Healthcare Quarterly
Rheumatoid Arthritis Surveillance in Ontario: Monitoring the Burden, Quality of Care and Patient Outcomes through Linkage of Administrative Health Data
Jessica Widdifield, Sasha Bernatsky, Claire Bombardier and Michael Paterson
Abstract
Rheumatoid arthritis (RA) is the most common chronic inflammatory joint disease. Using the Ontario administrative health data housed at the Institute for Clinical Evaluative Sciences, researchers have quantified the population-level burden and epidemiology of RA, mapped its geographic distribution in relation to rheumatologist supply, studied trends in access to rheumatology care and treatment and evaluated patient outcomes. The findings highlight the excess morbidity and mortality associated with the growing burden of RA in the face of a strained rheumatology supply, and raise urgent questions about how best to meet the needs of Ontarians with RA.
The Issue
Given the rising levels of chronic disease and multimorbidity in Canada, researchers and decision-makers are increasingly looking to administrative health data as an information source for chronic disease detection and surveillance. Rheumatoid arthritis (RA) is just one condition for which administrative data-based research on disease burden, quality of care and patient outcomes is helping to transform the lives of Canadians with chronic disease.
RA is the most common chronic inflammatory joint disease, affecting millions of people worldwide, and one of the most disabling and costly of all chronic diseases (Cross et al. 2014). At disease onset, RA is considered a medical emergency requiring prompt referral to a rheumatologist. To control symptoms and inhibit disease progression, treatment guidelines include disease-modifying antirheumatic drugs (DMARDs), biologic agents such as anti-tumour necrosis factor agents and corticosteroids (Bykerk et al. 2012). However, uncontrolled RA activity can lead to irreversible joint damage requiring surgery, multiple comorbidities and premature mortality. Many factors contribute to increased morbidity and mortality in patients with RA, including immune abnormalities, organ system manifestations associated with the disease, genetic predisposition, the immunosuppressive and cytotoxic effects of treatments and, possibly, poor quality of care.
Here we highlight some recent Institute for Clinical Evaluative Sciences (ICES) research aimed at helping to improve the care and outcomes of patients with RA.
Key Findings
Optimizing Administrative Data Accuracy
Validation of administrative data for identifying patients with various health states improves our understanding of when and how such data can be used for chronic disease surveillance and research. To assess the accuracy of administrative data for identifying RA patients, two independent validation studies were performed at ICES (Widdifield et al. 2013a, 2014a). This foundational work led to the establishment of the Ontario Rheumatoid Arthritis Database (ORAD), a validated, population-based registry. Derived by linking physician service claims, hospital discharge abstracts and public health insurance records, ORAD is just one of several validated, ICES-derived chronic disease cohorts.
RA Burden and Epidemiology
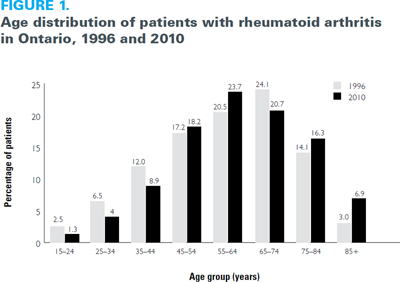
The number of RA patients in Ontario increased steadily from 42,734 (0.5%) in 1996 to 97,499 (0.9%) in 2010. The crude number of new patients diagnosed each year varied from 5,523 patients in 1996 to 6,395 patients in 2010. After standardizing for age and sex, RA prevalence per 100,000 population showed a steady increase over time, from 473 in 1996 to 784 in 2010. Prevalence also increased with advancing age, and approximately twice as many women as men were affected. Age- and sex-standardized incidence per 100,000 varied from 62 in 1996 to 54 in 2010. Incidence rates were highest among women and also increased with age. Between 1996 and 2010, in keeping with the province's aging population, the age profile of the RA population changed (Figure 1). As of 2010, 44% of persons with RA were 65 years and older, and 72% were female. Geographic variation was also evident, with prevalence being higher in northern rural communities than in southern urban areas (Widdifield et al. 2013b).
Timely Access to Specialty Care
Despite the increasing RA burden over the past decade, the number of rheumatologists in Ontario has remained relatively stable at 160, or 1.5 rheumatologists per 100,000 population (Widdifield et al. 2014b). Moreover, few rheumatologists are located in northern communities where RA prevalence is high (Widdifield et al. 2014b). Despite the shortage, access to rheumatologists has improved among patients newly diagnosed with RA (Widdifield et al. 2014c). Greater exposure to DMARDs for new or "incident" RA patients has also occurred over time, reflective of the increasing access to rheumatologists (Widdifield et al. 2011). These findings also highlight improvements relative to RA guideline implementation (Bernatsky et al. 2009). However, established wait-time measure benchmarks are seldom achieved, as only 38% of RA patients are seen within four weeks from their referral date (the target is 100%) (Widdifield et al. 2014d).
Outcomes Important to RA Patients
Greater cumulative exposures to DMARDs within one year of RA diagnosis have been shown to be associated with reductions in the need for joint surgery (Widdifield et al. 2015a); this could reflect the joint-sparing effects of DMARDs. However, patients undergoing joint surgery are at higher risk for complications. Dislocation following total hip arthroplasty and infection following total knee arthroplasty are more common among RA patients compared with patients with osteoarthritis (Ravi et al. 2014a). Moreover, increased surgeon experience in performing joint arthroplasty in RA patients, irrespective of hospital factors, has been associated with a lower risk of surgical complications (Ravi et al. 2014b).
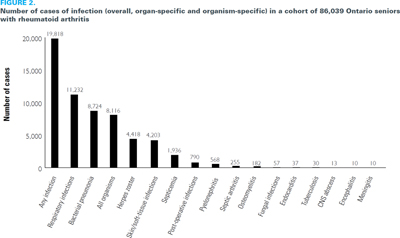
Experiencing a serious infection is relatively common in older adults with RA, occurring at a rate of 46 events per 1,000 patient-years. The most frequently occurring infections include respiratory infections (Figure 2). While the risk of infection was elevated for all DMARDs, the increased infection rate was most strongly associated with corticosteroid use. However, comorbidities also increased infection risk (Widdifield et al. 2013c). Mycobacterial infections while relatively rare in the general population are more common in RA patients and increase the risk of death (Brode et al. 2014). Biologic therapies and DMARDs also appear to be associated with mycobacterial infections (Brode et al. 2015).
All-cause mortality for Ontarians with RA has decreased over the past decade but remains elevated compared with the general population, with 40–50% more deaths among RA patients. This relative excess mortality is strongest among the younger age groups and has improved little over the last decade (Widdifield et al. 2015b).
Disparities in Care and Outcomes
Everyone deserves to receive similar high-quality care, yet patients in rural areas have reduced accessed to rheumatology care (Widdifield et al. 2014c), are more likely to experience adverse events (Widdifield et al. 2013c, Brode et al. 2014, Ravi et al. 2014a) and are at greater risk of early death (Widdifield et al. 2015c). Male patients are also at relatively greater risk of early death (Widdifield et al. 2015b). Finally, patients of lower socioeconomic status are less likely to receive timely rheumatology care (Widdifield et al. 2014c).
Implications
The increasing RA burden in Ontario and the significant morbidity and mortality associated with these patients suggest that efforts to address this disease are not meeting the burden it imposes. The number of RA patients has more than doubled in the past 15 years. Without a parallel increase in the number of rheumatologists, health human resources shortages and geographic variation in the supply of rheumatology services will further strain our healthcare system if policymakers fail to respond to the needs of this vulnerable population. Furthermore, the changing demographics of the RA population have implications regarding appropriate health services provision in delivering high-quality, patient-centred care. Compared with the younger population, older patients tend to have more comorbidities and the resultant polypharmacy can further complicate chronic disease management.
Some progress has been made in improving access to appropriate care for RA patients. However, much more can be done, particularly for patients in rural areas, who have poorer access to specialists and are more likely to experience adverse health outcomes. Proactive, tailored approaches are needed to provide appropriate care to such populations.
The significant morbidity and excess mortality among RA patients has implications for clinical decision-making, as these patients require enhanced vigilance in the management of their pharmacotherapy and comorbidities. Their greater risk for surgical complications also has implications for surgical decision-making. Moreover, the finding that more experienced surgeons have fewer complications has important implications for surgical training and practice (Rodriguez-Elizalde et al. 2012).
In sum, administrative data have played a critical role in improving our understanding of the disease burden, quality of care and outcomes in Ontarians with RA. The growing RA burden is exceeding rheumatology supply, yet for rheumatologists to provide optimal care, they must see new patients sooner while monitoring existing patients more closely to prevent adverse outcomes. This challenges current models of care. Innovations are urgently needed if we are to keep pace with the growing needs of Ontarians with RA.
About the Author(s)
Jessica Widdifield, PhD, is a postdoctoral research fellow at the Institute for Clinical Evaluative Sciences (ICES) and McGill University. She is supported by fellowship awards from The Arthritis Society and the Canadian Institutes of Health Research.
Sasha Bernatsky, MD, FRCPC, PhD, is a rheumatologist, a medical scientist in the Divisions of Clinical Epidemiology and Rheumatology at the McGill University Health Centre and an associate professor in the Department of Medicine at McGill University. She holds a career award from the Fonds de la recherche en santé du Québec.
Claire Bombardier, MD, FRCPC, is a rheumatologist at Mount Sinai Hospital in Toronto, a professor of medicine at the University of Toronto and a senior scientist at the University Health Network, the Toronto General Research Institute and the Institute for Work and Health. She holds a Canada Research Chair in Knowledge Transfer for Musculoskeletal Care and a Pfizer Research Chair in Rheumatology.
Michael Paterson, MSc, is a scientist and lead of the Chronic Disease and Pharmacotherapy Research Program at ICES. He is also an assistant professor in the Department of Family Medicine at McMaster University and the Institute of Health Policy, Management and Evaluation at the University of Toronto.
References
Bernatsky, S., M. Paterson, C. Thorne, A. Cividino, J. Pope, J. Hux et al. 2009. "Potential Effects of a National Consensus Statement on Optimal Treatment of Early Rheumatoid Arthritis in Ontario." Scandinavian Journal of Rheumatology 38(5): 390–91.
Brode, S.K., F.B. Jamieson, R. Ng, M.A. Campitelli, J.C. Kwong, J.M. Paterson et al. 2014. "Risk of Mycobacterial Infections Associated with Rheumatoid Arthritis in Ontario, Canada." Chest 146(3): 563–72.
Brode, S.K., F.B. Jamieson, R. Ng, M.A. Campitelli, J.C. Kwong, J.M. Paterson et al. 2015. "Increased Risk of Mycobacterial Infections Associated with Anti-Rheumatic Medications." Thorax 70(7): 677–82.
Bykerk, V.P., P. Akhavan, G.S. Hazlewood, O. Schieir, A. Dooley, B. Haraoui et al. 2012. "Canadian Rheumatology Association Recommendations for Pharmacological Management of Rheumatoid Arthritis with Traditional and Biologic Disease-Modifying Antirheumatic Drugs." Journal of Rheumatology 39(8): 1559–82.
Cross, M., E. Smith, D. Hoy, L. Carmona, F. Wolfe, T. Vos et al. 2014. "The Global Burden of Rheumatoid Arthritis: Estimates from the Global Burden of Disease 2010 Study." Annals of the Rheumatic Diseases 73(7): 1316–22.
Ravi, B., R. Croxford, S. Hollands, J.M. Paterson, E. Bogoch, H. Kreder et al. 2014a. "Increased Risk of Complications Following Total Joint Arthroplasty in Patients with Rheumatoid Arthritis." Arthritis and Rheumatology 66(2): 254–63.
Ravi, B., R. Croxford, P.C. Austin, S. Hollands, J.M. Paterson, E. Bogoch et al. 2014b. "Increased Surgeon Experience with Rheumatoid Arthritis Reduces the Risk of Complications Following Total Joint Arthroplasty." Arthritis and Rheumatology 66(3): 488–96.
Rodriguez-Elizalde, S., R. Jenkinson, H. Kreder and J.M. Paterson. 2012. "Provider Volumes and Surgical Outcomes in Total Hip and Knee Replacement." In S.K. Fokter, Ed., Recent Advances in Arthroplasty. Rijeka, Croatia: InTech.
Widdifield, J., S. Bernatsky, J.M. Paterson, J.C. Thorne, A. Cividino, J. Pope et al. 2011. "Quality Care in Seniors with New-Onset Rheumatoid Arthritis: A Canadian Perspective." Arthritis Care and Research (Hoboken) 63(1): 53–57.
Widdifield, J., S. Bernatsky, J.M. Paterson, K. Tu, R. Ng, J.C. Thorne et al. 2013a. "Accuracy of Canadian Health Administrative Databases in Identifying Patients with Rheumatoid Arthritis: A Validation Study Using the Medical Records of Rheumatologists." Arthritis Care and Research (Hoboken) 65(10): 1582–91.
Widdifield, J., J.M. Paterson, S. Bernatsky, K. Tu, J.C. Thorne, V. Ahluwalia et al. 2013b. "The Rising Burden of Rheumatoid Arthritis Surpasses Rheumatology Supply in Ontario." Canadian Journal of Public Health 104(7): e450–55.
Widdifield, J., S. Bernatsky, J.M. Paterson, N. Gunraj, J.C. Thorne, J. Pope et al. 2013c. "Serious Infections in a Population-Based Cohort of 86,039 Seniors with Rheumatoid Arthritis." Arthritis Care and Research (Hoboken) 65(3): 353–61.
Widdifield, J., C. Bombardier, S. Bernatsky, J.M. Paterson, D. Green, J. Young et al. 2014a. "An Administrative Data Validation Study of the Accuracy of Algorithms for Identifying Rheumatoid Arthritis: The Influence of the Reference Standard on Algorithm Performance." BMC Musculoskeletal Disorders 15: 216.
Widdifield, J., J.M. Paterson, S. Bernatsky, K. Tu, G. Tomlinson, B. Kuriya et al. 2014b. "The Epidemiology of Rheumatoid Arthritis (RA) in Ontario, Canada." Arthritis and Rheumatology 66(4): 786–93.
Widdifield, J., J.M. Paterson, S. Bernatsky, K. Tu, J.C. Thorne, N. Ivers et al. 2014c. "Access to Rheumatologists among Patients with Newly Diagnosed Rheumatoid Arthritis in a Canadian Universal Public Healthcare System." BMJ Open 4(1): e003888.
Widdifield, J., C. Bombardier, J.C. Thorne, R.L. Jaakkimainen, J.M. Paterson, S. Bernatsky et al. 2014d. "A Novel Approach to Assess Wait-Times to Rheumatologists." Arthritis and Rheumatology 66(Suppl 10): 2309
Widdifield, J., C.S. Moura, Y. Wang, M. Abrahamowicz, M. Beauchamp, J.M. Paterson et al. 2015a. "The Influence of Drug Exposures on Joint Surgeries in Rheumatoid Arthritis Patients: Cross-Provincial Comparisons." Annals of the Rheumatic Diseases 74(Suppl 2): 72.
Widdifield, J., S. Bernatsky, J.M. Paterson, G. Tomlinson, K. Tu, B. Kuriya et al. 2015b. "Trends in Excess Mortality among Patients with Rheumatoid Arthritis in Ontario, Canada." Arthritis Care and Research (Hoboken) 67(8): 1047–53.
Widdifield, J., M. Abrahamowicz, J.M. Paterson, C. Bombardier, G. Tomlinson, A. Huang et al. 2015c. "The Influence of Drug Exposures and Comorbidity on Survival in Seniors with Rheumatoid Arthritis." Annals of the Rheumatic Diseases 74(Suppl 2): 321.
Comments
Be the first to comment on this!
Personal Subscriber? Sign In
Note: Please enter a display name. Your email address will not be publically displayed