstrate results in terms of reduced cancer incidence for 20 years or longer. For example, while smoking rates for Ontario males began to decline around 1960, lung cancer incidence rates continued to increase until 1982 (Cancer Care Ontario 2002), before starting to decline. In this way, similar delays may be expected when considering the effects of policies geared towards tobacco exposure and control, such as smoking bans in public places and tobacco taxation. Nevertheless, while long-term goals of cancer prevention programs and policies may not be reflected at a population level for many years, the significant health benefits of risk factor reduction at the individual level, such as those of smoking cessation, are well-documented. While it is not possible to show changes in cancer rates in the near term, CCO continues to monitor the prevalence of major cancer risk factors through health surveys such as the Canadian Community Health Survey and other ongoing data sources.
Providing Evidence-Based Support and Policy Advice
In addition to the Taking Action initiative, CCO is instrumental in furthering provincial chronic disease prevention policy, such as tobacco control. As well, CCO frequently responds to emerging public health prevention issues and provides evidence-based support and leadership for diverse prevention activities. Key partnerships and initiatives are described in the following text.
The Taking Action Initiative
Taking action to prevent chronic disease: recommendations for a healthier Ontario is a comprehensive strategy document consisting of 22 recommendations to the provincial government for policy interventions aimed at reducing chronic disease. Released in 2012, the report is the result of a year-long partnership between CCO and Public Health Ontario.
While several other factors play an important role in the development of cancer, including genetics, ultraviolet (UV) radiation exposure and exposure to environmental and workplace carcinogens, Taking Action focuses on the key modifiable risk factors of tobacco use, alcohol consumption, physical inactivity and unhealthy eating. This is in keeping with the United Nations report on non-communicable diseases and in order to achieve maximal chronic disease reduction at the population level. Recommendations are wide-ranging and include actions targeted to education policy reform, taxation, socially responsible pricing, infrastructure and capacity, assessment and accountability and health equity (Table 1).
| Taking action to prevent chronic disease: recommendations for a healthier Ontario |
| Policy Recommendations and Interventions |
| 1. Increase tobacco tax |
| 2. Broaden and extend integrated tobacco cessation system |
| 3. Implement a sustained social marketing campaign for tobacco |
| 4. Ban smoking on unenclosed bar and restaurant patios |
| 5. Maintain and reinforce socially responsible pricing for alcohol |
| 6. Ensure effective controls on alcohol availability |
| 7. Strengthen targeted controls on alcohol marketing and promotion |
| 8. Increase access to brief counselling interventions |
| 9. Require physical education credits for high school graduation |
| 10. Evaluate daily physical activity in elementary schools |
| 11. Support active transportation |
| 12. Provide leadership through workplace physical activity policy |
| 13. Create an Ontario food and nutrition strategy |
| 14. Include compulsory food skills in curricula |
| 15. Support healthy eating in publicly funded institutions |
| 16. Implement mandatory menu labelling in food service operations |
| 17. Adopt a whole-of-government approach |
| 18. Improve measurement, increase accountability |
| 19. Connect knowledge with practice |
| 20. Implement a coordinated health communications campaign |
| 21. Reduce health inequities |
| 22. Address First Nations, Inuit and Métis health |
Current approaches to reducing exposure to modifiable chronic disease risk factors demonstrate that social, physical, economic and environmental factors all play important roles in influencing exposure and that policy interventions targeting these factors enable long-term population health gains. For example, greater access to alcohol is related to increased alcohol consumption and health-related problems (Popova et al. 2009). Policies affecting availability and access, such as government-controlled alcohol outlets, appropriate taxation and minimum pricing, have been effective in lowering consumption and reducing alcohol-related chronic disease.
The report also recommends a centrally coordinated, whole-of-government approach to policy development with collaborations between ministries and integration across all levels of government. Currently, tobacco use is the only key chronic disease risk factor subject to a comprehensive prevention strategy in Ontario – Smoke-Free Ontario (Cancer Care Ontario/Public Health Ontario 2012). For example, multiple government sectors, ministries and non-governmental agencies, in addition to the Ministry of Health and Long-Term Care (MOHLTC), are responsible for food and nutrition policy. To maximize effectiveness, Taking Action recommends a coordinated food and nutrition strategy that acknowledges the interconnectedness of food and nutrition programs and policies throughout agriculture, education, health, culture and social and economic development. Promising initiatives take into account the cross-sectorial nature of food and nutrition would be a cornerstone of a provincial food and nutrition strategy. For example, the government's pilot program, Fresh from the Farm: Healthy fundraising for Ontario schools, raises funds for schools by selling fresh Ontario produce to communities. The program delivers healthy food choices, encourages opportunities for learning about food and agriculture in the classroom and supports Ontario's farmers and the local economy. British Columbia and Nova Scotia have implemented provincially integrated food and nutrition strategies with good results (Cancer Care Ontario/Public Health Ontario 2012).
CCO is co-leading (with Dietitians of Canada and Sustain Ontario) the development of an Ontario Food and Nutrition Strategy. Through a collective impact model, more than 20 organizations have come together to design a strategy for the province that has the potential to support the health and well-being of Ontarians through a productive, equitable and sustainable food system. Strategic directions focus on: ensuring Ontarians access to healthy foods; providing opportunities to develop food literacy and skills; and enabling a diverse, healthy and resilient food production system that contributes to an equitable and prosperous economy (Sustain Ontario 2013).
In order for a whole-of-government approach to work, all sectors of the government must be engaged, as well as non-governmental partners and sectors outside of the traditional health system. So far, results are promising. Since the release of Taking Action, several milestones have been attained, including the planned renewal of Smoke-Free Ontario, a coordinated approach to smoking cessation in ambulatory settings at Regional Cancer Centres (RCCs), MOHLTC Healthy Kids Panel recommendations to reduce childhood obesity, a preliminary inter-ministerial meeting on food and nutrition programming and policies and the preparation of Taking Action recommendations designed in consultation with First Nations, Inuit and Métis in Ontario. A Taking Action report card, evaluating the progress of policy interventions, is planned for 2015.
Tobacco-Prevention Policy Advice and Support
CCO's Program Training and Consultation Centre (PTCC) is recognized as a leader in evidence-based tobacco prevention advice and is instrumental in furthering tobacco control and tobacco use reduction policy in support of the MOHLTC's Smoke-Free Ontario strategy. In partnership with the University of Waterloo, the PTCC conducts applied research, collecting and synthesizing scientific and practice-based evidence, to support tobacco control planning and decision-making. This expertise is used to provide training, technical assistance and knowledge exchange services to public health practitioners working in tobacco control. In addition, PTCC's health promotion specialists provide direct field support to Ontario's 36 public health departments and seven tobacco control area networks to assist them in effectively implementing tobacco control initiatives.
The PTCC also fosters knowledge exchange among decision-makers, practitioners and researchers through provincial communities of practice (CoP), through which groups of peers meet to deepen their understanding and build a collective knowledge base. The Tobacco Use Reduction for Young Adults CoP, for example, aims to enhance knowledge exchange and provide a platform for problem-solving and skill development in tobacco use reduction for young adults aged 18–34, the age group which has the highest smoking rate in Canada.
Policy Advice on Emerging Issues
CCO's success in providing evidence-based advice is closely tied to its ability to respond to emerging issues. In early 2012, a bill was put forward to ban tanning bed use for individuals under age 18. Use of tanning equipment has been associated with the development of skin cancer, with increased risk for people who first use tanning beds before age 35 (International Agency for Research on Cancer 2012). Tanning bed legislation is already in place in five other provinces. In support of the bill, CCO prepared briefing notes summarizing the evidence. In 2013, the Skin Cancer Prevention Act was passed in Ontario, legislating the banning of tanning beds for individuals under age 18 and prohibiting youth-targeted marketing.
In relation to alcohol consumption, CCO recently used its expertise and published research to publicly counter the government's intention to expand liquor sales to grocery outlets and the sale of wine at farmers' markets, providing evidence that alcohol is carcinogenic and that policy actions to facilitate access have been demonstrated to increase consumption and, thereby, increase the associated chronic disease health risks.
Cancer System Quality Improvement through Measurement – A Prevention System Quality Index
Building on its experience in metrics, measurement, surveillance and reporting, CCO is developing a framework for assessing the performance of the prevention system. The long-term goal of assessment is to identify policy gaps and recommend actions, so that the prevention system can be improved to support reduction in risk factors and, ultimately, in cancer and chronic disease incidence. Measurement of prevention activity at the system level – encompassing legislation, strategies, policies and programs – is not currently coordinated in Ontario. CCO's Prevention System Quality Index (PSQI) envisages a set of metrics for reporting on these factors, where there is evidence that they influence risk factor prevalence.
For example, while the online Cancer System Quality Index (CSQI) currently reports on the proportion of Ontarians at risk due to higher than recommended levels of alcohol consumption it did not report on system-level factors that influence exposure, such as policy-related disincentives like alcohol pricing or retail access, until 2014.
Similar to the CSQI, the PSQI's intention is to enable the reporting of system-level indicators at the regional level over time, including comparison with other jurisdictions wherever possible. Public reporting will allow for successful efforts to be recognized as well as system improvement to occur. Where policy-related shortfalls or gaps are identified, actions such as monitoring, regulation and enforcement can be recommended. Initial system-level indicators related to alcohol policy and environmental exposures are included in the 2014 CSQI. To our knowledge, this is the first coordinated attempt at assessing primary prevention at a system level in the country.
Providing Evidence-Based Support for Risk Reduction
My CancerIQ
Research suggests that individuals may over- or under-estimate their cancer risk and that there is a need for better cancer risk information and engagement among the public (Colditz et al. 2000). The MOHLTC funded CCO to create an online tool that will allow Ontarians to assess their personal cancer risk and learn about risk factors, disease prevention and cancer screening. In an effort to encourage Ontarians to engage in prevention activities, My CancerIQ provides links to provincial and community supports, such as programs geared towards smoking cessation and healthy eating. Built on an evidence-based algorithm, the first release (early 2015) of My CancerIQ focuses on lung, female breast, colorectal and cervical cancers. In addition to increasing Ontarians' knowledge about disease prevention, My CancerIQ can be used as a platform to inform discussions with healthcare providers and is intended to increase awareness and uptake of breast, colorectal and cervical cancer screening (Figure 2).
Population Cancer Risk Factor Profiles
An important support provided by CCO to internal divisions, regional cancer programs and chronic disease partners is specific cancer risk profiles. In-depth analyses are conducted to provide a deep understanding of cancer risk factors as they occur over time, by sex, in youth (where data are available), among sub-populations and as they affect equity (e.g., median cigarette smoking by sex, age or income group). The analyses are used to inform prevention and policy work. For example, CCO's monthly Cancer Fact Sheets are often timed to coincide with public health and awareness campaigns on topics such as smoking cessation.
In addition, Cancer Risk Factors in Ontario – in-depth epidemiologic reports describing how specific risk factors influence the development of cancer and other chronic diseases in the province – are used to inform prevention recommendations, ensuring they are based on a foundation of evidence. Because the epidemiological analysis in the reports may reveal that a risk factor affects a particular sub-population disproportionately, the information can also be used to help plan interventions and as a baseline for reporting. Cancer Risk Factor reports on tobacco use and alcohol consumption were released in 2014 and provide scientific information to assist in informing the development of Taking Action policy recommendations and prevention initiatives.
Sun Safety Messaging
Excess exposure to the sun and other sources of UV radiation increases the risk of skin cancer and some eye diseases. Melanoma, which is the main cause of skin cancer mortality, is the sixth most commonly occurring cancer in the country (Canadian Cancer Society 2013). Evidence shows that Canadians are spending an increasing amount of time in the sun without increasing their protection, suggesting that more needs to be done to inform them about the risks of UV exposure (The Ontario Sun Safety Working Group 2010).
In an effort to reduce overexposure to UV radiation, the Ontario Sun Safety Working Group (of which CCO is a member) has led a process to update public sun safety messages, identifying gaps and reflecting current evidence. CCO is working with relevant system partners (Canadian Cancer Society, Canadian Dermatology Association) to build a consensus process to ensure broad, national and cross-provincial agreement on and adoption of consistent, evidence-based sun safety messages.
Conclusion
CCO's most important contribution to cancer and chronic disease prevention is its ability to provide scientific, evidence-based advice to support the effective implementation of policy, promote action on chronic disease prevention, increase the effectiveness of the prevention system and work towards health equity. CCO's expertise in generating new knowledge, summarizing evidence and measuring and reporting on progress in risk factor reduction is central to this process. The policy document Taking action to prevent chronic disease: recommendations for a healthier Ontario presents a strategy for policy interventions aimed at reducing chronic disease in the province and forms a platform for future prevention work. Maintaining the expertise and fluidity to respond to and support emerging legislative and policy developments and maximizing collaborations with external organizations and chronic disease partners to achieve common goals are key to the success of CCO's prevention work.
About the Author(s)
Mary Spayne, BA, MPH, is an epidemiologist and scientific and medical writer. A graduate of the UHN Rotman Leadership Development Program, she was a Public Affairs Fellow with the CORO Foundation.
Linda Rabeneck, MD, MPH, FRCPC, is the Vice-President, Prevention and Cancer Control, at Cancer Care Ontario. She is a Professor of Medicine; Professor of Health Policy, Management and Evaluation; and Professor, Dalla Lana School of Public Health at the University of Toronto. Dr. Rabeneck also holds an appointment as a Senior Scientist at the Institute for Clinical Evaluative Sciences (ICES).
Loraine Marrett, PhD, is a Senior Scientist and former Director, Prevention & Surveillance at Cancer Care Ontario.
Alice Peter, MA, MBA, is the Director, Population Health and Prevention at Cancer Care Ontario.
Acknowledgment
The authors gratefully acknowledge Beth Theis, Shawn Chirrey, Steven Savvaidis and Rebecca Truscott for their help in the development and review of this manuscript.
References
Canadian Cancer Society's Steering Committee. 2013. Canadian Cancer Statistics. Toronto, ON: Canadian Cancer Society.
Cancer Care Ontario. 2002. Tobacco or Health in Ontario. Retrieved March 7, 2014. <https://www.cancercare.on.ca/common/pages/UserFile.aspx?fileId=14456>.
Cancer Care Ontario. 2011. Ontario Cancer Plan 2011–2015. Retrieved January 22, 2014. <http://ocp.cancercare.on.ca/>.
Cancer Care Ontario, Ontario Agency for Health Protection and Promotion (Public Health Ontario). 2012. Taking Action to Prevent Chronic Disease: Recommendations for a Healthier Ontario. Retrieved January 22, 2014. <https://www.cancercare.on.ca/pcs/prevention/healthieron/?WT.mc_id=/takingaction>.
Cancer Quality Council of Ontario. 2014. Annual Cancer System Quality Index (CSQI). <www.csqi.on.ca>.
Colditz, G.A., K.A. Atwood, K. Emmons, R.R. Monson, W.C. Willett, D. Trichopoulos et al. 2000. "Harvard Report on Cancer Prevention. Volume 4: Harvard Cancer Risk Index." Cancer Causes and Control 11: 477–88.
International Agency for Research on Cancer. 2012. IARC Monographs on the Evaluation of Carcinogenic Risks to Humans. Volume 100D. A Review of Human Carcinogens. Part D: Radiation. Lyon: IARC.
Popova, S., N. Giesbrecht, D. Bekmuradov and J. Patra. 2009. "Hours and Days of Sale and Density of Alcohol Outlets: Impacts on Alcohol Consumption and Damage: A Systematic Review." Alcohol 44(5): 500–16.
Sustain Ontario. 2013. Draft Ontario Food and Nutrition Strategy. Retrieved March 7, 2014. <http://sustainontario.com/initiatives/ontario-food-and-nutrition-strategy>.
The Ontario Sun Safety Working Group. 2010. Sun Exposure and Protective Behaviours in Ontario: An Ontario Report Based on the 2006 Second National Sun Survey. Toronto, ON: Canadian Cancer Society (Ontario Division). Retrieved March 7, 2014. <https://www.cancercare.on.ca/common/pages/UserFile.aspx?fileId=87528>.
United Nations, General Assembly. 2011. Prevention and Control of Non-Communicable Diseases. Report of the Secretary-General (A/66/83). Retrieved January 22, 2014. <http://www.un.org/ga/search/view_doc.asp?symbol=A/66/83&Lang=E>.
World Cancer Research Fund/American Institute for Cancer Research. 2010. Policy and Action for Cancer Prevention: Food, Nutrition, and Physical Activity. Washington, DC: American Institute for Cancer Research (AICR).
World Health Organization, Commission on Social Determinants of Health. 2008. Closing the Gap in a Generation: Health Equity through Action on the Social Determinants of Health, Final Report. Retrieved January 22, 2014. <http://whqlibdoc.who.int/publications/2008/9789241563703_eng.pdf>.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed